The Painful Mouth
Total Page:16
File Type:pdf, Size:1020Kb
Load more
Recommended publications
-

The Use of Biologic Agents in the Treatment of Oral Lesions Due to Pemphigus and Behçet's Disease: a Systematic Review
Davis GE, Sarandev G, Vaughan AT, Al-Eryani K, Enciso R. The Use of Biologic Agents in the Treatment of Oral Lesions due to Pemphigus and Behçet’s Disease: A Systematic Review. J Anesthesiol & Pain Therapy. 2020;1(1):14-23 Systematic Review Open Access The Use of Biologic Agents in the Treatment of Oral Lesions due to Pemphigus and Behçet’s Disease: A Systematic Review Gerald E. Davis II1,2, George Sarandev1, Alexander T. Vaughan1, Kamal Al-Eryani3, Reyes Enciso4* 1Advanced graduate, Master of Science Program in Orofacial Pain and Oral Medicine, Herman Ostrow School of Dentistry of USC, Los Angeles, California, USA 2Assistant Dean of Academic Affairs, Assistant Professor, Restorative Dentistry, Meharry Medical College, School of Dentistry, Nashville, Tennessee, USA 3Assistant Professor of Clinical Dentistry, Division of Periodontology, Dental Hygiene & Diagnostic Sciences, Herman Ostrow School of Dentistry of USC, Los Angeles, California, USA 4Associate Professor (Instructional), Division of Dental Public Health and Pediatric Dentistry, Herman Ostrow School of Dentistry of USC, Los Angeles, California, USA Article Info Abstract Article Notes Background: Current treatments for pemphigus and Behçet’s disease, such Received: : March 11, 2019 as corticosteroids, have long-term serious adverse effects. Accepted: : April 29, 2020 Objective: The objective of this systematic review was to evaluate the *Correspondence: efficacy of biologic agents (biopharmaceuticals manufactured via a biological *Dr. Reyes Enciso, Associate Professor (Instructional), Division source) on the treatment of intraoral lesions associated with pemphigus and of Dental Public Health and Pediatric Dentistry, Herman Ostrow Behçet’s disease compared to glucocorticoids or placebo. School of Dentistry of USC, Los Angeles, California, USA; Email: [email protected]. -
Median Rhomboid Glossitis
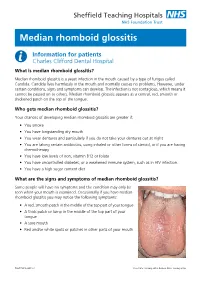
Median rhomboid glossitis Information for patients Charles Clifford Dental Hospital What is median rhomboid glossitis? Median rhomboid glossitis is a yeast infection in the mouth caused by a type of fungus called Candida. Candida lives harmlessly in the mouth and normally causes no problems. However, under certain conditions, signs and symptoms can develop. The infection is not contagious, which means it cannot be passed on to others. Median rhomboid glossitis appears as a central, red, smooth or thickened patch on the top of the tongue. Who gets median rhomboid glossitis? Your chances of developing median rhomboid glossitis are greater if: • You smoke • You have longstanding dry mouth • You wear dentures and particularly if you do not take your dentures out at night • You are taking certain antibiotics, using inhaled or other forms of steroid, or if you are having chemotherapy • You have low levels of iron, vitamin B12 or folate • You have uncontrolled diabetes, or a weakened immune system, such as in HIV infection. • You have a high sugar content diet What are the signs and symptoms of median rhomboid glossitis? Some people will have no symptoms and the condition may only be seen when your mouth is examined. Occasionally if you have median rhomboid glossitis you may notice the following symptoms: • A red, smooth patch in the middle of the top part of your tongue • A thick patch or lump in the middle of the top part of your tongue • A sore mouth • Red and/or white spots or patches in other parts of your mouth PD6779-PIL2645 v4 Issue Date: January 2019. -

Zeroing in on the Cause of Your Patient's Facial Pain
Feras Ghazal, DDS; Mohammed Ahmad, Zeroing in on the cause MD; Hussein Elrawy, DDS; Tamer Said, MD Department of Oral Health of your patient's facial pain (Drs. Ghazal and Elrawy) and Department of Family Medicine/Geriatrics (Drs. Ahmad and Said), The overlapping characteristics of facial pain can make it MetroHealth Medical Center, Cleveland, Ohio difficult to pinpoint the cause. This article, with a handy at-a-glance table, can help. [email protected] The authors reported no potential conflict of interest relevant to this article. acial pain is a common complaint: Up to 22% of adults PracticE in the United States experience orofacial pain during recommendationS F any 6-month period.1 Yet this type of pain can be dif- › Advise patients who have a ficult to diagnose due to the many structures of the face and temporomandibular mouth, pain referral patterns, and insufficient diagnostic tools. disorder that in addition to Specifically, extraoral facial pain can be the result of tem- taking their medication as poromandibular disorders, neuropathic disorders, vascular prescribed, they should limit disorders, or atypical causes, whereas facial pain stemming activities that require moving their jaw, modify their diet, from inside the mouth can have a dental or nondental cause and minimize stress; they (FIGURE). Overlapping characteristics can make it difficult to may require physical therapy distinguish these disorders. To help you to better diagnose and and therapeutic exercises. C manage facial pain, we describe the most common causes and underlying pathological processes. › Consider prescribing a tricyclic antidepressant for patients with persistent idiopathic facial pain. C Extraoral facial pain Extraoral pain refers to the pain that occurs on the face out- 2-15 Strength of recommendation (SoR) side of the oral cavity. -

Management of Oral Submucous Fibrosis – an Update
European Journal of Molecular & Clinical Medicine ISSN 2515-8260 Volume 07, Issue 5, 2020 Management Of Oral Submucous Fibrosis – An Update Aishwarya V1; Dr. A. Amudhan2, Dr. A. Amudhan Professor, Dept. of Oral Medicine and Radiology, Sree Balaji Dental College and Hospital, Bharath Institute of Higher Education and Research, Chennai. 1. Undergraduate student, Sree Balaji Dental College and Hospital, Bharath Institute of Higher Education and Research, Chennai. 2. Professor, Dept of Oral Medicine and Radiology, Sree Balaji Dental College and Hospital, Bharath Institute of Higher Education and Research, Chennai. Professor, Dept. of Oral Medicine and Radiology, Sree Balaji Dental College and Hospital, Bharath Institute of Higher Education and Research, Chennai. Email ID: [email protected] ABSTRACT: Oral submucous fibrosis (OSF) is an insidious, chronic, progressive, debilitating disease. It is mostly prevalent in the South-east Asian countries. Areca nut chewing usually causes the condition. The hallmark of the disease being sub mucosal fibrosis that affects most parts of the oral cavity, pharynx and upper third of the oesophagus and its clinical presentation depends on the stage of the disease at detection. As the disease has a spectrum of presentation, the management differs with the various stages of the disease. This article reviews the various medical management techniques of oral submucous fibrosis. KEYWORDS: Arecanut; Etiopathogenesis; Management; Oral submucous fibrosis INTRODUCTION: Oral submucous fibrosis was first described -

Caudal Stomatitis and Other Autoimmune Oral Disease
Caudal Stomatitis and Other Autoimmune Oral Disease Yuck, no practitioner wants to deal with these cases… But treating these will benefit your patients Autoimmune Oral Disease Multiple expressions of over response of the immune system Most common are; Caudal Stomatitis Chronic Ulcerative Paradental Stomatitis Juvenile Periodontitis Caudal Stomatitis Primarily in feline patients Hallmarks in history: Oral pain Dysphagia Ptyalism Vocalizing Distinct halitosis Diagnosis of Caudal Stomatitis Primarily a diagnosis of history and oral evaluation Oral evaluation hallmarks Palatitis Glossitis Mucositis PALATOGLOSSAL FOLD PROLIFERATION, ULCERATION Other useful diagnostic tools Hypergammaglobulinemia Bartonella titer (this is of questionable clinical relevance) Histopathology almost always shows lymphoplasmacytic infiltrate with mild to moderate fibrosis Some neutrophilic infiltrate is common WHEN IN DOUBT, SUBMIT INCISIONAL BIOPSY Pathogenesis Well…This is really up for grabs. Thought to be auto-antibodies directed at the periodontal ligament There are certainly multiple etiologies and much needs to be elucidated Probable Caudal Stomatitis Unlikely Caudal Stomatitis OK, this is the big one THERAPY OF CAUDAL STOMATITIS Divide therapy into acute therapy directed at return to eating and definitive therapy directed at long term analgesia and return to function THERE IS NO CURE, WE ARE TREATING SYMPTOMS Acute Therapy 1. In anorexic, painful cats a. Analgesics 1. Opioids 2. Non-steroidal anti-inflammatories 3. Oral antibiotics -

Oral Lesions in Sjögren's Syndrome
Med Oral Patol Oral Cir Bucal. 2018 Jul 1;23 (4):e391-400. Oral lesions in Sjögren’s syndrome patients Journal section: Oral Medicine and Pathology doi:10.4317/medoral.22286 Publication Types: Review http://dx.doi.org/doi:10.4317/medoral.22286 Oral lesions in Sjögren’s syndrome: A systematic review Julia Serrano 1, Rosa-María López-Pintor 1, José González-Serrano 1, Mónica Fernández-Castro 2, Elisabeth Casañas 1, Gonzalo Hernández 1 1 Department of Oral Medicine and Surgery, School of Dentistry, Complutense University, Madrid, Spain 2 Rheumatology Service, Hospital Infanta Sofía, Madrid, Spain Correspondence: Departamento de Especialidades Clínicas Odontológicas Facultad de Odontología Universidad Complutense de Madrid Plaza Ramón y Cajal s/n, 28040 Madrid. Spain [email protected] Serrano J, López-Pintor RM, González-Serrano J, Fernández-Castro M, Casañas E, Hernández G. Oral lesions in Sjögren’s syndrome: A system- atic review. Med Oral Patol Oral Cir Bucal. 2018 Jul 1;23 (4):e391-400. Received: 18/11/2017 http://www.medicinaoral.com/medoralfree01/v23i4/medoralv23i4p391.pdf Accepted: 09/05/2018 Article Number: 22291 http://www.medicinaoral.com/ © Medicina Oral S. L. C.I.F. B 96689336 - pISSN 1698-4447 - eISSN: 1698-6946 eMail: [email protected] Indexed in: Science Citation Index Expanded Journal Citation Reports Index Medicus, MEDLINE, PubMed Scopus, Embase and Emcare Indice Médico Español Abstract Background: Sjögren’s syndrome (SS) is an autoimmune disease related to two common symptoms: dry mouth and eyes. Although, xerostomia and hyposialia have been frequently reported in these patients, not many studies have evaluated other oral manifestations. -

Benign Migratory Glossitis: Case Report and Literature Review
Volume 1- Issue 5 : 2017 DOI: 10.26717/BJSTR.2017.01.000482 Sarfaraz Khan. Biomed J Sci & Tech Res ISSN: 2574-1241 Case Report Open Access Benign Migratory Glossitis: Case Report and Literature Review Sarfaraz Khan1*, Syed AsifHaider Shah2, Tanveer Ahmed Mujahid3 and Muhammad Ishaq4 1Consultant Oral and Maxillofacial Surgeon, Pak Field Hospital Darfur, Sudan 2MDC Gujranwala, Pakistan 3Consultant Dermatologist, Pak Field Hospital Darfur, Sudan 4Registrar Dermatologist, Pak Field Hospital Darfur, Sudan Received: October 25, 2017; Published: October 31, 2017 *Corresponding author: Sarfaraz Khan, Consultant Oral and Maxillofacial Surgeon, Pakistan Field Hospital Darfur, Sudan, Tel: ; Email: Abstract Benign migratory Glossitis (BMG) is a benign, usually asymptomatic mucosal lesion of dorsal surface of the tongue, characterized by depapillated erythematous patches separated by white irregular borders. Etiology of BMG is unknown. Risk factors include psoriasis, fissured tongue, diabetes mellitus, hypersensitivity and psychological factors. We report BMG in an Egyptian soldier of UN peace keeping force, with stressKeywords: as a possible Geographic etiological tongue; factor Benign and migratory provide literature Glossitis; reviewErythema of this migrans disorder. Introduction Benign migratory Glossitis (BMG) is a benign, immune- spicy/salty food and/or alcoholic drinks [4,5].The lesion typically usually characterized by asymptomatic erythematous patches changes its shape with time owing to the change in pattern of mediated, chronic inflammatory lesion of unknown etiology, depapillation.Similar lesions may also be seen in atrophic candidiasis, local chemical or mechanical trauma, drug induced reactions, psoriasis with whitish margins across the surface of the tongue. This condition is also known as geographic tongue, erythema migrans, Treatment of symptomatic BMG aims at provision of symptomatic Glossitis exfoliativa and wandering rash of the tongue. -

Case Report Treatment of Geographic Tongue
Scholars Journal of Dental Sciences (SJDS) ISSN 2394-496X (Online) Sch. J. Dent. Sci., 2015; 2(7):409-413 ISSN 2394-4951 (Print) ©Scholars Academic and Scientific Publisher (An International Publisher for Academic and Scientific Resources) www.saspublisher.com Case Report Treatment of Geographic Tongue Superimposing Fissured Tongue: A literature review with case report Jalaleddin H Hamissi1, Mahsa EsFehani2, Zahra Hamissi3 1Associate Professor in periodontics and Dental Caries Prevention Research Center, Qazvin University Medical Sciences, Qazvin, Iran. 2Assistant Professor, Department of Oral Medicine & Diagnosis, college dentistry, Qazvin University Medical Sciences, Qazvin, Iran. 3Dental Student, College of Dentistry, Shahied Behesti University of Medical Sciences, Teheran, Iran *Corresponding author Dr Jalaleddin H Hamissi Email: [email protected] ; [email protected] Abstract: Tongue is a most sensitive part of the oral cavity. It is responsible for many functions in the mouth like swallowing, speech, mastication, speaking and breathing. Geographic tongue (Benign migratory glossitis, erythema migrans) is an asymptomatic inflammatory disorder of tongue with controversial etiology. This disease is characterized by erythematous areas showing raised greyish or white circinate lines or bands with irregular pattern on the dorsal surface of the tongue and depapillation. The objective in presenting the case report and literature review is to discuss the clinical presentation, associated causative factors and management strategies of geographic tongue. Keywords: Asymptomatic; Characteristics; Fissured tongue; Geographic tongue; Migratory INTRODUCTION in approximately three percent (3%) majority of female Geographic tongue is an asymptomatic population [9]. On other aspects of oral mucosa, such as inflammatory condition of the dorsum of tongue on commissure of lip, floor of mouth, cheek etc., which occasionally extending towards the lateral borders. -

Oral Manifestations of Systemic Disease Their Clinical Practice
ARTICLE Oral manifestations of systemic disease ©corbac40/iStock/Getty Plus Images S. R. Porter,1 V. Mercadente2 and S. Fedele3 provide a succinct review of oral mucosal and salivary gland disorders that may arise as a consequence of systemic disease. While the majority of disorders of the mouth are centred upon the focus of therapy; and/or 3) the dominant cause of a lessening of the direct action of plaque, the oral tissues can be subject to change affected person’s quality of life. The oral features that an oral healthcare or damage as a consequence of disease that predominantly affects provider may witness will often be dependent upon the nature of other body systems. Such oral manifestations of systemic disease their clinical practice. For example, specialists of paediatric dentistry can be highly variable in both frequency and presentation. As and orthodontics are likely to encounter the oral features of patients lifespan increases and medical care becomes ever more complex with congenital disease while those specialties allied to disease of and effective it is likely that the numbers of individuals with adulthood may see manifestations of infectious, immunologically- oral manifestations of systemic disease will continue to rise. mediated or malignant disease. The present article aims to provide This article provides a succinct review of oral manifestations a succinct review of the oral manifestations of systemic disease of of systemic disease. It focuses upon oral mucosal and salivary patients likely to attend oral medicine services. The review will focus gland disorders that may arise as a consequence of systemic upon disorders affecting the oral mucosa and salivary glands – as disease. -

Oral Candidosis: Aetiology, Clinical Manifestations, Diagnosis and Management Birsay Gümrü Tarçın
MÜSBED 2011;1(2):140-148 Derleme / Review Oral Candidosis: Aetiology, Clinical Manifestations, Diagnosis and Management Birsay Gümrü Tarçın Marmara University Faculty of Dentistry, Department of Oral Diagnosis and Radiology, Istanbul-Turkey Ya zış ma Ad re si / Add ress rep rint re qu ests to: Birsay Gümrü Tarçın Marmara University Faculty of Dentistry, Department of Oral Diagnosis and Radiology, Büyükçiftlik Sok. No: 6 34365 Nişantaşı, Şişli, İstanbul-Turkey Telefon / Phone: +90-212-231-9120 Faks / Fax: +90-212-246-5247 Elekt ro nik pos ta ad re si / E-ma il add ress: [email protected] Ka bul ta ri hi / Da te of ac cep tan ce: 22 Ağustos 2011 / August 22, 2011 ÖZET ABS TRACT Oral kandidozis: Etiyoloji, klinik özellikler, tanı Oral candidosis: aetiology, clinical ve tedavi manifestations, diagnosis and management Oral kandidozis dişhekimliği pratiğinde en sık karşılaşılan fungal Oral candidosis is the most common fungal infection encountered enfeksiyondur. Birçok farklı klinik görünümde ortaya çıkabildi- in dental practice. Clinical diagnosis and management of oral ğinden, klinik tanı ve tedavisi genellikle zordur. Hastalık sıklıkla candidosis is usually complicated, because it is encountered in a sistemik rahatsızlığı olan spesifik hasta gruplarında ortaya çık- wide variety of clinical presentations. The disease often manifests maktadır. Bu nedenle, oral kandidozis tedavisi öncelikle predis- in specific patient groups that are systemically compromised. pozisyon yaratan durumların kapsamlı tetkikini içermelidir. Bu Therefore, the management should always cover a thorough derlemede sık karşılaşılan oral kandidal lezyonların etiyolojisi, investigation of underlying predisposing conditions. This klinik görünümü, tanı ve tedavi stratejileri kapsamlı bir şekilde review provides a comprehensive overview of the aetiology, gözden geçirilmektedir. -

Alcohol Use and Oral Health Fact Sheet for PROVIDERS OCTOBER 2017
Alcohol Use and Oral Health Fact Sheet FOR PROVIDERS OCTOBER 2017 The Challenge… Glossitis – tongue inflammation Patients who drink alcohol regularly may experience specific problems related to their oral health and hygiene. Angular cheilitis – corners of the mouth chronically inflamed and cracked What you need to know… Candida – yeast infection • Patients who drink high amounts of alcohol daily may brush Oral Ulceration – painful round or oval less effectively than those who don’t drink alcohol, despite sores reporting similar brushing frequency. Also, impaired motor Acute Necrotizing activity can affect their ability to perform basic dental hygiene adequately.1 Ulcerative Gingivitis – infection of the gums that causes ulcers, swelling, and • Alcohol is also the most common cause of sialadenosis dead tissue in the mouth of the parotid gland. This condition causes swelling of the parotid gland and decreased secretion of saliva.2 Ways You Can Help… • Poor nutrient intake and absorption combined with decreased salivary excretion frequently can lead to glossitis, Recommend: angular cheilitis, candida infection, oral ulceration, and acute • Brushing thoroughly two times daily with a necrotizing ulcerative gingivitis (ANUG).2 fluoridated toothpaste. • A decreased immune response combined with a nutritionally • Rinse mouth with non-alcoholic mouth rinse. poor diet, poor oral hygiene, decreased salivary flow, and a • Have an oral examination and cleaning by a high incidence of smoking among these patients, provides dental professional at least two times per year. an environment conducive to rapid progression of periodontal • Regular oral exams that include a periodontal disease, dental caries and increased risk of oral thoracic evaluation and oral cancer screenings to detect cancers.2 any signs of suspicious lesions.3 • High consumption of alcohol may damage the liver and bone marrow resulting in excessive bleeding during dental treatment. -

Burning Mouth Syndrome 25/03/13 11:36
Burning Mouth Syndrome 25/03/13 11:36 Medscape Reference Reference News Reference Education MEDLINE Burning Mouth Syndrome Author: Vincent D Eusterman, MD, DDS; Chief Editor: Arlen D Meyers, MD, MBA more... Updated: Jan 26, 2012 Background Burning mouth syndrome (BMS) is an idiopathic condition characterized by a continuous burning sensation of the mucosa of the mouth, typically involving the tongue, with or without extension to the lips and oral mucosa. Classically, burning mouth syndrome (BMS) is accompanied by gustatory disturbances (dysgeusia, parageusia) and subjective xerostomia. By definition, no macroscopic alterations in oral mucosa are apparent. Burning mouth syndrome (BMS) occurs most frequently, but not exclusively, in peri-menopausal and postmenopausal women. See the following illustration. A 29-year-old female presents with tongue irritation. A diagnosis of benign migratory glossitis (geographic tongue) is made by the appearance. The portions of the tongue with atrophic filiform papilla are symptomatic to acidic foods. Burning mouth syndrome (BMS) is a clinical diagnosis made via the exclusion of all other causes. No universally accepted diagnostic criteria, laboratory tests, imaging studies or other modalities definitively diagnose or exclude burning mouth syndrome (BMS). Various attempts to classify burning mouth syndrome (BMS) based on etiology and symptoms have been made. In a classification by etiology or cause, idiopathic burning mouth syndrome (BMS) is considered “primary BMS” (or "true BMS"), whereas “secondary BMS” has an identifiable cause. For the purposes of this article, we will use these terms. Another classification of burning mouth syndrome (BMS) is based on symptoms, stratifying cases into 3 types, as follows:[1] Type 1 burning mouth syndrome (BMS): Patients have no symptoms upon waking, with progression throughout the day.