Otolaryngology-Head and Neck Surgery Clinical
Total Page:16
File Type:pdf, Size:1020Kb
Load more
Recommended publications
-

Respiratory Therapy Program
UNIVERSITY OF THE DISTRICT OF COLUMBIA RESPIRATORY THERAPY PROGRAM The University offers the A.A.S. Degree in Respiratory ASSOCIATE IN APPLIED SCIENCE DEGREE IN Therapy. The curriculum reflects high standards of RESPIRATORY THERAPY professional practice and incorporates guidelines from practice trends, professional organizations and accrediting Total Credit Hours of College-Level Courses Required agencies. Students develop the knowledge base and For Graduation: 70 clinical competencies required to meet the health care needs of patients with cardiopulmonary disorders. The program offers both a day and an evening option. Respiratory Therapists treat patients along the age and health-care continuums – from premature infants to the PROGRAM OF STUDY aged in critical care, acute care, rehabilitation, and home care settings. PREREQUISITES 1535-101 General College Math I 3 ACCREDITATION & CREDENTIALING 1133-111 English Composition I 3 1401-112 Anatomy and Physiology II – Lecture 3 The UDC Respiratory Therapy Program is accredited by 1401-114 Anatomy and Physiology II – Lab 1 the Commission on Accreditation of Allied Health Total 10 Credits Education Programs (CAAHEP), in collaboration with the FIRST YEAR – FALL SEMESTER Committee on Accreditation for Respiratory Care 1431-170 Introduction to Health Sciences 2 1431-171 Principles and Practice of Resp Therapy I 4 (CoARC). Graduates are eligible for both the entry-level licensure/ CRT examination (required by the District of 1401-112 Anatomy and Physiology II – Lecture 3 Columbia, Maryland and Virginia) and the advanced 1401-114 Anatomy and Physiology II – Lab 1 1133-112 or 1535-102 English Composition II or practice RRT examinations, both offered by the National Board for Respiratory Care (NBRC). -

Middle Nasal Valve Collapse: a Way to Resolve
Journal of Otolaryngology-ENT Research Case Report Open Access Middle nasal valve collapse: a way to resolve Abstract Volume 10 Issue 3 - 2018 Middle nasal valve collapse is a partial or complete collapsing of soft structures of Dunja Milicic,1 Carolina Serodio2 nasal pyramid, due to negative intranasal pressures resulting in complete anterior nasal 1 obstruction of air-flow. Even though is relatively common, it is often misdiagnosed or Hospital da Luz Arrabida, Department of Otorhinolaryngology, Portugal neglected in diagnosis. There are too many suggestions of surgical resolution of the 2Hospital da Luz Póvoa de Varzim, Department of problem, giving an idea that all of them are actually only partially or insufficiently Otorhinolaryngology, Portugal resolving the problem. In this paper a possible solution of middle nasal vault collapse was presented. A Correspondence: Dunja Milicic, Hospital da Luz Arrábida, triangle cartilage grafting with respecting of anatomical and functional principles was Praceta de Henrique Moreira 150, 4400-346 Vila Nova de Gaia, Portugal, Tel +351-22 377-6800, suggested. An open rhinoplasty approach by its large exposure was, in our hands, the Email [email protected] election method for resolving the problem. Received: February 01, 2018 | Published: May 21, 2018 Keywords: nasal valve collapse, triangular cartilage, graft, open rhinoplasty Introduction the nostril (lateral alar crura) is usually annoying the patients, by its hardness and cosmetic deformity, even though some authors minimize Collapse -

Globus Hystericus — an Overview
Bangladesh Journal of Psychiatry. June, 1995, 7, 1, 32 GLOBUS HYSTERICUS — AN OVERVIEW Anwarul Haider1, M S I Mullick2, Md Shakhawat Islam3 Introduction Globus hystericus, Globus pharynges, Functional no abnormality7. The condition may be due to dysphagia, Globus syndrome are synonymous1. spasm of upper oesophageal sphincter. Many of It is a pscyhogenic disorder of alimentary tract the patients have reflux oesophagities. extremely common, the cause is poorly Oesphageal reflux due to abnormality in cardia understood, indeed may be relieved by may produce vague upper end symptoms, swallowing food or drink, occurs in tense anxious antacids reported to help if this is the case589. individuals23. Globus hystericus should not be diagnosed until an organic lesion especially a malignancy has been excluded10, all other causes of dysphagia Natural History : has to be excluded carefully. The patient often Persistent feeling or sensation of a lump in the admits to psychological stress or cancer phobia11. throat, usually in mid line, localised just above An attempt should be made to offer insight in the the supra steranl notch around the level of cricoid nature of the problem, a detail history, careful cartilage, is the commonest complain, mainly examination with x-ray if appropriate will help to occurs in anxious, middle aged, menopausal reassure a certain number of patients. A history ladies34. There is interference with swallowing but of friends or relatives with throat disease requires no true dysphagia for solid & liquid and the sympathetic probing12. symptoms often noticeable in empty swallowing One also has to remember that even most of saliva, are often diagnosed as globus if on neurotic patient, however on rare occasions is examination nothing found5. -

Dorsal Approach Rhinoplasty Dorsal Approach Rhinoplasty
AIJOC 10.5005/jp-journals-10003-1105 ORIGINAL ARTICLE Dorsal Approach Rhinoplasty Dorsal Approach Rhinoplasty Kenneth R Dubeta Part I: Historical Milestones in Rhinoplasty ABSTRACT Direct dorsal excision of skin and subcutaneous tissue is employed in rhinoplasty cases characterized by thick rigid skin to achieve satisfactory esthetic results, in which attempted repair by more conventional means would most likely frustrate both surgeon and patient. This historical review reminds us of the lesson: ‘History repeats itself.’ Built on a foundation of reconstructive rhinoplasty, modern cosmetic and corrective rhinoplasty have seen the parallel development of both open and closed techniques as ‘new’ methods are introduced and reintroduced again. It is from the perspective of constant evolution in the art of rhinoplasty surgery that the author presents, in Part II, his unique ‘eagle wing’ chevron incision technique of dorsal approach rhinoplasty, to overcome the problems posed by the rigid skin nose. Keywords: Dorsal approach rhinoplasty, Eagle wing incision, Fig. 1: Ancient Greek ‘perikephalea’ to support the Rigid skin nose, External approach rhinoplasty, Historical straightened nose1 milestones. How to cite this article: Dubeta KR. Dorsal Approach and functions of the nose. Refinement of these techniques Rhinoplasty. Int J Otorhinolaryngol Clin 2013;5(1):1-23. seemingly had to await three antecedent developments; Source of support: Nil topical vasoconstriction; topical, systemic and local Conflict of interest: None declared anesthesia; and safe, reliable sources of illumination. The last half of the 20th century has seen the dissemination of INTRODUCTION two of the most important developments in the history of Throughout the ages, numerous techniques of altering, nasal surgery: correcting and more recently, improving the appearance and 1. -
Pediatrics-EOR-Outline.Pdf
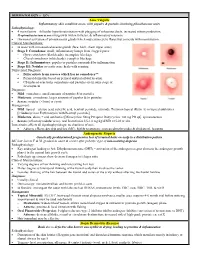
DERMATOLOGY – 15% Acne Vulgaris Inflammatory skin condition assoc. with papules & pustules involving pilosebaceous units Pathophysiology: • 4 main factors – follicular hyperkeratinization with plugging of sebaceous ducts, increased sebum production, Propionibacterium acnes overgrowth within follicles, & inflammatory response • Hormonal activation of pilosebaceous glands which may cause cyclic flares that coincide with menstruation Clinical Manifestations: • In areas with increased sebaceous glands (face, back, chest, upper arms) • Stage I: Comedones: small, inflammatory bumps from clogged pores - Open comedones (blackheads): incomplete blockage - Closed comedones (whiteheads): complete blockage • Stage II: Inflammatory: papules or pustules surrounded by inflammation • Stage III: Nodular or cystic acne: heals with scarring Differential Diagnosis: • Differentiate from rosacea which has no comedones** • Perioral dermatitis based on perioral and periorbital location • CS-induced acne lacks comedones and pustules are in same stage of development Diagnosis: • Mild: comedones, small amounts of papules &/or pustules • Moderate: comedones, larger amounts of papules &/or pustules • Severe: nodular (>5mm) or cystic Management: • Mild: topical – azelaic acid, salicylic acid, benzoyl peroxide, retinoids, Tretinoin topical (Retin A) or topical antibiotics [Clindamycin or Erythromycin with Benzoyl peroxide] • Moderate: above + oral antibiotics [Minocycline 50mg PO qd or Doxycycline 100 mg PO qd], spironolactone • Severe (refractory nodular acne): oral -

Lung Decortication in Phase III Pleural Empyema by Video-Assisted Thoracoscopic Surgery (VATS)—Results of a Learning Curve Study
4320 Original Article Lung decortication in phase III pleural empyema by video-assisted thoracoscopic surgery (VATS)—results of a learning curve study Martin Reichert1, Bernd Pösentrup1, Andreas Hecker1, Winfried Padberg1, Johannes Bodner2,3 1Department of General, Visceral, Thoracic, Transplant and Pediatric Surgery, University Hospital of Giessen, Giessen, Germany; 2Department of Thoracic Surgery, Klinikum Bogenhausen, Munich, Germany; 3Department of Visceral, Transplant and Thoracic Surgery, Center of Operative Medicine, Innsbruck Medical University, Innsbruck, Austria Contributions: (I) Conception and design: M Reichert, J Bodner; (II) Administrative support: A Hecker, W Padberg; (III) Provision of study materials or patients: W Padberg, J Bodner; (IV) Collection and assembly of data: M Reichert, B Pösentrup; (V) Data analysis and interpretation: All authors; (VI) Manuscript writing: All authors; (VII) Final approval of manuscript: All authors. Correspondence to: Martin Reichert, MD. Department of General, Visceral, Thoracic, Transplant and Pediatric Surgery, University Hospital of Giessen, Rudolf-Buchheim Strasse 7, 35392 Giessen, Germany. Email: [email protected]. Background: Pleural empyema (PE) is a devastating disease with a high morbidity and mortality. According to the American Thoracic Society it is graduated into three phases and surgery is indicated in intermediate phase II and organized phase III. In the latter, open decortication of the lung via thoracotomy is the gold standard whereas the evidence for feasibility and safety of a minimally-invasive video-assisted thoracoscopic approach is still poor. Methods: Retrospective single-center analysis of patients undergoing surgery for phase III PE from 02/2011 to 03/2015 [n=138, including n=130 VATS approach (n=3 of them with bilateral disease) and n=8 open approach]. -

Download Download
1 Contribution of dental private practitioners to 2 publications on anatomical variations using 3 cone beam computed tomography. 4 5 Authors: 6 Hebda A1,*MS, 7 Theys S2 DDS, 8 De Roissart J3 MD, 9 Perez E4 DDS, 10 Olszewski R1,3 DDS,MD,PhD,DrSc 11 Affiliations: 12 1 Oral and maxillofacial surgery research Lab, NMSK, IREC, SSS, UCLouvain, 13 Brussels, Belgium 14 2 Department of pediatric dentistry and special care, Cliniques universitaires saint 15 Luc, UCLouvain, Brussels, Belgium 16 3 Department of oral and maxillofacial surgery, Cliniques universitaires saint Luc, 17 UCLouvain, Brussels, Belgium 18 4 Department of orthodontics, Cliniques universitaires saint Luc, UCLouvain, 19 Brussels, Belgium 20 *Corresponding author: Hebda A, Oral and maxillofacial surgery research Lab, 21 NMSK, IREC, SSS, UCLouvain, Brussels, Belgium, ORCID Id 0000-0001-5111- 22 0021 1 2 [Nemesis] Titre de l’article (PUL - En- tête paire) 23 Disclaimer: the views expressed in the submitted article are our own and not an 24 official position of the institution or funder. 25 26 27 28 29 30 31 32 33 34 35 36 37 38 39 40 41 42 43 44 45 46 47 48 49 50 51 52 53 54 55 56 57 58 59 60 [Nemesis] Titre de l’article (PUL - En- tête impaire) 3 61 Abstract 62 Objective: To investigate the participation of citizens-dental private practitioner in 63 scientific articles about anatomical variations on dentomaxillofacial CBCT. Our null 64 hypothesis was that private practice practitioners are not involved in publications on 65 anatomical variations using cone beam computed tomography. -

A Small Road to Misery in Necrotizing External Otitis
Published August 8, 2019 as 10.3174/ajnr.A6161 ORIGINAL RESEARCH HEAD & NECK A Persistent Foramen of Huschke: A Small Road to Misery in Necrotizing External Otitis X W.L. van der Meer, X M. van Tilburg, X C. Mitea, and X A.A. Postma ABSTRACT BACKGROUND AND PURPOSE: Necrotizing external otitis is a serious complication of external otitis with different spreading patterns. A persistent foramen of Huschke is a dehiscence located antero-inferior in the osseous external ear canal and posterior-medial to the temporomandibular joint. This dehiscence can facilitate extension of infection in an anterior pattern next to classic spread along the fissures of Santorini. The aim of this study was to define the prevalence and size of a persistent foramen of Huschke in patients with necrotizing external otitis. MATERIALS AND METHODS: We retrospectively examined 78 CT temporal bone studies (39 patients with necrotizing external otitis, 39 control subjects). The side and presence of the foramen were noted, and its prevalence was calculated. The maximal width of the foramen of Huschke was measured in the axial plane and classified as subtle, mild, moderate, or extensive. RESULTS: A persistent foramen of Huschke was present in 21 patients (26 ears) and 7 control subjects (9 ears). Prevalence was 50% (20/40) and 11.5% (9/78) in affected ears of patients with necrotizing external otitis and control subjects, respectively. Almost all affected ears showed an anterior distribution pattern of necrotizing external otitis. The extensive dehiscence was most common in affected ears. CONCLUSIONS: An anterior necrotizing external otitis spreading pattern is associated with the presence and increased size of a persis- tent foramen of Huschke. -

Table of Contents 1
GENERAL THORACIC SURGERY DATABASE v.2.3 TRAINING MANUAL August 2017 Table of Contents 1. Demographics ................................................................................................................................................................. 2 2. Follow Up ........................................................................................................................................................................ 9 3. Admission ..................................................................................................................................................................... 10 4. Pre-Operative Evaluation ............................................................................................................................................. 14 5. Diagnosis (Category of Disease) ................................................................................................................................... 48 6. Procedure ..................................................................................................................................................................... 70 7. Post-Operative Events ................................................................................................................................................ 111 8. Discharge .................................................................................................................................................................... 135 9. Quality Measures ...................................................................................................................................................... -

Cricopharyngeal Myotomy Revisited
10.5005/jp-journals-10023-1019 Sudhakara M Rao et al CASE REPORT Cricopharyngeal Myotomy Revisited 1Sudhakara M Rao, 2Satishchandra T, 2PSN Murthy 1Associate Professor, Department of ENT and Head and Neck Surgery, Dr PSIMS and RF, Gannavaram, Andhra Pradesh, India 2Professor and Head, Department of ENT and Head and Neck Surgery, Dr PSIMS and RF, Gannavaram, Andhra Pradesh, India Correspondence: PSN Murthy, Professor and Head, Department of ENT and Head and Neck Surgery, Dr PSIMS and RF Gannavaram, Andhra Pradesh, India, e-mail: [email protected] ABSTRACT Dysphagia due to neuromuscular in coordination is major disability for the patient. Not able to swallow food or liquids inspite of healthy appetite makes the patient most irritable and can lead to psychological problems. Added to the swallowing problem patient also encounters symptoms and signs of laryngeal penetration or aspiration. For these patients, surgical option of cricopharyngeal myotomy offers a very good relief. We describe two cases where CP myotomy could facilitate a good swallow and prevent laryngeal stimulation or penetration and made a significant improvement in the quality of life of the patients. Keywords: Cricopharyngeal myotomy, Cricopharyngeal spasm, Neurogenic dysphasia, Cricopharyngeus muscle. INTRODUCTION myotomy in the same sitting under GA. He was given nasogastric feeds for 3 days before surgery. During surgery, hypo- Cricopharyngeal spasm can be a primary or secondary to several pharyngoscopy revealed no abnormality of postcricoid area. neurologic disorders.1 Mainly these are the patients who have a Another endotracheal tube was placed in the esophagus to identify basic neurologic disorder from which they were recovering but cricopharyngeal sphincter. -

Identification of Two Novel LAMP2 Gene Mutations in Danon Disease
The Laryngoscope © 2016 the American Laryngological, Rhinological and Otological Society, Inc. Rotational Thyrotracheopexy After Cricoidectomy for Low-Grade Laryngeal Chrondrosarcoma László Rovó, MD, PhD; Ádám Bach, MD; Balázs Sztanó, MD, PhD; Vera Matievics, MD; Ilona Szegesdi, MD; Paul F. Castellanos, MD, FCCP Objectives:The complex laryngeal functions are fundamentally defined by the cricoid cartilage. Thus, lesions requiring subtotal or total resection of the cricoid cartilage commonly warrant total laryngectomy. However, from an oncological per spective, the resection of the cricoid cartilage would be an optimal solution in these cases. The poor functional results of the few reported cases of total and subtotal cricoidectomy with different reconstruction techniques confirm the need for new approaches to reconstruct the infrastructure of the larynx post cricoidectomy. Study Design:Retrospective case series review. Methods:Four consecutive patients with low-grade chondrosarcoma were treated by cricoidectomy with rotational thy rotracheopexy reconstruction to enable the functional creation of a complete cartilaginous ring that can substitute the func tions of the cricoid cartilage. The glottic structures were stabilized with endoscopic arytenoid abduction lateropexy. Patients were evaluated with objective and subjective function tests. Results: Tumor-free margins were proven; patients were successfully decannulated within 3 weeks. Voice outcomes were adequate for social conversation in all cases. Oral feeding was possible in three patients. Conclusion:Total and subtotal cricoidectomy can be a surgical option to avoid total laryngectomy in cases of large chondrosarcomas destroying the cricoid cartilage. The thyrotracheopexy rotational advancement technique enables the effec tive reconstruction of the structural deficit of the resected cricoid cartilage in cases of total and subtotal cricoidectomy. -

Respiratory Therapy Handbook
WASHINGTON STATE COMMUNITY COLLEGE RESPIRATORY THERAPY STUDENT HANDBOOK 2020-2021 Written: July, 1996 Revised: December, 2020 TABLE OF CONTENTS Statement of Non-Discrimination…………………………………………………………………………….. 2 Introduction……………………………………………………………………………………………………………..3 Goal………………………………………………………………………………………………………………………5-6 Accreditation……………………………………………………………………………………………………………6 Program Organization………………………………………………………………………………………………7 Plan for Consistency of Clinical Instruction & Evaluation of Clinical courses, Preceptors & Clinical Sites…………………………………………………………………………………………………………9 STUDENT POLICIES Course of Study………………………………………………………………………………………………………11 Student Schedule/Class sessions……………………………………………………………………………..11 Clinical Experiences…………………………………………………………………………………………..11-12 Tardiness……………………………………………………………………………………………………………….12 Absenteeism, Clinical…………………………………………………………………………………………12-13 Absenteeism, Classroom………………………………………………………………………………………….13 Absenteeism, Lab……………………………………………………………………………………………….13-14 Clinical Evaluations……………………………………………………………………………………………15-16 Clinical Competency…………………………………………………………………………………………..17-20 ACADEMIC POLICIES Clinical Evaluation Forms…………………………………………………………………………………..15-16 Clinical Competency Evaluation………………………………………………………………………….17-20 Promotion………………………………………………………………………………………………………………21 Evaluation………………………………………………………………………………………………………………21 Remediation …………………………………………………………………………………………………………..22 Probation/Dismissal……………………………………………………………………………………………….22 Leave of Absence…………………………………………………………………………………………………….22