Hormone: Any Substance Produced and Secreted by One Cell That Regulates Another Cell
Total Page:16
File Type:pdf, Size:1020Kb
Load more
Recommended publications
-

Effects of Streptozotocin-Induced Diabetes on the Pineal Gland in the Domestic Pig
International Journal of Molecular Sciences Article Effects of Streptozotocin-Induced Diabetes on the Pineal Gland in the Domestic Pig Bogdan Lewczuk 1,* , Magdalena Prusik 1 , Natalia Ziółkowska 1, Michał D ˛abrowski 2, Kamila Martniuk 1, Maria Hanuszewska 1 and Łukasz Zielonka 2 1 Department of Histology and Embryology, Faculty of Veterinary Medicine, University of Warmia and Mazury in Olsztyn, Oczapowskiego 13, 10-719 Olsztyn, Poland; [email protected] (M.P.); [email protected] (N.Z.); [email protected] (K.M.); [email protected] (M.H.) 2 Department of Veterinary Prevention and Feed Hygiene, Faculty of Veterinary Medicine, University of Warmia and Mazury in Olsztyn, Oczapowskiego 13, 10-719 Olsztyn, Poland; [email protected] (M.D.); [email protected] (Ł.Z.) * Correspondence: [email protected]; Tel.: +48-89-523-39-49; Fax: +48-89-523-34-40 Received: 15 July 2018; Accepted: 5 October 2018; Published: 9 October 2018 Abstract: Several observations from experiments in rodents and human patients suggest that diabetes affects pineal gland function, including melatonin secretion; however, the accumulated data are not consistent. The aim of the present study was to determine the effects of streptozotocin-induced diabetes on the pineal gland in the domestic pig, a species widely used as a model in various biomedical studies. The study was performed on 10 juvenile pigs, which were divided into two groups: control and diabetic. Diabetes was evoked by administration of streptozotocin (150 mg/kg of body weight). After six weeks, the animals were euthanized between 12.00 and 14.00, and the pineal glands were removed and divided into two equal parts, which were used for biochemical analyses and for preparation of explants for the superfusion culture. -

Expression Pattern of Delta-Like 1 Homolog in Developing Sympathetic Neurons and Chromaffin Cells
Published in "Gene Expression Patterns 30: 49–54, 2018" which should be cited to refer to this work. Expression pattern of delta-like 1 homolog in developing sympathetic neurons and chromaffin cells ∗ Tehani El Faitwria,b, Katrin Hubera,c, a Institute of Anatomy & Cell Biology, Albert-Ludwigs-University Freiburg, Albert-Str. 17, 79104, Freiburg, Germany b Department of Histology and Anatomy, Faculty of Medicine, Benghazi University, Benghazi, Libya c Department of Medicine, University of Fribourg, Route Albert-Gockel 1, 1700, Fribourg, Switzerland ABSTRACT Keywords: Delta-like 1 homolog (DLK1) is a member of the epidermal growth factor (EGF)-like family and an atypical notch Sympathetic neurons ligand that is widely expressed during early mammalian development with putative functions in the regulation Chromaffin cells of cell differentiation and proliferation. During later stages of development, DLK1 is downregulated and becomes DLK1 increasingly restricted to specific cell types, including several types of endocrine cells. DLK1 has been linked to Adrenal gland various tumors and associated with tumor stem cell features. Sympathoadrenal precursors are neural crest de- Organ of Zuckerkandl rived cells that give rise to either sympathetic neurons of the autonomic nervous system or the endocrine Development ffi Neural crest chroma n cells located in the adrenal medulla or extraadrenal positions. As these cells are the putative cellular Phox2B origin of neuroblastoma, one of the most common malignant tumors in early childhood, their molecular char- acterization is of high clinical importance. In this study we have examined the precise spatiotemporal expression of DLK1 in developing sympathoadrenal cells. We show that DLK1 mRNA is highly expressed in early sympa- thetic neuron progenitors and that its expression depends on the presence of Phox2B. -

TEE UNIVERSITY of OKLAHOMA GRADUATE Coiiiege ' A
TEE UNIVERSITY OF OKLAHOMA GRADUATE COIIiEGE ' A COMPARATIVE HISTOLOGICAL AND HISTOCHEMICAL STUDY OF THE ADRENAL GLANDS OF NATIVE RABBITS A THESIS SUBMITTED TO THE GRADUATE FACULTY ±n partial fiolflllment of the requirements for the degree of DOCTOR OF PHILOSOPHY BY I. ERNEST GONZALEZ Oklahoma City, Oklahoma 1955 A COMPARATIVE HISTOLOGICAL AND HISTOCHEMICAL STUDY OF THE ADRENAL GLANDS OF NATIVE RABBITS APEROVED BY THESIS COMMIT' ACKN0WEE33GEMENT The writer wishes to express his profound appreciation and sincere thanks to Dr. Kenneth M. Richter, Department of Anatomy, University of Oklahoma Medical School, for his valuable time, coopera- I _ ition, helpful criticisms, and timely suggestions during the course of j I this investigation; to Dr. Ernest Lachman, Chairman of the Department of Anatomy, for his encouragement and cooperation; to Dr. Garman Daron, Professor of Anatomy, for his many helpful suggestions % and to the University of Oklahoma for a University scholarship. Many other persons have cooperated indirectly in making this investigation possible, and the writer would like to acknowledge also the assistance of Dr. C. Lynn Hayward and Dr. D. Eldon Beck, Depart ment of Zoology, Brigham Young University, for procuring and identify ing many of the native rabbit species; of Mr. Ernest Reiser for his advice during the preparation of the graphic models; and of Mr. Neil Woodward for his assistance with the photomicrographic reproductions. ill TABLE OF CONTENTS Page CHAPTER I 1 Introduction CHAPTER II Materials and MetHods CHAPTER III Observations .............................. 7 Ocbbtona princeps ............»...... ...... 7 Pexicapsular tissue^ capsule, and stroma 7 Vasculature . ......... ............. 8 Innervation............... .... ........ 9 Cortex ........ , . ... ........ ... .. 9 Zona glomerulosa....... ............ 9 Zona fasciculata ............. -

The Morphology, Androgenic Function, Hyperplasia, and Tumors of the Human Ovarian Hilus Cells * William H
THE MORPHOLOGY, ANDROGENIC FUNCTION, HYPERPLASIA, AND TUMORS OF THE HUMAN OVARIAN HILUS CELLS * WILLIAM H. STERNBERG, M.D. (From the Department of Pathology, School of Medicine, Tulane University of Louisiana and the Charity Hospital of Louisiana, New Orleans, La.) The hilus of the human ovary contains nests of cells morphologically identical with testicular Leydig cells, and which, in all probability, pro- duce androgens. Multiple sections through the ovarian hilus and meso- varium will reveal these small nests microscopically in at least 8o per cent of adult ovaries; probably in all adult ovaries if sufficient sections are made. Although they had been noted previously by a number of authors (Aichel,l Bucura,2 and von Winiwarter 3"4) who failed to recog- nize their significance, Berger,5-9 in 1922 and in subsequent years, pre- sented the first sound morphologic studies of the ovarian hilus cells. Nevertheless, there is comparatively little reference to these cells in the American medical literature, and they are not mentioned in stand- ard textbooks of histology, gynecologic pathology, nor in monographs on ovarian tumors (with the exception of Selye's recent "Atlas of Ovarian Tumors"10). The hilus cells are found in clusters along the length of the ovarian hilus and in the adjacent mesovarium. They are, almost without excep- tion, found in contiguity with the nonmyelinated nerves of the hilus, often in intimate relationship to the abundant vascular and lymphatic spaces in this area. Cytologically, a point for point correspondence with the testicular Leydig cells can be established in terms of nuclear and cyto- plasmic detail, lipids, lipochrome pigment, and crystalloids of Reinke. -

Thyroid Gland Parathyroid Glands
Human Physiology Course Thyroid Gland Parathyroid Glands Assoc. Prof. Mária Pallayová, MD, PhD [email protected] Department of Human Physiology, UPJŠ LF April 13, 2020 (10th week – Summer Semester 2019/2020) Hormones and Functions Thyroid gland Parathyroids Thymus Adrenal glands Endocrine pancreas Ovaries, Testes Pineal Pituitary Hypothalamus-Pituitary Axis GIT, adipose tissue, brain, heart, kidney, ... Hormones and Functions Thyroid gland Parathyroids Thymus Adrenal glands Endocrine pancreas Ovaries, Testes Pineal Pituitary Hypothalamus-Pituitary Axis GIT, adipose tissue, brain, heart, kidney, ... Lecture Outline Functional anatomy of the thyroid gland Synthesis, secretion, and metabolism of the thyroid hormones The mechanism of thyroid action Role of the thyroid hormones in development, growth, and metabolism Thyroid hormone deficiency and excess in adults Physiology of the parathyroids Functional Anatomy of the Thyroid Gland two lobes + isthmus (just below the cricoid cartilage) attached to the trachea by connective tissue A normal THGL in a healthy adult weighs about 15-20 g. Functional Anatomy of the Thyroid Gland arterial blood supply: from a superior and an inferior thyroid a., which arise from the external carotid and subclavian a., respectively. venous blood supply: a series of thyroid veins drain into the ext. jugular and innominate vv. ( a rich blood supply to the thyroid gland w/ a higher rate of blood flow per gram than even that of the kidneys). innervation: adrenergic innervation from the cervical ganglia; cholinergic innervation from the n. vagus (regulation of vasomotor function to increase the delivery of TSH, iodide, and metabolic substrates to the THGL). Functional Anatomy of the Thyroid Gland The colloid (a thick, gel-like substance) is a solution composed primarily of thyroglobulin (10-25% the high viscosity), a large protein that is a storage form of the thyroid hormones. -

I. Introduction B. Adrenal Cortex
I. Introduction Adrenal Glands • suprarenal – they sit on top of the kidneys • each is composed of 2 distinct regions: A. Adrenal Medulla - the inner region - comprises 20% of the gland - secretes epinephrine and norepinephrine - derived from ectoderm B. Adrenal Cortex 1) Zona Glomerulosa (outermost region) - produces mineralocorticoids (aldosterone) • the outer region 2) Zona Fasiculata (middle region) - produces glucocorticoids (cortisol) as well as • comprises 80% of the gland estrogens and androgens • secretes corticosteroids 3) Zona Reticularis (innermost region) • derived from mesoderm - same function as zona fasiculata DHEA – dehydroepiandrosterone • an adrenal androgen in females • responsible for growth of pubic and axillary hair C. Pathologies Associated with Adrenal II. Mineralocorticoids (Aldosterone) Androgen Hypersecretion A. Functions 1.Adrenogenital Syndrome - promotes reabsorption of Na+ and - hypersecretion of androgens or estrogens secretion of K+ from the distal portion of the a) in the adult female: nephron..primary regulator of salt balance and extracellular volume - masculinization (i.e. hirsutism) -Similar (but less important) effect on salt b) in the female embryo: transport in colon, salivary glands, and - female pseudohermaphroditism sweat glands. c) in the adult male: - no effect d) in young boys: - precocious pseudopuberty 1 II. Mineralocorticoids (Aldosterone) C. Pathologies B. Regulation of Secretion 1. Hypersecretion 1. Renin Angiotensin a. primary hyperaldosteronism - Angiotensin II stimulates aldost. secretion - Conn’s syndrome 2. Potassium - usually due to a tumor on the gland + - high levels of K induce aldost. secretion - too much secretion of gland itself 3. ACTH –no direct role b. secondary hyperaldosteronism - default in renin angiotensin system - most common in atherosclerosis of renal arteries C. Pathologies III. Glucocorticoids (Cortisol) 1. -
HYPOTHALAMUS – PITUITARY-ADRENAL AXIS Learning Objectives OVERVIEW FUNCTIONAL ANATOMY
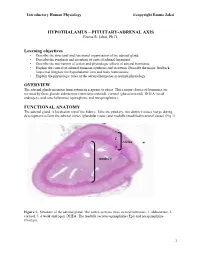
Introductory Human Physiology ©copyright Emma Jakoi HYPOTHALAMUS – PITUITARY-ADRENAL AXIS Emma R. Jakoi, Ph.D. Learning objectives • Describe the structural and functional organization of the adrenal gland. • Describe the synthesis and secretion of cortical adrenal hormones. • Describe the mechanism of action and physiologic effects of adrenal hormones. • Explain the control of adrenal hormone synthesis and secretion. Describe the major feedback loops that integrate the hypothalamic axis and body homeostasis. • Explain the physiologic roles of the adrenal hormones in normal physiology. OVERVIEW The adrenal glands maintain homeostasis in response to stress. Three major classes of hormones are secreted by these glands: aldosterone (mineralocorticoid), cortisol (glucocorticoid), DHEA (weak androgen), and catecholamines (epinephrine and norepinephrine). FUNCTIONAL ANATOMY The adrenal gland is located on top of the kidney. Like the pituitary, two distinct tissues merge during development to form the adrenal cortex (glandular tissue) and medulla (modified neuronal tissue) (Fig 1). 1 2 cortex 3 medulla Figure 1. Structure of the adrenal gland. The cortex secretes three steroid hormones: 1. aldosterone, 2. cortisol, 3. a weak androgen, DHEA. The medulla secretes epinephrine (Epi) and norepinephrine (NorEpi). 1 Introductory Human Physiology ©copyright Emma Jakoi MINERALOCORTICOIDS The major mineralocorticoid in humans is aldosterone. Aldosterone is NOT under the hypothalamus- pituitary control and does not mediate a negative feedback to this axis. Aldosterone secretion is increased by the vasoconstrictor, angiotensin II, and by elevated plasma K+ concentration. Elevated plasma Na+ inhibits the secretion of aldosterone. Aldosterone, acts in the kidney to promote secretion of K+ into the urine from the blood and the reabsorption of Na+ from the urine into the blood. -

Vocabulario De Morfoloxía, Anatomía E Citoloxía Veterinaria
Vocabulario de Morfoloxía, anatomía e citoloxía veterinaria (galego-español-inglés) Servizo de Normalización Lingüística Universidade de Santiago de Compostela COLECCIÓN VOCABULARIOS TEMÁTICOS N.º 4 SERVIZO DE NORMALIZACIÓN LINGÜÍSTICA Vocabulario de Morfoloxía, anatomía e citoloxía veterinaria (galego-español-inglés) 2008 UNIVERSIDADE DE SANTIAGO DE COMPOSTELA VOCABULARIO de morfoloxía, anatomía e citoloxía veterinaria : (galego-español- inglés) / coordinador Xusto A. Rodríguez Río, Servizo de Normalización Lingüística ; autores Matilde Lombardero Fernández ... [et al.]. – Santiago de Compostela : Universidade de Santiago de Compostela, Servizo de Publicacións e Intercambio Científico, 2008. – 369 p. ; 21 cm. – (Vocabularios temáticos ; 4). - D.L. C 2458-2008. – ISBN 978-84-9887-018-3 1.Medicina �������������������������������������������������������������������������veterinaria-Diccionarios�������������������������������������������������. 2.Galego (Lingua)-Glosarios, vocabularios, etc. políglotas. I.Lombardero Fernández, Matilde. II.Rodríguez Rio, Xusto A. coord. III. Universidade de Santiago de Compostela. Servizo de Normalización Lingüística, coord. IV.Universidade de Santiago de Compostela. Servizo de Publicacións e Intercambio Científico, ed. V.Serie. 591.4(038)=699=60=20 Coordinador Xusto A. Rodríguez Río (Área de Terminoloxía. Servizo de Normalización Lingüística. Universidade de Santiago de Compostela) Autoras/res Matilde Lombardero Fernández (doutora en Veterinaria e profesora do Departamento de Anatomía e Produción Animal. -

Gross Anatomy of the Suprarenal Glands
Edited by: Malak Shalfawi, Noor Adnan Gross Anatomy of the suprarenal glands 5/10/2020 Dr. shatarat. The University of Jordan In the sagittal section below, you can see the retroperitoneal space (encircled by a blue line), which contains structures that lie deep on the posterior abdominal wall and are called retroperitoneal structures, they are the kidneys and suprarenal (adrenal) glands. ➔ The adrenal glands are two small triangular structures located retroperitoneally at the upper poles of the kidneys. [notice the black arrow] 5/10/2020 Dr. shatarat. The University of Jordan You can again notice the kidneys (lying on the posterior abdominal wall and covered by fat), The peritoneum and retroperitoneal space. ➔ The adrenal glands are covered with a thick connective tissue capsule from which the trabeculae extend into the parenchyma carrying blood vessels and nerves. **Extra note: all soft structures in the abdomen, such as the spleen, kidneys and suprarenal glands, have hilum into which all blood vessels and nerve supply getting in or out of them. But each one of these soft structures has its specific modifications on its In this section, you can see the hilum. For example, the ureter getting vertebral column and the muscles of out from the kidneys. the posterior abdominal wall (quadratus lumborum and Psoas 5/10/2020 Dr. shatarat. The University of Jordan major) ➔ Adrenal glands are found on the posterior parietal wall, on each side of the vertebral column, at the level of the 11th thoracic rib and lateral to the first lumber vertebra. They are in the upper part of the abdomen, almost near the diaphragm, NOT in the middle and NOT inferior!!!! ➔ They have flattened triangular shape and are embedded in the perirenal fat at the superior poles of the kidneys. -

Beyond the Fixed Setpoint of the Hypothalamus–Pituitary–Thyroid Axis
E Fliers and others Hypothalamus–pituitary– 171:5 R197–R208 Review thyroid axis MECHANISMS IN ENDOCRINOLOGY Beyond the fixed setpoint of the hypothalamus–pituitary–thyroid axis Eric Fliers1, Andries Kalsbeek1,2 and Anita Boelen1 Correspondence should be addressed 1Department of Endocrinology and Metabolism, Academic Medical Center, University of Amsterdam, 1105 AZ to E Fliers Amsterdam, The Netherlands and 2Hypothalamic Integration Mechanisms, Netherlands Institute for Neuroscience, Email Amsterdam, The Netherlands e.fl[email protected] Abstract The hypothalamus–pituitary–thyroid (HPT) axis represents a classical example of an endocrine feedback loop. This review discusses dynamic changes in HPT axis setpoint regulation, identifying their molecular and cellular determinants, and speculates about their functional role. Hypothalamic thyrotropin-releasing hormone neurons were identified as key components of thyroid hormone (TH) setpoint regulation already in the 1980s, and this was followed by the demonstration of a pivotal role for the thyroid hormone receptor beta in negative feedback of TH on the hypothalamic and pituitary level. Gradually, the concept emerged of the HPT axis setpoint as a fixed entity, aiming at a particular TH serum concentration. However, TH serum concentrations appear to be variable and highly responsive to physiological and pathophysiological environmental factors, including the availability or absence of food, inflammation and clock time. During food deprivation and inflammation, TH serum concentrations decrease without a concomitant rise in serum TSH, reflecting a deviation from negative feedback regulation in the HPT axis. Surprisingly, TH action in peripheral organs in these conditions cannot be simply predicted by decreased serum TH concentrations. Instead, diverse environmental stimuli have differential effects on local TH metabolism, e.g. -

1-Anatomy of the Pituitary Gland
Color Code Important Anatomy of Pituitary Gland Doctors Notes Notes/Extra explanation Please view our Editing File before studying this lecture to check for any changes. Objectives At the end of the lecture, students should be able to: ✓ Describe the position of the pituitary gland. ✓ List the structures related to the pituitary gland. ✓ Differentiate between the lobes of the gland. ✓ Describe the blood supply of pituitary gland & the hypophyseal portal system. الغدة النخامية Pituitary Gland (also called Hypophysis Cerebri) o It is referred to as the master of endocrine glands. o It is a small oval structure 1 cm in diameter. o It doubles its size during pregnancy. lactation ,(الحمل) pregnancy ,(الحيض) A women experiences changes in her hormone levels during menstruation But only the pituitary gland will only increase in size during pregnancy .(سن اليأس) and menopause ,(الرضاعة) X-RAY SKULL: LATERAL VIEW SAGITTAL SECTION OF HEAD & NECK Extra Pituitary Gland Position o It lies in the middle cranial fossa. o It is well protected in sella turcica* (hypophyseal fossa) of body of sphenoid o It lies between optic chiasma (anteriorly) & mamillary bodies** (posteriorly). Clinical point: *سرج الحصان Anterior to the pituitary gland is the optic chiasm, so if there was a tumor in the pituitary gland or it was ** Part of hypothalamus enlarged this could press on the chiasm and disrupt the patients vision (loss of temporal field). Extra Pictures The purple part is the sphenoid bone Hypophyseal fossa Pituitary Gland The relations are important Important Relations • SUPERIOR: Diaphragma sellae: A fold of dura mater covers the pituitary gland & has an opening for passage of infundibulum (pituitary stalk) connecting the gland to hypothalamus. -

Endocrine Cell Type Sorting and Mature Architecture in the Islets Of
www.nature.com/scientificreports OPEN Endocrine cell type sorting and mature architecture in the islets of Langerhans require expression of Received: 16 April 2018 Accepted: 4 July 2018 Roundabout receptors in β cells Published: xx xx xxxx Melissa T. Adams, Jennifer M. Gilbert, Jesus Hinojosa Paiz, Faith M. Bowman & Barak Blum Pancreatic islets of Langerhans display characteristic spatial architecture of their endocrine cell types. This architecture is critical for cell-cell communication and coordinated hormone secretion. Islet architecture is disrupted in type-2 diabetes. Moreover, the generation of architecturally correct islets in vitro remains a challenge in regenerative approaches to type-1 diabetes. Although the characteristic islet architecture is well documented, the mechanisms controlling its formation remain obscure. Here, we report that correct endocrine cell type sorting and the formation of mature islet architecture require the expression of Roundabout (Robo) receptors in β cells. Mice with whole-body deletion of Robo1 and conditional deletion of Robo2 either in all endocrine cells or selectively in β cells show complete loss of endocrine cell type sorting, highlighting the importance of β cells as the primary organizer of islet architecture. Conditional deletion of Robo in mature β cells subsequent to islet formation results in a similar phenotype. Finally, we provide evidence to suggest that the loss of islet architecture in Robo KO mice is not due to β cell transdiferentiation, cell death or loss of β cell diferentiation or maturation. Te islets of Langerhans display typical, species-specifc architecture, with distinct spatial organization of their various endocrine cell types1–5. In the mouse, the core of the islet is composed mostly of insulin-secreting β cells, while glucagon-secreting α cells, somatostatin-secreting δ cells and pancreatic polypeptide-secreting PP cells are located at the islet periphery3.