NONMALIGNANT LEUKOCYTE DISORDERS Dr.Ghorbani
Total Page:16
File Type:pdf, Size:1020Kb

Load more
Recommended publications
-

My Beloved Neutrophil Dr Boxer 2014 Neutropenia Family Conference
The Beloved Neutrophil: Its Function in Health and Disease Stem Cell Multipotent Progenitor Myeloid Lymphoid CMP IL-3, SCF, GM-CSF CLP Committed Progenitor MEP GMP GM-CSF, IL-3, SCF EPO TPO G-CSF M-CSF IL-5 IL-3 SCF RBC Platelet Neutrophil Monocyte/ Basophil B-cells Macrophage Eosinophil T-Cells Mast cell NK cells Mature Cell Dendritic cells PRODUCTION AND KINETICS OF NEUTROPHILS CELLS % CELLS TIME Bone Marrow: Myeloblast 1 7 - 9 Mitotic Promyelocyte 4 Days Myelocyte 16 Maturation/ Metamyelocyte 22 3 – 7 Storage Band 30 Days Seg 21 Vascular: Peripheral Blood Seg 2 6 – 12 hours 3 Marginating Pool Apoptosis and ? Tissue clearance by 0 – 3 macrophages days PHAGOCYTOSIS 1. Mobilization 2. Chemotaxis 3. Recognition (Opsonization) 4. Ingestion 5. Degranulation 6. Peroxidation 7. Killing and Digestion 8. Net formation Adhesion: β 2 Integrins ▪ Heterodimer of a and b chain ▪ Tight adhesion, migration, ingestion, co- stimulation of other PMN responses LFA-1 Mac-1 (CR3) p150,95 a2b2 a CD11a CD11b CD11c CD11d b CD18 CD18 CD18 CD18 Cells All PMN, Dendritic Mac, mono, leukocytes mono/mac, PMN, T cell LGL Ligands ICAMs ICAM-1 C3bi, ICAM-3, C3bi other other Fibrinogen other GRANULOCYTE CHEMOATTRACTANTS Chemoattractants Source Activators Lipids PAF Neutrophils C5a, LPS, FMLP Endothelium LTB4 Neutrophils FMLP, C5a, LPS Chemokines (a) IL-8 Monocytes, endothelium LPS, IL-1, TNF, IL-3 other cells Gro a, b, g Monocytes, endothelium IL-1, TNF other cells NAP-2 Activated platelets Platelet activation Others FMLP Bacteria C5a Activation of complement Other Important Receptors on PMNs ñ Pattern recognition receptors – Detect microbes - Toll receptor family - Mannose receptor - bGlucan receptor – fungal cell walls ñ Cytokine receptors – enhance PMN function - G-CSF, GM-CSF - TNF Receptor ñ Opsonin receptors – trigger phagocytosis - FcgRI, II, III - Complement receptors – ñ Mac1/CR3 (CD11b/CD18) – C3bi ñ CR-1 – C3b, C4b, C3bi, C1q, Mannose binding protein From JG Hirsch, J Exp Med 116:827, 1962, with permission. -
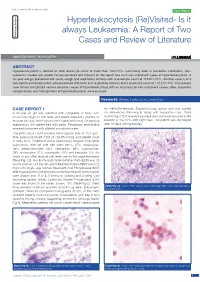
Hyperleukocytosis (Re)Visited- Is It Case Series Always Leukaemia: a Report of Two Pathology Section Cases and Review of Literature Short Communication
Review Article Clinician’s corner Original Article Images in Medicine Experimental Research Miscellaneous Letter to Editor DOI: 10.7860/JCDR/2020/40556.13409 Case Report Postgraduate Education Hyperleukocytosis (Re)Visited- Is it Case Series always Leukaemia: A Report of Two Pathology Section Cases and Review of Literature Short Communication ASHUTOSH RATH1, RICHA GUPTA2 ABSTRACT Hyperleukocytosis is defined as total leukocyte count of more than 100×109/L. Commonly seen in leukaemic conditions, non- leukaemic causes are usually not encountered and thought of. We report two such non-malignant cases of hyperleukocytosis. A six-year old girl presented with fever, cough and respiratory distress with a leukocyte count of 125.97×109/L. Another case is of a two-month old female infant, who presented with fever and respiratory distress and a leukocyte count of 112.27×109/L. The present case thrives to highlight various possible causes of hyperleukocytosis with an emphasis on non-malignant causes. Also, important complications and management of hyperleukocytosis are discussed. Keywords: Benign, Leukocytosis, Leukostasis CASE REPORT 1 for methicillin-resistant Staphylococcus aureus and was started A six-year-old girl was admitted with complaints of fever, non- on intravenous Vancomycin along with supportive care. Serial productive cough for one week and severe respiratory distress for monitoring of TLC revealed a gradual reduction and it returned to the the past one day. There was no other significant history. On physical baseline of 15×109/L after eight days. The patient was discharged examination, the patient had mild pallor. Respiratory examination after 10 days of hospital stay. -

Practice Parameter for the Diagnosis and Management of Primary Immunodeficiency
Practice parameter Practice parameter for the diagnosis and management of primary immunodeficiency Francisco A. Bonilla, MD, PhD, David A. Khan, MD, Zuhair K. Ballas, MD, Javier Chinen, MD, PhD, Michael M. Frank, MD, Joyce T. Hsu, MD, Michael Keller, MD, Lisa J. Kobrynski, MD, Hirsh D. Komarow, MD, Bruce Mazer, MD, Robert P. Nelson, Jr, MD, Jordan S. Orange, MD, PhD, John M. Routes, MD, William T. Shearer, MD, PhD, Ricardo U. Sorensen, MD, James W. Verbsky, MD, PhD, David I. Bernstein, MD, Joann Blessing-Moore, MD, David Lang, MD, Richard A. Nicklas, MD, John Oppenheimer, MD, Jay M. Portnoy, MD, Christopher R. Randolph, MD, Diane Schuller, MD, Sheldon L. Spector, MD, Stephen Tilles, MD, Dana Wallace, MD Chief Editor: Francisco A. Bonilla, MD, PhD Co-Editor: David A. Khan, MD Members of the Joint Task Force on Practice Parameters: David I. Bernstein, MD, Joann Blessing-Moore, MD, David Khan, MD, David Lang, MD, Richard A. Nicklas, MD, John Oppenheimer, MD, Jay M. Portnoy, MD, Christopher R. Randolph, MD, Diane Schuller, MD, Sheldon L. Spector, MD, Stephen Tilles, MD, Dana Wallace, MD Primary Immunodeficiency Workgroup: Chairman: Francisco A. Bonilla, MD, PhD Members: Zuhair K. Ballas, MD, Javier Chinen, MD, PhD, Michael M. Frank, MD, Joyce T. Hsu, MD, Michael Keller, MD, Lisa J. Kobrynski, MD, Hirsh D. Komarow, MD, Bruce Mazer, MD, Robert P. Nelson, Jr, MD, Jordan S. Orange, MD, PhD, John M. Routes, MD, William T. Shearer, MD, PhD, Ricardo U. Sorensen, MD, James W. Verbsky, MD, PhD GlaxoSmithKline, Merck, and Aerocrine; has received payment for lectures from Genentech/ These parameters were developed by the Joint Task Force on Practice Parameters, representing Novartis, GlaxoSmithKline, and Merck; and has received research support from Genentech/ the American Academy of Allergy, Asthma & Immunology; the American College of Novartis and Merck. -

Primary Immunodeficiency Disorders
ALLERGY AND IMMUNOLOGY 00954543 /98 $8.00 + .OO PRIMARY IMMUNODEFICIENCY DISORDERS Robert J. Mamlok, MD Immunodeficiency is a common thought among both patients and physicians when confronted with what is perceived as an excessive num- ber, duration, or severity of infections. Because of this, the starting point for evaluating patients for suspected immunodeficiency is based on what constitutes ”too many infections.” It generally is agreed that children with normal immune systems may have an average of 6 to 8 respiratory tract infections per year for the first decade of life. Even after a pattern of ab- normal infection is established, questions of secondary immunodeficiency should first be raised. The relatively uncommon primary immunodefi- ciency diseases are statistically dwarfed by secondary causes of recurrent infection, such as malnutrition, respiratory allergy, chronic cardiovascular, pulmonary, and renal disease, and environmental factors. On the other hand, a dizzying spiral of progress in our understanding of the genetics and immunology of primary immunodeficiency disease has resulted in improved diagnostic and therapeutic tools. Twenty-five newly recognized immunologic disease genes have been cloned in the last 5 ~ears.2~It has become arguably more important than ever for us to recognize the clinical and laboratory features of these relatively uncommon, but increasingly treatable, disorders. CLASSIFICATION The immune system has been classically divided into four separate arms: The B-cell system responsible for antibody formation, the T-cell sys- From the Division of Pediatric Allergy and Immunology, Texas Tech University Health Sci- ences Center, Lubbock, Texas PRIMARY CARE VOLUME 25 NUMBER 4 DECEMBER 1998 739 740 MAMLOK tem responsible for immune cellular regulation, the phagocytic (poly- morphonuclear and mononuclear) system and the complement (opsonic) system. -

Reptile Clinical Pathology Vickie Joseph, DVM, DABVP (Avian)
Reptile Clinical Pathology Vickie Joseph, DVM, DABVP (Avian) Session #121 Affiliation: From the Bird & Pet Clinic of Roseville, 3985 Foothills Blvd. Roseville, CA 95747, USA and IDEXX Laboratories, 2825 KOVR Drive, West Sacramento, CA 95605, USA. Abstract: Hematology and chemistry values of the reptile may be influenced by extrinsic and intrinsic factors. Proper processing of the blood sample is imperative to preserve cell morphology and limit sample artifacts. Identifying the abnormal changes in the hemogram and biochemistries associated with anemia, hemoparasites, septicemias and neoplastic disorders will aid in the prognostic and therapeutic decisions. Introduction Evaluating the reptile hemogram is challenging. Extrinsic factors (season, temperature, habitat, diet, disease, stress, venipuncture site) and intrinsic factors (species, gender, age, physiologic status) will affect the hemogram numbers, distribution of the leukocytes and the reptile’s response to disease. Certain procedures should be ad- hered to when drawing and processing the blood sample to preserve cell morphology and limit sample artifact. The goal of this paper is to briefly review reptile red blood cell and white blood cell identification, normal cell morphology and terminology. A detailed explanation of abnormal changes seen in the hemogram and biochem- istries in response to anemia, hemoparasites, septicemias and neoplasia will be addressed. Hematology and Chemistries Blood collection and preparation Although it is not the scope of this paper to address sites of blood collection and sample preparation, a few im- portant points need to be explained. For best results to preserve cell morphology and decrease sample artifacts, hematologic testing should be performed as soon as possible following blood collection. -

Fracp Lecture 2010 Immune Deficiency 3
FRACP LECTURE 2010 IMMUNE DEFICIENCY 3 DR MARNIE ROBINSON PAEDIATRIC IMMUNOLOGIST/ALLERGIST IMMUNOLOGY LECTURE 3 • Neutrophil defects • INTERFERON –Y /IL‐12 pathway defect • Dysregulatory immune dfiideficienc ies NEUTROPHIL DEFECTS • Neutropaenia – Allo immune /au to immune – Kostmann, WHIM – cyclllical • Chronic granulomatous disease • Leukocyte adhesion deficiency • Neutrophil specific granule deficiency • Chediak –higashi syndrome AUTOIMMUNE NEUTROPAENIA • Antibodies against different neutrophil antigen • Aeitiology unknown • Slightly more common in females • Present with skin and upper respiratory tract infections (pneumonia /menin gitis /se psis less common) • Neutrophil count usually <0. 5 but may increase during infection • Treatment with G‐CSF (IVIG) • Usually remits spontaneously by <24 months ALLOIMMUNE NEUTROPAENIA • Caused by transplacental transfer of maternal against the FcyRIIIb isotypes of NA 1 and NA2 causing immune destruction of neutrophils • Incidence of 1/500 • Usually presents in first weeks of life • Present with omphalitis, cellulitis, pneumonia • Diagnosed by detection of neutrophil specific alloantibodies in maternal blood • Treat with G‐CSF • resolves with waning of maternal antibodies KOSTMANN’S SYNDROME • Bone marrow granulocyte arrest at promyeolocyte or myelocyte stage • Present early in life (usually <6 months) • Present with omphalitis , respiratory tract ifinfect ions, skin and liver abscesses • Increased susceptibility to AML • Treatment is with G‐CSF CYCLICAL NEUTROPAENIA • Defect in elastase 2 • Sporadic -

The Significance of Various Granulocytic Inclusions
4/8/19 THE SIGNIFICANCE OF VARIOUS DISCLOSURES GRANULOCYTIC INCLUSIONS ¡ No relevant financial interests to disclose. KRISTLE HABERICHTER, DO, FCAP GRAND TRAVERSE PATHOLOGY, PLLC OBJECTIVES GRANULOCYTES ¡ Innate immune system ¡ Travel to sites of infection, recognize and phagocytose pathogens ¡ Recognize common and uncommon granulocytic inclusions, including those associated with certain ¡ Utilize numerous cytotoxic mechanisms to kill pathogens inherited disorders and infectious etiologies ¡ Granulopoiesis occurs in the bone marrow ¡ Sufficient stem cells, adequate microenvironment, and regulatory factors ¡ Identify newly described green neutrophilic inclusions ¡ Granulocyte colony stimulating factor (G-CSF) → Granulocytes ¡ Monocyte colony stimulating factor (M-CSF) → Monocytes ¡ Understand the clinical significance and implications of various inclusions ¡ Granulocyte-monocytes colony stimulating factor (GM-CSF) → Granulocytes & Monocytes ¡ 1-3 weeks for complete granulopoiesis to occur ¡ Neutrophils only circulate for a few hours before migrating to the tissues Photo by K. Haberichter (Giemsa, 1000x) GRANULOCYTES INCLUSION CATEGORIES ¡ Primary granules → Myeloperoxidase Reactive/Acquired Changes Congenital Abnormalities Infectious Etiologies ¡ “Late” myeloblasts and promyelocytes ¡ To x ic G r a n u la t io n ¡ Chédiak-Higashi Syndrome ¡ Anaplasma ¡ Secondary granules → Leukocyte alkaline phosphatase ¡ Döhle Bodies ¡ Alder-Reilly Anomaly ¡ Ehrlichia ¡ Myelocytes, metamyelocytes, band and segmented neutrophils ¡ Cytokine Effect ¡ May-Hegglin -

Blood and Immunity
Chapter Ten BLOOD AND IMMUNITY Chapter Contents 10 Pretest Clinical Aspects of Immunity Blood Chapter Review Immunity Case Studies Word Parts Pertaining to Blood and Immunity Crossword Puzzle Clinical Aspects of Blood Objectives After study of this chapter you should be able to: 1. Describe the composition of the blood plasma. 7. Identify and use roots pertaining to blood 2. Describe and give the functions of the three types of chemistry. blood cells. 8. List and describe the major disorders of the blood. 3. Label pictures of the blood cells. 9. List and describe the major disorders of the 4. Explain the basis of blood types. immune system. 5. Define immunity and list the possible sources of 10. Describe the major tests used to study blood. immunity. 11. Interpret abbreviations used in blood studies. 6. Identify and use roots and suffixes pertaining to the 12. Analyse several case studies involving the blood. blood and immunity. Pretest 1. The scientific name for red blood cells 5. Substances produced by immune cells that is . counteract microorganisms and other foreign 2. The scientific name for white blood cells materials are called . is . 6. A deficiency of hemoglobin results in the disorder 3. Platelets, or thrombocytes, are involved in called . 7. A neoplasm involving overgrowth of white blood 4. The white blood cells active in adaptive immunity cells is called . are the . 225 226 ♦ PART THREE / Body Systems Other 1% Proteins 8% Plasma 55% Water 91% Whole blood Leukocytes and platelets Formed 0.9% elements 45% Erythrocytes 10 99.1% Figure 10-1 Composition of whole blood. -

BHS Leucocytosis and Leucopenia Dr Caers
Leucocytoses & leucopenia Jo Caers Dept of Clinical Hematology [email protected] Bone marrow Blood Granulopoiesis Proliferation & 5 days maturation Storage 1 day Marginisation& Circulation 1 day Tissues 1-2 days Granulopoiesis Proliferation & 5 days maturation Storage 1 day Marginisation& Circulation 1 day Tissues 1-2 days Granulopoiesis Proliferation & 5 days maturation Storage 1 day Marginisation& Circulation 1 day Tissues 1-2 days Lymphocytes Monocytes NORMAL BLOOD CELL COUNT Hemoglobin 12.0 – 15.0 g/dl (F) 13.0 – 17.0 g/dl (M) Red Blood Cells 3.9 – 5.6 x 10 6/µl (F) 4.5 – 6.5 x 10 6/µl (M) Hematocrit 36 – 48% (F) 40 – 52% (M) Mean Corpuscular Volume 80 – 95µ³ Mean Hb Concentration 27 – 34 pg Conc corp mean Hb 30 – 35 g/dl Reticulocytes 0.5 – 20 % Leucocytes 4.0 – 10.0 x 10 3/µl ¨ Neutophils 1.8 – 7.5 Lymphocytes 1.5 – 3.5 Monocytes 0.2 – 0.8 Eosinophils 0.04 – 0.45 Basophils 0.01 – 0.1 Platelets 100 – 400 x 10 3/dl Hyperleucocytosis > 10.000 WBC/mm³ Normal Cells Abnormal cells or blastic cells Infections ? Neutrophilia (> 7.500/mm³) Acute Leukemias Lymphocytosis (> 4.500/mm³) Chronic Myelomonocytic Leukemias Chronic Lymhocytic leukemia Chronic Myeloid Leukemia Non Hodgkin Lymphoma Chronic Monocytosis (> 800/mm³) … Inflammations? Eosinophilia (> 400/mm³) Basophilia (> 100/mm³) Leukoerythroblastic reaction Cytopenia with immature RBCs (normoblasts) immature WBCs (agranular neutrophils, myelocytes, metamyelocytes ) Causes BM infiltration • Solid tumor or hematological malignancy • Myelofibrosis Strong BM stimulation • Infection, -

Persistent Eosinophilia Is a Challenging Problem
DOI: 10.26717/BJSTR.2017.01.000244 Nahla A M Hamed. Biomed J Sci & Tech Res ISSN: 2574-1241 Editorial Open Access Persistent Eosinophilia is a Challenging Problem Nahla AM Hamed* Professor of Hematology, Faculty of Medicine, Alexandria University, Egypt Received: July 25, 2017; Published: August 01, 2017 *Corresponding author: Nahla AM Hamed, Professor of Hematology, Faculty of Medicine, Alexandria University, Egypt Abstract 9 HE is defined as >1.5 x 10 /L eosinophils in the blood on 2 examinations (interval >1 mo) and/or tissue HE defined by: eosinophils percentage in BM section exceeding 20% of all nucleated cells; and/or extensive eosinophilic tissue infiltration by pathologist opinion; and/or presenceAbbreviations: of marked deposition of eosinophil granule proteins (in the absence or presence of major tissue eosinophils infiltration). AEC: absolute eosinophil count; HE: Hypereosinophilia; ABPA: Allergic Bronchopulmonary Aspergillosis; B-ALL: Acute B-cell lymphoblastic leukemia; GVHD: Graft-Versus-Host Disease; BM: Bone Marrow; PB: Peripheral Blood; IL5: Interleukin 5; AML: Acute Myeloid Leukemia; LV: Lymphocytic Variant; Th2:T-cells have a helper type 2; EPPER: Eosinophilic, polymorphic, and pruritic Eruption Associated with Radiotherapy; MPN: Myeloproliferative Neoplasm; HES: Hypereosinophilic Syndrome; PDGFRA: Platelet-Derived Growth Factor Receptor Alpha; PDGFRB: Platelet-Derived Growth Factor Receptor Beta; FGFR1: Fibroblast Growth Factor Receptor 1; CEL-NOS: Chronic Eosinophilic Leukemia-Not Otherwise Specified; MDS: Myelodysplastic Syndrome; IgH: Ig Heavy Chain; EBV: Epstein-Barr virus Introduction cystic structures (e.g. hydatid cyst, neurocysticercosis) are unlikely Eosinophilia3 is defined as an AEC >500/μL [1].3 The severity ), and severe to cause eosinophilia [7]. Disseminated coccidioidomycosis and of eosinophilia has3 been arbitrarily divided into mild9 (AEC: 500- aspergillosis (when presenting as ABPA) are well-known fungal 1,500/mm ), moderate (AEC: 1,500-5,000/mm causes of eosinophilia. -

Canine Granulocytopathy Syndrome an Inherited Disorder Ofleukocyte Function
Canine Granulocytopathy Syndrome An Inherited Disorder ofLeukocyte Function Harland W. Renshaw, DVM, PhD, and William C. Davis, PhD A disease closely resembling the human neutrophil dysfunction syndromes has been identified in a colony of dogs. The syndrome, referred to as the canine gran- ulocytopathy syndrome, is characterized by recurrent life-threatening bacterial infec- tions and a greatly shortened life span. The disease is genetically determined, being transmitted as an autosomal recessive trait. The increased susceptibility to pyogenic infections and shortened life span is related to an impairment of leukocvte function at the cellular level. Preparations of neutrophils from affected animals exhibit impaired in ritro killing of Escherichia coli. The defect in bactericidal activity is associated with reduced glucose oxidation by the hexose monophosphate shunt and an increased capac- ity to reduce nitroblue tetrazolium dye. The data obtained thus far indicate the canine granulocytopathy syndrome will be of considerable value as a model for the study of granulocytopathy syndromes in man. (Am J Pathol 95:731-744, 1979) STUDIES OF LEUKOCY-TE structure and function in host defense failure syndromes of man and animals have provided dramatic evidence for the necessitv of adequate neutrophil function for normal host resis- tance.`6 A group of human diseases, characterized clinically bv enhanced susceptibilitv to pyogenic infections, has been related to impaired killing of microorganisms by neutrophils and monocytes.7-12 A direct correlation -

Eosinophilia and Neutrophilia Associated with Antipd-1 Use In
ISSN: 2688-8203 DOI: 10.33552/ACRCI.2021.03.000555 Advances in Cancer Research & Clinical Imaging Case Report Copyright © All rights are reserved by Yasir Khan Eosinophilia and Neutrophilia Associated with Anti- PD-1 use in Metastatic Non-Small Cell Lung Cancer – A Case Report Yasir Khan* and Christopher Lomma Department of Medical Oncology, Fiona Stanley Hospital, Western Australia, Australia *Corresponding author: Yasir Khan, Department of Medical Oncology, Fiona Stanley Received Date: January 23, 2021 Hospital, Australia. Published Date: January 29, 2021 Abstract The use of immunotherapy has dramatically changed the way many cancers are treated with several studies having looked at the relationship between eosinophils and immunotherapy. This case study reports nivolumab induced eosinophilia and neutrophilia with no other systemic adverse effects in a patient with metastatic non-small cell lung cancer. A 61-year-old woman with Eastern Cooperative Oncology Group performance status 1 was diagnosed with metastatic non-small cell lung cancer without any driver mutations and was commenced on nivolumab after progressing on platinum doublet therapy. She had mild eosinophilia and neutrophilia at baseline in the context of a lower respiratory tract infection which peak levels at week-35. She developed postural hypotension during the course of her disease and prednisolone was commenced to treat possible became more pronounced with the introduction of nivolumab. Nivolumab was ceased at week-26 due to significant eosinophilia and reached for 8 months after commencement of immunotherapy before progression of disease leading to clinical deterioration and death. Asymptomatic adrenal insufficiency from metastasis. The introduction of steroids led to the improvement in eosinophilia and neutrophilia.