Neutrophil Disorders and Their Management J Clin Pathol: First Published As 10.1136/Jcp.54.1.7 on 1 January 2001
Total Page:16
File Type:pdf, Size:1020Kb

Load more
Recommended publications
-

My Beloved Neutrophil Dr Boxer 2014 Neutropenia Family Conference
The Beloved Neutrophil: Its Function in Health and Disease Stem Cell Multipotent Progenitor Myeloid Lymphoid CMP IL-3, SCF, GM-CSF CLP Committed Progenitor MEP GMP GM-CSF, IL-3, SCF EPO TPO G-CSF M-CSF IL-5 IL-3 SCF RBC Platelet Neutrophil Monocyte/ Basophil B-cells Macrophage Eosinophil T-Cells Mast cell NK cells Mature Cell Dendritic cells PRODUCTION AND KINETICS OF NEUTROPHILS CELLS % CELLS TIME Bone Marrow: Myeloblast 1 7 - 9 Mitotic Promyelocyte 4 Days Myelocyte 16 Maturation/ Metamyelocyte 22 3 – 7 Storage Band 30 Days Seg 21 Vascular: Peripheral Blood Seg 2 6 – 12 hours 3 Marginating Pool Apoptosis and ? Tissue clearance by 0 – 3 macrophages days PHAGOCYTOSIS 1. Mobilization 2. Chemotaxis 3. Recognition (Opsonization) 4. Ingestion 5. Degranulation 6. Peroxidation 7. Killing and Digestion 8. Net formation Adhesion: β 2 Integrins ▪ Heterodimer of a and b chain ▪ Tight adhesion, migration, ingestion, co- stimulation of other PMN responses LFA-1 Mac-1 (CR3) p150,95 a2b2 a CD11a CD11b CD11c CD11d b CD18 CD18 CD18 CD18 Cells All PMN, Dendritic Mac, mono, leukocytes mono/mac, PMN, T cell LGL Ligands ICAMs ICAM-1 C3bi, ICAM-3, C3bi other other Fibrinogen other GRANULOCYTE CHEMOATTRACTANTS Chemoattractants Source Activators Lipids PAF Neutrophils C5a, LPS, FMLP Endothelium LTB4 Neutrophils FMLP, C5a, LPS Chemokines (a) IL-8 Monocytes, endothelium LPS, IL-1, TNF, IL-3 other cells Gro a, b, g Monocytes, endothelium IL-1, TNF other cells NAP-2 Activated platelets Platelet activation Others FMLP Bacteria C5a Activation of complement Other Important Receptors on PMNs ñ Pattern recognition receptors – Detect microbes - Toll receptor family - Mannose receptor - bGlucan receptor – fungal cell walls ñ Cytokine receptors – enhance PMN function - G-CSF, GM-CSF - TNF Receptor ñ Opsonin receptors – trigger phagocytosis - FcgRI, II, III - Complement receptors – ñ Mac1/CR3 (CD11b/CD18) – C3bi ñ CR-1 – C3b, C4b, C3bi, C1q, Mannose binding protein From JG Hirsch, J Exp Med 116:827, 1962, with permission. -
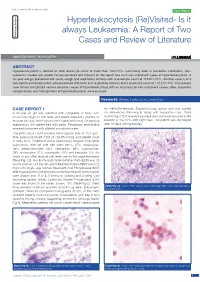
Hyperleukocytosis (Re)Visited- Is It Case Series Always Leukaemia: a Report of Two Pathology Section Cases and Review of Literature Short Communication
Review Article Clinician’s corner Original Article Images in Medicine Experimental Research Miscellaneous Letter to Editor DOI: 10.7860/JCDR/2020/40556.13409 Case Report Postgraduate Education Hyperleukocytosis (Re)Visited- Is it Case Series always Leukaemia: A Report of Two Pathology Section Cases and Review of Literature Short Communication ASHUTOSH RATH1, RICHA GUPTA2 ABSTRACT Hyperleukocytosis is defined as total leukocyte count of more than 100×109/L. Commonly seen in leukaemic conditions, non- leukaemic causes are usually not encountered and thought of. We report two such non-malignant cases of hyperleukocytosis. A six-year old girl presented with fever, cough and respiratory distress with a leukocyte count of 125.97×109/L. Another case is of a two-month old female infant, who presented with fever and respiratory distress and a leukocyte count of 112.27×109/L. The present case thrives to highlight various possible causes of hyperleukocytosis with an emphasis on non-malignant causes. Also, important complications and management of hyperleukocytosis are discussed. Keywords: Benign, Leukocytosis, Leukostasis CASE REPORT 1 for methicillin-resistant Staphylococcus aureus and was started A six-year-old girl was admitted with complaints of fever, non- on intravenous Vancomycin along with supportive care. Serial productive cough for one week and severe respiratory distress for monitoring of TLC revealed a gradual reduction and it returned to the the past one day. There was no other significant history. On physical baseline of 15×109/L after eight days. The patient was discharged examination, the patient had mild pallor. Respiratory examination after 10 days of hospital stay. -

Digitalcommons@UNMC Granulocytopenia
University of Nebraska Medical Center DigitalCommons@UNMC MD Theses Special Collections 5-1-1936 Granulocytopenia Howard E. Mitchell University of Nebraska Medical Center This manuscript is historical in nature and may not reflect current medical research and practice. Search PubMed for current research. Follow this and additional works at: https://digitalcommons.unmc.edu/mdtheses Part of the Medical Education Commons Recommended Citation Mitchell, Howard E., "Granulocytopenia" (1936). MD Theses. 457. https://digitalcommons.unmc.edu/mdtheses/457 This Thesis is brought to you for free and open access by the Special Collections at DigitalCommons@UNMC. It has been accepted for inclusion in MD Theses by an authorized administrator of DigitalCommons@UNMC. For more information, please contact [email protected]. G PA~lULOCYTOPENI A SENIOR THESIS By Howard E. Mitchell April 17, 1936 TABLE OF CONT'ENTS Introduction Definition • · 1 History . • • • 1 Nomenclature • • • • • 4 ClassificBtion • • • • 6 Physiology • • • • .10 Etiology • • 22 Geographic Distribution • 23 Age, Sex, and R9ce • • ·• 23 Occupation • .. • • • • .. • 23 Ba.cteria • • • • .. 24 Glandu18.r Dysfunction • • • 27 Radiation • • • • 28 Allergy • • • 28 Chemotactic and Maturation Factors • • 28 Chemicals • • • • • 30 Pathology • • • • • 36 Symptoms • • • • • • • 43 DiEtgnosis • • • • • .. • • • • • .. • 4'7 Prognosis 48 '" • • • • • • • • • • • • Treatment • • • • • • • • 49 Non"'specific Therapy • • • • .. 50 Transfusion • • • • .. 51 X-Ray • • • • • • • • • 52 Liver ·Extract • • • • • • • 53 Nucleotides • • • • • • • • • • • 53 General Ca.re • • • • • • • • 57 Conclusion • • • • • • • • • 58 480805 INTHODUCTION Although t~ere is reference in literature of the Nineteenth Century to syndromes similating the disease (granulocytopenia) 9.8 W(~ know it todes, it "vas not un til the year 1922 that Schultz 8ctually described his C8se as a disease entity and by so doing, stimulated the interest of tne medical profession to further in vestigation. -

Chediak Higashi Syndrome Masquerading As Acute Leukemia / Storage Disorder - a Rare Case Report
International Journal of Research in Medical Sciences Asif Baig M et al. Int J Res Med Sci. 2015 Jul;3(7):1785-1787 www.msjonline.org pISSN 2320-6071 | eISSN 2320-6012 DOI: http://dx.doi.org/10.18203/2320-6012.ijrms20150271 Case Report Chediak Higashi Syndrome masquerading as acute leukemia / storage disorder - A rare case report Mirza Asif Baig1,*, Anil Sirasgi2 1Former Asst. professor, BLDUs Shri B.M. Patil Medical College, Bijapure, Karnataka, India 2Associate professor, ESI Medical College, Gulbarga, Karnataka, India Received: 19 April 2015 Revised: 09 May 2015 Accepted: 23 May 2015 *Correspondence: Dr. Mirza Asif Baig, E-mail: [email protected] Copyright: © the author(s), publisher and licensee Medip Academy. This is an open-access article distributed under the terms of the Creative Commons Attribution Non-Commercial License, which permits unrestricted non-commercial use, distribution, and reproduction in any medium, provided the original work is properly cited. ABSTRACT Chediak higashi Syndrome (CHS) is a rare autosomal recessive multisystem disorder with a defect in granule morphogenesis with giant lysosomes in leucocyte and other cells. CHS is a rare disease, approximately 200 cases have been reported so far. It was described in detail by Chediak in 1952 and Higashi in 1954. 1½ year old male child presented with multiple hypopigment patches on lower extremities, light colored hair, Hepatosplenomegaly and generalised Lymphadenopathy. PBS shows giant prominent liliac to purple granules in neutrophils, band forms, few lymphocytes and monocytes. Bone marrow is hypercellular showing giant prominent gray blue to purple heterogeneous granules often multiple seen in many myeloid precursors, Neutrophils, few lymphocytes and monocytes. -

Clozapine, Agranulocytosis, and Benign Ethnic Neutropenia
EDITORIAL 545 Postgrad Med J: first published as 10.1136/pgmj.2004.031641 on 2 September 2005. Downloaded from Pharmacology and toxicology ethnic groups in the Middle East, ....................................................................................... including Yemenite Jews and Jordanians, have BEN.12 13 BEN has only been reported in ethnic groups that have Clozapine, agranulocytosis, and tanned or dark skin.13 Subjects with BEN do not show increased incidence of benign ethnic neutropenia infections, and their response to infec- tions is similar to those without BEN.13 S Rajagopal ................................................................................... CLINICAL IMPLICATIONS In the United Kingdom and Ireland, the Current knowledge and clinical implications Clozaril patient monitoring service (CPMS) supervises the prescribing of clozapine and the haematological test- lozapine is an atypical antipsycho- agranulocytosis, is more common in ing (Clozaril is the brand name of tic that is effective in treatment black people.6 A white cell count spike clozapine). The CPMS uses a lower cut resistant schizophrenia.1 The of 15% or more above the immediately C off point for patients with BEN than for National Institute for Health and preceding measurement may predict the general population (table 1). A Clinical Excellence (NICE) guidelines agranulocytosis within the next ‘‘green’’ alert indicates satisfactory for schizophrenia specify that ‘‘in indi- 75 days.7 However, as these differences count, an ‘‘amber’’ alert requires a viduals with evidence of treatment between the risk factors for agranulocy- repeat FBC test while clozapine can be resistant schizophrenia, clozapine tosis and neutropenia have been extra- should be introduced at the earliest polated primarily from epidemiological continued, and a ‘‘red’’ alert warrants opportunity’’.2 studies, they may be subject to change immediate cessation of clozapine. -

Severe Agranulocytosis in Two Patients with Drug-Induced Hypersensitivity Syndrome/Drug Reaction with Eosinophilia and Systemic Symptoms
Acta Derm Venereol 2016; 96: 842–843 SHORT COMMUNICATION Severe Agranulocytosis in Two Patients with Drug-induced Hypersensitivity Syndrome/Drug Reaction with Eosinophilia and Systemic Symptoms Miyuki Kato, Yoko Kano*, Yohei Sato and Tetsuo Shiohara Department of Dermatology, Kyorin University School of Medicine, 6-20-2 Shinkawa Mitaka, Tokyo 181-8611, Japan. *E-mail: [email protected] Accepted Mar 24, 2016; Epub ahead of print Mar 30, 2016 Drug-induced hypersensitivity syndrome/drug reac- No evidence was seen of lymphoma or other haematological tion with eosinophilia and systemic symptoms (DIHS/ malignancies. Granulocyte-colony stimulating factor (G-CSF) DRESS) is a life-threatening adverse reaction characteri- and intravenous immunoglobulin at 5 g/day were administered for 5 days. As high-grade fever continued, antibiotics were zed by skin rashes, fever, leukocytosis with eosinophilia started. During the appearance of agranulocytosis, atypical and/or atypical lymphocytosis, lymph node enlargement, lymphocytosis (2–11%) was detected. On day 24 after onset, and liver and/or renal dysfunctions (1, 2). A wide variety leucocyte count was normalized, but liver dysfunction ap- of other involvements have also been reported, including peared (aspartate aminotransferase (AST) 276 IU/l (normal limbic encephalitis, myocarditis, and gastrointestinal < 33 IU/l); alanine aminotransferase (ALT) 159 IU/l (normal < 30 IU/l)). Renal function was also exacerbated (BUN 86.6 disease, developing during the course of the disease mg/dl; Cr 2.8 mg/dl). Seven days later, leucocytes overshot (3–5). It has been demonstrated that human herpesvirus to 21.3 × 109/l (neutrophil 81.0%; eosinophil 0.5%; monocyte 6 (HHV-6), Epstein-Barr virus (EBV) and cytomegalo- 8%; lymphocyte 10%; atypical lymphocyte 0.5%). -

Practice Parameter for the Diagnosis and Management of Primary Immunodeficiency
Practice parameter Practice parameter for the diagnosis and management of primary immunodeficiency Francisco A. Bonilla, MD, PhD, David A. Khan, MD, Zuhair K. Ballas, MD, Javier Chinen, MD, PhD, Michael M. Frank, MD, Joyce T. Hsu, MD, Michael Keller, MD, Lisa J. Kobrynski, MD, Hirsh D. Komarow, MD, Bruce Mazer, MD, Robert P. Nelson, Jr, MD, Jordan S. Orange, MD, PhD, John M. Routes, MD, William T. Shearer, MD, PhD, Ricardo U. Sorensen, MD, James W. Verbsky, MD, PhD, David I. Bernstein, MD, Joann Blessing-Moore, MD, David Lang, MD, Richard A. Nicklas, MD, John Oppenheimer, MD, Jay M. Portnoy, MD, Christopher R. Randolph, MD, Diane Schuller, MD, Sheldon L. Spector, MD, Stephen Tilles, MD, Dana Wallace, MD Chief Editor: Francisco A. Bonilla, MD, PhD Co-Editor: David A. Khan, MD Members of the Joint Task Force on Practice Parameters: David I. Bernstein, MD, Joann Blessing-Moore, MD, David Khan, MD, David Lang, MD, Richard A. Nicklas, MD, John Oppenheimer, MD, Jay M. Portnoy, MD, Christopher R. Randolph, MD, Diane Schuller, MD, Sheldon L. Spector, MD, Stephen Tilles, MD, Dana Wallace, MD Primary Immunodeficiency Workgroup: Chairman: Francisco A. Bonilla, MD, PhD Members: Zuhair K. Ballas, MD, Javier Chinen, MD, PhD, Michael M. Frank, MD, Joyce T. Hsu, MD, Michael Keller, MD, Lisa J. Kobrynski, MD, Hirsh D. Komarow, MD, Bruce Mazer, MD, Robert P. Nelson, Jr, MD, Jordan S. Orange, MD, PhD, John M. Routes, MD, William T. Shearer, MD, PhD, Ricardo U. Sorensen, MD, James W. Verbsky, MD, PhD GlaxoSmithKline, Merck, and Aerocrine; has received payment for lectures from Genentech/ These parameters were developed by the Joint Task Force on Practice Parameters, representing Novartis, GlaxoSmithKline, and Merck; and has received research support from Genentech/ the American Academy of Allergy, Asthma & Immunology; the American College of Novartis and Merck. -

Primary Immunodeficiency Disorders
ALLERGY AND IMMUNOLOGY 00954543 /98 $8.00 + .OO PRIMARY IMMUNODEFICIENCY DISORDERS Robert J. Mamlok, MD Immunodeficiency is a common thought among both patients and physicians when confronted with what is perceived as an excessive num- ber, duration, or severity of infections. Because of this, the starting point for evaluating patients for suspected immunodeficiency is based on what constitutes ”too many infections.” It generally is agreed that children with normal immune systems may have an average of 6 to 8 respiratory tract infections per year for the first decade of life. Even after a pattern of ab- normal infection is established, questions of secondary immunodeficiency should first be raised. The relatively uncommon primary immunodefi- ciency diseases are statistically dwarfed by secondary causes of recurrent infection, such as malnutrition, respiratory allergy, chronic cardiovascular, pulmonary, and renal disease, and environmental factors. On the other hand, a dizzying spiral of progress in our understanding of the genetics and immunology of primary immunodeficiency disease has resulted in improved diagnostic and therapeutic tools. Twenty-five newly recognized immunologic disease genes have been cloned in the last 5 ~ears.2~It has become arguably more important than ever for us to recognize the clinical and laboratory features of these relatively uncommon, but increasingly treatable, disorders. CLASSIFICATION The immune system has been classically divided into four separate arms: The B-cell system responsible for antibody formation, the T-cell sys- From the Division of Pediatric Allergy and Immunology, Texas Tech University Health Sci- ences Center, Lubbock, Texas PRIMARY CARE VOLUME 25 NUMBER 4 DECEMBER 1998 739 740 MAMLOK tem responsible for immune cellular regulation, the phagocytic (poly- morphonuclear and mononuclear) system and the complement (opsonic) system. -

Agranulocytic Angina
University of Nebraska Medical Center DigitalCommons@UNMC MD Theses Special Collections 5-1-1939 Agranulocytic angina Louis T. Davies University of Nebraska Medical Center This manuscript is historical in nature and may not reflect current medical research and practice. Search PubMed for current research. Follow this and additional works at: https://digitalcommons.unmc.edu/mdtheses Part of the Medical Education Commons Recommended Citation Davies, Louis T., "Agranulocytic angina" (1939). MD Theses. 737. https://digitalcommons.unmc.edu/mdtheses/737 This Thesis is brought to you for free and open access by the Special Collections at DigitalCommons@UNMC. It has been accepted for inclusion in MD Theses by an authorized administrator of DigitalCommons@UNMC. For more information, please contact [email protected]. AGRANULOCYTIC ANGINA by LOUIS T. DAVIES Presented to the College of Medicine, University of Nebraska, Omaha, 1939 TABLE OF CONTENTS Introduction • . 1 Definition •• . • • 2 History . 3 Etiology ••• . • • 7 Classification .• 16 Symptoms and Course • . • • • 20 Experimental Work • • •• 40 Pathological Anatomy • • • . 43 Diagnosis and Differential Diagnosis •• . • 54 Therapy Prognosis • • • • • . 55 Discussion and Summary • • • • • • • 67 Conclusions • • • • • • • • • • • • • 73 ·Bibliography • • • • • • • • • • 75 * * * * * * 481028 _,,,....... ·- INTRODUCTION Agranulocytic Angina for the past seventeen years has been highly discussed both in medical centers and in literature. During this time the understanding of the disease has developed in the curriculum of the medical profession. Since 1922, when first described as a clinical entity by Schultz, it has been reported more frequently as the years passed until at the present time agranulocytosis is recognized widely as a disease process. Just as with the development of any medical problem this has been laden with various opinions on its course, etiology, etc., all of which has served to confuse the searching medical mind as to its true standing. -

Fatal Cerebral Hemorrhage Revealing Acute Lymphoblastic Leukemia with Leukostasis
www.ijcrt.org © 2020 IJCRT | Volume 8, Issue 6 June 2020 | ISSN: 2320-2882 Fatal cerebral hemorrhage revealing acute lymphoblastic leukemia with leukostasis 1Said Khallikane ,2 Mehdi Samali,3Aziz Benakrout, 4Abderrazzak Sabir, 5Samir Siah 1. Service of Anesthesiology and Intensive Care Unit, Third Military Hospital, Laayoune, Morocco 2. Service of Anesthesiology and Intensive Care Unit, Third Military Hospital, Laayoune, Morocco 3. Service of Anesthesiology and Intensive Care Unit, Military Teaching Mohammed V Hospital, Rabat, Morocco 4. Medico-Surgical Pole of laayoune, Sakia El Hamra Region, Service of Gastro-Enterology and Proctology, Third Military Hospital, Laayoune, Morocco 5. Service of Anesthesiology and Intensive Care Unit of Severe Burn Management, Military Teaching Mohammed V Hospital, Faculty of Medicine and Pharmacy of Rabat, Morocco 1. Service of Anesthesiology and Intensive Care Unit, Third Military Hospital, Laayoune, Morocco 1. Service of Cardiovascular Anesthesiology and Cardiac Intensive Care Unit, Mohammed V Military Teaching Hospital, Rabat, Morocco SUMMARY Neurological involvement is frequent in leukemia but is rarely the inaugural event. We report the case of a 15-year-old boy whose acute lymphoblastic leukemia was revealed by fatal cerebral hemorrhage associated with sepsis secondary to lung infection. Intracerebral hemorrhage remains a cause of death in hematologic malignancies. The patient presented with thrombocytopenia (24,000/mm3), leucostasis and hypofibrinogemia (1.10 g/L). Despite maximal medical and surgical treatment (platelets and fresh- frozen plasma transfusions, red blood cells transfusion, and craniotomy discharge), the patient died. The risk of death is high, and surgical treatment has not proven superior to medical therapy in terms of mortality rates and 6-month survival. -

CDG and Immune Response: from Bedside to Bench and Back Authors
CDG and immune response: From bedside to bench and back 1,2,3 1,2,3,* 2,3 1,2 Authors: Carlota Pascoal , Rita Francisco , Tiago Ferro , Vanessa dos Reis Ferreira , Jaak Jaeken2,4, Paula A. Videira1,2,3 *The authors equally contributed to this work. 1 Portuguese Association for CDG, Lisboa, Portugal 2 CDG & Allies – Professionals and Patient Associations International Network (CDG & Allies – PPAIN), Caparica, Portugal 3 UCIBIO, Departamento Ciências da Vida, Faculdade de Ciências e Tecnologia, Universidade NOVA de Lisboa, 2829-516 Caparica, Portugal 4 Center for Metabolic Diseases, UZ and KU Leuven, Leuven, Belgium Word count: 7478 Number of figures: 2 Number of tables: 3 This article has been accepted for publication and undergone full peer review but has not been through the copyediting, typesetting, pagination and proofreading process which may lead to differences between this version and the Version of Record. Please cite this article as doi: 10.1002/jimd.12126 This article is protected by copyright. All rights reserved. Abstract Glycosylation is an essential biological process that adds structural and functional diversity to cells and molecules, participating in physiological processes such as immunity. The immune response is driven and modulated by protein-attached glycans that mediate cell-cell interactions, pathogen recognition and cell activation. Therefore, abnormal glycosylation can be associated with deranged immune responses. Within human diseases presenting immunological defects are Congenital Disorders of Glycosylation (CDG), a family of around 130 rare and complex genetic diseases. In this review, we have identified 23 CDG with immunological involvement, characterised by an increased propensity to – often life-threatening – infection. -

Severe Congenital Neutropenia with Monocytosis and Non-Syndromic Sensorineural Hear
Venugopal et al. BMC Medical Genetics (2020) 21:35 https://doi.org/10.1186/s12881-020-0971-z RESEARCH ARTICLE Open Access Two monogenic disorders masquerading as one: severe congenital neutropenia with monocytosis and non-syndromic sensorineural hearing loss Parvathy Venugopal1,2†, Lucia Gagliardi1,2,3,4,5†, Cecily Forsyth6†, Jinghua Feng7,8, Kerry Phillips9, Milena Babic1,2, Nicola K. Poplawski9, Hugh Young Rienhoff Jr10, Andreas W. Schreiber2,7,8,11, Christopher N. Hahn1,2,3,8†, Anna L. Brown1,2,8† and Hamish S. Scott1,2,3,7,8*† Abstract Background: We report a large family with four successive generations, presenting with a complex phenotype of severe congenital neutropenia (SCN), partially penetrant monocytosis, and hearing loss of varying severity. Methods: We performed whole exome sequencing to identify the causative variants. Sanger sequencing was used to perform segregation analyses on remaining family members. Results: We identified and classified a pathogenic GFI1 variant and a likely pathogenic variant in MYO6 which together explain the complex phenotypes seen in this family. Conclusions: We present a case illustrating the benefits of a broad screening approach that allows identification of oligogenic determinants of complex human phenotypes which may have been missed if the screening was limited to a targeted gene panel with the assumption of a syndromic disorder. This is important for correct genetic diagnosis of families and disentangling the range and severity of phenotypes associated with high impact variants. Keywords: Neutropenia, Congenital neutropenia, Leukemia predisposition, Polygenic inheritance, Hearing loss Background cases [2]. It may also occur as a part of a syndrome with Severe congenital neutropenia (SCN) was first described other developmental defects (e.g.