CHAPTER 21 Adult Interdisciplinary Therapy: Diagnosis and Treatment 575
Total Page:16
File Type:pdf, Size:1020Kb
Load more
Recommended publications
-

Ankylosed Primary Molars, Andlaw (1974) Described Surface Defects from Bicuspids Preceded by Non-Ankylosed 11 Molars
PEDIATRICDENTISTRY/Copyright (~) 1980 The AmericanAcademy of Pedodontics/Vol. 2, No, 1 Ankylosedprimary mola.rs: Results and treatment recommendat,onsfrom an eight-year longitudinal study Louise Brearley Messer,B.D.Sc., L.D.S., M.D.Sc. Jay T. Cline, D.D.S., M.A. Abstract continues concomitantly with vertical alveolar bone growth,~,3 and the tooth is immobile to manual rock- A total of 263 ankyloscd primarymolars in 107 ing.4,5 children aged three to 12 years was studied for four years. Forty-six children remainedin the study for eight years. The etiology of the condition remains unknown. Extrinsic causative factors implicated are local me- Observationof affected dentitions showedthat the con- ~ ~ dition waslikely to recur. Threeclinical pa~ternsfor the chanical trauma, disturbed local metabolism, local- condition are described. Typically, maxillary molars be- ized infection, 6 chemical or thermal irritation 7 and came ankylosed earlier and demonstrated more severe tooth reimplantation, s Intrinsic factors cited include a in[raocclusion than mandibularmolars. Mandibularfirst genetic or congenital gap in the periodontal liga- molars usually remainedslightly or moderatelyin#a- ment. Since both erupting and exfoliating teeth show occluded; mandibularsecond molars and maxillary first alternating periods of resorption and deposition of and second molars showedprogressively severe infra- bone and cementum,° aberrant deposition of these tis- occlusion. Followingeither extraction or ex~oliation of the suesI° may produce an area of ankylosing tissue.Z, affected molars, the succedaneousbicuspids did not differ In a summaryof studies reporting the prevalence of in either coronal morphologyor in distribution of enamel ankylosed primary molars, Andlaw (1974) described surface defects from bicuspids preceded by non-ankylosed 11 molars. -

Pharmacology of Local Anesthesia
By Mohammad Hussein Zaki Lecturer Oral & Maxillofacial Surgery Faculty of Dentistry – Minia University . Impacted tooth. Failure of the tooth to fully erupt into the oral cavity within its expected developmental time period and can no longer reasonably be expected to do so. A tooth that can not, or will not, erupt into its normal functioning positions. Impacted tooth. An impacted tooth is one that is erupted, partially erupted or unerupted and will not eventually assume a normal arch relationship with the other teeth and tissues. Unerupted tooth. Includes impacted teeth and teeth that are in the process of erupting. Impacted teeth seen in the following order of frequency: 1. Mandibular third molars. 2. Maxillary third molars. 3. Maxillary canine. 4. Mandibular premolar. 5. Maxillary premolar. 6. Mandibular canine. 7. Maxillary central incisors. 8. Maxillary lateral incisors. Systemic factors: • Syndromes. Cleidocranial dysplasia. • Endocrine deficiencies. Hypothyroidism. • Irradiation. Local factors: • Obstruction for eruption. Irregularity in position of an adjacent tooth. Density of the overlying soft tissue or bone. Prolonged deciduous tooth retention. Supernumerary teeth. • Tooth ankylosis. • Dilaceration of roots. • Malposed tooth germs. Local factors: • Pathological lesions. • Cleft lip and palate. • Arch-length deficiency. Phylogenic theory. Mendelian theory. Clinical. Radiographic. • Periapical. Radiographic. • Periapical. Radiographic. • Occlusal. Radiographic. • Panorama. Radiographic. • Panorama. Radiographic. • CT. Radiographic. • CBCT. Impacted teeth other than third molars. Exposure. • A procedure that allows natural eruption of impacted teeth. • It should be done as soon as it is determined that the tooth is not going to erupt spontaneously. • Spontaneous eruption versus orthodontic assistance. Impacted teeth other than third molars. Exposure. Impacted teeth other than third molars. -

Eruption Abnormalities in Permanent Molars: Differential Diagnosis and Radiographic Exploration
DOI: 10.1051/odfen/2014054 J Dentofacial Anom Orthod 2015;18:403 © The authors Eruption abnormalities in permanent molars: differential diagnosis and radiographic exploration J. Cohen-Lévy1, N. Cohen2 1 Dental surgeon, DFO specialist 2 Dental surgeon ABSTRACT Abnormalities of permanent molar eruption are relatively rare, and particularly difficult to deal with,. Diagnosis is founded mainly on radiographs, the systematic analysis of which is detailed here. Necessary terms such as non-eruption, impaction, embedding, primary failure of eruption and ankylosis are defined and situated in their clinical context, illustrated by typical cases. KEY WORDS Molars, impaction, primary failure of eruption (PFE), dilaceration, ankylosis INTRODUCTION Dental eruption is a complex developmen- at 0.08% for second maxillary molars and tal process during which the dental germ 0.01% for first mandibular molars. More re- moves in a coordinated fashion through cently, considerably higher prevalence rates time and space as it continues the edifica- were reported in retrospective studies based tion of the root; its 3-dimensional pathway on orthodontic consultation records: 2.3% crosses the alveolar bone up to the oral for second molar eruption abnormalities as epithelium to reach its final position in the a whole, comprising 1.5% ectopic eruption, occlusion plane. This local process is regu- 0.2% impaction and 0.6% primary failure of lated by genes expressing in the dental fol- eruption (PFE) (Bondemark and Tsiopa4), and licle, at critical periods following a precise up to 1.36% permanent second molar iim- chronology, bilaterally coordinated with fa- paction according to Cassetta et al.6. cial growth. -

Oral Pathology and Oral Microbiology
3.3.2 SYLLABUS ( Including Teaching Hours.) MUST KNOW 109 HRS 1 Developmental Disturbances of oral and paraoral structures 03 HRS Developmental disturbances of hard tissues: -dental arch relations, -disturbances related to - -size,shape,number and structure of teeth, -disturbances related to eruption and shedding. Developmental disturbances of soft tissues: Lip,palate,oral mucosa,gingival,tongue and salivary glands Craniofacial anomalies 2 Benign and Malignant tumors of oral cavity 25 HRS Potentially Malignant Disorders of epithelial tissue origin. -Definitions and nomenclature -Epithelial dysplasia -Lesions and conditions:leukoplakia, erythroplakia,oral lichen planus and oral submucous fibrosis. Benign tumors of epithelial tissue origin. - Squamous papilloma, Oral nevi. Malignant tumors of epithelial tissue origin. -Oral squamous cell carcinoma: Definition and nomenclature,etiopathogenesis, TNM staging ,Broder’s and Bryne’s grading systems. -Verrucous carcinoma -Basal cell carcinoma: Definition etiopathogenesis and histopathology -Malignant melanoma: Definition etiopathogenesis and histopathology Benign and malignant tumors of connective tissue -Fibroblast origin:oral fibromas and fibromatosis,peripheral ossifying fibroma peripheral giant cell granuloma, pyogenic granuloma and Fibrosarcoma -Adipose tissue origin:Lipoma -Endothelial origin(blood and lymphatics: Hemangiomas and lymphangiomas, Hereditary hemorrhagic telangiactasia, Kaposi’s sarcoma Bone and cartilage: Chondroma,osteoma,osteoid osteoma, benign osteoblastoma, osteosarcoma, -

Iatrogenic Mandibular Fractures Following Removal of Impacted Third
Iatrogenic mandibular IN BRIEF • Serves as a reminder of a rare but significant complication. PRACTICE fractures following removal • Highlights timing and presentation of the event. • Summarises potential risk factors and measures to minimise them. of impacted third molars: • Describes the treatment options. • Illustrates the role of the dentist in an analysis of 130 cases the management. M. Ethunandan,1 D. Shanahan2 and M. Patel3 VERIFIABLE CPD PAPER Immediate and late mandibular fractures are a rare complication of third molar removal. We analysed 130 cases of mandibular fractures following removal of impacted third molars reported in the literature, including four managed in the maxillofacial unit and identified potential risk factors. Its occurrence is likely to be multi-factorial, with age, gender, angulation, laterality, extent and degree of impaction and associated pathologies contributing to the risk of fracture. Postoperative fractures were more common than intra-operative fractures (2.7:1) and occurred most frequently in the second and third weeks (57%). A ‘cracking’ noise was the most frequent presentation (77%). Intra-operative fractures were more frequent among females (M:F – 1:1.3), and differed from postoperative fractures (M:F – 3.9:1). This study analyses the results, providing suggestions to minimise the risk and to manage a mandibular fracture following removal of a third molar. INTRODUCTION seek to identify potential risk factors and Removal of third molars is a common preventive measures. surgical procedure carried out by a den- tal surgeon and can result in a variety MATERIALS AND METHODS complications, which include dry socket, We undertook a Medline search cover- bleeding, infection, trismus and nerve ing the period 1970–2011 and identified damage.1–3 Mandibular fracture is rare, English articles in the literature, which but a very serious complication following reported the occurrence of mandibu- Fig. -

An Investigation Into the Role of Rankl and Sclerostin in Dentoalveolar Ankylosis
AN INVESTIGATION INTO THE ROLE OF RANKL AND SCLEROSTIN IN DENTOALVEOLAR ANKYLOSIS A thesis submitted in partial fulfilment of the requirements for the degree of Doctor of Clinical Dentistry (Orthodontics) Dr Shelley Coburn, BDS (University of Otago) Orthodontic Unit School of Dentistry Faculty of Health Science The University of Adelaide South Australia AUSTRALIA June 2015 1 CONTENTS 1.1 Table of Contents 1 CONTENTS .............................................................................................................. 2 1.1 Table of Contents ............................................................................................... 2 1.2 List of Figures .................................................................................................... 5 1.3 List of Tables ...................................................................................................... 6 1.4 List of abbreviations ........................................................................................... 8 2 ACKNOWLEDGEMENTS ....................................................................................... 10 3 THESIS DECLARATION ........................................................................................ 11 4 ABSTRACT ............................................................................................................ 12 5 LITERATURE REVIEW .......................................................................................... 15 5.1 The Periodontal Complex ................................................................................ -

Statistical Analysis Plan
Cover Page for Statistical Analysis Plan Sponsor name: Novo Nordisk A/S NCT number NCT03061214 Sponsor trial ID: NN9535-4114 Official title of study: SUSTAINTM CHINA - Efficacy and safety of semaglutide once-weekly versus sitagliptin once-daily as add-on to metformin in subjects with type 2 diabetes Document date: 22 August 2019 Semaglutide s.c (Ozempic®) Date: 22 August 2019 Novo Nordisk Trial ID: NN9535-4114 Version: 1.0 CONFIDENTIAL Clinical Trial Report Status: Final Appendix 16.1.9 16.1.9 Documentation of statistical methods List of contents Statistical analysis plan...................................................................................................................... /LQN Statistical documentation................................................................................................................... /LQN Redacted VWDWLVWLFDODQDO\VLVSODQ Includes redaction of personal identifiable information only. Statistical Analysis Plan Date: 28 May 2019 Novo Nordisk Trial ID: NN9535-4114 Version: 1.0 CONFIDENTIAL UTN:U1111-1149-0432 Status: Final EudraCT No.:NA Page: 1 of 30 Statistical Analysis Plan Trial ID: NN9535-4114 Efficacy and safety of semaglutide once-weekly versus sitagliptin once-daily as add-on to metformin in subjects with type 2 diabetes Author Biostatistics Semaglutide s.c. This confidential document is the property of Novo Nordisk. No unpublished information contained herein may be disclosed without prior written approval from Novo Nordisk. Access to this document must be restricted to relevant parties.This -

Eruption of Teeth Assistant Professor Aseel Haidar
Lec. 3 Eruption of teeth Assistant Professor Aseel Haidar Lec.3 Pedodontics Forth stage Assistant Professor Aseel Haidar Early Eruption (NATAL AND NEONATAL TEETH) Natal teeth are (teeth present at birth) and neonatal teeth (teeth that erupt during the first 30 days) prevalence is low. About 85% of natal or neonatal teeth are mandibular primary incisors, and only small percentages are supernumerary teeth. It is common for natal and neonatal teeth to occur in pairs. Natal and neonatal molars are rare. Most studies suggest that the etiology for the premature eruption or the appearance of natal and neonatal teeth is multifactorial. A possible factor involving the early eruption of primary teeth seems to be familial, due to inheritance as an autosomal-dominant trait. A radiograph should be made to determine the amount of root development and the relationship of a prematurely erupted tooth to its adjacent teeth. One of the parents can hold the x-ray film in the infant’s mouth during the exposure. Most prematurely erupted teeth (immature type) are hypermobile because of limited root development. 1. If the tooth is extremely mobile to the extent that there is danger of displacement of the tooth and possible aspiration, so the treatment indicated in such a case is the removal of the tooth. 2. If the tooth has sharp incisal edge that may cause laceration of the lingual surface of the tongue, so treatment is the removal of the tooth. The preferable approach, however, is to leave the tooth in place and to explain to the parents the desirability of maintaining this tooth in the mouth because of its importance in the growth and uncomplicated eruption of the adjacent teeth. -
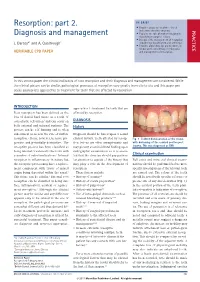
Resorption: Part 2. Diagnosis and Management
Resorption: part 2. IN BRIEF Provides an overview of the clinical indicators of root resorption. PRACTICE Diagnosis and management Explains the role of modern imaging in classifying resorptive lesions. Discusses the management of resorption J. Darcey*1 and A. Qualtrough2 considering classifcation and aetiology. Provides algorithms for practitioners to follow when considering the diagnosis VERIFIABLE CPD PAPER and management of resorption. In this second paper the clinical indicators of root resorption and their diagnosis and management are considered. While the clinical picture can be similar, pathological processes of resorption vary greatly from site to site and this paper pro- poses appropriate approaches to treatment for teeth that are affected by resorption. INTRODUCTION approaches to treatment for teeth that are Root resorption has been defned as the affected by resorption. loss of dental hard tissue as a result of osteoclastic cell action1 and can occur on DIAGNOSIS both external and internal surfaces. The History process can be self limiting and is often sub-clinical as seen in the case of surface Diagnosis should be based upon a sound resorption.2 It can, however, be more pro- clinical history. Teeth affected by resorp- Fig. 1 Evident discolouration of the crown gressive and potentially destructive.2 The tion lesions are often asymptomatic and with darkening of the cervical portion post resorptive process has been classifed as may present as an incidental fnding upon trauma. This was diagnosed as ERR being internal or external to the tooth with radiographic examination so it is essen- Clinical examination a number of sub-classifcations.3 Internal tial that the clinician should pay particu- resorption is infammatory in nature but lar attention to aspects of the history that Full extra and intra oral clinical exami- the resorptive process may have a replace- may play a role in the development of nations should be performed before more ment component with tissue of mixed resorption. -

Ankylosis of Permanent First Molar: Diagnosis by Cone Beam
Int. J. Odontostomat., 11(3):319-325, 2017. Ankylosis of Permanent First Molar: Diagnosis by Cone Beam Computed Tomography Anquilosis del Primer Molar Permanente: Diagnóstico por Tomografía Computarizada con Haz Cónico Eliana Dantas da Costa1; Priscila Dias Peyneau1; Francielle Silvestre Verner2; Rafael Binato Junqueira3; Solange Maria de Almeida1 & Glaucia Maria Bovi Ambrosano4 DA COSTA, E. D.; PEYNEAU, P. D.; VERNER, F. S.; JUNQUEIRA, R. B.; DE ALMEIDA, S. M. & AMBROSANO, G. M. B. Ankylosis of permanent first molar: Diagnosis by cone beam computed tomography. Int. J. Odontostomat., 11(3):319-325, 2017. ABSTRACT: Ankylosis is an anomaly of tooth eruption characterized by the fusion of cementum and alveolar bone, and may affect from small regions to the entire root surface. Clinical assessment combined with imaging exams can aid diagnosis. Radiographic testing enables assessing only proximal regions of possibly affected roots. Whereas cone beam computed tomography (CBCT) allows a three-dimensional assessment of axial, coronal, and sagittal planes of all dental extension, eliminating thus overlapping images and helping to confirm the correct diagnosis. The present study contains a case report of a male patient with ankylosis in tooth 16 diagnosed by CBCT, aiming at providing information for dentists about this anomaly, its characteristics and situations in which CBCT should be indicated. KEY WORDS: dental ankylosis, diagnosis, cone beam computed tomography. INTRODUCTION Dentoalveolar ankylosis is an anomaly of den- mandibular deciduous first molars (Loriato et al.; Alves tal eruption, caused by mechanical failure of eruption et al.; Bertl et al.; Parisay et al., 2013), followed by (Frazier-Bowers et al., 2007), characterized by the second mandibular and maxillary deciduous molars fusion of cementum and alveolar bone (Loriato et al., (Parisay et al.). -

Balkan Journal of Stomatology
BALKAN JOURNAL OF STOMATOLOGY Official publication of the BALKAN STOMATOLOGICAL SOCIETY Volume 12 No 3 November 2008 ISSN 1107 - 1141 BALKAN JOURNAL OF STOMATOLOGY Official publication of the BALKAN STOMATOLOGICAL SOCIETY Volume 12 No 3 November 2008 ISSN 1107 - 1141 Y T E I C O S L BALKAN JOURNAL OF STOMATOLOGY A ISSN 1107 - 1141 IC G LO TO STOMA Editor-in-Chief Ljubomir TODOROVIĆ, DDS, MSc, PhD Faculty of Stomatology, University of Belgrade Clinic of Oral Surgery PO Box 506 Dr Subotića 4, 11000 Belgrade Serbia Editorial board ALBANIA ROMANIA Ruzhdie QAFMOLLA - Editor Address: Andrei ILIESCU - Editor Address: Emil KUVARATI Dental University Clinic Victor NAMIGEAN Faculty of Stomatology Besnik GAVAZI Tirana, Albania Cinel MALITA Calea Plevnei 19, sect. 1 70754 Bucuresti BOSNIA AND HERZEGOVINA Address: Romania Maida GANIBEGOVIĆ Faculty of Dentistry SERBIA Naida HADŽIABDIĆ Bolnička 4a Dragan STAMENKOVIĆ - Editor Address: Mihael STANOJEVIĆ 71000 Sarajevo Zoran STAJČIĆ Faculty of Stomatology BIH Miloš TEODOSIJEVIĆ Dr Subotića 8 BULGARIA 11000 Beograd Nikolai POPOV - Editor Address: Serbia Nikola ATANASSOV Faculty of Stomatology TURKEY Nikolai SHARKOV G. Sofiiski str. 1 1431 Sofia, Bulgaria Ender KAZAZOGLU - Editor Address: Pinar KURSOGLU Yeditepe University FYROM Julijana GJORGOVA - Editor Address: Arzu CIVELEK Faculty of Dentistry Ana STAVREVSKA Faculty of Stomatology Bagdat Cad. No 238 Ljuben GUGUČEVSKI Vodnjanska 17, Skopje Göztepe 81006, Istanbul Republika Makedonija Turkey GREECE CYPRUS Anastasios MARKOPOULOS - Editor Address: George PANTELAS - Editor Address: Haralambos PETRIDIS Aristotle University Huseyn BIÇAK Gen. Hospital Nicosia Grigoris VENETIS Dental School Aikaterine KOSTEA No 10 Pallados St. Nicosia, Cyprus Thessaloniki, Greece Y T E I C O S BALKAN STOMATOLOGICAL SOCIETY L A IC G LO TO STOMA Council President: Prof. -

1 Oral Health Outcomes As Potential Indicators Of
ORAL HEALTH OUTCOMES AS POTENTIAL INDICATORS OF CANCER EXPERIENCE by Mariana Bezamat Coutinho Lucas Doctor of Dental Surgery, Federal University of Rio de Janeiro, 2013 Submitted to the Graduate Faculty of the School of Dental Medicine in partial fulfillment of the requirements for the degree of Doctor of Philosophy University of Pittsburgh 2021 1 Committee Page UNIVERSITY OF PITTSBURGH SCHOOL OF DENTAL MEDICINE This dissertation was presented by Mariana Bezamat Coutinho Lucas It was defended on January 22, 2021 and approved by Dobrawa Napierala, PhD, Department of Oral Biology Juan Taboas, PhD, Department of Oral Biology Adriana Modesto, DDS, MS, PhD, Department of Pediatric Dentistry Thesis Advisor/Dissertation Director: Alexandre R. Vieira, DDS, MS, PhD, Department of Oral Biology ii Copyright © by Mariana Bezamat Coutinho Lucas 2021 iii ORAL HEALTH OUTCOMES AS POTENTIAL INDICATORS OF CANCER EXPERIENCE Mariana Bezamat Coutinho Lucas, DDS, PhD University of Pittsburgh, 2021 According to an estimate from the American Cancer Society in 2018, 1,735,350 people were expected to be diagnosed with cancer in the United States, with 609,640 dying from the disease. The late diagnosis of cancer has a negative impact on the health care system due to higher treatment cost and decreased chances of favorable prognosis. Due to the nature of their profession, dentists and their teams are well positioned to identify oral risk markers related to cancer, which increases the potential for early diagnosis and chances of survival. For example, tooth agenesis has been associated with increased risk for ovarian cancer. A greater awareness of oral conditions that are linked to genetic predictors of cancer susceptibility will provide dentists an opportunity to improve patient outcomes by suggesting genetic screenings for prevention.