DVT Upper Extremity
Total Page:16
File Type:pdf, Size:1020Kb
Load more
Recommended publications
-

Prep for Practical II
Images for Practical II BSC 2086L "Endocrine" A A B C A. Hypothalamus B. Pineal Gland (Body) C. Pituitary Gland "Endocrine" 1.Thyroid 2.Adrenal Gland 3.Pancreas "The Pancreas" "The Adrenal Glands" "The Ovary" "The Testes" Erythrocyte Neutrophil Eosinophil Basophil Lymphocyte Monocyte Platelet Figure 29-3 Photomicrograph of a human blood smear stained with Wright’s stain (765). Eosinophil Lymphocyte Monocyte Platelets Neutrophils Erythrocytes "Blood Typing" "Heart Coronal" 1.Right Atrium 3 4 2.Superior Vena Cava 5 2 3.Aortic Arch 6 4.Pulmonary Trunk 1 5.Left Atrium 12 9 6.Bicuspid Valve 10 7.Interventricular Septum 11 8.Apex of The Heart 9. Chordae tendineae 10.Papillary Muscle 7 11.Tricuspid Valve 12. Fossa Ovalis "Heart Coronal Section" Coronal Section of the Heart to show valves 1. Bicuspid 2. Pulmonary Semilunar 3. Tricuspid 4. Aortic Semilunar 5. Left Ventricle 6. Right Ventricle "Heart Coronal" 1.Pulmonary trunk 2.Right Atrium 3.Tricuspid Valve 4.Pulmonary Semilunar Valve 5.Myocardium 6.Interventricular Septum 7.Trabeculae Carneae 8.Papillary Muscle 9.Chordae Tendineae 10.Bicuspid Valve "Heart Anterior" 1. Brachiocephalic Artery 2. Left Common Carotid Artery 3. Ligamentum Arteriosum 4. Left Coronary Artery 5. Circumflex Artery 6. Great Cardiac Vein 7. Myocardium 8. Apex of The Heart 9. Pericardium (Visceral) 10. Right Coronary Artery 11. Auricle of Right Atrium 12. Pulmonary Trunk 13. Superior Vena Cava 14. Aortic Arch 15. Brachiocephalic vein "Heart Posterolateral" 1. Left Brachiocephalic vein 2. Right Brachiocephalic vein 3. Brachiocephalic Artery 4. Left Common Carotid Artery 5. Left Subclavian Artery 6. Aortic Arch 7. -
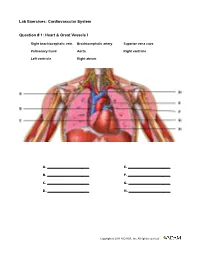
Lab Exercises: Cardiovascular System Question # 1: Heart & Great Vessels I
Lab Exercises: Cardiovascular System Question # 1: Heart & Great Vessels I Right brachiocephalic vein Brachiocephalic artery Superior vena cava Pulmonary trunk Aorta Right ventricle Left ventricle Right atrium A. E. B. F. C. G. D. H. Copyright © 2011 A.D.A.M., Inc. All rights reserved. Lab Exercises: Cardiovascular System Question # 2: Heart & Great Vessels II Left common carotid artery Brachiocephalic trunk Left subclavian artery Left brachiocephalic vein Left pulmonary artery Inferior vena cava Right pulmonary artery Right pulmonary vein A. E. B. F. C. G. D. H. Copyright © 2011 A.D.A.M., Inc. All rights reserved. Lab Exercises: Cardiovascular System Question # 3: Heart & Great Vessels (Post) Left pulmonary artery Left subclavian artery Right brachiocephalic vein Left common carotid artery Right pulmonary artery Right pulmonary vein Left pulmonary vein Inferior vena cava A. E. B. F. C. G. D. H. Copyright © 2011 A.D.A.M., Inc. All rights reserved. Lab Exercises: Cardiovascular System Question # 4: Arteries of Head & Neck Occipital artery Superficial temporal artery External carotid artery Internal carotid artery Facial artery Vertebral artery Common carotid artery A. E. B. F. C. G. D. Copyright © 2011 A.D.A.M., Inc. All rights reserved. Lab Exercises: Cardiovascular System Question # 5: Arteries of Trunk I Axillary artery Brachiocephailic trunk Right common carotid artery Left common carotid artery Left subclavian artery Axillary artery Arch of aorta Thoracic aorta A. E. B. F. C. G. D. H. Copyright © 2011 A.D.A.M., Inc. All rights reserved. Lab Exercises: Cardiovascular System Question # 6: Arteries of Trunk II Femoral artery Left common iliac artery Superior mesenteric artery Celiac trunk Inferior mesenteric artery Right renal artery Right testicular artery Left renal artery A. -

Vessels and Circulation
CARDIOVASCULAR SYSTEM OUTLINE 23.1 Anatomy of Blood Vessels 684 23.1a Blood Vessel Tunics 684 23.1b Arteries 685 23.1c Capillaries 688 23 23.1d Veins 689 23.2 Blood Pressure 691 23.3 Systemic Circulation 692 Vessels and 23.3a General Arterial Flow Out of the Heart 693 23.3b General Venous Return to the Heart 693 23.3c Blood Flow Through the Head and Neck 693 23.3d Blood Flow Through the Thoracic and Abdominal Walls 697 23.3e Blood Flow Through the Thoracic Organs 700 Circulation 23.3f Blood Flow Through the Gastrointestinal Tract 701 23.3g Blood Flow Through the Posterior Abdominal Organs, Pelvis, and Perineum 705 23.3h Blood Flow Through the Upper Limb 705 23.3i Blood Flow Through the Lower Limb 709 23.4 Pulmonary Circulation 712 23.5 Review of Heart, Systemic, and Pulmonary Circulation 714 23.6 Aging and the Cardiovascular System 715 23.7 Blood Vessel Development 716 23.7a Artery Development 716 23.7b Vein Development 717 23.7c Comparison of Fetal and Postnatal Circulation 718 MODULE 9: CARDIOVASCULAR SYSTEM mck78097_ch23_683-723.indd 683 2/14/11 4:31 PM 684 Chapter Twenty-Three Vessels and Circulation lood vessels are analogous to highways—they are an efficient larger as they merge and come closer to the heart. The site where B mode of transport for oxygen, carbon dioxide, nutrients, hor- two or more arteries (or two or more veins) converge to supply the mones, and waste products to and from body tissues. The heart is same body region is called an anastomosis (ă-nas ′tō -mō′ sis; pl., the mechanical pump that propels the blood through the vessels. -

Brachial Artery
VASCULAR Anatomy of the upper limb Dr Jamila EL M edany & Dr. Essam Eldin Salama Objectives At the end of the lecture, the students should be able to: • Identify the origin of the vascular supply for the upper limb. • Describe the main arteries and their branches of the arm, forearm & hand. • Describe the vascular arches for the hand. • Describe the superficial and deep veins of the upper limb Arteries Of The Upper Limb Right subclavian Left subclavian artery artery Axillary artery Brachial artery Ulnar artery Radial artery Palmar arches The Subclavian Artery The right artery originates from the brachiocephalic artery. The left artery Cotinues as originates from Axillary artery at the arch of the the lateral border aorta of the 1st rib The Axillary Artery Begins at the lateral border of the st 1 rib as continuation of the Subclavian artery subclavian artery. Continues as brachial artery at lower border of teres major muscle. Is closely related to the cords of brachial plexus and their branches Is enclosed within the axillary sheath. Is crossed anteriorly by the pectoralis minor muscle, and is st nd divided into three parts; 1 , 2 & Brachial artery Axillary artery 3rd. The 1st part of the axillary artery . Extends from the lateral st border of 1 rib to upper 1st part border of the pectoralis 2nd part minor muscle. Highest thoracic artery a. Related: 3rd part Pectoralis • Anterioly: to the minor pectoralis major muscle • Laterally: to the cords Teres of the brachial plexus. major . It gives; ONE branch: Highest thoracic artery The 2nd part of the axillary artery . -

Anatomy and Physiology in Relation to Compression of the Upper Limb and Thorax
Clinical REVIEW anatomy and physiology in relation to compression of the upper limb and thorax Colin Carati, Bren Gannon, Neil Piller An understanding of arterial, venous and lymphatic flow in the upper body in normal limbs and those at risk of, or with lymphoedema will greatly improve patient outcomes. However, there is much we do not know in this area, including the effects of compression upon lymphatic flow and drainage. Imaging and measuring capabilities are improving in this respect, but are often expensive and time-consuming. This, coupled with the unknown effects of individual, diurnal and seasonal variances on compression efficacy, means that future research should focus upon ways to monitor the pressure delivered by a garment, and its effects upon the fluids we are trying to control. More is known about the possible This paper will describe the vascular Key words effects of compression on the anatomy of the upper limb and axilla, pathophysiology of lymphoedema when and will outline current understanding of Anatomy used on the lower limbs (Partsch and normal and abnormal lymph drainage. It Physiology Junger, 2006). While some of these will also explain the mechanism of action Lymphatics principles can be applied to guide the use of compression garments and will detail Compression of compression on the upper body, it is the effects of compression on fluid important that the practitioner is movement. knowledgeable about the anatomy and physiology of the upper limb, axilla and Vascular drainage of the upper limb thorax, and of the anatomical and vascular It is helpful to have an understanding of Little evidence exists to support the differences that exist between the upper the vascular drainage of the upper limb, use of compression garments in the and lower limb, so that the effects of these since the lymphatic drainage follows a treatment of lymphoedema, particularly differences can be considered when using similar course (Figure 1). -

Redalyc.Anatomical Study of the Accessory Axillary Vein in Cadavers
Jornal Vascular Brasileiro ISSN: 1677-5449 [email protected] Sociedade Brasileira de Angiologia e de Cirurgia Vascular Brasil Barbosa Felix, Valtuir; Bernardino dos Santos, José André; Jucá de Moraes Fernandes, Katharina; Rolemberg Gama Cabral, Dhayanna; Silva dos Santos, Carlos Adriano; de Sousa Rodrigues, Célio Fernando; Silva Brito Lima, Jacqueline; Casado Ramalho, Antônio José Anatomical study of the accessory axillary vein in cadavers: a contribution to the axillary surgical approach Jornal Vascular Brasileiro, vol. 15, núm. 4, octubre-diciembre, 2016, pp. 275-279 Sociedade Brasileira de Angiologia e de Cirurgia Vascular São Paulo, Brasil Available in: http://www.redalyc.org/articulo.oa?id=245049803004 How to cite Complete issue Scientific Information System More information about this article Network of Scientific Journals from Latin America, the Caribbean, Spain and Portugal Journal's homepage in redalyc.org Non-profit academic project, developed under the open access initiative ORIGINAL ARTICLE Anatomical study of the accessory axillary vein in cadavers: a contribution to the axillary surgical approach Estudo anatômico da veia axilar acessória em cadáveres: uma contribuição à abordagem cirúrgica axilar Valtuir Barbosa Felix1,2, José André Bernardino dos Santos2, Katharina Jucá de Moraes Fernandes2, 2 3 3 Dhayanna Rolemberg Gama Cabral *, Carlos Adriano Silva dos Santos , Célio Fernando de Sousa Rodrigues , Jacqueline Silva Brito Lima4, Antônio José Casado Ramalho2 Abstract Background: The axillary vein is an important blood vessel that participates in drainage of the upper limb. Some individuals present a second axillary vein (accessory axillary vein), which is an important collateral drainage path. Objectives: The goal of this study was to determine the incidence of the accessory axillary vein and to describe this vessel’s topography. -

The Cardiovascular System
11 The Cardiovascular System WHAT The cardiovascular system delivers oxygen and HOW nutrients to the body tissues The heart pumps and carries away wastes blood throughout the body such as carbon dioxide in blood vessels. Blood flow via blood. requires both the pumping action of the heart and changes in blood pressure. WHY If the cardiovascular system cannot perform its functions, wastes build up in tissues. INSTRUCTORS Body organs fail to function properly, New Building Vocabulary and then, once oxygen becomes Coaching Activities for this depleted, they will die. chapter are assignable in hen most people hear the term cardio- only with the interstitial fluid in their immediate Wvascular system, they immediately think vicinity. Thus, some means of changing and of the heart. We have all felt our own “refreshing” these fluids is necessary to renew the heart “pound” from time to time when we are ner- nutrients and prevent pollution caused by vous. The crucial importance of the heart has been the buildup of wastes. Like a bustling factory, the recognized for ages. However, the cardiovascular body must have a transportation system to carry system is much more than just the heart, and its various “cargoes” back and forth. Instead of from a scientific and medical standpoint, it is roads, railway tracks, and subways, the body’s important to understand why this system is so vital delivery routes are its hollow blood vessels. to life. Most simply stated, the major function of the Night and day, minute after minute, our tril- cardiovascular system is transportation. Using lions of cells take up nutrients and excrete wastes. -

Brachial Vein Transposition with Consecutive Skin Incisions in a Hemodialysis Patient with Absence of Adequate Superficial Veins: a Case Report
Original Article Case Report Case Vascular Specialist International Vol. 36, No. 4, December 2020 pISSN 2288-7970 • eISSN 2288-7989 Brachial Vein Transposition with Consecutive Skin Incisions in a Hemodialysis Patient with Absence of Adequate Superficial Veins: A Case Report Pouya Tayebi1, Fatemeh Mahmoudlou2, Yasaman Daryabari2, and Atefeh Shamsian3 1Department of Vascular and Endovascular Surgery, Rouhani Hospital, Babol University of Medical Sciences, Babol, 2Student Research Committee, Babol University of Medical Sciences, Babol, 3MSc student in nursing, Rajaie Cardiovascular Medical and Research Center, Iran University of Medical Sciences,Tehran, Iran The creation of an arteriovenous fistula instead of a synthetic vascular graft is a Received September 24, 2020 Revised November 5, 2020 smart decision in hemodialysis patients who do not have a suitable superficial vein. Accepted November 30, 2020 Basilic vein transposition (BVT) is a viable option in most cases, except in patients who do not have a proper basilic vein. In patients with inadequate superficial veins, another source of the autogenous vein is the brachial vein, a deep vein of the up- per arm. Most surgeons choose a full medial arm incision to perform brachial vein Corresponding author: Pouya Tayebi exploration. We describe a patient in whom BVT was not possible and so brachial Department of Vascular and Endovascular Surgery, Rouhani Hospital, Babol University vein transposition using skip incisions was performed, with good results. of Medical Sciences, Keshavarz Boulevard, -
The Surgical Anatomy of the Mammary Gland. Vascularisation, Innervation, Lymphatic Drainage, the Structure of the Axillary Fossa (Part 2.)
NOWOTWORY Journal of Oncology 2021, volume 71, number 1, 62–69 DOI: 10.5603/NJO.2021.0011 © Polskie Towarzystwo Onkologiczne ISSN 0029–540X Varia www.nowotwory.edu.pl The surgical anatomy of the mammary gland. Vascularisation, innervation, lymphatic drainage, the structure of the axillary fossa (part 2.) Sławomir Cieśla1, Mateusz Wichtowski1, 2, Róża Poźniak-Balicka3, 4, Dawid Murawa1, 2 1Department of General and Oncological Surgery, K. Marcinkowski University Hospital, Zielona Gora, Poland 2Department of Surgery and Oncology, Collegium Medicum, University of Zielona Gora, Poland 3Department of Radiotherapy, K. Marcinkowski University Hospital, Zielona Gora, Poland 4Department of Urology and Oncological Urology, Collegium Medicum, University of Zielona Gora, Poland Dynamically developing oncoplasty, i.e. the application of plastic surgery methods in oncological breast surgeries, requires excellent knowledge of mammary gland anatomy. This article presents the details of arterial blood supply and venous blood outflow as well as breast innervation with a special focus on the nipple-areolar complex, and the lymphatic system with lymphatic outflow routes. Additionally, it provides an extensive description of the axillary fossa anatomy. Key words: anatomy of the mammary gland The large-scale introduction of oncoplasty to everyday on- axillary artery subclavian artery cological surgery practice of partial mammary gland resec- internal thoracic artery thoracic-acromial artery tions, partial or total breast reconstructions with the use of branches to the mammary gland the patient’s own tissue as well as an artificial material such as implants has significantly changed the paradigm of surgi- cal procedures. A thorough knowledge of mammary gland lateral thoracic artery superficial anatomy has taken on a new meaning. -

Central Venous Access Techniques for Cardiac Implantable Electronic Devices
Review Devices Central Venous Access Techniques for Cardiac Implantable Electronic Devices Sergey Barsamyan and Kim Rajappan Cardiology Department, John Radcliffe Hospital, Oxford University Hospitals NHS Trust, Oxford, UK DOI: https://doi.org/10.17925/EJAE.2018.4.2.66 he implantation of cardiac implantable electronic devices remains one of the core skills for a cardiologist. This article aims to provide beginners with a practical ‘how to’ guide to the first half of the implantation procedure – central venous access. Comparative descriptions Tof cephalic cutdown technique, conventional subclavian, extrathoracic subclavian and axillary venous punctures are provided, with tips for technique selection and troubleshooting. Keywords Implantation of cardiac implantable electronic devices (CIEDs) remains one of the core skills of Pacemaker, pacing, implantation, cardiac cardiologists; most cardiology trainees will require at least basic skills in permanent pacemaker implantable electronic devices, CIED, (PPM) implantation.1 The aim of this article is to provide a guide to the techniques of venous central venous access, techniques access – the first and important part of the implantation procedure. The bulk of the provided instruction is based on our pacing lab experience and references are provided, where necessary, Disclosures: Sergey Barsamyan and Kim Rajappan have nothing to declare in relation to this article. to describe techniques utilised in other centres. No article can be totally comprehensive and cover Review Process: Double-blind peer review. all the subtleties of a procedure. Like for any practical skill, it is possible to give only the core Compliance with Ethics: This study involves a concepts in writing, and nothing can replace hands-on training supervised by an experienced review of the literature and did not involve implanter in a pacing theatre. -

View, There Is No Doubt That the Elbow Should Be Reduced and Repositioned As Soon As the Diagnosis
ACTA SCIENTIFIC MEDICAL SCIENCES (ISSN: 2582-0931) Volume 4 Issue 1 January 2020 Case Report Use of A Brachial Vein Conduit and A Rotational Skin Flap Graft Repairing A Vascular Trauma Yuniel Hernandez Castillo* Consultant Angiologist and Vascular Surgeon, General Surgery, Milton Cato Memorial Hospital, Saint Vincent and the Grenadines, Caribbean *Corresponding Author: Yuniel Hernandez Castillo, Consultant Angiologist and Vascular Surgeon, General Surgery, Milton Cato Memorial Hospital, Saint Vincent and the Grenadines, Caribbean. Received: November 22, 2019; Published: December 04, 2019 DOI: 10.31080/ASMS.2020.04.0492 Abstract Introduction: Elbow dislocations are sometimes associated with neurovascular injuries where brachial artery is the most frequently injured artery requiring emergency and adequate often complex surgical treatment in order to manage their severe complications. The literature consists of only a few limited case reports on associated vascular or neurovascular injuries resulting from this type of trauma with no reference to the particular techniques we combined to treat our patient. Presentation of Case: We present a Brachial Artery reconstruction in a 31-year-old patient with an Open Complex Right Elbow Dislocation. In the Clinical and Surgical Examination an open wound in the Anterior-Medial Right Antecubital Fossa presented with to-End Anastomosis was conducted using an Autologous Reverse Brachial Vein Conduit graft from the ipsilateral arm under General accompanying Brachial Pedicle all structures Transection was confirm. To repair the Brachial Artery a Substitution By-Pass and End- Anesthesia. For the Wound Closure a Rotational Skin and subcutaneous Fat Flap Graft. Postoperative patient progress, it was suc- cessful developing no Systemic Complications nor Ischemic Signs in the Right Upper Limb being discharge for Out-Patient follow-up through the By-pass and distal limb. -

Vascular / Endovascular Surgery Vascular / Endovascular Surgery Combat Manual Combat Manual
Vascular / Endovascular Surgery / Endovascular Vascular Vascular / Endovascular Surgery Combat Manual Combat Manual Combat W. L. Gore & Associates, Inc. Flagstaff, AZ 86004 +65.67332882 (Asia Pacific) 800.437.8181 (United States) 00800.6334.4673 (Europe) 928.779.2771 (United States) goremedical.com Stone Stone AbuRahma Campbell GORE®, EXCLUDER®, TAG®, VIABAHN®, and designs are trademarks of W. L. Gore & Associates. AbuRahma © 2012, 2013 W. L. Gore & Associates, Inc. AS0315-EN1 JULY 2013 Campbell Compliments of W. L. Gore & Associates, Inc. This publication, compliments of W. L. Gore & Associates, Inc. (Gore), is intended to serve as an educational resource for medical students, residents, and fellows pursuing training in vascular and endovascular surgery. Readers are reminded to consult appropriate references before engaging in any patient diagnosis, treatment, or surgery, including Prescribing Information (including boxed warnings and medication guides), Instructions for Use, and other applicable current information available from manufacturers. Gore products referenced within are used within their FDA approved / cleared indications. Gore does not have knowledge of the indications and FDA approval / clearance status of non-Gore products, and Gore does not advise or recommend any surgical methods or techniques other than those described in the Instructions for Use for its devices. Gore makes no representations or warranties as to the PERCLOSE®, PROSTAR®, SPARTACORE®, STARCLOSE®, and SUPRACORE® are trademarks of Abbott Laboratories. surgical techniques, medical conditions, or other factors that OMNI FLUSH and SIMMONS SIDEWINDER are trademarks of AngioDynamics. ICAST is a trademark of Atrium Medical Corporation. ASPIRIN® is a trademark of Bayer HealthCare, LLC. MORPH® is a trademark of BioCardia, may be described in this publication.