Association of Increased Red Cell Distribution Width with Malignant Transformation of Oral Submucous Fibrosis
Total Page:16
File Type:pdf, Size:1020Kb
Load more
Recommended publications
-

Rebamipide to Manage Stomatopyrosis in Oral Submucous Fibrosis 1Joanna Baptist, 2Shrijana Shakya, 3Ravikiran Ongole
JCDP Rebamipide to Manage Stomatopyrosis10.5005/jp-journals-10024-1972 in Oral Submucous Fibrosis ORIGINAL RESEARCH Rebamipide to Manage Stomatopyrosis in Oral Submucous Fibrosis 1Joanna Baptist, 2Shrijana Shakya, 3Ravikiran Ongole ABSTRACT Source of support: Nil Introduction: Oral submucous fibrosis (OSF) causes progres- Conflict of interest: None sive debilitating symptoms, such as oral burning sensation (sto- matopyrosis) and limited mouth opening. The standard of care INTRODUCTION (SOC) protocol includes habit cessation, intralesional steroid and hyaluronidase injections, and mouth opening exercises. The Oral submucous fibrosis (OSF) is commonly seen in objective of the study was to evaluate efficacy of rebamipide the Indian subcontinent affecting individuals of all age in alleviating burning sensation of the oral mucosa in OSF in groups. It is a potentially malignant disorder caused comparison with SOC intralesional steroid injections. almost exclusively by the use of smokeless form of Materials and methods: Twenty OSF patients were divided into tobacco products. The malignant transformation rates two groups [rebamipide (100 mg TID for 21 days) and betametha- vary from 3 to 19%.1,2 sone (4 mg/mL biweekly for 4 weeks)] of 10 each by random Oral submucous fibrosis causes progressive debilitat- sampling. Burning sensation was assessed every week for 1 month. Burning sensation scores were analyzed using repeated ing symptoms affecting the oral cavity, such as burning measures analysis of variance (ANOVA) and paired t-test. sensation, loss of cheek elasticity, restricted tongue move- Results: Change in burning sensation score was significant ments, and limited mouth opening. Oral submucous (p < 0.05) in the first four visits. However, score between the fibrosis is an irreversible condition and the management 4th and 5th visit was not statistically significant (p > 0.05). -
Median Rhomboid Glossitis
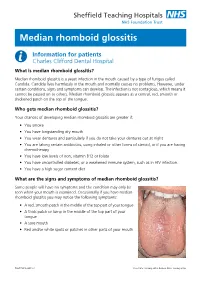
Median rhomboid glossitis Information for patients Charles Clifford Dental Hospital What is median rhomboid glossitis? Median rhomboid glossitis is a yeast infection in the mouth caused by a type of fungus called Candida. Candida lives harmlessly in the mouth and normally causes no problems. However, under certain conditions, signs and symptoms can develop. The infection is not contagious, which means it cannot be passed on to others. Median rhomboid glossitis appears as a central, red, smooth or thickened patch on the top of the tongue. Who gets median rhomboid glossitis? Your chances of developing median rhomboid glossitis are greater if: • You smoke • You have longstanding dry mouth • You wear dentures and particularly if you do not take your dentures out at night • You are taking certain antibiotics, using inhaled or other forms of steroid, or if you are having chemotherapy • You have low levels of iron, vitamin B12 or folate • You have uncontrolled diabetes, or a weakened immune system, such as in HIV infection. • You have a high sugar content diet What are the signs and symptoms of median rhomboid glossitis? Some people will have no symptoms and the condition may only be seen when your mouth is examined. Occasionally if you have median rhomboid glossitis you may notice the following symptoms: • A red, smooth patch in the middle of the top part of your tongue • A thick patch or lump in the middle of the top part of your tongue • A sore mouth • Red and/or white spots or patches in other parts of your mouth PD6779-PIL2645 v4 Issue Date: January 2019. -

Zeroing in on the Cause of Your Patient's Facial Pain
Feras Ghazal, DDS; Mohammed Ahmad, Zeroing in on the cause MD; Hussein Elrawy, DDS; Tamer Said, MD Department of Oral Health of your patient's facial pain (Drs. Ghazal and Elrawy) and Department of Family Medicine/Geriatrics (Drs. Ahmad and Said), The overlapping characteristics of facial pain can make it MetroHealth Medical Center, Cleveland, Ohio difficult to pinpoint the cause. This article, with a handy at-a-glance table, can help. [email protected] The authors reported no potential conflict of interest relevant to this article. acial pain is a common complaint: Up to 22% of adults PracticE in the United States experience orofacial pain during recommendationS F any 6-month period.1 Yet this type of pain can be dif- › Advise patients who have a ficult to diagnose due to the many structures of the face and temporomandibular mouth, pain referral patterns, and insufficient diagnostic tools. disorder that in addition to Specifically, extraoral facial pain can be the result of tem- taking their medication as poromandibular disorders, neuropathic disorders, vascular prescribed, they should limit disorders, or atypical causes, whereas facial pain stemming activities that require moving their jaw, modify their diet, from inside the mouth can have a dental or nondental cause and minimize stress; they (FIGURE). Overlapping characteristics can make it difficult to may require physical therapy distinguish these disorders. To help you to better diagnose and and therapeutic exercises. C manage facial pain, we describe the most common causes and underlying pathological processes. › Consider prescribing a tricyclic antidepressant for patients with persistent idiopathic facial pain. C Extraoral facial pain Extraoral pain refers to the pain that occurs on the face out- 2-15 Strength of recommendation (SoR) side of the oral cavity. -

Alcohol Use and Oral Health Fact Sheet for PROVIDERS OCTOBER 2017
Alcohol Use and Oral Health Fact Sheet FOR PROVIDERS OCTOBER 2017 The Challenge… Glossitis – tongue inflammation Patients who drink alcohol regularly may experience specific problems related to their oral health and hygiene. Angular cheilitis – corners of the mouth chronically inflamed and cracked What you need to know… Candida – yeast infection • Patients who drink high amounts of alcohol daily may brush Oral Ulceration – painful round or oval less effectively than those who don’t drink alcohol, despite sores reporting similar brushing frequency. Also, impaired motor Acute Necrotizing activity can affect their ability to perform basic dental hygiene adequately.1 Ulcerative Gingivitis – infection of the gums that causes ulcers, swelling, and • Alcohol is also the most common cause of sialadenosis dead tissue in the mouth of the parotid gland. This condition causes swelling of the parotid gland and decreased secretion of saliva.2 Ways You Can Help… • Poor nutrient intake and absorption combined with decreased salivary excretion frequently can lead to glossitis, Recommend: angular cheilitis, candida infection, oral ulceration, and acute • Brushing thoroughly two times daily with a necrotizing ulcerative gingivitis (ANUG).2 fluoridated toothpaste. • A decreased immune response combined with a nutritionally • Rinse mouth with non-alcoholic mouth rinse. poor diet, poor oral hygiene, decreased salivary flow, and a • Have an oral examination and cleaning by a high incidence of smoking among these patients, provides dental professional at least two times per year. an environment conducive to rapid progression of periodontal • Regular oral exams that include a periodontal disease, dental caries and increased risk of oral thoracic evaluation and oral cancer screenings to detect cancers.2 any signs of suspicious lesions.3 • High consumption of alcohol may damage the liver and bone marrow resulting in excessive bleeding during dental treatment. -

Download Download
628 Indian Journal of Forensic Medicine & Toxicology, July-September 2021, Vol. 15, No. 3 Tongue Lesions - A Review N.Anitha1, Dharini Jayachandran2 1Reader, Department of Oral Pathology and Microbiology,2Undergraduate Student, Sree Balaji Dental College and Hospital, Bharath Institute of Higher Education and Research Abstract Tongue is a vital organ within the oral cavity that has varied function,and it may act as an index for the underlying systemic diseases.The investigation of the tongue diseases may begin with mere clinical examination .This review is to highlight the signs and symptoms of the various lesions that affects the tongue and especially to talk in brief about the benign and malignant tumours that affect the tongue along with other inherited and congenital abnormalities.Tongue lesions are categorized as tumours,infections, reactionary,congenital,developmental,acquired,autoimmune and potentially malignant disorders for easy understanding and to arrive at appropriate diagnosis.Tongue playing an important role in maintaining the harmony in the oral environment,it should be treated from diseases. Keywords: Tongue lesions,benign tumours,malignant tumours,diseases of tongue. CLASSIFICATION OF LESIONS ● Pyogenic granuloma AFFECTING THE TONGUE. ● Frictional keratosis BENIGN TUMOURS OF THE TONGUE INFECTIOUS LESIONS OF TONGUE ● Capillary hemangioma ● Oral squamous papilloma ● Fibroma ● Oral hairy leukoplakia ● Cavernous hemangioma ● Candidiasiis ● Giant cell granuloma ● Median rhomboid glossitis ● Lipoma ● Sublingual abcess ● Lymphangioma INHERITED,CONGENITAL,DEVELOPMENT ● Schwannoma AND ACQUIRED ABNORMALITIES OF TONGUE MALIGNANT TUMOURS OF TONGUE ● White sponge nevus ● Squamous cell carcinoma ● Foliate papillitis ● Veruccous carcinoma ● Angina bullosa hemorrhagica ● Non-Hodgkin’s lymphoma ● Geographic tongue TRAUMATIC/REACTIONARY LESIONS OF ● Fissured tongue THE TONGUE ● Median rhomboid glossitis ● Fibrous reactive hyperplasia ● Bifurcated/tetrafurcated tongue ● Traumatic ulcer Indian Journal of Forensic Medicine & Toxicology, July-September 2021, Vol. -

Tobacco Induced Oral Keratosis. Oral Sub-Mucous Fibrosis. Nicotine Stomatitis
Tobacco induced oral keratosis. Oral sub-mucous fibrosis. Nicotine stomatitis. Actinic keratosis. Actinic cheilitis Assoc. prof. Zornitsa Mihaylova, DDS, PhD Dept. of Dental, oral and maxillofacial surgery, Faculty of Dental medicine, Medical Universtity- Sofia Precancerous lesions are morphologically altered tissues that possess greater than normal tissues risk of malignant transformation. The term “potentially malignant disorders” (PMD) is broadly accepted in order to avoid terminological confusion. In significant number of cases the oral cancer is preceded by a premalignancy. On the other hand PMD may not undergo malignant transformation (especially when the bad habits are ceased and proper treatment with long-term follow up have been conducted). The following risk factors may play a significant role in the development of PMD and cancer: tobacco smoking, smokeless tobacco, betel quid, alcohol consumption (the combination of smoking and alcohol significantly increases the risk of malignant transformation), oral HPV infection, radiation, vitamin deficiency, bacterial infections, immunosuppression and immunodeficiency, drugs, poor oral hygiene, chronic trauma. It is well established that the effects of the etiologic factors may vary depending on the geographic region, the lifestyle and the habits of the population. Tobacco induced oral keratosis There are three types of smokeless tobacco: dry snuff, moist snuff and chewing tobacco. Smokeless tobacco is mainly used by young males. The long-term/chronic smokeless tobacco use causes local alterations of the oral structures due to the significant nicotine absorption. Some of the most common oral changes related to smokeless tobacco are oral mucosa lesions, periodontal disease and dental caries. Clinically asymptomatic white lesions of the oral mucosa are identified. -

Cardiovascular Drugs-Induced Oral Toxicities: a Murky Area to Be Revisited and Illuminated
Pharmacological Research 102 (2015) 81–89 Contents lists available at ScienceDirect Pharmacological Research j ournal homepage: www.elsevier.com/locate/yphrs Review Cardiovascular drugs-induced oral toxicities: A murky area to be revisited and illuminated a, b b Pitchai Balakumar ∗, Muthu Kavitha , Suresh Nanditha a Pharmacology Unit, Faculty of Pharmacy, AIMST University, Semeling, 08100 Bedong, Malaysia b Faculty of Dentistry, AIMST University, 08100 Bedong, Malaysia a r t i c l e i n f o a b s t r a c t Article history: Oral health is an imperative part of overall human health. Oral disorders are often unreported, but are Received 20 July 2015 highly troublesome to human health in a long-standing situation. A strong association exists between Received in revised form 22 August 2015 cardiovascular drugs and oral adverse effects. Indeed, several cardiovascular drugs employed clinically Accepted 8 September 2015 have been reported to cause oral adverse effects such as xerostomia, oral lichen planus, angioedema, Available online 25 September 2015 aphthae, dysgeusia, gingival enlargement, scalded mouth syndrome, cheilitis, glossitis and so forth. Oral complications might in turn worsen the cardiovascular disease condition as some reports suggest an Keywords: adverse correlation between periodontal oral disease pathogenesis and cardiovascular disease. These are Cardiovascular drugs certainly important to be understood for a better use of cardiovascular medicines and control of associated Oral adverse effects oral adverse effects. This review sheds lights on the oral adverse effects pertaining to the clinical use of Dry mouth Angioedema cardiovascular drugs. Above and beyond, an adverse correlation between oral disease and cardiovascular Dysgeusia disease has been discussed. -
Atrophic Glossitis: Burning Agony of Nutritional Deficiency Anemia 1Neeti Swarup, 2Shreya Gupta, 3Chandrani Sagolsem, 4Zoya Chowdhary, 5Subhash Gupta, 6Nidhi Sinha
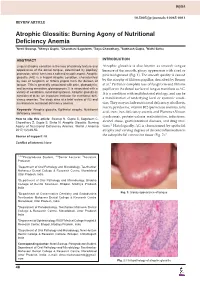
WJOA Neeti Swarup et al 10.5005/jp-journals-10065-0011 REVIEW ARTICLE Atrophic Glossitis: Burning Agony of Nutritional Deficiency Anemia 1Neeti Swarup, 2Shreya Gupta, 3Chandrani Sagolsem, 4Zoya Chowdhary, 5Subhash Gupta, 6Nidhi Sinha ABSTRACT INTRODUCTION Lingual atrophic condition is the loss of ordinary texture and Atrophic glossitis is also known as smooth tongue appearance of the dorsal tongue, determined by papillary because of the smooth, glossy appearance with a red or protrusion, which turns into a soft and smooth aspect. Atrophic pink background (Fig. 1). The smooth quality is caused glossitis (AG) is a lingual atrophic condition, characterized by loss of fungiform or filiform papilla from the dorsum of by the atrophy of filiform papillae, described by Reamy 1 tongue. This is generally associated with pain, glossodynia, et al. Partial or complete loss of fungiform and filiform and burning sensation, glossopyrosis. It is associated with a papillae on the dorsal surface of tongue manifests as AG. variety of conditions, local and systemic. Atrophic glossitis is It is a condition with multifactorial etiology, and can be considered to be an important indicator for nutritional defi- ciency anemias. The study aims at a brief review of AG and a manifestation of underlying local or systemic condi- its relation to nutritional deficiency anemia. tion. They may include nutritional deficiency, riboflavin, niacin, pyridoxine, vitamin B12 (pernicious anemia), folic Keywords: Atrophic glossitis, Epithelial atrophy, Nutritional deficiency anemia. acid, iron (iron deficiency anemia and Plummer-Vinson syndrome), protein-calorie malnutrition, infections, How to cite this article: Swarup N, Gupta S, Sagolsem C, alcohol abuse, gastrointestinal diseases, and drug reac- Chowdhary Z, Gupta S, Sinha N. -

Giant Cell Arteritis Misdiagnosed As Temporomandibular Disorder: a Case Report and Review of the Literature
360_Reiter.qxp 10/14/09 3:17 PM Page 360 Giant Cell Arteritis Misdiagnosed as Temporomandibular Disorder: A Case Report and Review of the Literature Shoshana Reiter, DMD Giant cell arteritis (GCA) is a systemic vasculitis involving medium Teacher and large-sized arteries, most commonly the extracranial branches Department of Oral Rehabilitation of the carotid artery. Early diagnosis and treatment are essential to avoid severe complications. This article reports on a GCA case Ephraim Winocur, DMD and discusses how the orofacial manifestations of GCA can lead to Lecturer misdiagnosis of GCA as temporomandibular disorder. GCA Department of Oral Rehabilitation should be included in the differential diagnosis of orofacial pain in Carole Goldsmith, DMD the elderly based on the knowledge of related signs and symptoms, Instructor mainly jaw claudication, hard end-feel limitation of range of Department of Oral Rehabilitation motion, and temporal headache. J OROFAC PAIN 2009;23:360–365 Alona Emodi-Perlman, DMD Key words: Giant cell arteritis, jaw claudication, Teacher temporomandibular disorders, trismus Department of Oral Rehabilitation Meir Gorsky, DMD Professor Department of Oral Pathology and Oral iant cell arteritis (GCA) is a systemic vasculitis involving Medicine the large and medium-sized vessels, particularly the extracranial branches of the carotid artery. It is more com- The Maurice and Gabriela Goldschleger G School of Dental Medicine mon in women (M:F ratio 2:5) and usually affects patients older 1 Tel Aviv University, Israel than 50 years with an increased risk with age. The highest preva- lence of GCA has been reported in Scandinavian populations and Correspondence to: in those with a strong Scandinavian ethnic background.2 Dr. -

Tropical Disease Treatment Guide
HOM Disease, Symptom, and Treatment Guide Medical practice in Haiti like many developing countries is very different from practice in the United States. The lack of resources can be challenging to medical providers who are accustomed to confirming their diagnosis with labs, x-rays and other diagnostic tests. In Haiti, even when the resources are available, few people have the money to pay for labs or other tests. Diagnosis and treatment often is based primarily on history and physical. This guide is not intended to be a substitute for professional medical judgment but to help providers to arrive at an appropriate treatment for diseases that are less common in the U.S. or are diagnosed or treated differently in Haiti. As most Haitian are antibiotic naïve, and more susceptible to side effects of many medications, lower doses for shorter duration is appropriate for most acute illnesses. Anemia Dengue Fever Lymphatic Filariasis Cellulitis Epigastric Pain Malaria Chikungunya Helminths Tropical Sprue Diarrheal pathogens Ascaris lumbricoides (Roundworm) Tuberculosis (TB) Amebiasis Enterobius (Pinworm) Typhoid Fever Cholera Hookworm infections Typhus Giardiantestinalis Hepatitis A & E Vit A deficiency (VAD) Schistosomiasis Leprosy Shigellosis Leptospirosis ANEMIA Signs and Symptoms • pale conjunctiva (inner eyelid), nail beds, gums, tongue, lips, skin, • fatigue • HA • breathlessness Treatment • Adult: 150-200mg/day of elemental iron for 3 months • Pregnant women: 1 tablet of iron & folic acid every day for 6 months • Children under 6 y/o at risk of iron poisoning ANTHRAX (Colloquially known as “malcharbon” or “sick charcoal”) Human anthrax usually involves the skin (neck, face and upper extremities.) Spores enter the skin through minor cuts or abrasions. -

Spectrum of Lip Lesions in a Tertiary Care Hospital: an Epidemiological Study of 3009 Indian Patients
Brief Report Spectrum of Lip Lesions in a Tertiary Care Hospital: An Epidemiological Study of 3009 Indian Patients Abstract Shivani Bansal, Aim: Large‑scale population‑based screening studies have identified lip lesions to be the most Sana Shaikh, common oral mucosal lesions; however, few studies have been carried out to estimate the prevalence Rajiv S. Desai, of lip lesions exclusively. The aim of present study is to highlight the diversity of lip lesions and determine their prevalence in an unbiased Indian population. Materials and Methods: Lip lesions Islam Ahmad, were selected from 3009 patients who visited the department over a period of 3 years (January Pavan Puri, 2012 to December 2014). Age, sex, location of lip lesions, a detailed family and medical history, Pooja Prasad, along with the history of any associated habit was recorded. Biopsy was carried out in necessary Pankaj Shirsat, cases to reach a final diagnosis. The pathologies of the lip were classified based on the etiology. Dipali Gundre Results: Among 3009 patients, 495 (16.5%) had lip lesions ranging from 4 years to 85 years with a Department of Oral Pathology, mean age of 39.7 years. There were 309 (62.4%) males and 185 (31.9%) females. Lower lip was the Nair Hospital Dental College, most affected region (54.1%) followed by the corner of the mouth (30.9%) and upper lip (11.7%). Mumbai Central, Mumbai, In 3.2% of the cases, both the lips were involved. Of the 495 lip lesions, the most common were Maharashtra, India Potentially Malignant Disorders (PMDs) (37.4%), herpes labialis (33.7%), mucocele (6.7%), angular cheilitis (6.1%), and allergic and immunologic lesions (5.7%). -

Comparative Evaluation of the Efficacy of Systemic Levamisole And
Journal of Advanced Clinical & Research Insights (2019), 6, 33–38 ORIGINAL ARTICLE Comparative evaluation of the efficacy of systemic levamisole and antioxidant in the management of oral submucous fibrosis – A randomized control trial Anuja Anil Shinge1, Preeti Kanchan-Talreja1, Deepa Das1, Amita Navalkar1, Prakash S. Talreja2, Ashutosh Kakade3 1Department of Oral Medicine and Radiology, Y.M.T. Dental College and Hospital, Navi Mumbai, Maharashtra, India, 2Department of Periodontics, Bharati Vidyapeeth Dental College and Hospital, Navi Mumbai, Maharashtra, India, 3Department of Pharmacology, M.G.M Medical College and Hospital, Navi Mumbai, Maharashtra, India Keywords: Abstract Cap. Antoxid, tab. levamisole, oral submucous Background: Oral submucous fibrosis (OSF) is a chronic, disabling disease involving fibrosis the entire oral mucosa, mainly reported in Indian population. A number of treatment Correspondence: modalities have been tried, but none of these have been completely therapeutic. Dr. Anuja Anil Shinge, Department of Levamisole, an immunomodulator, has been reported to be beneficial in oral mucosal Oral Medicine and Radiology, Y.M.T. lesions, but there are hardly any studies reported in literature for OSF patients, and Dental College and Hospital, Dr. G. D. Pol hence, the study was taken up. Foundations, Kharghar, Institutional Area, Aim: This study aims to compare the efficacy of levamisole with antioxidant for the Navi Mumbai - 410210. assessment of burning sensation and mouth opening in OSF patients. E-mail: [email protected] Materials and Methods: A total of 60 patients clinically diagnosed of OSF were selected for the study. We assessed patients for burning sensation and mouth opening. Patients Received: 02 February 2019; were divided into four groups according to staging of OSF (More et al., classification), Accepted: 11 March 2019 then randomly subdivided into three groups to dispense medicines.