Hennebert's Sign in Superior Semicircular Canal Dehiscence
Total Page:16
File Type:pdf, Size:1020Kb

Load more
Recommended publications
-

Assessment of Bone Conduction Thresholds After Surgical Treatment in Patients with Labyrinthine Fistula
Turkish Archives of Otorhinolaryngology Turk Arch Otorhinolaryngol 2018; 56(2): 89-94 89 Türk Otorinolarengoloji Arşivi Assessment of Bone Conduction Thresholds After Surgical Treatment in Patients with Labyrinthine Fistula Müzeyyen Yıldırım Baylan1 , Ümit Yılmaz1 , Zeki Akkuş2 , İsmail Topçu1 1Department of Otorhinolaryngology, Dicle University School of Medicine, Diyarbakır, Turkey Original Investigation 2Department of Biostatistics, Dicle University School of Medicine, Diyarbakır, Turkey Abstract Objective: This study aimed to analyze the bone con- years. In the post-operative period, it was possib- duction thresholds before and after surgery in chronic le to conduct audiological follow-up on 20 patients. otitis media patients with cholesteatoma who had In these follow-ups, 16 patients showed no change labyrinthine fistula and whose cholesteatoma matrix in bone conduction thresholds, two patients showed had been completely cleaned. worsening, and two showed improvement. When Methods: The study was performed between 2013 pre- and post-operative bone conduction thresholds to 2017 with 23 chronic otitis media patients who at each frequency were compared separately, no sig- had labyrinthine fistula with cholesteatoma and who were operated at the Department of Otorhinolar- nificant difference was found (p=0.937). No statis- yngology of Dicle University School of Medicine. tically significant difference was found between the Patients were assessed by anamnesis and examina- pre- and post-operative means at the four frequencies tion and when necessary, by temporal computerized (p=0.712). tomography and diffusion magnetic resonance ima- Conclusion: In this study, we found that to reduce ging. Bone conduction thresholds at frequencies of complications relating to cholesteatoma, it might be 500, 1000, 2000, and 4000 Hz were determined by audiometric examination and they were compared necessary to completely remove the matrix especially before and after surgery. -
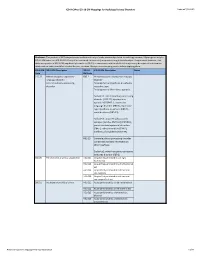
ICD-9/10 Mapping Spreadsheet
ICD-9-CM to ICD-10-CM Mappings for Audiology Related Disorders Updated 7/16/2015 Disclaimer: This product is NOT comprehensive and consists only of codes commonly related to audiology services. Mappings are only to ICD-10-CM codes, not ICD-10-PCS. Every effort was made to accurately map codes using detailed analysis. Keep in mind, however, that while many codes in ICD-9-CM map directly to codes in ICD-10, in some cases, additional clinical analysis may be required to determine which code or codes should be selected for your situation. Always review mapping results before applying them. ICD-9-CM ICD-9-CM Description ICD-10- ICD-10-CM Description Notes Code CM Code 315.32 Mixed receptive-expressive F80.2 Mixed receptive-expressive language language disorder disorder Central auditory processing Developmental dysphasia or aphasia, disorder receptive type Developmental Wernicke's aphasia Excludes1: central auditory processing disorder (H93.25), dysphasia or aphasia NOS (R47.-), expressive language disorder (F80.1), expressive type dysphasia or aphasia (F80.1), word deafness (H93.25) Excludes2: acquired aphasia with epilepsy [Landau-Kleffner] (G40.80-), pervasive developmental disorders (F84.-), selective mutism (F94.0), intellectual disabilities (F70-F79) H93.25 Central auditory processing disorder Congenital auditory imperception Word deafness Excludes1: mixed receptive-epxressive language disorder (F80.2) 380.00 Perichondritis of pinna, unspecified H61.001 Unspecified perichondritis of right external ear H61.002 Unspecified perichondritis -

Hearing Loss, Vertigo and Tinnitus
HEARING LOSS, VERTIGO AND TINNITUS Jonathan Lara, DO April 29, 2012 Hearing Loss Facts S Men are more likely to experience hearing loss than women. S Approximately 17 percent (36 million) of American adults report some degree of hearing loss. S About 2 to 3 out of every 1,000 children in the United States are born deaf or hard-of-hearing. S Nine out of every 10 children who are born deaf are born to parents who can hear. Hearing Loss Facts S The NIDCD estimates that approximately 15 percent (26 million) of Americans between the ages of 20 and 69 have high frequency hearing loss due to exposure to loud sounds or noise at work or in leisure activities. S Only 1 out of 5 people who could benefit from a hearing aid actually wears one. S Three out of 4 children experience ear infection (otitis media) by the time they are 3 years old. Hearing Loss Facts S There is a strong relationship between age and reported hearing loss: 18 percent of American adults 45-64 years old, 30 percent of adults 65-74 years old, and 47 percent of adults 75 years old or older have a hearing impairment. S Roughly 25 million Americans have experienced tinnitus. S Approximately 4,000 new cases of sudden deafness occur each year in the United States. Hearing Loss Facts S Approximately 615,000 individuals have been diagnosed with Ménière's disease in the United States. Another 45,500 are newly diagnosed each year. S One out of every 100,000 individuals per year develops an acoustic neurinoma (vestibular schwannoma). -

Hearing Loss for the Primary Care Physician
Hearing Loss for the Primary Care Physician Loriebeth D’Elia, Au.D. Doctor of Audiology Department of Otolaryngology The Ohio State University Wexner Medical Center What is an audiologist? Audiologists are the primary health-care professionals who evaluate, diagnose, treat, and manage hearing loss and balance disorders in adults and children Most earn a clinical doctorate in audiology (AuD), however some posses a PhD, doctor of science degree, (ScD) or a Master’s degree State licensed Additional certifications exist (ABA Board Certified, CCC-A, PASC, CISC) 1 Patient A • 80 year-old Female • Long-term patient • Accompanied by daughter who is speaking loudly to her • Difficulty communicating in office • Reported trying hearing aids 10 years ago • Limited benefit • Expensive Untreated Hearing loss • Physical, emotional and social consequences • Adherence to medical recommendations • More likely to report • Depression • Anxiety • Paranoia • Social isolation 2 Patient A in Office Screening? • Whispered voice test • Finger rubbing • Quick, simple, inexpensive • Limitations: subjective and not standardized • Tuning Fork • Hearing Handicap Inventory for Adults/Elderly (HHIA/E) • Standardized sound production device • Referral to audiology for confirmatory testing! Amplified Headset • Amplified headsets can be purchased through retail stores • Pros: • Inexpensive- around $150 • Ease of use for visually impaired and those with dexterity challenges • Cons: • Cosmetics • Limited distance for the microphone to pick up- hard wired to patient 3 Patient A’s hearing test PITCH (Hz) Low High Soft Range of Normal Hearing Right 75 dB Left 80 dB VOLUME (dB) VOLUME Loud Right 110 80 44 Left 105 75 52 Medical Clearance • Medical Clearance is required prior to a patient being fit with hearing aids. -

Spectrum of Third Window Abnormalities: Semicircular Canal Dehiscence and Beyond
Published August 25, 2016 as 10.3174/ajnr.A4922 REVIEW ARTICLE Spectrum of Third Window Abnormalities: Semicircular Canal Dehiscence and Beyond X M.-L. Ho, X G. Moonis, X C.F. Halpin, and X H.D. Curtin ABSTRACT SUMMARY: Third window abnormalities are defects in the integrity of the bony structure of the inner ear, classically producing sound-/ pressure-induced vertigo (Tullio and Hennebert signs) and/or a low-frequency air-bone gap by audiometry. Specific anatomic defects include semicircular canal dehiscence, perilabyrinthine fistula, enlarged vestibular aqueduct, dehiscence of the scala vestibuli side of the cochlea, X-linked stapes gusher, and bone dyscrasias. We discuss these various entities and provide key examples from our institutional teaching file with a discussion of symptomatology, temporal bone CT, audiometry, and vestibular-evoked myogenic potentials. ABBREVIATIONS: EVAS ϭ enlarged vestibular aqueduct syndrome; SSCCD ϭ superior semicircular canal dehiscence hird window abnormalities are defects in the integrity of the ing effects decrease air conduction. The 2 physiologic windows Tbony structure of the inner ear, first described by Minor et al between the middle and inner ear are the oval window, which in 1998.1 In 2008, Merchant and Rosowski2 proposed a universal transmits vibrations from the auditory ossicles, and the round theory for the underlying mechanism of hearing loss accompany- window of the cochlea. With air conduction, there is physiologic ing these defects. Normal sound conduction is transmitted entrainment of the oval and round windows due to coupling by through the oval and round windows, which serve as fluid inter- incompressible perilymph. Pressure differences between the co- faces between air in the middle ear and perilymphatic fluid spaces chlear perilymphatic spaces activate hair cells and create the per- of the inner ear. -

The Coexistence of Labyrinthine Fistula and the Facial Canal Dehiscence
The Mediterranean Journal of Otology ORIGINAL ARTICLE Management of Labyrinthine Fistula and Accompanying Findings: The Coexistence of Labyrinthine Fistula and the Facial Canal Dehiscence Masoud Naderpour, Ghodrat Mohammadi, Najmeh Doostmohammadian Department of Otorhinolaryngology, Tabriz University of Medical science, Tabriz, Iran OBJECTIVE: To describe the audio-vestibular results of labyrinthine fistula surgery in patients with cholesteatoma. Correspondent Author: PATIENTS AND METHODS: Data of 185 patients who had undergone Chodrat Mohammadi Dept. Otorhnotaryngology Tabriz surgery for cholesteatoma between 2001 and 2007 were reviewed. University of Medical Sciences, Three-layer sealing was used for the management of fistula. Tabriz, ‹ran RESULTS: Twenty patients were found to have labyrinthine fistula, of which 11 (55%) were male and 9(45%) female. Fistula wase located in lateral Tel: + 98- 9141141619 semicircular canal in all cases. Correlation of labyrinthine fistula and facial E-mail: [email protected] nerve dehiscence was statistically significant. Follow up was done for 1- 6 year. Postoperatively, vertigo disappeared in 19 (95 %) patients. Submitted: 14 April 2008 Revised: 10 July 2008 Hearing remained unchanged in 18 (90 %) patients. Worsening in bone Accepted: 17 July 2008 conduction thresholds was observed in 2 (10 %) patients. Postoperative deafness did not occur. Mediterr J Otol 2008; 4: 132-137 CONCLUSION: Possibility of facial nerve dehiscence and tegmen defect should be considered in patients with labyrinthine fistula. Three-layer Copyright 2005 © The Mediterranean sealing may be a valuable technique in surgical treatment of labyrinthine Society of Otology and Audiology fistula, lowering the risk of cochleovestibular functions. 132 Management of labyrinthine fistula and accompanying findings Cholesteatoma is a pocket or cystic lesion consisting of Labyrinthine fistula (LF) is encountered during stratified squamous epithelium and proliferative keratin surgery for cholesteatoma with an average frequency within the temporal bone. -

Head Spinning?? Evaluation of Dizziness
Head Spinning?? Evaluation of Dizziness 1 Kirsten Bonnin, M.M.S., PA-C ASAPA Fall Conference October 5, 2019 Learning Objectives 2 Describe the pathophysiology of vertigo Discuss the etiologies of vertigo Compare and contrast peripheral and central vertigo Discuss the diagnostic studies used in the evaluation of vertigo Discuss clinical presentation and management of various causes of vertigo Presenting Problem 3 . Dizziness . Imbalance . Whirling . Unsteadiness . Twisting . Wooziness . Turning . Floating . Rotating . Lightheadedness . Tilting . Disorientation . Moving . Nearly blacked out . Rocking . Presyncope . Disequilibrium Vertigo 4 • Vertigo is a symptom • Defined as a sensation of motion, when there is no motion or exaggerated sense of movement May be associated with nystagmus and postural instability Differential Diagnosis for Vertigo 5 o Anxiety disorder o Ménière disease o Arrhythmia o Motion sickness/disembarkment o Benign paroxysmal positional vertigo syndrome (BPPV) o Multiple sclerosis o Cardiogenic (heart failure, tamponade, o Neurocardiogenic (neurally mediated aortic stenosis) syncope, postural tachycardia o Cerebellar degeneration, hemorrhage, syndrome) or tumor o Orthostatic hypotension o Cerebrovascular ischemia or stroke o Ototoxicity (medication) o Dehydration o Perilymphatic fistula o Eustachian tube dysfunction/middle o Parkinson disease ear effusion o Peripheral neuropathy o Hypoglycemia o Syphilis o Herpes zoster oticus o Vestibular migraine o Labyrinthine concussion o Vestibular neuritis o Medication-induced -

Positive Perilymph Fistula Test with Semicircular Canal Dehiscence from Cholesteatoma
PRACTICE | CLINICAL IMAGES Positive perilymph fistula test with semicircular canal dehiscence from cholesteatoma Ming-Chih Hsieh MD, Chen Chi Wu MD PhD, Shih-Hao Wang MD n Cite as: CMAJ 2019 January 28;191:E104. doi: 10.1503/cmaj.180799 54-year-old man presented to our outpatient department with left-side hearing loss and tinnitus that had progressed for several years. The patient had vertigo with nausea, whichA was aggravated on applying pressure over the left external ear canal and tragus. Physical examination showed left-side tym- panic membrane retraction with a whitish mass at the epitympa- num, suggestive of cholesteatoma. Gently compressing the left-ear tragus induced apparently left-beating horizontal nystagmus (see video, Appendix 1, available at www.cmaj.ca/lookup/suppl/ doi:10.1503/cmaj.180799/-/DC1), consistent with a positive peri- lymph fistula test. Pure tone audiometry showed mixed-type hear- ing loss of 104 dB in the patient’s left ear and sensorineural hearing loss of 62 dB in his right. High-resolution computed tomography (CT) scan of the patient’s temporal bone showed a soft-tissue mass in his left middle ear and mastoid cavity with left lateral semicircular canal erosion (Appendix 2, available at www.cmaj.ca/lookup/suppl/ Figure 1: Microscopic view of left lateral semicircular canal dehiscence with doi:10.1503/cmaj.180799/-/DC1). These findings were compatible erosion of bony and membranous sections (arrows) in a 54-year-old man with with cholesteatoma with lateral semicircular canal dehiscence. cholesteatoma. Note: *the malleus handle; +second genu of the facial nerve; During surgery, we noted that the osseous and membranous por- dotted lines define the tympanic segment of the facial nerve. -

Radiology in Vertigo and Dizziness
10.5005/jp-journals-10003-1092 DeepakREVIEW Patkar ARTICLE et al Radiology in Vertigo and Dizziness Deepak Patkar, Girish Yevankar, Rashmi Parikh ABSTRACT • Cerebellopontine angle tumor Objective: Vertigo may or may not be associated with hearing • Cerebrovascular disease, such as transient ischemic loss. In addition, the imaging findings are often subtle. attack or stroke Underdiagnosis of cause of vertigo on imaging can lead to long • Migraine standing annoying symptom of vertigo. • Multiple sclerosis Conclusion: This article reviews the radiologic findings of • Other causes vertigo. After completing this article, the readers should have • Cervical vertigo an improved ability to diagnose the common causes of vertigo, • Drug-induced vertigo using the optimal imaging tools to achieve this goal. • Psychological Keywords: American College of Radiology, Magnetic The appropriate imaging modality depends upon the resonance imaging, Magnetic resonance angiogram. associated symptoms and is guided by ACR criterion as How to cite this article: Patkar D, Yevankar G, Parikh R. given in Table 1 (ACR Appropriateness Criteria)**.9 Radiology in Vertigo and Dizziness. Otorhinolaryngol Clin Int J 2012;4(2):86-92. Labyrinthitis Source of support: Nil Labyrinthitis is an inflammation of the membranous Conflict of interest: None declared labyrinth10 and can be divided according to etiology as follows: INTRODUCTION • Tympanogenic Imaging plays an important role in the diagnosis and • Post-traumatic treatment of the patients with vestibular abnormalities. • Meningogenic There are multiple imaging tools available for the • Hematogenic patients with vestibular and temporal bone abnormalities • Autoimmune viz computed tomography (CT) scan, magnetic resonance Prior to MRI, no imaging findings were described; imaging (MRI) including MR angiography and digital however, now enhancement of the labyrinth on postcontrast subtraction angiography. -

Surgical and Clinical Confirmation of Temporal Bone CT Findings In
ORIGINAL RESEARCH HEAD & NECK Surgical and Clinical Confirmation of Temporal Bone CT Findings in Patients with Otosclerosis with Failed Stapes Surgery J. Whetstone, A. Nguyen, A. Nguyen-Huynh, and B.E. Hamilton ABSTRACT BACKGROUND AND PURPOSE: Prior descriptions of imaging after failed stapes procedures for otosclerosis predated currently available CT technology and/or failed to assess commonly used metallic implants. The purpose of this study was to correlate temporal bone CT findings with clinically and intraoperatively determined causes of surgical failure. MATERIALS AND METHODS: All patients with otosclerosis undergoing stapedectomy between December 1999 and December 2010 were identified from a search of neurotology clinical records. Patients presenting because of failed stapes surgery and having temporal bone CT scans at the time of revision surgery or clinical evaluation were included. Imaging and clinical records were retrospectively evaluated by a medical student, radiology resident, and senior neuroradiologist. Stapes prosthesis complications and relevant anatomic CT findings were correlated to clinical and intraoperative findings. RESULTS: Twenty-two of 340 patients met inclusion criteria. Temporal bone CT findings were correlated to intraoperative findings in 17 of 22 patients and to clinical findings in 5 of 22 patients. Surgically confirmed abnormalities included 7 of 7 incus erosions, 3 of 6 piston re-sizings, 3 of 5 granulation tissues, 3 of 5 prosthesis disconnections, 3 of 4 obliterative otosclerosis, 2 of 2 oval window dislocations, and 1 labyrinthine ossificans. Clinically confirmed abnormalities included 2 cases each of superior semicircular canal dehiscence, and wrong piston size, and 1 each of piston disconnection, labyrinthine ossificans, and intravestibular footplate. CONCLUSIONS: CT evaluation in the setting of failed stapes surgery is challenging. -

Factors Potentially Affecting the Hearing of Petroleum Industry Workers
report no. 5/05 factors potentially affecting the hearing of petroleum industry workers Prepared for CONCAWE’s Health Management Group by: P. Hoet M. Grosjean Unité de toxicologie industrielle et pathologie professionnelle Ecole de santé publique Faculté de médecine Université catholique de Louvain (Belgium) C. Somaruga School of Occupational Health University of Milan (Italy) Reproduction permitted with due acknowledgement © CONCAWE Brussels June 2005 I report no. 5/05 ABSTRACT This report aims at giving an overview of the various factors that may influence the hearing of petroleum industry workers, including the issue of ‘ototoxic’ chemical exposure. It also provides guidance for occupational physicians on factors that need to be considered as part of health management programmes. KEYWORDS hearing, petroleum industry, hearing loss, audiometry, ototoxicity, chemicals INTERNET This report is available as an Adobe pdf file on the CONCAWE website (www.concawe.org). NOTE Considerable efforts have been made to assure the accuracy and reliability of the information contained in this publication. However, neither CONCAWE nor any company participating in CONCAWE can accept liability for any loss, damage or injury whatsoever resulting from the use of this information. This report does not necessarily represent the views of any company participating in CONCAWE. II report no. 5/05 CONTENTS Page SUMMARY IV 1. INTRODUCTION 1 2. HEARING, MECHANISMS AND TYPES OF HEARING LOSS 3 2.1. PHYSIOLOGY OF HEARING: HEARING BASICS 3 2.2. MECHANISMS AND TYPES OF HEARING LOSS 4 2.2.1. Transmission or conduction hearing loss 4 2.2.2. Sensorineural hearing loss 5 2.3. EVALUATION OF HEARING LOSS 6 3. -

Vertigo Workshop Mike Valdez, PA-C Updated 2/9/2015 Vertigo Workshop
March 19, 2015 Newport Beach, CA Vertigo Workshop Mike Valdez, PA-C Updated 2/9/2015 Vertigo Workshop Clear Live Hands-On Instruction Demonstration Practice Learn by doing Vertigo examination Neurological examination Rhomberg Test Fukada Stepping Test Demonstration ENG/VNG Canalith Repositioning Introduction There are multiple methods and techniques available to successfully complete all the topics presented in this workshop. Some are based on patient request, available equipment or supervising physician’s preference. The goal of this workshop is to correctly demonstrate the most common methods and give participants time for hands on training. Vertigo Workshop Learning Objectives • Discuss and demonstrate vertigo examination; – Neurological examination – Rhomberg Test – Fukada Stepping Test – Dix-Hallpike • Demonstrate ENG/VNG. • Demonstrate and practice canalith repositioning Balance Mercado 2013© Clinical Evaluation of Vertiginous Patient Central Peripheral Vascular disorders Labrynthitis (Vertibrobasilar Insufficiency) Vestibular Neuronitis (Vascular Loop Syndrome) BPPV Multiple Sclerosis Perilymphatic Fistula CNS Neoplasm (tumor) Meniere’s Disease Cardio (orthostatic hypotension) Autoimmune Cerebrovascular (CVA/TIA) Ataxia Migraine Systemic Medication Neurology/Cardiology Endocrine Otolaryngology Disequilibrium Mercado 2013© Algorithm History Physical Exam CN II-XII Peripheral Romberg Central Fukuda Dix-Hallpike IMAGING Hearing Test CT/MRI/MRA Audio/Tymps Carotid U/S ABR/OAE Diagnostic Tests Balance Test LABS ENG/VNG Mercado 2013©