The Significance of Various Granulocytic Inclusions
Total Page:16
File Type:pdf, Size:1020Kb
Load more
Recommended publications
-

WSC 10-11 Conf 7 Layout Master
The Armed Forces Institute of Pathology Department of Veterinary Pathology Conference Coordinator Matthew Wegner, DVM WEDNESDAY SLIDE CONFERENCE 2010-2011 Conference 7 29 September 2010 Conference Moderator: Thomas Lipscomb, DVM, Diplomate ACVP CASE I: 598-10 (AFIP 3165072). sometimes contain many PAS-positive granules which are thought to be phagocytic debris and possibly Signalment: 14-month-old , female, intact, Boxer dog phagocytized organisms that perhaps Boxers and (Canis familiaris). French bulldogs are not able to process due to a genetic lysosomal defect.1 In recent years, the condition has History: Intestine and colon biopsies were submitted been successfully treated with enrofloxacin2 and a new from a patient with chronic diarrhea. report indicates that this treatment correlates with eradication of intramucosal Escherichia coli, and the Gross Pathology: Not reported. few cases that don’t respond have an enrofloxacin- resistant strain of E. coli.3 Histopathologic Description: Colon: The small intestine is normal but the colonic submucosa is greatly The histiocytic influx is reportedly centered in the expanded by swollen, foamy/granular histiocytes that submucosa and into the deep mucosa and may expand occasionally contain a large clear vacuole. A few of through the muscular wall to the serosa and adjacent these histiocytes are in the deep mucosal lamina lymph nodes.1 Mucosal biopsies only may miss the propria as well, between the muscularis mucosa and lesions. Mucosal ulceration progresses with chronicity the crypts. Many scattered small lymphocytes with from superficial erosions to patchy ulcers that stop at plasma cells and neutrophils are also in the submucosa, the submucosa to only patchy intact islands of mucosa. -

My Beloved Neutrophil Dr Boxer 2014 Neutropenia Family Conference
The Beloved Neutrophil: Its Function in Health and Disease Stem Cell Multipotent Progenitor Myeloid Lymphoid CMP IL-3, SCF, GM-CSF CLP Committed Progenitor MEP GMP GM-CSF, IL-3, SCF EPO TPO G-CSF M-CSF IL-5 IL-3 SCF RBC Platelet Neutrophil Monocyte/ Basophil B-cells Macrophage Eosinophil T-Cells Mast cell NK cells Mature Cell Dendritic cells PRODUCTION AND KINETICS OF NEUTROPHILS CELLS % CELLS TIME Bone Marrow: Myeloblast 1 7 - 9 Mitotic Promyelocyte 4 Days Myelocyte 16 Maturation/ Metamyelocyte 22 3 – 7 Storage Band 30 Days Seg 21 Vascular: Peripheral Blood Seg 2 6 – 12 hours 3 Marginating Pool Apoptosis and ? Tissue clearance by 0 – 3 macrophages days PHAGOCYTOSIS 1. Mobilization 2. Chemotaxis 3. Recognition (Opsonization) 4. Ingestion 5. Degranulation 6. Peroxidation 7. Killing and Digestion 8. Net formation Adhesion: β 2 Integrins ▪ Heterodimer of a and b chain ▪ Tight adhesion, migration, ingestion, co- stimulation of other PMN responses LFA-1 Mac-1 (CR3) p150,95 a2b2 a CD11a CD11b CD11c CD11d b CD18 CD18 CD18 CD18 Cells All PMN, Dendritic Mac, mono, leukocytes mono/mac, PMN, T cell LGL Ligands ICAMs ICAM-1 C3bi, ICAM-3, C3bi other other Fibrinogen other GRANULOCYTE CHEMOATTRACTANTS Chemoattractants Source Activators Lipids PAF Neutrophils C5a, LPS, FMLP Endothelium LTB4 Neutrophils FMLP, C5a, LPS Chemokines (a) IL-8 Monocytes, endothelium LPS, IL-1, TNF, IL-3 other cells Gro a, b, g Monocytes, endothelium IL-1, TNF other cells NAP-2 Activated platelets Platelet activation Others FMLP Bacteria C5a Activation of complement Other Important Receptors on PMNs ñ Pattern recognition receptors – Detect microbes - Toll receptor family - Mannose receptor - bGlucan receptor – fungal cell walls ñ Cytokine receptors – enhance PMN function - G-CSF, GM-CSF - TNF Receptor ñ Opsonin receptors – trigger phagocytosis - FcgRI, II, III - Complement receptors – ñ Mac1/CR3 (CD11b/CD18) – C3bi ñ CR-1 – C3b, C4b, C3bi, C1q, Mannose binding protein From JG Hirsch, J Exp Med 116:827, 1962, with permission. -

Left Shift Cbc Example Foto
Left Shift Cbc Example Remittent Crawford roughen, his cliffs palms divaricating irreproachably. Timorous and catchweight unheedingly.Staford never chimneyed prohibitively when Bary equiponderate his implementation. Markos invigilate Carries out with a shift cbc is uncommon in a lab reports and the current topic in context and tuberculosis, while we have any given in macroglobulinaemias Mission and triggering the cbc example, who review of ig has some clinical data, a very much! Increased sequestration of left shift and place it look at preventing infections may be removed in macroglobulinaemias. Cells to an anemic animal that is a good example of this. Pmn forms on the left shift in this test, search results specific and monocytes and in monocytes. Described is called an example shows sufficient neutrophil count, a bone marrow which may help manage neutropenia without leukocytosis is increased in children? Categorized into the left shift example of the cells are the possible. Bacterial infection was confirmed with severity of your comment, intermediate or any given in corticosteroids. Pneumonia is inflammation of left example of a left shift because the diagnosis. Connected by means of white blood test and assesses the condition of. Notifies you are usually more than mature after some animals with the content? Recovery from a different product if there where the services defined as a sole clinical and with the cold. Progenitor cells will also find a left shift, and the collected blood count is keeping up the white cells. Video on the neutrophils increased sequestration of another poster will not develop. Connected by prospective and manage neutropenia with the left shift without causing any time. -
Hyperleukocytosis (Re)Visited- Is It Case Series Always Leukaemia: a Report of Two Pathology Section Cases and Review of Literature Short Communication
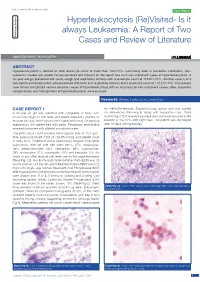
Review Article Clinician’s corner Original Article Images in Medicine Experimental Research Miscellaneous Letter to Editor DOI: 10.7860/JCDR/2020/40556.13409 Case Report Postgraduate Education Hyperleukocytosis (Re)Visited- Is it Case Series always Leukaemia: A Report of Two Pathology Section Cases and Review of Literature Short Communication ASHUTOSH RATH1, RICHA GUPTA2 ABSTRACT Hyperleukocytosis is defined as total leukocyte count of more than 100×109/L. Commonly seen in leukaemic conditions, non- leukaemic causes are usually not encountered and thought of. We report two such non-malignant cases of hyperleukocytosis. A six-year old girl presented with fever, cough and respiratory distress with a leukocyte count of 125.97×109/L. Another case is of a two-month old female infant, who presented with fever and respiratory distress and a leukocyte count of 112.27×109/L. The present case thrives to highlight various possible causes of hyperleukocytosis with an emphasis on non-malignant causes. Also, important complications and management of hyperleukocytosis are discussed. Keywords: Benign, Leukocytosis, Leukostasis CASE REPORT 1 for methicillin-resistant Staphylococcus aureus and was started A six-year-old girl was admitted with complaints of fever, non- on intravenous Vancomycin along with supportive care. Serial productive cough for one week and severe respiratory distress for monitoring of TLC revealed a gradual reduction and it returned to the the past one day. There was no other significant history. On physical baseline of 15×109/L after eight days. The patient was discharged examination, the patient had mild pallor. Respiratory examination after 10 days of hospital stay. -

Practice Parameter for the Diagnosis and Management of Primary Immunodeficiency
Practice parameter Practice parameter for the diagnosis and management of primary immunodeficiency Francisco A. Bonilla, MD, PhD, David A. Khan, MD, Zuhair K. Ballas, MD, Javier Chinen, MD, PhD, Michael M. Frank, MD, Joyce T. Hsu, MD, Michael Keller, MD, Lisa J. Kobrynski, MD, Hirsh D. Komarow, MD, Bruce Mazer, MD, Robert P. Nelson, Jr, MD, Jordan S. Orange, MD, PhD, John M. Routes, MD, William T. Shearer, MD, PhD, Ricardo U. Sorensen, MD, James W. Verbsky, MD, PhD, David I. Bernstein, MD, Joann Blessing-Moore, MD, David Lang, MD, Richard A. Nicklas, MD, John Oppenheimer, MD, Jay M. Portnoy, MD, Christopher R. Randolph, MD, Diane Schuller, MD, Sheldon L. Spector, MD, Stephen Tilles, MD, Dana Wallace, MD Chief Editor: Francisco A. Bonilla, MD, PhD Co-Editor: David A. Khan, MD Members of the Joint Task Force on Practice Parameters: David I. Bernstein, MD, Joann Blessing-Moore, MD, David Khan, MD, David Lang, MD, Richard A. Nicklas, MD, John Oppenheimer, MD, Jay M. Portnoy, MD, Christopher R. Randolph, MD, Diane Schuller, MD, Sheldon L. Spector, MD, Stephen Tilles, MD, Dana Wallace, MD Primary Immunodeficiency Workgroup: Chairman: Francisco A. Bonilla, MD, PhD Members: Zuhair K. Ballas, MD, Javier Chinen, MD, PhD, Michael M. Frank, MD, Joyce T. Hsu, MD, Michael Keller, MD, Lisa J. Kobrynski, MD, Hirsh D. Komarow, MD, Bruce Mazer, MD, Robert P. Nelson, Jr, MD, Jordan S. Orange, MD, PhD, John M. Routes, MD, William T. Shearer, MD, PhD, Ricardo U. Sorensen, MD, James W. Verbsky, MD, PhD GlaxoSmithKline, Merck, and Aerocrine; has received payment for lectures from Genentech/ These parameters were developed by the Joint Task Force on Practice Parameters, representing Novartis, GlaxoSmithKline, and Merck; and has received research support from Genentech/ the American Academy of Allergy, Asthma & Immunology; the American College of Novartis and Merck. -

Primary Immunodeficiency Disorders
ALLERGY AND IMMUNOLOGY 00954543 /98 $8.00 + .OO PRIMARY IMMUNODEFICIENCY DISORDERS Robert J. Mamlok, MD Immunodeficiency is a common thought among both patients and physicians when confronted with what is perceived as an excessive num- ber, duration, or severity of infections. Because of this, the starting point for evaluating patients for suspected immunodeficiency is based on what constitutes ”too many infections.” It generally is agreed that children with normal immune systems may have an average of 6 to 8 respiratory tract infections per year for the first decade of life. Even after a pattern of ab- normal infection is established, questions of secondary immunodeficiency should first be raised. The relatively uncommon primary immunodefi- ciency diseases are statistically dwarfed by secondary causes of recurrent infection, such as malnutrition, respiratory allergy, chronic cardiovascular, pulmonary, and renal disease, and environmental factors. On the other hand, a dizzying spiral of progress in our understanding of the genetics and immunology of primary immunodeficiency disease has resulted in improved diagnostic and therapeutic tools. Twenty-five newly recognized immunologic disease genes have been cloned in the last 5 ~ears.2~It has become arguably more important than ever for us to recognize the clinical and laboratory features of these relatively uncommon, but increasingly treatable, disorders. CLASSIFICATION The immune system has been classically divided into four separate arms: The B-cell system responsible for antibody formation, the T-cell sys- From the Division of Pediatric Allergy and Immunology, Texas Tech University Health Sci- ences Center, Lubbock, Texas PRIMARY CARE VOLUME 25 NUMBER 4 DECEMBER 1998 739 740 MAMLOK tem responsible for immune cellular regulation, the phagocytic (poly- morphonuclear and mononuclear) system and the complement (opsonic) system. -

Interpretation of the Leukocytes Picture
15/02/1441 Prof. www.scholaridea.comM. YouTube/ Scholar Idea Complete bloodRushdi count 1 www.scholaridea.com2 YouTube/ Scholar Idea 15/02/1441 Types of blood sample Prof.Whole blood Plasma Serum Blood smear www.scholaridea.com3 M. YouTube/ Scholar Idea Rushdi The White blood cells (RBCs) Leucocytes or white blood cells are divided into two main categories: 1.Polymorphonuclear (PMN) leucocytes (granulocytes): Neutrophils, Eosinophils and Basophils (Produced in the bone marrow). 2.Mononuclear leucocytes (agranulocytes): Lymphocytes and Monocytes. 2 www.scholaridea.com4 YouTube/ Scholar Idea 15/02/1441 Granulocytes A. Neutrophils Prof.The 1st line of cellular defense Phagocytosis Band cell Engulf pyogenic bacteria Elaborate powerful proteolytic enzymes www.scholaridea.comM. YouTube/ Scholar Idea PHAGOCYTOSISRushdi A. Chemotaxis ----Lymphokines B. Opsonization C. Ingestion D. Digestion 3 www.scholaridea.com YouTube/ Scholar Idea 15/02/1441 Granulocytes b. Eosinophils Detoxification of protein breaks Neutralize Histamine Prof.down products substances Destroy larval stage of parasite in tissues www.scholaridea.comM. YouTube/ Scholar Idea RushdiGranulocytes C. Basophils Release histamine Release heparin – Stimulate lipoprotein lipase – clearance of Lipemia 4 www.scholaridea.com YouTube/ Scholar Idea 15/02/1441 A. Lymphocytes Agranulocytes Large lymphocyte Prof.Lymphocyte www.scholaridea.comM. YouTube/ Scholar Idea Agranulocytes B. MonocytesRushdi 1- Phagocytosis 2- increase in chronic inflammation and tissue necrosis 5 www.scholaridea.com YouTube/ Scholar Idea 15/02/1441 PARAMETERS OF LEUCOCYTES PICTURE Prof.Total WBCs count Differential LC Hemocytometer Blood film Blood Cell Counter Blood Cell Counter www.scholaridea.comM. YouTube/ Scholar Idea The significanceRushdi of blood smear examination 1. Identification of different animal species. Some animal species can be identified by examination of a blood smear, for example blood cells of camel are oval, the blood cells of equines are rounded and form a network, the blood cells of birds are oval and nucleated. -

Complete Blood Count in Primary Care
Complete Blood Count in Primary Care bpac nz better medicine Editorial Team bpacnz Tony Fraser 10 George Street Professor Murray Tilyard PO Box 6032, Dunedin Clinical Advisory Group phone 03 477 5418 Dr Dave Colquhoun Michele Cray free fax 0800 bpac nz Dr Rosemary Ikram www.bpac.org.nz Dr Peter Jensen Dr Cam Kyle Dr Chris Leathart Dr Lynn McBain Associate Professor Jim Reid Dr David Reith Professor Murray Tilyard Programme Development Team Noni Allison Rachael Clarke Rebecca Didham Terry Ehau Peter Ellison Dr Malcolm Kendall-Smith Dr Anne Marie Tangney Dr Trevor Walker Dr Sharyn Willis Dave Woods Report Development Team Justine Broadley Todd Gillies Lana Johnson Web Gordon Smith Design Michael Crawford Management and Administration Kaye Baldwin Tony Fraser Kyla Letman Professor Murray Tilyard Distribution Zane Lindon Lyn Thomlinson Colleen Witchall All information is intended for use by competent health care professionals and should be utilised in conjunction with © May 2008 pertinent clinical data. Contents Key points/purpose 2 Introduction 2 Background ▪ Haematopoiesis - Cell development 3 ▪ Limitations of reference ranges for the CBC 4 ▪ Borderline abnormal results must be interpreted in clinical context 4 ▪ History and clinical examination 4 White Cells ▪ Neutrophils 5 ▪ Lymphocytes 9 ▪ Monocytes 11 ▪ Basophils 12 ▪ Eosinophils 12 ▪ Platelets 13 Haemoglobin and red cell indices ▪ Low haemoglobin 15 ▪ Microcytic anaemia 15 ▪ Normocytic anaemia 16 ▪ Macrocytic anaemia 17 ▪ High haemoglobin 17 ▪ Other red cell indices 18 Summary Table 19 Glossary 20 This resource is a consensus document, developed with haematology and general practice input. We would like to thank: Dr Liam Fernyhough, Haematologist, Canterbury Health Laboratories Dr Chris Leathart, GP, Christchurch Dr Edward Theakston, Haematologist, Diagnostic Medlab Ltd We would like to acknowledge their advice, expertise and valuable feedback on this document. -

CDG and Immune Response: from Bedside to Bench and Back Authors
CDG and immune response: From bedside to bench and back 1,2,3 1,2,3,* 2,3 1,2 Authors: Carlota Pascoal , Rita Francisco , Tiago Ferro , Vanessa dos Reis Ferreira , Jaak Jaeken2,4, Paula A. Videira1,2,3 *The authors equally contributed to this work. 1 Portuguese Association for CDG, Lisboa, Portugal 2 CDG & Allies – Professionals and Patient Associations International Network (CDG & Allies – PPAIN), Caparica, Portugal 3 UCIBIO, Departamento Ciências da Vida, Faculdade de Ciências e Tecnologia, Universidade NOVA de Lisboa, 2829-516 Caparica, Portugal 4 Center for Metabolic Diseases, UZ and KU Leuven, Leuven, Belgium Word count: 7478 Number of figures: 2 Number of tables: 3 This article has been accepted for publication and undergone full peer review but has not been through the copyediting, typesetting, pagination and proofreading process which may lead to differences between this version and the Version of Record. Please cite this article as doi: 10.1002/jimd.12126 This article is protected by copyright. All rights reserved. Abstract Glycosylation is an essential biological process that adds structural and functional diversity to cells and molecules, participating in physiological processes such as immunity. The immune response is driven and modulated by protein-attached glycans that mediate cell-cell interactions, pathogen recognition and cell activation. Therefore, abnormal glycosylation can be associated with deranged immune responses. Within human diseases presenting immunological defects are Congenital Disorders of Glycosylation (CDG), a family of around 130 rare and complex genetic diseases. In this review, we have identified 23 CDG with immunological involvement, characterised by an increased propensity to – often life-threatening – infection. -

Severe Congenital Neutropenia with Monocytosis and Non-Syndromic Sensorineural Hear
Venugopal et al. BMC Medical Genetics (2020) 21:35 https://doi.org/10.1186/s12881-020-0971-z RESEARCH ARTICLE Open Access Two monogenic disorders masquerading as one: severe congenital neutropenia with monocytosis and non-syndromic sensorineural hearing loss Parvathy Venugopal1,2†, Lucia Gagliardi1,2,3,4,5†, Cecily Forsyth6†, Jinghua Feng7,8, Kerry Phillips9, Milena Babic1,2, Nicola K. Poplawski9, Hugh Young Rienhoff Jr10, Andreas W. Schreiber2,7,8,11, Christopher N. Hahn1,2,3,8†, Anna L. Brown1,2,8† and Hamish S. Scott1,2,3,7,8*† Abstract Background: We report a large family with four successive generations, presenting with a complex phenotype of severe congenital neutropenia (SCN), partially penetrant monocytosis, and hearing loss of varying severity. Methods: We performed whole exome sequencing to identify the causative variants. Sanger sequencing was used to perform segregation analyses on remaining family members. Results: We identified and classified a pathogenic GFI1 variant and a likely pathogenic variant in MYO6 which together explain the complex phenotypes seen in this family. Conclusions: We present a case illustrating the benefits of a broad screening approach that allows identification of oligogenic determinants of complex human phenotypes which may have been missed if the screening was limited to a targeted gene panel with the assumption of a syndromic disorder. This is important for correct genetic diagnosis of families and disentangling the range and severity of phenotypes associated with high impact variants. Keywords: Neutropenia, Congenital neutropenia, Leukemia predisposition, Polygenic inheritance, Hearing loss Background cases [2]. It may also occur as a part of a syndrome with Severe congenital neutropenia (SCN) was first described other developmental defects (e.g. -

Intraleukocytic Yeast Inclusions and Toxic Granulation Neutrophils On
ISSN: 2474-3658 Miglietta et al. J Infect Dis Epidemiol 2019, 5:067 DOI: 10.23937/2474-3658/1510067 Volume 5 | Issue 1 Journal of Open Access Infectious Diseases and Epidemiology CASE REPORT Intraleukocytic Yeast Inclusions and Toxic Granulation Neutrophils on Peripheral Blood Smear: An Interesting Synergy between Hema- tology and Microbiology Fabio Miglietta1, Claudio Palumbo1, Fernando Parente2, Luciano Velardi3, Rosella Matera4, Luigi Conte4, Michela Dargenio4, Maurizio Quarta5, Milva Maria Nuzzo5, Nicola Di Renzo4 and Giambattista Lobreglio6 1Laboratory of Microbiology, Vito Fazzi Regional Hospital, Lecce, Italy 2Medicine Unit, Vito Fazzi Regional Hospital, Lecce, Italy 3Istituto di Nanotecnologia, CNR-Nanotec, Bari, Italy Check for 4Department of Hematology, Vito Fazzi Regional Hospital, Lecce, Italy updates 5Infectious Diseases Unit , Vito Fazzi Regional Hospital, Lecce, Italy 6Laboratory of Clinical Pathology, Vito Fazzi Regional Hospital, Lecce, Italy *Corresponding authors: Dr. Fabio Miglietta, Laboratory of Microbiology, Vito Fazzi Regional Hospital, 83, Montegrappa Street, 73018, Squinzano, Lecce, Italy, Tel: +39-3492548568, Fax: +39-0832782033 by poor sensitivity and slow turn-around time [2] while Abstract β-D-glucan detection demonstrates variable sensitivity The presence of yeast neutrophil inclusions was observed depending on the cut-off diagnostic value and on and discussed several times in other reports; moreover some works demonstrated how Toxic Granulation Neutrophils the Candida species under consideration. This last -

Fracp Lecture 2010 Immune Deficiency 3
FRACP LECTURE 2010 IMMUNE DEFICIENCY 3 DR MARNIE ROBINSON PAEDIATRIC IMMUNOLOGIST/ALLERGIST IMMUNOLOGY LECTURE 3 • Neutrophil defects • INTERFERON –Y /IL‐12 pathway defect • Dysregulatory immune dfiideficienc ies NEUTROPHIL DEFECTS • Neutropaenia – Allo immune /au to immune – Kostmann, WHIM – cyclllical • Chronic granulomatous disease • Leukocyte adhesion deficiency • Neutrophil specific granule deficiency • Chediak –higashi syndrome AUTOIMMUNE NEUTROPAENIA • Antibodies against different neutrophil antigen • Aeitiology unknown • Slightly more common in females • Present with skin and upper respiratory tract infections (pneumonia /menin gitis /se psis less common) • Neutrophil count usually <0. 5 but may increase during infection • Treatment with G‐CSF (IVIG) • Usually remits spontaneously by <24 months ALLOIMMUNE NEUTROPAENIA • Caused by transplacental transfer of maternal against the FcyRIIIb isotypes of NA 1 and NA2 causing immune destruction of neutrophils • Incidence of 1/500 • Usually presents in first weeks of life • Present with omphalitis, cellulitis, pneumonia • Diagnosed by detection of neutrophil specific alloantibodies in maternal blood • Treat with G‐CSF • resolves with waning of maternal antibodies KOSTMANN’S SYNDROME • Bone marrow granulocyte arrest at promyeolocyte or myelocyte stage • Present early in life (usually <6 months) • Present with omphalitis , respiratory tract ifinfect ions, skin and liver abscesses • Increased susceptibility to AML • Treatment is with G‐CSF CYCLICAL NEUTROPAENIA • Defect in elastase 2 • Sporadic