Tropical Disease Treatment Guide
Total Page:16
File Type:pdf, Size:1020Kb
Load more
Recommended publications
-
Median Rhomboid Glossitis
Median rhomboid glossitis Information for patients Charles Clifford Dental Hospital What is median rhomboid glossitis? Median rhomboid glossitis is a yeast infection in the mouth caused by a type of fungus called Candida. Candida lives harmlessly in the mouth and normally causes no problems. However, under certain conditions, signs and symptoms can develop. The infection is not contagious, which means it cannot be passed on to others. Median rhomboid glossitis appears as a central, red, smooth or thickened patch on the top of the tongue. Who gets median rhomboid glossitis? Your chances of developing median rhomboid glossitis are greater if: • You smoke • You have longstanding dry mouth • You wear dentures and particularly if you do not take your dentures out at night • You are taking certain antibiotics, using inhaled or other forms of steroid, or if you are having chemotherapy • You have low levels of iron, vitamin B12 or folate • You have uncontrolled diabetes, or a weakened immune system, such as in HIV infection. • You have a high sugar content diet What are the signs and symptoms of median rhomboid glossitis? Some people will have no symptoms and the condition may only be seen when your mouth is examined. Occasionally if you have median rhomboid glossitis you may notice the following symptoms: • A red, smooth patch in the middle of the top part of your tongue • A thick patch or lump in the middle of the top part of your tongue • A sore mouth • Red and/or white spots or patches in other parts of your mouth PD6779-PIL2645 v4 Issue Date: January 2019. -

Zeroing in on the Cause of Your Patient's Facial Pain
Feras Ghazal, DDS; Mohammed Ahmad, Zeroing in on the cause MD; Hussein Elrawy, DDS; Tamer Said, MD Department of Oral Health of your patient's facial pain (Drs. Ghazal and Elrawy) and Department of Family Medicine/Geriatrics (Drs. Ahmad and Said), The overlapping characteristics of facial pain can make it MetroHealth Medical Center, Cleveland, Ohio difficult to pinpoint the cause. This article, with a handy at-a-glance table, can help. [email protected] The authors reported no potential conflict of interest relevant to this article. acial pain is a common complaint: Up to 22% of adults PracticE in the United States experience orofacial pain during recommendationS F any 6-month period.1 Yet this type of pain can be dif- › Advise patients who have a ficult to diagnose due to the many structures of the face and temporomandibular mouth, pain referral patterns, and insufficient diagnostic tools. disorder that in addition to Specifically, extraoral facial pain can be the result of tem- taking their medication as poromandibular disorders, neuropathic disorders, vascular prescribed, they should limit disorders, or atypical causes, whereas facial pain stemming activities that require moving their jaw, modify their diet, from inside the mouth can have a dental or nondental cause and minimize stress; they (FIGURE). Overlapping characteristics can make it difficult to may require physical therapy distinguish these disorders. To help you to better diagnose and and therapeutic exercises. C manage facial pain, we describe the most common causes and underlying pathological processes. › Consider prescribing a tricyclic antidepressant for patients with persistent idiopathic facial pain. C Extraoral facial pain Extraoral pain refers to the pain that occurs on the face out- 2-15 Strength of recommendation (SoR) side of the oral cavity. -

Alcohol Use and Oral Health Fact Sheet for PROVIDERS OCTOBER 2017
Alcohol Use and Oral Health Fact Sheet FOR PROVIDERS OCTOBER 2017 The Challenge… Glossitis – tongue inflammation Patients who drink alcohol regularly may experience specific problems related to their oral health and hygiene. Angular cheilitis – corners of the mouth chronically inflamed and cracked What you need to know… Candida – yeast infection • Patients who drink high amounts of alcohol daily may brush Oral Ulceration – painful round or oval less effectively than those who don’t drink alcohol, despite sores reporting similar brushing frequency. Also, impaired motor Acute Necrotizing activity can affect their ability to perform basic dental hygiene adequately.1 Ulcerative Gingivitis – infection of the gums that causes ulcers, swelling, and • Alcohol is also the most common cause of sialadenosis dead tissue in the mouth of the parotid gland. This condition causes swelling of the parotid gland and decreased secretion of saliva.2 Ways You Can Help… • Poor nutrient intake and absorption combined with decreased salivary excretion frequently can lead to glossitis, Recommend: angular cheilitis, candida infection, oral ulceration, and acute • Brushing thoroughly two times daily with a necrotizing ulcerative gingivitis (ANUG).2 fluoridated toothpaste. • A decreased immune response combined with a nutritionally • Rinse mouth with non-alcoholic mouth rinse. poor diet, poor oral hygiene, decreased salivary flow, and a • Have an oral examination and cleaning by a high incidence of smoking among these patients, provides dental professional at least two times per year. an environment conducive to rapid progression of periodontal • Regular oral exams that include a periodontal disease, dental caries and increased risk of oral thoracic evaluation and oral cancer screenings to detect cancers.2 any signs of suspicious lesions.3 • High consumption of alcohol may damage the liver and bone marrow resulting in excessive bleeding during dental treatment. -

Cardiovascular Drugs-Induced Oral Toxicities: a Murky Area to Be Revisited and Illuminated
Pharmacological Research 102 (2015) 81–89 Contents lists available at ScienceDirect Pharmacological Research j ournal homepage: www.elsevier.com/locate/yphrs Review Cardiovascular drugs-induced oral toxicities: A murky area to be revisited and illuminated a, b b Pitchai Balakumar ∗, Muthu Kavitha , Suresh Nanditha a Pharmacology Unit, Faculty of Pharmacy, AIMST University, Semeling, 08100 Bedong, Malaysia b Faculty of Dentistry, AIMST University, 08100 Bedong, Malaysia a r t i c l e i n f o a b s t r a c t Article history: Oral health is an imperative part of overall human health. Oral disorders are often unreported, but are Received 20 July 2015 highly troublesome to human health in a long-standing situation. A strong association exists between Received in revised form 22 August 2015 cardiovascular drugs and oral adverse effects. Indeed, several cardiovascular drugs employed clinically Accepted 8 September 2015 have been reported to cause oral adverse effects such as xerostomia, oral lichen planus, angioedema, Available online 25 September 2015 aphthae, dysgeusia, gingival enlargement, scalded mouth syndrome, cheilitis, glossitis and so forth. Oral complications might in turn worsen the cardiovascular disease condition as some reports suggest an Keywords: adverse correlation between periodontal oral disease pathogenesis and cardiovascular disease. These are Cardiovascular drugs certainly important to be understood for a better use of cardiovascular medicines and control of associated Oral adverse effects oral adverse effects. This review sheds lights on the oral adverse effects pertaining to the clinical use of Dry mouth Angioedema cardiovascular drugs. Above and beyond, an adverse correlation between oral disease and cardiovascular Dysgeusia disease has been discussed. -
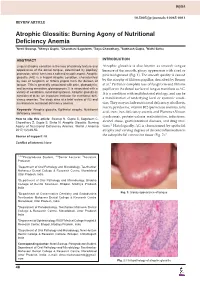
Atrophic Glossitis: Burning Agony of Nutritional Deficiency Anemia 1Neeti Swarup, 2Shreya Gupta, 3Chandrani Sagolsem, 4Zoya Chowdhary, 5Subhash Gupta, 6Nidhi Sinha
WJOA Neeti Swarup et al 10.5005/jp-journals-10065-0011 REVIEW ARTICLE Atrophic Glossitis: Burning Agony of Nutritional Deficiency Anemia 1Neeti Swarup, 2Shreya Gupta, 3Chandrani Sagolsem, 4Zoya Chowdhary, 5Subhash Gupta, 6Nidhi Sinha ABSTRACT INTRODUCTION Lingual atrophic condition is the loss of ordinary texture and Atrophic glossitis is also known as smooth tongue appearance of the dorsal tongue, determined by papillary because of the smooth, glossy appearance with a red or protrusion, which turns into a soft and smooth aspect. Atrophic pink background (Fig. 1). The smooth quality is caused glossitis (AG) is a lingual atrophic condition, characterized by loss of fungiform or filiform papilla from the dorsum of by the atrophy of filiform papillae, described by Reamy 1 tongue. This is generally associated with pain, glossodynia, et al. Partial or complete loss of fungiform and filiform and burning sensation, glossopyrosis. It is associated with a papillae on the dorsal surface of tongue manifests as AG. variety of conditions, local and systemic. Atrophic glossitis is It is a condition with multifactorial etiology, and can be considered to be an important indicator for nutritional defi- ciency anemias. The study aims at a brief review of AG and a manifestation of underlying local or systemic condi- its relation to nutritional deficiency anemia. tion. They may include nutritional deficiency, riboflavin, niacin, pyridoxine, vitamin B12 (pernicious anemia), folic Keywords: Atrophic glossitis, Epithelial atrophy, Nutritional deficiency anemia. acid, iron (iron deficiency anemia and Plummer-Vinson syndrome), protein-calorie malnutrition, infections, How to cite this article: Swarup N, Gupta S, Sagolsem C, alcohol abuse, gastrointestinal diseases, and drug reac- Chowdhary Z, Gupta S, Sinha N. -

Giant Cell Arteritis Misdiagnosed As Temporomandibular Disorder: a Case Report and Review of the Literature
360_Reiter.qxp 10/14/09 3:17 PM Page 360 Giant Cell Arteritis Misdiagnosed as Temporomandibular Disorder: A Case Report and Review of the Literature Shoshana Reiter, DMD Giant cell arteritis (GCA) is a systemic vasculitis involving medium Teacher and large-sized arteries, most commonly the extracranial branches Department of Oral Rehabilitation of the carotid artery. Early diagnosis and treatment are essential to avoid severe complications. This article reports on a GCA case Ephraim Winocur, DMD and discusses how the orofacial manifestations of GCA can lead to Lecturer misdiagnosis of GCA as temporomandibular disorder. GCA Department of Oral Rehabilitation should be included in the differential diagnosis of orofacial pain in Carole Goldsmith, DMD the elderly based on the knowledge of related signs and symptoms, Instructor mainly jaw claudication, hard end-feel limitation of range of Department of Oral Rehabilitation motion, and temporal headache. J OROFAC PAIN 2009;23:360–365 Alona Emodi-Perlman, DMD Key words: Giant cell arteritis, jaw claudication, Teacher temporomandibular disorders, trismus Department of Oral Rehabilitation Meir Gorsky, DMD Professor Department of Oral Pathology and Oral iant cell arteritis (GCA) is a systemic vasculitis involving Medicine the large and medium-sized vessels, particularly the extracranial branches of the carotid artery. It is more com- The Maurice and Gabriela Goldschleger G School of Dental Medicine mon in women (M:F ratio 2:5) and usually affects patients older 1 Tel Aviv University, Israel than 50 years with an increased risk with age. The highest preva- lence of GCA has been reported in Scandinavian populations and Correspondence to: in those with a strong Scandinavian ethnic background.2 Dr. -

1. Oral Infections.Pdf
ORAL INFECTIONS Viral infections Herpes Human Papilloma Viruses Coxsackie Paramyxoviruses Retroviruses: HIV Bacterial Infections Dental caries Periodontal disease Pharyngitis and tonsillitis Scarlet fever Tuberculosis - Mycobacterium Syphilis -Treponema pallidum Actinomycosis – Actinomyces Gonorrhea – Neisseria gonorrheae Osteomyelitis - Staphylococcus Fungal infections (Mycoses) Candida albicans Histoplasma capsulatum Coccidioides Blastomyces dermatitidis Aspergillus Zygomyces CDE (Oral Pathology and Oral Medicine) 1 ORAL INFECTIONS VIRAL INFECTIONS • Viruses consist of: • Single or double strand DNA or RNA • Protein coat (capsid) • Often with an Envelope. • Obligate intracellular parasites – enters host cell in order to replicate. • 3 most commonly encountered virus families in the oral cavity: • Herpes virus • Papovavirus (HPV) • Coxsackie virus (an Enterovirus). DNA Viruses: A. HUMAN HERPES VIRUS (HHV) GROUP: 1. HERPES SIMPLEX VIRUS • Double stranded DNA virus. • 2 types: HSV-1 and HSV-2. • Lytic to human epithelial cells and latent in neural tissue. Clinical features: • May penetrate intact mucous membrane, but requires breaks in skin. • Infects peripheral nerve, migrates to regional ganglion. • Primary infection, latency and recurrence occur. • 99% of cases are sub-clinical in childhood. • Primary herpes: Acute herpetic gingivostomatitis. • 1% of cases; severe symptoms. • Children 1 - 3 years; may occur in adults. • Incubation period 3 – 8 days. • Numerous small vesicles in various sites in mouth; vesicles rupture to form multiple small shallow punctate ulcers with red halo. • Child is ill with fever, general malaise, myalgia, headache, regional lymphadenopathy, excessive salivation, halitosis. • Self limiting; heals in 2 weeks. • Immunocompromised patients may develop a prolonged form. • Secondary herpes: Recurrent oral herpes simplex. • Presents as: a) herpes labialis (cold sores) or b) recurrent intra-oral herpes – palate or gingiva. -

Oral Signs of Systemic Disease CDA 2015 Lecture Notes
2015-08-28 Oral Signs of Oral Signs of Systemic Disease Systemic Disease Why do you need to know? ! AHA! I diagnosed your systemic disease – less likely ! Helping your patients with known Karen Burgess, DDS, MSc, FRCDC systemic diseases - more likely Oral Pathology and Oral Medicine, Faculty of Dentistry, University of Toronto Department of Dentistry, Princess Margaret Hospital Department of Dentistry, Mt Sinai Hospital 2015-08-29 2015-08-29 2015-08-29 2015-08-29 2015-08-29 2015-08-29 Normal or Abnormal? Clinical description ! Type of abnormality (shape) ! The hardest part of oral pathology ! Number ! Colour ! Consistency ! Size - measure accurately ! Surface texture ! Location 2015-08-29 2015-08-29 2015-08-29 1 2015-08-28 Vocabulary Clinical description ! Ulcer ! Type of abnormality (shape) ! Vesicle/Bulla ! Number ! Macule ! Colour ! Patch ! Consistency ! Plaque ! Size - measure accurately ! Polyp- sessile or pedunculated ! Surface texture ! Location 2015-08-29 2015-08-29 2015-08-29 Description 2015-08-29 2015-08-29 2015-08-29 Differential Diagnosis Differential Diagnosis Differential Diagnosis ! Erythema multiforme ! Mucous membrane pemphigoid ! Primary herpes ! Erythema multiforme –"Any genital or eye lesions –"How long has it been present? ! Mucous membrane pemphigoid –"Any blisters? –"Any skin lesions? ! Pemphigus vulgaris ! Pemphigus vulgaris –"any skin lesions? ! Lichen planus ! Primary herpes –"Any blisters? –"How long has it been present? ! Lichen planus What information will help you narrow down –"Any other symptoms – malaise, -

“Leukoplakia- Potentially Malignant Disorder of Oral Cavity -A Review”
DOI: 10.26717/BJSTR.2018.04.001126 Neha Aggarwal. Biomed J Sci & Tech Res ISSN: 2574-1241 Review Article Open Access “Leukoplakia- Potentially Malignant Disorder of Oral Cavity -a Review” Neha Aggarwal*1 and Sumit Bhateja2 1Department of Oral Medicine & Radiology, Manav Rachna Dental College & Hospital, Faridabad, India 2Reader Dept of Oral Medicine and Radiology, Manav Rachna Dental College, India Received: May 18, 2018; Published: May 29, 2018 *Corresponding author: Neha Aggarwal, Senior Lecturer (MDS), Department of Oral Medicine & Radiology, Manav Rachna Dental College & Hospital, Faridabad, India Abstract The term Leukoplakia simply means a “white patch”, and it has been used in a sense to describe any white lesion in the mouth. This lesions. Some investigators tried, although unsuccessfully, to restrict this term only to those white lesions that histologically indicated epithelial non-specific usage led to confusion among physician, surgeons and researchers who attributed a precancerous nature to many innocuous dysplasia. Since the mid-1960s there has been a considerable understanding and clarification in the concept of leukoplakia, and now leukoplakia isKeywords: recognized Leukoplakia; as a specific Potentially entity. malignant disorder Introduction increased risk for cancer. Leukoplakia is a clinical term and the le Leukoplakia is a greek word- Leucos means white and Plakia- - (acanthosis) and may or may not demonstrate epithelial dysplasia. ry by the Hungarian dermatologist, Schwimmer in 1877 [1,2]. WHO sion has no specific histology. It may show atrophy or hyperplasia means patch. It was first coined in the second half of the 19th centu It has a variable behavioural pattern but with an assessable tenden- (1978) [3]- A white patch or plaque that cannot be characterized cy to malignant transformation. -

TMJ Arthritis
Jemds.com Review Article TMJ Arthritis Subhashini Ramasubbu1, Shivangi Gaur2, Abdul Wahab P.U.3, Madhulaxmi Marimuthu4 1, 2, 3, 4 Department of Oral and Maxillofacial Surgery, Saveetha Dental College and Hospitals, Saveetha Institute of Medical and Technical Sciences, Saveetha University, Velappanchavadi, Chennai, Tamil Nadu, India. ABSTRACT BACKGROUND Temporomandibular Joint (TMJ) arthritis affects the joint and the surrounding Corresponding Author: musculature. Like any other joints, causes of temporomandibular joint arthritis could Dr. Subhashini Ramasubbu. Department of Oral and Maxillofacial be rheumatoid arthritis, osteo arthritis, or psoriatic arthritis. Severity of the disease Surgery, Saveetha differs from each other ranging from mild to severe. In case of temporomandibular Dental College and Hospitals, Saveetha joint trauma, it may lead to degeneration of the joint which may result in ankylosis of Institute of Medical and Technical Sciences, the joint if it is left untreated. In case of inflammatory arthropathies, even after the Saveetha University, No 162, Poonamallee treatment, inflammation of the joint still persists. To suppress the inflammation, High Road, Velappanchavadi, Chennai, patients can be prescribed immunosuppressive treatment. Long term use of Tamil Nadu, India. immunosuppressants is deleterious and may lead to failure of organs. One more E-mail: [email protected] adverse effect of immunosuppressive drugs is that it makes the patient prone for DOI: 10.14260/jemds/2020/690 infections if the patient undergoes surgery. Symptoms of temporomandibular joint arthritis include pain on involved side, restricted mouth opening, and difficulty in How to Cite This Article: eating. Origin of pain may be from the joint itself or from the muscles attached to it or Ramasubbu S, Gaur S, Abdul Wahab PU, et from both. -

Oral Submucous Fibrosis: Etiology, Pathogenesis, and Future Research R
Oral submucous fibrosis: etiology, pathogenesis, and future research R. Rajendran1 Oral submucous fibrosis (OSMF), a precancerous condition of the oral cavity, has been studied by a number of workers in the field. The available epidemiological data showed a clear-cut geographical and ethnic predisposition, which suggested that certain customs/habits prevalent among the population groups in south-east Asia might be possible etiological factors. However, none of these customs was shown to be causally linked and the association in many cases was 'casual'. This led some workers to consider the importance of systemic predisposition, in addition to the effects of local factors on the oral mucosa. More research is needed to elucidate this problem. Introduction tionship exists. The WHO definition (8) for an oral precancerous condition-a generalized pathological In 1952, Schwartz (1) described five Indian women state of the oral mucosa associated with a signifi- from Kenya with a condition of the oral mucosa cantly increased risk of cancer-accords well with including the palate and pillars of the fauces, which the characteristics of OSMF. he called "atrophia idiopathica (tropica) mucosae oris". Later it was termed oral submucous fibrosis Geographical distribution and prevalence (OSMF) (2); other names are "diffuse oral sub- mucous fibrosis", "idiopathic scleroderma of the Numerous published reports on OSMF allow an mouth", "idiopathic palatal fibrosis", "sclerosing informed appraisal of its geographical distribution stomatitis" and "juxta-epithelial fibrosis" (3). (Table 1), together with data on the percentage prev- Submucous fibrosis is an insidious, chronic dis- alence. A community-based epidemiological survey ease affecting any part of the oral cavity and some- in three areas of India (north and south) recorded the times the pharynx (4). -

Oral Non-Specific Lesions in Patient with Crohn's Disease-Case Report
Case Report ISSN: 2574 -1241 DOI: 10.26717/BJSTR.2020.25.004279 Oral Non-Specific Lesions in Patient with Crohn’s Disease-Case Report Katarzyna Szczeklik1*, Dagmara Darczuk2, Joanna Krok-Ziółkowska3, Joanna Ligara3, Mateusz Kuszaj1, Dorota Cibor4, Jolanta Pytko-Polończyk1 and Danuta Owczarek4 1Jagiellonian University Medical College, Institute of Dentistry, Department of Integrated Dentistry, Poland 2Jagiellonian University Medical College, Institute of Dentistry, Department of Periodontology and Oral Pathology, Poland 3University Dental Clinic, Poland 4Department of Gastrology and Hepatology, Jagiellonian University Medical College, Poland *Corresponding author: Katarzyna Szczeklik, Jagiellonian University Medical College, Institute of Dentistry, Department of Integrated Dentistry 4/58 Montelupich Street 31-155 Krakow, Poland ARTICLE INFO Abstract Received: February 17, 2020 Crohn’s disease together with ulcerative colitis belongs to inflammatory bowel Published: February 25, 2020 diseases. Granulomatous inflammatory process may affect all layers of the gastrointestinal wall , from the mouth to the anus, most often in the ileocecal region. The oral pathologies observed in patients with Crohn’s diseasemay be specific or non-specific, may anticipate Citation: Katarzyna Szczeklik, Dagmara the appearance of intestinal CD symptoms or occur after years of its duration. Case ofunspecific oral lesions observed in patient with Crohn’s disease is described in this article. Darczuk, Joanna Krok-Ziółkowska, Joanna Patient with Crohn’s Disease-Case Report. Keywords: Crohn’s Disease; Oral Pathology; Oral Manifestations Ligara, et al,. Oral Non-Specific Lesions in Biomed J Sci & Tech Res 25(5)-2020. BJSTR. Abbreviations: NOD2: Nucleotide-Binding Oligomerization Domain Containing 2; CRP: MS.ID.004279. C-Reactive Protein; CDAI: Crohn’s Disease Activity Index; TNF: Alfa - Tumor Necrosis Factor α Introduction sections of the altered intestinal mucosa.