Infectious Diseases in Critical Care Medicine
Total Page:16
File Type:pdf, Size:1020Kb
Load more
Recommended publications
-

Hepatitis B Patient with Fever Due to Focal Infection
DOI: 10.5272/jimab.2012184.251 Journal of IMAB - Annual Proceeding (Scientific Papers) 2012, vol. 18, book 4 HEPATITIS B PATIENT WITH FEVER DUE TO FOCAL INFECTION Assya Krasteva*, Dobriana Panova**, Krasimir Antonov**, Angelina Kisselova* * Department of Imaging and Oral Diagnostic, Faculty of Dental Medicine, ** Clinic of gastroenterology, “St. Ivan Rilski” University Hospital, Medical University - Sofia, Bulgaria. ABSTRACT enzymes, CRP and albumin returned to normal after Persistent undiagnosed fever remains a common performance of dental recommendations. problem in clinical practice. It is a fact that dental sepsis Key words: fever, focal infection, dental sepsis is one potential cause of persistent fever that can escape detection (Siminoski, K., 1993). INTRODUCTION We present a 50 years old woman with chronic Adult patients frequently visit physicians with date hepatitis B, febrile for the past two months (max. 38.60C) of persistent fever and the cause of the fever sometimes with characteristic of septic fever. She underwent cannot be found. consultations with endocrinologist, rheumatologist, The definition of fever of unknown origin (FUO), as neurologist, gynecologist, pulmonologist and infectionst. All based on a case series of 100 patients, is defined as a negative for any disease, also negative serology for Lyme temperature higher than 38.3 C (100.9 F) that lasts for more disease. She had no data for urine infection. She had than three weeks with no obvious source despite appropriate negative cultures. The patient was treated with investigation (Roth, A., 2003), and evaluation of at least 3 corticosteroids for 30 days with no effect; she had no outpatient visits or 3 days in hospital (Durack, DT.,1991). -

Clinical an Urgent Care Approach to Complications and Conditions of Pregnancy Part 2
Clinical An Urgent Care Approach to Complications and Conditions of Pregnancy Part 2 Urgent message: From pregnancy confirmation to the evaluation of bleeding, urgent care centers are often the initial location for management of obstetric-related issues. Careful use of evidence-based guidelines is the key to successful outcomes. DAVID N. JACKSON, MD, FACOG and PETAR PLANINIC, MD, FACOG Introduction rgent care providers are called upon to manage a Uvariety of complaints in pregnancy. Some conditions can be managed at the urgent care center whereas others require stabilization and transport to a center with expert obstetrical capabilities. In all situations, practitioners should consider that a gestational age of fetal viability (many centers now use 23 to 24 weeks) is best served with referral for continuous fetal monitor- ing if there is bleeding, trauma, significant hypertension, relative hypoxemia (O2 saturation less than 95% for pregnant women), or contractions. Part 2 of this two- part series will discuss: Ⅲ Bleeding in pregnancy Ⅲ Ectopic gestation Ⅲ Trauma and pregnancy Ⅲ Acute abdominal pain in pregnancy Dr. Jackson is Professor of Maternal-Fetal Medicine at the University of Nevada, School of Medicine, Las Vegas, Nevada. Dr. Planinic is Assistant Professor of Obstetrics and Gynecology at the University of Nevada, School of Medicine, Las Vegas, Nevada. © gettyimages.com www.jucm.com JUCM The Journal of Urgent Care Medicine | September 2013 9 AN URGENT CARE APPROACH TO COMPLICATIONS AND CONDITIONS OF PREGNANCY Figure 1. Bleeding endocervical polyp with Evaluation of vaginal bleeding should follow a sys- inflammation tematic process. History of last menses and sexual activ- ity determines the possibility of pregnancy. -

Melioidosis: an Emerging Infectious Disease
Review Article www.jpgmonline.com Melioidosis: An emerging infectious disease Raja NS, Ahmed MZ,* Singh NN** Department of Medical ABSTRACT Microbiology, University of Malaya Medical Center, Kuala Lumpur, Infectious diseases account for a third of all the deaths in the developing world. Achievements in understanding Malaysia, *St. the basic microbiology, pathogenesis, host defenses and expanded epidemiology of infectious diseases have Bartholomew’s Hospital, resulted in better management and reduced mortality. However, an emerging infectious disease, melioidosis, West Smithfield, London, is becoming endemic in the tropical regions of the world and is spreading to non-endemic areas. This article UK and **School of highlights the current understanding of melioidosis including advances in diagnosis, treatment and prevention. Biosciences, Cardiff Better understanding of melioidosis is essential, as it is life-threatening and if untreated, patients can succumb University, Cardiff, UK to it. Our sources include a literature review, information from international consensus meetings on melioidosis Correspondence: and ongoing discussions within the medical and scientific community. N. S. Raja, E-mail: [email protected] Received : 21-2-2005 Review completed : 20-3-2005 Accepted : 30-5-2005 PubMed ID : 16006713 KEY WORDS: Melioidosis, Burkholderia pseudomallei, Infection J Postgrad Med 2005;51:140-5 he name melioidosis [also known as Whitmore dis- in returning travellers to Europe from endemic areas.[14] The T ease] is taken from the Greek word ‘melis’ meaning geographic area of the prevalence of the organism is bound to distemper of asses and ‘eidos’ meaning resembles glanders. increase as the awareness increases. Melioidosis is a zoonotic disease caused by Pseudomonas pseudomallei [now known as Burkholderia pseudomallei], a B. -

USMLE – What's It
Purpose of this handout Congratulations on making it to Year 2 of medical school! You are that much closer to having your Doctor of Medicine degree. If you want to PRACTICE medicine, however, you have to be licensed, and in order to be licensed you must first pass all four United States Medical Licensing Exams. This book is intended as a starting point in your preparation for getting past the first hurdle, Step 1. It contains study tips, suggestions, resources, and advice. Please remember, however, that no single approach to studying is right for everyone. USMLE – What is it for? In order to become a licensed physician in the United States, individuals must pass a series of examinations conducted by the National Board of Medical Examiners (NBME). These examinations are the United States Medical Licensing Examinations, or USMLE. Currently there are four separate exams which must be passed in order to be eligible for medical licensure: Step 1, usually taken after the completion of the second year of medical school; Step 2 Clinical Knowledge (CK), this is usually taken by December 31st of Year 4 Step 2 Clinical Skills (CS), this is usually be taken by December 31st of Year 4 Step 3, typically taken during the first (intern) year of post graduate training. Requirements other than passing all of the above mentioned steps for licensure in each state are set by each state’s medical licensing board. For example, each state board determines the maximum number of times that a person may take each Step exam and still remain eligible for licensure. -

Current Microbiological, Clinical and Therapeutic Aspects of Impetigo Lior Zusmanovich, Lior Charach and Gideon Charach*
ISSN: 2378-3656 Zusmanovich et al. Clin Med Rev Case Rep 2018, 5:205 DOI: 10.23937/2378-3656/1410205 Volume 5 | Issue 3 Clinical Medical Reviews Open Access and Case Reports CASE REPORT Current Microbiological, Clinical and Therapeutic Aspects of Impetigo Lior Zusmanovich, Lior Charach and Gideon Charach* Department of Internal Medicine “C”, Affiliated to Tel Aviv University, Israel *Corresponding author: Gideon Charach, Department of Internal Medicine “C”, Tel Aviv Sourasky Check for Medical Center, Sackler Medical School, Affiliated to Tel Aviv University, 6 Weizman Street, Tel Aviv updates 6423906, Israel, Tel: +972-3-6973766, Fax: +972-3-6973929, E-mail: [email protected] nonpurulent and purulent cellulitis, and treatment is Abstract based on extent of infection and risk factors. Abscesses Impetigo is a highly contagious infection of the epidermis, involve the dermis and deeper skin tissues as a result of seen especially among children, and transmitted through direct contact. Two bacteria are associated with impetigo: pus formation. S. aureus and GAS. Over 140 million people are suffering Impetigo is observed most frequently among chil- from impetigo at each time point, over 100 million are chil- dren. Two forms of impetigo exist, namely impetigo conta- dren 2-5 years of age and is transmitted through direct giosa, known as the non-bullous form and the second one contact [1]. Risk factors for impetigo include poor hy- being bullous impetigo which presents with large and fragile giene, low economic status, crowding and underlying bullae. Treatment options for impetigo include systemic an- scabies [2,3]. Important consideration is carriage of tibiotics, topical antibiotics as well as topical disinfectants. -

Cutaneous Manifestations of HIV Infection Carrie L
Chapter Title Cutaneous Manifestations of HIV Infection Carrie L. Kovarik, MD Addy Kekitiinwa, MB, ChB Heidi Schwarzwald, MD, MPH Objectives Table 1. Cutaneous manifestations of HIV 1. Review the most common cutaneous Cause Manifestations manifestations of human immunodeficiency Neoplasia Kaposi sarcoma virus (HIV) infection. Lymphoma 2. Describe the methods of diagnosis and treatment Squamous cell carcinoma for each cutaneous disease. Infectious Herpes zoster Herpes simplex virus infections Superficial fungal infections Key Points Angular cheilitis 1. Cutaneous lesions are often the first Chancroid manifestation of HIV noted by patients and Cryptococcus Histoplasmosis health professionals. Human papillomavirus (verruca vulgaris, 2. Cutaneous lesions occur frequently in both adults verruca plana, condyloma) and children infected with HIV. Impetigo 3. Diagnosis of several mucocutaneous diseases Lymphogranuloma venereum in the setting of HIV will allow appropriate Molluscum contagiosum treatment and prevention of complications. Syphilis Furunculosis 4. Prompt diagnosis and treatment of cutaneous Folliculitis manifestations can prevent complications and Pyomyositis improve quality of life for HIV-infected persons. Other Pruritic papular eruption Seborrheic dermatitis Overview Drug eruption Vasculitis Many people with human immunodeficiency virus Psoriasis (HIV) infection develop cutaneous lesions. The risk of Hyperpigmentation developing cutaneous manifestations increases with Photodermatitis disease progression. As immunosuppression increases, Atopic Dermatitis patients may develop multiple skin diseases at once, Hair changes atypical-appearing skin lesions, or diseases that are refractory to standard treatment. Skin conditions that have been associated with HIV infection are listed in Clinical staging is useful in the initial assessment of a Table 1. patient, at the time the patient enters into long-term HIV care, and for monitoring a patient’s disease progression. -

CARDINAL SYMPTOMS of HEART DISEASE Exam 1 | Dr. Donato Marañon | September 24, 2012
OS 213: Cardiovascular System LEC 02: CARDINAL SYMPTOMS OF HEART DISEASE Exam 1 | Dr. Donato Marañon | September 24, 2012 OUTLINE Common Cardiac Symptomatology B. Dyspnea A. Chest Pain C. Palpitations 1. Attributes of Pain D. Edema 2. Definitions E. Cyanosis 3. Chronic Recurrent Chest Pain Syndrome F. Syncope 4. Acute Chest Pain Syndrome II. Importance of History and PE 5. Case Discussion The lecture is similar from block B’s Lecture but we changed the formatting though kasing ang gulo nung topic. So if mas naguluhan kayo sorry. Some changes: 1. All the symptomatology are now under common cardiac symptomatology. 2. Differentials for chest pain have been divided into chronic and acute. I. COMMON CARDIAC SYMPTOMATOLOGY Symptoms: complaints of the patient (most common complaint: pain); Includes chest pain, dyspnea, palpitations, edema, cyanosis, syncope Signs: doctors’ objective findings and observations A. CHEST PAIN Chest pain: most common but not exhaustive - can be caused by other factors such as hypertension ATTRIBUTES OF PAIN (PPQRSTO) Provocative – what provokes/triggers the pain o Is it precipitated by effort (exertional)? o At what time does it appear? When you are trying to get up, moving the body, etc… Palliative – what relieves/palliates the pain o Medications, therapy, etc… Quality – the nature of the pain o Sharp, burning, pricking, stabbing, strangulating, oppressing, ache similar to muscle ache, etc. Region/Radiation – location (primary region where the pain is felt), central region, how wide the coverage is and where the pain radiates or is worst o Central precordial pain where does it radiate? Back? Leg? o Hard to interview Filipinos – “doon, diyan” – vague descriptions of location Severity – intensity: mild, moderate, severe o May use a scale from 0 to 10 (worst) o Give open-ended questions Timing o Onset – abrupt, worse at start, insidious, builds up/gradual Ian, Aca, Hannah UPCM 2016A: XVI, Walang 1 of Kapantay! 14 OS 213: Cardiovascular System LEC 02: CARDINAL SYMPTOMS OF HEART DISEASE Exam 1 | Dr. -

An Atypical Case of Recurrent Cellulitis/Lymphangitis in a Dutch Warmblood Horse Treated by Surgical Intervention A
EQUINE VETERINARY EDUCATION / AE / JANUARY 2013 23 Case Report An atypical case of recurrent cellulitis/lymphangitis in a Dutch Warmblood horse treated by surgical intervention A. M. Oomen*, M. Moleman, A. J. M. van den Belt† and H. Brommer Department of Equine Sciences and †Companion Animals, Division of Diagnostic Imaging, Faculty of Veterinary Medicine, Utrecht University, Yalelaan, Utrecht, The Netherlands. *Corresponding author email: [email protected] Keywords: horse; lymphangitis; lymphoedema; surgery; lymphangiectasia Summary proposed as a possible contributing factor for chronic The case reported here describes an atypical presentation progressive lymphoedema of the limb in these breeds of of cellulitis/lymphangitis in an 8-year-old Dutch Warmblood horses (de Cock et al. 2003, 2006; Ferraro 2003; van mare. The horse was presented with a history of recurrent Brantegem et al. 2007). episodes of cellulitis/lymphangitis and the presence of Other diseases related to the lymphatic system are fluctuating cyst-like lesions on the left hindlimb. These lesions lymphangioma/lymphangiosarcoma and development appeared to be interconnected lymphangiectasias. Surgical of lymphangiectasia. Cutaneous lymphangioma has been debridement followed by primary wound closure and local described as a solitary mass on the limb, thigh or inguinal drainage was performed under general anaesthesia. Twelve region of horses without the typical signs of progressive months post surgery, no recurrence of cellulitis/lymphangitis lymphoedema (Turk et al. 1979; Gehlen and Wohlsein had occurred and the mare had returned to her former use as 2000; Junginger et al. 2010). Lymphangiectasias in horses a dressage horse. have been described in the intestinal wall of foals and horses with clinical signs of colic and diarrhoea (Milne et al. -

WO 2014/134709 Al 12 September 2014 (12.09.2014) P O P C T
(12) INTERNATIONAL APPLICATION PUBLISHED UNDER THE PATENT COOPERATION TREATY (PCT) (19) World Intellectual Property Organization International Bureau (10) International Publication Number (43) International Publication Date WO 2014/134709 Al 12 September 2014 (12.09.2014) P O P C T (51) International Patent Classification: (81) Designated States (unless otherwise indicated, for every A61K 31/05 (2006.01) A61P 31/02 (2006.01) kind of national protection available): AE, AG, AL, AM, AO, AT, AU, AZ, BA, BB, BG, BH, BN, BR, BW, BY, (21) International Application Number: BZ, CA, CH, CL, CN, CO, CR, CU, CZ, DE, DK, DM, PCT/CA20 14/000 174 DO, DZ, EC, EE, EG, ES, FI, GB, GD, GE, GH, GM, GT, (22) International Filing Date: HN, HR, HU, ID, IL, IN, IR, IS, JP, KE, KG, KN, KP, KR, 4 March 2014 (04.03.2014) KZ, LA, LC, LK, LR, LS, LT, LU, LY, MA, MD, ME, MG, MK, MN, MW, MX, MY, MZ, NA, NG, NI, NO, NZ, (25) Filing Language: English OM, PA, PE, PG, PH, PL, PT, QA, RO, RS, RU, RW, SA, (26) Publication Language: English SC, SD, SE, SG, SK, SL, SM, ST, SV, SY, TH, TJ, TM, TN, TR, TT, TZ, UA, UG, US, UZ, VC, VN, ZA, ZM, (30) Priority Data: ZW. 13/790,91 1 8 March 2013 (08.03.2013) US (84) Designated States (unless otherwise indicated, for every (71) Applicant: LABORATOIRE M2 [CA/CA]; 4005-A, rue kind of regional protection available): ARIPO (BW, GH, de la Garlock, Sherbrooke, Quebec J1L 1W9 (CA). GM, KE, LR, LS, MW, MZ, NA, RW, SD, SL, SZ, TZ, UG, ZM, ZW), Eurasian (AM, AZ, BY, KG, KZ, RU, TJ, (72) Inventors: LEMIRE, Gaetan; 6505, rue de la fougere, TM), European (AL, AT, BE, BG, CH, CY, CZ, DE, DK, Sherbrooke, Quebec JIN 3W3 (CA). -
Pediatrics-EOR-Outline.Pdf
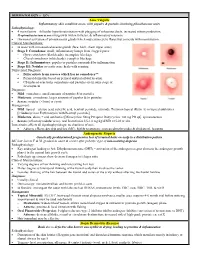
DERMATOLOGY – 15% Acne Vulgaris Inflammatory skin condition assoc. with papules & pustules involving pilosebaceous units Pathophysiology: • 4 main factors – follicular hyperkeratinization with plugging of sebaceous ducts, increased sebum production, Propionibacterium acnes overgrowth within follicles, & inflammatory response • Hormonal activation of pilosebaceous glands which may cause cyclic flares that coincide with menstruation Clinical Manifestations: • In areas with increased sebaceous glands (face, back, chest, upper arms) • Stage I: Comedones: small, inflammatory bumps from clogged pores - Open comedones (blackheads): incomplete blockage - Closed comedones (whiteheads): complete blockage • Stage II: Inflammatory: papules or pustules surrounded by inflammation • Stage III: Nodular or cystic acne: heals with scarring Differential Diagnosis: • Differentiate from rosacea which has no comedones** • Perioral dermatitis based on perioral and periorbital location • CS-induced acne lacks comedones and pustules are in same stage of development Diagnosis: • Mild: comedones, small amounts of papules &/or pustules • Moderate: comedones, larger amounts of papules &/or pustules • Severe: nodular (>5mm) or cystic Management: • Mild: topical – azelaic acid, salicylic acid, benzoyl peroxide, retinoids, Tretinoin topical (Retin A) or topical antibiotics [Clindamycin or Erythromycin with Benzoyl peroxide] • Moderate: above + oral antibiotics [Minocycline 50mg PO qd or Doxycycline 100 mg PO qd], spironolactone • Severe (refractory nodular acne): oral -

Bacterial Infections Diseases Picture Cause Basic Lesion
page: 117 Chapter 6: alphabetical Bacterial infections diseases picture cause basic lesion search contents print last screen viewed back next Bacterial infections diseases Impetigo page: 118 6.1 Impetigo alphabetical Bullous impetigo Bullae with cloudy contents, often surrounded by an erythematous halo. These bullae rupture easily picture and are rapidly replaced by extensive crusty patches. Bullous impetigo is classically caused by Staphylococcus aureus. cause basic lesion Basic Lesions: Bullae; Crusts Causes: Infection search contents print last screen viewed back next Bacterial infections diseases Impetigo page: 119 alphabetical Non-bullous impetigo Erythematous patches covered by a yellowish crust. Lesions are most frequently around the mouth. picture Lesions around the nose are very characteristic and require prolonged treatment. ß-Haemolytic streptococcus is cause most frequently found in this type of impetigo. basic lesion Basic Lesions: Erythematous Macule; Crusts Causes: Infection search contents print last screen viewed back next Bacterial infections diseases Ecthyma page: 120 6.2 Ecthyma alphabetical Slow and gradually deepening ulceration surmounted by a thick crust. The usual site of ecthyma are the legs. After healing there is a permanent scar. The pathogen is picture often a streptococcus. Ecthyma is very common in tropical countries. cause basic lesion Basic Lesions: Crusts; Ulcers Causes: Infection search contents print last screen viewed back next Bacterial infections diseases Folliculitis page: 121 6.3 Folliculitis -

Drug Prescribing for Dentistry Dental Clinical Guidance
Scottish Dental Clinical Effectiveness Programme SDcep Drug Prescribing For Dentistry Dental Clinical Guidance Second Edition August 2011 Scottish Dental Clinical Effectiveness Programme SDcep The Scottish Dental Clinical Effectiveness Programme (SDCEP) is an initiative of the National Dental Advisory Committee (NDAC) and is supported by the Scottish Government and NHS Education for Scotland. The programme aims to provide user-friendly, evidence-based guidance for the dental profession in Scotland. SDCEP guidance is designed to help the dental team provide improved care for patients by bringing together, in a structured manner, the best available information that is relevant to priority areas in dentistry, and presenting this information in a form that can interpreted easily and implemented. ‘Supporting the dental team to provide quality patient care’ Scottish Dental Clinical Effectiveness Programme SDcep Drug Prescribing For Dentistry Dental Clinical Guidance Second Edition August 2011 Drug Prescribing For Dentistry © Scottish Dental Clinical Effectiveness Programme SDCEP operates within NHS Education for Scotland. You may copy or reproduce the information in this document for use within NHS Scotland and for non-commercial educational purposes. Use of this document for commercial purpose is permitted only with written permission. ISBN 978 1 905829 13 2 First published 2008 Second edition published August 2011 Scottish Dental Clinical Effectiveness Programme Dundee Dental Education Centre, Frankland Building, Small’s Wynd, Dundee DD1