6/12/2018 1 Infectious Dermatopathology
Total Page:16
File Type:pdf, Size:1020Kb
Load more
Recommended publications
-

(ERYTHEMA NODOSUM LEPROSUM) the Term
? THE HISTOPATHOLOGY OF ACUTE PANNICULITIS NODOSA LEPROSA (ERYTHEMA NODOSUM LEPROSUM) w. J. PEPLER, M.B., Ch.B. Department of Pathology, South African Institute for Medical Research, Johannesburg R. KOOIJ, M.D. Westfort Institution, Pretoria AND J. MARSHALL, M.D. University of Pretoria, Pretoria The term "erythema nodosum leprosum" has frequently appeared in the literature on leprosy since the 1930's, apparently popularized by the Japanese (9). The occurrence of "erythema nodosum" in leprosy had previously been noted at the end of the nineteenth century by Brocq (6) and by Hansen and Looft (8), but the term seems to have fallen into disuse. As will become clear from our clinical and histological descriptions of the phenomenon commonly known as erythema nodosum leprosum, we believe the title to be a misnomer. We suggest that it would be more accurate to call it panniculitis nodosa leprosa (P.N.L,). This condition is commonly confused with acute lepra reaction, both processes being referred to as "acute reactions"; but a sharp line of distinction must be drawn between them. P.N.L. occurs only in patients with lepromatous leprosy as an acute, subacute or chronic skin eruption, with or without fever. It is characterized by showers of dusky red nodules, 0.5 to 2 cm. in diameter, on the extensor surfaces of the limbs, on the face, and, less often, on the trunk. The number of lesions appearing in an attack varies from a few to several hundreds, and they sometimes coalesce to form plaques. The nodules may be painful, and they are usually tender to touch. -

Chapter 3 Bacterial and Viral Infections
GBB03 10/4/06 12:20 PM Page 19 Chapter 3 Bacterial and viral infections A mighty creature is the germ gain entry into the skin via minor abrasions, or fis- Though smaller than the pachyderm sures between the toes associated with tinea pedis, His customary dwelling place and leg ulcers provide a portal of entry in many Is deep within the human race cases. A frequent predisposing factor is oedema of His childish pride he often pleases the legs, and cellulitis is a common condition in By giving people strange diseases elderly people, who often suffer from leg oedema Do you, my poppet, feel infirm? of cardiac, venous or lymphatic origin. You probably contain a germ The affected area becomes red, hot and swollen (Ogden Nash, The Germ) (Fig. 3.1), and blister formation and areas of skin necrosis may occur. The patient is pyrexial and feels unwell. Rigors may occur and, in elderly Bacterial infections people, a toxic confusional state. In presumed streptococcal cellulitis, penicillin is Streptococcal infection the treatment of choice, initially given as ben- zylpenicillin intravenously. If the leg is affected, Cellulitis bed rest is an important aspect of treatment. Where Cellulitis is a bacterial infection of subcutaneous there is extensive tissue necrosis, surgical debride- tissues that, in immunologically normal individu- ment may be necessary. als, is usually caused by Streptococcus pyogenes. A particularly severe, deep form of cellulitis, in- ‘Erysipelas’ is a term applied to superficial volving fascia and muscles, is known as ‘necrotiz- streptococcal cellulitis that has a well-demarcated ing fasciitis’. This disorder achieved notoriety a few edge. -

Leprosy in Refugees and Migrants in Italy and a Literature Review of Cases Reported in Europe Between 2009 and 2018
microorganisms Article Leprosy in Refugees and Migrants in Italy and a Literature Review of Cases Reported in Europe between 2009 and 2018 Anna Beltrame 1,* , Gianfranco Barabino 2, Yiran Wei 2, Andrea Clapasson 2, Pierantonio Orza 1, Francesca Perandin 1 , Chiara Piubelli 1 , Geraldo Badona Monteiro 1, Silvia Stefania Longoni 1, Paola Rodari 1 , Silvia Duranti 1, Ronaldo Silva 1 , Veronica Andrea Fittipaldo 3 and Zeno Bisoffi 1,4 1 Department of Infectious, Tropical Diseases and Microbiology, I.R.C.C.S. Sacro Cuore Don Calabria Hospital, Via Sempreboni 5, 37024 Negrar di Valpolicella, Italy; [email protected] (P.O.); [email protected] (F.P.); [email protected] (C.P.); [email protected] (G.B.M.); [email protected] (S.S.L.); [email protected] (P.R.); [email protected] (S.D.); [email protected] (R.S.); zeno.bisoffi@sacrocuore.it (Z.B.) 2 Dermatological Clinic, National Reference Center for Hansen’s Disease, Ospedale Policlinico San Martino, Sistema Sanitario Regione Liguria, Istituto di Ricovero e Cura a Carattere Scientifico per l’Oncologia, Largo Rosanna Benzi 10, 16132 Genoa, Italy; [email protected] (G.B.); [email protected] (Y.W.); [email protected] (A.C.) 3 Oncology Department, Mario Negri Institute for Pharmacological Research I.R.C.C.S., Via Giuseppe La Masa 19, 20156 Milano, Italy; vafi[email protected] 4 Department of Diagnostic and Public Health, University of Verona, P.le L. A. Scuro 10, 37134 Verona, Italy * Correspondence: [email protected]; Tel.: +39-045-601-4748 Received: 30 June 2020; Accepted: 23 July 2020; Published: 24 July 2020 Abstract: Leprosy is a chronic neglected infectious disease that affects over 200,000 people each year and causes disabilities in more than four million people in Asia, Africa, and Latin America. -

A Rare Case of Coexistence of Borderline Lepromatous Leprosy with Tuberculosis Verrucosa Cutis
Hindawi Publishing Corporation Case Reports in Infectious Diseases Volume 2016, Article ID 1746896, 4 pages http://dx.doi.org/10.1155/2016/1746896 Case Report A Rare Case of Coexistence of Borderline Lepromatous Leprosy with Tuberculosis Verrucosa Cutis Biswajit Dey,1 Debasis Gochhait,1 Nagendran Prabhakaran,2 Laxmisha Chandrashekar,2 and Biswanath Behera2 1 Department of Pathology, Jawaharlal Institute of Postgraduate Medical Education and Research (JIPMER), Pondicherry, India 2Department of Dermatology, Jawaharlal Institute of Postgraduate Medical Education and Research (JIPMER), Pondicherry, India Correspondence should be addressed to Debasis Gochhait; [email protected] Received 13 July 2016; Revised 23 October 2016; Accepted 31 October 2016 Academic Editor: Sinesio´ Talhari Copyright © 2016 Biswajit Dey et al. This is an open access article distributed under the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original work is properly cited. Occurrence of pulmonary tuberculosis with leprosy is known but association of cutaneous tuberculosis with leprosy is rare. We report a case of borderline lepromatous leprosy coexistent with tuberculosis verrucosa cutis in a 29-year-old male, who presented with multiple skin coloured nodules and hyperkeratotic scaly lesions of 3-month duration. Dual infections are associated with high mortality and morbidity. Therefore early diagnosis and management helps to reduce mortality and to mitigate the effects of morbidity. 1. Introduction or motor weakness. The patient denied any drug intake, fever, myalgia, spontaneous blistering or ulceration, neuritic Mycobacterium leprae is the causative agent of leprosy that pain, and testicular pain. None of the family members or affects the skin and peripheral nerves. -

Post-Traumatic Inoculation Tuberculoid Leprosy After Injury with a Glass Bangle
Lepr Rev (2009) 80, 215–218 CASE REPORT Post-traumatic inoculation tuberculoid leprosy after injury with a glass bangle ASHOK GHORPADE Department of Dermatology, Venereology & Leprosy, JLN Hospital & Research Centre, Bhilai Steel Plant, Bhilai, Chhattisgarh state, India Accepted for publication 27 March 2009 Summary A lesion of tuberculoid leprosy in an Indian lady presenting at the site of injury from a broken glass bangle is reported. The diagnosis was by classical clinical features and histopathology. The importance of the skin in leprosy transmission is emphasised. Case Report A 44 year-old Indian woman presented with a 2 month history of a skin lesion on her right hand. She was a coordinator in a school for slum children in this highly endemic region for 22 years. The lesion had started exactly over a site of an injury with her glass bangle, sustained about 2 years earlier. There was no family history of skin problems, or of any local or oral medication. Cutaneous examination showed a single, circular, raised, uniformly infiltrated, erythematous plaque around 3 cms in diameter, anaesthetic to temperature, touch and pain on the medial aspect of her right hand, near the wrist joint (Figure 1a). There was no other skin lesion and systemic examination was normal. Histopathological examination revealed multiple compact non-caseating granulomas of lymphocytes, epitheloid cells and Langhans’ giant cells in the upper dermis almost touching the normal epidermis from below, with a similar infiltrate invading a nerve in deeper dermis (Figure 2). Ziehl-Neelsen stain from the section and the slit smear examination from the lesion did not reveal any acid-fast bacilli. -
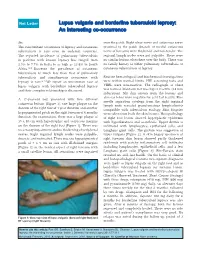
Lupus Vulgaris and Borderline Tuberculoid Leprosy: an Interesting Co-Occurrence
Net Letter Lupus vulgaris and borderline tuberculoid leprosy: An interesting co-occurrence Sir, over the patch. Right ulnar nerve and cutaneous nerve The concomitant occurrence of leprosy and cutaneous proximal to the patch (branch of medial cutaneous tuberculosis is rare even in endemic countries. nerve of forearm) were thickened and non-tender. The The reported incidence of pulmonary tuberculosis regional lymph nodes were not palpable. There were in patients with known leprosy has ranged from no similar lesions elsewhere over the body. There was 2.5% to 7.7% in India to as high as 13.4% in South no family history of either pulmonary tuberculosis or Africa.[1-3] However the prevalence of cutaneous cutaneous tuberculosis or leprosy. tuberculosis is much less than that of pulmonary tuberculosis and simultaneous occurrence with Routine hematological and biochemical investigations leprosy is rare.[4-7] We report an uncommon case of were within normal limits. HIV screening tests and lupus vulgaris with borderline tuberculoid leprosy VDRL were non-reactive. The radiograph of chest and their complex relationship is discussed. was normal. Mantoux test was hyper-reactive (18 mm induration). Slit skin smears from the lesions and also ear lobes were negative for acid fast bacilli. Fine A 17-year-old boy presented with two different needle aspiration cytology from the right inguinal cutaneous lesions [Figure 1], one large plaque on the lymph node revealed granulomatous lymphadenitis dorsum of the right foot of 1 year duration and another compatible with tuberculous etiology. Skin biopsies hypopigmented patch on the right forearm of 6 months were taken from both the skin lesions. -

Military Dermatology, Chapter 14, Leprosy
Leprosy Chapter 14 LEPROSY JAMES W. STEGER, M.D.* AND TERRY L. BARRETT, M.D.† INTRODUCTION HISTORY Leprosy in Antiquity Leprosy in Medieval and Renaissance Europe Modern Advances in the Study of Leprosy Leprosy in the U.S. Military EPIDEMIOLOGY MICROBIOLOGY Natural Reservoirs and Laboratory Transmission The Cell Wall Molecular Biology and Genetics IMMUNOLOGY Humoral Immunity Cell-Mediated Immunity The Lepromin Test LABORATORY DIAGNOSIS The Slit-Skin Examination Technique Bacterial Index Morphologic Index Cutaneous Nerve Biopsy Serologic Assays CLINICAL AND HISTOLOGICAL DIAGNOSTIC CRITERIA TREATMENT Paucibacillary Leprosy Multibacillary Leprosy The Most Potent Antileprosy Drugs Drug Resistance Microbial Persistence Promising New Drugs COMPLICATIONS: THE REACTIONAL STATES Reversal Reaction Erythema Nodosum Leprosum Downgrading Reaction Lucio’s Phenomenon VACCINATION LEPROSY AND ACQUIRED IMMUNODEFICIENCY SYNDROME SUMMARY *Captain, Medical Corps, U.S. Navy; Head, Dermatology Clinic, Naval Hospital, San Diego, California 92134-5000 †Captain, Medical Corps, U.S. Navy; Pathology and Dermatopathology Consultant, Naval Hospital, San Diego, California 92134-5000 319 Military Dermatology INTRODUCTION Leprosy (also called Hansen’s disease) is an in- one form to the next. These transitional forms arise fectious disease caused by Mycobacterium leprae that through fluctuations in the host’s immune system. affects principally the skin, the peripheral nervous Transitions from a higher to a lower immune status system, and certain other organs. Depending on are reactional states known as downgrading reac- their immune status, patients with leprosy may tions, the converse as reversal reactions. Both types present with a wide range of cutaneous and neu- of reactional states complicate therapy. An infected rological signs and symptoms. These signs and patient whose clinical presentation (usually a symptoms have been grouped together to delineate hypopigmented patch) is not diagnostic is said to leprosy into a spectrum of clinical forms or stages have indeterminate leprosy. -

Hodgkins Lymphoma: a Case Diagnosed by Pathology Section Fine Needle Aspiration Cytology
Case Report Lepromatous Lymphadenitis Mimicking Non- Hodgkins Lymphoma: A Case Diagnosed by Pathology Section Fine Needle Aspiration Cytology PREM SINGH, DEEBA MUSHTAQ, JYOTI BALA, KALYANI KAPUR, AKSHAY RANA ABSTRACT to be a case of non-Hodgkin’s lymphoma and was taken for Objectives: To report a case of generalized lymphadenopathy in further investigations. a man, clinically suspected as non-Hodgkin’s lymphoma and to Results: Fine needle aspiration was performed on the lymph present the usefulness of FNAC as a diagnostic tool for leprosy node which established lepromatous leprosy as the cause of in patients presenting with lymphadenopathy. lymphadenopathy.This was further confirmed by lymph node Methods: A 46 year old man from Uttar Pradesh (India) with biopsy and its histopathological examination. generalized lymphadenopathy. Initially diagnosed as tuber- Conclusion: The standard tools for diagnosis of leprosy are cular lymphadenitis, he was prescribed a course of anti- mainly skin slit smears or skin biopsy of the affected area of skin. tubercular treatment to which he did not respond. He was When the presentation is with lymphadenopathy, then FNAC of hence referred to our institute, where he clinically suspected the lymph node provides for an infallible tool for diagnosis. Key Words: Lepromatous lymphdenitis, Lymphoma, Non-Hodgkin`s lymphoma INTRODUCTION some were multinucleated, interspersed with reactive lymphoid Leprosy first described in ancient Indian texts from the 6th century cells and plasma cells. Few focal collections of epithelioid cells B.C. is a non fatal infectious disease caused by Mycobacterium were also seen. The foamy macrophages showed intracellular leprae whose clinical manifestations are largely confined to skin, and extracellular negative bacillary images arranged in a parallel peripheral nervous system and upper respiratory tract (1). -

Histoid Leprosy in an HIV Positive Patient Taking Cart
Lepr Rev (2010) 81, 221–223 CASE REPORT Histoid leprosy in an HIV positive patient taking cART R. A. BUMB, B. C. GHIYA, R. JAKHAR & N. PRASAD Department of Dermatology, Venereology and Leprosy, S P Medical College, Bikaner, Rajasthan, India Accepted for publication 09 July 2010 It is well known that HIV infected patients are more susceptible to infection with M. tuberculosis, but this is not clear for M. leprae. Only a few studies have reported this coexistence. Co-infected cases have been reported in the past in the whole spectrum of leprosy i.e. tuberculoid,1 borderline,2 and lepromatous.3,4 The deficiency of cell mediated immunity in leprosy is specific to M. leprae antigen and probably, the reason why the clinical course of leprosy is not influenced by HIV infection.5 When HIV positive patients are treated with highly active anti-retroviral treatment (cART) there is treatment-induced recovery of the immune system of the host which may lead to immune reconstitution inflammatory syndrome (IRIS). Various authors have reported tuberculoid leprosy6,7 and Type I lepra reaction8 as a manifestation of IRIS in HIV positive patients. We are reporting an HIV positive patient who developed histoid leprosy in spite of taking cART for 9 months, without any signs and symptoms of IRIS. Case report: A 42 year old married, male truck driver, presented with genital ulcers to the Department of Dermatology, SP Medical College, Bikaner. He gave a history of multiple unprotected acts of sexual intercourse with many roadside prostitutes in different parts of the country for many years. -

MYCOBACTERIUM Mycobacteria - in General • Aerobic Rods
MYCOBACTERIUM Mycobacteria - in general • Aerobic rods • Special cell wall composition (rich in lipids) – no Gram staining – hydrophobic cell surface very resistant! • Very slow growth! – generation time: 12-24 hrs (versus E. coli: 30 mins) – colony formation: up to 8 weeks !! (M. leprae can not be cultured at all) Cell wall structure of Mycobacteria VERY RICH IN LIPIDS !! Mycobacterial cell wall structure. The components include the (A) plasma membrane, (B) peptidoglycans, (C) arabinogalactan, (D) mannose-capped lipoarabinomannan, (E) plasma- associated and cell wall-associated proteins, (F) mycolic acids, and (G) glycolipid surface molecules associated with the mycolic acids. (Redrawn from Karakousis et al: Cell Microbiol 6:105-116, 2004.) Mycobacteria - I obligate pathogens • Tuberculosis (tb) – M. tuberculosis – M. bovis – M. africanum • Leprosy – M. leprae Mycobacteria - II Atypical Mycobacteria • facultative pathogens or apathogens • disease = “mycobacteriosis” M. kansasii M. avium-intracellulare M. ulcerans M. marinum M. scrofulaceum M. fortuitum-chelonei M. smegmatis Mycobacterium tuberculosis IncidenceTBC incidencia of TB in Magyarországon Hungary (újonnan(newly registered regisztrált, cases, aktív active betegek) patients) 50000 45000 40000 35000 30000 25000 20000 15000 10000 5000 0 1950 1955 1960 1965 1970 1980 1985 1990 1995 2000 2005 TB incidence since 1990 5000 4000 20%ooo 3000 2000 No. of cases of No. 1000 0 év Tuberculosis surveillance programme Korányi Bulletin, 2013. 1. szám (2012) Pathogenesis • Entry: aerosol -

Lymph Nodes in Leprosy' K
LYMPH NODES IN LEPROSY' K. D. SHARMA, M.B., B.S. (Cal.), M.Sc.Path. R eader in Pathology and Bacteriology Medical College, Jabalpur AND J. B. SHRIVASTAV, M.D. (Born.), D.B. (Lond.) Professor of Pathology and Bacteriology Nagpur Medical College, India The involvement of lymph nodes in leprosy is said to have been recorded by Gadesden in the 15th century (8) , and has been included as a feature in all modern textbooks dealing with leprosy. Klingmtiller (14), Basombrio (2), Schujman and Vaccaro (24) and Furniss (1) have described the gross and microscopic appearances of the lymph nodes in leprosy. Leprologists are unanimous that the lymph nodes are invariably involved in lepromatous leprosy, but there is disagreement about the finer histologic details; and there have been differences of findings in tuberculoid leprosy. The present investigation was undertaken to study in detail the structural alterations produced in lymph nodes in lepromatous leprosy, and also to see if the nodes are at all affected in tuberculoid leprosy, and if so to what extent. MATERIALS AND METHODS One hundred and fifty-five leprosy patients were examined clinically for enlarge ment of lymph nodes. Ninety-five of these patients showed enlargement of one or several groups of nodes, and of them 40 consented to lymph-node biopsy. Of these 40 patients, 24 had lepromatous leprosy (2 of them mixed) and 16 were tuberculoid. The nodes were removed from various regions: 31 were supratrochlear, 5 were inguinal, and 4 were cervical. The excised glands were examined in gross and then bisected. One-half of each was preserved in formalin-saline for histologic study, after making a smear for Ziehl-Neelsen staining. -

An Epidemiologist's View of Leprosy KENNETH W
Bull. Org. mond. Santg 1966, 34, 827-857 Bull. Wld Hlth Org. , An Epidemiologist's View of Leprosy KENNETH W. NEWELL1 While leprosy has been studied exhaustively by leprologists, it is only recently that persons in other disciplines have given this disease the attention it deserves. Various methods for its prevention and control are now being advocated and tested in thefield, and it appears reasonable for an epidemiologist to review the bases of current theories and to examine the evidence for existing hypotheses. This has been done by a review ofsome of the more recent literature. The conclusion is reached that the anergic, or factor N, hypothesis that has been evolved to relate the lepromin test to the findings in clinical leprosy appears to be the most promising, and that, if this hypothesis can be substantiated, it is unlikely that BCG vaccination can be a very useful tool for prevention. Many possibilities exist for epidemiological and laboratory research into this disease, which in many ways appears to be unique. INTRODUCTION theories on the subject. This has resulted in some emphasis and omissions that are hard to justify. Not only were leprosy patients walled up or Some basic observations well known to leprologists segregated in the past, but it would be fair to say that have been omitted; this could lead to difficulties in the leprologists and the subject of leprosy were also understanding by people who are unfamiliar with the cut off from the main body of medical thought and subject. Other apparently simple points have been research. Many pleas have been made, generally in described in detail, and this could be thought of as specialist publications read only by leprologists, for undignified and as " padding " by the leprosy expert.