Proteomic Analyses of Kidney Glomerular Extracellular Matrix in Health and Disease
Total Page:16
File Type:pdf, Size:1020Kb
Load more
Recommended publications
-

New Concepts in Basement Membrane Biology Willi Halfter1, Philipp Oertle2, Christophe A
REVIEW ARTICLE New concepts in basement membrane biology Willi Halfter1, Philipp Oertle2, Christophe A. Monnier2,*, Leon Camenzind2, Magaly Reyes-Lua1, Huaiyu Hu3, Joseph Candiello4, Anatalia Labilloy5,†, Manimalha Balasubramani6, Paul Bernhard Henrich1 and Marija Plodinec2,7 1 Department of Ophthalmology, University Hospital Basel, Switzerland 2 Biozentrum and the Swiss Nanoscience Institute, University of Basel, Switzerland 3 Department of Neurobiology and Physiology, Upstate University Hospital, SUNY University, Syracuse, NY, USA 4 Department of Bioengeneering, University of Pittsburgh, PA, USA 5 Department of Renal Physiology, University of Pittsburgh, PA, USA 6 Proteomics Core Facility of the University of Pittsburgh, PA, USA 7 Department of Pathology, University Hospital Basel, Switzerland Keywords Basement membranes (BMs) are thin sheets of extracellular matrix that basal lamina; basement membrane; outline epithelia, muscle fibers, blood vessels and peripheral nerves. The biomechanical properties; collagen IV; current view of BM structure and functions is based mainly on transmis- laminin; membrane asymmetry; nidogen; sion electron microscopy imaging, in vitro protein binding assays, and phe- perlecan notype analysis of human patients, mutant mice and invertebrata. Correspondence Recently, MS-based protein analysis, biomechanical testing and cell adhe- W. Halfter, Department of Ophthalmology, sion assays with in vivo derived BMs have led to new and unexpected University Hospital Basel, Mittlere insights. Proteomic analysis combined with ultrastructural studies showed Strasse 91, 4031 Basel, Switzerland that many BMs undergo compositional and structural changes with Fax: +41 61 267 21 09 advancing age. Atomic force microscopy measurements in combination Tel: +49 7624 982528 with phenotype analysis have revealed an altered mechanical stiffness that E-mail: [email protected] M. -

Ophthalmological Features Associated with COL4A1 Mutations
OPHTHALMIC MOLECULAR GENETICS SECTION EDITOR: JANEY L. WIGGS, MD, PhD Ophthalmological Features Associated With COL4A1 Mutations Isabelle Coupry, PhD; Igor Sibon, MD, PhD; Bruno Mortemousque, MD; Franc¸ois Rouanet, MD; Manuele Mine, PharmD, PhD; Cyril Goizet, MD, PhD Objective: To investigate the wide variability of ocular Conclusions: The COL4A1 mutations may be associ- manifestations associated with mutations in the COL4A1 ated with various ophthalmologic developmental anoma- gene that encodes collagen IV␣1. lies of anterior segment dysgenesis type, which are reminiscent of Axenfeld-Rieger anomalies (ARA). Cere- Methods: We clinically evaluated 7 patients from 2 un- brovascular disorders should be added to the list of signs related families in whom ocular features segregated with potentially associated with ARA. COL4A1 mutations that were identified by direct se- quencing. Clinical Relevance: These data suggest that cerebral magnetic resonance imaging may be recommended in Results: The G2159A transition (c.2159GϾA) that leads the clinical treatment of patients with apparently iso- tothemissensemutationp.Gly720Aspwasidentifiedinfam- lated ARA, even when neurological symptoms or signs ily A. An ocular phenotype of variable severity was observed are lacking. in all affected relatives. The missense mutation c.2263GϾA, p.Gly755Arg was identified in family B. One patient from family B also displayed notable ocular features. Arch Ophthalmol. 2010;128(4):483-489 NEW FORM OF HEREDITARY constellation of ocular findings that in- cerebrovascular disorder clude anomalies of the anterior chamber was recently associated angle and aqueous drainage structures (iri- with mutations in the dogoniodysgenesis), iris hypoplasia, ec- COL4A1 gene that en- centric pupil (corectopia), iris tears (poly- Acodes collagen IV␣1.1,2 Mutations in coria), and iridocorneal adhesions COL4A1 were initially associated with ce- traversing the anterior chamber. -

The Mutational Landscape of Myeloid Leukaemia in Down Syndrome
cancers Review The Mutational Landscape of Myeloid Leukaemia in Down Syndrome Carini Picardi Morais de Castro 1, Maria Cadefau 1,2 and Sergi Cuartero 1,2,* 1 Josep Carreras Leukaemia Research Institute (IJC), Campus Can Ruti, 08916 Badalona, Spain; [email protected] (C.P.M.d.C); [email protected] (M.C.) 2 Germans Trias i Pujol Research Institute (IGTP), Campus Can Ruti, 08916 Badalona, Spain * Correspondence: [email protected] Simple Summary: Leukaemia occurs when specific mutations promote aberrant transcriptional and proliferation programs, which drive uncontrolled cell division and inhibit the cell’s capacity to differentiate. In this review, we summarize the most frequent genetic lesions found in myeloid leukaemia of Down syndrome, a rare paediatric leukaemia specific to individuals with trisomy 21. The evolution of this disease follows a well-defined sequence of events and represents a unique model to understand how the ordered acquisition of mutations drives malignancy. Abstract: Children with Down syndrome (DS) are particularly prone to haematopoietic disorders. Paediatric myeloid malignancies in DS occur at an unusually high frequency and generally follow a well-defined stepwise clinical evolution. First, the acquisition of mutations in the GATA1 transcription factor gives rise to a transient myeloproliferative disorder (TMD) in DS newborns. While this condition spontaneously resolves in most cases, some clones can acquire additional mutations, which trigger myeloid leukaemia of Down syndrome (ML-DS). These secondary mutations are predominantly found in chromatin and epigenetic regulators—such as cohesin, CTCF or EZH2—and Citation: de Castro, C.P.M.; Cadefau, in signalling mediators of the JAK/STAT and RAS pathways. -

Upon Microbial Challenge, Human Neutrophils Undergo Rapid Changes in Nuclear Architecture and Chromatin Folding to Orchestrate an Immediate Inflammatory Gene Program
Downloaded from genesdev.cshlp.org on October 5, 2021 - Published by Cold Spring Harbor Laboratory Press Upon microbial challenge, human neutrophils undergo rapid changes in nuclear architecture and chromatin folding to orchestrate an immediate inflammatory gene program Matthew Denholtz,1,5 Yina Zhu,1,5 Zhaoren He,1 Hanbin Lu,1 Takeshi Isoda,1,4 Simon Döhrmann,2 Victor Nizet,2,3 and Cornelis Murre1 1Division of Biological Sciences, Department of Molecular Biology, University of California at San Diego, La Jolla, California 92039, USA; 2Department of Pediatrics, University of California at San Diego School of Medicine, La Jolla, California 92093, USA; 3Skaggs School of Pharmaceutical Sciences, University of California at San Diego, La Jolla, California 92093, USA Differentiating neutrophils undergo large-scale changes in nuclear morphology. How such alterations in structure are established and modulated upon exposure to microbial agents is largely unknown. Here, we found that prior to encounter with bacteria, an armamentarium of inflammatory genes was positioned in a transcriptionally passive environment suppressing premature transcriptional activation. Upon microbial exposure, however, human neu- trophils rapidly (<3 h) repositioned the ensemble of proinflammatory genes toward the transcriptionally permissive compartment. We show that the repositioning of genes was closely associated with the swift recruitment of cohesin across the inflammatory enhancer landscape, permitting an immediate transcriptional response upon bacterial exposure. We found that activated enhancers, marked by increased deposition of H3K27Ac, were highly enriched for cistromic elements associated with PU.1, CEBPB, TFE3, JUN, and FOSL2 occupancy. These data reveal how upon microbial challenge the cohesin machinery is recruited to an activated enhancer repertoire to instruct changes in chromatin folding, nuclear architecture, and to activate an inflammatory gene program. -

Structure of the Human Cohesin Inhibitor Wapl
Structure of the human cohesin inhibitor Wapl Zhuqing Ouyanga,1, Ge Zhenga,1, Jianhua Songb, Dominika M. Borekc, Zbyszek Otwinowskic, Chad A. Brautigamc, Diana R. Tomchickc, Susannah Rankinb, and Hongtao Yua,2 aHoward Hughes Medical Institute, Department of Pharmacology, and cDepartment of Biophysics, University of Texas Southwestern Medical Center, Dallas, TX 75390; and bProgram in Cell Cycle and Cancer Biology, Oklahoma Medical Research Foundation, Oklahoma City, OK 73104 Edited by Douglas Koshland, University of California, Berkeley, CA, and approved May 23, 2013 (received for review March 11, 2013) Cohesin, along with positive regulators, establishes sister-chromatid trigger cohesin release from chromosome arms (15, 18–21). A pool of cohesion by forming a ring to circle chromatin. The wings apart-like cohesin at centromeres is protected by the shugoshin (Sgo1)–protein protein (Wapl) is a key negative regulator of cohesin and forms phosphatase 2A (PP2A) complex (22, 23), which binds to cohesin, a complex with precocious dissociation of sisters protein 5 (Pds5) to dephosphorylates sororin, and protects cohesin from Wapl promote cohesin release from chromatin. Here we report the at centromeres (24). After all sister kinetochores attach properly crystal structure and functional characterization of human Wapl. to the mitotic spindle and are under tension, separase cleaves Wapl contains a flexible, variable N-terminal region (Wapl-N) and centromeric cohesin to initiate sister-chromatid separation. The a conserved C-terminal domain (Wapl-C) consisting of eight HEAT separated chromatids are evenly partitioned into the two daughter (Huntingtin, Elongation factor 3, A subunit, and target of rapamycin) cells through their attachment to microtubules originating from the repeats. -

A Collagen Glucosyltransferase Drives Lung Adenocarcinoma Progression in Mice
ARTICLE https://doi.org/10.1038/s42003-021-01982-w OPEN A collagen glucosyltransferase drives lung adenocarcinoma progression in mice Hou-Fu Guo 1, Neus Bota-Rabassedas 1, Masahiko Terajima 2, B. Leticia Rodriguez1, Don L. Gibbons 1, Yulong Chen1, Priyam Banerjee1, Chi-Lin Tsai 3, Xiaochao Tan1, Xin Liu1, Jiang Yu1, Michal Tokmina-Roszyk4, Roma Stawikowska4, Gregg B. Fields4, Mitchell D. Miller 5, Xiaoyan Wang3, Juhoon Lee6,7, Kevin N. Dalby6,7, Chad J. Creighton 8,9, George N. Phillips Jr 5,10, John A. Tainer 3, Mitsuo Yamauchi2 & ✉ Jonathan M. Kurie 1 Cancer cells are a major source of enzymes that modify collagen to create a stiff, fibrotic tumor stroma. High collagen lysyl hydroxylase 2 (LH2) expression promotes metastasis and 1234567890():,; is correlated with shorter survival in lung adenocarcinoma (LUAD) and other tumor types. LH2 hydroxylates lysine (Lys) residues on fibrillar collagen’s amino- and carboxy-terminal telopeptides to create stable collagen cross-links. Here, we show that electrostatic interac- tions between the LH domain active site and collagen determine the unique telopeptidyl lysyl hydroxylase (tLH) activity of LH2. However, CRISPR/Cas-9-mediated inactivation of tLH activity does not fully recapitulate the inhibitory effect of LH2 knock out on LUAD growth and metastasis in mice, suggesting that LH2 drives LUAD progression, in part, through a tLH- independent mechanism. Protein homology modeling and biochemical studies identify an LH2 isoform (LH2b) that has previously undetected collagen galactosylhydroxylysyl glucosyl- transferase (GGT) activity determined by a loop that enhances UDP-glucose-binding in the GLT active site and is encoded by alternatively spliced exon 13 A. -

Ultrasound-Assisted Nonviral Gene Transfer of AQP1 to the Irradiated Minipig Parotid Gland Restores fluid Secretion
Gene Therapy (2015) 22, 739–749 © 2015 Macmillan Publishers Limited All rights reserved 0969-7128/15 www.nature.com/gt ORIGINAL ARTICLE Ultrasound-assisted nonviral gene transfer of AQP1 to the irradiated minipig parotid gland restores fluid secretion Z Wang1, L Zourelias1,CWu1, PC Edwards2, M Trombetta3 and MJ Passineau1 Xerostomia is a common side effect of ionizing radiation used to treat head and neck cancer. A groundbreaking Phase I human clinical trial using Adenoviral gene transfer of Aquaporin-1 (AQP1) to a single salivary gland of individuals suffering from radiation- induced xerostomia has recently been reported. Unfortunately, the limitations of the Adenoviral vector system used in this pioneering trial preclude its advancement to a Phase II trial, and we have thus undertaken to evaluate the therapeutic potential of ultrasound-assisted nonviral gene transfer (UAGT) as an alternative means of delivering AQP1 gene therapy to the salivary gland by comparing head-to-head with the canonical Adenoviral vector in a swine model. Swine irradiated unilaterally with a 10-Gy electron beam targeted at the parotid gland suffered from significant, sustained hyposalivation that was bilateral, despite irradiation being confined to the targeted gland. Unilateral AQP1 gene therapy with UAGT resulted in bilateral restoration of stimulated salivary flow at 48 h and 1 week post treatment (1.62 ± 0.48 ml and 1.87 ± 0.45 ml) to preinjury levels (1.34 ± 0.14 ml) in a manner comparable to Adenoviral delivery (2.32 ± 0.6 ml and 1.33 ± 0.97 ml). UAGT can replace the Adenoviral vector as a means of delivering AQP1 gene therapy in the irradiated swine model, and it is a candidate for advancement to a Phase I human clinical trial. -

Role of Phytochemicals in Colon Cancer Prevention: a Nutrigenomics Approach
Role of phytochemicals in colon cancer prevention: a nutrigenomics approach Marjan J van Erk Promotor: Prof. Dr. P.J. van Bladeren Hoogleraar in de Toxicokinetiek en Biotransformatie Wageningen Universiteit Co-promotoren: Dr. Ir. J.M.M.J.G. Aarts Universitair Docent, Sectie Toxicologie Wageningen Universiteit Dr. Ir. B. van Ommen Senior Research Fellow Nutritional Systems Biology TNO Voeding, Zeist Promotiecommissie: Prof. Dr. P. Dolara University of Florence, Italy Prof. Dr. J.A.M. Leunissen Wageningen Universiteit Prof. Dr. J.C. Mathers University of Newcastle, United Kingdom Prof. Dr. M. Müller Wageningen Universiteit Dit onderzoek is uitgevoerd binnen de onderzoekschool VLAG Role of phytochemicals in colon cancer prevention: a nutrigenomics approach Marjan Jolanda van Erk Proefschrift ter verkrijging van graad van doctor op gezag van de rector magnificus van Wageningen Universiteit, Prof.Dr.Ir. L. Speelman, in het openbaar te verdedigen op vrijdag 1 oktober 2004 des namiddags te vier uur in de Aula Title Role of phytochemicals in colon cancer prevention: a nutrigenomics approach Author Marjan Jolanda van Erk Thesis Wageningen University, Wageningen, the Netherlands (2004) with abstract, with references, with summary in Dutch ISBN 90-8504-085-X ABSTRACT Role of phytochemicals in colon cancer prevention: a nutrigenomics approach Specific food compounds, especially from fruits and vegetables, may protect against development of colon cancer. In this thesis effects and mechanisms of various phytochemicals in relation to colon cancer prevention were studied through application of large-scale gene expression profiling. Expression measurement of thousands of genes can yield a more complete and in-depth insight into the mode of action of the compounds. -

A Requirement for STAG2 in Replication Fork Progression Creates a Targetable Synthetic Lethality in Cohesin-Mutant Cancers
ARTICLE https://doi.org/10.1038/s41467-019-09659-z OPEN A requirement for STAG2 in replication fork progression creates a targetable synthetic lethality in cohesin-mutant cancers Gourish Mondal1, Meredith Stevers1, Benjamin Goode 1, Alan Ashworth2,3 & David A. Solomon 1,2 Cohesin is a multiprotein ring that is responsible for cohesion of sister chromatids and formation of DNA loops to regulate gene expression. Genomic analyses have identified that 1234567890():,; the cohesin subunit STAG2 is frequently inactivated by mutations in cancer. However, the reason STAG2 mutations are selected during tumorigenesis and strategies for therapeutically targeting mutant cancer cells are largely unknown. Here we show that STAG2 is essential for DNA replication fork progression, whereby STAG2 inactivation in non-transformed cells leads to replication fork stalling and collapse with disruption of interaction between the cohesin ring and the replication machinery as well as failure to establish SMC3 acetylation. As a con- sequence, STAG2 mutation confers synthetic lethality with DNA double-strand break repair genes and increased sensitivity to select cytotoxic chemotherapeutic agents and PARP or ATR inhibitors. These studies identify a critical role for STAG2 in replication fork procession and elucidate a potential therapeutic strategy for cohesin-mutant cancers. 1 Department of Pathology, University of California, San Francisco, CA 94143, USA. 2 UCSF Helen Diller Family Comprehensive Cancer Center, San Francisco, CA 94158, USA. 3 Division of Hematology and Oncology, Department of Medicine, University of California, San Francisco, CA 94158, USA. Correspondence and requests for materials should be addressed to D.A.S. (email: [email protected]) NATURE COMMUNICATIONS | (2019) 10:1686 | https://doi.org/10.1038/s41467-019-09659-z | www.nature.com/naturecommunications 1 ARTICLE NATURE COMMUNICATIONS | https://doi.org/10.1038/s41467-019-09659-z ohesin is a multi-protein complex composed of four core transcriptional dysregulation22,23. -

Human Genome Center Laboratory of Genome Database Laboratory of Sequence Analysis ゲノムデータベース分野 シークエンスデータ情報処理分野
136 Human Genome Center Laboratory of Genome Database Laboratory of Sequence Analysis ゲノムデータベース分野 シークエンスデータ情報処理分野 Professor Minoru Kanehisa, Ph.D. 教授(委嘱) 理学博士 金 久 實 Research Associate Toshiaki Katayama, M.Sc. 助 手 理学修士 片山俊明 Research Associate Shuichi Kawashima, M.Sc. 助 手 理学修士 川島秀一 Lecturer Tetsuo Shibuya, Ph.D. 講 師 理学博士 渋谷哲朗 Research Associate Michihiro Araki, Ph.D. 助 手 薬学博士 荒木通啓 Owing to continuous developments of high-throughput experimental technologies, ever-increasing amounts of data are being generated in functional genomics and proteomics. We are developing a new generation of databases and computational technologies, beyond the traditional genome databases and sequence analysis tools, for making full use of such large-scale data in biomedical applications, espe- cially for elucidating cellular functions as behaviors of complex interaction systems. 1. Comprehensive repository for community We have been developing the server based on genome annotation open source software including BioRuby, BioPerl, BioDAS and GMOD/GBrowse to make Toshiaki Katayama, Mari Watanabe and Mi- the system consistent with the existing open noru Kanehisa standards. The contents of the KEGG DAS data- base can be accessed graphically in a web KEGG DAS is an advanced genome database browser using GBrowse GUI (graphical user in- system providing DAS (Distributed Annotation terface) and also programatically by the DAS System) service for all organisms in the protocol. The DAS, which is an XML over HTTP GENOME and GENES databases in KEGG data retrieving protocol, enables the user to (Kyoto Encyclopedia of Genes and Genomes). write various kinds of automated programs for Currently, KEGG DAS contains 6,943,951 anno- analyzing genome sequences and annotations. -

Collagen Type XVIII (H-140): Sc-25720
SANTA CRUZ BIOTECHNOLOGY, INC. Collagen Type XVIII (H-140): sc-25720 The Power to Question BACKGROUND APPLICATIONS Type XV and XVIII collagens form the new subgroup MULTIPLEXIN, within the Collagen Type XVIII (H-140) is recommended for detection of Collagen α1 diverse family of collagens, which contains nineteen distinct types of collagens Type XVIII of mouse, rat and human origin by Western Blotting (starting found in vertebrates. Both type XV and XVIII collagens are characterized by dilution 1:200, dilution range 1:100-1:1000), immunoprecipitation [1–2 µg extensive interruptions in their collagenous sequences. Members of the MUL- per 100–500 µg of total protein (1 ml of cell lysate)] and immunofluores- TIPLEXIN subgroup contain polypeptides with multiple triple-helical domains cence (starting dilution 1:50, dilution range 1:50-1:500). separated and flanked by non-triple-helical regions. Type XV is predominantly Suitable for use as control antibody for Collagen Type XVIII siRNA (h): expressed in internal organs such as adrenal gland, kidney and pancreas. Type sc-43072 and Collagen Type XVIII siRNA (m): sc-43073. XVIII encodes two different α1 chains, which have different signal peptides and variant N-terminal non-collagenous NC1 domains of 495 and 303 amino Molecular Weight of Collagen Type XVIII: 20-22 kDa. acids. The long variant NC1-434 Type XVIII mRNAs are prominently expressed Positive Controls: rat C6 glioblastoma, human PBL or rat lung extract: sc-2396. in liver, while the variant NC1-303 mRNAs are predominantly expressed in heart, kidney, placenta, prostate, ovaries, skeletal muscle and small intestine. RECOMMENDED SECONDARY REAGENTS Endostatin is a fragment of the C-terminal domain NC1 of collagen XV and XVIII that inhibits angiogenesis and tumor growth. -
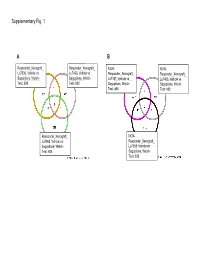
Supplementary Data
Supplementary Fig. 1 A B Responder_Xenograft_ Responder_Xenograft_ NON- NON- Lu7336, Vehicle vs Lu7466, Vehicle vs Responder_Xenograft_ Responder_Xenograft_ Sagopilone, Welch- Sagopilone, Welch- Lu7187, Vehicle vs Lu7406, Vehicle vs Test: 638 Test: 600 Sagopilone, Welch- Sagopilone, Welch- Test: 468 Test: 482 Responder_Xenograft_ NON- Lu7860, Vehicle vs Responder_Xenograft_ Sagopilone, Welch - Lu7558, Vehicle vs Test: 605 Sagopilone, Welch- Test: 333 Supplementary Fig. 2 Supplementary Fig. 3 Supplementary Figure S1. Venn diagrams comparing probe sets regulated by Sagopilone treatment (10mg/kg for 24h) between individual models (Welsh Test ellipse p-value<0.001 or 5-fold change). A Sagopilone responder models, B Sagopilone non-responder models. Supplementary Figure S2. Pathway analysis of genes regulated by Sagopilone treatment in responder xenograft models 24h after Sagopilone treatment by GeneGo Metacore; the most significant pathway map representing cell cycle/spindle assembly and chromosome separation is shown, genes upregulated by Sagopilone treatment are marked with red thermometers. Supplementary Figure S3. GeneGo Metacore pathway analysis of genes differentially expressed between Sagopilone Responder and Non-Responder models displaying –log(p-Values) of most significant pathway maps. Supplementary Tables Supplementary Table 1. Response and activity in 22 non-small-cell lung cancer (NSCLC) xenograft models after treatment with Sagopilone and other cytotoxic agents commonly used in the management of NSCLC Tumor Model Response type