Chapter 3: AKI Associated with Malignancies
Total Page:16
File Type:pdf, Size:1020Kb

Load more
Recommended publications
-

Impact of Urolithiasis and Hydronephrosis on Acute Kidney Injury in Patients with Urinary Tract Infection
bioRxiv preprint doi: https://doi.org/10.1101/2020.07.13.200337; this version posted July 13, 2020. The copyright holder for this preprint (which was not certified by peer review) is the author/funder, who has granted bioRxiv a license to display the preprint in perpetuity. It is made available under aCC-BY 4.0 International license. Impact of urolithiasis and hydronephrosis on acute kidney injury in patients with urinary tract infection Short title: Impact of urolithiasis and hydronephrosis on AKI in UTI Chih-Yen Hsiao1,2, Tsung-Hsien Chen1, Yi-Chien Lee3,4, Ming-Cheng Wang5,* 1Division of Nephrology, Department of Internal Medicine, Ditmanson Medical Foundation Chia-Yi Christian Hospital, Chia-Yi, Taiwan 2Department of Hospital and Health Care Administration, Chia Nan University of Pharmacy and Science, Tainan, Taiwan 3Department of Internal Medicine, Fu Jen Catholic University Hospital, Fu Jen Catholic University, New Taipei, Taiwan 4School of Medicine, College of Medicine, Fu Jen Catholic University, New Taipei, Taiwan 5Division of Nephrology, Department of Internal Medicine, National Cheng Kung University Hospital, College of Medicine, National Cheng Kung University, Tainan, Taiwan *[email protected] 1 bioRxiv preprint doi: https://doi.org/10.1101/2020.07.13.200337; this version posted July 13, 2020. The copyright holder for this preprint (which was not certified by peer review) is the author/funder, who has granted bioRxiv a license to display the preprint in perpetuity. It is made available under aCC-BY 4.0 International license. Abstract Background: Urolithiasis is a common cause of urinary tract obstruction and urinary tract infection (UTI). This study aimed to identify whether urolithiasis with or without hydronephrosis has an impact on acute kidney injury (AKI) in patients with UTI. -

The Links Between Microbiome and Uremic Toxins in Acute Kidney Injury: Beyond Gut Feeling—A Systematic Review
toxins Article The Links between Microbiome and Uremic Toxins in Acute Kidney Injury: Beyond Gut Feeling—A Systematic Review Alicja Rydzewska-Rosołowska 1,* , Natalia Sroka 1, Katarzyna Kakareko 1, Mariusz Rosołowski 2 , Edyta Zbroch 1 and Tomasz Hryszko 1 1 2nd Department of Nephrology and Hypertension with Dialysis Unit, Medical University of Białystok, 15-276 Białystok, Poland; [email protected] (N.S.); [email protected] (K.K.); [email protected] (E.Z.); [email protected] (T.H.) 2 Department of Gastroenterology and Internal Medicine, Medical University of Białystok, 15-276 Białystok, Poland; [email protected] * Correspondence: [email protected] Received: 30 October 2020; Accepted: 9 December 2020; Published: 11 December 2020 Abstract: The last years have brought an abundance of data on the existence of a gut-kidney axis and the importance of microbiome in kidney injury. Data on kidney-gut crosstalk suggest the possibility that microbiota alter renal inflammation; we therefore aimed to answer questions about the role of microbiome and gut-derived toxins in acute kidney injury. PubMed and Cochrane Library were searched from inception to October 10, 2020 for relevant studies with an additional search performed on ClinicalTrials.gov. We identified 33 eligible articles and one ongoing trial (21 original studies and 12 reviews/commentaries), which were included in this systematic review. Experimental studies prove the existence of a kidney-gut axis, focusing on the role of gut-derived uremic toxins and providing concepts that modification of the microbiota composition may result in better AKI outcomes. Small interventional studies in animal models and in humans show promising results, therefore, microbiome-targeted therapy for AKI treatment might be a promising possibility. -

Renal Papillary Necrosis in Infancy PETER HUSBAND* and K
Arch Dis Child: first published as 10.1136/adc.48.2.116 on 1 February 1973. Downloaded from Archives of Disease in Childhood, 1973, 48, 116. Renal papillary necrosis in infancy PETER HUSBAND* and K. A. HOWLETT From the Departments of Paediatrics and Radiology, Charing Cross Group of Hospitals, Fulham Hospital, London Husband, P., and Howlett, K. A. (1973). Archives of Disease in Childhood, 48, 116. Renal papillary necrosis in infancy. Two infants developed renal papillary necrosis after acute illnesses associated with dehydration. After a short oliguric phase there was a longer phase characterized by impaired urinary concen- tration, hyponatraemia, metabolic acidosis, and a raised blood urea. Intravenous urograms showed contrast collecting in the papillae, with subsequent sinus formation extending into the medulla. In one case impaired urinary concentration was still present 21 months after the initial illness. Renal papillary necrosis was originally described admitted to hospital 9 days later after he had been by Friedreich (1877) in a man aged 70 years. found in his cot, grey, with respiratory distress and a Since then the majority of further cases reported high temperature. 3 days before he had diarrhoea and have also been in adults. It has been thought to vomiting for 24 hours but subsequently tolerated feeds be uncommon and usually to have a fatal outcome of full cream Cow and Gate milk, 180 ml 5 times a day. He was again extremely ill: temperature 40 3 °C, pale, copyright. in infancy and childhood (Davies, Kennedy, and cyanosed with a rapid respiratory rate, but not dehydra- Roberts, 1969). In the newborn infant renal ted. -

Risk of Renal Function Decline in Patients with Ketamine-Associated Uropathy
International Journal of Environmental Research and Public Health Article Risk of Renal Function Decline in Patients with Ketamine-Associated Uropathy Shih-Hsiang Ou 1,2,3, Ling-Ying Wu 4, Hsin-Yu Chen 1,2, Chien-Wei Huang 1,2, Chih-Yang Hsu 1,2, Chien-Liang Chen 1,2 , Kang-Ju Chou 1,2, Hua-Chang Fang 1,2 and Po-Tsang Lee 1,2,* 1 Division of Nephrology, Department of Internal Medicine, Kaohsiung Veterans General Hospital, Kaohsiung 813, Taiwan; [email protected] (S.-H.O.); [email protected] (H.-Y.C.); [email protected] (C.-W.H.); [email protected] (C.-Y.H.); [email protected] (C.-L.C.); [email protected] (K.-J.C.); [email protected] (H.-C.F.) 2 Faculty of Medicine, School of Medicine, National Yang-Ming University, Taipei 112, Taiwan 3 Graduate Institute of Clinical Medicine, College of Medicine, Kaohsiung Medical University, Kaohsiung 807, Taiwan 4 Department of Obstetrics and Gynecology, Kaohsiung Chang Gung Memorial Hospital, Kaohsiung 833, Taiwan; [email protected] * Correspondence: [email protected]; Tel.: +886-7342-2121 (ext. 8090) Received: 8 August 2020; Accepted: 29 September 2020; Published: 4 October 2020 Abstract: Ketamine-associated diseases have been increasing with the rise in ketamine abuse. Ketamine-associated uropathy is one of the most common complications. We investigated the effects of ketamine-associated uropathy on renal health and determined predictors of renal function decline in chronic ketamine abusers. This retrospective cohort study analyzed 51 patients (22 with ketamine- associated hydronephrosis and 29 with ketamine cystitis) from Kaohsiung Veterans General Hospital in Taiwan. -
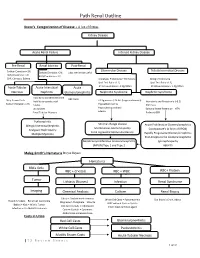
Path Renal Outline
Path Renal Outline Krane’s Categorization of Disease + A lot of Extras Kidney Disease Acute Renal Failure Intrinsic Kidney Disease Pre‐Renal Renal Intrinsic Post‐Renal Sodium Excretion <1% Glomerular Disease Tubulointerstitial Disease Sodium Excretion < 1% Sodium Excretion >2% Labs aren’t that useful BUN/Creatinine > 20 BUN/Creatinine < 10 CHF, Cirrhosis, Edema Urinalysis: Proteinuria + Hematuria Benign Proteinuria Spot Test Ratio >1.5, Spot Test Ratio <1.5, Acute Tubular Acute Interstitial Acute 24 Urine contains > 2.0g/24hrs 24 Urine contains < 1.0g/24hrs Necrosis Nephritis Glomerulonephritis Nephrotic Syndrome Nephritic Syndrome Inability to concentrate Urine RBC Casts Dirty Brown Casts Inability to secrete acid >3.5g protein / 24 hrs (huge proteinuria) Hematuria and Proteinuria (<3.5) Sodium Excretion >2% Edema Hypoalbuminemia RBC Casts Hypercholesterolemia Leukocytes Salt and Water Retention = HTN Focal Tubular Necrosis Edema Reduced GFR Pyelonephritis Minimal change disease Allergic Interstitial Nephritis Acute Proliferative Glomerulonephritis Membranous Glomerulopathy Analgesic Nephropathy Goodpasture’s (a form of RPGN) Focal segmental Glomerulosclerosis Rapidly Progressive Glomerulonephritis Multiple Myeloma Post‐Streptococcal Glomerulonephritis Membranoproliferative Glomerulonephritis IgA nephropathy (MPGN) Type 1 and Type 2 Alport’s Meleg‐Smith’s Hematuria Break Down Hematuria RBCs Only RBC + Crystals RBC + WBC RBC+ Protein Tumor Lithiasis (Stones) Infection Renal Syndrome Imaging Chemical Analysis Culture Renal Biopsy Calcium -

Acute Tubular Necrosıs After Nephrectomy: Case Presentatıon
Case Report JOJ Case Stud Volume 7 Issue 1 - May 2018 Copyright © All rights are reserved by Ebru Canakci DOI: 10.19080/JOJCS.2018.07.555703 Acute Tubular Necrosıs after Nephrectomy: Case Presentatıon Ebru Canakci1*, Ahmet Karatas2, Ahmet Gultekin1, Zubeyir Cebeci1, Ilker Coskun1 and Anıl Kılınc1 1Department of Anaesthesiology and Reanimation, Ordu University, Turkey 2Department of Internal Medicine & Nephrology, Ordu University, Turkey Submission: May 07, 2018; Published: May 18, 2018 *Corresponding author: Ebru Canakci, Faculty of Medicine, Department of Anaesthesiology and Reanimation, Ordu University, Ordu, Turkey, Email: Abstract ATN, contrary to prerenal azotemia, is not immediately cured upon the recovery of renal perfusion. In its severe form, renal hypoperfusion leads Acute renal failure (ARF) has a clinical presentation with declining renal function and glomerular filtration rate within hours-days. Ischemic trauma, severe hypovolemia, sepsis and severe burns. Acute kidney injury (AKI) is one of the frequently encountered causes of morbidity and mortalityto bilateral in renal hospitals. cortical The necrosis aim of this and study irreversible is to present renal the insufficiency. case with ATN Ischemic after major ATN often surgery develops and subsequent as a result permanent of major surgical kidney injuryintervention, in light of the information from the literature. Keywords: Nephrectomy; Acute Tubular Necrosis; Hemodialysis Introductıon and Objectıve to endogenous or exogenous toxins. Toxins cause intrarenal Acute renal failure (ARF) has a clinical presentation with vasoconstriction, direct tubular toxicity and/or intratubular obstruction and thus lead to ARF [4]. Acute kidney injury (AKI) hours-days. Although there are several differences in the declining renal function and glomerular filtration rate within is one of the frequently encountered causes of morbidity and mortality in hospitals. -

Original Article Thrombocytopenia As a Predictor of Acute Kidney Injury in Patients with Emphysematous Pyelonephritis
Int J Clin Exp Med 2019;12(1):849-854 www.ijcem.com /ISSN:1940-5901/IJCEM0078347 Original Article Thrombocytopenia as a predictor of acute kidney injury in patients with emphysematous pyelonephritis Heng Fan1,3*, Yu Zhao2*, Min Sun1, Jian-Hua Zhu1 1Department of Intensive Care Unit, Ningbo First Hospital, Ningbo, PR China; 2Department of Nephrology, Ningbo Urology and Nephrology Hospital, Ningbo, PR China; 3The Second School of Clinical Medicine, Southern Medical University, Guangzhou, PR China. *Equal contributors and co-first authors. Received April 22, 2018; Accepted September 12, 2018; Epub January 15, 2019; Published January 30, 2019 Abstract: Objective: The goal of this study was to investigate the relationship between thrombocytopenia and acute kidney injury (AKI) in patients with emphysematous pyelonephritis (EPN). Methods: A retrospective study was con- ducted in three university hospitals, and early hematological biomarkers were detected to predict the development of AKI in EPN patients. Results: Of 56 EPN patients, 32 (59%) developed AKI. Spearman correlation analysis showed that the nadir platelet count was negatively associated with the peak leukocyte count (r=-0.354, P<0.001), peak serum creatinine (r=-0.429, P<0.001), peak blood urea nitrogen (r=-0.317, P<0.001), and the length of hospital stay (r=-0.442, P<0.001). Furthermore, the area under the receiver-operating-characteristic curve (AU-ROC) was used to evaluate the accuracy of thrombocytopenia for the diagnosis of AKI in EPN patients, and the accuracy of nadir platelet count (AU-ROC: 0.92, 95% CI: 0.85-0.99, P<0.001) predicted AKI was significantly higher than admis- sion platelet count (AU-ROC: 0.84, 95% CI: 0.73-0.94, P<0.001). -

Effects of Bodybuilding Supplements on the Kidney
Ali et al. BMC Nephrology (2020) 21:164 https://doi.org/10.1186/s12882-020-01834-5 RESEARCH ARTICLE Open Access Effects of bodybuilding supplements on the kidney: A population-based incidence study of biopsy pathology and clinical characteristics among middle eastern men Alaa Abbas Ali1, Safaa E. Almukhtar2†, Dana A. Sharif3†, Zana Sidiq M. Saleem4†, Dana N. Muhealdeen1 and Michael D. Hughson1* Abstract Background: The incidence of kidney diseases among bodybuilders is unknown. Methods: Between January 2011 and December 2019, the Iraqi Kurdistan 15 to 39 year old male population averaged 1,100,000 with approximately 56,000 total participants and 25,000 regular participants (those training more than 1 year). Annual age specific incidence rates (ASIR) with (95% confidence intervals) per 100,000 bodybuilders were compared with the general age-matched male population. Results: Fifteen male participants had kidney biopsies. Among regular participants, diagnoses were: focal segmental glomerulosclerosis (FSGS), 2; membranous glomerulonephritis (MGN), 2; post-infectious glomeruonephritis (PIGN), 1; tubulointerstitial nephritis (TIN), 1; and nephrocalcinosis, 2. Acute tubular necrosis (ATN) was diagnosed in 5 regular participants and 2 participants training less than 1 year. Among regular participants, anabolic steroid use was self- reported in 26% and veterinary grade vitamin D injections in 2.6%. ASIR for FSGS, MGN, PIGN, and TIN among regular participants was not statistically different than the general population. ASIR of FSGS adjusted for anabolic steroid use was 3.4 (− 1.3 to 8.1), a rate overlapping with FSGS in the general population at 2.0 (1.2 to 2.8). ATN presented as exertional muscle injury with myoglobinuria among new participants. -

An Unusual Cause of Glomerular Hematuria and Acute Kidney Injury in a Chronic Kidney Disease Patient During Warfarin Therapy Clara Santos, Ana M
11617 14/5/13 12:11 Página 400 http://www.revistanefrologia.com casos clínicos © 2013 Revista Nefrología. Órgano Oficial de la Sociedad Española de Nefrología An unusual cause of glomerular hematuria and acute kidney injury in a chronic kidney disease patient during warfarin therapy Clara Santos, Ana M. Gomes, Ana Ventura, Clara Almeida, Joaquim Seabra Department of Nephrology. Centro Hospitalar Vila Nova de Gaia. Vila Nova de Gaia (Portugal) Nefrologia 2013;33(3):400-3 doi:10.3265/Nefrologia.pre2012.Oct.11617 ABSTRACT Un caso inusual de hematuria glomerular y fracaso renal agudo en un paciente con enfermedad renal crónica Warfarin is a well-established cause of gross hematuria. durante terapia con warfarina However, impaired kidney function does not occur RESUMEN except in the rare instance of severe blood loss or clot La warfarina es una causa muy conocida de hematuria ma- formation that obstructs the urinary tract. It has been croscópica. Sin embargo, el deterioro de la función renal no ocurre salvo en el caso inusual de gran pérdida de sangre o recently described an entity called warfarin-related formación de coágulos que obstruyen el tracto urinario. Re- nephropathy, in which acute kidney injury is caused by cientemente se ha descrito una entidad denominada nefro- glomerular hemorrhage and renal tubular obstruction patía relacionada con la warfarina en la que el fracaso renal by red blood cell casts. We report a patient under agudo es provocado por hemorragia glomerular y obstruc- warfarin treatment with chronic kidney disease, ción tubular renal por cilindros de glóbulos rojos. Exponemos macroscopic hematuria and acute kidney injury. -

Renal Artery Stenosis Management Strategies: an Updated Comparative Effectiveness Review Comparative Effectiveness Review Number 179
Comparative Effectiveness Review Number 179 Renal Artery Stenosis Management Strategies: An Updated Comparative Effectiveness Review Comparative Effectiveness Review Number 179 Renal Artery Stenosis Management Strategies: An Updated Comparative Effectiveness Review Prepared for: Agency for Healthcare Research and Quality U.S. Department of Health and Human Services 5600 Fishers Lane Rockville, MD 20857 www.ahrq.gov Contract No. 290-2015-00002-I Prepared by: Brown Evidence-based Practice Center Providence, RI Investigators: Ethan M. Balk, M.D., M.P.H. Gowri Raman, M.D., M.S. Gaelen P. Adam, M.L.I.S. Christopher W. Halladay, B.A., Sc.M. Valerie N. Langberg, Sc.M. Ijeoma A. Azodo, M.D., Ch.M. Thomas A. Trikalinos, M.D., Ph.D. AHRQ Publication No. 16-EHC026-EF August 2016 This report is based on research conducted by the Brown Evidence-based Practice Center (EPC) under contract to the Agency for Healthcare Research and Quality (AHRQ), Rockville, MD (Contract No. 290-2015-00002-I). The findings and conclusions in this document are those of the authors, who are responsible for its contents; the findings and conclusions do not necessarily represent the views of AHRQ. Therefore, no statement in this report should be construed as an official position of AHRQ or of the U.S. Department of Health and Human Services. None of the investigators have any affiliations or financial involvement that conflicts with the material presented in this report. The information in this report is intended to help health care decisionmakers—patients and clinicians, health system leaders, and policymakers, among others—make well-informed decisions and thereby improve the quality of health care services. -

Acute Toxic Nephropathies: Clinical Pathologic Correlations - ROBERT C
ANNALS OF CLINICAL AND LABORATORY SCIENCE, Vol. 6, No. 6 Copyright © 1976, Institute for Clinical Science Acute Toxic Nephropathies: Clinical Pathologic Correlations - ROBERT C. MUEHRCKE, M.D.,* FREDERICK I. VOLINI, M.D.,f ARTHUR M. MORRIS, M.D.,f JOSEPH B. MOLES, M.D.,f and ARTHUR G. LAWRENCE, M.D.,f *West Suburban Kidney Center and fWest Suburban Hospital, Oak Park, IL 60302 ABSTRACT Man’s ever increasing exposure to numerous drugs and chemicals, which are the results of medical and industrial progress, produces a by-product of acute toxic nephropathies. These include acute toxic renal failure, drug- induced acute oliguric renal failure, acute hemorrhagic glomerulonephritis, nephrotic syndrome, tubular disturbances and potassium deficiency. In depth information is provided for the previously mentioned disorders. Introduction have extremely vascular renal medullae Acute toxic nephropathy is a by and rete mirabile that function in the product of man’s ever increasing expo final dilution and concentration of the sure to a vast array of various chemicals urine. This complex mechanism results and drugs that result from industrial and in hypertonicity of the renal interstitium medical progress. The kidney, with its with concentration of nephrotoxic chemi rich blood supply, numerous enzyme sys cals, biologic products and drugs. tems and superior excretory function, is In our experience, approximately 25 especially vulnerable to the adverse ef percent of all patients with acute oliguria fects of chemicals, biologic products and have renal failure induced by drugs or drugs.44,226 The kidneys comprise 0.4 chem icals.188 The other main clinical percent of the total body weight and re syndrome of toxic nephropathy include quire a high oxygen consumption. -

Acute Kidney Injury in Urology Patients: Incidence, Causes and Outcomes
Nephro Urol Mon. 2013 November; 5(5): 955-61. DOI: 10.5812/numonthly.12721 Research Article Published online 2013 November 13. Acute Kidney Injury in Urology Patients: Incidence, Causes and Outcomes 1 1 2,3 2,3,* Giacomo Caddeo , Simon T. Williams , Christopher W. McIntyre , Nicholas M. Selby 1Department of Urology, Royal Derby Hospital, Derby, UK 2Department of Renal Medicine, Royal Derby Hospital, Derby, UK 3Division of Medical Sciences and Graduate Entry Medicine, School of Medicine, University of Nottingham, Nottingham, UK *Corresponding author : Nicholas M. Selby, Department of Renal Medicine, Royal Derby Hospital, Uttoxeter Road, DE22 3NE, Derby, UK. Tel:+44-01332340131, Fax: +44-01332789352, E-mail: [email protected]. Received: ; Accepted: June 5, 2013 June 27, 2013 Background: Acute kidney injury (AKI) is common in hospitalised patients and is associated with high mortality rates. However, the epidemiology of AKI in urology patients may differ due to a higher proportion of post-renal causes and surgical procedures that result in the intentional removal of renal parenchyma. Objectives: We performed a study to examine the incidence, aetiology and outcomes of AKI in a urological population. Patients and Methods: We performed a single-centre observational study including all hospitalised patients who sustained AKI within the Urology Department over an 18 month period. Patients with AKI were prospectively identified by a hospital-wide, electronic AKI reporting system that also allows demographic, hospital admission and co-morbidity data collection. Data regarding aetiology of AKI and details of surgical procedures were added retrospectively by manual case-note search. Results: 587 episodes of AKI occurred in 410 urology patients, giving an overall incidence of 6.7%.