Pfeiffer Syndrome Type II Discovered Perinatally
Total Page:16
File Type:pdf, Size:1020Kb
Load more
Recommended publications
-

Megalencephaly and Macrocephaly
277 Megalencephaly and Macrocephaly KellenD.Winden,MD,PhD1 Christopher J. Yuskaitis, MD, PhD1 Annapurna Poduri, MD, MPH2 1 Department of Neurology, Boston Children’s Hospital, Boston, Address for correspondence Annapurna Poduri, Epilepsy Genetics Massachusetts Program, Division of Epilepsy and Clinical Electrophysiology, 2 Epilepsy Genetics Program, Division of Epilepsy and Clinical Department of Neurology, Fegan 9, Boston Children’s Hospital, 300 Electrophysiology, Department of Neurology, Boston Children’s Longwood Avenue, Boston, MA 02115 Hospital, Boston, Massachusetts (e-mail: [email protected]). Semin Neurol 2015;35:277–287. Abstract Megalencephaly is a developmental disorder characterized by brain overgrowth secondary to increased size and/or numbers of neurons and glia. These disorders can be divided into metabolic and developmental categories based on their molecular etiologies. Metabolic megalencephalies are mostly caused by genetic defects in cellular metabolism, whereas developmental megalencephalies have recently been shown to be caused by alterations in signaling pathways that regulate neuronal replication, growth, and migration. These disorders often lead to epilepsy, developmental disabilities, and Keywords behavioral problems; specific disorders have associations with overgrowth or abnor- ► megalencephaly malities in other tissues. The molecular underpinnings of many of these disorders are ► hemimegalencephaly now understood, providing insight into how dysregulation of critical pathways leads to ► -

Genetics of Congenital Hand Anomalies
G. C. Schwabe1 S. Mundlos2 Genetics of Congenital Hand Anomalies Die Genetik angeborener Handfehlbildungen Original Article Abstract Zusammenfassung Congenital limb malformations exhibit a wide spectrum of phe- Angeborene Handfehlbildungen sind durch ein breites Spektrum notypic manifestations and may occur as an isolated malforma- an phänotypischen Manifestationen gekennzeichnet. Sie treten tion and as part of a syndrome. They are individually rare, but als isolierte Malformation oder als Teil verschiedener Syndrome due to their overall frequency and severity they are of clinical auf. Die einzelnen Formen kongenitaler Handfehlbildungen sind relevance. In recent years, increasing knowledge of the molecu- selten, besitzen aber aufgrund ihrer Häufigkeit insgesamt und lar basis of embryonic development has significantly enhanced der hohen Belastung für Betroffene erhebliche klinische Rele- our understanding of congenital limb malformations. In addi- vanz. Die fortschreitende Erkenntnis über die molekularen Me- tion, genetic studies have revealed the molecular basis of an in- chanismen der Embryonalentwicklung haben in den letzten Jah- creasing number of conditions with primary or secondary limb ren wesentlich dazu beigetragen, die genetischen Ursachen kon- involvement. The molecular findings have led to a regrouping of genitaler Malformationen besser zu verstehen. Der hohe Grad an malformations in genetic terms. However, the establishment of phänotypischer Variabilität kongenitaler Handfehlbildungen er- precise genotype-phenotype correlations for limb malforma- schwert jedoch eine Etablierung präziser Genotyp-Phänotyp- tions is difficult due to the high degree of phenotypic variability. Korrelationen. In diesem Übersichtsartikel präsentieren wir das We present an overview of congenital limb malformations based Spektrum kongenitaler Malformationen, basierend auf einer ent- 85 on an anatomic and genetic concept reflecting recent molecular wicklungsbiologischen, anatomischen und genetischen Klassifi- and developmental insights. -
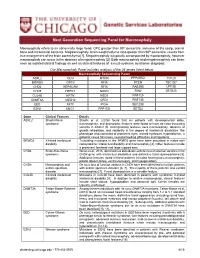
Macrocephaly Information Sheet 6-13-19
Next Generation Sequencing Panel for Macrocephaly Clinical Features: Macrocephaly refers to an abnormally large head, OFC greater than 98th percentile, inclusive of the scalp, cranial bone and intracranial contents. Megalencephaly, brain weight/volume ratio greater than 98th percentile, results from true enlargement of the brain parenchyma [1]. Megalencephaly is typically accompanied by macrocephaly, however macrocephaly can occur in the absence of megalencephaly [2]. Both macrocephaly and megalencephaly can been seen as isolated clinical findings as well as clinical features of a mutli-systemic syndromic diagnosis. Our Macrocephaly Panel includes analysis of the 36 genes listed below. Macrocephaly Sequencing Panel ASXL2 GLI3 MTOR PPP2R5D TCF20 BRWD3 GPC3 NFIA PTEN TBC1D7 CHD4 HEPACAM NFIX RAB39B UPF3B CHD8 HERC1 NONO RIN2 ZBTB20 CUL4B KPTN NSD1 RNF125 DNMT3A MED12 OFD1 RNF135 EED MITF PIGA SEC23B EZH2 MLC1 PPP1CB SETD2 Gene Clinical Features Details ASXL2 Shashi-Pena Shashi et al. (2016) found that six patients with developmental delay, syndrome macrocephaly, and dysmorphic features were found to have de novo truncating variants in ASXL2 [3]. Distinguishing features were macrocephaly, absence of growth retardation, and variability in the degree of intellectual disabilities The phenotype also consisted of prominent eyes, arched eyebrows, hypertelorism, a glabellar nevus flammeus, neonatal feeding difficulties and hypotonia. BRWD3 X-linked intellectual Truncating mutations in the BRWD3 gene have been described in males with disability nonsyndromic intellectual disability and macrocephaly [4]. Other features include a prominent forehead and large cupped ears. CHD4 Sifrim-Hitz-Weiss Weiss et al., 2016, identified five individuals with de novo missense variants in the syndrome CHD4 gene with intellectual disabilities and distinctive facial dysmorphisms [5]. -

Sotos Syndrome
European Journal of Human Genetics (2007) 15, 264–271 & 2007 Nature Publishing Group All rights reserved 1018-4813/07 $30.00 www.nature.com/ejhg PRACTICAL GENETICS In association with Sotos syndrome Sotos syndrome is an autosomal dominant condition characterised by a distinctive facial appearance, learning disability and overgrowth resulting in tall stature and macrocephaly. In 2002, Sotos syndrome was shown to be caused by mutations and deletions of NSD1, which encodes a histone methyltransferase implicated in chromatin regulation. More recently, the NSD1 mutational spectrum has been defined, the phenotype of Sotos syndrome clarified and diagnostic and management guidelines developed. Introduction In brief Sotos syndrome was first described in 1964 by Juan Sotos Sotos syndrome is characterised by a distinctive facial and the major diagnostic criteria of a distinctive facial appearance, learning disability and childhood over- appearance, childhood overgrowth and learning disability growth. were established in 1994 by Cole and Hughes.1,2 In 2002, Sotos syndrome is associated with cardiac anomalies, cloning of the breakpoints of a de novo t(5;8)(q35;q24.1) renal anomalies, seizures and/or scoliosis in B25% of translocation in a child with Sotos syndrome led to the cases and a broad variety of additional features occur discovery that Sotos syndrome is caused by haploinsuffi- less frequently. ciency of the Nuclear receptor Set Domain containing NSD1 abnormalities, such as truncating mutations, protein 1 gene, NSD1.3 Subsequently, extensive analyses of missense mutations in functional domains, partial overgrowth cases have shown that intragenic NSD1 muta- gene deletions and 5q35 microdeletions encompass- tions and 5q35 microdeletions encompassing NSD1 cause ing NSD1, are identifiable in the majority (490%) of 490% of Sotos syndrome cases.4–10 In addition, NSD1 Sotos syndrome cases. -

(12) Patent Application Publication (10) Pub. No.: US 2010/0210567 A1 Bevec (43) Pub
US 2010O2.10567A1 (19) United States (12) Patent Application Publication (10) Pub. No.: US 2010/0210567 A1 Bevec (43) Pub. Date: Aug. 19, 2010 (54) USE OF ATUFTSINASATHERAPEUTIC Publication Classification AGENT (51) Int. Cl. A638/07 (2006.01) (76) Inventor: Dorian Bevec, Germering (DE) C07K 5/103 (2006.01) A6IP35/00 (2006.01) Correspondence Address: A6IPL/I6 (2006.01) WINSTEAD PC A6IP3L/20 (2006.01) i. 2O1 US (52) U.S. Cl. ........................................... 514/18: 530/330 9 (US) (57) ABSTRACT (21) Appl. No.: 12/677,311 The present invention is directed to the use of the peptide compound Thr-Lys-Pro-Arg-OH as a therapeutic agent for (22) PCT Filed: Sep. 9, 2008 the prophylaxis and/or treatment of cancer, autoimmune dis eases, fibrotic diseases, inflammatory diseases, neurodegen (86). PCT No.: PCT/EP2008/007470 erative diseases, infectious diseases, lung diseases, heart and vascular diseases and metabolic diseases. Moreover the S371 (c)(1), present invention relates to pharmaceutical compositions (2), (4) Date: Mar. 10, 2010 preferably inform of a lyophilisate or liquid buffersolution or artificial mother milk formulation or mother milk substitute (30) Foreign Application Priority Data containing the peptide Thr-Lys-Pro-Arg-OH optionally together with at least one pharmaceutically acceptable car Sep. 11, 2007 (EP) .................................. O7017754.8 rier, cryoprotectant, lyoprotectant, excipient and/or diluent. US 2010/0210567 A1 Aug. 19, 2010 USE OF ATUFTSNASATHERAPEUTIC ment of Hepatitis BVirus infection, diseases caused by Hepa AGENT titis B Virus infection, acute hepatitis, chronic hepatitis, full minant liver failure, liver cirrhosis, cancer associated with Hepatitis B Virus infection. 0001. The present invention is directed to the use of the Cancer, Tumors, Proliferative Diseases, Malignancies and peptide compound Thr-Lys-Pro-Arg-OH (Tuftsin) as a thera their Metastases peutic agent for the prophylaxis and/or treatment of cancer, 0008. -

Identifying the Misshapen Head: Craniosynostosis and Related Disorders Mark S
CLINICAL REPORT Guidance for the Clinician in Rendering Pediatric Care Identifying the Misshapen Head: Craniosynostosis and Related Disorders Mark S. Dias, MD, FAAP, FAANS,a Thomas Samson, MD, FAAP,b Elias B. Rizk, MD, FAAP, FAANS,a Lance S. Governale, MD, FAAP, FAANS,c Joan T. Richtsmeier, PhD,d SECTION ON NEUROLOGIC SURGERY, SECTION ON PLASTIC AND RECONSTRUCTIVE SURGERY Pediatric care providers, pediatricians, pediatric subspecialty physicians, and abstract other health care providers should be able to recognize children with abnormal head shapes that occur as a result of both synostotic and aSection of Pediatric Neurosurgery, Department of Neurosurgery and deformational processes. The purpose of this clinical report is to review the bDivision of Plastic Surgery, Department of Surgery, College of characteristic head shape changes, as well as secondary craniofacial Medicine and dDepartment of Anthropology, College of the Liberal Arts characteristics, that occur in the setting of the various primary and Huck Institutes of the Life Sciences, Pennsylvania State University, State College, Pennsylvania; and cLillian S. Wells Department of craniosynostoses and deformations. As an introduction, the physiology and Neurosurgery, College of Medicine, University of Florida, Gainesville, genetics of skull growth as well as the pathophysiology underlying Florida craniosynostosis are reviewed. This is followed by a description of each type of Clinical reports from the American Academy of Pediatrics benefit from primary craniosynostosis (metopic, unicoronal, bicoronal, sagittal, lambdoid, expertise and resources of liaisons and internal (AAP) and external reviewers. However, clinical reports from the American Academy of and frontosphenoidal) and their resultant head shape changes, with an Pediatrics may not reflect the views of the liaisons or the emphasis on differentiating conditions that require surgical correction from organizations or government agencies that they represent. -

Bagatelle Cassidy Syndrome: Macrocephaly
Journal of Clinical and Experimental Genetics Volume 1 | Issue 1 Case Report Open Access Bagatelle Cassidy Syndrome: Macrocephaly with Fronto-Facial Dysmorphism and Hearing Loss; an Extremely Rare Case Avina Fierro JA*1 and Hernandez Avina DA2 1Department of Pediatric Dysmorphology, IMSS Medical Center; Guadalajara, Mexico 2General Hospital Zona 2, IMSS Aguascalientes, Mexico *Corresponding author: Avina Fierro JA, Department of Pediatric Dysmorphology, IMSS Medical Center; Guadalajara, Mexico, Tel: (52)3336-743701, E-mail: [email protected] Citation: Avina Fierro JA, Hernandez Avina DA (2015) Bagatelle Cassidy Syndrome: Macrocephaly with Fronto-Facial Dysmorphism and Hearing Loss; an Extremely Rare Case. J Clin Exp Gen 1(1): 101 Abstract Bagatelle Cassidy syndrome is a very rare disease first described in 1995 in a boy with macrocephaly, hypertelorism, hearing loss, developmental delay and facial dysmorphism. The cause of this syndrome is unknown and has no specific diagnostic test. We report the case of a 9-year-old girl with a cerebro-fronto-facial malformation syndrome with macrocephaly, with significant decrease of the hearing, moderate hearing loss (50 db HL at 4000 Hz); mild mental retardation (IQ 50) and noticeable speech delay, psychomotor and developmental delay. Facial anomalies show prominent forehead (frontal bossing) , hypertelorism, downslanting palpebral fissures, flat nasal bridge, short nose with anteverted nostrils; broad columella, long smooth philtrum and carp-like mouth; this phenotype represents the specific -

RIN2 Deficiency Results in Macrocephaly, Alopecia, Cutis Laxa
REPORT RIN2 Deficiency Results in Macrocephaly, Alopecia, Cutis Laxa, and Scoliosis: MACS Syndrome Lina Basel-Vanagaite,1,2,14 Ofer Sarig,4,14 Dov Hershkovitz,6,7 Dana Fuchs-Telem,2,4 Debora Rapaport,3 Andrea Gat,5 Gila Isman,4 Idit Shirazi,4 Mordechai Shohat,1,2 Claes D. Enk,10 Efrat Birk,2 Ju¨rgen Kohlhase,11 Uta Matysiak-Scholze,11 Idit Maya,1 Carlos Knopf,9 Anette Peffekoven,12 Hans-Christian Hennies,12 Reuven Bergman,8 Mia Horowitz,3 Akemi Ishida-Yamamoto,13 and Eli Sprecher2,4,6,* Inherited disorders of elastic tissue represent a complex and heterogeneous group of diseases, characterized often by sagging skin and occasionally by life-threatening visceral complications. In the present study, we report on an autosomal-recessive disorder that we have termed MACS syndrome (macrocephaly, alopecia, cutis laxa, and scoliosis). The disorder was mapped to chromosome 20p11.21-p11.23, and a homozygous frameshift mutation in RIN2 was found to segregate with the disease phenotype in a large consan- guineous kindred. The mutation identified results in decreased expression of RIN2, a ubiquitously expressed protein that interacts with Rab5 and is involved in the regulation of endocytic trafficking. RIN2 deficiency was found to be associated with paucity of dermal micro- fibrils and deficiency of fibulin-5, which may underlie the abnormal skin phenotype displayed by the patients. Disorders of elastic tissue often share common phenotypic shown to result in decreased secretion of elastin.9,10 In features, including redundant skin, hyperlaxity of joints, addition, -

Congenital Anomalies and in Utero Antiretroviral Exposure in Human Immunodeficiency Virus– Exposed Uninfected Infants
Supplementary Online Content Williams PL, Crain MJ, Yildirim C, et al; Pediatric HIV/AIDS Cohort Study. Congenital anomalies and in utero antiretroviral exposure in human immunodeficiency virus– exposed uninfected infants. Published online November 10, 2014. JAMA Pediatr. doi:10.1001/jamapediatrics.2014.1889. eTable 1. Frequency of Specific Major Congenital Anomalies Within Anomaly Categories eTable 2. Anomalies Reported Among Children Exposed to Atazanavir During the First Trimester eTable 3. Association of Timing of the First ARV Exposure During Pregnancy With Congenital Anomalies by ARV Drug Class and for Specific ARV Drugs This supplementary material has been provided by the authors to give readers additional information about their work. © 2014 American Medical Association. All rights reserved. Downloaded From: https://jamanetwork.com/ on 09/24/2021 eTable 1. Frequency of Specific Major Congenital Anomalies Within Anomaly Categories # of children with at Total # of least one major anomaly in Anomaly anomalies category Category (Total=242) (Total=201) List of Major Anomalies Musculoskeletal 72 59 Polydactyly (15), torticollis/muscular anomaly (12), clubfoot, talipes, other foot deformity (9), congenital dislocation of hip (5), craniosynostosis (4), plagiocephaly (4), pectus excavatum/funnel chest (3), lower limb anomaly (3), hypertelorism/other face or skull anomaly (3), spina bifida occulta/spine anomaly (3), syndactyly (3), inguinal hernia (2), diaphragmatic hernia/Morgagni, genu recurvatum/bowed legs, rib/sternum anomaly, scoliosis/congenital -

Improving Diagnosis and Treatment of Craniofacial Malformations Utilizing Animal Models
CHAPTER SEVENTEEN From Bench to Bedside and Back: Improving Diagnosis and Treatment of Craniofacial Malformations Utilizing Animal Models Alice F. Goodwin*,†, Rebecca Kim*,†, Jeffrey O. Bush*,{,},1, Ophir D. Klein*,†,},},1 *Program in Craniofacial Biology, University of California San Francisco, San Francisco, California, USA †Department of Orofacial Sciences, University of California San Francisco, San Francisco, California, USA { Department of Cell and Tissue Biology, University of California San Francisco, San Francisco, California, USA } Department of Pediatrics, University of California San Francisco, San Francisco, California, USA } Institute for Human Genetics, University of California San Francisco, San Francisco, California, USA 1Corresponding authors: e-mail address: [email protected]; [email protected] Contents 1. Models to Uncover Genetics of Cleft Lip and Palate 460 2. Treacher Collins: Proof of Concept of a Nonsurgical Therapeutic for a Craniofacial Syndrome 467 3. RASopathies: Understanding and Developing Treatment for Syndromes of the RAS Pathway 468 4. Craniosynostosis: Pursuing Genetic and Pharmaceutical Alternatives to Surgical Treatment 473 5. XLHED: Developing Treatment Based on Knowledge Gained from Mouse and Canine Models 477 6. Concluding Thoughts 481 Acknowledgments 481 References 481 Abstract Craniofacial anomalies are among the most common birth defects and are associated with increased mortality and, in many cases, the need for lifelong treatment. Over the past few decades, dramatic advances in the surgical and medical care of these patients have led to marked improvements in patient outcomes. However, none of the treat- ments currently in clinical use address the underlying molecular causes of these disor- ders. Fortunately, the field of craniofacial developmental biology provides a strong foundation for improved diagnosis and for therapies that target the genetic causes # Current Topics in Developmental Biology, Volume 115 2015 Elsevier Inc. -

Date Due Date Due Date Due
PLACE ll RETURN BOX to roman this chockout from your mood. TO AVOID FINES Mom on or baton dd. duo. DATE DUE DATE DUE DATE DUE MSU In An Affirmative Action/Equal Opponfirmy Inflation mm: SCREENING FOR MUTATIONS IN PAX3 AND MITF IN WAARDENBURG SYNDROME AND WAARDENBURG SYNDROME-LIKE INDIVIDUALS By Melisa Lynn Carey A THESIS Submitted to Michigan State University in partial fulfillment of the requirements for a degree of MASTER OF SCIENCE Department of Zoology 1 996 ABSTRACT SCREENING FOR MUTATIONS IN PAX3 AND MITF IN WAARDENBURG SYNDROME AND WAARDENBURG SYNDROME-LIKE INDIVIDUALS BY Melisa L. Carey Waardenburg Syndrome (WS) is an autosomal dominant disorder characterized by pigmentary and facial anomalies and congenital deafness. Mutations causing WS have been reported in PAX3 and MITF. The goal of this study was to characterize the molecular defects in 33 unrelated WS individuals. Mutation detection was performed using Single Strand Conformational Polymorphism (SSCP) analysis and sequencing methods. Among the 33 WS individuals, a total of eight mutations were identified, seven in PAX3 and one in MITF. In this study, one of the eight mutations was identified and characterized in PAX3 exon seven in a WSI family (UoM1). The proband of UoM1 also has Septo-Optic Dysplasia. In a large family (MSU22) with WS-Iike dysmorphology and additional craniofacial anomalies, linkage was excluded to PAX3 and no mutations were identified in MITF. Herein I review the status of mutation detection in our proband screening set and add to the understanding of the role of PAX3 and MITF in development by exploring new phenotypic characteristics associated with WS. -

(12) United States Patent (10) Patent No.: US 8,853,266 B2 Dalton Et Al
USOO8853266B2 (12) United States Patent (10) Patent No.: US 8,853,266 B2 Dalton et al. (45) Date of Patent: *Oct. 7, 2014 (54) SELECTIVE ANDROGEN RECEPTOR 3,875,229 A 4, 1975 Gold MODULATORS FOR TREATING DABETES 4,036.979 A 7, 1977 Asato 4,139,638 A 2f1979 Neri et al. 4,191,775 A 3, 1980 Glen (75) Inventors: James T. Dalton, Upper Arlington, OH 4,239,776 A 12/1980 Glen et al. (US): Duane D. Miller, Germantown, 4,282,218 A 8, 1981 Glen et al. TN (US) 4,386,080 A 5/1983 Crossley et al. 4411,890 A 10/1983 Momany et al. (73) Assignee: University of Tennessee Research 4,465,507 A 8/1984 Konno et al. F dati Kn ille, TN (US) 4,636,505 A 1/1987 Tucker Oundation, Knoxv1lle, 4,880,839 A 1 1/1989 Tucker 4,977,288 A 12/1990 Kassis et al. (*) Notice: Subject to any disclaimer, the term of this 5,162,504 A 11/1992 Horoszewicz patent is extended or adjusted under 35 5,179,080 A 1/1993 Rothkopfet al. U.S.C. 154(b) by 992 days. 5,441,868 A 8, 1995 Lin et al. 5,547.933 A 8, 1996 Lin et al. This patent is Subject to a terminal dis- 5,609,849 A 3/1997 Kung claimer. 5,612,359 A 3/1997 Murugesan et al. 5,618,698 A 4/1997 Lin et al. 5,621,080 A 4/1997 Lin et al. (21) Appl. No.: 11/785,064 5,656,651 A 8/1997 Sovak et al.