IV to PO Conversion Developed by Dr
Total Page:16
File Type:pdf, Size:1020Kb
Load more
Recommended publications
-

Severe Sepsis and Septic Shock Antibiotic Guide
Stanford Health Issue Date: 05/2017 Stanford Antimicrobial Safety and Sustainability Program Severe Sepsis and Septic Shock Antibiotic Guide Table 1: Antibiotic selection options for healthcare associated and/or immunocompromised patients • Healthcare associated: intravenous therapy, wound care, or intravenous chemotherapy within the prior 30 days, residence in a nursing home or other long-term care facility, hospitalization in an acute care hospital for two or more days within the prior 90 days, attendance at a hospital or hemodialysis clinic within the prior 30 days • Immunocompromised: Receiving chemotherapy, known systemic cancer not in remission, ANC <500, severe cell-mediated immune deficiency Table 2: Antibiotic selection options for community acquired, immunocompetent patients Table 3: Antibiotic selection options for patients with simple sepsis, community acquired, immunocompetent patients requiring hospitalization. Risk Factors for Select Organisms P. aeruginosa MRSA Invasive Candidiasis VRE (and other resistant GNR) Community acquired: • Known colonization with MDROs • Central venous catheter • Liver transplant • Prior IV antibiotics within 90 day • Recent MRSA infection • Broad-spectrum antibiotics • Known colonization • Known colonization with MDROs • Known MRSA colonization • + 1 of the following risk factors: • Prolonged broad antibacterial • Skin & Skin Structure and/or IV access site: ♦ Parenteral nutrition therapy Hospital acquired: ♦ Purulence ♦ Dialysis • Prolonged profound • Prior IV antibiotics within 90 days ♦ Abscess -

Antimicrobial Stewardship Guidance
Antimicrobial Stewardship Guidance Federal Bureau of Prisons Clinical Practice Guidelines March 2013 Clinical guidelines are made available to the public for informational purposes only. The Federal Bureau of Prisons (BOP) does not warrant these guidelines for any other purpose, and assumes no responsibility for any injury or damage resulting from the reliance thereof. Proper medical practice necessitates that all cases are evaluated on an individual basis and that treatment decisions are patient-specific. Consult the BOP Clinical Practice Guidelines Web page to determine the date of the most recent update to this document: http://www.bop.gov/news/medresources.jsp Federal Bureau of Prisons Antimicrobial Stewardship Guidance Clinical Practice Guidelines March 2013 Table of Contents 1. Purpose ............................................................................................................................................. 3 2. Introduction ...................................................................................................................................... 3 3. Antimicrobial Stewardship in the BOP............................................................................................ 4 4. General Guidance for Diagnosis and Identifying Infection ............................................................. 5 Diagnosis of Specific Infections ........................................................................................................ 6 Upper Respiratory Infections (not otherwise specified) .............................................................................. -
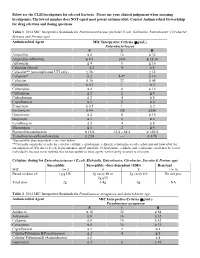
Below Are the CLSI Breakpoints for Selected Bacteria. Please Use Your Clinical Judgement When Assessing Breakpoints
Below are the CLSI breakpoints for selected bacteria. Please use your clinical judgement when assessing breakpoints. The lowest number does NOT equal most potent antimicrobial. Contact Antimicrobial Stewardship for drug selection and dosing questions. Table 1: 2014 MIC Interpretive Standards for Enterobacteriaceae (includes E.coli, Klebsiella, Enterobacter, Citrobacter, Serratia and Proteus spp) Antimicrobial Agent MIC Interpretive Criteria (g/mL) Enterobacteriaceae S I R Ampicillin ≤ 8 16 ≥ 32 Ampicillin-sulbactam ≤ 8/4 16/8 ≥ 32/16 Aztreonam ≤ 4 8 ≥ 16 Cefazolin (blood) ≤ 2 4 ≥ 8 Cefazolin** (uncomplicated UTI only) ≤ 16 ≥ 32 Cefepime* ≤ 2 4-8* ≥ 16 Cefotetan ≤ 16 32 ≥ 64 Ceftaroline ≤ 0.5 1 ≥ 2 Ceftazidime ≤ 4 8 ≥ 16 Ceftriaxone ≤ 1 2 ≥ 4 Cefpodoxime ≤ 2 4 ≥ 8 Ciprofloxacin ≤ 1 2 ≥ 4 Ertapenem ≤ 0.5 1 ≥ 2 Fosfomycin ≤ 64 128 ≥256 Gentamicin ≤ 4 8 ≥ 16 Imipenem ≤ 1 2 ≥ 4 Levofloxacin ≤ 2 4 ≥ 8 Meropenem ≤ 1 2 ≥ 4 Piperacillin-tazobactam ≤ 16/4 32/4 – 64/4 ≥ 128/4 Trimethoprim-sulfamethoxazole ≤ 2/38 --- ≥ 4/76 *Susceptibile dose-dependent – see chart below **Cefazolin can predict results for cefaclor, cefdinir, cefpodoxime, cefprozil, cefuroxime axetil, cephalexin and loracarbef for uncomplicated UTIs due to E.coli, K.pneumoniae, and P.mirabilis. Cefpodoxime, cefinidir, and cefuroxime axetil may be tested individually because some isolated may be susceptible to these agents while testing resistant to cefazolin. Cefepime dosing for Enterobacteriaceae ( E.coli, Klebsiella, Enterobacter, Citrobacter, Serratia & Proteus spp) Susceptible Susceptible –dose-dependent (SDD) Resistant MIC </= 2 4 8 >/= 16 Based on dose of: 1g q12h 1g every 8h or 2g every 8 h Do not give 2g q12 Total dose 2g 3-4g 6g NA Table 2: 2014 MIC Interpretive Standards for Pseudomonas aeruginosa and Acinetobacter spp. -

Piperacillin/Tazobactam Drug Class1 Antibiotic – Penicillin with Β-Lactamase Inhibitor
Monographs for Commonly Administered Intravenous Medications in Home and Community Care Piperacillin/Tazobactam Drug Class1 Antibiotic – penicillin with β-lactamase inhibitor Spectrum1 Refer to product monograph for complete spectrum For β-lactamase producing bacteria strains (e.g., Haemophilus influenza, Escherichia coli, and Staphylococcus aureus). Also to susceptible Acinetobacter species, Klebsiella pneumonia, Pseudomonas aeruginosa often combined with aminoglycoside). Cross Sensitivities / Allergies1 Cross sensitivities with penicillin and possibly cephalosporin and/or beta-lactam inhibitors Indications1,2 Intra-abdominal Respiratory tract Skin and skin structure Septicemia Gynecological Urinary tract Other conditions based on culture and sensitivity results Outpatient Considerations1 For patients with a documented allergy to penicillin, cephalosporin or beta-lactam inhibitor, the first dose should be administered in a hospital or clinic setting. Must be able to access laboratory monitoring (either at outpatient laboratory or by arranging in-home lab) if using an interacting oral medication (see Potential Drug Interactions section) Prescribing Considerations At time of ordering please provide the following to the pharmacist: and Dosage in Adults1,2 Height, weight Most recent serum creatinine with date obtained Indication (infection being treated) Usually dosed every 6 to 8 hours. Available as 2 g/0.25 g, 3 g/0.375 g, 4 g/0.5 g piperacillin/tazobactam (dose selected based on indication) Maximum 18 g/ 2.25 g piperacillin/tazobactam daily Dose and administration interval require adjustment for renal impairment Errors have occurred due to unusual ordering as combined dose of piperacillin and tazobactam. Order may be expressed only as piperacillin component or as a total of piperacillin + tazobactam (8:1 ratio). -

CEFTIN® Tablets CEFTIN® for Oral Suspension
PRODUCT INFORMATION CEFTIN® Tablets (cefuroxime axetil tablets) CEFTIN® for Oral Suspension (cefuroxime axetil powder for oral suspension) DESCRIPTION: CEFTIN Tablets and CEFTIN for Oral Suspension contain cefuroxime as cefuroxime axetil. CEFTIN is a semisynthetic, broad-spectrum cephalosporin antibiotic for oral administration. Chemically, cefuroxime axetil, the 1-(acetyloxy) ethyl ester of cefuroxime, is (RS)-1-hydroxyethyl (6R,7R)-7-[2-(2-furyl)glyoxylamido]-3-(hydroxymethyl)-8-oxo-5- thia-1-azabicyclo[4.2.0]oct-2-ene-2-carboxylate, 72-(Z)-(O-methyl-oxime), 1-acetate 3-carbamate. Its molecular formula is C20H22N4O10S, and it has a molecular weight of 510.48. Cefuroxime axetil is in the amorphous form and has the following structural formula: CEFTIN Tablets are film-coated and contain the equivalent of 125, 250, or 500 mg of cefuroxime as cefuroxime axetil. CEFTIN Tablets contain the inactive ingredients colloidal silicon dioxide, croscarmellose sodium, FD&C Blue No. 1 (250- and 500-mg tablets only), hydrogenated vegetable oil, hydroxypropyl methylcellulose, methylparaben, microcrystalline cellulose, propylene glycol, propylparaben, sodium benzoate (125-mg tablets only), sodium lauryl sulfate, and CEFTIN® Tablets (cefuroxime axetil tablets) CEFTIN® for Oral Suspension (cefuroxime axetil powder for oral suspension) titanium dioxide. CEFTIN for Oral Suspension, when reconstituted with water, provides the equivalent of 125 mg or 250 mg of cefuroxime (as cefuroxime axetil) per 5 mL of suspension. CEFTIN for Oral Suspension contains the inactive ingredients povidone K30, stearic acid, sucrose, and tutti-frutti flavoring. CLINICAL PHARMACOLOGY: Absorption and Metabolism: After oral administration, cefuroxime axetil is absorbed from the gastrointestinal tract and rapidly hydrolyzed by nonspecific esterases in the intestinal mucosa and blood to cefuroxime. -

Ceftaroline in Complicated Skin and Skin-Structure Infections
Infection and Drug Resistance Dovepress open access to scientific and medical research Open Access Full Text Article REVIEW Ceftaroline in complicated skin and skin-structure infections Paul O Hernandez1 Abstract: Ceftaroline is an advanced-generation cephalosporin antibiotic recently approved by Sergio Lema2 the US Food and Drug Administration for the treatment of complicated skin and skin-structure Stephen K Tyring3 infections (cSSSIs). This intravenous broad-spectrum antibiotic exerts potent bactericidal activity Natalia Mendoza2,4 by inhibiting bacterial cell wall synthesis. A high affinity for the penicillin-binding protein 2a (PBP2a) of methicillin-resistant Staphylococcus aureus (MRSA) makes the drug especially 1University of Texas School of Medicine at San Antonio, beneficial to patients with MRSA cSSSIs. Ceftaroline has proved in multiple well-conducted San Antonio, TX, 2Woodhull clinical trials to have an excellent safety and efficacy profile. In adjusted doses it is also recom- Medical and Mental Health Center, mended for patients with renal or hepatic impairment. Furthermore, the clinical effectiveness Brooklyn, NY, 3Department of Dermatology, University of Texas and high cure rate demonstrated by ceftaroline in cSSSIs, including those caused by MRSA Health Science Center at Houston, and other multidrug-resistant strains, warrants its consideration as a first-line treatment option 4 Houston, TX, USA; Department of for cSSSIs. This article reviews ceftaroline and its pharmacology, efficacy, and safety data to Dermatology, El -

A Thesis Entitled an Oral Dosage Form of Ceftriaxone Sodium Using Enteric
A Thesis entitled An oral dosage form of ceftriaxone sodium using enteric coated sustained release calcium alginate beads by Darshan Lalwani Submitted to the Graduate Faculty as partial fulfillment of the requirements for the Master of Science Degree in Pharmaceutical Sciences with Industrial Pharmacy Option _________________________________________ Jerry Nesamony, Ph.D., Committee Chair _________________________________________ Sai Hanuman Sagar Boddu, Ph.D, Committee Member _________________________________________ Youssef Sari, Ph.D., Committee Member _________________________________________ Patricia R. Komuniecki, PhD, Dean College of Graduate Studies The University of Toledo May 2015 Copyright 2015, Darshan Narendra Lalwani This document is copyrighted material. Under copyright law, no parts of this document may be reproduced without the expressed permission of the author. An Abstract of An oral dosage form of ceftriaxone sodium using enteric coated sustained release calcium alginate beads by Darshan Lalwani Submitted to the Graduate Faculty as partial fulfillment of the requirements for the Master of Science Degree in Pharmaceutical Sciences with Industrial Pharmacy option The University of Toledo May 2015 Purpose: Ceftriaxone (CTZ) is a broad spectrum semisynthetic, third generation cephalosporin antibiotic. It is an acid labile drug belonging to class III of biopharmaceutical classification system (BCS). It can be solvated quickly but suffers from the drawback of poor oral bioavailability owing to its limited permeability through -

Journal Club: “Effect of Piperacillin-Tazobactam Vs
Infectious Disease Update 02/25/19 Steven T. Park Division of Infectious Diseases Objectives • Zosyn versus Meropenem for ESBL bacteremia • 7 versus 14 days for gram negative bacteremia • Oral versus IV for osteomyelitis “Effect of Piperacillin-Tazobactam vs Meropenem on 30-Day Mortality for Patients With E coli or Klebsiella pneumoniae Bloodstream Infection and Ceftriaxone Resistance” (MERINO trial) Harris PNA et al. JAMA 2018. Sep 11; 320:984. Introduction • Treatment of choice for ESBL organisms are thought to be carbapenems • Reports of failure of non-carbapenems in the past even when microbiologic data showed susceptibility • Most reported before CLSI lowered the breakpoints for Enterobacteriaceae • Recent reviews looking at retrospective data conclude that you can use non-carbapenems (Zosyn, Cefepime) for urine infections • However no randomized controlled trial testing this hypothesis • First randomized controlled trial testing whether Zosyn is equivalent to meropenem for ESBL bacteremia Design, Setting, Participants • Non-inferiority, parallel group, randomized clinical trial • Hospitalized patients enrolled from 26 sites in 9 countries (mostly from Singapore, Australia, Italy, Saudi Arabia, and Turkey) from February 2014 to July 2017 • Patients over the age of 21 was eligible if he/she had at least 1 positive blood culture with E coli or Klebsiella spp that was non-susceptible to ceftriaxone but susceptible to pip-tazo and meropenem • Of 1646 patients screened, 391 were included in the study. • Meropenem 1g IV q8h (n = 191) or piperacillin/tazobactam 4.5g IV q6h (not extended infusion, n = 188) was given for a minimum of 4 days and up to 14 days. The duration of therapy was determined by the treating clinician. -

Cefuroxime Axetil
Cefuroxime axetil Zinnat® Tablets PRODUCT DESCRIPTION Cefuroxime (as axetil) (Zinnat®) 250mg tablet:. Each white, film-coated, capsule-shaped tablet engraved with ‘GXES7' on one side tablet contains 250mg of Cefuroxime (as axetil). Cefuroxime (as axetil) (Zinnat®) 500mg tablet: Each white, film-coated, capsule-shaped tablet engraved with 'GXEG2' on one side tablet contains 500mg of Cefuroxime (as axetil). PHARMACOLOGIC PROPERTIES Pharmacodynamics The prevalence of acquired resistance is geographically and time dependent and for select species may be very high. Local information on resistance is desirable, particularly when treating severe infections. In vitro susceptibility of micro-organisms to Cefuroxime Where clinical efficacy of cefuroxime axetil has been demonstrated in clinical trials this is indicated with an asterisk (*). Commonly Susceptible Species Gram-Positive Aerobes: Staphylococcus aureus (methicillin susceptible)* Coagulase negative staphylococcus (methicillin susceptible) Streptococcus pyogenes* Beta-hemolytic streptococci Gram-Negative Aerobes: Haemophilus influenzae* including ampicillin resistant strains Haemophilus parainfluenzae* Moraxella catarrhalis* Neisseria gonorrhoea* including penicillinase and non-penicillinase producing strains Gram-Positive Anaerobes: Peptostreptococcus spp. Propionibacterium spp. Spirochetes: Borrelia burgdorferi* Organisms for which acquired resistance may be a problem Gram-Positive Aerobes: Streptococcus pneumoniae* Gram-Negative Aerobes: Citrobacter spp. not including C. freundii Enterobacter -

Antimicrobials As Single and Combination Therapy for Colistin-Resistant Pseudomonas Aeruginosa at a University Hospital in Thailand
antibiotics Article Antimicrobials as Single and Combination Therapy for Colistin-Resistant Pseudomonas aeruginosa at a University Hospital in Thailand Supanun Pungcharoenkijkul 1,2, Jantima Traipattanakul 3, Sudaluck Thunyaharn 4 and Wichai Santimaleeworagun 5,6,* 1 College of Pharmacotherapy Thailand, Nontaburi 11000, Thailand; [email protected] 2 Department of Pharmacist, Nopparat Rajathanee Hospital, Bangkok 10230, Thailand 3 Division of Infectious Disease, Department of Medicine, Phramongkutklao Hospital, Bangkok 10400, Thailand; [email protected] 4 Faculty of Medical Technology, Nakhonratchasima College, Nakhon Ratchasima 30000, Thailand; [email protected] 5 Department of Pharmacy, Faculty of Pharmacy, Silpakorn University, Nakorn Pathom 73000, Thailand 6 Pharmaceutical Initiative for Resistant Bacteria and Infectious Disease Working Group (PIRBIG), Nakorn Pathom 73000, Thailand * Correspondence: [email protected]; Tel.: +66-3425-580-0 Received: 29 June 2020; Accepted: 31 July 2020; Published: 3 August 2020 Abstract: Global infections with colistin-resistant Pseudomonas aeruginosa (CoR-PA) are increasing; there are currently very few studies focused on the antimicrobial susceptibility of CoR-PA isolates, and none from Thailand. Here, we investigated the impact of various antimicrobials, alone and in combination, via the in vitro testing of CoR-PA clinical isolates. Eighteen CoR-PA isolates were obtained from patients treated at Phramongkutklao Hospital from January 2010 through June 2019; these were classified into six different clonal types by using the enterobacterial repetitive intergenic consensus (ERIC)-PCR method, with a high prevalence of Group A (27.8%). The antimicrobial susceptibility was determined as the minimal inhibitory concentrations (MICs) using the epsilometer-test (E-test) method. The synergistic activities of six antimicrobial combinations were reported via the fractional-inhibitory-concentration index. -

Vancomycin Plus Piperacillin/Tazobactam and Acute Kidney Injury in Adults: a Systematic Review and Meta-Analysis
University of Rhode Island DigitalCommons@URI Pharmacy Practice Faculty Publications Pharmacy Practice 2017 Vancomycin plus piperacillin/tazobactam and acute kidney injury in adults: a systematic review and meta-analysis Megan Luther Tristan Timbrook Aisling R. Caffrey University of Rhode Island, [email protected] David Dosa Thomas Lodise FSeeollow next this page and for additional additional works authors at: https:/ /digitalcommons.uri.edu/php_facpubs The University of Rhode Island Faculty have made this article openly available. Please let us know how Open Access to this research benefits you. This is a pre-publication author manuscript of the final, published article. Terms of Use This article is made available under the terms and conditions applicable towards Open Access Policy Articles, as set forth in our Terms of Use. Citation/Publisher Attribution Luther MK, Timbrook TT, Caffrey AR, Dosa D, Lodise TP, LaPlante KL. Vancomycin plus piperacillin/ tazobactam and acute kidney injury in adults: a systematic review and meta-analysis. Critical Care Medicine 2018; 46(1):12-20. doi: 10.1097/CCM.0000000000002769 Available at: http://dx.doi.org/10.1097/CCM.0000000000002769 This Article is brought to you for free and open access by the Pharmacy Practice at DigitalCommons@URI. It has been accepted for inclusion in Pharmacy Practice Faculty Publications by an authorized administrator of DigitalCommons@URI. For more information, please contact [email protected]. Authors Megan Luther, Tristan Timbrook, Aisling R. Caffrey, David Dosa, Thomas Lodise, and Kerry L. LaPlante This article is available at DigitalCommons@URI: https://digitalcommons.uri.edu/php_facpubs/142 1 Vancomycin plus piperacillin-tazobactam and acute kidney injury in adults: A systematic review 2 and meta-analysis 3 4 Date: August 19, 2017 5 6 Megan K. -

List Item Assessment Report for Zinacef
10 September 2012 EMA/CHMP/633654/2012 Assessment report for Zinacef and associated names Pursuant to Article 30 of Directive 2001/83/EC INN : cefuroxime (cefuroxime sodium) Procedure no: EMEA/H/A-30/1158 Assessment Report as adopted by the CHMP with all information of a commercially confidential nature deleted. 7 Westferry Circus ● Canary Wharf ● London E14 4HB ● United Kingdom Telephone +44 (0)20 7418 8400 Facsimile +44 (0)20 7523 7051 E -mail [email protected] Website www.ema.europa.eu An agency of the European Union © European Medicines Agency, 2013. Reproduction is authorised provided the source is acknowledged. Table of contents Table of contents ......................................................................................... 2 1. Background information on the procedure .............................................. 3 1.1. Background information on the basis of the grounds for referral ................................. 3 2.1. Introduction......................................................................................................... 3 2.2. Critical Evaluation ................................................................................................ 4 Section 4.1 - Therapeutic indications ............................................................................. 4 Section 4.2 - Posology and method of administration .................................................... 30 Section 4.3 - Contraindications ................................................................................... 33 Section 4.4 - Special