Platelet Counting: Ugly Traps and Good Advice
Total Page:16
File Type:pdf, Size:1020Kb
Load more
Recommended publications
-

Section 8: Hematology CHAPTER 47: ANEMIA
Section 8: Hematology CHAPTER 47: ANEMIA Q.1. A 56-year-old man presents with symptoms of severe dyspnea on exertion and fatigue. His laboratory values are as follows: Hemoglobin 6.0 g/dL (normal: 12–15 g/dL) Hematocrit 18% (normal: 36%–46%) RBC count 2 million/L (normal: 4–5.2 million/L) Reticulocyte count 3% (normal: 0.5%–1.5%) Which of the following caused this man’s anemia? A. Decreased red cell production B. Increased red cell destruction C. Acute blood loss (hemorrhage) D. There is insufficient information to make a determination Answer: A. This man presents with anemia and an elevated reticulocyte count which seems to suggest a hemolytic process. His reticulocyte count, however, has not been corrected for the degree of anemia he displays. This can be done by calculating his corrected reticulocyte count ([3% × (18%/45%)] = 1.2%), which is less than 2 and thus suggestive of a hypoproliferative process (decreased red cell production). Q.2. A 25-year-old man with pancytopenia undergoes bone marrow aspiration and biopsy, which reveals profound hypocellularity and virtual absence of hematopoietic cells. Cytogenetic analysis of the bone marrow does not reveal any abnormalities. Despite red blood cell and platelet transfusions, his pancytopenia worsens. Histocompatibility testing of his only sister fails to reveal a match. What would be the most appropriate course of therapy? A. Antithymocyte globulin, cyclosporine, and prednisone B. Prednisone alone C. Supportive therapy with chronic blood and platelet transfusions only D. Methotrexate and prednisone E. Bone marrow transplant Answer: A. Although supportive care with transfusions is necessary for treating this patient with aplastic anemia, most cases are not self-limited. -

Development of Plasmacytoid and Conventional Dendritic Cell Subtypes from Single Precursor Cells Derived in Vitro and in Vivo
ARTICLES Development of plasmacytoid and conventional dendritic cell subtypes from single precursor cells derived in vitro and in vivo Shalin H Naik1,2, Priyanka Sathe1,3, Hae-Young Park1,4, Donald Metcalf1, Anna I Proietto1,3, Aleksander Dakic1, Sebastian Carotta1, Meredith O’Keeffe1,4, Melanie Bahlo1, Anthony Papenfuss1, Jong-Young Kwak1,4,LiWu1 & Ken Shortman1 The development of functionally specialized subtypes of dendritic cells (DCs) can be modeled through the culture of bone marrow with the ligand for the cytokine receptor Flt3. Such cultures produce DCs resembling spleen plasmacytoid DCs (pDCs), http://www.nature.com/natureimmunology CD8+ conventional DCs (cDCs) and CD8– cDCs. Here we isolated two sequential DC-committed precursor cells from such cultures: dividing ‘pro-DCs’, which gave rise to transitional ‘pre-DCs’ en route to differentiating into the three distinct DC subtypes (pDCs, CD8+ cDCs and CD8– cDCs). We also isolated an in vivo equivalent of the DC-committed pro-DC precursor cell, which also gave rise to the three DC subtypes. Clonal analysis of the progeny of individual pro-DC precursors demonstrated that some pro-DC precursors gave rise to all three DC subtypes, some produced cDCs but not pDCs, and some were fully committed to a single DC subtype. Thus, commitment to particular DC subtypes begins mainly at this pro-DC stage. Dendritic cells (DCs) are antigen-presenting cells crucial for the innate macrophages12. Further ‘downstream’, ‘immediate’ precursors have and adaptive response to infection as well as for maintaining immune been identified for several DC types, including Ly6Chi monocytes as 3,4,6 13 Nature Publishing Group Group Nature Publishing tolerance to self tissue. -

The Biochemical and Biophysical Mechanisms of Macrophage Migration
University of Pennsylvania ScholarlyCommons Publicly Accessible Penn Dissertations 2015 The Biochemical and Biophysical Mechanisms of Macrophage Migration Laurel Erin Hind University of Pennsylvania, [email protected] Follow this and additional works at: https://repository.upenn.edu/edissertations Part of the Allergy and Immunology Commons, Biomedical Commons, Immunology and Infectious Disease Commons, and the Medical Immunology Commons Recommended Citation Hind, Laurel Erin, "The Biochemical and Biophysical Mechanisms of Macrophage Migration" (2015). Publicly Accessible Penn Dissertations. 1062. https://repository.upenn.edu/edissertations/1062 This paper is posted at ScholarlyCommons. https://repository.upenn.edu/edissertations/1062 For more information, please contact [email protected]. The Biochemical and Biophysical Mechanisms of Macrophage Migration Abstract The ability of macrophages to migrate is critical for a proper immune response. During an innate immune response, macrophages migrate to sites of infection or inflammation where they clear pathogens through phagocytosis and activate an adaptive immune response by releasing cytokines and acting as antigen- presenting cells. Unfortunately, improper regulation of macrophage migration is associated with a variety of dieases including cancer, atherosclerosis, wound-healing, and rheumatoid arthritis. In this thesis, engineered substrates were used to study the chemical and physical mechanisms of macrophage migration. We first used microcontact printing to generate surfaces -

Peripheral Blood Cells Changes After Two Groups of Splenectomy And
ns erte ion p : O y p H e f Yunfu et al., J Hypertens (Los Angel) 2018, 7:1 n o l A a DOI: 10.4172/2167-1095.1000249 c c n r e u s o s J Journal of Hypertension: Open Access ISSN: 2167-1095 Research Article Open Access Peripheral Blood Cells Changes After Two Groups of Splenectomy and Prevention and Treatment of Postoperative Complication Yunfu Lv1*, Xiaoguang Gong1, XiaoYu Han1, Jie Deng1 and Yejuan Li2 1Department of General Surgery, Hainan Provincial People's Hospital, Haikou, China 2Department of Reproductive, Maternal and Child Care of Hainan Province, Haikou, China *Corresponding author: Yunfu Lv, Department of General Surgery, Hainan Provincial People's Hospital, Haikou 570311, China, Tel: 86-898-66528115; E-mail: [email protected] Received Date: January 31, 2018; Accepted Date: March 12, 2018; Published Date: March 15, 2018 Copyright: © 2018 Lv Y, et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited. Abstract Objective: This study aimed to investigate the changes in peripheral blood cells after two groups of splenectomy in patients with traumatic rupture of the spleen and portal hypertension group, as well as causes and prevention and treatment of splenectomy related portal vein thrombosis. Methods: Clinical data from 109 patients with traumatic rupture of the spleen who underwent splenectomy in our hospital from January 2001 to August 2015 were retrospectively analyzed, and compared with those from 240 patients with splenomegaly due to cirrhotic portal hypertension who underwent splenectomy over the same period. -

Complete Blood Count in Primary Care
Complete Blood Count in Primary Care bpac nz better medicine Editorial Team bpacnz Tony Fraser 10 George Street Professor Murray Tilyard PO Box 6032, Dunedin Clinical Advisory Group phone 03 477 5418 Dr Dave Colquhoun Michele Cray free fax 0800 bpac nz Dr Rosemary Ikram www.bpac.org.nz Dr Peter Jensen Dr Cam Kyle Dr Chris Leathart Dr Lynn McBain Associate Professor Jim Reid Dr David Reith Professor Murray Tilyard Programme Development Team Noni Allison Rachael Clarke Rebecca Didham Terry Ehau Peter Ellison Dr Malcolm Kendall-Smith Dr Anne Marie Tangney Dr Trevor Walker Dr Sharyn Willis Dave Woods Report Development Team Justine Broadley Todd Gillies Lana Johnson Web Gordon Smith Design Michael Crawford Management and Administration Kaye Baldwin Tony Fraser Kyla Letman Professor Murray Tilyard Distribution Zane Lindon Lyn Thomlinson Colleen Witchall All information is intended for use by competent health care professionals and should be utilised in conjunction with © May 2008 pertinent clinical data. Contents Key points/purpose 2 Introduction 2 Background ▪ Haematopoiesis - Cell development 3 ▪ Limitations of reference ranges for the CBC 4 ▪ Borderline abnormal results must be interpreted in clinical context 4 ▪ History and clinical examination 4 White Cells ▪ Neutrophils 5 ▪ Lymphocytes 9 ▪ Monocytes 11 ▪ Basophils 12 ▪ Eosinophils 12 ▪ Platelets 13 Haemoglobin and red cell indices ▪ Low haemoglobin 15 ▪ Microcytic anaemia 15 ▪ Normocytic anaemia 16 ▪ Macrocytic anaemia 17 ▪ High haemoglobin 17 ▪ Other red cell indices 18 Summary Table 19 Glossary 20 This resource is a consensus document, developed with haematology and general practice input. We would like to thank: Dr Liam Fernyhough, Haematologist, Canterbury Health Laboratories Dr Chris Leathart, GP, Christchurch Dr Edward Theakston, Haematologist, Diagnostic Medlab Ltd We would like to acknowledge their advice, expertise and valuable feedback on this document. -

Red Blood Cell Morphology in Patients with Β-Thalassemia Minor
J Lab Med 2017; 41(1): 49–52 Short Communication Carolin Körber, Albert Wölfler, Manfred Neubauer and Christoph Robier* Red blood cell morphology in patients with β-thalassemia minor DOI 10.1515/labmed-2016-0052 Keywords: β-thalassemia minor; erythrocytes; red blood Received July 11, 2016; accepted October 20, 2016; previously published cells; red blood cell morphology. online December 10, 2016 Abstract In β-thalassemias, the examination of a peripheral blood (PB) smear may provide relevant clues to initial diagnosis. Background: A systematic analysis of the occurrence of Complete laboratory investigation consists of the determina- red blood cell (RBC) abnormalities in β-thalassemia minor tion of the complete blood count, assessment of red blood has not been performed to date. This study aimed to iden- cell (RBC) morphology, high performance liquid chroma- tify and quantify the frequency of RBC abnormalities in tography (HPLC), hemoglobin electrophoresis and, where patients with β-thalassemia minor. necessary, DNA analysis [1]. Especially in the clinically Methods: We examined blood smears of 33 patients with severe forms referred to as β-thalassemia major and interme- β-thalassemia minor by light microscopy for the occur- dia, RBC abnormalities are often markedly apparent [2]. In rence of 15 defined RBC abnormalities. In the case of posi- β-thalassemia minor, also called β-thalassemia trait, the car- tivity, the abnormal cells/20 high power fields (HPF) at riers are usually clinically asymptomatic, showing persistent 1000-fold magnification were counted. microcytosis and hypochromia or mild microcytic anemia [1, Results: Anisocytosis, poikilocytosis and target cells 3]. The PB smear may show microcytosis, hypochromia and, (median 42/20 HPF) were observed in all, and ovalocytes infrequently, poikilocytosis [2]. -

Hematological Issues in Critical Care
HEMATOLOGICAL ISSUES IN ACUTE CARE: PART A- RBC DISORDERS Dheeraj Reddy, MD Objectives- Part A To understand how various blood cell types are produced from pluripotent hematopoietic stem cells and how hematopoiesis is regulated To appreciate the importance of a thorough history and physical exam in the diagnostic approach to hematologic abnormalities Basic interpretation of peripheral blood smear Approach to RBC disorders Anemia Polycythemia Hematopoesis Production of all types of blood cells including formation, development, and differentiation of all types of blood cells. 11 12 10 –10 new blood cells are produced daily in our body to maintain steady state levels in the peripheral circulation All types of new blood cells are derived from “pluripotent stem cells” 1 Sites of Hematopoesis in pre- and postnatal periods MUCH SIMPLER! 2 Key Elements in History Weight loss Fever, night sweats (B symptoms) Fatigue, malaise, and lassitude Weakness Drugs and Chemicals Exposure Family History Sexual History Lumps and Bumps Bone Pain Skin rash/pruritus Surgical History Key Elements in Physical Exam LYMPH NODES 3 Splenomegaly Increased function Abnormal blood flow Infiltration (Congestion) Immune hyperplasia - Liver Cirrhosis Malignant - Response to infection (viral, - hepatic vein obstruction - Leukemias (acute, chronic, bacterial, fungal, parasitic) - portal vein obstruction lymphoid, and myeloid) - Disordered immunoregulation - Budd-Chiari syndrome - Lymphomas (Hodgkins and (RA, SLE, autoimmune hemolytic (associated with classical -

Single-Cell Mass Cytometry of Differential Immune and Drug
RESEARCH ARTICLE Performance assessmentofmasscytometry. The workflow for mass cytometry is comparable with that of fluorescence flow cytometry (Fig. 1A). Single-Cell Mass Cytometry of Differential Antibodies coupled to distinct, stable, transition element isotopes were used to bind target epitopes on and within cells. Cells, with bound antibody- Immune and Drug Responses Across isotope conjugates, were sprayed as single-cell droplets into an inductively coupled argon plasma a Human Hematopoietic Continuum (created by passing argon gas through an induc- tion coil with a high radio-frequency electric cur- 1 1 2 3 1 1 Sean C. Bendall, * Erin F. Simonds, * Peng Qiu, El-ad D. Amir, Peter O. Krutzik, Rachel Finck, rent) at approximately 5500 K. This vaporizes 1,7 3 1 4,5 6 Robert V. Bruggner, Rachel Melamed, Angelica Trejo, Olga I. Ornatsky, Robert S. Balderas, each cell and induces ionization of its atomic con- 2 1 3 4,5 1 Sylvia K. Plevritis, Karen Sachs, Dana Pe’er, Scott D. Tanner, Garry P. Nolan † stituents. The resulting elemental ions were then sampled by a time-of-flight (TOF) mass spectrom- Flow cytometry is an essential tool for dissecting the functional complexity of hematopoiesis. We used eter and quantified. The signal for each transi- single-cell “mass cytometry” to examine healthy human bone marrow, measuring 34 parameters tion element isotope reporter was integrated as simultaneously in single cells (binding of 31 antibodies, viability, DNA content, and relative cell size). The each cell’s constituent ions reached the detector. signaling behavior of cell subsets spanning a defined hematopoietic hierarchy was monitored with 18 Currently, TOF sampling resolution enables the simultaneous markers of functional signaling states perturbed by a set of ex vivo stimuli and inhibitors. -

Combined Effect of Granulocyte-Colony-Stimulating
J Korean Med. 2016;37(4):36-44 http://dx.doi.org/10.13048/jkm.16046 pISSN 1010-0695 • eISSN 2288-3339 Original Article Combined Effect of Granulocyte-Colony-Stimulating Factor-Induced Bone Marrow-Derived Stem Cells and Red Ginseng in Patients with Decompensated Liver Cirrhosis (Combined Effect of G-CSF and Red Ginseng in Liver Cirrhosis) Hyun Hee Kim1, Seung Mo Kim2, Kyung Soon Kim2, Min A Kwak2, Sang Gyung Kim3, Byung Seok Kim1, Chang Hyeong Lee1 1Department of Internal Medicine, Catholic University of Daegu School of Medicine 2Department of Internal Medicine, College of Korean Medicine, Daegu Haany University 3Department of Laboratory Medicine, Catholic University of Daegu School of Medicine Objectives: Granulocyte-colony-stimulating factor (G-CSF) mobilized bone marrow (BM)-derived hematopoietic stem cells could contribute to improvement of liver function. In addition, liver fibrosis can reportedly be prevented by the Rg 1 component of red ginseng. This study investigated the combined effect of G-CSF and red ginseng on decompensated liver cirrhosis. Methods: Four patients with decompensated liver cirrhosis were injected with G-CSF to proliferate BM stem cells for 4 days (5 μg/kg bid subcutaneously) and followed-up for 3 months. The patients also received red ginseng for 4 days (2 tablets tid per os). We analyzed Child-Pugh scores, Model for End-Stage Liver Disease (MELD) scores and cirrhotic complications. Results: All patients showed marked increases in White blood cell (WBC) and CD34+ cells in the peripheral blood, with a peak time of 4 days after G-CSF injection. Spleen size also increased after G-CSF injection, but not severely. -

A Study of the Neonatal Haematology of Children with Down Syndrome
A study of the neonatal haematology of children with Down syndrome Rebecca James submitted in accordance with the requirements for the degree of Doctor of Philosophy Department of Health Sciences University of York, March 2011 Abstract This thesis describes the establishment and initial findings of the Children with Down Syndrome Study, a birth cohort of children with DS. The Children with Down Syndrome Study was set up in order to characterise the haematology of neonates with Down syndrome and specifically to test the hypothesis that that this differed in this population. The study was carried out with the support of the Down Syndrome Association and the Down Syndrome Medical Interest Group, and through consultation with clinicians and families. Following a pilot study in the Yorkshire region it was established in over 60 hospitals across the north of England. The Children with Down Syndrome Study is the largest birth cohort of children with Down syndrome established to date, and this is the largest reported analysis of the haematology of neonates with Down syndrome. The results confirm that neonates with Down syndrome have a distinct haematological profile. Means and ranges for haematological parameters throughout the neonatal period are provided. The effects of gestational age, birth weight, postnatal age and the venepuncture to processing interval on the neonatal full blood count were examined, and this is the first report of factors that influence the haematological parameters in neonates with Down syndrome. In order to analyse the blood cell morphology a new approach to morphology was developed and validated. Morphological review of samples from neonates with Down syndrome demonstrated that blasts were common. -

Monocyte and Macrophage Heterogeneity
REVIEWS MONOCYTE AND MACROPHAGE HETEROGENEITY Siamon Gordon and Philip R. Taylor Abstract | Heterogeneity of the macrophage lineage has long been recognized and, in part, is a result of the specialization of tissue macrophages in particular microenvironments. Circulating monocytes give rise to mature macrophages and are also heterogeneous themselves, although the physiological relevance of this is not completely understood. However, as we discuss here, recent studies have shown that monocyte heterogeneity is conserved in humans and mice, allowing dissection of its functional relevance: the different monocyte subsets seem to reflect developmental stages with distinct physiological roles, such as recruitment to inflammatory lesions or entry to normal tissues. These advances in our understanding have implications for the development of therapeutic strategies that are targeted to modify particular subpopulations of monocytes. OSTEOCLAST Circulating monocytes give rise to a variety of tissue- elicit increased recruitment of monocytes to peripheral A multinucleate cell that resident macrophages throughout the body, as well as sites4, where differentiation into macrophages and DCs resorbs bone. to specialized cells such as dendritic cells (DCs) and occurs, contributing to host defence, and tissue remod- OSTEOCLASTS. Monocytes are known to originate in the elling and repair. Studies of the mononuclear-phagocyte bone marrow from a common myeloid progenitor that system, using monoclonal antibodies specific for vari- is shared with neutrophils, and they are then released ous cell-surface receptors and differentiation antigens, into the peripheral blood, where they circulate for have shown that there is substantial heterogeneity of several days before entering tissues and replenishing phenotype, which most probably reflects the special- the tissue macrophage populations1. -
10 11 Cyto Slides 81-85
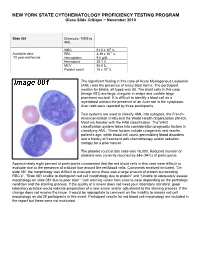
NEW YORK STATE CYTOHEMATOLOGY PROFICIENCY TESTING PROGRAM Glass Slide Critique ~ November 2010 Slide 081 Diagnosis: MDS to AML 9 WBC 51.0 x 10 /L 12 Available data: RBC 3.39 x 10 /L 72 year-old female Hemoglobin 9.6 g/dL Hematocrit 29.1 % MCV 86.0 fL Platelet count 16 x 109 /L The significant finding in this case of Acute Myelogenous Leukemia (AML) was the presence of many blast forms. The participant median for blasts, all types was 88. The blast cells in this case (Image 081) are large, irregular in shape and contain large prominent nucleoli. It is difficult to identify a blast cell as a myeloblast without the presence of an Auer rod in the cytoplasm. Auer rods were reported by three participants. Two systems are used to classify AML into subtypes, the French- American-British (FAB) and the World Health Organization (WHO). Most are familiar with the FAB classification. The WHO classification system takes into consideration prognostic factors in classifying AML. These factors include cytogenetic test results, patient’s age, white blood cell count, pre-existing blood disorders and a history of treatment with chemotherapy and/or radiation therapy for a prior cancer. The platelet count in this case was 16,000. Reduced number of platelets was correctly reported by 346 (94%) of participants. Approximately eight percent of participants commented that the red blood cells in this case were difficult to evaluate due to the presence of a bluish hue around the red blood cells. Comments received included, “On slide 081 the morphology was difficult to evaluate since there was a large amount of protein surrounding RBC’s”, “Slide 081 unable to distinguish red cell morphology due to protein” and “Unable to adequately assess morphology on slide 081 due to poor stain”.