Anatomy and Physiology in Relation to Compression of the Upper Limb and Thorax
Total Page:16
File Type:pdf, Size:1020Kb
Load more
Recommended publications
-
Chapter 2 ROLE of LYMPHOSCINTIGRAPHY for SELECTIVE SENTINEL LYMPHADENECTOMY
Chapter 2 ROLE OF LYMPHOSCINTIGRAPHY FOR SELECTIVE SENTINEL LYMPHADENECTOMY Roger F. Uren, Robert B. Howman-Giles, David Chung, John F. Thompson* Nuclear Medicine and Diagnostic Ultrasound, RPAH Medical Centre and Discipline oj Medicine, The University of Sydney, Sydney, NSW, Australia and The Sydney Melanoma Unit, Royal Prince Alfred Hospital, Camperdown, NSW and Discipline of Surgery*, The University of Sydney, Sydney, NSW, Australia Abstract: An essential prerequisite for a successful sentinel node biopsy (SNB) procedure is an accurate map of the pattern of lymphatic drainage from the primary tumor site. The role of lymphoscintigraphy(LS) in SNB is to provide such a map in each patient. This map should indicate not only the location of all sentinel nodes but also the number of SNs at each location. Such mapping can be achieved using 99mTc-labeled small particle radiocolloids, high- resolution collimators with minimal septal penetration, and imaging protocols that detect all SNs in every patient regardless of their location. This is especially important in melanoma patients, since high-quality LS can identify the actual lymphatic collecting vessels as they drain into each SN. The SN is not always found in the nearest node field and is best defined as "any lymph node receiving direct lymphatic drainage from a primary tumor site." Reliable clinical prediction of lymphatic drainage from the skin or breast is not possible. Patterns of lymphatic drainage from the skin are highly variable from patient to patient, even from the same area of the skin. Unexpected lymphatic drainage has been found from the skin of the back to SNs in the triangular intermuscular space and in some patients through the posterior body wall to SNs in the para-aortic, paravertebral, and retroperitoneal areas. -

Health Tip: Swollen Lymph "Glands" - When Should You Be Concerned?
Printer Friendly Version Page 1 of 3 Health Tip: Swollen lymph "glands" - When should you be concerned? Lymph nodes, sometimes referred to as lymph "glands", are part of the body's lymphatic system. The lymphatic system consists of a system of conduits and organized collections of lymphoid tissue that include nodes, the tonsils, and the spleen. Coursing through these channels is liquid called lymph that eventually drains into the bloodstream near the heart, but along the way, it is "filtered" by the lymph nodes. Within these lymph nodes are high concentrations of disease fighting cells, particularly lymphocytes. While performing their intended function of fighting infection, lymph nodes typically become enlarged. In fact, infection is most common reason for lymph nodes enlargement. Lymph nodes are found throughout the body, but when enlarged, are usually noticed in characteristic locations, particularly the neck, groin and armpit regions. Lymph node enlargement can be localized to one group of lymph nodes or can be generalized (involving several sites of lymph nodes). For example, enlarged lymph nodes localized to the arm pit could occur as a result of a bacterial infection in a hand wound. Generalized lymph node swelling, on the other hand, could be seen in a systemic illness such as viral mononucleosis. In addition to viral and bacterial infections, other causes for enlarged lymph nodes include immune disorders (lupus, rheumatoid arthritis, etc.), cancers affecting the lymphatic system (leukemia, lymphoma, Hodgkin's disease), and cancers that have spread (metastasized) from some other part of the body to the lymphatic system. The discovery of enlarged lymph nodes often causes concern because many people are aware that lymph node enlargement can be an early sign of cancer. -

Prep for Practical II
Images for Practical II BSC 2086L "Endocrine" A A B C A. Hypothalamus B. Pineal Gland (Body) C. Pituitary Gland "Endocrine" 1.Thyroid 2.Adrenal Gland 3.Pancreas "The Pancreas" "The Adrenal Glands" "The Ovary" "The Testes" Erythrocyte Neutrophil Eosinophil Basophil Lymphocyte Monocyte Platelet Figure 29-3 Photomicrograph of a human blood smear stained with Wright’s stain (765). Eosinophil Lymphocyte Monocyte Platelets Neutrophils Erythrocytes "Blood Typing" "Heart Coronal" 1.Right Atrium 3 4 2.Superior Vena Cava 5 2 3.Aortic Arch 6 4.Pulmonary Trunk 1 5.Left Atrium 12 9 6.Bicuspid Valve 10 7.Interventricular Septum 11 8.Apex of The Heart 9. Chordae tendineae 10.Papillary Muscle 7 11.Tricuspid Valve 12. Fossa Ovalis "Heart Coronal Section" Coronal Section of the Heart to show valves 1. Bicuspid 2. Pulmonary Semilunar 3. Tricuspid 4. Aortic Semilunar 5. Left Ventricle 6. Right Ventricle "Heart Coronal" 1.Pulmonary trunk 2.Right Atrium 3.Tricuspid Valve 4.Pulmonary Semilunar Valve 5.Myocardium 6.Interventricular Septum 7.Trabeculae Carneae 8.Papillary Muscle 9.Chordae Tendineae 10.Bicuspid Valve "Heart Anterior" 1. Brachiocephalic Artery 2. Left Common Carotid Artery 3. Ligamentum Arteriosum 4. Left Coronary Artery 5. Circumflex Artery 6. Great Cardiac Vein 7. Myocardium 8. Apex of The Heart 9. Pericardium (Visceral) 10. Right Coronary Artery 11. Auricle of Right Atrium 12. Pulmonary Trunk 13. Superior Vena Cava 14. Aortic Arch 15. Brachiocephalic vein "Heart Posterolateral" 1. Left Brachiocephalic vein 2. Right Brachiocephalic vein 3. Brachiocephalic Artery 4. Left Common Carotid Artery 5. Left Subclavian Artery 6. Aortic Arch 7. -

Venous and Lymphatic Vessels. ANATOM.UA PART 1
Lection: Venous and lymphatic vessels. ANATOM.UA PART 1 https://fipat.library.dal.ca/ta2/ Ch. 1 Anatomia generalis PART 2 – SYSTEMATA MUSCULOSKELETALIA Ch. 2 Ossa Ch. 3 Juncturae Ch. 4 Musculi PART 3 – SYSTEMATA VISCERALIA Ch. 5 Systema digestorium Ch. 6 Systema respiratorium Ch. 7 Cavitas thoracis Ch. 8 Systema urinarium Ch. 9 Systemata genitalia Ch. 10 Cavitas abdominopelvica PART 4 – SYSTEMATA INTEGRANTIA I Ch. 11 Glandulae endocrinae Ch. 12 Systema cardiovasculare Ch. 13 Organa lymphoidea PART 5 – SYSTEMATA INTEGRANTIA II Ch. 14 Systema nervosum Ch. 15 Organa sensuum Ch. 16 Integumentum commune ANATOM.UA ANATOM.UA Cardiovascular system (systema cardiovasculare) consists of the heart and the tubes, that are used for transporting the liquid with special functions – the blood or lymph, that are necessary for supplying the cells with nutritional substances and the oxygen. ANATOM.UA 5 Veins Veins are blood vessels that bring blood back to theheart. All veins carry deoxygenatedblood with the exception of thepulmonary veins and umbilical veins There are two types of veins: Superficial veins: close to the surface of thebody NO corresponding arteries Deep veins: found deeper in the body With corresponding arteries Veins of the systemiccirculation: Superior and inferior vena cava with their tributaries Veins of the portal circulation: Portal vein ANATOM.UA Superior Vena Cava Formed by the union of the right and left Brachiocephalic veins. Brachiocephalic veins are formed by the union of internal jugular and subclavianveins. Drains venous blood from: Head &neck Thoracic wall Upper limbs It Passes downward and enter the rightatrium. Receives azygos vein on the posterior aspect just before it enters theheart. -

Axillary Lymph Nodes in Breast Cancer Patients: Sonographic Evaluation*
Pinheiro DJPCArtigo et al. / deLinfonodos Revisão axilares – avaliação ultrassonográfica Linfonodos axilares em pacientes com câncer de mama: avaliação ultrassonográfica* Axillary lymph nodes in breast cancer patients: sonographic evaluation Denise Joffily Pereira da Costa Pinheiro1, Simone Elias2, Afonso Celso Pinto Nazário3 Pinheiro DJPC, Elias S, Nazário ACP. Linfonodos axilares em pacientes com câncer de mama: avaliação ultrassonográfica. Radiol Bras. 2014 Jul/Ago; 47(4):240–244. Resumo O estadiamento axilar nas pacientes portadoras de câncer de mama inicial é fator essencial no planejamento terapêutico. Atualmente este é realizado durante o tratamento cirúrgico, mas há uma tendência em buscar técnicas pré-operatórias e de menor morbidade para avaliação dos linfonodos axilares. A ultrassonografia é um exame amplamente usado para esta finalidade e muitas vezes associado a punção aspirativa por agulha fina ou por agulha grossa. Entretanto, os critérios ultrassonográficos de suspeição para linfonodos axilares não apresentam valores preditivos significativos, gerando resultados discrepantes em estudos sobre sensibilidade e especificidade do método. O objetivo deste trabalho é realizar uma revisão na literatura médica sobre a ultrassonografia no estadiamento axilar e as principais alterações morfológicas do linfonodo metastático. Unitermos: Câncer de mama; Linfonodos axilares; Ultrassonografia; Aspectos morfológicos. Abstract Axillary staging of patients with early-stage breast cancer is essential in the treatment planning. Currently such staging is intraoperatively performed, but there is a tendency to seek a preoperative and less invasive technique to detect lymph node metastasis. Ultrasonography is widely utilized for this purpose, many times in association with fine-needle aspiration biopsy or core needle biopsy. However, the sonographic criteria for determining malignancy in axillary lymph nodes do not present significant predictive values, producing discrepant results in studies evaluating the sensitivity and specificity of this method. -

Impact of the Number of Dissected Axillary Lymph Nodes on Survival
ISSN: 2643-4563 Nabil et al. Int J Oncol Res 2019, 2:015 DOI: 10.23937/2643-4563/1710015 Volume 2 | Issue 1 International Journal of Open Access Oncology Research RESEARCH ARTICLE Impact of the Number of Dissected Axillary Lymph Nodes on Survival in Breast Cancer Patients Emad Eldin Nabil1, Ahmed M Maklad2,3, Ashraf Elyamany4,5*, Emad Gomaa6 and Moamen M Ali3,7 1Clinical Oncology and Nuclear Medicine Department, Sohag University Hospitals, Egypt 2Clinical Oncology and Nuclear Medicine Department, Sohag University Hospitals, Egypt 3King Fahad Medical City, Riyadh, KSA 4 Medical Oncology Department, SECI, Assiut University, Egypt Check for updates 5King Saud Medical City, Riyadh, KSA 6General Surgery Department, Sohag University Hospitals, Egypt 7Medical Physics, Radiation Oncology Department, SECI, Assiut University, Egypt *Corresponding author: Ashraf Elyamany, Medical Oncology Department, SECI, Assiut University, Egypt; King Saud Medical City, Riyadh, KSA Abstract regard median OS for patients having more than 10 LN excised was for N0, N1, N2, N3 5.57, 5.94, 4.97, 4.61 years Background: For patients with breast cancer, axillary dis- respectively while in the other group having less than 10 LN section was a standard treatment, especially with patient excised OS was 5.4, 5.14, 5.14 years respectively with P = with positive metastases in the sentinel nodes. For some 0.117. Regarding Lymphedema There was highly significant patients axillary dissection might be over-treatment, includ- difference between both arms p value 0.000, with higher ing those who have had a mastectomy. Especially with grades in arm I (moderate 17 cases and 6 cases severe the new trend of many radiation-therapy centers, provide edema). -

Managing Arm Lymphedema After Breast Cancer Video Transcript.Pdf
Transcript for Managing Lymphedema after Breast Cancer video Slide 1 ● Welcome to this presentation of “Lymphedema After Breast Cancer Surgery.” The goal of this presentation is to discuss lymphedema after breast cancer treatment, including risk factors and approaches to prevention and treatment. This presentation is part of the University of California San Francisco lymphedema prevention program. Slide 2 ● While most of us know that our cardiovascular system pumps blood through our body and provides oxygen and nutrients to cells and tissues, the lymphatic system is less well understood. But the lymphatic system serves very important functions. ● The lymphatic system removes excess fluid, microorganisms, and toxins from tissue spaces, and after the fluid has been filtered by the lymph nodes, returns this excess tissue fluid back into the circulatory system. In addition to this important role in fluid regulation, the lymphatic system also plays an important role in immune function, through the lymph nodes which filter foreign particles and cancer cells, and by producing immune cells - including antibodies. Another important function of the lymphatic system is absorption of fats from the gastrointestinal tract. Slide 3 ● Lymph originates from plasma, which is the liquid part of our blood. Our blood moves through our arteries (seen in red in the image on the left) and then into the capillary beds. Here, some of the plasma moves out of the blood capillaries into the surrounding tissues. This tissue fluid (called interstitial fluid) bathes the cells that make up the surrounding tissues, and carries nutrients, oxygen, and hormones to these cells. Cellular waste products and proteins leave the cells and also enter this interstitial fluid. -

Brachium and Cubital Fossa
Anatomy Guy Dissection Sheet 1/15/2012 Brachium and Cubital Fossa Dr. Craig Goodmurphy Anatomy Guy Major Dissection Objectives – Anterior Compartment 1. Maintain the superficial veins but work the fascia of the brachium off the anterior compartment noting the intermuscular septae 2. Clean and identify the three muscle of the anterior arm and their attachments 3. Mobilize the contents of the brachial fascia as it extends from the axillary fascia to the elbow noting the median, ulnar and medial brachial and medial antebrachial cutaneous nerves 4. Follow the musculocutaneous nerve as it passes through the coracobrachialis and between the biceps and brachialis noting motor branches and the lateral antebrachial cutaneous nerve Major Dissection Objectives – Cubital Fossa & Posterior Compartment 6. Mobilize the cubital fossa veins and review the boundaries 7. Clean the biceps tendon and reflect the aponeurosis 8. Locate the contents of the fossa including the bifurcation of the brachial artery, median nerve and floor muscles 9. Have a partner elevate the arm to dissect posteriorly and remove the skin and fascia 10. Locate the three heads of the triceps and their attachments 11. Locate the profunda brachii artery and radial nerve at the triangular interval and between the brachialis and brachioradialis muscles Eastern Virginia Medical School 1 Anatomy Guy Dissection Sheet 1/15/2012 Brachium and Cubital Fossa Pearls & Problems Don’t 1. Cut the biceps muscle just mobilize it Do 2. Follow the cords and tubes from known to unknown as you clean them Do 3. Remove the duplicated deep veins but save the unpaired superficial veins Do 4. -

Lymphatic Dysregulation in Patients with Heart Failure JACC Review Topic of the Week
JOURNAL OF THE AMERICAN COLLEGE OF CARDIOLOGY VOL. 78, NO. 1, 2021 ª 2021 BY THE AMERICAN COLLEGE OF CARDIOLOGY FOUNDATION PUBLISHED BY ELSEVIER THE PRESENT AND FUTURE JACC REVIEW TOPIC OF THE WEEK Lymphatic Dysregulation in Patients With Heart Failure JACC Review Topic of the Week a,b c d e Marat Fudim, MD, MHS, Husam M. Salah, MD, Janarthanan Sathananthan, MBCHB, MPH, Mathieu Bernier, MD, f g e,h i Waleska Pabon-Ramos, MD, MPH, Robert S. Schwartz, MD, Josep Rodés-Cabau, MD, PHD, François Côté, MD, j d a,b Abubaker Khalifa, MD, Sean A. Virani, MD, MSC, MPH, Manesh R. Patel, MD ABSTRACT The lymphatic system is an integral part of the circulatory system and plays an important role in the volume homeostasis of the human body. The complex anatomy and physiology paired with a lack of simple diagnostic tools to study the lymphatic system have led to an underappreciation of the contribution of the lymphatic system to acute and chronic heart failure (HF). Herein, we discuss the physiological role of the lymphatic system in volume management and the evidence demonstrating the dysregulation of the lymphatic system in HF. Further, we discuss the opportunity to target the lymphatic system in the management of HF and different potential approaches to accessing the lymphatic system. (J Am Coll Cardiol 2021;78:66–76) © 2021 by the American College of Cardiology Foundation. he circulatory system consists of the cardio- lead to interstitial edema with clinical manifestations T vascular system and the lymphatic system. such as extremity and tissue edema, including pulmo- The cardiovascular system is a closed, high- nary edema. -

Elbow Checklist
Workbook Musculoskeletal Ultrasound September 26, 2013 Shoulder Checklist Long biceps tendon Patient position: Facing the examiner Shoulder in slight medial rotation; elbow in flexion and supination Plane/ region: Transverse (axial): from a) intraarticular portion to b) myotendinous junction (at level of the pectoralis major tendon). What you will see: Long head of the biceps tendon Supraspinatus tendon Transverse humeral ligament Subscapularis tendon Lesser tuberosity Greater tuberosity Short head of the biceps Long head of the biceps (musculotendinous junction) Humeral shaft Pectoralis major tendon Plane/ region: Logitudinal (sagittal): What you will see: Long head of biceps; fibrillar structure Lesser tuberosity Long head of the biceps tendon Notes: Subscapularis muscle and tendon Patient position: Facing the examiner Shoulder in lateral rotation; elbow in flexion/ supination Plane/ region: longitudinal (axial): full vertical width of tendon. What you will see: Subscapularis muscle, tendon, and insertion Supraspinatus tendon Coracoid process Deltoid Greater tuberosity Lesser tuberosity Notes: Do passive medial/ lateral rotation while examining Plane/ region: Transverse (sagittal): What you will see: Lesser tuberosity Fascicles of subscapularis tendon Supraspinatus tendon Patient position: Lateral to examiner Shoulder in extension and medial rotation Hand on ipsilateral buttock Plane/ region: Longitudinal (oblique sagittal) Identify the intra-articular portion of biceps LH in the transverse plane; then -
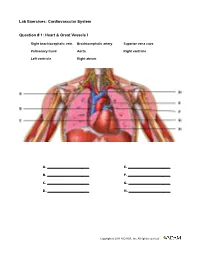
Lab Exercises: Cardiovascular System Question # 1: Heart & Great Vessels I
Lab Exercises: Cardiovascular System Question # 1: Heart & Great Vessels I Right brachiocephalic vein Brachiocephalic artery Superior vena cava Pulmonary trunk Aorta Right ventricle Left ventricle Right atrium A. E. B. F. C. G. D. H. Copyright © 2011 A.D.A.M., Inc. All rights reserved. Lab Exercises: Cardiovascular System Question # 2: Heart & Great Vessels II Left common carotid artery Brachiocephalic trunk Left subclavian artery Left brachiocephalic vein Left pulmonary artery Inferior vena cava Right pulmonary artery Right pulmonary vein A. E. B. F. C. G. D. H. Copyright © 2011 A.D.A.M., Inc. All rights reserved. Lab Exercises: Cardiovascular System Question # 3: Heart & Great Vessels (Post) Left pulmonary artery Left subclavian artery Right brachiocephalic vein Left common carotid artery Right pulmonary artery Right pulmonary vein Left pulmonary vein Inferior vena cava A. E. B. F. C. G. D. H. Copyright © 2011 A.D.A.M., Inc. All rights reserved. Lab Exercises: Cardiovascular System Question # 4: Arteries of Head & Neck Occipital artery Superficial temporal artery External carotid artery Internal carotid artery Facial artery Vertebral artery Common carotid artery A. E. B. F. C. G. D. Copyright © 2011 A.D.A.M., Inc. All rights reserved. Lab Exercises: Cardiovascular System Question # 5: Arteries of Trunk I Axillary artery Brachiocephailic trunk Right common carotid artery Left common carotid artery Left subclavian artery Axillary artery Arch of aorta Thoracic aorta A. E. B. F. C. G. D. H. Copyright © 2011 A.D.A.M., Inc. All rights reserved. Lab Exercises: Cardiovascular System Question # 6: Arteries of Trunk II Femoral artery Left common iliac artery Superior mesenteric artery Celiac trunk Inferior mesenteric artery Right renal artery Right testicular artery Left renal artery A. -

Cancer and Lymphatics: Part I
Cancer And Lymphatics: Part I Jassin M. Jouria, MD Dr. Jassin M. Jouria is a medical doctor, professor of academic medicine, and medical author. He graduated from Ross University School of Medicine and has completed his clinical clerkship training in various teaching hospitals throughout New York, including King’s County Hospital Center and Brookdale Medical Center, among others. Dr. Jouria has passed all USMLE medical board exams, and has served as a test prep tutor and instructor for Kaplan. He has developed several medical courses and curricula for a variety of educational institutions. Dr. Jouria has also served on multiple levels in the academic field including faculty member and Department Chair. Dr. Jouria continues to serves as a Subject Matter Expert for several continuing education organizations covering multiple basic medical sciences. He has also developed several continuing medical education courses covering various topics in clinical medicine. Recently, Dr. Jouria has been contracted by the University of Miami/Jackson Memorial Hospital’s Department of Surgery to develop an e-module training series for trauma patient management. Dr. Jouria is currently authoring an academic textbook on Human Anatomy & Physiology. ABSTRACT In the human body, cells receive nutrition and oxygen from lymph, a fluid that is recirculated through the body via an extensive network of vessels. Upon arriving at one of many nodes found within the body, the lymph is filtered to discern healthy cells from those carrying disease or infection. However, cancer can either develop in the lymph nodes around the body, or it can travel there via the lymphatic vessel network.