The Dysfunctional Autonomic Nervous System in ME/CFS
Total Page:16
File Type:pdf, Size:1020Kb
Load more
Recommended publications
-
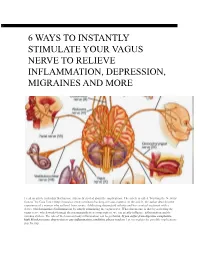
6 Ways to Instantly Stimulate Your Vagus Nerve to Relieve Inflammation, Depression, Migraines and More
O 6 WAYS TO INSTANTLY STIMULATE YOUR VAGUS NERVE TO RELIEVE INFLAMMATION, DEPRESSION, MIGRAINES AND MORE I read an article yesterday that has me extremely excited about the implications. The article is called “Hacking the Nervous System” by Gaia Vince (http://mosaicscience.com/story/hacking-nervous-system). In the article, the author describes the experience of a woman who suffered from severe, debilitating rheumatoid arthritis and her eventual treatment with a device which minimized inflammation by simply stimulating the vagus nerve. What this means, is that by activating the vagus nerve which works through the parasympathetic nervous system, we can greatly influence inflammation and the immune system. The role of the brain on body inflammation can be profound. If you suffer from digestive complaints, high blood pressure, depression or any inflammatory condition, please read on. Let me explain the possible implications step by step. What is the vagus nerve? First of all, the vagus nerve is the longest nerve in the body which originates in the brain as cranial nerve ten, travels down the from go the neck and then passes around the digestive system, liver, spleen, pancreas, heart and lungs. This nerve is a major player in the parasympathetic nervous system, which is the ‘rest and digest’ part (opposite to the sympathetic nervous system which is ‘fight of flight’). Vagal tone The tone of the vagus nerve is key to activating the parasympathetic nervous system. Vagal tone is measured by tracking your heart-rate alongside your breathing rate. Your heart-rate speeds up a little when your breathe in, and slows down a little when you breathe out. -

The Baseline Structure of the Enteric Nervous System and Its Role in Parkinson’S Disease
life Review The Baseline Structure of the Enteric Nervous System and Its Role in Parkinson’s Disease Gianfranco Natale 1,2,* , Larisa Ryskalin 1 , Gabriele Morucci 1 , Gloria Lazzeri 1, Alessandro Frati 3,4 and Francesco Fornai 1,4 1 Department of Translational Research and New Technologies in Medicine and Surgery, University of Pisa, 56126 Pisa, Italy; [email protected] (L.R.); [email protected] (G.M.); [email protected] (G.L.); [email protected] (F.F.) 2 Museum of Human Anatomy “Filippo Civinini”, University of Pisa, 56126 Pisa, Italy 3 Neurosurgery Division, Human Neurosciences Department, Sapienza University of Rome, 00135 Rome, Italy; [email protected] 4 Istituto di Ricovero e Cura a Carattere Scientifico (I.R.C.C.S.) Neuromed, 86077 Pozzilli, Italy * Correspondence: [email protected] Abstract: The gastrointestinal (GI) tract is provided with a peculiar nervous network, known as the enteric nervous system (ENS), which is dedicated to the fine control of digestive functions. This forms a complex network, which includes several types of neurons, as well as glial cells. Despite extensive studies, a comprehensive classification of these neurons is still lacking. The complexity of ENS is magnified by a multiple control of the central nervous system, and bidirectional communication between various central nervous areas and the gut occurs. This lends substance to the complexity of the microbiota–gut–brain axis, which represents the network governing homeostasis through nervous, endocrine, immune, and metabolic pathways. The present manuscript is dedicated to Citation: Natale, G.; Ryskalin, L.; identifying various neuronal cytotypes belonging to ENS in baseline conditions. -

Autonomic Nerve Activity and Cardiac Arrhythmias
ACORP Complete (with appendices) Last Name of PI► Protocol No. Assigned by the IACUC►02002 Official Date of Approval► 1. Caging needs. Complete the table below to describe the housing that will have to be accommodated by the housing sites for this protocol: d. Is this housing e. Estimated c. Number of consistent with the maximum number a. Species b. Type of housing* individuals per Guide and USDA of housing units housing unit** regulations? needed at any one (yes/no***) time Chain link run, 3x6 Canines 1 no 7 and 4x10 feet cage *See ACORP Instructions, for guidance on describing the type of housing needed. If animals are to be housed according to a local Standard Operating Procedure (SOP), enter “standard (see SOP)” here, and enter the SOP into the table in Item Y. If the local standard housing is not described in a SOP, enter “standard, see below” in the table and describe the standard housing here: Chain link run, 3x6 feet cages ** The Guide states that social animals should generally be housed in stable pairs or groups. Provide a justification if any animals will be housed singly (if species is not considered “social”, then so note) Dogs are housed singly in chain link runs but can socialize with one another since each room has two to five dog runs. In addition, while their runs are being cleaned on a daily basis, pairs of dogs are allowed to exercise and play together in a designated "romper room". Animals are fitted with DSI transmitters and need to be housed singly in a cage for which DSI receivers are installed to receive signals from the transmitters. -

What Is the Autonomic Nervous System?
J Neurol Neurosurg Psychiatry: first published as 10.1136/jnnp.74.suppl_3.iii31 on 21 August 2003. Downloaded from AUTONOMIC DISEASES: CLINICAL FEATURES AND LABORATORY EVALUATION *iii31 Christopher J Mathias J Neurol Neurosurg Psychiatry 2003;74(Suppl III):iii31–iii41 he autonomic nervous system has a craniosacral parasympathetic and a thoracolumbar sym- pathetic pathway (fig 1) and supplies every organ in the body. It influences localised organ Tfunction and also integrated processes that control vital functions such as arterial blood pres- sure and body temperature. There are specific neurotransmitters in each system that influence ganglionic and post-ganglionic function (fig 2). The symptoms and signs of autonomic disease cover a wide spectrum (table 1) that vary depending upon the aetiology (tables 2 and 3). In some they are localised (table 4). Autonomic dis- ease can result in underactivity or overactivity. Sympathetic adrenergic failure causes orthostatic (postural) hypotension and in the male ejaculatory failure, while sympathetic cholinergic failure results in anhidrosis; parasympathetic failure causes dilated pupils, a fixed heart rate, a sluggish urinary bladder, an atonic large bowel and, in the male, erectile failure. With autonomic hyperac- tivity, the reverse occurs. In some disorders, particularly in neurally mediated syncope, there may be a combination of effects, with bradycardia caused by parasympathetic activity and hypotension resulting from withdrawal of sympathetic activity. The history is of particular importance in the consideration and recognition of autonomic disease, and in separating dysfunction that may result from non-autonomic disorders. CLINICAL FEATURES c copyright. General aspects Autonomic disease may present at any age group; at birth in familial dysautonomia (Riley-Day syndrome), in teenage years in vasovagal syncope, and between the ages of 30–50 years in familial amyloid polyneuropathy (FAP). -

Brainstem Dysfunction in Critically Ill Patients
Benghanem et al. Critical Care (2020) 24:5 https://doi.org/10.1186/s13054-019-2718-9 REVIEW Open Access Brainstem dysfunction in critically ill patients Sarah Benghanem1,2 , Aurélien Mazeraud3,4, Eric Azabou5, Vibol Chhor6, Cassia Righy Shinotsuka7,8, Jan Claassen9, Benjamin Rohaut1,9,10† and Tarek Sharshar3,4*† Abstract The brainstem conveys sensory and motor inputs between the spinal cord and the brain, and contains nuclei of the cranial nerves. It controls the sleep-wake cycle and vital functions via the ascending reticular activating system and the autonomic nuclei, respectively. Brainstem dysfunction may lead to sensory and motor deficits, cranial nerve palsies, impairment of consciousness, dysautonomia, and respiratory failure. The brainstem is prone to various primary and secondary insults, resulting in acute or chronic dysfunction. Of particular importance for characterizing brainstem dysfunction and identifying the underlying etiology are a detailed clinical examination, MRI, neurophysiologic tests such as brainstem auditory evoked potentials, and an analysis of the cerebrospinal fluid. Detection of brainstem dysfunction is challenging but of utmost importance in comatose and deeply sedated patients both to guide therapy and to support outcome prediction. In the present review, we summarize the neuroanatomy, clinical syndromes, and diagnostic techniques of critical illness-associated brainstem dysfunction for the critical care setting. Keywords: Brainstem dysfunction, Brain injured patients, Intensive care unit, Sedation, Brainstem -

The Autonomic Nervous System and Gastrointestinal Tract Disorders
NEUROMODULATION THE AUTONOMIC NERVOUS SYSTEM AND GASTROINTESTINALTRACT DISORDERS TERRY L. POWLEY, PH.D. PURDUE UNIVERSITY • MULTIPLE REFRACTORY GI DISORDERS EXIST. • VISCERAL ATLASES OF THE GI TRACT ARE AVAILABLE. • REMEDIATION WITH ELECTROMODULATION MAY BE PRACTICAL. TERRY l. POWLEY, PH.D. PURDUE NEUROMODUlATION: THE AUTONOMIC NERVOUS SYSTEM AND GASTP.OINTESTINAL TRACT DISORDERS UNIVERSITY 50 INTERNATIONAL I:"' NEUROMODULATION SOCIETY 0 40 ·IS 12TH WORLD CONGRESS -I: -• 30 !"' A. -..0 20 ..a• E 10 z::::t TERRY l. POWLEY, PH.D. PURDUE NEUROMODUlATION: THE AUTONOMIC NERVOUS SYSTEM AND GASTP.OINTESTINAL TRACT DISORDERS UNIVERSITY DISORDERS TO TREAT WITH NEUROMODULATION ACHALASIA DYSPHAGIA GASTROPARESIS GERD GUT DYSMOTILITY MEGA ESOPHAGUS DYSPEPSIA ,, VISCERAL PAIN l1 ' I NAUSEA, EMESIS OBESITY ,, ' 11 I PYLORIC STENOSIS ==..:.= --- "" .:.= --- .. _ _, DUMPING REFLUX COLITIS I:' . - IBS -·-- - CROHN'S DISEASE HIRSCHSPRUNG DISEASE CHAGAS DISUSE Gastrointestinal Tract Awodesk@ Ma;·a@ TERRY l. POWLEY, PH.D. PURDUE NEUROMODUlATION: THE AUTONOMIC NERVOUS SYSTEM AND GASTP.OINTESTINAL TRACT DISORDERS UNIVERSITY TIME The Obesity Epidemic in America ·. TERRY l. POWLEY, PH.D. PURDUE NEU ROMODUlATION : THE AUTO N OMIC NERVOUS SYSTEM A N D G A STP.OINTESTINAL TRACT DISORDERS UNI V E R SI TY ROUX-EN-Y BYPASS Bypassed portion of stomach Gastric -"'~ pouch Bypassed - Jejunum duodenum -1" food -___----_,,.,. digestivejuice TERRY l. POWLEY, PH.D. PURDUE NEU ROMODUlATION: THE AUTONOMIC NERVOUS SYSTEM A N D GASTP.OINTESTINAL TRACT DISORDERS UNIVERSITY 8y~s~ portionof i t()(l\3Ch • TERRYl. POWLEY, PH.D. PURDUE NEUROMOOUlATION: THE AUTONOMIC NERVOUS SYSTEM ANO 0.-STP.OINTESTINAL TRACT DISORDERS UHIVlflSITY • DESPERATE PATIENTS • ABSENCE OF SATISFACTORY PHARMACOLOGICAL TREATMENTS • POPULAR MEDIA HYPE • ABSENCE OF A SOLID MECHANISTIC UNDERSTANDING • UNCRITICAL ACCEPTANCE OF PROPONENT'S CLAIMS • MYOPIA REGARDING SIDE EFFECTS TERRY l. -

Dear Subscribers! This Issue of Our Magazine Is Devoted to Cooperation of Our Editorial Board with Ukrainian Medical Scientists
Deutscher Wissenschaftsherold • German Science Herald, N 4/2016 Dear subscribers! This issue of our magazine is devoted to cooperation of our editorial board with Ukrainian medical scientists. We present you the results of their researches. UDC: 611.831.1:611.216-018.73 Boichuk O.M. Higher State Educational Institution of Ukraine “Bukovinian State Medical University”, M.H. Turkevych Department of Human Anatomy, Chernivtsi, Ukraine, [email protected] Kryvetska I.I. Higher State Educational Institution of Ukraine “Bukovinian State Medical University”, S.M. Savenko Department of Neurology, Psychiatry and Medical Psychology Chernivtsi, Ukraine Bambuliak A.V. Higher State Educational Institution of Ukraine “Bukovinian State Medical University”, Department of Surgical and Pediatric Dentistry, Chernivtsi, Ukraine, [email protected] Sapunkov O.D. Higher State Educational Institution of Ukraine “Bukovinian State Medical University”, Department of Pediatric Surgery and Otolaryngology, Chernivtsi, Ukraine STRUCTURAL COMPONENTS OF AUTONOMIC INNERVATION OF MUCOSA OF NASAL CAVITY AND PARANASAL SINUSES Abstract. Autonomic innervation of mucosa of the nasal cavity and paranasal sinuses has been studied using complex morphological methods. It was determined that autonomic innervation of the nasal cavity and paranasal sinuses mostly occurs due to the branches of the pterygopalatine ganglion Keywords: nasal cavity, paranasal sinuses, innervation, pterygopalatine ganglion, mucosa, anatomy. Introduction. Mucosa of nasal cavity is peripheral element of olfactory analyzer functionally large receptor surface with a very consists of highly specialized epithelium of the complex and various reflex connections. It is upper nasal passage, short dendrites, which equipped with lots of blood and lymphatic ends with receptors, and axons form olfactory vessels, which are surrounded with numerous filaments that enter the olfactory bulb where nerve endings. -

Characterisation of Breathing and Associated Central Autonomic
Arch Dis Child 2001;85:29–37 29 Characterisation of breathing and associated Arch Dis Child: first published as 10.1136/adc.85.1.29 on 1 July 2001. Downloaded from central autonomic dysfunction in the Rett disorder P O O Julu, A M Kerr, F Apartopoulos, S Al-Rawas, I Witt Engerström, L Engerström, G A Jamal, S Hansen Abstract is associated with non-epileptic vacant spells.11 Aim—To investigate breathing rhythm Low resting cardiac vagal tone and weak vagal and brain stem autonomic control in response to hyperventilation and breath hold- patients with Rett disorder. ing suggest inadequate parasympathetic con- Setting—Two university teaching hospi- trol.12 tals in the United Kingdom and the Rett Our aim in this study was to characterise the Centre, Sweden. abnormalities of respiratory rhythm and inves- Patients—56 female patients with Rett tigate the central autonomic competence in disorder, aged 2–35 years; 11 controls aged Rett disorder. 5–28 years. Design—One hour recordings of breath- ing movement, blood pressure, ECG R-R Methods interval, heart rate, transcutaneous blood SUBJECTS Fifty six subjects were referred for diagnostic gases, cardiac vagal tone, and cardiac assessment. Control values came from 11 sensitivity to baroreflex measured on-line female volunteers and from previous with synchronous EEG and video. Breath- studies.12–14 Parents received written explana- ing rhythms were analysed in 47 cases. tions of procedures and results and provided Results—Respiratory rhythm was normal consent. The ethics committee at South during sleep and abnormal in the waking Glasgow University Hospitals NHS Trust state. -

Biology 251 Fall 2015 1 TOPIC 6: CENTRAL NERVOUS SYSTEM I
Biology 251 Fall 2015 TOPIC 6: CENTRAL NERVOUS SYSTEM I. Introduction to the Nervous System A. Objective: We’ve discussed mechanisms of how electrical signals are transmitted within a neuron (Topic 4), and how they are transmitted from neuron to neuron (Topic 5). For the next 3 Topics, we will discuss how neurons are organized into functioning units that allow you to think, walk, smell, feel pain, etc. B. Organization of nervous system. Note that this is a subdivision of a single integrated system, based on differences in structure, function and location (Fig 7.1). Such a subdivision allows easier analysis and understanding than trying to comprehend the system as a whole. 1. Central Nervous System (integrates and issues information) a) brain b) spinal cord 2. Peripheral Nervous System a) Afferent Division (sends information to CNS) b) Efferent Division (receives information from CNS) (1) Somatic nervous system (2) Autonomic nervous system (a) Sympathetic nervous system (b) Parasympathetic nervous system C. Three classes of neurons (Fig 7.4) 1. afferent neurons a) have sensory receptors b) axon terminals in CNS c) send information to CNS from body 2. efferent neurons a) cell body in CNS b) axon terminals in effector organ c) send information from CNS to body 3. interneurons a) lie within CNS b) some connect afferent neurons and efferent neurons (1) integrate peripheral responses and peripheral information c) some connect other interneurons (1) responsible for activity of the “mind”, i.e., thoughts, emotions, motivation, etc. d) 99% of all neurons are interneurons II. The Brain: Gross Structure and Associated Functions (Fig 9.11) A. -

The Sacral Autonomic Outflow Is Sympathetic
View metadata, citation and similar papers at core.ac.uk brought to you by CORE provided by UCL Discovery The sacral autonomic outflow is sympathetic Isabel Espinosa-Medina1,†, Orthis Saha1,†, Franck Boismoreau1, Zoubida Chettouh1, Francesca Rossi1, William D. Richardson2 and Jean-François Brunet1* 1 Institut de Biologie de l’ENS (IBENS), INSERM, CNRS, École Normale Supérieure, PSL Research University, Paris, 75005 France. 2 Wolfson Institute for Biomedical Research, University College London, London UK. †These authors contributed equally to this work *Correspondence to [email protected] 1 Abstract In the autonomic nervous system of mammals and birds, sacral preganglionic neurons are considered parasympathetic, as are their targets in the pelvic ganglia that prominently control rectal, bladder and genital functions. The allocation of the sacral autonomic outflow to the parasympathetic nervous system —i.e. as the second tier of a “cranio-sacral outflow”— has an ancient history: rooted in the work of Gaskell 1, formalized by Langley2 and universally accepted ever since (e.g. 3). The rationale lied in several perceived similarities between the sacral and cranial outflows: anatomical —separation from the thoracolumbar, sympathetic outflow by a gap at limb levels 1, a target territory less diffuse than that of the latter and a lack of projections to the paravertebral sympathetic chain 1; physiological —an influence on some organs opposite to that of the thoracolumbar outflow 4; and pharmacological — an overall sensitivity to muscarinic antagonists2. However, cell-phenotypic criteria have been lacking and were never sought. Here we uncover fifteen phenotypic and ontogenetic features that distinguish pre- and postganglionic neurons of the cranial parasympathetic outflow from those of the thoracolumbar sympathetic outflow. -

Sympathetic Tales: Subdivisons of the Autonomic Nervous System and the Impact of Developmental Studies Uwe Ernsberger* and Hermann Rohrer
Ernsberger and Rohrer Neural Development (2018) 13:20 https://doi.org/10.1186/s13064-018-0117-6 REVIEW Open Access Sympathetic tales: subdivisons of the autonomic nervous system and the impact of developmental studies Uwe Ernsberger* and Hermann Rohrer Abstract Remarkable progress in a range of biomedical disciplines has promoted the understanding of the cellular components of the autonomic nervous system and their differentiation during development to a critical level. Characterization of the gene expression fingerprints of individual neurons and identification of the key regulators of autonomic neuron differentiation enables us to comprehend the development of different sets of autonomic neurons. Their individual functional properties emerge as a consequence of differential gene expression initiated by the action of specific developmental regulators. In this review, we delineate the anatomical and physiological observations that led to the subdivision into sympathetic and parasympathetic domains and analyze how the recent molecular insights melt into and challenge the classical description of the autonomic nervous system. Keywords: Sympathetic, Parasympathetic, Transcription factor, Preganglionic, Postganglionic, Autonomic nervous system, Sacral, Pelvic ganglion, Heart Background interplay of nervous and hormonal control in particular The “great sympathetic”... “was the principal means of mediated by the sympathetic nervous system and the ad- bringing about the sympathies of the body”. With these renal gland in adapting the internal -

Influence of Inhalation/Exhalation Ratio and of Respiratory
sustainability Article Slow-Paced Breathing: Influence of Inhalation/Exhalation Ratio and of Respiratory Pauses on Cardiac Vagal Activity Sylvain Laborde 1,2,* , Maša Iskra 1, Nina Zammit 1, Uirassu Borges 1,3, Min You 4, Caroline Sevoz-Couche 5 and Fabrice Dosseville 6,7 1 Department of Performance Psychology, Institute of Psychology, German Sport University Cologne, Cologne 50933, Germany; [email protected] (M.I.); [email protected] (N.Z.) 2 UFR STAPS, EA 4260 CESAMS, Normandie Université, 14000 Caen, France 3 Department of Health & Social Psychology, Institute of Psychology, German Sport University Cologne, 50933 Cologne, Germany; [email protected] 4 UFR Psychologie, EA3918 CERREV, Normandie Université, 14000 Caen, France; [email protected] 5 INSERM, Unité Mixte de Recherche (UMR) S1158 Neurophysiologie Respiratoire Expérimentale et Clinique, Sorbonne Université, 75000 Paris, France; [email protected] 6 UMR-S 1075 COMETE, Normandie Université, 14000 Caen, France 7 INSERM, UMR-S 1075 COMETE, 14000 Caen, France; [email protected] * Correspondence: [email protected]; Tel.: +49-221-49-82-57-01 Abstract: Slow-paced breathing has been shown to enhance the self-regulation abilities of athletes via its influence on cardiac vagal activity. However, the role of certain respiratory parameters (i.e., inhalation/exhalation ratio and presence of a respiratory pause between respiratory phases) still needs to be clarified. The aim of this experiment was to investigate the influence of these respiratory Citation: Laborde, S.; Iskra, M.; parameters on the effects of slow-paced breathing on cardiac vagal activity. A total of 64 athletes Zammit, N.; Borges, U.; You, M.; (27 female; Mage = 22, age range = 18–30 years old) participated in a within-subject experimental Sevoz-Couche, C.; Dosseville, F.