Epigenetic Reprogramming Towards Mesenchymal-Epithelial Transition
Total Page:16
File Type:pdf, Size:1020Kb
Load more
Recommended publications
-

Entrez Symbols Name Termid Termdesc 117553 Uba3,Ube1c
Entrez Symbols Name TermID TermDesc 117553 Uba3,Ube1c ubiquitin-like modifier activating enzyme 3 GO:0016881 acid-amino acid ligase activity 299002 G2e3,RGD1310263 G2/M-phase specific E3 ubiquitin ligase GO:0016881 acid-amino acid ligase activity 303614 RGD1310067,Smurf2 SMAD specific E3 ubiquitin protein ligase 2 GO:0016881 acid-amino acid ligase activity 308669 Herc2 hect domain and RLD 2 GO:0016881 acid-amino acid ligase activity 309331 Uhrf2 ubiquitin-like with PHD and ring finger domains 2 GO:0016881 acid-amino acid ligase activity 316395 Hecw2 HECT, C2 and WW domain containing E3 ubiquitin protein ligase 2 GO:0016881 acid-amino acid ligase activity 361866 Hace1 HECT domain and ankyrin repeat containing, E3 ubiquitin protein ligase 1 GO:0016881 acid-amino acid ligase activity 117029 Ccr5,Ckr5,Cmkbr5 chemokine (C-C motif) receptor 5 GO:0003779 actin binding 117538 Waspip,Wip,Wipf1 WAS/WASL interacting protein family, member 1 GO:0003779 actin binding 117557 TM30nm,Tpm3,Tpm5 tropomyosin 3, gamma GO:0003779 actin binding 24779 MGC93554,Slc4a1 solute carrier family 4 (anion exchanger), member 1 GO:0003779 actin binding 24851 Alpha-tm,Tma2,Tmsa,Tpm1 tropomyosin 1, alpha GO:0003779 actin binding 25132 Myo5b,Myr6 myosin Vb GO:0003779 actin binding 25152 Map1a,Mtap1a microtubule-associated protein 1A GO:0003779 actin binding 25230 Add3 adducin 3 (gamma) GO:0003779 actin binding 25386 AQP-2,Aqp2,MGC156502,aquaporin-2aquaporin 2 (collecting duct) GO:0003779 actin binding 25484 MYR5,Myo1e,Myr3 myosin IE GO:0003779 actin binding 25576 14-3-3e1,MGC93547,Ywhah -

SUPPLEMENTAL DATA Supplemental Materials And
SUPPLEMENTAL DATA Supplemental Materials and Methods Cells and Cell Culture Human breast carcinoma cell lines, MDA-MB-231 and MCF7, were purchased from American Type Tissue Culture Collection (ATCC). 231BoM-1833, 231BrM-2a, CN34, CN34-BoM2d, CN34-BrM2c and MCF7- BoM2d cell lines were kindly provided by Dr. Joan Massagué (Memorial Sloan-Kettering Cancer Center) (1-3). Luciferase-labeled cells were generated by infecting the lentivirus carrying the firefly luciferase gene. The immortalized mouse bone microvascular endothelial cell (mBMEC) was a generous gift from Dr. Isaiah J. Fidler (M.D. Anderson Cancer Center) (4). MCF10A and MCF10DCIS.com cells were purchased from ATCC and Asterand, respectively. MDA-MB-231, its variant cells, MCF7 and MCF-BoM2d cells were cultured in DMEM medium supplemented with 10% FBS and antibiotics. CN34 and its variant cells were cultured in Medium199 supplemented with 2.5% FBS, 10 µg/ml insulin, 0.5 µg/ml hydrocortisone, 20 ng/ml EGF, 100 ng/ml cholera toxin and antibiotics. MCF10DCIS.com cells were cultured in RPMI-1640 medium supplemented with 10% FBS and antibiotics. MCF10A cells were cultured in MEGM mammary epithelial cell growth medium (Lonza). mBMEC was maintained at 8% CO2 at 33 °C in DMEM with 10% FBS, 2 mM L-glutamine, 1 mM sodium pyruvate, 1% non-essential amino acids and 1% vitamin mixture. Bone marrow stromal fibroblast cell lines HS5 and HS27A, and osteoblast cell line, hFOB1.19, were purchased from ATCC. Bone marrow derived human mesenchymal stem cells, BM-hMSC, were isolated for enrichment of plastic adherent cells from unprocessed bone marrow (Lonza) which was depleted of red blood cells. -
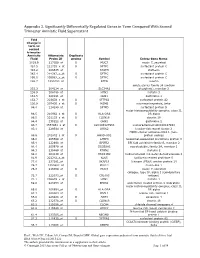
Appendix 2. Significantly Differentially Regulated Genes in Term Compared with Second Trimester Amniotic Fluid Supernatant
Appendix 2. Significantly Differentially Regulated Genes in Term Compared With Second Trimester Amniotic Fluid Supernatant Fold Change in term vs second trimester Amniotic Affymetrix Duplicate Fluid Probe ID probes Symbol Entrez Gene Name 1019.9 217059_at D MUC7 mucin 7, secreted 424.5 211735_x_at D SFTPC surfactant protein C 416.2 206835_at STATH statherin 363.4 214387_x_at D SFTPC surfactant protein C 295.5 205982_x_at D SFTPC surfactant protein C 288.7 1553454_at RPTN repetin solute carrier family 34 (sodium 251.3 204124_at SLC34A2 phosphate), member 2 238.9 206786_at HTN3 histatin 3 161.5 220191_at GKN1 gastrokine 1 152.7 223678_s_at D SFTPA2 surfactant protein A2 130.9 207430_s_at D MSMB microseminoprotein, beta- 99.0 214199_at SFTPD surfactant protein D major histocompatibility complex, class II, 96.5 210982_s_at D HLA-DRA DR alpha 96.5 221133_s_at D CLDN18 claudin 18 94.4 238222_at GKN2 gastrokine 2 93.7 1557961_s_at D LOC100127983 uncharacterized LOC100127983 93.1 229584_at LRRK2 leucine-rich repeat kinase 2 HOXD cluster antisense RNA 1 (non- 88.6 242042_s_at D HOXD-AS1 protein coding) 86.0 205569_at LAMP3 lysosomal-associated membrane protein 3 85.4 232698_at BPIFB2 BPI fold containing family B, member 2 84.4 205979_at SCGB2A1 secretoglobin, family 2A, member 1 84.3 230469_at RTKN2 rhotekin 2 82.2 204130_at HSD11B2 hydroxysteroid (11-beta) dehydrogenase 2 81.9 222242_s_at KLK5 kallikrein-related peptidase 5 77.0 237281_at AKAP14 A kinase (PRKA) anchor protein 14 76.7 1553602_at MUCL1 mucin-like 1 76.3 216359_at D MUC7 mucin 7, -

Supplementary Methods
Supplementary methods Human lung tissues and tissue microarray (TMA) All human tissues were obtained from the Lung Cancer Specialized Program of Research Excellence (SPORE) Tissue Bank at the M.D. Anderson Cancer Center (Houston, TX). A collection of 26 lung adenocarcinomas and 24 non-tumoral paired tissues were snap-frozen and preserved in liquid nitrogen for total RNA extraction. For each tissue sample, the percentage of malignant tissue was calculated and the cellular composition of specimens was determined by histological examination (I.I.W.) following Hematoxylin-Eosin (H&E) staining. All malignant samples retained contained more than 50% tumor cells. Specimens resected from NSCLC stages I-IV patients who had no prior chemotherapy or radiotherapy were used for TMA analysis by immunohistochemistry. Patients who had smoked at least 100 cigarettes in their lifetime were defined as smokers. Samples were fixed in formalin, embedded in paraffin, stained with H&E, and reviewed by an experienced pathologist (I.I.W.). The 413 tissue specimens collected from 283 patients included 62 normal bronchial epithelia, 61 bronchial hyperplasias (Hyp), 15 squamous metaplasias (SqM), 9 squamous dysplasias (Dys), 26 carcinomas in situ (CIS), as well as 98 squamous cell carcinomas (SCC) and 141 adenocarcinomas. Normal bronchial epithelia, hyperplasia, squamous metaplasia, dysplasia, CIS, and SCC were considered to represent different steps in the development of SCCs. All tumors and lesions were classified according to the World Health Organization (WHO) 2004 criteria. The TMAs were prepared with a manual tissue arrayer (Advanced Tissue Arrayer ATA100, Chemicon International, Temecula, CA) using 1-mm-diameter cores in triplicate for tumors and 1.5 to 2-mm cores for normal epithelial and premalignant lesions. -

Discovery of a Molecular Glue That Enhances Uprmt to Restore
bioRxiv preprint doi: https://doi.org/10.1101/2021.02.17.431525; this version posted February 17, 2021. The copyright holder for this preprint (which was not certified by peer review) is the author/funder. All rights reserved. No reuse allowed without permission. Title: Discovery of a molecular glue that enhances UPRmt to restore proteostasis via TRKA-GRB2-EVI1-CRLS1 axis Authors: Li-Feng-Rong Qi1, 2 †, Cheng Qian1, †, Shuai Liu1, 2†, Chao Peng3, 4, Mu Zhang1, Peng Yang1, Ping Wu3, 4, Ping Li1 and Xiaojun Xu1, 2 * † These authors share joint first authorship Running title: Ginsenoside Rg3 reverses Parkinson’s disease model by enhancing mitochondrial UPR Affiliations: 1 State Key Laboratory of Natural Medicines, China Pharmaceutical University, 210009, Nanjing, Jiangsu, China. 2 Jiangsu Key Laboratory of Drug Discovery for Metabolic Diseases, China Pharmaceutical University, 210009, Nanjing, Jiangsu, China. 3. National Facility for Protein Science in Shanghai, Zhangjiang Lab, Shanghai Advanced Research Institute, Chinese Academy of Science, Shanghai 201210, China 4. Shanghai Science Research Center, Chinese Academy of Sciences, Shanghai, 201204, China. Corresponding author: Ping Li, State Key Laboratory of Natural Medicines, China Pharmaceutical University, 210009, Nanjing, Jiangsu, China. Email: [email protected], Xiaojun Xu, State Key Laboratory of Natural Medicines, Jiangsu Key Laboratory of Drug Discovery for Metabolic Diseases, China Pharmaceutical University, 210009, Nanjing, Jiangsu, China. Telephone number: +86-2583271203, E-mail: [email protected]. bioRxiv preprint doi: https://doi.org/10.1101/2021.02.17.431525; this version posted February 17, 2021. The copyright holder for this preprint (which was not certified by peer review) is the author/funder. -

Sox2 Promotes Malignancy in Glioblastoma by Regulating
Volume 16 Number 3 March 2014 pp. 193–206.e25 193 www.neoplasia.com Artem D. Berezovsky*, Laila M. Poisson†, Sox2 Promotes Malignancy in ‡ ‡ David Cherba , Craig P. Webb , Glioblastoma by Regulating Andrea D. Transou*, Nancy W. Lemke*, Xin Hong*, Laura A. Hasselbach*, Susan M. Irtenkauf*, Plasticity and Astrocytic Tom Mikkelsen*,§ and Ana C. deCarvalho* Differentiation1,2 *Department of Neurosurgery, Henry Ford Hospital, Detroit, MI; †Department of Public Health Sciences, Henry Ford Hospital, Detroit, MI; ‡Program of Translational Medicine, Van Andel Research Institute, Grand Rapids, MI; §Department of Neurology, Henry Ford Hospital, Detroit, MI Abstract The high-mobility group–box transcription factor sex-determining region Y–box 2 (Sox2) is essential for the maintenance of stem cells from early development to adult tissues. Sox2 can reprogram differentiated cells into pluripotent cells in concert with other factors and is overexpressed in various cancers. In glioblastoma (GBM), Sox2 is a marker of cancer stemlike cells (CSCs) in neurosphere cultures and is associated with the proneural molecular subtype. Here, we report that Sox2 expression pattern in GBM tumors and patient-derived mouse xenografts is not restricted to a small percentage of cells and is coexpressed with various lineage markers, suggesting that its expression extends beyond CSCs to encompass more differentiated neoplastic cells across molecular subtypes. Employing a CSC derived from a patient with GBM and isogenic differentiated cell model, we show that Sox2 knockdown in the differentiated state abolished dedifferentiation and acquisition of CSC phenotype. Furthermore, Sox2 deficiency specifically impaired the astrocytic component of a biphasic gliosarcoma xenograft model while allowing the formation of tumors with sarcomatous phenotype. -

Potential Role Vasculogenesis in Lupus Are Mediated
Downloaded from http://www.jimmunol.org/ by guest on September 28, 2021 Kaplan is online at: on α average * The Journal of Immunology published online 30 August 2010 from submission to initial decision 4 weeks from acceptance to publication The Detrimental Effects of IFN- http://www.jimmunol.org/content/early/2010/08/30/jimmun ol.1001782 Vasculogenesis in Lupus Are Mediated by Repression of IL-1 Pathways: Potential Role in Atherogenesis and Renal Vascular Rarefaction J Immunol Seth G. Thacker, Celine C. Berthier, Deborah Mattinzoli, Maria Pia Rastaldi, Matthias Kretzler and Mariana J. Submit online. Every submission reviewed by practicing scientists ? is published twice each month by Receive free email-alerts when new articles cite this article. Sign up at: http://jimmunol.org/alerts http://jimmunol.org/subscription Submit copyright permission requests at: http://www.aai.org/About/Publications/JI/copyright.html http://www.jimmunol.org/content/suppl/2010/08/30/jimmunol.100178 2.DC1 Information about subscribing to The JI No Triage! Fast Publication! Rapid Reviews! 30 days* Why • • • Material Permissions Email Alerts Subscription Supplementary The Journal of Immunology The American Association of Immunologists, Inc., 1451 Rockville Pike, Suite 650, Rockville, MD 20852 All rights reserved. Print ISSN: 0022-1767 Online ISSN: 1550-6606. This information is current as of September 28, 2021. Published August 30, 2010, doi:10.4049/jimmunol.1001782 The Journal of Immunology The Detrimental Effects of IFN-a on Vasculogenesis in Lupus Are Mediated by Repression of IL-1 Pathways: Potential Role in Atherogenesis and Renal Vascular Rarefaction Seth G. Thacker,*,1 Celine C. Berthier,†,1 Deborah Mattinzoli,‡ Maria Pia Rastaldi,‡ Matthias Kretzler,† and Mariana J. -

The DNA Sequence and Comparative Analysis of Human Chromosome 20
articles The DNA sequence and comparative analysis of human chromosome 20 P. Deloukas, L. H. Matthews, J. Ashurst, J. Burton, J. G. R. Gilbert, M. Jones, G. Stavrides, J. P. Almeida, A. K. Babbage, C. L. Bagguley, J. Bailey, K. F. Barlow, K. N. Bates, L. M. Beard, D. M. Beare, O. P. Beasley, C. P. Bird, S. E. Blakey, A. M. Bridgeman, A. J. Brown, D. Buck, W. Burrill, A. P. Butler, C. Carder, N. P. Carter, J. C. Chapman, M. Clamp, G. Clark, L. N. Clark, S. Y. Clark, C. M. Clee, S. Clegg, V. E. Cobley, R. E. Collier, R. Connor, N. R. Corby, A. Coulson, G. J. Coville, R. Deadman, P. Dhami, M. Dunn, A. G. Ellington, J. A. Frankland, A. Fraser, L. French, P. Garner, D. V. Grafham, C. Grif®ths, M. N. D. Grif®ths, R. Gwilliam, R. E. Hall, S. Hammond, J. L. Harley, P. D. Heath, S. Ho, J. L. Holden, P. J. Howden, E. Huckle, A. R. Hunt, S. E. Hunt, K. Jekosch, C. M. Johnson, D. Johnson, M. P. Kay, A. M. Kimberley, A. King, A. Knights, G. K. Laird, S. Lawlor, M. H. Lehvaslaiho, M. Leversha, C. Lloyd, D. M. Lloyd, J. D. Lovell, V. L. Marsh, S. L. Martin, L. J. McConnachie, K. McLay, A. A. McMurray, S. Milne, D. Mistry, M. J. F. Moore, J. C. Mullikin, T. Nickerson, K. Oliver, A. Parker, R. Patel, T. A. V. Pearce, A. I. Peck, B. J. C. T. Phillimore, S. R. Prathalingam, R. W. Plumb, H. Ramsay, C. M. -

Targeting the DEK Oncogene in Head and Neck Squamous Cell Carcinoma: Functional and Transcriptional Consequences
Targeting the DEK oncogene in head and neck squamous cell carcinoma: functional and transcriptional consequences A dissertation submitted to the Graduate School of the University of Cincinnati in partial fulfillment of the requirements to the degree of Doctor of Philosophy (Ph.D.) in the Department of Cancer and Cell Biology of the College of Medicine March 2015 by Allie Kate Adams B.S. The Ohio State University, 2009 Dissertation Committee: Susanne I. Wells, Ph.D. (Chair) Keith A. Casper, M.D. Peter J. Stambrook, Ph.D. Ronald R. Waclaw, Ph.D. Susan E. Waltz, Ph.D. Kathryn A. Wikenheiser-Brokamp, M.D., Ph.D. Abstract Head and neck squamous cell carcinoma (HNSCC) is one of the most common malignancies worldwide with over 50,000 new cases in the United States each year. For many years tobacco and alcohol use were the main etiological factors; however, it is now widely accepted that human papillomavirus (HPV) infection accounts for at least one-quarter of all HNSCCs. HPV+ and HPV- HNSCCs are studied as separate diseases as their prognosis, treatment, and molecular signatures are distinct. Five-year survival rates of HNSCC hover around 40-50%, and novel therapeutic targets and biomarkers are necessary to improve patient outcomes. Here, we investigate the DEK oncogene and its function in regulating HNSCC development and signaling. DEK is overexpressed in many cancer types, with roles in molecular processes such as transcription, DNA repair, and replication, as well as phenotypes such as apoptosis, senescence, and proliferation. DEK had never been previously studied in this tumor type; therefore, our studies began with clinical specimens to examine DEK expression patterns in primary HNSCC tissue. -

Supplementary Table 1
Protein Associated Description NC miR1 NC miR-1 Base 2 Log Name Gene Name Peptides Peptides PepHits PepHits of NC/miR-1 ENSP00000338413 UBA1 ubiquitin-like modifier activating enzyme 1 14 0 59 0 5.9 ENSP00000304592 FASN fatty acid synthase 33 1 99 1 5.6 ENSP00000296122 PPP1CB protein phosphatase 1, catalytic subunit, beta isozyme 6 0 36 0 5.2 ENSP00000220849 EIF3E eukaryotic translation initiation factor 3, subunit E 9 0 35 0 5.2 ENSP00000346037 RPLP1 ribosomal protein, large, P1 1 0 32 0 5.0 ENSP00000262982 CSE1L CSE1 chromosome segregation 1-like 12 0 32 0 5.0 ENSP00000353157 septin 2 septin 2 5 0 28 0 4.9 ENSP00000326031 PPP1CA protein phosphatase 1, catalytic subunit, alpha isozyme 8 0 28 0 4.9 ENSP00000401802 PSMC6 proteasome (prosome, macropain) 26S subunit, ATPase, 6 8 0 28 0 4.9 ENSP00000327539 HNRNPH1 heterogeneous nuclear ribonucleoprotein H1 5 0 28 0 4.9 ENSP00000335084 PPP1CC protein phosphatase 1, catalytic subunit, gamma isozyme 6 0 27 0 4.8 ENSP00000300648 GCN1L1 GCN1 general control of amino-acid synthesis 1-like 1 13 0 27 0 4.8 (yeast) ENSP00000358765 4 0 27 0 4.8 ENSP00000325002 COPG1 coatomer protein complex, subunit gamma 1 9 0 26 0 4.8 ENSP00000298852 PSMC3 proteasome (prosome, macropain) 26S subunit, ATPase, 3 5 0 24 0 4.6 ENSP00000322419 RPLP2 ribosomal protein, large, P2 4 1 47 1 4.6 ENSP00000307288 MCM7 minichromosome maintenance complex component 7 9 0 23 0 4.6 ENSP00000309474 PSMD1 proteasome (prosome, macropain) 26S subunit, non-ATPase, 8 0 22 0 4.5 1 ENSP00000358921 ACTR1A ARP1 actin-related protein 1 homolog -

Enzymatische Alkinfunktionalisierung Zur Markierung Und Identifizierung
Enzymatische Alkinfunktionalisierung zur Markierung und Identifizierung von Protein-Methyltransferase-Substraten Von der Fakultat¨ f¨ur Mathematik, Informatik und Naturwissenschaften der RWTH Aachen University zur Erlangung des akademischen Grades einer Doktorin der Naturwissenschaften genehmigte Dissertation vorgelegt von Diplom-Gymnasiallehrerin Sophie Willnow aus Hattingen Berichter: Universitatsprofessor¨ Dr. Elmar Weinhold Universitatsprofessor¨ Dr. Bernhard L¨uscher Tag der m¨undlichen Pr¨ufung: 06. Juli 2012 Diese Dissertation ist auf den Internetseiten der Hochschulbibliothek online verf¨ugbar. Diese Arbeit wurde im Zeitraum von September 2008 bis Oktober 2011 am Institut f¨ur Orga- nische Chemie der Rheinisch-Westf¨alischen Technischen Hochschule Aachen (RWTH Aachen University) unter Anleitung von Prof. Dr. Elmar Weinhold und am Institut f¨ur Biochemie und Molekularbiologie des Universit¨atsklinikums Aachen unter Anleitung von Prof. Dr. Bernhard L¨uscher angefertigt. Mein Dank gilt an erster Stelle Prof. Dr. Elmar Weinhold f¨ur die interessante interdisziplin¨are Themenstellung zwischen Chemie und Biologie, f¨ur das entgegengebrachte Vertrauen, auch eigene Ideen umsetzen zu k¨onnen, und f¨ur die vielen konstruktiven Diskussionen. Ich bedanke mich außerdem herzlich bei Prof. Dr. Bernhard L¨uscher f¨ur die vielen hilfreichen Anmerkungen und Einsch¨atzungen. Teile dieser Arbeit wurden bereits ver¨offentlicht: 1. W. Peters, S. Willnow, M. Duisgen, H. Kleine, T. Macherey, K. E. Duncan, D. W. Litch- field, B. L¨uscher, E. Weinhold. Enzymatic Site-Specific Functionalization of Protein Me- thyltransferase Substrates with Alkynes for Click Labeling. Angew. Chem. 2010, 122, 5296–5299; Angew. Chem. Int. Ed. 2010, 49, 5170–5173. 2. Y. Motorin, J. Burhenne, R. Teimer, K. Koynov, S. Willnow, E. Weinhold, M. -

Immortalization of Common Marmoset Monkey Fibroblasts by Piggybac Transposition of Htert
RESEARCH ARTICLE Immortalization of common marmoset monkey fibroblasts by piggyBac transposition of hTERT 1,2☯ 1☯¤a 3 3 Stoyan PetkovID , Tobias Kahland , Orr Shomroni , Thomas Lingner , Gabriela Salinas3, Sigrid Fuchs4, Katharina Debowski1¤b, RuÈ diger Behr1,2* 1 Platform Degenerative Diseases, German Primate Center- Leibniz Institute for Primate Research, GoÈttingen, Germany, 2 DZHK (German Center for Cardiovascular Research), Partner Site GoÈttingen, GoÈttingen, Germany, 3 Microarray and Deep-Sequencing Core Facility, University Medical Center GoÈttingen a1111111111 (UMG), GoÈttingen, Germany, 4 Department of Human Genetics, University Medical Center Hamburg- a1111111111 Eppendorf, Hamburg, Germany a1111111111 ☯ These authors contributed equally to this work. a1111111111 ¤a Current address: a-tune Software AG, Darmstadt, Germany a1111111111 ¤b Current address: STEMCELL Technologies Germany GmbH, Cologne, Germany * [email protected] Abstract OPEN ACCESS Citation: Petkov S, Kahland T, Shomroni O, Following a certain type-specific number of mitotic divisions, terminally differentiated cells Lingner T, Salinas G, Fuchs S, et al. (2018) undergo proliferative senescence, thwarting efforts to expand different cell populations in Immortalization of common marmoset monkey vitro for the needs of scientific research or medical therapies. The primary cause of this phe- fibroblasts by piggyBac transposition of hTERT. PLoS ONE 13(9): e0204580. https://doi.org/ nomenon is the progressive shortening of the telomeres and the subsequent activation of 10.1371/journal.pone.0204580 cell cycle control pathways leading to a block of cell proliferation. Restoration of telomere Editor: Gabriele Saretzki, University of Newcastle, length by transgenic expression of telomerase reverse transcriptase (TERT) usually results UNITED KINGDOM in bypassing of the replicative senescence and ultimately in cell immortalization.