Chapter 3 Bacterial and Viral Infections
Total Page:16
File Type:pdf, Size:1020Kb
Load more
Recommended publications
-
Letters to the Editor
Lepr Rev (1994) 65, 282-285 Letters to the Editor CONCOMITANT OCCURRENCE OF LEPROSY, CUTANEOUS TUBERCULOSIS AND PULMONARY TUBERCULOSIS-A CASE REPORT Sir, We report a leprosy patient also suffering from both cutaneous and pulmonary tuberculosis, a concomitant occurrence that has not previously been reported in the literature available to us. We report here a case of such rare combination. Though both the diseases are caused by mycobacter iae, no true antagonism exists to stop coexistence. The concomitant occurrence of leprosy and pulmonary tuberculosis has been well documented in the literature, 1,2 but the association of leprosy and cutaneous tuberculosis has rarely been reported.3,4,5 A 23-year-old male presented complaining of an erythematous lesion around the left orbit that Figure 1. An erythematous, oedematous lesion on the left sideof the forehead and infraorbital area, that almost encircles the orbit. 282 Letters to the Editor 283 Figure 2. Multiple ulcers in linear fashion with undermined edges and marginal hyperpigmentation on the left side of the neck. had continued for I month and multiple ulcerations with a discharge of pus on the left side of the neck for 15 days; ulcerations followed rupturing of the swelling in the neck. The swelling was of I!-months' duration, mildly painful and was gradually increasing in size. There was a history of a rise of temperature each evening and of significantweight loss. He had not been treated for leprosy and/or tuberculosis. Cutaneous examination revealed a well-defined erythematous plaque around the left orbit (Figure I). There were multiple ulcers in linear fa shion over the left side of the neck with undermined edges and hyperpigmented borders (Figure 2). -

Smelly Foot Rash
CLINICAL Smelly foot rash Paulo Morais Ligia Peralta Keywords: skin diseases, infectious Case study A previously healthy Caucasian girl, 6 years of age, presented with pruritic rash on both heels of 6 months duration. The lesions appeared as multiple depressions 1–2 mm in diameter that progressively increased in size. There was no history of trauma or insect bite. She reported local pain when walking, worse with moisture and wearing sneakers. On examination, multiple small crater- like depressions were present, some Figure 1. Heel of patient coalescing into a larger lesion on both heels (Figure 1). There was an unpleasant ‘cheesy’ protective/occluded footwear for prolonged odour and a moist appearance. Wood lamp periods.1–4 examination and potassium hydroxide testing for fungal hyphae were negative. Answer 2 Question 1 Pitted keratolysis is frequently seen during What is the diagnosis? summer and rainy seasons, particularly in tropical regions, although it occurs Question 2 worldwide.1,3,4 It is caused by Kytococcus What causes this condition? sedentarius, Dermatophilus congolensis, or species of Corynebacterium, Actinomyces or Question 3 Streptomyces.1–4 Under favourable conditions How would you confirm the diagnosis? (ie. hyperhidrosis, prolonged occlusion and increased skin surface pH), these bacteria Question 4 proliferate and produce proteinases that destroy What are the differential diagnoses? the stratum corneum, creating pits. Sulphur containing compounds produced by the bacteria Question 5 cause the characteristic malodor. What is your management strategy? Answer 3 Answer 1 Pitted keratolysis is usually a clinical Based on the typical clinical picture and the negative diagnosis with typical hyperhidrosis, malodor ancillary tests, the diagnosis of pitted keratolysis (PK) (bromhidrosis) and occasionally, tenderness, is likely. -

(ERYTHEMA NODOSUM LEPROSUM) the Term
? THE HISTOPATHOLOGY OF ACUTE PANNICULITIS NODOSA LEPROSA (ERYTHEMA NODOSUM LEPROSUM) w. J. PEPLER, M.B., Ch.B. Department of Pathology, South African Institute for Medical Research, Johannesburg R. KOOIJ, M.D. Westfort Institution, Pretoria AND J. MARSHALL, M.D. University of Pretoria, Pretoria The term "erythema nodosum leprosum" has frequently appeared in the literature on leprosy since the 1930's, apparently popularized by the Japanese (9). The occurrence of "erythema nodosum" in leprosy had previously been noted at the end of the nineteenth century by Brocq (6) and by Hansen and Looft (8), but the term seems to have fallen into disuse. As will become clear from our clinical and histological descriptions of the phenomenon commonly known as erythema nodosum leprosum, we believe the title to be a misnomer. We suggest that it would be more accurate to call it panniculitis nodosa leprosa (P.N.L,). This condition is commonly confused with acute lepra reaction, both processes being referred to as "acute reactions"; but a sharp line of distinction must be drawn between them. P.N.L. occurs only in patients with lepromatous leprosy as an acute, subacute or chronic skin eruption, with or without fever. It is characterized by showers of dusky red nodules, 0.5 to 2 cm. in diameter, on the extensor surfaces of the limbs, on the face, and, less often, on the trunk. The number of lesions appearing in an attack varies from a few to several hundreds, and they sometimes coalesce to form plaques. The nodules may be painful, and they are usually tender to touch. -

Pattern of Cutaneous Tuberculosis Among Children and Adolescent
Bangladesh Med Res Counc Bull 2012; 38: 94-97 Pattern of cutaneous tuberculosis among children and adolescent Sultana A1, Bhuiyan MSI1, Haque A2, Bashar A3, Islam MT4, Rahman MM5 1Dept. of Dermatology, Bangabandhu Sheikh Mujib Medical University (BSMMU), Dhaka, 2Dept. of Public health and informatics, BSMMU, Dhaka, 3SK Hospital, Mymensingh Medical College, Mymensingh, 4Dept. of Physical Medicine and Rehabilitation, BSMMU, Dhaka, 5Dept. of Dermatology, National Medical College, Dhaka. Email: [email protected] Abstract Cutaneous tuberculosis is one of the most subtle and difficult diagnoses for dermatologists practicing in developing countries. It has widely varied manifestations and it is important to know the spectrum of manifestations in children and adolescent. Sixty cases (age<19 years) of cutaneous tuberculosis were included in this one period study. The diagnosis was based on clinical examination, tuberculin reaction, histopathology, and response to antitubercular therapy. Histopahology revealed 38.3% had skin tuberculosis and 61.7% had diseases other than tuberculosis. Among 23 histopathologically proved cutaneous tuberculosis, 47.8% had scrofuloderma, 34.8% had lupus vulgaris and 17.4% had tuberculosis verrucosa cutis (TVC). Most common site for scrofuloderma lesions was neck and that for lupus vulgaris and TVC was lower limb. Cutaneous tuberculosis in children continues to be an important cause of morbidity, there is a high likelihood of internal involvement, especially in patients with scrofuloderma. A search is required for more sensitive, economic diagnostic tools. Introduction of Child Health (BICH) and Institute of Diseases of Tuberculosis (TB), an ancient disease has affected Chest and Hospital (IDCH) from January to humankind for more than 4,000 years1 and its December 2010. -

Disseminated Mycobacterium Tuberculosis with Ulceronecrotic Cutaneous Disease Presenting As Cellulitis Kelly L
Lehigh Valley Health Network LVHN Scholarly Works Department of Medicine Disseminated Mycobacterium Tuberculosis with Ulceronecrotic Cutaneous Disease Presenting as Cellulitis Kelly L. Reed DO Lehigh Valley Health Network, [email protected] Nektarios I. Lountzis MD Lehigh Valley Health Network, [email protected] Follow this and additional works at: http://scholarlyworks.lvhn.org/medicine Part of the Dermatology Commons, and the Medical Sciences Commons Published In/Presented At Reed, K., Lountzis, N. (2015, April 24). Disseminated Mycobacterium Tuberculosis with Ulceronecrotic Cutaneous Disease Presenting as Cellulitis. Poster presented at: Atlantic Dermatological Conference, Philadelphia, PA. This Poster is brought to you for free and open access by LVHN Scholarly Works. It has been accepted for inclusion in LVHN Scholarly Works by an authorized administrator. For more information, please contact [email protected]. Disseminated Mycobacterium Tuberculosis with Ulceronecrotic Cutaneous Disease Presenting as Cellulitis Kelly L. Reed, DO and Nektarios Lountzis, MD Lehigh Valley Health Network, Allentown, Pennsylvania Case Presentation: Discussion: Patient: 83 year-old Hispanic female Cutaneous tuberculosis (CTB) was first described in the literature in 1826 by Laennec and has since been History of Present Illness: The patient presented to the hospital for chest pain and shortness of breath and was treated for an NSTEMI. She was noted reported to manifest in a variety of clinical presentations. The most common cause is infection with the to have redness and swelling involving the right lower extremity she admitted to having for 5 months, which had not responded to multiple courses of antibiotics. She acid-fast bacillus Mycobacterium tuberculosis via either primary exogenous inoculation (direct implantation resided in Puerto Rico but recently moved to the area to be closer to her children. -

Leprosy – Eliminated and Forgotten: a Case Report Shiva Raj K.C.1,5* , Geetika K.C.1, Purnima Gyawali2, Manisha Singh3 and Milesh Jung Sijapati4
K.C. et al. Journal of Medical Case Reports (2019) 13:276 https://doi.org/10.1186/s13256-019-2198-1 CASE REPORT Open Access Leprosy – eliminated and forgotten: a case report Shiva Raj K.C.1,5* , Geetika K.C.1, Purnima Gyawali2, Manisha Singh3 and Milesh Jung Sijapati4 Abstract Background: Leprosy is a disease that was declared eliminated in 2010 from Nepal; however, new cases are diagnosed every year. The difficulty arises when the presentation of the patient is unusual. Case presentation: In this case report we present a case of a 22-year-old Tamang man, from the Terai region of Nepal, with a clinical presentation of fever, malaise, and arthralgia for the past 2 weeks with hepatosplenomegaly and bilateral cervical, axillary, and inguinal lymphadenopathy. Features of chronic inflammation with elevated erythrocyte sedimentation rate of 90 mm/hour and liver enzymes were noted. With no specific investigative findings, a diagnosis of Still’s disease was made and he was given prednisolone. On tapering the medication, after 2 weeks, the lymphadenopathy and fever reappeared. On biopsy of a lymph node, diagnosis of possible tuberculosis was made. On that basis anti-tuberculosis treatment category I was started. During his hospital stay, our patient developed nodular skin rashes on his shoulder, back, and face. The biopsy of a skin lesion showed erythema nodosum leprosum and he was diagnosed as having lepromatous leprosy with erythema nodosum leprosum; he was treated with anti-leprosy medication. Conclusion: An unusual presentations of leprosy may delay its prompt diagnosis and treatment; thus, increasing morbidity and mortality. -

Lepromatous Leprosy Simulating Sweet Syndrome
ISSN: 2469-5750 Zemmez et al. J Dermatol Res Ther 2018, 4:056 DOI: 10.23937/2469-5750/1510056 Volume 4 | Issue 1 Journal of Open Access Dermatology Research and Therapy CASE REPORT Lepromatous Leprosy Simulating Sweet Syndrome Youssef Zemmez1*, Ahmed Bouhamidi1, Salwa Belhabib2, Rachid Frikh1, Mohamed Boui1 1 and Naoufal Hjira Check for updates 1Department of Dermatology-Venereology, Mohammed V Military Training Hospital, Rabat, Morocco 2Department of Pathological Anatomy, Mohammed V Military Training Hospital, Rabat, Morocco *Corresponding author: Youssef Zemmez, Department of Dermatology-Venereology, Mohammed V Military Training Hospital, Rabat, Morocco, Tel: 0658150805, E-mail: [email protected] Abstract Leprosy or Hansen's disease is an infection by Mycobac- terium leprae (M. leprae), whose prevalence has consid- erably decreased since the application of the new anti-lep- rosy strategies advocated since 1982 by the World Health Organization (WHO). However, in the endemic countries several cases of leprosy are reported annually. We report a clinical case of lepromatous leprosy revealed by dissemi- nated maculopapular lesions simulating a Sweet syndrome highlighting the importance of knowing how to evoke this diagnosis in patients from endemic areas. Keywords Lepromatous leprosy, Rash, Sweet syndrome Introduction Lepromatous leprosy is generally manifested by Figure 1: a) Maculopapular erythematous lesions of the non-inflammatory lesions, hypochromic macules, and face; b) Papulonodular erythematous lesions in forearms progressive erythematous papulo-nodules. We report and hands. an observation of lepromatous leprosy in a 62-year-old patient from rural Morocco who was diagnosed with abdomen (Figure 2a and Figure 2b). The neurological maculopapular lesions. examination showed hypoesthesia in gloves and socks, with bilateral hypertrophy of the ulnar nerve. -
Lepromatous Leprosy with Erythema Nodosum Leprosum Presenting As
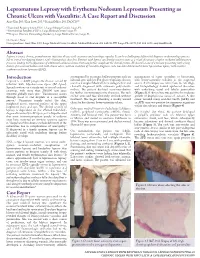
Lepromatous Leprosy with Erythema Nodosum Leprosum Presenting as Chronic Ulcers with Vasculitis: A Case Report and Discussion Anny Xiao, DO,* Erin Lowe, DO,** Richard Miller, DO, FAOCD*** *Traditional Rotating Intern, PGY-1, Largo Medical Center, Largo, FL **Dermatology Resident, PGY-2, Largo Medical Center, Largo, FL ***Program Director, Dermatology Residency, Largo Medical Center, Largo, FL Disclosures: None Correspondence: Anny Xiao, DO; Largo Medical Center, Graduate Medical Education, 201 14th St. SW, Largo, FL 33770; 510-684-4190; [email protected] Abstract Leprosy is a rare, chronic, granulomatous infectious disease with cutaneous and neurologic sequelae. It can be a challenging differential diagnosis in dermatology practice due to several overlapping features with rheumatologic disorders. Patients with leprosy can develop reactive states as a result of immune complex-mediated inflammatory processes, leading to the appearance of additional cutaneous lesions that may further complicate the clinical picture. We describe a case of a woman presenting with a long history of a recurrent bullous rash with chronic ulcers, with an evolution of vasculitic diagnoses, who was later determined to have lepromatous leprosy with reactive erythema nodosum leprosum (ENL). Introduction accompanied by an intense bullous purpuric rash on management of sepsis secondary to bacteremia, Leprosy is a slowly progressive disease caused by bilateral arms and face. For these complaints she was with lower-extremity cellulitis as the suspected infection with Mycobacterium leprae (M. leprae). seen in a Complex Medical Dermatology Clinic and source. A skin biopsy was taken from the left thigh, Spread continues at a steady rate in several endemic clinically diagnosed with cutaneous polyarteritis and histopathology showed epidermal ulceration countries, with more than 200,000 new cases nodosa. -

WO 2014/134709 Al 12 September 2014 (12.09.2014) P O P C T
(12) INTERNATIONAL APPLICATION PUBLISHED UNDER THE PATENT COOPERATION TREATY (PCT) (19) World Intellectual Property Organization International Bureau (10) International Publication Number (43) International Publication Date WO 2014/134709 Al 12 September 2014 (12.09.2014) P O P C T (51) International Patent Classification: (81) Designated States (unless otherwise indicated, for every A61K 31/05 (2006.01) A61P 31/02 (2006.01) kind of national protection available): AE, AG, AL, AM, AO, AT, AU, AZ, BA, BB, BG, BH, BN, BR, BW, BY, (21) International Application Number: BZ, CA, CH, CL, CN, CO, CR, CU, CZ, DE, DK, DM, PCT/CA20 14/000 174 DO, DZ, EC, EE, EG, ES, FI, GB, GD, GE, GH, GM, GT, (22) International Filing Date: HN, HR, HU, ID, IL, IN, IR, IS, JP, KE, KG, KN, KP, KR, 4 March 2014 (04.03.2014) KZ, LA, LC, LK, LR, LS, LT, LU, LY, MA, MD, ME, MG, MK, MN, MW, MX, MY, MZ, NA, NG, NI, NO, NZ, (25) Filing Language: English OM, PA, PE, PG, PH, PL, PT, QA, RO, RS, RU, RW, SA, (26) Publication Language: English SC, SD, SE, SG, SK, SL, SM, ST, SV, SY, TH, TJ, TM, TN, TR, TT, TZ, UA, UG, US, UZ, VC, VN, ZA, ZM, (30) Priority Data: ZW. 13/790,91 1 8 March 2013 (08.03.2013) US (84) Designated States (unless otherwise indicated, for every (71) Applicant: LABORATOIRE M2 [CA/CA]; 4005-A, rue kind of regional protection available): ARIPO (BW, GH, de la Garlock, Sherbrooke, Quebec J1L 1W9 (CA). GM, KE, LR, LS, MW, MZ, NA, RW, SD, SL, SZ, TZ, UG, ZM, ZW), Eurasian (AM, AZ, BY, KG, KZ, RU, TJ, (72) Inventors: LEMIRE, Gaetan; 6505, rue de la fougere, TM), European (AL, AT, BE, BG, CH, CY, CZ, DE, DK, Sherbrooke, Quebec JIN 3W3 (CA). -

Leprosy' Revi"Ew
LEPROSY' REVI"EW lbe QD8rterIy Publication of THE BRITISH LEPROSY RELIEF ASSOCIAll0N VOL. XXVIII. No 3. JULY 1957 Principal Contents EditoriaIs Secondary Infections and Neoplasms in Leprosy Patients. Leprosy of the Eye. Thiosemicarbazone in the Treatment of the Reactional and Bordeline Forms of Leprosy. Some Data on the Influence of B.C.G. Vaccination in Leprosy Patients. Abstracts 8 PORTMAN STREET, LONDON, W.l Price: Three Shillings and Sixpence, plus posfage Annual Subscripfion: Fiffeen Shillings, including posfage LEPROSY REVIEW VOL. XXVIII, No. 3. JULY, 1957 CONTENTS PAGE Editorials: Corticosteroids in Leprosy 91 Is there a place for hypnotherapy in leprosy treatment? 92 Secondary Infections and Neoplasms in Leprosy Patients FELIX CONTRERAS 95 Leprosy of the Eye .. W. ]. HOLMES 108 Thiosemicarbazone in the Treatment of the Reactional and Borderline Forms of Leprosy H. W. WHEATE 124 Some Data on the Influence of BCG Vaccination in Leprosy Patients ]. VAN DE HEYNING 130 Abstracts 131 Edited by DR. J. Ross INNES, Medical Secretary of the British Leprosy Relief Association, 8 Portman Street, London, W.l, to whom all communications should be sent. The Association does not accept responsibilty for views expressed by writers. Contributors of original articles will receive 25 loose reprints free, but more formal bound reprints must be ordered at time of submitting the article, and the cost reimbursed later. THE ONE DOSE REMEDY , ANTEPAR ' is such a simple and practical ascarifuge, it enables you to tackle tbe roundworm problem on a large scale. You simply givc each adult or child onc dosc of 'A TEPAR' }!'Iixir. 0 purging, fasting or dieling is necessary. -

Leprosy in Two Patients with Relapsing Remitting Multiple Sclerosis Treated with Fingolimod Alfred Balasa, M.D.1 and George J
Leprosy in Two Patients with Relapsing Remitting Multiple Sclerosis Treated with Fingolimod Alfred Balasa, M.D.1 and George J. Hutton, M.D.2 1 Department of Pediatrics, Section of Pediatric Neurology and Developmental Neuroscience; 2 Department of Neurology; Baylor College of Medicine, Houston, Texas Background A B Leprosy (Hansen’s disease) is a chronic infection caused by Mycobacterium leprae. The disease develops over months to years and may cause extensive damage to the skin and peripheral nervous system. A B In multiple sclerosis (MS), fingolimod treatment is Figure 3. Immune response in the polar clinical forms of leprosy. known to increase the risk for infections. There is one prior reported case of leprosy while on [A] In tuberculoid leprosy (TT) patients, the innate immune response is activated by M. leprae through toll-like receptors (TLR2/1). IL-15 fingolimod for relapsing remitting multiple sclerosis stimulates the vitamin D-dependent antimicrobial program in macrophages and inhibits phagocytosis of mycobacteria. These events (RRMS). We report two further cases of leprosy in promote a Th1 T-cell cytokine response (IFN-γ, IL-2, TNF, and IL-15) that contains the infection in well-formed granulomas, and a Th17 patients with RRMS and treated with fingolimod. C D response (IL-17A, IL-17F, IL-21 and IL-22) that leads to tissue inflammation and destruction, neutrophil recruitment, macrophage activation, and enhancement of Th1 effector cells. [B] In lepromatous leprosy (LL) patients, IL-4, IL-10, leukocyte immunoglobulin-like receptor subfamily A member 2 (LILRA2), and oxidized phospholipids inhibit TLR2/1-induced cytokine responses but preserve IL-10 release. -

Bacterial Skin Infections
BACTERIAL SKIN INFECTIONS SPEAKER: DR LUIZ ALBERTO BOMJARDIM PÔRTO DERMATOLOGIST BRAZIL MRSA INFECTIONS • Concept: Methicillin- resistant Staphylococcus aureus • Epidemiology: Gradual increase of resistance. • Nosocomial MRSA risk factors: Hospitalization, ICU, invasive procedures, previous antibiotic therapy, health professionals, diabetes mellitus, EV drugs, immunosuppression and chronic diseases. MRSA INFECTIONS • Community MARSA risk factors: Children, EV drugs, indigenous, homosexual men, military, prisoners and athletes. • Microorganisms more virulent by genetic characteristics. MRSA INFECTIONS • Clinic caracteristics: -Abscess, cellulitis, folliculitis, impetigo, infected wounds, external otitis, paronychia and colonization of the skin in cases of atopic dermatitis. - Increased morbidity. • Propedeutics: Culture blood, tissue or secretion. MRSA INFECTIONS • Treatment: - Pathology-specific treatment. - Prefer non-beta-lactam antibiotics, such as: clindamycin, sulfamethoxazole- trimethoprim and tetracyclines. - On suspicion of MARSA infection, start empirical antibiotics and stagger specific antibiotics by culture with antibiograma. MRSA INFECTIONS • Treatment: - Decolonization: systemic antibiotic therapy, topical 2% mupirocin, personal hygiene with antiseptic or antimicrobial solutions (iodine-povidine, chlorhexidine or triclosan). MRSA INFECTIONS • Prevention: - Avoid skin-to-skin contact and share personal belongings / clothing. - Hand washing. - Use of alcohol gels. - Cover wounds. - Isolation contact of MARSA carriers. - Early