Imaging of Central Metatarsalgia
Total Page:16
File Type:pdf, Size:1020Kb
Load more
Recommended publications
-

Chief Complaint
Chief Complaint Please choose the primary reason you are coming to our office. Complaints are listed alphabetically. Please do not select more than 5 complaints. Upper Back: Thigh/Hip: Calf: o Asthma o Arterial insufficiency o Left calf pain o Bronchitis o Left hip pain o Left leg cramps o Emphysema o Left hip tendonitis o Left leg numbness o Left Flank Pain o Left leg cramps o Left leg pain o Midback pain o Left leg numbness o Left leg weakness o Left leg pain o Leg cramps Lower Back: o Left leg weakness o Leg numbness o Fatigue o Left post. thigh pain o Leg weakness o Left flank pain o Left thigh pain o Varicose veins o Low back pain o Sciatica o Venous insufficiency o Low back spasm o Venous insufficiency o Arterial insufficiency o Lumbar arthritis o Right hip pain o Right calf pain o Menstrual cramps o Right hip tendonitis Right leg o Right leg cramps o Nervousness cramps o Right leg numbness o Pain during BM o Right leg numbness o Right leg pain o Right flank pain o Right leg pain o Right leg weakness o Sacroiliac pain o Right leg weakness o Sciatica o Right post. thigh pain Neck: o Stiffness o Right thigh pain o Bronchitis o Whole body pain o Clavicular pain Head: Buttocks: o Cold o Agitation o Bleeding during BM o Coughing o Anxiety attack o Bursitis of hip o Dysphagia o Cold o Gluteal pain o Goiter o Diminished concentration o Hemorrhoids o Hoarseness o Dizziness o Left gluteal pain o Neck pain o Dysphagia o Left hip pain o Neck spasm o Ear pain o Left post. -

Acral Manifestations of Soft Tissue Tumors Kristen M
Clinics in Dermatology (2017) 35,85–98 Acral manifestations of soft tissue tumors Kristen M. Paral, MD, Vesna Petronic-Rosic, MD, MSc⁎ Section of Dermatology, University of Chicago Pritzker School of Medicine, Chicago, IL Abstract This group of biologically diverse entities is united by topographic localization to the hands and feet. Categorizing tumors by body site narrows the differential into a short list of possibilities that can facil- itate accurate and rapid diagnosis. The goal of this review is to provide a practical approach to soft tissue tumors of acral locations for clinicians, pathologists, and researchers alike. What ensues in the following text is that tight coupling of the clinical picture and histopathologic findings should produce the correct diagno- sis, or at least an abbreviated differential. The salient clinicopathologic, immunohistochemical, and molec- ular features are presented alongside current treatment recommendations for each entity. © 2017 Elsevier Inc. All rights reserved. Introduction actin (SMA) and are deemed “myofibroblasts.”1 The tumors under this heading express combinations of CD34, FXIIIa, fi The entities presented herein are categorized on the basis of and SMA. The synthesis of collagen by broblasts translates fi fi morphogenesis (where possible) and by biologic potential as to a brous consistency that clinically imparts a rm texture benign, intermediate, and malignant neoplasms. on palpation, and, macroscopically, a gray-white or white-tan cut surface. The entities discussed next have no metastatic po- tential; that is, simple excision is adequate. Fibrous and related tissues: Benign lesions Fibroma of tendon sheath fi fl The ontogenetic classi cation of benign lesions re ects appar- Also known as tenosynovial fibroma, compared with other fi fi fi ent broblastic or broblast-like morphogenesis. -
Billing and Coding: Injections - Tendon, Ligament, Ganglion Cyst, Tunnel Syndromes and Morton's Neuroma (A57079)
Local Coverage Article: Billing and Coding: Injections - Tendon, Ligament, Ganglion Cyst, Tunnel Syndromes and Morton's Neuroma (A57079) Links in PDF documents are not guaranteed to work. To follow a web link, please use the MCD Website. Contractor Information CONTRACTOR NAME CONTRACT TYPE CONTRACT JURISDICTION STATE(S) NUMBER Noridian Healthcare Solutions, A and B MAC 01111 - MAC A J - E California - Entire State LLC Noridian Healthcare Solutions, A and B MAC 01112 - MAC B J - E California - Northern LLC Noridian Healthcare Solutions, A and B MAC 01182 - MAC B J - E California - Southern LLC Noridian Healthcare Solutions, A and B MAC 01211 - MAC A J - E American Samoa LLC Guam Hawaii Northern Mariana Islands Noridian Healthcare Solutions, A and B MAC 01212 - MAC B J - E American Samoa LLC Guam Hawaii Northern Mariana Islands Noridian Healthcare Solutions, A and B MAC 01311 - MAC A J - E Nevada LLC Noridian Healthcare Solutions, A and B MAC 01312 - MAC B J - E Nevada LLC Noridian Healthcare Solutions, A and B MAC 01911 - MAC A J - E American Samoa LLC California - Entire State Guam Hawaii Nevada Northern Mariana Created on 09/28/2019. Page 1 of 33 CONTRACTOR NAME CONTRACT TYPE CONTRACT JURISDICTION STATE(S) NUMBER Islands Article Information General Information Original Effective Date 10/01/2019 Article ID Revision Effective Date A57079 N/A Article Title Revision Ending Date Billing and Coding: Injections - Tendon, Ligament, N/A Ganglion Cyst, Tunnel Syndromes and Morton's Neuroma Retirement Date N/A Article Type Billing and Coding AMA CPT / ADA CDT / AHA NUBC Copyright Statement CPT codes, descriptions and other data only are copyright 2018 American Medical Association. -

Clinical Guidelines: Foot / Ankle
Clinical Guidelines: Foot / Ankle Plantar Fasciitis/Heel spurs: Initial Evaluation: History includes usually atraumatic plantar medial heel pain, worst first thing in the morning or after prolonged sitting. Exam includes tenderness with deep palpation of the plantar medial heel. Squeezing the heel bone side to side is NOT tender, but if present could represent a calcaneal stress fracture. X-rays may or may not reveal a heel spur, but the spur is NOT the source of the pain despite podiatry frequently referring to this as “heel spur syndrome.” Follow-up: The plantar fascia is the soft tissue under our foot that runs from the heel to the toes, much like the palm of our hand; it is the sole of our foot. The plantar fascia stretch includes crossing your legs and dorsiflexing the ankle and stretching the toes into extension. This is the most effective stretch. A night splint is imperative for improvement and should be used at night for 6 weeks. Cortisone injections and physical therapy can be helpful. NSAIDS and a frozen water bottle rolled on the plantar foot could be used with the above treatment, but the most effective treatment is a night splint. Referral: 90% of heel pain resolves with non-op treatment, but make a referral to a foot / ankle ortho surgeon with any atypical heel pain or failure of 6-8 weeks of non-operative treatment. Atypical heel pain usually gets an MRI, but classic plantar fasciitis does not. Bunion (hallux valgus): Initial Treatment: Bunion deformity includes a bump on the medial side of the big toe, the big toe going the wrong way, and a widened forefoot. -

The Best Diagnosis Is
Dermatopathology Diagnosis Superficial Plantar Fibromatosis The best diagnosis is: H&E, original magnification 40. a. dermatofibroma b. keloid CUTISc. neurofibroma d. nodular fasciitis Do Note. superficialCopy plantar fibromatosis H&E, original magnification 400. PLEASE TURN TO PAGE 225 FOR DERMATOPATHOLOGY DIAGNOSIS DISCUSSION Luke Lennox, BA; Anna Li, BS; Thomas N. Helm, MD Mr. Lennox and Dr. Helm are from the Department of Dermatology, University at Buffalo, The State University of New York. Ms. Li is from the Department of Dermatology, Ross University, Dominica, West Indies. The authors report no conflict of interest. Correspondence: Thomas N. Helm, MD, Dermatopathology Laboratory, 6255 Sheridan Dr, Building B, Ste 208, Williamsville, NY 14221 ([email protected]). 220 CUTIS® WWW.CUTIS.COM Copyright Cutis 2013. No part of this publication may be reproduced, stored, or transmitted without the prior written permission of the Publisher. Dermatopathology Diagnosis Discussion Superficial Plantar Fibromatosis lantar fibromatosis typically presents as firm represents a reactive proliferation of spindle cells most plaques or nodules on the plantar surface of the often encountered on the extremities of young adults. Pfoot.1 The process is caused by a proliferation of Spindle cells are loosely arranged in a mucinous fibroblasts and collagen and has been associated with stroma and are not circumscribed (tissue culture ap- trauma, liver disease, diabetes mellitus, epilepsy, and pearance). Vesicular nuclei are encountered, but there alcoholism.2 Unlike the fibromatoses associated with is no remarkable nuclear pleomorphism. Extravasated Gardner syndrome, superficial plantar fibromatosis has not been associated with abnormalities in the ade- nomatous polyposis coli gene or with the -catenin gene.3,4 Lesions typically present in middle-aged or elderly individuals and involve the medial plantar fas- cia. -
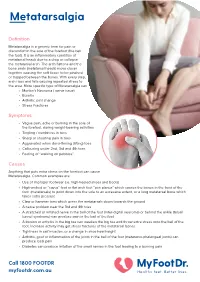
Metatarsalgia
Metatarsalgia Definition Metatarsalgia is a generic term for pain or discomfort in the sole of the forefoot (the ball of the foot). It is an inflammatory condition of the metatarsal heads due to a drop or collapse of the metatarsal arch. The arch flattens and the bone ends (metatarsal heads) move closer together causing the soft tissue to be pinched or trapped between the bones. With every step, the arch rises and falls causing repeated stress to the area. More specific type of Metatarsalgia can be: • Morton’s Neuroma ( nerve issue) • Bursitis • Arthritic joint change • Stress Fractures Symptoms • Vague pain, ache or burning in the sole of the forefoot, during weight-bearing activities • Tingling / numbness in toes • Sharp or shooting pain in toes • Aggravated when dorsi-flexing (lifting) toes • Callousing under 2nd, 3rd and 4th toes • Feeling of “walking on pebbles” Causes Anything that puts extra stress on the forefoot can cause Metatarsalgia. Common examples are: • Use of improper footwear (i.e. high-heeled shoes and boots) • High-arched or “cavus” foot or flat arch feet “pes planus” which causes the bones in the front of the foot (metatarsals) to point down into the sole to an excessive extent, or a long metatarsal bone which takes extra pressure • Claw or hammer toes which press the metatarsals down towards the ground • A nerve problem near the 3rd and 4th toes • A stretched or irritated nerve in the ball of the foot (inter-digital neuroma) or behind the ankle (tarsal tunnel syndrome) can produce pain in the ball of the foot • A bunion or arthritis in the big toe can weaken the big toe and throw extra stress onto the ball of the foot. -

Chronic Foot Pain
Revised 2020 American College of Radiology ACR Appropriateness Criteria® Chronic Foot Pain Variant 1: Chronic foot pain. Unknown etiology. Initial imaging. Procedure Appropriateness Category Relative Radiation Level Radiography foot Usually Appropriate ☢ US foot Usually Not Appropriate O MRI foot without and with IV contrast Usually Not Appropriate O MRI foot without IV contrast Usually Not Appropriate O CT foot with IV contrast Usually Not Appropriate ☢ CT foot without and with IV contrast Usually Not Appropriate ☢ CT foot without IV contrast Usually Not Appropriate ☢ Bone scan foot Usually Not Appropriate ☢☢☢ Variant 2: Persistent posttraumatic foot pain. Radiographs negative or equivocal. Clinical concern includes complex regional pain syndrome type I. Next imaging study. Procedure Appropriateness Category Relative Radiation Level MRI foot without IV contrast Usually Appropriate O 3-phase bone scan foot Usually Appropriate ☢☢☢ MRI foot without and with IV contrast May Be Appropriate O US foot Usually Not Appropriate O CT foot with IV contrast Usually Not Appropriate ☢ CT foot without and with IV contrast Usually Not Appropriate ☢ CT foot without IV contrast Usually Not Appropriate ☢ Variant 3: Chronic metatarsalgia including plantar great toe pain. Radiographs negative or equivocal. Clinical concern includes sesamoiditis, Morton’s neuroma, intermetatarsal bursitis, chronic plantar plate injury, or Freiberg’s infraction. Next imaging study. Procedure Appropriateness Category Relative Radiation Level MRI foot without IV contrast Usually Appropriate O US foot May Be Appropriate O MRI foot without and with IV contrast May Be Appropriate O CT foot without IV contrast May Be Appropriate ☢ Bone scan foot May Be Appropriate ☢☢☢ CT foot with IV contrast Usually Not Appropriate ☢ CT foot without and with IV contrast Usually Not Appropriate ☢ ACR Appropriateness Criteria® 1 Chronic Foot Pain Variant 4: Chronic plantar heel pain. -

A Follow-Up of Patient Reported Outcomes in Chronic Plantar Heel Pain Participants Treated with Graston Technique: a Mixed Methods Approach
University of Northern Iowa UNI ScholarWorks Dissertations and Theses @ UNI Student Work 2016 A follow-up of patient reported outcomes in chronic plantar heel pain participants treated with Graston Technique: A mixed methods approach Troy Richard Garrett University of Northern Iowa Let us know how access to this document benefits ouy Copyright ©2016 Troy Richard Garrett Follow this and additional works at: https://scholarworks.uni.edu/etd Part of the Physical Therapy Commons, and the Physiotherapy Commons Recommended Citation Garrett, Troy Richard, "A follow-up of patient reported outcomes in chronic plantar heel pain participants treated with Graston Technique: A mixed methods approach" (2016). Dissertations and Theses @ UNI. 344. https://scholarworks.uni.edu/etd/344 This Open Access Dissertation is brought to you for free and open access by the Student Work at UNI ScholarWorks. It has been accepted for inclusion in Dissertations and Theses @ UNI by an authorized administrator of UNI ScholarWorks. For more information, please contact [email protected]. Copyright by TROY RICHARD GARRETT 2016 All Rights Reserved A FOLLOW-UP OF PATIENT REPORTED OUTCOMES IN CHRONIC PLANTAR HEEL PAIN PARTICIPANTS TREATED WITH GRASTON TECHNIQUE: A MIXED METHODS APPROACH An Abstract of a Dissertation Submitted in Partial Fulfillment of the Requirements for the Degree Doctor of Education Approved: ____________________________________ Dr. Peter J. Neibert, Committee Chair ____________________________________ Dr. Kavita R. Dhanwada Dean of the Graduate College Troy Richard Garrett University of Northern Iowa December 2016 ABSTRACT Chronic Plantar Heel Pain (CPHP), commonly known as “plantar fasciitis,” is a condition that is estimated to affect 10% of the American population. -

A Pilot Study of a Novel Treatment Method for Refractory Painful Plantar Fibromas
Open Access Austin Journal of Orthopedics & Rheumatology Research Article A Pilot Study of a Novel Treatment Method for Refractory Painful Plantar Fibromas Mihir M. Patel*, Sahvan M. Patel, Sia S. Patel and Jacob Daynes Abstract Department of Orthopedic Surgery, OrthoIndy, USA Introduction: Painful plantar fibromas may make ambulation difficult *Corresponding author: Mihir M Patel, Department for patients. They may recur and can make shoe wear difficult to purchase. of Orthopedic Surgery, OrthoIndy 8450 Northwest Blvd, Treatment modalities may include conservative care, modified shoe wear, Indianapolis, Indiana 46278, USA injections and orthotics. Surgical treatment may include open excision. The TX1A probe by Tenex Inc may be a useful alternative treatment modality for Received: March 18, 2015; Accepted: April 22, 2015; these painful lesions. Published: April 22, 2015 Materials and Methods: From 2011 through 2014, eight patients who had painful plantar fibromas elected to undergo definitive treatment for the fibromas. They all had had conservative care including modifications of shoes and either over the counter orthotics or custom orthotics. They all had advanced imaging tests (MRI or CT) preoperatively to help delineate the lesions. The definitive treatment utilized arthroscopy and the TX1A probe and was performed on an outpatient basis. Results: Preoperative AOFAS score was 30.8 (20-36). Postoperative AOFAS score was 90.1 (85-92). Average time of resolution of symptoms was 63.5 days (30-112) and average follow-up was 2.5 years. One patient had another lesion become painful but it was in a different location than the index operation. No others have had a recurrence to date. -

These Feet Won't Walk! What's Next?
2/1/2018 THESE FEET WON’T KARRIE LYNN CROSBY, WALK! WHAT’S NEXT? MPAS, PA-C OBJECTIVE DISCUSS DIAGNOSIS AND TREATMENT OF COMMON FOOT AND ANKLE PROBLEMS PLANTAR FASCIITIS 1 2/1/2018 PLANTAR FASCIITIS DIAGNOSIS/HISTORY: .FIRST STEP OR AM PAIN .RECENT SHOE GEAR CHANGE .STAND FOR LONG PERIODS OF TIME .WHAT TYPE OF FLOORING DO THEY HAVE OR STAND ON? .BAREFOOT .PLANTAR FASCIA PAIN ON PALPATION, TIGHT GASTROCS .NO OTHER DIAGNOSIS SUPPORTED ON XRAYS PLANTAR FASCIITIS TREATMENT: . AVOID GOING BAREFOOT . SHOE GEAR CHANGE . DON’T WEAR SAME PAIR OF SHOES MORE THEN 1 DAY . DON’T WEAR SHOES FOR MORE THEN 500 MILES . WONDERZORB HEEL PADS (CUSTOM ACCOMMODATIVE ORTHOTICS) . ICING . MASSAGE PLANTAR FASCIA BEFORE GETTING OUT OF BED PLANTAR FASCIITIS TREATMENT CONTINUED… .GASTROC/SOLEUS STRETCHING .TOPICAL NSAIDS .ORAL NSAIDS .STEROID DOSEPACK .BOOT (NIGHT SPLINTS) .SURGERY- GASTROC SLIDE, TOPAZ PROCEDURE 2 2/1/2018 PLANTAR FASCIITIS HAGLUND’S DEFORMITY ACHILLES TENDONITIS DIAGNOSIS/HISTORY: . OVERUSE . CONCENTRIC EXERCISES LIKE TOE RAISES OR SIMILAR . SHOES THAT HAVE A SEAM OR SHARP HEEL COUNTER . TIGHT GASTROCS . BODY MECHANICS . XRAYS- CALCIFICATIONS IN ACHILLES OR HAGLUND’S DEFORMITY . IF TEAR IS SUSPECT ORDER MRI . THOMPSON TESTING 3 2/1/2018 ACHILLES TENDONITIS TREATMENT: .BOOT OR SHOE WITH HEEL LIFT, REST .ICING .PHYSICAL THERAPY (GASTROC/SOLEUS STRETCH) ECCENTRIC STRETCHING .ULTRASOUND .SHOE GEAR MODIFICATION .NEVER INJECT WITH STEROIDS- RISK OF ACHILLES RUPTURE GASTROCNEMIUS ACHILLES TENDONITIS TREATMENT CONTINUED… .ORAL &/0R TOPICAL NSAIDS, ORAL STEROIDS .WARN ABOUT RECURRANCE OF PAIN AND RESTARTING BEHAVIOR MODIFICATIONS EARLY .SURGERY- GASTROC SLIDE, TOPAZ PROCEDURE, ACHILLES TENDON REPAIR 4 2/1/2018 MORTON’S FOOT TYPE METATARSALGIA DIAGNOSIS/HISTORY: .PLANTAR METATARSAL PAIN .OVERUSE, ACTIVITIES THAT PUT AREA UNDER STRESS .POOR SHOE GEAR OR POOR FIT .NO SIGN OF FRACTURE ON PLAIN FILMS .PREVIOUS STEROID INJECTION AROUND THE REGION IF THE SHOE FITS, WEAR IT 5 2/1/2018 METATARSALGIA TREATMENT: . -

Orthosports Orthopaedic Update 2012
2012 LATEST ORTHOPAEDIC UPDATES 47-49 Burwood Rd Lvl 3, 29-31 Dora Street Lvl 3, 1a Barber Ave 160 Belmore Rd CONCORD NSW 2137 HURSTVILLE NSW 2220 KINGSWOOD NSW 2747 RANDWICK NSW 2031 Tel: 02 9744 2666 Tel: 02 9580 6066 Tel: 02 4721 1865 Tel: 02 9399 5333 Fax: 02 9744 3706 Fax: 02 9580 0890 Fax: 02 4721 2832 Fax: 02 9398 8673 www.orthosports.com.au Doctors Consulting here Dr Mel Cusi Dr David Dilley 47-49 Burwood Road Tel 02 9744 2666 Dr Todd Gothelf Concord CONCORD NSW 2137 Fax 02 9744 3706 Dr George Konidaris Dr John Negrine Dr Rodney Pattinson Dr Doron Sher Dr Kwan Yeoh Doctors Consulting here Dr Paul Annett Dr Mel Cusi Dr Jerome Goldberg Suite F-Level 3 Tel 02 9580 6066 Dr Todd Gothelf Hurstville Medica Centre Fax 02 9580 0890 Dr George Konidaris 29-31 Dora Street Dr Andreas Loefler HURSTVILLE NSW 2220 Dr John Negrine Dr Rodney Pattinson Dr Ivan Popoff Dr Allen Turnbull Dr Kwan Yeoh Level 3 Doctors Consulting here Tel 4721 1865 Penrith 1a Barber Avenue Dr Todd Gothelf Fax 4721 2832 KINGSWOOD NSW 2747 Dr Kwan Yeoh Doctors Consulting here Dr John Best Dr Mel Cusi Dr Jerome Goldberg 160 Belmore Road Tel 02 9399 5333 Dr Todd Gothelf Randwick RANDWICK NSW 2031 Fax 02 9398 8673 Dr Andreas Loefler Dr John Negrine Dr Rodney Pattinson Dr Ivan Popoff Dr Doron Sher Dr Kwan Yeoh www.orthosports.com.au Thank you for attending our Latest Orthopaedic Updates Lecture. All of the presentations and handouts are available for viewing on the Teaching Section of our website: www.orthosports.com.au We would love your feedback – Tell us what you liked about the day and what you think we could improve for next year. -

Common Forefoot Conditions Mr Nadeem Mushtaq
Common Forefoot Conditions What can I do in the Primary Care Setting & when to Refer? Mr Nadeem Mushtaq Department of Trauma & Orthopaedics Contact Mr Nadeem Mushtaq Consultant Trauma & Orthopaedic Surgeon Imperial College Healthcare, London Head of Foot & Ankle and Trauma . St Mary’s Hospital, Paddington . The Lindo Wing – St. Mary’s Paddington . The Hospital of St. John & St. Elizabeth . The Bupa Cromwell NHS Secretary Private Secretary tel: 02078673747 [email protected] email: [email protected] Aims Todays topics Understanding the Foot Hallux valgus Hallux rigidus Morton’s Neuroma Plantar Fasciitis Friedberg’s Disease Lesser Toe Disorders Introduction . 26 Bones (+ sesamoids & accessory) . Joints . Muscles . Tendons . Function . Weight - standing / walking / running Hallux valgus ( not bunion) • Hallux valgus • is lateral deviation of the big toe at 1st MTPJ • BUT – is that all •? clinical • 9:1 female : male • 15:1 shoes : barefoot • 23% in aged 18-65 years (CI: 16.3 to 29.6) • 35.7% in aged over 65 years (CI: 29.5 to 42.0) • Prevalence increases with age and is higher in females Causes . genetic predisposition with an imbalance of intrinsic and extrinsic forces on the joint. Instability in the MTPJ or TMT joint combined with tight footwear results in the classical deformity which over time becomes fixed and painful. Medical conditions may also predispose to developing the condition (Table 1). Medical conditions predisposing Gout Rheumatoid arthritis Psoriatic arthropathy Joint hypermobility Ehlers-Danlos syndrome, Marfan's syndrome ligamentous laxity Down's syndrome Multiple sclerosis Charcot-Marie-Tooth disease Cerebral palsy Presentation: usually due to pain . pain over the bunion (bursa pain) .