Dermatology Usmleworld Notes
Total Page:16
File Type:pdf, Size:1020Kb
Load more
Recommended publications
-
Pediatrics-EOR-Outline.Pdf
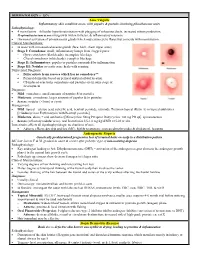
DERMATOLOGY – 15% Acne Vulgaris Inflammatory skin condition assoc. with papules & pustules involving pilosebaceous units Pathophysiology: • 4 main factors – follicular hyperkeratinization with plugging of sebaceous ducts, increased sebum production, Propionibacterium acnes overgrowth within follicles, & inflammatory response • Hormonal activation of pilosebaceous glands which may cause cyclic flares that coincide with menstruation Clinical Manifestations: • In areas with increased sebaceous glands (face, back, chest, upper arms) • Stage I: Comedones: small, inflammatory bumps from clogged pores - Open comedones (blackheads): incomplete blockage - Closed comedones (whiteheads): complete blockage • Stage II: Inflammatory: papules or pustules surrounded by inflammation • Stage III: Nodular or cystic acne: heals with scarring Differential Diagnosis: • Differentiate from rosacea which has no comedones** • Perioral dermatitis based on perioral and periorbital location • CS-induced acne lacks comedones and pustules are in same stage of development Diagnosis: • Mild: comedones, small amounts of papules &/or pustules • Moderate: comedones, larger amounts of papules &/or pustules • Severe: nodular (>5mm) or cystic Management: • Mild: topical – azelaic acid, salicylic acid, benzoyl peroxide, retinoids, Tretinoin topical (Retin A) or topical antibiotics [Clindamycin or Erythromycin with Benzoyl peroxide] • Moderate: above + oral antibiotics [Minocycline 50mg PO qd or Doxycycline 100 mg PO qd], spironolactone • Severe (refractory nodular acne): oral -

15. Dermatology Eponyms
Dermatology Eponyms DERMATOLOGY EPONYMS – PHENOMEN / SIGN – LEXICON (D) Brzeziński Piotr1, Wollina Uwe2, Poklękowska Katarzyna3, Khamesipour Ali4, Herrero Gonzalez Jose Eugenio5, Bimbi Cesar6, Di Lernia Vito7, Karwan Krzysztof 8 16th Military Support Unit, Ustka, Poland. [email protected] 2Department of Dermatology & Allergology, Hospital Dresden-Friedrichstadt, Academic Teaching Hospital of the Technical University of Dresden, Dresden, Germany [email protected] 3Mazowiecki Branch of the National Health Fund, Warsaw, Poland [email protected] 4Center for Research and Training in Skin Diseases and Leprosy, Tehran University of Medical Sciences, Tehran, Iran [email protected] 5Malalties Ampul.lars i Porfíries, Departament de Dermatologia, Hospital del Mar, Barcelona, Spain [email protected] 6Brazilian Society of Dermatology [email protected] 7Department of Dermatology, Arcispedale Santa Maria Nuova, Reggio Emilia, Italy [email protected] 8The Emergency Department, Military Institute of Medicine, Warsaw, Poland [email protected] N Dermatol Online. 2011; 2(3): 158-170 Date of submission: 08.04.2011 / acceptance: 29.05.2011 Conflicts of interest: None DANIELSSEN’S SIGN Anesthetic leprosy. A form of leprosy chiefly affecting the nerves, marked by hyperesthesia succeeded by anesthesia, and by paralysis, ulceration, and various trophic disturbances, terminating in gangrene and mutilation. In 1895 I presented to the Ohio State Medical Society two sisters, natives of Ohio, who manifested appearances of anesthetic leprosy. Synonyms: Danielssen disease, Danielssen-Boeck disease, dry leprosy, trophoneurotic leprosy. OBJAW DANIELSSENA Anesthetic leprosy. Postać trądu głównie wpływająca na nerwy, początkowo charakteryzuje się oznaczone przeczulicą, następcą znieczulicą i paraliŜem, owrzodzeniem i róŜnymi zaburzeniami troficznymi, kończąca się w gangreną i okaleczeniem. W 1895 roku przedstawiono w Ohio State Medical Society dwie siostry z Ohio, u których występowały objawy anesthetic Figure 1. -

Clinical Dermatology Notice
This page intentionally left blank Clinical Dermatology Notice Medicine is an ever-changing science. As new research and clinical experience broaden our knowledge, changes in treatment and drug therapy are required. The editors and the publisher of this work have checked with sources believed to be reliable in their efforts to provide information that is complete and generally in accord with the standards accepted at the time of publication. However, in view of the possibility of human error or changes in medical sciences, neither the editors nor the publisher nor any other party who has been involved in the preparation or publication of this work warrants that the information contained herein is in every respect accurate or complete, and they disclaim all responsibility for any errors or omissions or for the results obtained from use of such information contained in this work. Readers are encouraged to confirm the information contained herein with other sources. For example and in particular, readers are advised to check the product information sheet included in the package of each drug they plan to administer to be certain that the information contained in this work is accurate and that changes have not been made in the recommended dose or in the contraindications for administration. This recommendation is of particular importance in connection with new or infrequently used drugs. a LANGE medical book Clinical Dermatology Carol Soutor, MD Clinical Professor Department of Dermatology University of Minnesota Medical School Minneapolis, Minnesota Maria K. Hordinsky, MD Chair and Professor Department of Dermatology University of Minnesota Medical School Minneapolis, Minnesota New York Chicago San Francisco Lisbon London Madrid Mexico City Milan New Delhi San Juan Seoul Singapore Sydney Toronto Copyright © 2013 by McGraw-Hill Education, LLC. -

A ABCD, 19, 142, 152 ABCDE, 19, 142 Abramowitz Sign, 3, 5
Index A Atopic dermatitis, 2, 18, 19, 20, 30, ABCD, 19, 142, 152 61, 81, 82, 84, 86, 99 ABCDE, 19, 142 Atrophie blanche, 173, 177 Abramowitz sign, 3, 5 Atrophy, crinkling, 143, 160 Acanthosis nigricans, 105, 106, 132 Atypical nevus, 144, 145, 163, 164 Addison disease (primary adrenal eclipse, 144, 164 insufficiency), 137 ugly duckling, 144, 163 Albright (McCune–Albright Auspitz sign, 3, 5, 6, 18, 104 syndrome), 83, 93 All in different stages, 33, 34, 40 All in same stage, 33, 34, 38 B Alopecia, 57, 77, 94, 105, 106, 111, Bamboo hair, 84, 99, 171, 172 117, 119, 127, 133, 171, 172, Basal cell carcinoma, 17, 104, 140, 182, 184 151, 162, 170 Alopecia areata, 105, 106, 127, 171 Bioterrorism, 33, 38 Amyloid, 107, 119 Black dot (tinea capitis), 37, 57 Angiofibroma, 89 Blue angel (see Tumors, painful) Angiokeratoma, 3, 79, 81, 85 Blue rubber bleb nevus, 144, Angiolipoma, 142, 155 154, 168 Angioma, spider, 107, 109, 134 angiolipioma, 142, 155 Angiomatosis, leptomeningeal, 90 neurilemmoma, 142, 156 Anticoagulant, lupus, 108, 121 glomus tumor, 142, 157 Antiphospholipid syndrome eccrine spiradenoma, 142, 158 (APLS), 19, 107, 108, 121 leiomyoma, 142, 159 Apocrine hidrocystoma, 144, Blue cyst (apocrine hidrocystoma), 166, 168 144, 166, 168 Apple jelly, 36, 37, 47 Blue nose (purpura fulminans), 19, Ash leaf macule (confetti macule), 108, 122 82, 89 Blue papule (blue nevus), 1, 144, Asymmetry, 19, 118, 136, 152 166, 167, 168 187 188 Index Blue rubber bleb nevus, 144, 154, 168 Coast of California, 82, 83, 91 Border Coast of Maine, 83, 93 irregular, 83, -
Dermatological Indications of Disease - Part II This Patient on Dialysis Is Showing: A
“Cutaneous Manifestations of Disease” ACOI - Las Vegas FR Darrow, DO, MACOI Burrell College of Osteopathic Medicine This 56 year old man has a history of headaches, jaw claudication and recent onset of blindness in his left eye. Sed rate is 110. He has: A. Ergot poisoning. B. Cholesterol emboli. C. Temporal arteritis. D. Scleroderma. E. Mucormycosis. Varicella associated. GCA complex = Cranial arteritis; Aortic arch syndrome; Fever/wasting syndrome (FUO); Polymyalgia rheumatica. This patient missed his vaccine due at age: A. 45 B. 50 C. 55 D. 60 E. 65 He must see a (an): A. neurologist. B. opthalmologist. C. cardiologist. D. gastroenterologist. E. surgeon. Medscape This 60 y/o male patient would most likely have which of the following as a pathogen? A. Pseudomonas B. Group B streptococcus* C. Listeria D. Pneumococcus E. Staphylococcus epidermidis This skin condition, erysipelas, may rarely lead to septicemia, thrombophlebitis, septic arthritis, osteomyelitis, and endocarditis. Involves the lymphatics with scarring and chronic lymphedema. *more likely pyogenes/beta hemolytic Streptococcus This patient is susceptible to: A. psoriasis. B. rheumatic fever. C. vasculitis. D. Celiac disease E. membranoproliferative glomerulonephritis. Also susceptible to PSGN and scarlet fever and reactive arthritis. Culture if MRSA suspected. This patient has antithyroid antibodies. This is: • A. alopecia areata. • B. psoriasis. • C. tinea. • D. lichen planus. • E. syphilis. Search for Hashimoto’s or Addison’s or other B8, Q2, Q3, DRB1, DR3, DR4, DR8 diseases. This patient who works in the electronics industry presents with paresthesias, abdominal pain, fingernail changes, and the below findings. He may well have poisoning from : A. lead. B. -

B K B Ld I MD Brooke Baldwin, MD Private Practice, Lutz, Florida Chief
BBkrooke BBldialdwin, MD Private Practice, Lutz, Florida Chief of Dermatology James A Haley VA Hospital Adjunct Assistant Professor of Dermatology University of Florida What we are going to cover today Dermatologic Emergencies Common benign skin growths Malignant skin tumors Common Rashes Photoprotecti on and CiCosmetics Dermatologic Emergencies Erythroderma PlPustular psoriiiasis Pemphigus DRESS Syndrome SJS / TEN EEthdrythroderma Erythroderma Generalized redness and scaling of skin involving >90% BSA Systemic manifestations PihPeripheral edema & ffilacial edema Tachycardia Loss of fluids and proteins Disturbed thermoregulation Most common etiologies Atopic dermatitis, psoriasis, CTCL, drug reactions Despite intensive evaluation, the cause remains unknown in 25‐30% PPlustular psoriiiasis Pustular Psoriasis Generalized pustular psoriasis Unusual mani festation o f psoriasis Triggering factors Pregnancy (impetigo herpetiformis) Tapering of corticosteroids (Von Zumbusch reaction) HliHypocalcemia Infections Topical irritants Rarely treatment with TNF alpha blockers (palms and soles) Pemphigus Group of chronic autoimmune blistering diseases presenting with painful erosions IgG Autoantibodies are directed against the cell surface of keratinocytes Results in blistering in varying areas of the epidermis Diagnosi s is confirmed wihith direct iflimmunofluorescence on skin biopsy 3 ma jor forms P. vulgaris, P. foliaceus, paraneoplastic Do not confuse with Bullous pemphigoid which presents with tense bullae Pempgphigus -

Dermatology Grand Rounds 2019 Skin Signs of Internal Disease
Dermatology Grand Rounds 2019 skin signs of internal disease John Strasswimmer, MD, PhD Affiliate Clinical Professor (Dermatology), FAU College of Medicine Research Professor of Biochemistry, FAU College of Science Associate Clinical Professor, U. Miami Miller School of Medicine Dermatologist and Internal Medicine “Normal” abnormal skin findings in internal disease • Thyroid • Renal insufficiency • Diabetes “Abnormal” skin findings as clue to internal disease • Markers of infectious disease • Markers of internal malignancy risk “Consultation Cases” • Very large dermatology finding • A very tiny dermatology finding Dermatologist and Internal Medicine The "Red and Scaly” patient “Big and Small” red rashes not to miss The "Red and Scaly” patient • 29 Year old man with two year pruritic eruption • PMHx: • seasonal allergies • childhood eczema • no medications Erythroderma Erythroderma • Also called “exfoliative dermatitis” • Not stevens-Johnson / toxic epidermal necrosis ( More sudden onset, associated with target lesions, mucosal) • Generalized erythema and scale >80-90% of body surface • May be associated with telogen effluvium It is not a diagnosis per se Erythroderma Erythroderma Work up 1) Exam for pertinent positives and negatives: • lymphadenopathy • primary skin lesions (i.e. nail pits of psoriasis) • mucosal involvement • Hepatosplenomagaly 2) laboratory • Chem 7, LFT, CBC • HIV • Multiple biopsies over time 3) review of medications 4) age-appropriate malignancy screening 5) evaluate hemodynamic stability Erythroderma Management 1) -

Comparative Study of Halobetasol and Tacrolimus in Treatment of Lichen Planus
COMPARATIVE STUDY OF HALOBETASOL AND TACROLIMUS IN TREATMENT OF LICHEN PLANUS Dissertation Submitted in fulfillment of the university regulations for MD DEGREE IN DERMATOLOGY, VENEREOLOGY AND LEPROSY (BRANCH XII A) Madras Medical College Chennai THE TAMILNADU DR.M.G.R.MEDICAL UNIVERSITY CHENNAI APRIL 2011 CERTIFICATE Certified that this dissertation entitled “COMPARATIVE STUDY OF HALOBETASOL AND TACROLIMUS IN TREATMENT OF LICHEN PLANUS ” is a bonafide work done by Dr.VIDHYA RAVINDRAN, Post Graduate Student of the Department of Dermatology, Venereology and Leprosy, Madras Medical College, Chennai – 600 003, during the academic year 2008 – 2011. This work has not previously formed the basis for the award of any degree. Prof.Dr.D.PRABHAVATHY, MD.DD, Professor and Head of the Department, Department of Dermatology and Leprology, Madras Medical College, Chennai-600003. Prof. Dr. J.MOHANASUNDARAM, M.D.Ph.D, DNB., Dean, Madras Medical College, Chennai-600003 SPECIAL ACKNOWLEDGEMENT My sincere thanks to Prof. Dr.J.MOHANASUNDARAM, M.D ., PhD,DNB Dean, Madras Medical College for allowing me to do this dissertation and utilize the institutional facilities. ACKNOWLEDGEMENT This study which has been an integral part of my stay in the Department of Dermatology, Madras Medical College, Chennai wouldn’t have been completed without the help of great number of people. It gives me great pleasure in thanking them in the beginning. In the first place, I express my sincere gratitude to Prof. Dr.D.PRABHAVATHY, M.D.,D.D., Professor and Head, Department of Dermatology and Leprology and my co-ordinator for her invaluable guidance, motivation and help throughout the study. -

Mallory Prelims 27/1/05 1:16 Pm Page I
Mallory Prelims 27/1/05 1:16 pm Page i Illustrated Manual of Pediatric Dermatology Mallory Prelims 27/1/05 1:16 pm Page ii Mallory Prelims 27/1/05 1:16 pm Page iii Illustrated Manual of Pediatric Dermatology Diagnosis and Management Susan Bayliss Mallory MD Professor of Internal Medicine/Division of Dermatology and Department of Pediatrics Washington University School of Medicine Director, Pediatric Dermatology St. Louis Children’s Hospital St. Louis, Missouri, USA Alanna Bree MD St. Louis University Director, Pediatric Dermatology Cardinal Glennon Children’s Hospital St. Louis, Missouri, USA Peggy Chern MD Department of Internal Medicine/Division of Dermatology and Department of Pediatrics Washington University School of Medicine St. Louis, Missouri, USA Mallory Prelims 27/1/05 1:16 pm Page iv © 2005 Taylor & Francis, an imprint of the Taylor & Francis Group First published in the United Kingdom in 2005 by Taylor & Francis, an imprint of the Taylor & Francis Group, 2 Park Square, Milton Park Abingdon, Oxon OX14 4RN, UK Tel: +44 (0) 20 7017 6000 Fax: +44 (0) 20 7017 6699 Website: www.tandf.co.uk All rights reserved. No part of this publication may be reproduced, stored in a retrieval system, or transmitted, in any form or by any means, electronic, mechanical, photocopying, recording, or otherwise, without the prior permission of the publisher or in accordance with the provisions of the Copyright, Designs and Patents Act 1988 or under the terms of any licence permitting limited copying issued by the Copyright Licensing Agency, 90 Tottenham Court Road, London W1P 0LP. Although every effort has been made to ensure that all owners of copyright material have been acknowledged in this publication, we would be glad to acknowledge in subsequent reprints or editions any omissions brought to our attention. -

Otolaryngology-Head and Neck Surgery Clinical
OTOLARYNGOLOGY HEAD &NECK SURGERY CLINICAL REFERENCE GUIDE Fifth Edition OTOLARYNGOLOGY HEAD &NECK SURGERY CLINICAL REFERENCE GUIDE Fifth Edition Raza Pasha, MD Justin S. Golub, MD, MS 5521 Ruffin Road San Diego, CA 92123 e-mail: [email protected] Website: www.pluralpublishing.com Copyright © 2018 by Plural Publishing, Inc. Typeset in 9/11 Adobe Garamond Pro by Flanagan’s Publishing Services, Inc. Printed in the United States of America by McNaughton & Gunn All rights, including that of translation, reserved. No part of this publication may be reproduced, stored in a retrieval system, or transmitted in any form or by any means, electronic, mechanical, recording, or otherwise, including photocopying, recording, taping, Web distribution, or information storage and retrieval systems without the prior written consent of the publisher. For permission to use material from this text, contact us by Telephone: (866) 758-7251 Fax: (888) 758-7255 e-mail: [email protected] Every attempt has been made to contact the copyright holders for material originally printed in another source. If any have been inadvertently overlooked, the publishers will gladly make the necessary arrangements at the first opportunity. NOTICE TO THE READER Care has been taken to confirm the accuracy of the indications, procedures, drug dosages, and diagnosis and remediation protocols presented in this book and to ensure that they conform to the practices of the general medical and health services communities. However, the authors, editors, and publisher are not responsible for errors or omissions or for any consequences from application of the information in this book and make no warranty, expressed or implied, with respect to the currency, completeness, or accuracy of the contents of the publication. -

View the 2019 Index
Index A Abnormal uterine bleeding (AUB), heart failure, 311 Achondroplasia, 454 A-a gradient 618, 619 hypertension, 319 chromosome disorder, 64 in elderly, 654 adenomyosis, 634 naming convention for, 253 endochondral ossification in, 450 with hypoxemia, 654, 655 anemia with, 410 preload/afterload effects, 282 inheritance, 60 restrictive lung disease, 661 Asherman syndrome, 634 teratogenicity, 600 AChR (acetylcholine receptor), 229 Abacavir, 201, 203 leiomyoma (fibroid), 634 Acetaldehyde, 72 Acid-base physiology, 580 Abciximab, 122 polyps (endometrial), 634 Acetaldehyde dehydrogenase, 70, 72 Acidemia, 580 Glycoprotein IIb/IIIa inhibitors, thecoma, 632 Acetaminophen, 474 diuretic effect on, 595 429 ABO blood classification, 397 vs. aspirin for pediatric patients, 474 Acid-fast oocysts, 177 thrombogenesis and, 403 newborn hemolysis, 397 free radical injury and, 210 Acid-fast organisms, 125, 140, 155 Abdominal aorta, 357 Abruptio placentae, 626 hepatic necrosis from, 249 Acidic amino acids, 81 atherosclerosis in, 305, 687 cocaine use, 600 N-acetylcysteine for overdose, 671 Acid maltase, 86 bifurcation of, 649 preeclampsia, 629 for osteoarthritis, 458 Acidosis, 578, 580 Abdominal aortic aneurysm, 306 Abscess, 470 toxicity effects, 474 contractility in, 282 Abdominal colic acute inflammation and, 215 toxicity treatment for, 247 hyperkalemia with, 578 lead poisoning, 411 lung, 670 Acetazolamide, 252, 539, 594 Acid phosphatase in neutrophils, 398 Abdominal pain Absence seizures idiopathic intracranial Acid reflux bacterial peritonitis, 384 characteristics -

Osteopathic Manipulative Medicine for Inflammatory Skin Diseases
Volume 31 JAOCDJournal Of The American Osteopathic College Of Dermatology Focus on Osteopathy: Osteopathic Manipulative Medicine for Inflammatory Skin Diseases Also in this issue: Lichen Planopilaris: A Therapeutic Management Review Clinical Manifestations of Livedoid Vasculopathy “8 to Z” Yin and Yang: A Novel Double Rotation Flap last modified on December 19, 2014 10:29 AM JOURNAL OF THE AMERICAN OSTEOPATHIC COLLEGE OF DERMATOLOGY Page 1 JOURNAL OF THE AMERICAN OSTEOPATHIC COLLEGE OF DERMATOLOGY 2014-2015 AOCD OFFICERS PRESIDENT Rick Lin, DO, FAOCD PRESIDENT-ELECT Alpesh Desai, DO, FAOCD FIRST VICE-PRESIDENT Karthik Krishnamurthy, DO, FAOCD SECOND VICE-PRESIDENT Daniel Ladd, DO, FAOCD THIRD VICE-PRESIDENT John P. Minni, DO, FAOC Editor-in-Chief SECRETARY-TREASURER Karthik Krishnamurthy, DO Jere J. Mammino, DO, FAOCD TRUSTEES Danica Alexander, DO, FAOCD (2012-2015) Reagan Anderson, DO, FAOCD (2012-2015) Michael Whitworth, DO, FAOCD (2013-2016) Tracy Favreau, DO, FAOCD (2013-2016) Sponsors: David Cleaver, DO, FAOCD (2014-2017) Amy Spizuoco, DO, FAOCD (2014-2017) Bayer Immediate Past-President AuroraDx Suzanne Sirota Rozenberg, DO, FAOCD EEC Representatives Ranbaxy James Bernard, DO, FAOCD Michael Scott, DO, FAOCD Valeant Finance Committee Representative Steven K. Grekin, DO, FAOCD AOBD Representative Stephen Purcell, DO, FAOCD Executive Director Marsha A. Wise, BS AOCD • 2902 N. Baltimore St. • Kirksville, MO 63501 800-449-2623 • FAX: 660-627-2623 • www.aocd.org COPYRIGHT AND PERMISSION: Written permission must be obtained from the Journal of the American Osteopathic College of Dermatology for copying or reprinting text of more than half a page, tables or figures. Permissions are normally granted contingent upon similar permission from the author(s), inclusion of acknowledgment of the original source, and a payment of $15 per page, table or figure of reproduced material.