Diagnosis and Management of Immunodeficiencies in Adults By
Total Page:16
File Type:pdf, Size:1020Kb
Load more
Recommended publications
-

IDF Patient & Family Handbook
Immune Deficiency Foundation Patient & Family Handbook for Primary Immunodeficiency Diseases This book contains general medical information which cannot be applied safely to any individual case. Medical knowledge and practice can change rapidly. Therefore, this book should not be used as a substitute for professional medical advice. FIFTH EDITION COPYRIGHT 1987, 1993, 2001, 2007, 2013 IMMUNE DEFICIENCY FOUNDATION Copyright 2013 by Immune Deficiency Foundation, USA. REPRINT 2015 Readers may redistribute this article to other individuals for non-commercial use, provided that the text, html codes, and this notice remain intact and unaltered in any way. The Immune Deficiency Foundation Patient & Family Handbook may not be resold, reprinted or redistributed for compensation of any kind without prior written permission from the Immune Deficiency Foundation. If you have any questions about permission, please contact: Immune Deficiency Foundation, 110 West Road, Suite 300, Towson, MD 21204, USA; or by telephone at 800-296-4433. Immune Deficiency Foundation Patient & Family Handbook for Primary Immunodeficency Diseases 5th Edition This publication has been made possible through a generous grant from Baxalta Incorporated Immune Deficiency Foundation 110 West Road, Suite 300 Towson, MD 21204 800-296-4433 www.primaryimmune.org [email protected] EDITORS R. Michael Blaese, MD, Executive Editor Francisco A. Bonilla, MD, PhD Immune Deficiency Foundation Boston Children’s Hospital Towson, MD Boston, MA E. Richard Stiehm, MD M. Elizabeth Younger, CPNP, PhD University of California Los Angeles Johns Hopkins Los Angeles, CA Baltimore, MD CONTRIBUTORS Mark Ballow, MD Joseph Bellanti, MD R. Michael Blaese, MD William Blouin, MSN, ARNP, CPNP State University of New York Georgetown University Hospital Immune Deficiency Foundation Miami Children’s Hospital Buffalo, NY Washington, DC Towson, MD Miami, FL Francisco A. -

The Pathophysiology of Paroxysmal Nocturnal Haemoglobinuria.Pdf
The Pathophysiology of Paroxysmal Nocturnal Haemoglobinuria Richard John Kelly Submitted in accordance with the requirements for the degree of Doctor of Philosophy The University of Leeds School of Medicine January 2014 1 Jointly-Authored Publications The candidate confirms that the work submitted is his own, except where work which has formed part of jointly authored publications has been included. The contribution of the candidate and the other authors to this work has been explicitly indicated below. The candidate confirms that appropriate credit has been given within the thesis where reference has been made to the work of others. The work in Chapter 3 of the thesis has appeared in publication as follows: Kelly RJ, Hill A, Arnold LM, Brooksbank GL, Richards SJ, Cullen M, Mitchell LD, Cohen DR, Gregory WM, Hillmen P. Long-term treatment with eculizumab in paroxysmal nocturnal hemoglobinuria: sustained efficacy and improved survival. Blood 2011;117:6786-6792. I was responsible for designing the study, collecting and analysing the data and writing the paper. Dena Cohen and Walter Gregory performed the statistical analysis. All the other authors reviewed the paper. The work in Chapter 4 of the thesis has appeared in publication as follows: Kelly R, Arnold L, Richards S, Hill A, Bomken C, Hanley J, Loughney A, Beauchamp J, Khursigara G, Rother RP, Chalmers E, Fyfe A, Fitzsimons E, Nakamura R, Gaya A, Risitano AM, Schubert J, Norfolk D, Simpson N, Hillmen P. The management of pregnancy in paroxysmal nocturnal haemoglobinuria on long term eculizumab. Br J Haematol 2010;149:446-450. I was responsible for designing the study, collecting and analysing the data and writing the paper. -

IDF Guide to Hematopoietic Stem Cell Transplantation
Guide to Hematopoietic Stem Cell Transplantation Immune Deficiency Foundation Guide to Hematopoietic Stem Cell Transplantation This publication contains general medical information that cannot be applied safely to any individual case. Medical knowledge and practice can change rapidly. Therefore, this publication should not be used as a substitute for professional medical advice. In all cases, patients and caregivers should consult their healthcare providers. Each patient’s condition and treatment are unique. Copyright 2018 by Immune Deficiency Foundation, USA Readers may redistribute this guide to other individuals for non-commercial use, provided that the text, html codes, and this notice remain intact and unaltered in any way. Immune Deficiency Foundation Guide to Hematopoietic Stem Cell Transplantation may not be resold, reprinted or redistributed for compensation of any kind without prior written permission from the Immune Deficiency Foundation (IDF). If you have any questions about permission, please contact: Immune Deficiency Foundation, 110 West Road, Suite 300, Towson, MD 21204, USA, or by telephone: 800-296-4433. For more information about IDF, go to: www.primaryimmune.org. This publication has been made possible through the IDF SCID Initiative and the SCID, Angels for Life Foundation. Acknowledgements The Immune Deficiency Foundation would like to thank the organizations and individuals who helped make this publication possible and contributed to the development of the Immune Deficiency Foundation Guide to Hematopoietic Stem -

My Beloved Neutrophil Dr Boxer 2014 Neutropenia Family Conference
The Beloved Neutrophil: Its Function in Health and Disease Stem Cell Multipotent Progenitor Myeloid Lymphoid CMP IL-3, SCF, GM-CSF CLP Committed Progenitor MEP GMP GM-CSF, IL-3, SCF EPO TPO G-CSF M-CSF IL-5 IL-3 SCF RBC Platelet Neutrophil Monocyte/ Basophil B-cells Macrophage Eosinophil T-Cells Mast cell NK cells Mature Cell Dendritic cells PRODUCTION AND KINETICS OF NEUTROPHILS CELLS % CELLS TIME Bone Marrow: Myeloblast 1 7 - 9 Mitotic Promyelocyte 4 Days Myelocyte 16 Maturation/ Metamyelocyte 22 3 – 7 Storage Band 30 Days Seg 21 Vascular: Peripheral Blood Seg 2 6 – 12 hours 3 Marginating Pool Apoptosis and ? Tissue clearance by 0 – 3 macrophages days PHAGOCYTOSIS 1. Mobilization 2. Chemotaxis 3. Recognition (Opsonization) 4. Ingestion 5. Degranulation 6. Peroxidation 7. Killing and Digestion 8. Net formation Adhesion: β 2 Integrins ▪ Heterodimer of a and b chain ▪ Tight adhesion, migration, ingestion, co- stimulation of other PMN responses LFA-1 Mac-1 (CR3) p150,95 a2b2 a CD11a CD11b CD11c CD11d b CD18 CD18 CD18 CD18 Cells All PMN, Dendritic Mac, mono, leukocytes mono/mac, PMN, T cell LGL Ligands ICAMs ICAM-1 C3bi, ICAM-3, C3bi other other Fibrinogen other GRANULOCYTE CHEMOATTRACTANTS Chemoattractants Source Activators Lipids PAF Neutrophils C5a, LPS, FMLP Endothelium LTB4 Neutrophils FMLP, C5a, LPS Chemokines (a) IL-8 Monocytes, endothelium LPS, IL-1, TNF, IL-3 other cells Gro a, b, g Monocytes, endothelium IL-1, TNF other cells NAP-2 Activated platelets Platelet activation Others FMLP Bacteria C5a Activation of complement Other Important Receptors on PMNs ñ Pattern recognition receptors – Detect microbes - Toll receptor family - Mannose receptor - bGlucan receptor – fungal cell walls ñ Cytokine receptors – enhance PMN function - G-CSF, GM-CSF - TNF Receptor ñ Opsonin receptors – trigger phagocytosis - FcgRI, II, III - Complement receptors – ñ Mac1/CR3 (CD11b/CD18) – C3bi ñ CR-1 – C3b, C4b, C3bi, C1q, Mannose binding protein From JG Hirsch, J Exp Med 116:827, 1962, with permission. -

Comprehensive Genetic Testing for Primary Immunodeficiency
Woon and Ameratunga Allergy Asthma Clin Immunol (2016) 12:65 Allergy, Asthma & Clinical Immunology DOI 10.1186/s13223-016-0169-2 RESEARCH Open Access Comprehensive genetic testing for primary immunodeficiency disorders in a tertiary hospital: 10‑year experience in Auckland, New Zealand See‑Tarn Woon and Rohan Ameratunga* Abstract Background and purpose: New Zealand is a developed geographically isolated country in the South Pacific with a population of 4.4 million. Genetic diagnosis is the standard of care for most patients with primary immunodeficiency disorders (PIDs). Methods: Since 2005, we have offered a comprehensive genetic testing service for PIDs and other immune-related disorders with a published sequence. Here we present results for this program, over the first decade, between 2005 and 2014. Results: We undertook testing in 228 index cases and 32 carriers during this time. The three most common test requests were for X-linked lymphoproliferative (XLP), tumour necrosis factor receptor associated periodic syndrome (TRAPS) and haemophagocytic lymphohistiocytosis (HLH). Of the 32 suspected XLP cases, positive diagnoses were established in only 2 patients. In contrast, genetic defects in 8 of 11 patients with suspected X-linked agammaglobu‑ linemia (XLA) were confirmed. Most XLA patients were initially identified from absence of B cells. Overall, positive diagnoses were made in about 23% of all tests requested. The diagnostic rate was lowest for several conditions with locus heterogeneity. Conclusions: Thorough clinical characterisation of patients can assist in prioritising which genes should be tested. The clinician-driven customised comprehensive genetic service has worked effectively for New Zealand. Next genera‑ tion sequencing will play an increasing role in disorders with locus heterogeneity. -

Are Complement Deficiencies Really Rare?
G Model MIMM-4432; No. of Pages 8 ARTICLE IN PRESS Molecular Immunology xxx (2014) xxx–xxx Contents lists available at ScienceDirect Molecular Immunology j ournal homepage: www.elsevier.com/locate/molimm Review Are complement deficiencies really rare? Overview on prevalence, ଝ clinical importance and modern diagnostic approach a,∗ b Anete Sevciovic Grumach , Michael Kirschfink a Faculty of Medicine ABC, Santo Andre, SP, Brazil b Institute of Immunology, University of Heidelberg, Heidelberg, Germany a r a t b i c s t l e i n f o r a c t Article history: Complement deficiencies comprise between 1 and 10% of all primary immunodeficiencies (PIDs) accord- Received 29 May 2014 ing to national and supranational registries. They are still considered rare and even of less clinical Received in revised form 18 June 2014 importance. This not only reflects (as in all PIDs) a great lack of awareness among clinicians and gen- Accepted 23 June 2014 eral practitioners but is also due to the fact that only few centers worldwide provide a comprehensive Available online xxx laboratory complement analysis. To enable early identification, our aim is to present warning signs for complement deficiencies and recommendations for diagnostic approach. The genetic deficiency of any Keywords: early component of the classical pathway (C1q, C1r/s, C2, C4) is often associated with autoimmune dis- Complement deficiencies eases whereas individuals, deficient of properdin or of the terminal pathway components (C5 to C9), are Warning signs Prevalence highly susceptible to meningococcal disease. Deficiency of C1 Inhibitor (hereditary angioedema, HAE) Meningitis results in episodic angioedema, which in a considerable number of patients with identical symptoms Infections also occurs in factor XII mutations. -
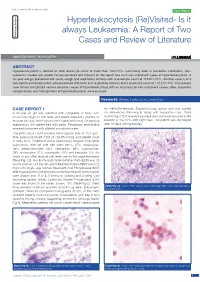
Hyperleukocytosis (Re)Visited- Is It Case Series Always Leukaemia: a Report of Two Pathology Section Cases and Review of Literature Short Communication
Review Article Clinician’s corner Original Article Images in Medicine Experimental Research Miscellaneous Letter to Editor DOI: 10.7860/JCDR/2020/40556.13409 Case Report Postgraduate Education Hyperleukocytosis (Re)Visited- Is it Case Series always Leukaemia: A Report of Two Pathology Section Cases and Review of Literature Short Communication ASHUTOSH RATH1, RICHA GUPTA2 ABSTRACT Hyperleukocytosis is defined as total leukocyte count of more than 100×109/L. Commonly seen in leukaemic conditions, non- leukaemic causes are usually not encountered and thought of. We report two such non-malignant cases of hyperleukocytosis. A six-year old girl presented with fever, cough and respiratory distress with a leukocyte count of 125.97×109/L. Another case is of a two-month old female infant, who presented with fever and respiratory distress and a leukocyte count of 112.27×109/L. The present case thrives to highlight various possible causes of hyperleukocytosis with an emphasis on non-malignant causes. Also, important complications and management of hyperleukocytosis are discussed. Keywords: Benign, Leukocytosis, Leukostasis CASE REPORT 1 for methicillin-resistant Staphylococcus aureus and was started A six-year-old girl was admitted with complaints of fever, non- on intravenous Vancomycin along with supportive care. Serial productive cough for one week and severe respiratory distress for monitoring of TLC revealed a gradual reduction and it returned to the the past one day. There was no other significant history. On physical baseline of 15×109/L after eight days. The patient was discharged examination, the patient had mild pallor. Respiratory examination after 10 days of hospital stay. -

Hereditary Angioedema: a Broad Review for Clinicians
REVIEW ARTICLE Hereditary Angioedema A Broad Review for Clinicians Ugochukwu C. Nzeako, MD, MPH; Evangelo Frigas, MD; William J. Tremaine, MD ereditary angioedema (HAE) is an autosomal dominant disease that afflicts 1 in 10000 to 1 in 150000 persons; HAE has been reported in all races, and no sex predomi- nance has been found. It manifests as recurrent attacks of intense, massive, localized edema without concomitant pruritus, often resulting from one of several known trig- Hgers. However, attacks can occur in the absence of any identifiable initiating event. Historically, 2 types of HAE have been described. However, a variant, possibly X-linked, inherited angioedema has recently been described, and tentatively it has been named “type 3” HAE. Signs and symptoms are identical in all types of HAE. Skin and visceral organs may be involved by the typically massive local edema. The most commonly involved viscera are the respiratory and gastrointestinal sys- tems. Involvement of the upper airways can result in severe life-threatening symptoms, including the risk of asphyxiation, unless appropriate interventions are taken. Quantitative and functional analyses of C1 esterase inhibitor and complement components C4 and C1q should be performed when HAE is suspected. Acute exacerbations of the disease should be treated with intravenous purified C1 esterase inhibitor concentrate, where available. Intravenous administration of fresh frozen plasma is also useful in acute HAE; however, it occasionally exacerbates symptoms. Corti- costeroids, antihistamines, and epinephrine can be useful adjuncts but typically are not effica- cious in aborting acute attacks. Prophylactic management involves long-term use of attenuated androgens or antifibrinolytic agents. -

Practice Parameter for the Diagnosis and Management of Primary Immunodeficiency
Practice parameter Practice parameter for the diagnosis and management of primary immunodeficiency Francisco A. Bonilla, MD, PhD, David A. Khan, MD, Zuhair K. Ballas, MD, Javier Chinen, MD, PhD, Michael M. Frank, MD, Joyce T. Hsu, MD, Michael Keller, MD, Lisa J. Kobrynski, MD, Hirsh D. Komarow, MD, Bruce Mazer, MD, Robert P. Nelson, Jr, MD, Jordan S. Orange, MD, PhD, John M. Routes, MD, William T. Shearer, MD, PhD, Ricardo U. Sorensen, MD, James W. Verbsky, MD, PhD, David I. Bernstein, MD, Joann Blessing-Moore, MD, David Lang, MD, Richard A. Nicklas, MD, John Oppenheimer, MD, Jay M. Portnoy, MD, Christopher R. Randolph, MD, Diane Schuller, MD, Sheldon L. Spector, MD, Stephen Tilles, MD, Dana Wallace, MD Chief Editor: Francisco A. Bonilla, MD, PhD Co-Editor: David A. Khan, MD Members of the Joint Task Force on Practice Parameters: David I. Bernstein, MD, Joann Blessing-Moore, MD, David Khan, MD, David Lang, MD, Richard A. Nicklas, MD, John Oppenheimer, MD, Jay M. Portnoy, MD, Christopher R. Randolph, MD, Diane Schuller, MD, Sheldon L. Spector, MD, Stephen Tilles, MD, Dana Wallace, MD Primary Immunodeficiency Workgroup: Chairman: Francisco A. Bonilla, MD, PhD Members: Zuhair K. Ballas, MD, Javier Chinen, MD, PhD, Michael M. Frank, MD, Joyce T. Hsu, MD, Michael Keller, MD, Lisa J. Kobrynski, MD, Hirsh D. Komarow, MD, Bruce Mazer, MD, Robert P. Nelson, Jr, MD, Jordan S. Orange, MD, PhD, John M. Routes, MD, William T. Shearer, MD, PhD, Ricardo U. Sorensen, MD, James W. Verbsky, MD, PhD GlaxoSmithKline, Merck, and Aerocrine; has received payment for lectures from Genentech/ These parameters were developed by the Joint Task Force on Practice Parameters, representing Novartis, GlaxoSmithKline, and Merck; and has received research support from Genentech/ the American Academy of Allergy, Asthma & Immunology; the American College of Novartis and Merck. -

Primary Immunodeficiency Disorders
ALLERGY AND IMMUNOLOGY 00954543 /98 $8.00 + .OO PRIMARY IMMUNODEFICIENCY DISORDERS Robert J. Mamlok, MD Immunodeficiency is a common thought among both patients and physicians when confronted with what is perceived as an excessive num- ber, duration, or severity of infections. Because of this, the starting point for evaluating patients for suspected immunodeficiency is based on what constitutes ”too many infections.” It generally is agreed that children with normal immune systems may have an average of 6 to 8 respiratory tract infections per year for the first decade of life. Even after a pattern of ab- normal infection is established, questions of secondary immunodeficiency should first be raised. The relatively uncommon primary immunodefi- ciency diseases are statistically dwarfed by secondary causes of recurrent infection, such as malnutrition, respiratory allergy, chronic cardiovascular, pulmonary, and renal disease, and environmental factors. On the other hand, a dizzying spiral of progress in our understanding of the genetics and immunology of primary immunodeficiency disease has resulted in improved diagnostic and therapeutic tools. Twenty-five newly recognized immunologic disease genes have been cloned in the last 5 ~ears.2~It has become arguably more important than ever for us to recognize the clinical and laboratory features of these relatively uncommon, but increasingly treatable, disorders. CLASSIFICATION The immune system has been classically divided into four separate arms: The B-cell system responsible for antibody formation, the T-cell sys- From the Division of Pediatric Allergy and Immunology, Texas Tech University Health Sci- ences Center, Lubbock, Texas PRIMARY CARE VOLUME 25 NUMBER 4 DECEMBER 1998 739 740 MAMLOK tem responsible for immune cellular regulation, the phagocytic (poly- morphonuclear and mononuclear) system and the complement (opsonic) system. -

Package Insert Has Been Approved by the U.S
HIGHLIGHTS OF PRESCRIBING INFORMATION **Doses up to 1,000 U every 3 to 4 days may be considered based on These highlights do not include all the information needed to use individual patient response. ® CINRYZE safely and effectively. See full prescribing information for ---------------------- DOSAGE FORMS AND STRENGTHS -------------------- CINRYZE. Approximately 500 Units (lyophilized) in an 8 mL vial. (3) CINRYZE (C1 Esterase Inhibitor [Human]) ---------------------------- CONTRAINDICATIONS ------------------------------- For Intravenous Use, Freeze-Dried Powder for Reconstitution Patients who have manifested life-threatening immediate hypersensitivity Initial U.S. Approval: 2008. reactions, including anaphylaxis, to the product (4). --------------------------- RECENT MAJOR CHANGES -------------------------- ----------------------------- WARNINGS/PRECAUTIONS ------------------------ • Indications and Usage (1) 06/2018 • Hypersensitivity reactions may occur. Have epinephrine immediately • Dosage and Administration (2.1) 06/2018 available for treatment of acute severe hypersensitivity reaction (5.1) • --------------------------- INDICATIONS AND USAGE --------------------------- Serious arterial and venous thromboembolic (TE) events have been CINRYZE is a C1 esterase inhibitor indicated for routine prophylaxis against reported at the recommended dose of C1 Esterase Inhibitor (Human) angioedema attacks in adults, adolescents and pediatric patients (6 years of products, including CINRYZE, following administration in patients with age and older) -

European Society for Immunodeficiencies (ESID)
Journal of Clinical Immunology https://doi.org/10.1007/s10875-020-00754-1 ORIGINAL ARTICLE European Society for Immunodeficiencies (ESID) and European Reference Network on Rare Primary Immunodeficiency, Autoinflammatory and Autoimmune Diseases (ERN RITA) Complement Guideline: Deficiencies, Diagnosis, and Management Nicholas Brodszki1 & Ashley Frazer-Abel2 & Anete S. Grumach3 & Michael Kirschfink4 & Jiri Litzman5 & Elena Perez6 & Mikko R. J. Seppänen7 & Kathleen E. Sullivan8 & Stephen Jolles9 Received: 5 June 2019 /Accepted: 20 January 2020 # The Author(s) 2020 Abstract This guideline aims to describe the complement system and the functions of the constituent pathways, with particular focus on primary immunodeficiencies (PIDs) and their diagnosis and management. The complement system is a crucial part of the innate immune system, with multiple membrane-bound and soluble components. There are three distinct enzymatic cascade pathways within the complement system, the classical, alternative and lectin pathways, which converge with the cleavage of central C3. Complement deficiencies account for ~5% of PIDs. The clinical consequences of inherited defects in the complement system are protean and include increased susceptibility to infection, autoimmune diseases (e.g., systemic lupus erythematosus), age-related macular degeneration, renal disorders (e.g., atypical hemolytic uremic syndrome) and angioedema. Modern complement analysis allows an in-depth insight into the functional and molecular basis of nearly all complement deficiencies. However, therapeutic options remain relatively limited for the majority of complement deficiencies with the exception of hereditary angioedema and inhibition of an overactivated complement system in regulation defects. Current management strategies for complement disor- ders associated with infection include education, family testing, vaccinations, antibiotics and emergency planning. Keywords Complement .