Platelet Morphology Received January 20, 2020; Accepted March 28, 2020 Introduction
Total Page:16
File Type:pdf, Size:1020Kb
Load more
Recommended publications
-

Peripheral Blood Cells Changes After Two Groups of Splenectomy And
ns erte ion p : O y p H e f Yunfu et al., J Hypertens (Los Angel) 2018, 7:1 n o l A a DOI: 10.4172/2167-1095.1000249 c c n r e u s o s J Journal of Hypertension: Open Access ISSN: 2167-1095 Research Article Open Access Peripheral Blood Cells Changes After Two Groups of Splenectomy and Prevention and Treatment of Postoperative Complication Yunfu Lv1*, Xiaoguang Gong1, XiaoYu Han1, Jie Deng1 and Yejuan Li2 1Department of General Surgery, Hainan Provincial People's Hospital, Haikou, China 2Department of Reproductive, Maternal and Child Care of Hainan Province, Haikou, China *Corresponding author: Yunfu Lv, Department of General Surgery, Hainan Provincial People's Hospital, Haikou 570311, China, Tel: 86-898-66528115; E-mail: [email protected] Received Date: January 31, 2018; Accepted Date: March 12, 2018; Published Date: March 15, 2018 Copyright: © 2018 Lv Y, et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited. Abstract Objective: This study aimed to investigate the changes in peripheral blood cells after two groups of splenectomy in patients with traumatic rupture of the spleen and portal hypertension group, as well as causes and prevention and treatment of splenectomy related portal vein thrombosis. Methods: Clinical data from 109 patients with traumatic rupture of the spleen who underwent splenectomy in our hospital from January 2001 to August 2015 were retrospectively analyzed, and compared with those from 240 patients with splenomegaly due to cirrhotic portal hypertension who underwent splenectomy over the same period. -

Combined Effect of Granulocyte-Colony-Stimulating
J Korean Med. 2016;37(4):36-44 http://dx.doi.org/10.13048/jkm.16046 pISSN 1010-0695 • eISSN 2288-3339 Original Article Combined Effect of Granulocyte-Colony-Stimulating Factor-Induced Bone Marrow-Derived Stem Cells and Red Ginseng in Patients with Decompensated Liver Cirrhosis (Combined Effect of G-CSF and Red Ginseng in Liver Cirrhosis) Hyun Hee Kim1, Seung Mo Kim2, Kyung Soon Kim2, Min A Kwak2, Sang Gyung Kim3, Byung Seok Kim1, Chang Hyeong Lee1 1Department of Internal Medicine, Catholic University of Daegu School of Medicine 2Department of Internal Medicine, College of Korean Medicine, Daegu Haany University 3Department of Laboratory Medicine, Catholic University of Daegu School of Medicine Objectives: Granulocyte-colony-stimulating factor (G-CSF) mobilized bone marrow (BM)-derived hematopoietic stem cells could contribute to improvement of liver function. In addition, liver fibrosis can reportedly be prevented by the Rg 1 component of red ginseng. This study investigated the combined effect of G-CSF and red ginseng on decompensated liver cirrhosis. Methods: Four patients with decompensated liver cirrhosis were injected with G-CSF to proliferate BM stem cells for 4 days (5 μg/kg bid subcutaneously) and followed-up for 3 months. The patients also received red ginseng for 4 days (2 tablets tid per os). We analyzed Child-Pugh scores, Model for End-Stage Liver Disease (MELD) scores and cirrhotic complications. Results: All patients showed marked increases in White blood cell (WBC) and CD34+ cells in the peripheral blood, with a peak time of 4 days after G-CSF injection. Spleen size also increased after G-CSF injection, but not severely. -
10 11 Cyto Slides 81-85
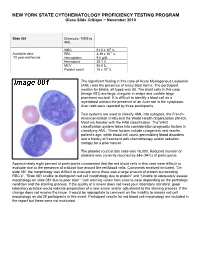
NEW YORK STATE CYTOHEMATOLOGY PROFICIENCY TESTING PROGRAM Glass Slide Critique ~ November 2010 Slide 081 Diagnosis: MDS to AML 9 WBC 51.0 x 10 /L 12 Available data: RBC 3.39 x 10 /L 72 year-old female Hemoglobin 9.6 g/dL Hematocrit 29.1 % MCV 86.0 fL Platelet count 16 x 109 /L The significant finding in this case of Acute Myelogenous Leukemia (AML) was the presence of many blast forms. The participant median for blasts, all types was 88. The blast cells in this case (Image 081) are large, irregular in shape and contain large prominent nucleoli. It is difficult to identify a blast cell as a myeloblast without the presence of an Auer rod in the cytoplasm. Auer rods were reported by three participants. Two systems are used to classify AML into subtypes, the French- American-British (FAB) and the World Health Organization (WHO). Most are familiar with the FAB classification. The WHO classification system takes into consideration prognostic factors in classifying AML. These factors include cytogenetic test results, patient’s age, white blood cell count, pre-existing blood disorders and a history of treatment with chemotherapy and/or radiation therapy for a prior cancer. The platelet count in this case was 16,000. Reduced number of platelets was correctly reported by 346 (94%) of participants. Approximately eight percent of participants commented that the red blood cells in this case were difficult to evaluate due to the presence of a bluish hue around the red blood cells. Comments received included, “On slide 081 the morphology was difficult to evaluate since there was a large amount of protein surrounding RBC’s”, “Slide 081 unable to distinguish red cell morphology due to protein” and “Unable to adequately assess morphology on slide 081 due to poor stain”. -

Factors Influencing Platelet Recovery After Blood Cell Transplantation in Multiple Myeloma
Bone Marrow Transplantation, (1997) 20, 375–380 1997 Stockton Press All rights reserved 0268–3369/97 $12.00 Factors influencing platelet recovery after blood cell transplantation in multiple myeloma MA Gertz1, MQ Lacy1, DJ Inwards1, AA Pineda2, MG Chen3, DA Gastineau1, A Tefferi1, RA Kyle1 and MR Litzow1 1Division of Hematology and Internal Medicine, 2Division of Transfusion Medicine, and 3Division of Radiation Oncology, Mayo Clinic and Mayo Foundation, Rochester, MN, USA Summary: cells result in durable engraftment after transplantation.2 Hematopoietic recovery can be accelerated by the use of We sought to determine factors that impact on the blood stem cells mobilized with growth factors or chemo- recovery of platelets after blood cell transplantation in therapy (or both). Hematopoietic recovery is more rapid patients with multiple myeloma. We performed retro- after mobilized peripheral blood stem cell transplantation spective analyses in 51 patients undergoing blood cell than after autologous bone marrow transplantation, and transplantation for multiple myeloma. The pro- hematopoietic recovery has been shown to be sustained, portional-hazards model was applied to determine sig- indicating that accessory cells found in the bone marrow nificant risk factors. Of 51 transplants, 14 patients failed are not required for durable engraftment.3 The more rapid to achieve a platelet count of 50 × 109/l. Median time to engraftment with mobilized stem cells is likely due to an a neutrophil count of 0.5 × 109/l was 10.5 days. Median increase in committed -
Blood Lab First Week
Blood Lab First Week This is a self propelled powerpoint study atlas of blood cells encountered in examination of the peripheral blood smear. It is a requirement of this course that you begin review of these slides with the first day of class in order to familiarize yourself with terms used in describing peripheral blood morphology. Laboratory final exam questions are derived directly from these slides. The content of these slides may duplicate slides (1-37) listed on the Hematopathology Website. You must familiarize yourself with both sets of slides in order to have the best learning opportunity. Before Beginning This Slide Review • Please read the Laboratory information PDF under Laboratory Resources file to learn about – Preparation of a blood smear – How to select an area of the blood smear for review of morphology and how to perform a white blood cell differential – Platelet estimation – RBC morphology descriptors • Anisocytosis • Poikilocytosis • Hypochromia • Polychromatophilia Normal blood smear. Red blood cells display normal orange pink cytoplasm with central pallor 1/3-1/2 the diameter of the red cell. There is mild variation in size (anisocytosis) but no real variation in shape (poikilocytosis). To the left is a lymphocyte. To the right is a typical neutrophil with the usual 3 segmentations of the nucleus. Med. Utah pathology Normal blood: thin area Ref 2 Normal peripheral blood smear. This field is good for exam of cell morphology, although there are a few minor areas of overlap of red cells. Note that most cells are well dispersed and the normal red blood cell central pallor is noted throughout the smear. -

ORIGINAL ARTICLE PML–Rara Initiates Leukemia by Conferring Properties of Self-Renewal to Committed Promyelocytic Progenitors
Leukemia (2009) 23, 1462–1471 & 2009 Macmillan Publishers Limited All rights reserved 0887-6924/09 $32.00 www.nature.com/leu ORIGINAL ARTICLE PML–RARa initiates leukemia by conferring properties of self-renewal to committed promyelocytic progenitors S Wojiski1,2, FC Guibal3, T Kindler1,2, BH Lee1,2, JL Jesneck4,5, A Fabian1,2, DG Tenen3,6 and DG Gilliland1,2,6 1Division of Hematology, Brigham and Women’s Hospital, Boston, MA, USA; 2Department of Genetics, Howard Hughes Medical Institute, Harvard Medical School, Boston, MA, USA; 3Department of Hematology/Oncology, Harvard Institutes of Medicine, Boston, MA, USA; 4Cancer Program, Broad Institute of Harvard and MIT, Cambridge, MA, USA; 5Department of Pediatric Oncology, Dana-Farber Cancer Institute, Harvard Medical School, Boston, MA, USA and 6Harvard Stem Cell Institute, Harvard University, Boston, MA, USA Acute promyelocytic leukemia (APL) is characterized by the leukemia stem cells (LSCs) are rare cells contained within hyperproliferation of promyelocytes, progenitors that are the more primitive CD34 þ CD38À population, resembling committed to terminal differentiation into granulocytes, making it an ideal disease in which to study the transforming potential transformed hematopoietic stem cells (HSCs). LSC activity was of less primitive cell types. We utilized a murine model of APL in shown by these investigators in all AML subtypes tested, but which the PML–RARa oncogene is expressed from the were not shown in acute promyelocytic leukemia (APL) endogenous cathepsin G promoter to test the hypothesis that associated with the expression of the PML–RARa fusion as a leukemia stem cell (LSC) activity resides within the differen- consequence of an acquired t(15;17). -

Difference Between Promyelocyte and Myelocyte Key Difference
Difference Between Promyelocyte and Myelocyte www.differencebetween.com Key Difference - Promyelocyte vs Myelocyte Granulated blood cells include eosinophils, basophils, and neutrophils which participate in a variety of functions in the body. The precursor stem cells of these cells which arise from the hematopoietic stem cells are of the myeloid lineage. Myeloblasts are the precursor cells of granulated blood cells. Myeloblasts then mature into promyelocytes, myelocytes, metamyelocytes, bands, and segments to finally give rise to granulocytes in the peripheral blood tissue. The development process is known as Granulopoiesis. Promyelocyte is the second stage of Myeloblast development. Myelocyte is the third stage of Myeloblast development. The key difference between the promyelocyte and the myelocyte is the level of differentiation it exhibits. Promyelocytes do not show differentiation while myelocytes show differentiation. What is a Promyelocyte? Promyelocyte is the second stage of the Myeloblast development process. The promyelocyte is larger than the myeloblast. It has a diameter of 12-25µm and is the largest cell type in the myeloid series. It has a prominent nucleus, and the nucleus is placed slightly intended in the cytoplasm. Chromatin and nucleoli are prominent in this. Final structures of chromatin can be identified through microscopic observations. Towards the complete maturation of the promyelocyte, the chromatins appear as well-condensed structures. The condensed chromatin is placed along the nuclear membrane. The cytoplasm of the promyelocyte is granulated, and these granules are termed as the primary azurophilic granules. Since the promyelocyte is not differentiated, it is formed of a basophilic cytoplasm. The cell organelle organization is prominent in the promyelocyte stage of the blood cells. -

Advanced Blood Cell Identification
ADVANCED BLOOD CELL ID: LEUKOCYTES AND ERYTHROCYTES IN AN ACUTE LEUKEMIA Educational commentary is provided for participants enrolled in program #259- Advanced Blood Cell Identification. This virtual blood cell identification program includes case studies with more difficult challenges. To view the blood cell images in more detail, click on the sample identification numbers underlined in the paragraphs below. This will open a virtual image of the selected cell and the surrounding fields. If the image opens in the same window as the commentary, saving the commentary PDF and opening it outside your browser will allow you to switch between the commentary and the images more easily. Click on this link for the API ImageViewerTM Instructions. Learning Outcomes After completing this exercise, participants should be able to: • Discuss morphologic characteristics of normal peripheral blood leukocytes. • Describe morphologic features of immature granulocytes. • Identify morphologic abnormalities in erythrocyte shape and chromaticity/coloration. Case Study An 18 year old male was seen by his physician for bruising and severe nosebleeds. His CBC results are as follows: WBC=7.5 x 109/L, RBC=2.79 1012/L, Hgb=8.7 g/dL, Hct=24.6%, MCV=88 fL, MCH=31 pg, MCHC=35 g/dL, RDW=18.4%, Platelet=41 x 109/L, MPV=10.4. Educational Commentary The cells selected for identification and discussion in this exercise are from the peripheral blood smear of an 18 year old man diagnosed with acute promyelocytic leukemia (APL). APL is also referred to as acute myeloid leukemia, M3 (AML-M3). As with other acute leukemias, APL has a rapid onset. -

Henry Ford Hospital Clinicopathological Conference: Metamorphosis in Chronic Granulocytic Leukemia in a 60-Year-Old Man
Henry Ford Hospital Medical Journal Volume 28 Number 1 Article 7 3-1980 Henry Ford Hospital Clinicopathological Conference: Metamorphosis in chronic granulocytic leukemia in a 60-year-old man Follow this and additional works at: https://scholarlycommons.henryford.com/hfhmedjournal Part of the Life Sciences Commons, Medical Specialties Commons, and the Public Health Commons Recommended Citation (1980) "Henry Ford Hospital Clinicopathological Conference: Metamorphosis in chronic granulocytic leukemia in a 60-year-old man," Henry Ford Hospital Medical Journal : Vol. 28 : No. 1 , 37-46. Available at: https://scholarlycommons.henryford.com/hfhmedjournal/vol28/iss1/7 This Article is brought to you for free and open access by Henry Ford Health System Scholarly Commons. It has been accepted for inclusion in Henry Ford Hospital Medical Journal by an authorized editor of Henry Ford Health System Scholarly Commons. Henry Ford Hosp Med Journal Vol 28, No 1, 1980 Henry Ford Hospital Clinicopathological Conference Metamorphosis in chronic granulocytic leukemia in a 60-year-old man Participants: Protocol: Dr. Ellis J. Van Slyck, Department of Internal Medicine, Division of Hematology Discussant: Dr. Robert K. Nixon, Department of Internal Medicine, Second Medical Division Radiology: Dr. Mark C. Weingarden, Department of Diagnostic Radiology Pathology: Dr. John W. Rebuck, Department of Pathology, Division of Hematology Case Presentation As an outpatient, his myleran dosage was gradually tapered as the This 60-year-old white man came to Henry Ford Hospital in blood counts responded. On February 27, the white count was December 1975, complaining of increased fatigability over the 40,000 and the platelet count 400,000. On May 10, the white preceding year. -

Causes of Peripheral Blood Cytopenias in Patients with Liver Cirrhosis Portal Hypertension and Clinical Significances
Open Journal of Endocrine and Metabolic Diseases, 2014, 4, 85-89 Published Online April 2014 in SciRes. http://www.scirp.org/journal/ojemd http://dx.doi.org/10.4236/ojemd.2014.44010 Causes of Peripheral Blood Cytopenias in Patients with Liver Cirrhosis Portal Hypertension and Clinical Significances Yunfu Lv Department of General Surgery, People’s Hospital of Hainan Province, Haikou, China Email: [email protected] Received 18 March 2014; revised 12 April 2014; accepted 19 April 2014 Copyright © 2014 by author and Scientific Research Publishing Inc. This work is licensed under the Creative Commons Attribution International License (CC BY). http://creativecommons.org/licenses/by/4.0/ Abstract Liver cirrhosis portal hypertension patients to reduce the number of blood cells are common in clinical, and often affect the prognosis. This paper discusses cirrhotic portal hypertension patients complicated by the reason of the decrease in the number of peripheral blood cells and what is the clinical significance of these reasons so as to provide theoretical support for the choice of treat- ment. Splenomegaly and hypersplenism caused should be the main reason for reducing the num- ber of blood cells, but not all, other reasons are alcohol and virus inhibition of bone marrow, liver function impairment, autoimmune damage and loss of blood, etc. If it is a function of the spleen hyperfunction caused by blood cells decreases, blood should rise to normal after splenectomy, or consider other reason or there are other reasons at the same time. Keywords Liver Cirrhosis Portal Hypertension, Peripheral Blood Cytopenias, Causes, Cilinical Significances 1. Introduction There are approximately 350 million carriers of hepatitis B virus (HBV) worldwide, and more than half of them are in the Asia-Pacific region. -

Identifying Abnormalities in Peripheral Blood Cells
EDUCATIONAL COMMENTARY – IDENTIFYING ABNORMALITIES IN PERIPHERAL BLOOD CELLS Educational commentary is provided through our affiliation with the American Society for Clinical Pathology (ASCP). To obtain FREE CME/CMLE credits click on Earn CE Credits under Continuing Education on the left side of the screen. Learning Outcomes Upon completion of this exercise, participants will be able to: describe the morphologic features of normal peripheral blood leukocytes. identify abnormalities in red blood cells (RBCs) that are characteristic of hereditary spherocytosis. discuss the pathophysiology of hereditary spherocytosis. An 8 year old female was seen in the pediatric hematology clinic. Laboratory findings included: WBC= 13.6 x 109/L, RBC= 2.63 x 1012/L, Hgb= 8.5 g/dL, Hct= 22%, MCV= 85.0 fL, MCH= 32.4 pg, MCHC= 38.1 g/dL, RDW= 21.4%, and Platelets= 897 x 109/L. This patient has been diagnosed with hereditary spherocytosis. Normal leukocytes and abnormalities in erythrocytes that may be seen in this condition are presented in the images. BCI-01 shows an eosinophil. Eosinophils characteristically have large, red-orange cytoplasmic granules. These granules are numerous and uniform in size. The nucleus of an eosinophil is often bilobed, although in this image, it is round. The chromatin is generally dense and clumped. American Proficiency Institute – 2011 1st Test Event EDUCATIONAL COMMENTARY – IDENTIFYING ABNORMALITIES IN PERIPHERAL BLOOD CELLS (cont.) The cell identified in BCI-02 is a segmented neutrophil. Neutrophils usually have 2 to 5 nuclear lobes connected by thin filaments of chromatin. The chromatin is coarse and densely clumped. In contrast to the eosinophil shown in BCI-01, segmented neutrophils have numerous small granules that normally stain light-violet or pink. -

Perforin-2 Is Essential for Intracellular Defense of Parenchymal Cells And
RESEARCH ARTICLE elifesciences.org Perforin-2 is essential for intracellular defense of parenchymal cells and phagocytes against pathogenic bacteria Ryan M McCormack1, Lesley R de Armas1, Motoaki Shiratsuchi1, Desiree G Fiorentino1, Melissa L Olsson1, Mathias G Lichtenheld1, Alejo Morales1, Kirill Lyapichev1, Louis E Gonzalez1, Natasa Strbo1, Neelima Sukumar2, Olivera Stojadinovic3, Gregory V Plano1, George P Munson1, Marjana Tomic- Canic3, Robert S Kirsner3, David G Russell2, Eckhard R Podack1* 1Department of Microbiology and Immunology, Miller School of Medicine, University of Miami, Miami, United States; 2Department of Microbiology and Immunology, College of Veterinary Medicine, Cornell University, Ithaca, United States; 3Wound Healing and Regenerative Medicine Research Program, Department of Dermatology and Cutaneous Surgery, Miller School of Medicine, University of Miami, Miami, United States Abstract Perforin-2 (MPEG1) is a pore-forming, antibacterial protein with broad-spectrum activity. Perforin-2 is expressed constitutively in phagocytes and inducibly in parenchymal, tissue-forming cells. In vitro, Perforin-2 prevents the intracellular replication and proliferation of bacterial pathogens in these cells. Perforin-2 knockout mice are unable to control the systemic dissemination of methicillin-resistant Staphylococcus aureus (MRSA) or Salmonella typhimurium and perish shortly after epicutaneous or orogastric infection respectively. In contrast, Perforin-2-sufficient littermates clear the infection. Perforin-2 is a transmembrane protein of cytosolic vesicles -derived from multiple organelles- that translocate to and fuse with bacterium containing vesicles. Subsequently, Perforin-2 polymerizes and forms large clusters of 100 A˚ pores in the bacterial surface with Perforin-2 cleavage products present in bacteria. Perforin-2 is also required for the bactericidal activity of reactive oxygen and nitrogen species and hydrolytic enzymes.