A Pilot Investigation Into Brain-Computer Interface Use During a Lucid Dream
Total Page:16
File Type:pdf, Size:1020Kb
Load more
Recommended publications
-

Participant Guide
Participant Guide Get Enough Sleep Session Focus Getting enough sleep can help you prevent or delay type 2 diabetes. This session we will talk about: z Why sleep matters z Some challenges of getting enough sleep and ways to cope with them You will also make a new action plan! Tips: ✓ Go to bed and get up at the same time each day. This helps your body get on a schedule. ✓ Follow a bedtime routine that helps you wind down. Participant Guide: Get Enough Sleep 2 Jenny’s Story Jenny is at risk for type 2 diabetes. Her doctor asks her if she gets at least 7 hours of sleep each night. Jenny laughs. “Are you serious?” she asks. “I’m lucky if I get 5 hours.” Jenny usually doesn’t have much trouble falling asleep. But she often has to use the bathroom in the early morning. This gets her thinking about all the things she needs to do the next day. Plus, her husband’s breathing is loud. Both of these things make it hard for Jenny to fall back to sleep. She often lies awake for hours. These days, Jenny drinks less water and avoids caffeine in the evening. She makes a list of things to do the next day. Then she sets it aside. Jenny rarely needs to get up to use the bathroom during the night. If she does, she breathes deeply to help her get back to sleep. She also runs a fan to cover up the sound of her husband’s breathing. Jenny is closer to getting 7 hours of sleep a night. -

Sleep Apnea Sleep Apnea
Health and Safety Guidelines 1 Sleep Apnea Sleep Apnea Normally while sleeping, air is moved at a regular rhythm through the throat and in and out the lungs. When someone has sleep apnea, air movement becomes decreased or stops altogether. Sleep apnea can affect long term health. Types of sleep apnea: 1. Obstructive sleep apnea (narrowing or closure of the throat during sleep) which is seen most commonly, and, 2. Central sleep apnea (the brain is causing a change in breathing control and rhythm) Obstructive sleep apnea (OSA) About 25% of all adults are at risk for sleep apnea of some degree. Men are more commonly affected than women. Other risk factors include: 1. Middle and older age 2. Being overweight 3. Having a small mouth and throat Down syndrome Because of soft tissue and skeletal alterations that lead to upper airway obstruction, people with Down syndrome have an increased risk of obstructive sleep apnea. Statistics show that obstructive sleep apnea occurs in at least 30 to 75% of people with Down syndrome, including those who are not obese. In over half of person’s with Down syndrome whose parents reported no sleep problems, sleep studies showed abnormal results. Sleep apnea causing lowered oxygen levels often contributes to mental impairment. How does obstructive sleep apnea occur? The throat is surrounded by muscles that are active controlling the airway during talking, swallowing and breathing. During sleep, these muscles are much less active. They can fall back into the throat, causing narrowing. In most people this doesn’t affect breathing. However in some the narrowing can cause snoring. -

Towards a Passive BCI to Induce Lucid Dream Morgane Hamon, Emma Chabani, Philippe Giraudeau
Towards a Passive BCI to Induce Lucid Dream Morgane Hamon, Emma Chabani, Philippe Giraudeau To cite this version: Morgane Hamon, Emma Chabani, Philippe Giraudeau. Towards a Passive BCI to Induce Lucid Dream. Journée Jeunes Chercheurs en Interfaces Cerveau-Ordinateur et Neurofeedback 2019 (JJC- ICON ’19), Mar 2019, Villeneuve d’Ascq, France. hal-02108903 HAL Id: hal-02108903 https://hal.archives-ouvertes.fr/hal-02108903 Submitted on 29 Apr 2019 HAL is a multi-disciplinary open access L’archive ouverte pluridisciplinaire HAL, est archive for the deposit and dissemination of sci- destinée au dépôt et à la diffusion de documents entific research documents, whether they are pub- scientifiques de niveau recherche, publiés ou non, lished or not. The documents may come from émanant des établissements d’enseignement et de teaching and research institutions in France or recherche français ou étrangers, des laboratoires abroad, or from public or private research centers. publics ou privés. TOWARDS A PASSIVE BCI TO INDUCE LUCID DREAM JJC-ICON ’19 Morgane Hamon Emma Chabani Philippe Giraudeau Ullo Institut du Cerveau et de la Moelle épinière Inria La Rochelle, France Paris, France Bordeaux, France [email protected] [email protected] [email protected] April 29, 2019 ABSTRACT Lucid dreaming (LD) is a phenomenon during which the person is aware that he/she dreaming and is able to control the dream content. Studies have shown that only 20% of people can experience lucid dreams on a regular basis. However, LD frequency can be increased through induction techniques. External stimulation technique relies on the ability to integrate external information into the dream content. -

Obstructive Sleep Apnea in Adults? NORMAL AIRWAY OBSTRUCTED AIRWAY
American Thoracic Society PATIENT EDUCATION | INFORMATION SERIES What Is Obstructive Sleep Apnea in Adults? NORMAL AIRWAY OBSTRUCTED AIRWAY Obstructive sleep apnea (OSA) is a common problem that affects a person’s breathing during sleep. A person with OSA has times during sleep in which air cannot flow normally into the lungs. The block in CPAP DEVICE airflow (obstruction) is usually caused by the collapse of the soft tissues in the back of the throat (upper airway) and tongue during sleep. Apnea means not breathing. In OSA, you may stop ■■ Gasping breathing for short periods of time. Even when you are or choking trying to breathe, there may be little or no airflow into sounds. the lungs. These pauses in airflow (obstructive apneas) ■■ Breathing pauses observed by someone watching can occur off and on during sleep, and cause you to you sleep. wake up from a sound sleep. Frequent apneas can cause ■■ Sudden or jerky body movements. many problems. With time, if not treated, serious health ■■ Restless tossing and turning. problems may develop. ■■ Frequent awakenings from sleep. OSA is more common in men, women after menopause CLIP AND COPY AND CLIP Common symptoms you may have while awake: and people who are over the age of 65. OSA can also ■■ Wake up feeling like you have not had enough sleep, occur in children. Also see ATS Patient Information Series even after sleeping many hours. fact sheet on OSA in Children. People who are at higher ■■ Morning headache. risk of developing sleep apnea include those with: ■■ Dry or sore throat in the morning from breathing ■■ enlarged tonsils and/or adenoids through your mouth during sleep. -

Sleep Self-Care
University of California, Berkeley 2222 Bancroft Way Berkeley, CA 94720 SLEEP SELF-CARE All of us have trouble sleeping from time to time. This is perfectly normal. Sleep problems (also known as insomnia) are often triggered by sudden life changes that lead to increased stress. For instance, following the death of a loved one, a car accident or a promotion to a new job, many people experience difficulties getting a good night’s sleep. This normal response to stress usually lasts for a short time, rarely longer than a week or two. However, some people have chronic problems sleeping which do not seem to go away. If you are one of these people, or you are having temporary insomnia, this Self-Care Guide should help. It will give you some general information about sleep, as well as provide a number of helpful suggestions to aid those with sleep problems. Read it carefully, as many common sleep problems are caused by one’s own habits, and by adopting some of the following sleep-promoting behaviors, most people can get a good night’s rest without the aid of drugs. Taking sleeping pills is not the answer! For people whose only complaint is I can’t sleep well or I can’t get to sleep easily, taking sleeping pills may do more harm than good. Most authorities recommend against the regular use of sedative drugs (like Valium, Dalmane, Librium and barbiturates) for the following reasons: ! Sedatives change nervous system activities during sleep; for example, they may reduce the normal periods of dreaming. -
Brain Computer Interface for Sleep Apnea Detection
Special Issue - 2020 International Journal of Engineering Research & Technology (IJERT) ISSN: 2278-0181 NCAIT - 2020 Conference Proceedings Brain Computer Interface for Sleep Apnea Detection Poorvitha H R1, Aishwarya K Gowda2, Kavya K B2, Nayana R2 Vivekananda Institute of Technology Gudimavu, Kumbalagodu Post, Kengeri Hobli, Bengaluru – 560 074 Abstract - A brain-computer interface (BCI) is the varied phases of sleep and may be a crucial step in a interface method that someone to deliver instructions and shot to assist doctor within the designation and medical messages to a automated gadget, via way of means of care of connected sleep obstruction. using person mind activity. An electroencephalogram (EEG), mounted BCI became related with a synthetic gadget to command a home automation application. It provides an alternative to built-in interface and control. It is a digital surroundings shape that enters the body’s everyday prepared pathways, which might be neuromuscular output passage. Sleep apnea is personification of sickness which occurs during sleep, which impacts the human fitness via way of means of blockage in respiratory for positive period of time. The prognosis is critical that's viable via way of means of the perceiving of apnea episodes the use of electroencephalogram (EEG) reports. EEG is an adjustable decomposition for the identifying of apnea events using EEG signals. EEG plays an essential role in identifying the sleep apnea by recognizing and producing the brain neurons activities. The EEG sign dataset is filtered, the purified EEG sign is subjected for sub-band separation and 5 frequency bands inclusive of Gamma, Beta, Alpha, Theta, and Delta. -

What%Is%Idiopathic%Hypersomnia?%
What%is%Idiopathic%Hypersomnia?% Idiopathic*hypersomnia*is*sleeping*too*much*(hypersomnia)*without*an*obvious*cause.*It*is*different* from*narcolepsy,*because*idiopathic*hypersomnia*does*not*involve*suddenly*falling*asleep*or*losing* muscle*control*due*to*strong*emotions*(cataplexy).* Causes* The*usual*approach*is*to*consider*other*potential*causes*of*excessive*daytime*sleepiness.* Other*sleep*disorders*that*may*cause*daytime*sleepiness*include:* •Isolated*sleep*paralysis* •Narcolepsy* •Obstructive*sleep*apnea* •Restless*leg*syndrome* Other*causes*of*excessive*sleepiness*include:* •Atypical*depression* •Certain*medications* •Drug*and*alcohol*use* •Low*thyroid*function*(hypothyroidism)* •Previous*head*injury* Symptoms* Symptoms*often*develop*slowly*during*adolescence*or*young*adulthood.*They*include:* •Daytime*naps*that*do*not*relieve*drowsiness* •Difficulty*waking*from*a*long*sleep*KK*may*feel*confused*or*disoriented* •Increased*need*for*sleep*during*the*day*KK*even*while*at*work,*or*during*a*meal*or*conversation* •Increased*sleep*time*KK*up*to*14*K*18*hours*per*day* Other*symptoms*may*include:* •Anxiety* •Feeling*irritated* •Loss*of*appetite* •Low*energy* •Restlessness* •Slow*thinking*or*speech* •Trouble*remembering* Cataplexy*KK*suddenly*falling*asleep*or*losing*muscle*control*KK*which*is*part*of*narcolepsy,*is*NOT*a* symptom*of*idiopathic*hypersomnia.* Exams*and*Tests* The*health*care*provider*will*take*a*detailed*sleep*history.*Tests*may*include:* •MultipleKsleep*latency*test* •Sleep*study*(polysomnography,*to*identify*other*sleep*disorders)* -

Insomnia-1111 30/11/11 4:37 PM Page 1
SHF-Insomnia-1111 30/11/11 4:37 PM Page 1 Insomnia Important Things to Know About Insomnia • Around 1 in 3 people have at least mild insomnia. • Many poor sleepers have developed poor sleep habits. • For specialist help, cognitive behavioural therapy for insomnia is best • In the long run, taking sleeping pills isn’t effective. • There are sleep specialists, clinics and on-line programs that can help. What is insomnia? How common is insomnia? Insomnia is said to be present when you regularly find it Most people have experience insomnia symptoms at hard to fall asleep or stay asleep. It has several patterns. some time of their lives. At any given time around 10% You may have trouble getting to sleep initially. Or even if of people have at least mild insomnia. you can fall asleep, you might not be able to stay asleep for as long as you would like. Also you may wake up Who is at risk? during the night and not be able to go back to sleep for a long time. Many people have two of the above problems, Older people with poor health have a higher risk. Also or even all three. Because of these, you might feel tired women have twice the rates compared to men. This may during the day. be related to higher rates of anxiety and depression, which can be associated with insomnia. Shift workers What causes insomnia? have a higher risk too. Insomnia has many causes which can include: How does it affect people? • Some medicines and drugs, e.g. -

Non-24-Hour Sleep-Wake Disorder Revisited – a Case Study
CASE REPORT published: 29 February 2016 doi: 10.3389/fneur.2016.00017 Non-24-Hour Sleep-Wake Disorder Revisited – a Case study Corrado Garbazza1,2† , Vivien Bromundt3† , Anne Eckert2,4 , Daniel P. Brunner5 , Fides Meier2,4 , Sandra Hackethal6 and Christian Cajochen1,2* 1 Centre for Chronobiology, Psychiatric Hospital of the University of Basel, Basel, Switzerland, 2 Transfaculty Research Platform Molecular and Cognitive Neurosciences, University of Basel, Basel, Switzerland, 3 Sleep-Wake-Epilepsy-Centre, Department of Neurology, Inselspital, Bern University Hospital, Bern, Switzerland, 4 Neurobiology Laboratory for Brain Aging and Mental Health, Psychiatric Hospital of the University of Basel, Basel, Switzerland, 5 Center for Sleep Medicine, Hirslanden Clinic Zurich, Zurich, Switzerland, 6 Charité – Universitaetsmedizin Berlin, Berlin, Germany The human sleep-wake cycle is governed by two major factors: a homeostatic hourglass process (process S), which rises linearly during the day, and a circadian process C, which determines the timing of sleep in a ~24-h rhythm in accordance to the external Edited by: Ahmed S. BaHammam, light–dark (LD) cycle. While both individual processes are fairly well characterized, the King Saud University, Saudi Arabia exact nature of their interaction remains unclear. The circadian rhythm is generated by Reviewed by: the suprachiasmatic nucleus (“master clock”) of the anterior hypothalamus, through Axel Steiger, cell-autonomous feedback loops of DNA transcription and translation. While the phase Max Planck Institute of Psychiatry, Germany length (tau) of the cycle is relatively stable and genetically determined, the phase of Timo Partonen, the clock is reset by external stimuli (“zeitgebers”), the most important being the LD National Institute for Health and Welfare, Finland cycle. -

Adult NREM Parasomnias: an Update
Review Adult NREM Parasomnias: An Update Maria Hrozanova 1, Ian Morrison 2 and Renata L Riha 3,* 1 Department of Neuromedicine and Movement Science, Norwegian University of Science and Technology, N-7491 Trondheim, Norway; [email protected] 2 Department of Neurology, Ninewells Hospital and Medical School, DD1 9SY Dundee, UK; [email protected] 3 Department of Sleep Medicine, Royal Infirmary of Edinburgh, EH16 4SA Edinburgh, UK * Correspondence: [email protected] or [email protected]; Tel.: +44-013-242-3872 Received: 23 August 2018; Accepted: 15 November 2018; Published: 23 November 2018 Abstract: Our understanding of non-rapid eye movement (NREM) parasomnias has improved considerably over the last two decades, with research that characterises and explores the causes of these disorders. However, our understanding is far from complete. The aim of this paper is to provide an updated review focusing on adult NREM parasomnias and highlighting new areas in NREM parasomnia research from the recent literature. We outline the prevalence, clinical characteristics, role of onset, pathophysiology, role of predisposing, priming and precipitating factors, diagnostic criteria, treatment options and medico-legal implications of adult NREM parasomnias. Keywords: NREM parasomnias; slow-wave sleep disorders; parasomnias; adult; arousal disorders; review 1. Introduction Non-rapid eye movement (NREM) parasomnias constitute a category of sleep disorders characterised by abnormal behaviours and physiological events primarily arising from N3sleep [1–3] and occuring outside of conscious awareness. Due to their specific association with slow wave sleep (SWS), NREM parasomnias are also termed ‘SWS disorders’. Behaviours such as confusional arousals, sleepwalking, sleep eating (also called sleep-related eating disorder, or SRED), night terrors, sexualised behaviour in sleep (also called sexsomnia) and sleep-related violence are NREM parasomnias that arise from N3 sleep. -

Daily Sleep Diary
Daily Sleep Diary Complete the diary each morning (“Day 1” will be your first morning). Don’t worry too much about giving exact answers, an estimate will do. Your Name___________________________ The date of Day 1_______________ Day 1 Day 2 Day 3 Day 4 Day 5 Day 6 Day 7 Enter the Weekday (Mon, Tues, Wed, etc.) At what time did you go to 1 bed last night? After settling down, how long did it take you to fall 2 asleep? After falling asleep, about how many times did you 3 wake up in the night? After falling asleep, for how long were you awake during 4 the night in total? At what time did you finally 5 wake up? At what time did you get 6 up? How long did you spend in bed last night (from first 7 getting in, to finally getting up) How would you rate the quality of your sleep last night? 8 1 2 3 4 5 V. Poor V. Good 10 Rules for Improved Sleep Hygiene If you have problems sleeping, then it is important that you practise good Sleep Hygiene. This means doing things which are known to improve sleep, and avoiding those things which are known to disturb sleep. Here are 10 things you should know about getting better sleep; each of these points is based on scientific research, and could help you to get the most out of your sleep. Remember, this advice applies only if you have a sleep problem: Products containing caffeine (tea, coffee, cocoa, chocolate, soft drinks, etc.) 1 should be discontinued at least 4 hours before bedtime. -
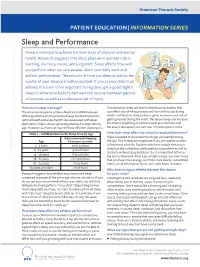
Sleep and Performance
American Thoracic Society PATIENT EDUCATION | INFORMATION SERIES Sleep and Performance Sleep is essential to achieve the best state of physical and mental health. Research suggests that sleep plays an important role in learning, memory, mood, and judgment. Sleep affects how well you perform when you are awake—both your daily work and athletic performance. The amount of time you sleep as well as the quality of your sleep are both important. If you or your child is an athlete, it is even more important to regularly get a good night’s sleep to allow your body to rest well and recover between periods of exercise, as well as to decrease risk of injury. How much sleep is enough? Constant poor sleep can lead to depression or anxiety that The American Academy of Sleep Medicine (AASM) released can affect your drive to practice and how well you do during official guidelines on the amount of sleep needed to promote events. Getting less sleep before a game increases your risk of optimal health and avoid health risks associated with sleep getting injured during the event. Decreased sleep can increase deprivation. Table 1 shows general guidelines for sleep time by the chance of getting an infection such as a common cold age. However, each person may still have different sleep needs. because it decreases how well your immune system works. Table 1 – AASM Guidelines for Sleep Time by Age How does sleep affect my school or work performance? Recommended sleeping Sleep is needed to remember the things you learned during Age hours per 24 hours the day.