ICD-10 Codes for Trigger Point Injections
Total Page:16
File Type:pdf, Size:1020Kb
Load more
Recommended publications
-

18-0969: R.S. and DEPARTMENT of the ARMY, WALTER
United States Department of Labor Employees’ Compensation Appeals Board __________________________________________ ) R.S., Appellant ) ) and ) Docket No. 18-0969 ) Issued: March 27, 2019 DEPARTMENT OF THE ARMY, WALTER ) REED NATIONAL MILITARY MEDICAL ) CENTER, Bethesda, MD, Employer ) _________________________________________ ) Appearances: Case Submitted on the Record Appellant, pro se Office of Solicitor, for the Director DECISION AND ORDER Before: CHRISTOPHER J. GODFREY, Chief Judge PATRICIA H. FITZGERALD, Deputy Chief Judge VALERIE D. EVANS-HARRELL, Alternate Judge JURISDICTION On April 10, 2018 appellant filed a timely appeal from a December 22, 2017 merit decision of the Office of Workers’ Compensation Programs (OWCP). Pursuant to the Federal Employees’ Compensation Act1 (FECA) and 20 C.F.R. §§ 501.2(c) and 501.3, the Board has jurisdiction over the merits of this case.2 ISSUE The issue is whether appellant has met her burden of proof to establish lumbar and/or right shoulder conditions causally related to an April 7, 2016 employment incident. 1 5 U.S.C. § 8101 et seq. 2 The Board notes that following the December 22, 2017 decision, OWCP received additional evidence. However, the Board’s Rules of Procedure provides: “The Board’s review of a case is limited to the evidence in the case record that was before OWCP at the time of its final decision. Evidence not before OWCP will not be considered by the Board for the first time on appeal.” 20 C.F.R. § 501.2(c)(1). Thus, the Board is precluded from reviewing this additional evidence for the first time on appeal. Id. FACTUAL HISTORY On April 15, 2016 appellant, then a 64-year-old radiology technology supervisor, filed a traumatic injury claim (Form CA-1) alleging that on April 7, 2016 she injured her lower back and right shoulder while in the performance of duty. -

Medical Policy Ultrasound Accelerated Fracture Healing Device
Medical Policy Ultrasound Accelerated Fracture Healing Device Table of Contents Policy: Commercial Coding Information Information Pertaining to All Policies Policy: Medicare Description References Authorization Information Policy History Policy Number: 497 BCBSA Reference Number: 1.01.05 Related Policies Electrical Stimulation of the Spine as an Adjunct to Spinal Fusion Procedures, #498 Electrical Bone Growth Stimulation of the Appendicular Skeleton, #499 Bone Morphogenetic Protein, #097 Policy Commercial Members: Managed Care (HMO and POS), PPO, and Indemnity Members Low-intensity ultrasound treatment may be MEDICALLY NECESSARY when used as an adjunct to conventional management (i.e., closed reduction and cast immobilization) for the treatment of fresh, closed fractures in skeletally mature individuals. Candidates for ultrasound treatment are those at high risk for delayed fracture healing or nonunion. These risk factors may include either locations of fractures or patient comorbidities and include the following: Patient comorbidities: Diabetes, Steroid therapy, Osteoporosis, History of alcoholism, History of smoking. Fracture locations: Jones fracture, Fracture of navicular bone in the wrist (also called the scaphoid), Fracture of metatarsal, Fractures associated with extensive soft tissue or vascular damage. Low-intensity ultrasound treatment may be MEDICALLY NECESSARY as a treatment of delayed union of bones, including delayed union** of previously surgically-treated fractures, and excluding the skull and vertebra. 1 Low-intensity ultrasound treatment may be MEDICALLY NECESSARY as a treatment of fracture nonunions of bones, including nonunion*** of previously surgically-treated fractures, and excluding the skull and vertebra. Other applications of low-intensity ultrasound treatment are INVESTIGATIONAL, including, but not limited to, treatment of congenital pseudarthroses, open fractures, fresh* surgically-treated closed fractures, stress fractures, arthrodesis or failed arthrodesis. -

Tuberculous Spondylitis, Pyogenic Spondylitis, X-Ray and Tomographic Features
American Journal of Medicine and Medical Sciences 2021, 11(5): 398-401 DOI: 10.5923/j.ajmms.20211105.08 X-Ray and Tomographic Manifestations of Tuberculous Spondylitis Babоev Abduvakhob Sakhibnazarovich Bone and Joint Tuberculosis Department of Rebuplican Specialized Scientific Practical Medical Center of Phtiziology and Pulmonology, Tashkent, Uzbekistan Abstract X-ray and tomographic data of seventy-eight patients with spine disorders (31 patients with tuberculous spondylitis, 23 patients with pyogenic spondylitis, and 24 patients with degenerative spondylopathy) after clinical, laboratory, bacteriologic, and histologic verification of diagnosis was comparatively analyzed. Current X-ray and tomographic features of tuberculous spondylitis are relatively equal thoracic and lumbosacral spine segments localization, with more than two adjacent vertebrae involvement in 22,6±7,5% of cases, the collapse of the vertebra(s) in 35.5 ± 8.6% of cases, unclear or osteoporotic border of bone tissue around TB focus in 64.5 ± 8.6%, formation of abscesses in 74.2±7.9% and their subligamentous spread to more than two vertebrae in 25,8±7,9% of cases, intact intervertebral disc in 16.1 ± 6.6% of cases, and specific process in the lungs in 48.4 ± 9.0% of cases. Keywords Tuberculous spondylitis, Pyogenic spondylitis, X-ray and tomographic features identify differential diagnostic features of tuberculous 1. Introduction spondylitis (TS). X-ray and tomographic (MRI and CT) methods of examination play a leading role in the diagnosis of 3. Materials and Methods tuberculous (TB) lesions of the spine [1,2,3]. Features of radiological changes of spine TB depend on The study was conducted at the bone and joint TB the activity and duration of the specific process [1,2]. -

6.3.3 Distal Radius and Wrist
6 Specific fractures 6.3 Forearm and hand 6.3.3 Distal radius and wrist 1 Assessment 657 1.1 Biomechanics 657 1.2 Pathomechanics and classification 657 1.3 Imaging 658 1.4 Associated lesions 659 1.5 Decision making 659 2 Surgical anatomy 660 2.1 Anatomy 660 2.2 Radiographic anatomy 660 2.3 Preoperative planning 661 2.4 Surgical approaches 662 2.4.1 Dorsal approach 2.4.2 Palmar approach 3 Management and surgical treatment 665 3.1 Type A—extraarticular fractures 665 3.2 Type B—partial articular fractures 667 3.3 Type C—complete articular fractures 668 3.4 Ulnar column lesions 672 3.4.1 Ulnar styloid fractures 3.4.2 Ulnar head, neck, and distal shaft fractures 3.5 Postoperative care 674 3.6 Complications 676 3.7 Results 676 4 Bibliography 677 5 Acknowledgment 677 656 PFxM2_Section_6_I.indb 656 9/19/11 2:45:49 PM Authors Daniel A Rikli, Doug A Campbell 6.3.3 Distal radius and wrist of this stable pivot. The TFCC allows independent flexion/ 1 Assessment extension, radial/ulnar deviation, and pronation/supination of the wrist. It therefore plays a crucial role in the stability of 1.1 Biomechanics the carpus and forearm. Significant forces are transmitted across the ulnar column, especially while making a tight fist. The three-column concept (Fig 6.3.3-1) [1] is a helpful bio- mechanical model for understanding the pathomechanics of 1.2 Pathomechanics and classification wrist fractures. The radial column includes the radial styloid and scaphoid fossa, the intermediate column consists of the Virtually all types of distal radial fractures, with the exception lunate fossa and sigmoid notch (distal radioulnar joint, DRUJ), of dorsal rim avulsion fractures, can be produced by hyper- and the ulnar column comprises the distal ulna (DRUJ) with extension forces [2]. -

Neurological Impairment in a Patient with Concurrent Cervical Disc Herniation and POEMS Syndrome
European Spine Journal (2019) 28 (Suppl 2):S51–S55 https://doi.org/10.1007/s00586-019-05914-5 CASE REPORT Neurological impairment in a patient with concurrent cervical disc herniation and POEMS syndrome Tingxian Ling1 · Limin Liu1 · Yueming Song1 · Shilian Zhou1 · Chunguang Zhou1 Received: 24 July 2018 / Revised: 16 December 2018 / Accepted: 9 February 2019 / Published online: 13 February 2019 © Springer-Verlag GmbH Germany, part of Springer Nature 2019 Abstract Purpose POEMS syndrome is a rare clonal plasma cell disease characterized by polyneuropathy, organomegaly, endocrinopa- thy, M protein, and skin changes. We report a rare case of neurological impairment in patients with concurrent cervical disc herniation and POEMS syndrome. Methods A patient presented to a local hospital with C3/4 and C4/5 disc herniation, apparent spinal cord compression con- comitant with neurological signs, and concurrent POEMS syndrome. Anterior cervical discectomy and fusion was performed. Results The limb numbness was only slightly alleviated, and 10 days postoperatively the patient complained of muscle weak- ness of the extremities and was referred to our hospital. The patients exhibited non-typical neurological signs and an enlarged liver and spleen that could not be explained. Electroneuromyography and immunofxation electrophoresis produced abnormal results. We diagnosed concurrent POEMS syndrome, for which drug therapy was prescribed. The patient’s symptoms receded. Conclusion Patients presenting with cervical spondylopathy and non-typical neurological signs and symptoms or other systemic problems should be evaluated for the presence of concurrent disease and ruled out diferential diagnoses. Keywords Neurological impairment · POMES syndrome · Cervical disc herniation · Cervical spondylosis Introduction a chronic demyelinating autoimmune disease that has symp- toms similar to those associated with myelopathy: spasticity, Cervical disc herniation is a common spinal disorder that sensory disturbances, gait ataxia, weakness. -
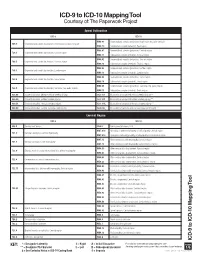

ICD-9 to ICD-10 Mapping Tool Courtesy Of: the Paperwork Project
ICD-9 to ICD-10 Mapping Tool Courtesy of: The Paperwork Project Spinal Subluxation ICD-9 ICD-10 M99.00 Segmental and somatic dysfunction, Head region (occipito-cervical) 739.0 Segmental and somatic dysfunction, Head region (occipito-cervical) M99.10 Subluxation complex (vertebral), Head region M99.01 Segmental and somatic dysfunction, Cervical region 739.1 Segmental and somatic dysfunction, Cervical region M99.11 Subluxation complex (vertebral), Cervical region M99.02 Segmental and somatic dysfunction, Thoracic region 739.2 Segmental and somatic dysfunction, Thoracic region M99.12 Subluxation complex (vertebral), Thoracic region M99.03 Segmental and somatic dysfunction, Lumbar region 739.3 Segmental and somatic dysfunction, Lumbar region M99.13 Subluxation complex (vertebral), Lumbar region M99.04 Segmental and somatic dysfunction, Sacral region 739.4 Segmental and somatic dysfunction, Sacral region M99.14 Subluxation complex (vertebral), Sacral region M99.05 Segmental and somatic dysfunction, Sacroiliac, hip, pubic regions 739.5 Segmental and somatic dysfunction, Sacroiliac, hip, pubic regions M99.15 Subluxation complex (vertebral), Pelvic region 839.08 Closed dislocation, Multiple cervical vertebra (injury) S13.101_ Dislocation of unspecified cervical vertebra (injury) ** 839.20 Closed dislocation, Lumbar vertebra (injury) S33.101_ Dislocation of unspecified lumbar vertebra (injury) ** 839.21 Closed dislocation, Thoracic vertebra (injury) S23.101_ Dislocation of unspecified thoracic vertebra (injury) ** 839.42 Closed dislocation, Sacrum, -

IN the UNITED STATES COURT of FEDERAL CLAIMS OFFICE of SPECIAL MASTERS No
IN THE UNITED STATES COURT OF FEDERAL CLAIMS OFFICE OF SPECIAL MASTERS No. 10-565V Filed: June 11, 2014 For Publication * * * * * * * * * * * * * * * * * * * * * * * * * * * * MEGAN L. GODFREY, * HPV Vaccine; Gardasil; Juvenile * Ankylosing Spondylitis; JAS; Petitioner, * Causation-in-Fact; Expert; v. * Qualifications. * SECRETARY OF HEALTH * AND HUMAN SERVICES, * * Respondent. * * * * * * * * * * * * * * * * * * * * * * * * * * * * * Milton Clay Ragsdale, IV, Ragsdale LLC, Birmingham, AL, for petitioner. Jennifer Reynaud, U.S. Department of Justice, Washington, DC, for respondent. DECISION1 Vowell, Chief Special Master: On August 20, 2010, Megan Godfrey [“petitioner”] filed a petition for compensation under the National Vaccine Injury Compensation Program, 42 U.S.C. §300aa-10, et seq.2 [the “Vaccine Act” or “Program”]. The petition alleged that the human papillomavirus [“HPV”] and meningococcal conjugate vaccines Ms. Godfrey received on August 22, 2007, caused her to develop juvenile rheumatoid arthritis. Petition at 1-2. 1 Because this decision contains a reasoned explanation for my action in this case, it will be posted on the United States Court of Federal Claims’ website, in accordance with the E-Government Act of 2002, Pub. L. No. 107-347, 116 Stat. 2899, 2913 (Dec. 17, 2002). As provided by Vaccine Rule 18(b), each party has 14 days within which to request redaction “of any information furnished by that party: (1) that is a trade secret or commercial or financial in substance and is privileged or confidential; or (2) that includes medical files or similar files, the disclosure of which would constitute a clearly unwarranted invasion of privacy.” Vaccine Rule 18(b). Otherwise, the entire decision will be available to the public. 2 National Childhood Vaccine Injury Act of 1986, Pub. -

Treatment of Distal Radius Fractures – Clinical Outcome, Regional Variation and Health Economics
From THE DEPARTMENT OF CLINICAL SCIENCE AND EDUCATION, SÖDERSJUKHUSET Karolinska Institutet, Stockholm, Sweden TREATMENT OF DISTAL RADIUS FRACTURES – CLINICAL OUTCOME, REGIONAL VARIATION AND HEALTH ECONOMICS Jenny Saving Stockholm 2019 All previously published papers were reproduced with permission from the publisher. Published by Karolinska Institutet. Printed by Eprint AB 2019 © Jenny Saving, 2019 ISBN 978-91-7831-339-6 Treatment of distal radius fractures – clinical outcome, regional variation and health economics THESIS FOR DOCTORAL DEGREE (Ph.D.) By Jenny Saving, MD Principal Supervisor: Opponent: MD, Associate Professor Anders Enocson MD, Professor Lars Adolfsson Karolinska Institutet University of Linköping Department of Clinical Science and Education Department of Clinical and Experimental Division of Orthopaedics Medicine Södersjukhuset Examination Board: Co-supervisor(s): MD, Professor Hans Mallmin MD, PhD, Cecilia Mellstrand Navarro Uppsala University Karolinska Institutet Department of Surgical Sciences Department of Clinical Science and Education Section of Orthopaedics Division of Hand Surgery Södersjukhuset MD, Associate Professor Rüdiger Weiss Karolinska Institutet MD, Professor Sari Ponzer Department of Molecular Medicine and Surgery Karolinska Instiutet Karolinska University Hospital Department of Clinical Science and Education Division of Orthopaedics MD, Professor Olof Nilsson Södersjukhuset Uppsala University Department of Surgical Sciences Section of Orthopaedics To my family 3 4 ABSTRACT A distal radius fracture (DRF) remains the most common fracture encountered in health care. DRFs have traditionally been treated with a plaster or surgically with percutaneous methods. Since the end of the 20th century, when internal fixation with a volar locking plate (VLP) was introduced, the incidence of DRF surgery in general and of plating in particular have increased markedly. -
Orthopaedics Instructions: to Best Navigate the List, First Download This PDF File to Your Computer
Orthopaedics Instructions: To best navigate the list, first download this PDF file to your computer. Then navigate the document using the bookmarks feature in the left column. The bookmarks expand and collapse. Finally, ensure that you look at the top of each category and work down to review notes or specific instructions. Bookmarks: Bookmarks: notes or specific with expandable instructions and collapsible topics As you start using the codes, it is recommended that you also check in Index and Tabular lists to ensure there is not a code with more specificity or a different code that may be more appropriate for your patient. Copyright APTA 2016, ALL RIGHTS RESERVED. Last Updated: 09/14/16 Contact: [email protected] Orthopaedics Disorder by site: Ankle Achilles tendinopathy ** Achilles tendinopathy is not listed in ICD10 M76.6 Achilles tendinitis Achilles bursitis M76.61 Achilles tendinitis, right leg M76.62 Achilles tendinitis, left leg ** Tendinosis is not listed in ICD10 M76.89 Other specified enthesopathies of lower limb, excluding foot M76.891 Other specified enthesopathies of right lower limb, excluding foot M76.892 Other specified enthesopathies of left lower limb, excluding foot Posterior tibialis dysfunction **Posterior Tibial Tendon Dysfunction (PTTD) is not listed in ICD10 M76.82 Posterior tibial tendinitis M76.821 Posterior tibial tendinitis, right leg M76.822 Posterior tibial tendinitis, left leg M76.89 Other specified enthesopathies of lower limb, excluding foot M76.891 Other specified enthesopathies of right lower limb, -

Metacarpal Fractures
METACARPAL FRACTURES BY LORYN P. WEINSTEIN, MD, AND DOUGLAS P. HANEL, MD The majority of metacarpal fractures are closed injuries amenable to conservative treatment with external immobilization and subsequent rehabilitation. Internal fixation is favored for unstable fracture patterns and patients who require early motion. Percutaneous pinning usually is successful for metacarpal neck fractures and comminuted head fractures. Shaft and base fractures can be treated with pinning or open reduction and internal fixation; the latter, being more rigid, allows early rehabilitation. External fixation has a limited yet defined role for metacarpal fractures with complex soft-tissue injury and/or segmental bone loss. The recent development of bioabsorbable implants holds promise for skeletal rigidity with minimal soft-tissue morbidity, but long-term in vivo data support- ing the use of these implants is not currently available. Copyright © 2002 by the American Society for Surgery of the Hand arly treatment of metacarpal fractures was lim- Surgical techniques rapidly expanded to include ret- ited to the only tools available: manipulation rograde fracture pinning, intramedullary pinning, and Eand casting. The discovery of percutaneous transfixion pinning. Many of the K-wires in use today fracture fixation near the turn of the century opened have the same diamond-shaped tip and sizing speci- up a new world of possibilities. It was 25 years after fications as the original design. Bennett’s original manuscript that Lambotte de- The first plate and screw set for the hand was scribed the first surgical stabilization of a basilar introduced in the late 1930s. By today’s standards, the thumb fracture by using a thin carpenter’s nail.1 By Hermann Metacarpal Bone Set was quite lean; it 1913, Lambotte had authored a fracture text with included 3 longitudinal plates of 2, 3, and 4 holes, a multiple examples of pinning, wiring, and plating of drill, screwdriver, and 9 screws.1 Improvements in hand fractures. -

A Study on Management of Comminuted Colles Fracture by Closed Reduction and Ulnocarpal Stabilisation with 2 K-Wires
IOSR Journal of Dental and Medical Sciences (IOSR-JDMS) e-ISSN: 2279-0853, p-ISSN: 2279-0861.Volume 14, Issue 4 Ver. IV (Apr. 2015), PP 45-51 www.iosrjournals.org A Study on Management of Comminuted Colles Fracture by Closed Reduction and Ulnocarpal Stabilisation with 2 K-Wires Dr. Addepalli Srinivasa Rao, M.S, M.ch (Ortho), Dr. K.N.Sandeep M.S(Ortho) Department of Orthopaedics, Siddhartha Medical College, Vijayawada, Andhrapradesh ,India 520008 Abstract Background – In comminuted Colles fractures treated by conventional method , malunion during healing due to progressive radial collapse is a common complication. Many modalities of treatment have been described with their merits and demerits. Ulnocarpal stabilization is an effective method to prevent radial collapse and hence this study. Materials And Methods – A prospective study of 100 patients of comminuted Colles fracture between 20-70 years age irrespective of sex treated by closed reduction and percutaneous stabilization of ulnocarpal articulation and above elbow POP cast for 6weeks has been presented. Patients were evaluated at 1 year follow up and functionally by Sarmiento’s modification of Lindstrom criteria and Gartland and Werley’s criteria. Results – Excellent to good results in 92%,fair in 4% and poor in 4% of total cases. Complications observed were malunion (n=6), pin tract infection (n=7), pullout of k-wire (n=5), sudeck’s osteodystrophy (n=7), residual pain (n=4),reduced grip strength (n=8) . Conclusion – Percutaneous pinnng by ulnocarpal stabilization is minimally invasive, yet an effective method to maintain the reduction and stability of distal radioulnar joint and radial collapse during healing ,even when the fracture is grossly comminuted ,intraarticular or unstable . -

Doctoral Thesis Effectiveness of Tumor Necrosis Factor Inhibitors in Patients
Bente Glintborg 2018 Glintborg Bente UNIVERSITY OF COPENHAGEN FACULTY OF HEALTH AND MEDICAL SCIENCES Effectiveness of Effectiveness Doctoral thesis Doctoral thesis Bente Glintborg, 2018 Bente Glintborg, 2018 tumor Effectiveness of tumor necrosis factor inhibitors in patients necrosis factor inhibitors in patients with psoriatic arthritis and arthritiswithaxial psoriatic inhibitorsin patients factor necrosis with psoriatic arthritis and axial spondyloarthritis – treatment response, drug retention and predictors thereof Results from the nationwide DANBIO registry Copenhagen Center for Arthritis Research (COPECARE) Center for Rheumatology and Spine Diseases Centre of Head and Orthopaedics Rigshospitalet, Glostrup spondyloarthritis ISBN 978-87-970989-0-5 Doctoral thesis Effectiveness of tumor necrosis factor inhibitors in patients with psoriatic arthritis and axial spondyloarthritis – treatment response, drug retention and predictors thereof Results from the nationwide DANBIO registry Bente Glintborg, MD, PhD 2018 The DANBIO registry and Copenhagen Center for Arthritis Research, COPECARE Center for Rheumatology and Spine Diseases Centre of Head and Orthopedics Rigshospitalet 1 © Bente Glintborg 2018 ISBN 978-87-970989-0-5 All rights reserved. No parts of this publication may be reproduced or transmitted, in any form or by any means, without permission The Faculty of Health and Medical Sciences at the University of Copenhagen has accepted this dissertation, which consists of the already published dissertations listed below, for public defence