WJARR-2020-0334.Pdf
Total Page:16
File Type:pdf, Size:1020Kb
Load more
Recommended publications
-
Median Rhomboid Glossitis
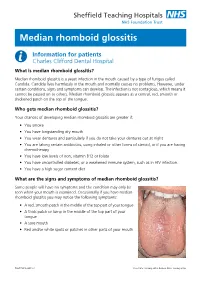
Median rhomboid glossitis Information for patients Charles Clifford Dental Hospital What is median rhomboid glossitis? Median rhomboid glossitis is a yeast infection in the mouth caused by a type of fungus called Candida. Candida lives harmlessly in the mouth and normally causes no problems. However, under certain conditions, signs and symptoms can develop. The infection is not contagious, which means it cannot be passed on to others. Median rhomboid glossitis appears as a central, red, smooth or thickened patch on the top of the tongue. Who gets median rhomboid glossitis? Your chances of developing median rhomboid glossitis are greater if: • You smoke • You have longstanding dry mouth • You wear dentures and particularly if you do not take your dentures out at night • You are taking certain antibiotics, using inhaled or other forms of steroid, or if you are having chemotherapy • You have low levels of iron, vitamin B12 or folate • You have uncontrolled diabetes, or a weakened immune system, such as in HIV infection. • You have a high sugar content diet What are the signs and symptoms of median rhomboid glossitis? Some people will have no symptoms and the condition may only be seen when your mouth is examined. Occasionally if you have median rhomboid glossitis you may notice the following symptoms: • A red, smooth patch in the middle of the top part of your tongue • A thick patch or lump in the middle of the top part of your tongue • A sore mouth • Red and/or white spots or patches in other parts of your mouth PD6779-PIL2645 v4 Issue Date: January 2019. -

Zeroing in on the Cause of Your Patient's Facial Pain
Feras Ghazal, DDS; Mohammed Ahmad, Zeroing in on the cause MD; Hussein Elrawy, DDS; Tamer Said, MD Department of Oral Health of your patient's facial pain (Drs. Ghazal and Elrawy) and Department of Family Medicine/Geriatrics (Drs. Ahmad and Said), The overlapping characteristics of facial pain can make it MetroHealth Medical Center, Cleveland, Ohio difficult to pinpoint the cause. This article, with a handy at-a-glance table, can help. [email protected] The authors reported no potential conflict of interest relevant to this article. acial pain is a common complaint: Up to 22% of adults PracticE in the United States experience orofacial pain during recommendationS F any 6-month period.1 Yet this type of pain can be dif- › Advise patients who have a ficult to diagnose due to the many structures of the face and temporomandibular mouth, pain referral patterns, and insufficient diagnostic tools. disorder that in addition to Specifically, extraoral facial pain can be the result of tem- taking their medication as poromandibular disorders, neuropathic disorders, vascular prescribed, they should limit disorders, or atypical causes, whereas facial pain stemming activities that require moving their jaw, modify their diet, from inside the mouth can have a dental or nondental cause and minimize stress; they (FIGURE). Overlapping characteristics can make it difficult to may require physical therapy distinguish these disorders. To help you to better diagnose and and therapeutic exercises. C manage facial pain, we describe the most common causes and underlying pathological processes. › Consider prescribing a tricyclic antidepressant for patients with persistent idiopathic facial pain. C Extraoral facial pain Extraoral pain refers to the pain that occurs on the face out- 2-15 Strength of recommendation (SoR) side of the oral cavity. -

Oral Lesions in Sjögren's Syndrome
Med Oral Patol Oral Cir Bucal. 2018 Jul 1;23 (4):e391-400. Oral lesions in Sjögren’s syndrome patients Journal section: Oral Medicine and Pathology doi:10.4317/medoral.22286 Publication Types: Review http://dx.doi.org/doi:10.4317/medoral.22286 Oral lesions in Sjögren’s syndrome: A systematic review Julia Serrano 1, Rosa-María López-Pintor 1, José González-Serrano 1, Mónica Fernández-Castro 2, Elisabeth Casañas 1, Gonzalo Hernández 1 1 Department of Oral Medicine and Surgery, School of Dentistry, Complutense University, Madrid, Spain 2 Rheumatology Service, Hospital Infanta Sofía, Madrid, Spain Correspondence: Departamento de Especialidades Clínicas Odontológicas Facultad de Odontología Universidad Complutense de Madrid Plaza Ramón y Cajal s/n, 28040 Madrid. Spain [email protected] Serrano J, López-Pintor RM, González-Serrano J, Fernández-Castro M, Casañas E, Hernández G. Oral lesions in Sjögren’s syndrome: A system- atic review. Med Oral Patol Oral Cir Bucal. 2018 Jul 1;23 (4):e391-400. Received: 18/11/2017 http://www.medicinaoral.com/medoralfree01/v23i4/medoralv23i4p391.pdf Accepted: 09/05/2018 Article Number: 22291 http://www.medicinaoral.com/ © Medicina Oral S. L. C.I.F. B 96689336 - pISSN 1698-4447 - eISSN: 1698-6946 eMail: [email protected] Indexed in: Science Citation Index Expanded Journal Citation Reports Index Medicus, MEDLINE, PubMed Scopus, Embase and Emcare Indice Médico Español Abstract Background: Sjögren’s syndrome (SS) is an autoimmune disease related to two common symptoms: dry mouth and eyes. Although, xerostomia and hyposialia have been frequently reported in these patients, not many studies have evaluated other oral manifestations. -

Benign Migratory Glossitis: Case Report and Literature Review
Volume 1- Issue 5 : 2017 DOI: 10.26717/BJSTR.2017.01.000482 Sarfaraz Khan. Biomed J Sci & Tech Res ISSN: 2574-1241 Case Report Open Access Benign Migratory Glossitis: Case Report and Literature Review Sarfaraz Khan1*, Syed AsifHaider Shah2, Tanveer Ahmed Mujahid3 and Muhammad Ishaq4 1Consultant Oral and Maxillofacial Surgeon, Pak Field Hospital Darfur, Sudan 2MDC Gujranwala, Pakistan 3Consultant Dermatologist, Pak Field Hospital Darfur, Sudan 4Registrar Dermatologist, Pak Field Hospital Darfur, Sudan Received: October 25, 2017; Published: October 31, 2017 *Corresponding author: Sarfaraz Khan, Consultant Oral and Maxillofacial Surgeon, Pakistan Field Hospital Darfur, Sudan, Tel: ; Email: Abstract Benign migratory Glossitis (BMG) is a benign, usually asymptomatic mucosal lesion of dorsal surface of the tongue, characterized by depapillated erythematous patches separated by white irregular borders. Etiology of BMG is unknown. Risk factors include psoriasis, fissured tongue, diabetes mellitus, hypersensitivity and psychological factors. We report BMG in an Egyptian soldier of UN peace keeping force, with stressKeywords: as a possible Geographic etiological tongue; factor Benign and migratory provide literature Glossitis; reviewErythema of this migrans disorder. Introduction Benign migratory Glossitis (BMG) is a benign, immune- spicy/salty food and/or alcoholic drinks [4,5].The lesion typically usually characterized by asymptomatic erythematous patches changes its shape with time owing to the change in pattern of mediated, chronic inflammatory lesion of unknown etiology, depapillation.Similar lesions may also be seen in atrophic candidiasis, local chemical or mechanical trauma, drug induced reactions, psoriasis with whitish margins across the surface of the tongue. This condition is also known as geographic tongue, erythema migrans, Treatment of symptomatic BMG aims at provision of symptomatic Glossitis exfoliativa and wandering rash of the tongue. -

Case Report Treatment of Geographic Tongue
Scholars Journal of Dental Sciences (SJDS) ISSN 2394-496X (Online) Sch. J. Dent. Sci., 2015; 2(7):409-413 ISSN 2394-4951 (Print) ©Scholars Academic and Scientific Publisher (An International Publisher for Academic and Scientific Resources) www.saspublisher.com Case Report Treatment of Geographic Tongue Superimposing Fissured Tongue: A literature review with case report Jalaleddin H Hamissi1, Mahsa EsFehani2, Zahra Hamissi3 1Associate Professor in periodontics and Dental Caries Prevention Research Center, Qazvin University Medical Sciences, Qazvin, Iran. 2Assistant Professor, Department of Oral Medicine & Diagnosis, college dentistry, Qazvin University Medical Sciences, Qazvin, Iran. 3Dental Student, College of Dentistry, Shahied Behesti University of Medical Sciences, Teheran, Iran *Corresponding author Dr Jalaleddin H Hamissi Email: [email protected] ; [email protected] Abstract: Tongue is a most sensitive part of the oral cavity. It is responsible for many functions in the mouth like swallowing, speech, mastication, speaking and breathing. Geographic tongue (Benign migratory glossitis, erythema migrans) is an asymptomatic inflammatory disorder of tongue with controversial etiology. This disease is characterized by erythematous areas showing raised greyish or white circinate lines or bands with irregular pattern on the dorsal surface of the tongue and depapillation. The objective in presenting the case report and literature review is to discuss the clinical presentation, associated causative factors and management strategies of geographic tongue. Keywords: Asymptomatic; Characteristics; Fissured tongue; Geographic tongue; Migratory INTRODUCTION in approximately three percent (3%) majority of female Geographic tongue is an asymptomatic population [9]. On other aspects of oral mucosa, such as inflammatory condition of the dorsum of tongue on commissure of lip, floor of mouth, cheek etc., which occasionally extending towards the lateral borders. -

Alcohol Use and Oral Health Fact Sheet for PROVIDERS OCTOBER 2017
Alcohol Use and Oral Health Fact Sheet FOR PROVIDERS OCTOBER 2017 The Challenge… Glossitis – tongue inflammation Patients who drink alcohol regularly may experience specific problems related to their oral health and hygiene. Angular cheilitis – corners of the mouth chronically inflamed and cracked What you need to know… Candida – yeast infection • Patients who drink high amounts of alcohol daily may brush Oral Ulceration – painful round or oval less effectively than those who don’t drink alcohol, despite sores reporting similar brushing frequency. Also, impaired motor Acute Necrotizing activity can affect their ability to perform basic dental hygiene adequately.1 Ulcerative Gingivitis – infection of the gums that causes ulcers, swelling, and • Alcohol is also the most common cause of sialadenosis dead tissue in the mouth of the parotid gland. This condition causes swelling of the parotid gland and decreased secretion of saliva.2 Ways You Can Help… • Poor nutrient intake and absorption combined with decreased salivary excretion frequently can lead to glossitis, Recommend: angular cheilitis, candida infection, oral ulceration, and acute • Brushing thoroughly two times daily with a necrotizing ulcerative gingivitis (ANUG).2 fluoridated toothpaste. • A decreased immune response combined with a nutritionally • Rinse mouth with non-alcoholic mouth rinse. poor diet, poor oral hygiene, decreased salivary flow, and a • Have an oral examination and cleaning by a high incidence of smoking among these patients, provides dental professional at least two times per year. an environment conducive to rapid progression of periodontal • Regular oral exams that include a periodontal disease, dental caries and increased risk of oral thoracic evaluation and oral cancer screenings to detect cancers.2 any signs of suspicious lesions.3 • High consumption of alcohol may damage the liver and bone marrow resulting in excessive bleeding during dental treatment. -

Cardiovascular Drugs-Induced Oral Toxicities: a Murky Area to Be Revisited and Illuminated
Pharmacological Research 102 (2015) 81–89 Contents lists available at ScienceDirect Pharmacological Research j ournal homepage: www.elsevier.com/locate/yphrs Review Cardiovascular drugs-induced oral toxicities: A murky area to be revisited and illuminated a, b b Pitchai Balakumar ∗, Muthu Kavitha , Suresh Nanditha a Pharmacology Unit, Faculty of Pharmacy, AIMST University, Semeling, 08100 Bedong, Malaysia b Faculty of Dentistry, AIMST University, 08100 Bedong, Malaysia a r t i c l e i n f o a b s t r a c t Article history: Oral health is an imperative part of overall human health. Oral disorders are often unreported, but are Received 20 July 2015 highly troublesome to human health in a long-standing situation. A strong association exists between Received in revised form 22 August 2015 cardiovascular drugs and oral adverse effects. Indeed, several cardiovascular drugs employed clinically Accepted 8 September 2015 have been reported to cause oral adverse effects such as xerostomia, oral lichen planus, angioedema, Available online 25 September 2015 aphthae, dysgeusia, gingival enlargement, scalded mouth syndrome, cheilitis, glossitis and so forth. Oral complications might in turn worsen the cardiovascular disease condition as some reports suggest an Keywords: adverse correlation between periodontal oral disease pathogenesis and cardiovascular disease. These are Cardiovascular drugs certainly important to be understood for a better use of cardiovascular medicines and control of associated Oral adverse effects oral adverse effects. This review sheds lights on the oral adverse effects pertaining to the clinical use of Dry mouth Angioedema cardiovascular drugs. Above and beyond, an adverse correlation between oral disease and cardiovascular Dysgeusia disease has been discussed. -
Atrophic Glossitis: Burning Agony of Nutritional Deficiency Anemia 1Neeti Swarup, 2Shreya Gupta, 3Chandrani Sagolsem, 4Zoya Chowdhary, 5Subhash Gupta, 6Nidhi Sinha
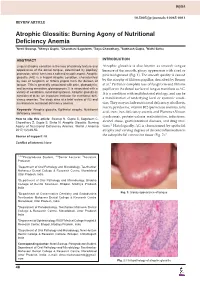
WJOA Neeti Swarup et al 10.5005/jp-journals-10065-0011 REVIEW ARTICLE Atrophic Glossitis: Burning Agony of Nutritional Deficiency Anemia 1Neeti Swarup, 2Shreya Gupta, 3Chandrani Sagolsem, 4Zoya Chowdhary, 5Subhash Gupta, 6Nidhi Sinha ABSTRACT INTRODUCTION Lingual atrophic condition is the loss of ordinary texture and Atrophic glossitis is also known as smooth tongue appearance of the dorsal tongue, determined by papillary because of the smooth, glossy appearance with a red or protrusion, which turns into a soft and smooth aspect. Atrophic pink background (Fig. 1). The smooth quality is caused glossitis (AG) is a lingual atrophic condition, characterized by loss of fungiform or filiform papilla from the dorsum of by the atrophy of filiform papillae, described by Reamy 1 tongue. This is generally associated with pain, glossodynia, et al. Partial or complete loss of fungiform and filiform and burning sensation, glossopyrosis. It is associated with a papillae on the dorsal surface of tongue manifests as AG. variety of conditions, local and systemic. Atrophic glossitis is It is a condition with multifactorial etiology, and can be considered to be an important indicator for nutritional defi- ciency anemias. The study aims at a brief review of AG and a manifestation of underlying local or systemic condi- its relation to nutritional deficiency anemia. tion. They may include nutritional deficiency, riboflavin, niacin, pyridoxine, vitamin B12 (pernicious anemia), folic Keywords: Atrophic glossitis, Epithelial atrophy, Nutritional deficiency anemia. acid, iron (iron deficiency anemia and Plummer-Vinson syndrome), protein-calorie malnutrition, infections, How to cite this article: Swarup N, Gupta S, Sagolsem C, alcohol abuse, gastrointestinal diseases, and drug reac- Chowdhary Z, Gupta S, Sinha N. -

Giant Cell Arteritis Misdiagnosed As Temporomandibular Disorder: a Case Report and Review of the Literature
360_Reiter.qxp 10/14/09 3:17 PM Page 360 Giant Cell Arteritis Misdiagnosed as Temporomandibular Disorder: A Case Report and Review of the Literature Shoshana Reiter, DMD Giant cell arteritis (GCA) is a systemic vasculitis involving medium Teacher and large-sized arteries, most commonly the extracranial branches Department of Oral Rehabilitation of the carotid artery. Early diagnosis and treatment are essential to avoid severe complications. This article reports on a GCA case Ephraim Winocur, DMD and discusses how the orofacial manifestations of GCA can lead to Lecturer misdiagnosis of GCA as temporomandibular disorder. GCA Department of Oral Rehabilitation should be included in the differential diagnosis of orofacial pain in Carole Goldsmith, DMD the elderly based on the knowledge of related signs and symptoms, Instructor mainly jaw claudication, hard end-feel limitation of range of Department of Oral Rehabilitation motion, and temporal headache. J OROFAC PAIN 2009;23:360–365 Alona Emodi-Perlman, DMD Key words: Giant cell arteritis, jaw claudication, Teacher temporomandibular disorders, trismus Department of Oral Rehabilitation Meir Gorsky, DMD Professor Department of Oral Pathology and Oral iant cell arteritis (GCA) is a systemic vasculitis involving Medicine the large and medium-sized vessels, particularly the extracranial branches of the carotid artery. It is more com- The Maurice and Gabriela Goldschleger G School of Dental Medicine mon in women (M:F ratio 2:5) and usually affects patients older 1 Tel Aviv University, Israel than 50 years with an increased risk with age. The highest preva- lence of GCA has been reported in Scandinavian populations and Correspondence to: in those with a strong Scandinavian ethnic background.2 Dr. -
Geographic Tongue
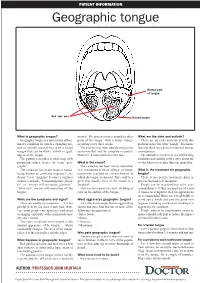
PATIENT INFORMATION Geographic tongue Normal part of tongue Red ‘raw’ area Raised border What is geographic tongue? normal. The process moves around to other What are the risks and outlook? Geographic tongue is a non-serious inflam- parts of the tongue with a major change There are no risks associated with this matory condition in which a changing pat- occurring every three weeks. problem, hence the term “benign”. It is harm- tern of smooth red patches, with a raised The process may then subside and go into less and there have been no reported serious margin that can be white, yellow or grey, remission that may be complete or partial. consequences. appear on the tongue. However, it may return at a later time. The outlook is excellent. It is a self-limiting The pattern resembles a relief map with condition and usually settles after about six mountain ridges, hence the term “geo- What is the cause? weeks. However, it may flare up again later. graphic”. The cause has not been clearly identified. The condition has many medical names, It is considered to be an allergic or hyper- What is the treatment for geographic being known as erythema migrans (“ery- sensitivity reaction to certain factors to tongue? thema” = red, “migrans” because it migrates which the tongue is exposed. This could be a There is no specific treatment, drug or or moves around), “benign migratory glossi- germ that usually lives in the mouth or a process that makes it disappear. tis” or “benign inflammatory glossitis”. foodstuff. People can be reassured not to be con- “Glossitis” means inflammation of the This reaction causes excessive shedding of cerned about it. -
On the Tip of the Tongue
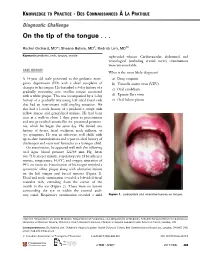
KNOWLEDGE TO PRACTICE DES CONNAISSANCES ÀLA PRATIQUE Diagnostic Challenge On the tip of the tongue . Rachel Orchard, MD*; Sheena Belisle, MD†; Rodrick Lim, MD†‡ Keywords: pediatric, rash, tongue, vesicle right-sided wheeze. Cardiovascular, abdominal, and neurological (including cranial nerve) examinations were unremarkable. CASE HISTORY What is the most likely diagnosis? A 14-year-old male presented to the pediatric emer- a) Drug eruption gency department (ED) with a chief complaint of b) Varicella zoster virus (VZV) changes to his tongue. He described a 3-day history of a c) Oral candidiasis gradually worsening sore, swollen tongue associated with a white plaque. This was accompanied by a 3-day d) Epstein-Barr virus history of a gradually worsening left-sided facial rash e) Oral lichen planus that had an intermittent mild tingling sensation. He also had a 1-week history of a productive cough with yellow mucus and generalized malaise. He had been seen at a walk-in clinic 2 days prior to presentation and was prescribed amoxicillin for presumed pneumo- nia, which he began the same day. He denied any history of fevers, facial weakness, neck stiffness, or eye symptoms. He was an otherwise well child, with up-to-date immunizations and a past medical history of chickenpox and recurrent furuncles as a younger child. On examination, he appeared well with the following vital signs: blood pressure 122/64 mm Hg, heart rate 73 beats per minute, respiratory rate 18 breaths per minute, temperature 36.8°C, and oxygen saturation of 99% on room air. Examination of his tongue revealed a symmetric white plaque along with ulcerative lesions on the left tongue and buccal mucosa (Figure 1). -

Tropical Disease Treatment Guide
HOM Disease, Symptom, and Treatment Guide Medical practice in Haiti like many developing countries is very different from practice in the United States. The lack of resources can be challenging to medical providers who are accustomed to confirming their diagnosis with labs, x-rays and other diagnostic tests. In Haiti, even when the resources are available, few people have the money to pay for labs or other tests. Diagnosis and treatment often is based primarily on history and physical. This guide is not intended to be a substitute for professional medical judgment but to help providers to arrive at an appropriate treatment for diseases that are less common in the U.S. or are diagnosed or treated differently in Haiti. As most Haitian are antibiotic naïve, and more susceptible to side effects of many medications, lower doses for shorter duration is appropriate for most acute illnesses. Anemia Dengue Fever Lymphatic Filariasis Cellulitis Epigastric Pain Malaria Chikungunya Helminths Tropical Sprue Diarrheal pathogens Ascaris lumbricoides (Roundworm) Tuberculosis (TB) Amebiasis Enterobius (Pinworm) Typhoid Fever Cholera Hookworm infections Typhus Giardiantestinalis Hepatitis A & E Vit A deficiency (VAD) Schistosomiasis Leprosy Shigellosis Leptospirosis ANEMIA Signs and Symptoms • pale conjunctiva (inner eyelid), nail beds, gums, tongue, lips, skin, • fatigue • HA • breathlessness Treatment • Adult: 150-200mg/day of elemental iron for 3 months • Pregnant women: 1 tablet of iron & folic acid every day for 6 months • Children under 6 y/o at risk of iron poisoning ANTHRAX (Colloquially known as “malcharbon” or “sick charcoal”) Human anthrax usually involves the skin (neck, face and upper extremities.) Spores enter the skin through minor cuts or abrasions.