Pierre Robin Syndrome
Total Page:16
File Type:pdf, Size:1020Kb
Load more
Recommended publications
-

FROGLOG Newsletter of the Declining Amphibian Populations Task Force
Salamandra salamandra by Franco Andreone ISSN 1026-0269 FROGLOG Newsletter of the Declining Amphibian Populations Task Force August 2004, Number 64. Meteyer et al. (2000) and Ouellet very low number of abnormalities. We (2000). only found one L. kuhlii, which may We examined a total of 4,331 have strayed from a nearby stream. frogs of 23 species and found 20 A third of abnormalities were types of deformities in 9 species of due to trauma; these included digit frogs. We divided deformities into two amputations (16% of all general types: developmental abnormalities), limb amputations (2%), abnormalities and trauma (injuries). fractured limbs (7%) and skin wounds Morphological Abnormalities in We distinguished trauma (4%). The most common Frogs of West Java, Indonesia abnormalities based on the developmental abnormalities were appearance of old scars or, if they digital (43%) and, of these, By Mirza D. Kusrini, Ross A. Alford, involved digits, the occurrence of brachydactyly (16.3%), syndactyly Anisa Fitri, Dede M. Nasir, Sumantri digital re-growth. Developmental (14.6%) and ectrodactyly (11.4%) Rahardyansah abnormalities occurred in limbs were the three most common. In recent decades, amphibian (amelia, micromelia, brachymelia, The oldest specimen of F. deformities have generated public hemimelia, ectromelia, taumelia, cuta- limnocharis stored in the MZB that interest as high incidences have been neous fusions), digits (ectrodactyly, exhibited abnormalities was a juvenile found in several locations, notably in brachydactyly, syndactyly, polydactyly, frog captured on 16 November 1921 North America (Helgen et al., 1998; clinodactyly), the back-bone (scoli- from Bogor without one leg (amelia) Ouellet, 2000). The only report on the osis), the eyes (anophthalmy) and the (ID057.10). -

Genetics of Congenital Hand Anomalies
G. C. Schwabe1 S. Mundlos2 Genetics of Congenital Hand Anomalies Die Genetik angeborener Handfehlbildungen Original Article Abstract Zusammenfassung Congenital limb malformations exhibit a wide spectrum of phe- Angeborene Handfehlbildungen sind durch ein breites Spektrum notypic manifestations and may occur as an isolated malforma- an phänotypischen Manifestationen gekennzeichnet. Sie treten tion and as part of a syndrome. They are individually rare, but als isolierte Malformation oder als Teil verschiedener Syndrome due to their overall frequency and severity they are of clinical auf. Die einzelnen Formen kongenitaler Handfehlbildungen sind relevance. In recent years, increasing knowledge of the molecu- selten, besitzen aber aufgrund ihrer Häufigkeit insgesamt und lar basis of embryonic development has significantly enhanced der hohen Belastung für Betroffene erhebliche klinische Rele- our understanding of congenital limb malformations. In addi- vanz. Die fortschreitende Erkenntnis über die molekularen Me- tion, genetic studies have revealed the molecular basis of an in- chanismen der Embryonalentwicklung haben in den letzten Jah- creasing number of conditions with primary or secondary limb ren wesentlich dazu beigetragen, die genetischen Ursachen kon- involvement. The molecular findings have led to a regrouping of genitaler Malformationen besser zu verstehen. Der hohe Grad an malformations in genetic terms. However, the establishment of phänotypischer Variabilität kongenitaler Handfehlbildungen er- precise genotype-phenotype correlations for limb malforma- schwert jedoch eine Etablierung präziser Genotyp-Phänotyp- tions is difficult due to the high degree of phenotypic variability. Korrelationen. In diesem Übersichtsartikel präsentieren wir das We present an overview of congenital limb malformations based Spektrum kongenitaler Malformationen, basierend auf einer ent- 85 on an anatomic and genetic concept reflecting recent molecular wicklungsbiologischen, anatomischen und genetischen Klassifi- and developmental insights. -

Syndromic Ear Anomalies and Renal Ultrasounds
Syndromic Ear Anomalies and Renal Ultrasounds Raymond Y. Wang, MD*; Dawn L. Earl, RN, CPNP‡; Robert O. Ruder, MD§; and John M. Graham, Jr, MD, ScD‡ ABSTRACT. Objective. Although many pediatricians cific MCA syndromes that have high incidences of renal pursue renal ultrasonography when patients are noted to anomalies. These include CHARGE association, Townes- have external ear malformations, there is much confusion Brocks syndrome, branchio-oto-renal syndrome, Nager over which specific ear malformations do and do not syndrome, Miller syndrome, and diabetic embryopathy. require imaging. The objective of this study was to de- Patients with auricular anomalies should be assessed lineate characteristics of a child with external ear malfor- carefully for accompanying dysmorphic features, includ- mations that suggest a greater risk of renal anomalies. We ing facial asymmetry; colobomas of the lid, iris, and highlight several multiple congenital anomaly (MCA) retina; choanal atresia; jaw hypoplasia; branchial cysts or syndromes that should be considered in a patient who sinuses; cardiac murmurs; distal limb anomalies; and has both ear and renal anomalies. imperforate or anteriorly placed anus. If any of these Methods. Charts of patients who had ear anomalies features are present, then a renal ultrasound is useful not and were seen for clinical genetics evaluations between only in discovering renal anomalies but also in the diag- 1981 and 2000 at Cedars-Sinai Medical Center in Los nosis and management of MCA syndromes themselves. Angeles and Dartmouth-Hitchcock Medical Center in A renal ultrasound should be performed in patients with New Hampshire were reviewed retrospectively. Only pa- isolated preauricular pits, cup ears, or any other ear tients who underwent renal ultrasound were included in anomaly accompanied by 1 or more of the following: the chart review. -
Macrocephaly Information Sheet 6-13-19
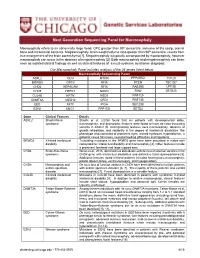
Next Generation Sequencing Panel for Macrocephaly Clinical Features: Macrocephaly refers to an abnormally large head, OFC greater than 98th percentile, inclusive of the scalp, cranial bone and intracranial contents. Megalencephaly, brain weight/volume ratio greater than 98th percentile, results from true enlargement of the brain parenchyma [1]. Megalencephaly is typically accompanied by macrocephaly, however macrocephaly can occur in the absence of megalencephaly [2]. Both macrocephaly and megalencephaly can been seen as isolated clinical findings as well as clinical features of a mutli-systemic syndromic diagnosis. Our Macrocephaly Panel includes analysis of the 36 genes listed below. Macrocephaly Sequencing Panel ASXL2 GLI3 MTOR PPP2R5D TCF20 BRWD3 GPC3 NFIA PTEN TBC1D7 CHD4 HEPACAM NFIX RAB39B UPF3B CHD8 HERC1 NONO RIN2 ZBTB20 CUL4B KPTN NSD1 RNF125 DNMT3A MED12 OFD1 RNF135 EED MITF PIGA SEC23B EZH2 MLC1 PPP1CB SETD2 Gene Clinical Features Details ASXL2 Shashi-Pena Shashi et al. (2016) found that six patients with developmental delay, syndrome macrocephaly, and dysmorphic features were found to have de novo truncating variants in ASXL2 [3]. Distinguishing features were macrocephaly, absence of growth retardation, and variability in the degree of intellectual disabilities The phenotype also consisted of prominent eyes, arched eyebrows, hypertelorism, a glabellar nevus flammeus, neonatal feeding difficulties and hypotonia. BRWD3 X-linked intellectual Truncating mutations in the BRWD3 gene have been described in males with disability nonsyndromic intellectual disability and macrocephaly [4]. Other features include a prominent forehead and large cupped ears. CHD4 Sifrim-Hitz-Weiss Weiss et al., 2016, identified five individuals with de novo missense variants in the syndrome CHD4 gene with intellectual disabilities and distinctive facial dysmorphisms [5]. -

Massachusetts Birth Defects 2002-2003
Massachusetts Birth Defects 2002-2003 Massachusetts Birth Defects Monitoring Program Bureau of Family Health and Nutrition Massachusetts Department of Public Health January 2008 Massachusetts Birth Defects 2002-2003 Deval L. Patrick, Governor Timothy P. Murray, Lieutenant Governor JudyAnn Bigby, MD, Secretary, Executive Office of Health and Human Services John Auerbach, Commissioner, Massachusetts Department of Public Health Sally Fogerty, Director, Bureau of Family Health and Nutrition Marlene Anderka, Director, Massachusetts Center for Birth Defects Research and Prevention Linda Casey, Administrative Director, Massachusetts Center for Birth Defects Research and Prevention Cathleen Higgins, Birth Defects Surveillance Coordinator Massachusetts Department of Public Health 617-624-5510 January 2008 Acknowledgements This report was prepared by the staff of the Massachusetts Center for Birth Defects Research and Prevention (MCBDRP) including: Marlene Anderka, Linda Baptiste, Elizabeth Bingay, Joe Burgio, Linda Casey, Xiangmei Gu, Cathleen Higgins, Angela Lin, Rebecca Lovering, and Na Wang. Data in this report have been collected through the efforts of the field staff of the MCBDRP including: Roberta Aucoin, Dorothy Cichonski, Daniel Sexton, Marie-Noel Westgate and Susan Winship. We would like to acknowledge the following individuals for their time and commitment to supporting our efforts in improving the MCBDRP. Lewis Holmes, MD, Massachusetts General Hospital Carol Louik, ScD, Slone Epidemiology Center, Boston University Allen Mitchell, -

Guidelines for Conducting Birth Defects Surveillance
NATIONAL BIRTH DEFECTS PREVENTION NETWORK HTTP://WWW.NBDPN.ORG Guidelines for Conducting Birth Defects Surveillance Edited By Lowell E. Sever, Ph.D. June 2004 Support for development, production, and distribution of these guidelines was provided by the Birth Defects State Research Partnerships Team, National Center on Birth Defects and Developmental Disabilities, Centers for Disease Control and Prevention Copies of Guidelines for Conducting Birth Defects Surveillance can be viewed or downloaded from the NBDPN website at http://www.nbdpn.org/bdsurveillance.html. Comments and suggestions on this document are welcome. Submit comments to the Surveillance Guidelines and Standards Committee via e-mail at [email protected]. You may also contact a member of the NBDPN Executive Committee by accessing http://www.nbdpn.org and then selecting Network Officers and Committees. Suggested citation according to format of Uniform Requirements for Manuscripts ∗ Submitted to Biomedical Journals:∗ National Birth Defects Prevention Network (NBDPN). Guidelines for Conducting Birth Defects Surveillance. Sever, LE, ed. Atlanta, GA: National Birth Defects Prevention Network, Inc., June 2004. National Birth Defects Prevention Network, Inc. Web site: http://www.nbdpn.org E-mail: [email protected] ∗International Committee of Medical Journal Editors. Uniform requirements for manuscripts submitted to biomedical journals. Ann Intern Med 1988;108:258-265. We gratefully acknowledge the following individuals and organizations who contributed to developing, writing, editing, and producing this document. NBDPN SURVEILLANCE GUIDELINES AND STANDARDS COMMITTEE STEERING GROUP Carol Stanton, Committee Chair (CO) Larry Edmonds (CDC) F. John Meaney (AZ) Glenn Copeland (MI) Lisa Miller-Schalick (MA) Peter Langlois (TX) Leslie O’Leary (CDC) Cara Mai (CDC) EDITOR Lowell E. -

CASE REPORT Radiographic Diagnosis of a Rare Case Of
CASE REPORT Radiographic diagnosis of a rare case of oculodentodigital dysplasia Umesh Chandra Parashari, M.D. Sachin Khanduri, M.D. Samarjit Bhadury, M.D. Fareena Akbar Qayyum, M.B.B.S. Department of Radiodiagnosis, Lucknow Medical College, Lucknow, Uttar Pradesh, India Corresponding author: U Parashari ([email protected]) Abstract Oculodentodigital dysplasia (ODDD), also known as oculodento- osseous dysplasia, is an extremely rare autosomal dominant disorder with high penetrance, intra- and interfamilial phenotypic variability, and advanced paternal age in sporadic cases. The incidence of this disease is not precisely known, with only 243 cases reported in the scientific literature, suggesting an incidence of around 1 in 10 million people. It is marked mainly by eye abnormalities, craniofacial dysmorphism, dental anomalies, hand and foot malformations, various skeletal defects, and mildly Fig. 1. Photograph of the patient at age one year (1A) and 16 years (1B and 1C) showing hypotrichosis and pili annulati. The face is small with narrow delayed mental development. Neurological changes may appear eyes, thin nose, prominent columella and wide mandible. The fingers are earlier in each subsequent generation. This case report describes underdeveloped and deformed. a radiological diagnosis of ODDD based on physical appearance, clinical features and radiographic findings in a 16-year-old girl. Case report A 16-year-old girl presented to the hospital with complaints of weakness Introduction in her lower limbs, abnormal dentition and bladder incontinence. On Oculodentodigital dysplasia (ODDD) is a condition that affects many general examination, her gait was ataxic with moderate spasticity in parts of the body, particularly the eyes, teeth and fingers, as the both legs. -

Polydactyly of the Hand
A Review Paper Polydactyly of the Hand Katherine C. Faust, MD, Tara Kimbrough, BS, Jean Evans Oakes, MD, J. Ollie Edmunds, MD, and Donald C. Faust, MD cleft lip/palate, and spina bifida. Thumb duplication occurs in Abstract 0.08 to 1.4 per 1000 live births and is more common in Ameri- Polydactyly is considered either the most or second can Indians and Asians than in other races.5,10 It occurs in a most (after syndactyly) common congenital hand ab- male-to-female ratio of 2.5 to 1 and is most often unilateral.5 normality. Polydactyly is not simply a duplication; the Postaxial polydactyly is predominant in black infants; it is most anatomy is abnormal with hypoplastic structures, ab- often inherited in an autosomal dominant fashion, if isolated, 1 normally contoured joints, and anomalous tendon and or in an autosomal recessive pattern, if syndromic. A prospec- ligament insertions. There are many ways to classify tive San Diego study of 11,161 newborns found postaxial type polydactyly, and surgical options range from simple B polydactyly in 1 per 531 live births (1 per 143 black infants, excision to complicated bone, ligament, and tendon 1 per 1339 white infants); 76% of cases were bilateral, and 3 realignments. The prevalence of polydactyly makes it 86% had a positive family history. In patients of non-African descent, it is associated with anomalies in other organs. Central important for orthopedic surgeons to understand the duplication is rare and often autosomal dominant.5,10 basic tenets of the abnormality. Genetics and Development As early as 1896, the heritability of polydactyly was noted.11 As olydactyly is the presence of extra digits. -

Information About Pierre Robin Sequence/Complex
Information about Pierre Robin Sequence/Complex What is Pierre Robin Sequence/Complex? How common is this condition? Pierre Robin Sequence or Complex (pronounced “Roban”) is the name given to a birth condition that Robin Sequence/Complex is rather uncommon. involves the lower jaw being either small in size Frequency estimates range from 1 in 2,000 to 30,000 (micrognathia) or set back from the upper jaw births, based on how strictly the condition is defined. (retrognathia). As a result, the tongue tends to be In contrast, cleft lip and/or palate occurs once in displaced back towards the throat, where it can fall every 700 live births. back and obstruct the airway (glossoptosis). Most infants, but not all, will also have a cleft palate, but Will future children be affected? none will have a cleft lip. It is important to understand that Robin Over the years, there have been several names given Sequence/Complex can occur by itself (described as to the condition, including Pierre Robin Syndrome, “isolated”) or as a feature of another syndrome. Pierre Robin Triad, and Robin Anomalad. Based on Parents who have had one child with isolated Robin the varying features and causes of the condition, Sequence probably have between 1 and 5% chance either “Robin Sequence” or “Robin Complex” may of having another child with this condition. There be an appropriate description for a specific patient. have not yet been enough large-scale studies to make Pierre Robin was a French physician who first more accurate predictions. reported the combination of small lower jaw, cleft palate, and tongue displacement in 1923. -

A Progressive and Complex Clinical Course in Two Family Members With
Körberg et al. BMC Medical Genetics (2020) 21:90 https://doi.org/10.1186/s12881-020-01015-z CASE REPORT Open Access A progressive and complex clinical course in two family members with ERF-related craniosynostosis: a case report Izabella Körberg1*, Daniel Nowinski2, Marie-Louise Bondeson1, Malin Melin1, Lars Kölby3 and Eva-Lena Stattin1 Abstract Background: ERF-related craniosynostosis are a rare, complex, premature trisutural fusion associated with a broad spectrum of clinical features and heterogeneous aetiology. Here we describe two cases with the same pathogenic variant and a detailed description of their clinical course. Case presentation: Two subjects; a boy with a BLSS requiring repeated skull expansions and his mother who had been operated once for sagittal synostosis. Both developed intracranial hypertension at some point during the course, which was for both verified by formal invasive intracranial pressure monitoring. Exome sequencing revealed a pathogenic truncating frame shift variant in the ERF gene. Conclusions: Here we describe a boy and his mother with different craniosynostosis patterns, but both with verified intracranial hypertension and heterozygosity for a truncating variant of ERF c.1201_1202delAA (p.Lys401Glufs*10). Our work provides supplementary evidence in support of previous phenotypic descriptions of ERF-related craniosynostosis, particularly late presentation, an evolving synostotic pattern and variable expressivity even among affected family members. Keywords: ERF, Craniosynostosis, Intracranial hypertension Background pressure and intellectual disability. It is usually classified Craniosynostosis (CS) is clinically and genetically a based on suture fusion type: sagittal, metopic, bi−/unicor- heterogenous congenital anomaly with an incidence of 1 onal, bi−/unilambdoid and complex, or multisutural. -

Familial Poland Anomaly
J Med Genet: first published as 10.1136/jmg.19.4.293 on 1 August 1982. Downloaded from Journal ofMedical Genetics, 1982, 19, 293-296 Familial Poland anomaly T J DAVID From the Department of Child Health, University of Manchester, Booth Hall Children's Hospital, Manchester SUMMARY The Poland anomaly is usually a non-genetic malformation syndrome. This paper reports two second cousins who both had a typical left sided Poland anomaly, and this constitutes the first recorded case of this condition affecting more than one member of a family. Despite this, for the purposes of genetic counselling, the Poland anomaly can be regarded as a sporadic condition with an extremely low recurrence risk. The Poland anomaly comprises congenital unilateral slightly reduced. The hands were normal. Another absence of part of the pectoralis major muscle in son (Greif himself) said that his own left pectoralis combination with a widely varying spectrum of major was weaker than the right. "Although the ipsilateral upper limb defects.'-4 There are, in difference is obvious, the author still had to carry addition, patients with absence of the pectoralis out his military duties"! major in whom the upper limbs are normal, and Trosev and colleagues9 have been widely quoted as much confusion has been caused by the careless reporting familial cases of the Poland anomaly. labelling of this isolated defect as the Poland However, this is untrue. They described a mother anomaly. It is possible that the two disorders are and child with autosomal dominant radial sided part of a single spectrum, though this has never been upper limb defects. -

Current Advances in Holt-Oram Syndrome Taosheng Huang, MD, Phd
Current advances in Holt-Oram syndrome Taosheng Huang, MD, PhD Holt-Oram syndrome is an autosomal-dominant condition Clinical features characterized by congenital cardiac and forelimb anomalies. It Holt and Oram first described this syndrome when they is caused by mutations of the TBX5 gene, a member of the reported on a family with atrial septal defects and con- T-box family that encodes a transcription factor. Molecular genital anomalies of the thumbs [1]. Since then, about studies have demonstrated that mutations predicted to create 200 clinical papers have been published that further de- null alleles cause substantial abnormalities in both the limbs lineate the clinical features of Holt-Oram syndrome and heart, and that missense mutations of TBX5 can produce (HOS). The prevalence of HOS is 1 of 100,000 live distinct phenotypes. One class of missense mutations causes births, and it occurs with wide ethnic and geographic significant cardiac malformations but only minor skeletal distribution. Its clinical manifestations have proved to be abnormalities; others might cause extensive upper limb variable [2,3•,4•], but with complete penetrance. All pa- malformations but less significant cardiac abnormalities. tients with HOS have upper limb anomaly and about Intrafamilial variations of the malformations strongly suggest 85% to 95% have cardiac malformation. On the basis of that genetic background or modifier genes play an important these findings, the criteria for diagnosis include either role in the phenotypic expression of HOS. Efforts to the presence of cardiac malformations, conduction de- understand the intracellular pathway of TBX5 would provide a fects and radial ray abnormalities (or both) in an indi- unique window onto the molecular basis of common vidual, or the presence of radial ray abnormalities with or congenital heart diseases and limb malformations.