Fungal Diseases of Horses
Total Page:16
File Type:pdf, Size:1020Kb
Load more
Recommended publications
-

Candida Krusei: Biology, Epidemiology, Pathogenicity and Clinical Manifestations of an Emerging Pathogen
J. Med. Microbiol. - Vol. 41 (1994), 295-310 0 1994 The Pathological Society of Great Britain and Ireland REVIEW ARTICLE: CLINICAL MYCOLOGY Candida krusei: biology, epidemiology, pathogenicity and clinical manifestations of an emerging pathogen YUTHIKA H. SAMARANAYAKE and L. P. SAMARANAYAKE” Department of Pathology (Oral), Faculty of Medicine and Ord diology Unit, Faculty of Dentistry, University of Hong Kong, 34 Hospital Road, Hong Kong Summary. Early reports of Candida krusei in man describe the organism as a transient, infrequent isolate of minor clinical significance inhabiting the mucosal surfaces. More recently it has emerged as a notable pathogen with a spectrum of clinical manifestations such as fungaemia, endophthalmitis, arthritis and endocarditis, most of which usually occur in compromised patient groups in a nosocomial setting. The advent of human immunodeficiency virus infection and the widespread use of the newer triazole fluconazole to suppress fungal infections in these patients have contributed to a significant increase in C. krusei infection, particularly because of the high incidence of resistance of the yeast to this drug. Experimental studies have generally shown C. krusei to be less virulent than C. albicans in terms of its adherence to both epithelial and prosthetic surfaces, proteolytic potential and production of phospholipases. Furthermore, it would seem that C. krusei is significantlydifferent from other medically important Candida spp. in its structural and metabolic features, and exhibits different behaviour patterns towards host defences, adding credence to the belief that it should be re-assigned taxonomically. An increased awareness of the pathogenic potential of this yeast coupled with the newer molecular biological approaches to its study may facilitate the continued exploration of the epidemiology and pathogenesis of C. -

Coccidioides Immitis
24/08/2017 FUNGAL AGENTS CAUSING INFECTION OF THE LUNG Microbiology Lectures of the Respiratory Diseases Prepared by: Rizalinda Sjahril Microbiology Department Faculty of Medicine Hasanuddin University 2016 OVERVIEW OF CLINICAL MYCOLOGY . Among 150.000 fungi species only 100-150 are human pathogens 25 spp most common pathogens . Majority are saprophyticLiving on dead or decayed organic matter . Transmission Person to person (rare) SPORE INHALATION OR ENTERS THE TISSUE FROM TRAUMA Animal to person (rare) – usually in dermatophytosis 1 24/08/2017 OVERVIEW OF CLINICAL MYCOLOGY . Human is usually resistant to infection, unless: Immunoscompromised (HIV, DM) Serious underlying disease Corticosteroid/antimetabolite treatment . Predisposing factors: Long term intravenous cannulation Complex surgical procedures Prolonged/excessive antibacterial therapy OVERVIEW OF CLINICAL MYCOLOGY . Several fungi can cause a variety of infections: clinical manifestation and severity varies. True pathogens -- have the ability to cause infection in otherwise healthy individuals 2 24/08/2017 Opportunistic/deep mycoses which affect the respiratory system are: Cryptococcosis Aspergillosis Zygomycosis True pathogens are: Blastomycosis Seldom severe Treatment not required unless extensive tissue Coccidioidomycosis destruction compromising respiratory status Histoplasmosis Or extrapulmonary fungal dissemination Paracoccidioidomycosis COMMON PATHOGENS OBTAINED FROM SPECIMENS OF PATIENTS WITH RESPIRATORY DISEASE Fungi Common site of Mode of Infectious Clinical -

Serious Fungal Infections in Peru
Eur J Clin Microbiol Infect Dis DOI 10.1007/s10096-017-2924-9 ORIGINAL ARTICLE Serious fungal infections in Peru B. Bustamante1 & D. W. Denning2 & P. E. Campos3 Received: 21 December 2016 /Accepted: 21 December 2016 # Springer-Verlag Berlin Heidelberg 2017 Abstract Epidemiological data about mycotic diseases are This first attempt to assess the fungal burden in Peru needs limited in Peru and estimation of the fungal burden has not to be refined. We believe the figure obtained is an underesti- been previously attempted. Data were obtained from the mation, because of under diagnosis, non-mandatory reporting Peruvian National Institute of Statistics and Informatics, and lack of a surveillance system and of good data about the UNAIDS and from the Ministry of Health’s publications. size of populations at risk. We also searched the bibliography for Peruvian data on my- cotic diseases, asthma, COPD, cancer and transplants. Incidence or prevalence for each fungal disease were estimat- Introduction ed in specific populations at risk. The Peruvian population for 2015 was 31,151,543. In 2014, the estimated number of HIV/ While candidemia and invasive aspergillosis (IA) are clearly AIDS and pulmonary tuberculosis cases was 88,625, 38,581 recognized as important causes of morbidity and mortality, of them not on ART, and 22,027, respectively. A total of other mycotic agents or different clinical presentations are im- 581,174 cases of fungal diseases were estimated, representing portant in specific regions. Socio-economic and geo- approximately 1.9% of the Peruvian population. This figure ecological characteristics and size of susceptible populations includes 498,606, 17,361 and 4,431 vulvovaginal, oral and are the main determinants of variations on incidence of fungal esophageal candidiasis, respectively, 1,557 candidemia cases, infections across the world. -

Candida Auris
microorganisms Review Candida auris: Epidemiology, Diagnosis, Pathogenesis, Antifungal Susceptibility, and Infection Control Measures to Combat the Spread of Infections in Healthcare Facilities Suhail Ahmad * and Wadha Alfouzan Department of Microbiology, Faculty of Medicine, Kuwait University, P.O. Box 24923, Safat 13110, Kuwait; [email protected] * Correspondence: [email protected]; Tel.: +965-2463-6503 Abstract: Candida auris, a recently recognized, often multidrug-resistant yeast, has become a sig- nificant fungal pathogen due to its ability to cause invasive infections and outbreaks in healthcare facilities which have been difficult to control and treat. The extraordinary abilities of C. auris to easily contaminate the environment around colonized patients and persist for long periods have recently re- sulted in major outbreaks in many countries. C. auris resists elimination by robust cleaning and other decontamination procedures, likely due to the formation of ‘dry’ biofilms. Susceptible hospitalized patients, particularly those with multiple comorbidities in intensive care settings, acquire C. auris rather easily from close contact with C. auris-infected patients, their environment, or the equipment used on colonized patients, often with fatal consequences. This review highlights the lessons learned from recent studies on the epidemiology, diagnosis, pathogenesis, susceptibility, and molecular basis of resistance to antifungal drugs and infection control measures to combat the spread of C. auris Citation: Ahmad, S.; Alfouzan, W. Candida auris: Epidemiology, infections in healthcare facilities. Particular emphasis is given to interventions aiming to prevent new Diagnosis, Pathogenesis, Antifungal infections in healthcare facilities, including the screening of susceptible patients for colonization; the Susceptibility, and Infection Control cleaning and decontamination of the environment, equipment, and colonized patients; and successful Measures to Combat the Spread of approaches to identify and treat infected patients, particularly during outbreaks. -

Molecular Analysis of Dermatophytes Suggests Spread of Infection Among Household Members
Molecular Analysis of Dermatophytes Suggests Spread of Infection Among Household Members Mahmoud A. Ghannoum, PhD; Pranab K. Mukherjee, PhD; Erin M. Warshaw, MD; Scott Evans, PhD; Neil J. Korman, MD, PhD; Amir Tavakkol, PhD, DipBact Practice Points When a patient presents with tinea pedis or onychomycosis, inquire if other household members also have the infection, investigate if they have a history of concomitant tinea pedis and onychomycosis, and examine for plantar scaling and/or nail discoloration. If the variables above areCUTIS observed, think about spread of infection and treatment options. Dermatophyte infection from the same strains may Drs. Ghannoum, Mukherjee, and Korman are from University be an important route for transmission of derma- Hospitals Case Medical Center, Cleveland, Ohio. Dr. Warshaw is from the University of Minnesota, Minneapolis, and Minneapolis Veterans tophytoses within a household. In this study, we AffairsDo Medical Center. Dr. Evans is from Notthe Harvard School of Public used molecularCopy methods to identify dermatophytes Health, Boston, Massachusetts. Dr. Tavakkol was from Novartis in members of dermatophyte-infected households Pharmaceuticals Corporation, East Hanover, New Jersey, and and evaluated variables associated with the currently is from Topica Pharmaceuticals, Inc, Los Altos, California. spread of infection. Fungal species were identi- This article was supported by a grant from Novartis Pharmaceuticals Corporation. Dr. Ghannoum has served as a consultant and/or fied by polymerase chain reaction (PCR) using speaker for and has received grants and contracts from Merck & Co, primers targeting the internal transcribed spacer Inc; Novartis Pharmaceuticals Corporation; Pfizer Inc; and Stiefel, (ITS) regions (ITS1 and ITS4). For strain differen- a GSK company. -

Dermatophyte and Non-Dermatophyte Onychomycosis in Singapore
Australas J. Dermatol 1992; 33: 159-163 DERMATOPHYTE AND NON-DERMATOPHYTE ONYCHOMYCOSIS IN SINGAPORE JOYCE TENG-EE LIM, HOCK CHENG CHUA AND CHEE LEOK GOH Singapore SUMMARY Onychomycosis is caused by dermatophytes, moulds and yeasts. It is important to identify the non-dermatophyte moulds as they are resistant to the usual anti-fungals. A prospective study was undertaken in the National Skin Centre, Singapore to study the pattern of dermatophyte and non-dermatophyte onychomycosis. 53 male and 47 female patients seen between June 1990 and June 1991 were entered into the study. Direct microscopy was done and the nail clippings were cultured. Toe and finger nails were equally infected. Dermatophytes were isolated from 21 patients namely, T. rubrum (12/21), T. interdigitale (5/21), T. mentagrophytes (3/21) and T. violaceum (1/21). Candida onychomycosis occurred in 39 patients and was caused by C. albicans (38/39) and C. parapsilosis (1/39). 37/39 patients had associated paronychia. 5 types of moulds were isolated from 12 patients, namely Fusarium species (6/12), Aspergillus species (3/12), S. brevicaulis (1/12), Aureobasilium species (1/12) and Penicillium species (1/12). Although the clinical pattern and microscopy may predict the type of organisms, in practice this is difficult. Only cultures were confirmatory. 28% (28/100) had negative cultures despite a positive microscopy, and moulds (12/100) grown might be contaminants rather than pathogens. Key words: Moulds, yeasts, fungi, tinea, onychomycosis, dermatophyte, non-dermatophyte INTRODUCTION METHODS AND MATERIALS Onychomycosis, a common nail disorder, is 100 consecutive patients, seen in our centre caused by dermatophytes, non-dermatophyte between June 1990 and June 1991, with a new moulds, or yeasts. -

Turning on Virulence: Mechanisms That Underpin the Morphologic Transition and Pathogenicity of Blastomyces
Virulence ISSN: 2150-5594 (Print) 2150-5608 (Online) Journal homepage: http://www.tandfonline.com/loi/kvir20 Turning on Virulence: Mechanisms that underpin the Morphologic Transition and Pathogenicity of Blastomyces Joseph A. McBride, Gregory M. Gauthier & Bruce S. Klein To cite this article: Joseph A. McBride, Gregory M. Gauthier & Bruce S. Klein (2018): Turning on Virulence: Mechanisms that underpin the Morphologic Transition and Pathogenicity of Blastomyces, Virulence, DOI: 10.1080/21505594.2018.1449506 To link to this article: https://doi.org/10.1080/21505594.2018.1449506 © 2018 The Author(s). Published by Informa UK Limited, trading as Taylor & Francis Group© Joseph A. McBride, Gregory M. Gauthier and Bruce S. Klein Accepted author version posted online: 13 Mar 2018. Submit your article to this journal Article views: 15 View related articles View Crossmark data Full Terms & Conditions of access and use can be found at http://www.tandfonline.com/action/journalInformation?journalCode=kvir20 Publisher: Taylor & Francis Journal: Virulence DOI: https://doi.org/10.1080/21505594.2018.1449506 Turning on Virulence: Mechanisms that underpin the Morphologic Transition and Pathogenicity of Blastomyces Joseph A. McBride, MDa,b,d, Gregory M. Gauthier, MDa,d, and Bruce S. Klein, MDa,b,c a Division of Infectious Disease, Department of Medicine, University of Wisconsin School of Medicine and Public Health, 600 Highland Avenue, Madison, WI 53792, USA; b Division of Infectious Disease, Department of Pediatrics, University of Wisconsin School of Medicine and Public Health, 1675 Highland Avenue, Madison, WI 53792, USA; c Department of Medical Microbiology and Immunology, University of Wisconsin School of Medicine and Public Health, 1550 Linden Drive, Madison, WI 53706, USA. -

Managing Athlete's Foot
South African Family Practice 2018; 60(5):37-41 S Afr Fam Pract Open Access article distributed under the terms of the ISSN 2078-6190 EISSN 2078-6204 Creative Commons License [CC BY-NC-ND 4.0] © 2018 The Author(s) http://creativecommons.org/licenses/by-nc-nd/4.0 REVIEW Managing athlete’s foot Nkatoko Freddy Makola,1 Nicholus Malesela Magongwa,1 Boikgantsho Matsaung,1 Gustav Schellack,2 Natalie Schellack3 1 Academic interns, School of Pharmacy, Sefako Makgatho Health Sciences University 2 Clinical research professional, pharmaceutical industry 3 Professor, School of Pharmacy, Sefako Makgatho Health Sciences University *Corresponding author, email: [email protected] Abstract This article is aimed at providing a succinct overview of the condition tinea pedis, commonly referred to as athlete’s foot. Tinea pedis is a very common fungal infection that affects a significantly large number of people globally. The presentation of tinea pedis can vary based on the different clinical forms of the condition. The symptoms of tinea pedis may range from asymptomatic, to mild- to-severe forms of pain, itchiness, difficulty walking and other debilitating symptoms. There is a range of precautionary measures available to prevent infection, and both oral and topical drugs can be used for treating tinea pedis. This article briefly highlights what athlete’s foot is, the different causes and how they present, the prevalence of the condition, the variety of diagnostic methods available, and the pharmacological and non-pharmacological management of the -

Oral Antifungals Month/Year of Review: July 2015 Date of Last
© Copyright 2012 Oregon State University. All Rights Reserved Drug Use Research & Management Program Oregon State University, 500 Summer Street NE, E35 Salem, Oregon 97301-1079 Phone 503-947-5220 | Fax 503-947-1119 Class Update with New Drug Evaluation: Oral Antifungals Month/Year of Review: July 2015 Date of Last Review: March 2013 New Drug: isavuconazole (a.k.a. isavunconazonium sulfate) Brand Name (Manufacturer): Cresemba™ (Astellas Pharma US, Inc.) Current Status of PDL Class: See Appendix 1. Dossier Received: Yes1 Research Questions: Is there any new evidence of effectiveness or safety for oral antifungals since the last review that would change current PDL or prior authorization recommendations? Is there evidence of superior clinical cure rates or morbidity rates for invasive aspergillosis and invasive mucormycosis for isavuconazole over currently available oral antifungals? Is there evidence of superior safety or tolerability of isavuconazole over currently available oral antifungals? • Is there evidence of superior effectiveness or safety of isavuconazole for invasive aspergillosis and invasive mucormycosis in specific subpopulations? Conclusions: There is low level evidence that griseofulvin has lower mycological cure rates and higher relapse rates than terbinafine and itraconazole for adult 1 onychomycosis.2 There is high level evidence that terbinafine has more complete cure rates than itraconazole (55% vs. 26%) for adult onychomycosis caused by dermatophyte with similar discontinuation rates for both drugs.2 There is low -

HIV Infection and AIDS
G Maartens 12 HIV infection and AIDS Clinical examination in HIV disease 306 Prevention of opportunistic infections 323 Epidemiology 308 Preventing exposure 323 Global and regional epidemics 308 Chemoprophylaxis 323 Modes of transmission 308 Immunisation 324 Virology and immunology 309 Antiretroviral therapy 324 ART complications 325 Diagnosis and investigations 310 ART in special situations 326 Diagnosing HIV infection 310 Prevention of HIV 327 Viral load and CD4 counts 311 Clinical manifestations of HIV 311 Presenting problems in HIV infection 312 Lymphadenopathy 313 Weight loss 313 Fever 313 Mucocutaneous disease 314 Gastrointestinal disease 316 Hepatobiliary disease 317 Respiratory disease 318 Nervous system and eye disease 319 Rheumatological disease 321 Haematological abnormalities 322 Renal disease 322 Cardiac disease 322 HIV-related cancers 322 306 • HIV INFECTION AND AIDS Clinical examination in HIV disease 2 Oropharynx 34Neck Eyes Mucous membranes Lymph node enlargement Retina Tuberculosis Toxoplasmosis Lymphoma HIV retinopathy Kaposi’s sarcoma Progressive outer retinal Persistent generalised necrosis lymphadenopathy Parotidomegaly Oropharyngeal candidiasis Cytomegalovirus retinitis Cervical lymphadenopathy 3 Oral hairy leucoplakia 5 Central nervous system Herpes simplex Higher mental function Aphthous ulcers 4 HIV dementia Kaposi’s sarcoma Progressive multifocal leucoencephalopathy Teeth Focal signs 5 Toxoplasmosis Primary CNS lymphoma Neck stiffness Cryptococcal meningitis 2 Tuberculous meningitis Pneumococcal meningitis 6 -
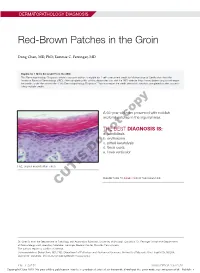
Red-Brown Patches in the Groin
DERMATOPATHOLOGY DIAGNOSIS Red-Brown Patches in the Groin Dong Chen, MD, PhD; Tammie C. Ferringer, MD Eligible for 1 MOC SA Credit From the ABD This Dermatopathology Diagnosis article in our print edition is eligible for 1 self-assessment credit for Maintenance of Certification from the American Board of Dermatology (ABD). After completing this activity, diplomates can visit the ABD website (http://www.abderm.org) to self-report the credits under the activity title “Cutis Dermatopathology Diagnosis.” You may report the credit after each activity is completed or after accumu- lating multiple credits. A 66-year-old man presented with reddish arciform patchescopy in the inguinal area. THE BEST DIAGNOSIS IS: a. candidiasis b. noterythrasma c. pitted keratolysis d. tinea cruris Doe. tinea versicolor H&E, original magnification ×600. PLEASE TURN TO PAGE 419 FOR THE DIAGNOSIS CUTIS Dr. Chen is from the Department of Pathology and Anatomical Sciences, University of Missouri, Columbia. Dr. Ferringer is from the Departments of Dermatology and Laboratory Medicine, Geisinger Medical Center, Danville, Pennsylvania. The authors report no conflict of interest. Correspondence: Dong Chen, MD, PhD, Department of Pathology and Anatomical Sciences, University of Missouri, One Hospital Dr, MA204, DC018.00, Columbia, MO 65212 ([email protected]). 416 I CUTIS® WWW.MDEDGE.COM/CUTIS Copyright Cutis 2018. No part of this publication may be reproduced, stored, or transmitted without the prior written permission of the Publisher. DERMATOPATHOLOGY DIAGNOSIS DISCUSSION THE DIAGNOSIS: Erythrasma rythrasma usually involves intertriginous areas surface (Figure 1) compared to dermatophyte hyphae that (eg, axillae, groin, inframammary area). Patients tend to be parallel to the surface.2 E present with well-demarcated, minimally scaly, red- Pitted keratolysis is a superficial bacterial infection brown patches. -

Tinea Capitis 2014 L.C
BJD GUIDELINES British Journal of Dermatology British Association of Dermatologists’ guidelines for the management of tinea capitis 2014 L.C. Fuller,1 R.C. Barton,2 M.F. Mohd Mustapa,3 L.E. Proudfoot,4 S.P. Punjabi5 and E.M. Higgins6 1Department of Dermatology, Chelsea & Westminster Hospital, Fulham Road, London SW10 9NH, U.K. 2Department of Microbiology, Leeds General Infirmary, Leeds LS1 3EX, U.K. 3British Association of Dermatologists, Willan House, 4 Fitzroy Square, London W1T 5HQ, U.K. 4St John’s Institute of Dermatology, Guy’s and St Thomas’ NHS Foundation Trust, St Thomas’ Hospital, Westminster Bridge Road, London SE1 7EH, U.K. 5Department of Dermatology, Hammersmith Hospital, 150 Du Cane Road, London W12 0HS, U.K. 6Department of Dermatology, King’s College Hospital, Denmark Hill, London SE5 9RS, U.K. 1.0 Purpose and scope Correspondence Claire Fuller. The overall objective of this guideline is to provide up-to- E-mail: [email protected] date, evidence-based recommendations for the management of tinea capitis. This document aims to update and expand Accepted for publication on the previous guidelines by (i) offering an appraisal of 8 June 2014 all relevant literature since January 1999, focusing on any key developments; (ii) addressing important, practical clini- Funding sources cal questions relating to the primary guideline objective, i.e. None. accurate diagnosis and identification of cases; suitable treat- ment to minimize duration of disease, discomfort and scar- Conflicts of interest ring; and limiting spread among other members of the L.C.F. has received sponsorship to attend conferences from Almirall, Janssen and LEO Pharma (nonspecific); has acted as a consultant for Alliance Pharma (nonspe- community; (iii) providing guideline recommendations and, cific); and has legal representation for L’Oreal U.K.