Aortic Valve Stenosis and Regurgitation
Total Page:16
File Type:pdf, Size:1020Kb
Load more
Recommended publications
-

Antithrombotic Therapy in Atrial Fibrillation Associated with Valvular Heart Disease
Europace (2017) 0, 1–21 EHRA CONSENSUS DOCUMENT doi:10.1093/europace/eux240 Antithrombotic therapy in atrial fibrillation associated with valvular heart disease: a joint consensus document from the European Heart Rhythm Association (EHRA) and European Society of Cardiology Working Group on Thrombosis, endorsed by the ESC Working Group on Valvular Heart Disease, Cardiac Arrhythmia Society of Southern Africa (CASSA), Heart Rhythm Society (HRS), Asia Pacific Heart Rhythm Society (APHRS), South African Heart (SA Heart) Association and Sociedad Latinoamericana de Estimulacion Cardıaca y Electrofisiologıa (SOLEACE) Gregory Y. H. Lip1*, Jean Philippe Collet2, Raffaele de Caterina3, Laurent Fauchier4, Deirdre A. Lane5, Torben B. Larsen6, Francisco Marin7, Joao Morais8, Calambur Narasimhan9, Brian Olshansky10, Luc Pierard11, Tatjana Potpara12, Nizal Sarrafzadegan13, Karen Sliwa14, Gonzalo Varela15, Gemma Vilahur16, Thomas Weiss17, Giuseppe Boriani18 and Bianca Rocca19 Document Reviewers: Bulent Gorenek20 (Reviewer Coordinator), Irina Savelieva21, Christian Sticherling22, Gulmira Kudaiberdieva23, Tze-Fan Chao24, Francesco Violi25, Mohan Nair26, Leandro Zimerman27, Jonathan Piccini28, Robert Storey29, Sigrun Halvorsen30, Diana Gorog31, Andrea Rubboli32, Ashley Chin33 and Robert Scott-Millar34 * Corresponding author. Tel/fax: þ44 121 5075503. E-mail address: [email protected] Published on behalf of the European Society of Cardiology. All rights reserved. VC The Author 2017. For permissions, please email: [email protected]. 2 G.Y.H. Lip 1Institute of Cardiovascular Sciences, University of Birmingham and Aalborg Thrombosis Research Unit, Department of Clinical Medicine, Aalborg University, Denmark (Chair, representing EHRA); 2Sorbonne Universite´ Paris 6, ACTION Study Group, Institut De Cardiologie, Groupe Hoˆpital Pitie´-Salpetrie`re (APHP), INSERM UMRS 1166, Paris, France; 3Institute of Cardiology, ‘G. -

Cardiovascular Magnetic Resonance Pocket Guide
Series Editors Bernhard A. Herzog John P. Greenwood Sven Plein Cardiovascular Magnetic Resonance Congenital Heart Disease Pocket Guide Bernhard A. Herzog Ananth Kidambi George Ballard First Edition 2014 Congenital Pocket Guide Tetralogy / Foreword Pulmonary Atresia Standard Views TGA Difficult Scans Single Ventricle Sequential Ebstein Anomaly Segmental Analysis Coronary Artery Shunts Anomalies AV Disease / References Aortic Coarctation Terminology Series Editors Authors Bernhard A. Herzog Bernhard A. Herzog John P. Greenwood Ananth Kidambi Sven Plein George Ballard Foreword The role of cardiovascular magnetic resonance (CMR) in evaluating the adult population with congenital heart disease continues to expand. This pocket guide aims to provide a day-to-day companion for those new to congenital CMR and for those looking for a quick reference guide in routine practice. The booklet gives an overview of the most common abnormalities and interventions as well as post-operative complications. It also provides typical scan protocols, key issues and a guide for reporting for each topic. Bernhard A. Herzog Ananth Kidambi George Ballard The Cardiovascular Magnetic Resonance Pocket Guide represents the views of the ESC Working Group on Cardiovascular Magnetic Resonance and was arrived at after careful consideration of the available evidence at the time it was written. Health professionals are encouraged to take it fully into account when exercising their clinical judgment. This pocket guide does not, however, override the individual responsibility of health professionals to make appropriate decisions in the circumstances of the individual patients, in consultation with that patient and, where appropriate and necessary, the patient's guardian or carer. It is also the health professional's responsibility to verify the applicable rules and regulations applicable to drugs and devices at the time of prescription. -

Avalus™ Pericardial Aortic Surgical Valve System
FACT SHEET Avalus™ Pericardial Aortic Surgical Valve System Aortic stenosis is a common heart problem caused by a narrowing of the heart’s aortic valve due to excessive calcium deposited on the valve leaflets. When the valve narrows, it does not open or close properly, making the heart work harder to pump blood throughout the body. Eventually, this causes the heart to weaken and function poorly, which may lead to heart failure and increased risk for sudden cardiac death. Disease The standard treatment for patients with aortic valve disease is surgical aortic valve Overview: replacement (SAVR). During this procedure, a surgeon will make an incision in the sternum to open the chest and expose the heart. The diseased native valve is then Aortic removed and a new artificial valve is inserted. Once in place, the device is sewn into Stenosis the aorta and takes over the original valve’s function to enable oxygen-rich blood to flow efficiently out of the heart. For patients that are unable to undergo surgical aortic valve replacement, or prefer a minimally-invasive therapy option, an alternative procedure to treat severe aortic stenosis is called transcatheter aortic valve replacement (TAVR). The Avalus Pericardial Aortic Surgical Valve System is a next- generation aortic surgical valve from Medtronic, offering advanced design concepts and unique features for the millions of patients with severe aortic stenosis who are candidates for open- heart surgery. The Avalus Surgical Valve The Avalus valve, made of bovine tissue, is also the only stented surgical aortic valve on the market that is MRI-safe (without restrictions) enabling patients with severe aortic stenosis who have the Avalus valve to undergo screening procedures for potential co-morbidities. -
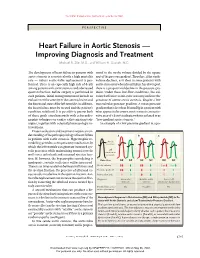
Heart Failure in Aortic Stenosis — Improving Diagnosis and Treatment Michael R
The new england journal of medicine perspective Heart Failure in Aortic Stenosis — Improving Diagnosis and Treatment Michael R. Zile, M.D., and William H. Gaasch, M.D. The development of heart failure in patients with tional to the stroke volume divided by the square aortic stenosis is associated with a high mortality root of the pressure gradient. Therefore, if the stroke rate — unless aortic-valve replacement is per- volume declines, as it does in some patients with formed. There is an especially high risk of death aortic stenosis in whom heart failure has developed, among patients with aortic stenosis and a decreased there is a proportional decline in the pressure gra- ejection fraction. Before surgery is performed in dient. Under these low-flow conditions, the cal- such patients, initial management must include an culated effective aortic-valve area may indicate the evaluation of the severity of the stenotic lesion and presence of severe aortic stenosis, despite a low the functional state of the left ventricle; in addition, transvalvular pressure gradient. A mean pressure the heart failure must be treated and the patient’s gradient that is less than 30 mm Hg in a patient with condition stabilized. It is possible to pursue both what appears to be severe aortic stenosis (an aortic- of these goals simultaneously with echocardio- valve area of <1 cm2) indicates what is referred to as graphic techniques or cardiac catheterization tech- “low-gradient aortic stenosis.” niques, together with selected pharmacologic in- An example of a low pressure gradient in a pa- terventions. Proper evaluation and treatment require an un- derstanding of the pathophysiology of heart failure ABC in patients with aortic stenosis. -

Norepinephrine Induced Pulmonary Congestion in Patients with Aortic Valve Regurgitation
NOREPINEPHRINE INDUCED PULMONARY CONGESTION IN PATIENTS WITH AORTIC VALVE REGURGITATION Timothy J. Regan, … , Kenan Binak, Harper K. Hellems J Clin Invest. 1959;38(9):1564-1571. https://doi.org/10.1172/JCI103935. Research Article Find the latest version: https://jci.me/103935/pdf NOREPINEPHRINE INDUCED PULMONARY CONGESTION IN PATIENTS WITH AORTIC VALVE REGURGITATION * By TIMOTHY J. REGAN, VALENTINO DEFAZIO, KENAN BINAKt AND HARPER K. HELLEMS (From the Cardiovascular Research Laboratories, Departments of Medicine, Wayne State Uni- versity College of Medicine, and City of Detroit Receiving Hospital, Detroit, Mich.) (Submitted for publication March 3, 1959; accepted May 14, 1959) The regulation of venous blood flow into the METHODS heart and the effects of blood volume redistribution All subjects were studied in the fasting state approxi- upon cardiac function have not been amply defined. mately two hours after receiving 0.1 Gm. of pentobarbital While enhanced venomotor tone induced by nor- sodium. A double lumen catheter was used to measure epinephrine has been found to increase the volume pressures simultaneously from the pulmonary "capillary" and pulmonary artery. The "capillary" position was as- of a central reservoir in the dog (1), such a vol- sumed to be present when the catheter could not be ad- ume shift has not been demonstrated in man, ex- vanced farther in the lung bed, the tip did not move with cept inferentially by the finding of a decrease in the cardiac cycle and a compatible pressure pattern was the limb venous volume (2). obtained. A specimen of blood saturated with oxygen This type of alteration might be expected to af- was secured from the wedged catheter tip whenever this particularly was possible. -

(BP1–BP2) Deletion in the UK Biobank
European Journal of Human Genetics (2020) 28:1265–1273 https://doi.org/10.1038/s41431-020-0626-8 ARTICLE Association of congenital cardiovascular malformation and neuropsychiatric phenotypes with 15q11.2 (BP1–BP2) deletion in the UK Biobank 1 1 2 1 1 1 Simon G. Williams ● Apostol Nakev ● Hui Guo ● Simon Frain ● Gennadiy Tenin ● Anna Liakhovitskaia ● 3 3 4 1 Priyanka Saha ● James R. Priest ● Kathryn E. Hentges ● Bernard D. Keavney Received: 3 September 2019 / Revised: 12 February 2020 / Accepted: 24 March 2020 / Published online: 23 April 2020 © The Author(s) 2020. This article is published with open access Abstract Deletion of a non-imprinted 500kb genomic region at chromosome 15q11.2, between breakpoints 1 and 2 of the Prader–Willi/ Angelman locus (BP1–BP2 deletion), has been associated in previous studies with phenotypes including congenital cardiovascular malformations (CVM). Previous studies investigating association between BP1–BP2 deletion and CVM have tended to recruit cases with rarer and more severe CVM phenotypes; the impact of CVM on relatively unselected population cohorts, anticipated to contain chiefly less severe but commoner CHD phenotypes, is relatively unexplored. More precisely 1234567890();,: 1234567890();,: defining the impact of BP1–BP2 deletion on CVM risk could be useful to guide genetic counselling, since the deletion is frequently identified in the neurodevelopmental clinic. Using the UK Biobank (UKB) cohort of ~500,000 individuals, we identified individuals with CVM and investigated the association with deletions at the BP1–BP2 locus. In addition, we assessed the association of BP1–BP2 deletions with neuropsychiatric diagnoses, cognitive function and academic achievement. Cases of CVM had an increased prevalence of the deletion compared with controls (0.64%; OR = 1.73 [95% CI 1.08–2.75]; p = 0.03), as did those with neuropsychiatric diagnoses (0.68%; OR = 1.84 [95% CI 1.23–2.75]; p = 0.004). -

Accuracy of the Single Cycle Length Method for Calculation of Aortic Effective Orifice Area in Irregular Heart Rhythms
AORTIC STENOSIS Accuracy of the Single Cycle Length Method for Calculation of Aortic Effective Orifice Area in Irregular Heart Rhythms Kerry A. Esquitin, MD, Omar K. Khalique, MD, Qi Liu, MD, Susheel K. Kodali, MD, Leo Marcoff, MD, Tamim M. Nazif, MD, Isaac George, MD, Torsten P. Vahl, MD, Martin B. Leon, MD, and Rebecca T. Hahn, MD, New York, New York; and Morristown, New Jersey Introduction: In irregular heart rhythms, echocardiographic calculation of aortic effective orifice area (EOA) re- quires averaging measurements from multiple cardiac cycles. Whether a single cycle length method can be used to calculate aortic EOA in aortic stenosis with nonsinus rhythms is not known. Methods: Transthoracic echocardiograms of 100 patients with aortic stenosis and either atrial fibrillation (AF) or frequent ectopy (FE) were retrospectively reviewed. The aortic valve velocity time integral (VTIAV) and the left ven- tricular outflow tract VTI (VTILVOT) were measured by two methods: the standard method (averaging multiple beats) and the single cycle length method. The latter matches the R-R intervals for VTIAV and VTILVOT.Stroke volume, EOA, and Doppler velocity index were calculated by both methods in all patients. The single cycle length method was used for short and long R-R cycles in AF and for postectopic beats (long R-R cycles) in FE. Results: In AF, long R-R cycles resulted in larger stroke volumes (73 6 21 vs 63 6 18 mL; P # .0001) but no difference in EOA (0.84 6 0.27 vs 0.82 6 0.27 cm2; P = .11), whereas short R-R cycles resulted in smaller stroke volumes (55 6 18 vs 63 6 18 mL, P # .0001) but a larger EOA (0.86 6 0.28 vs 0.82 6 0.27 cm2; P = .01). -

Imaging and Impact of Myocardial Fibrosis in Aortic Stenosis
JACC: CARDIOVASCULAR IMAGING VOL. 12, NO. 2, 2019 ª 2019 THE AUTHORS. PUBLISHED BY ELSEVIER ON BEHALF OF THE AMERICAN COLLEGE OF CARDIOLOGY FOUNDATION. THIS IS AN OPEN ACCESS ARTICLE UNDER THE CC BY LICENSE (http://creativecommons.org/licenses/by/4.0/). FOCUS ISSUE: IMAGING IN AORTIC STENOSIS: PART II STATE-OF-THE-ART PAPER Imaging and Impact of Myocardial Fibrosis in Aortic Stenosis a b a c Rong Bing, MBBS, BMEDSCI, João L. Cavalcante, MD, Russell J. Everett, MD, BSC, Marie-Annick Clavel, DVM, PHD, a a David E. Newby, DM, PHD, DSC, Marc R. Dweck, MD, PHD ABSTRACT Aortic stenosis is characterized both by progressive valve narrowing and the left ventricular remodeling response that ensues. The only effective treatment is aortic valve replacement, which is usually recommended in patients with severe stenosis and evidence of left ventricular decompensation. At present, left ventricular decompensation is most frequently identified by the development of typical symptoms or a marked reduction in left ventricular ejection fraction <50%. However, there is growing interest in using the assessment of myocardial fibrosis as an earlier and more objective marker of left ventricular decompensation, particularly in asymptomatic patients, where guidelines currently rely on non- randomized data and expert consensus. Myocardial fibrosis has major functional consequences, is the key pathological process driving left ventricular decompensation, and can be divided into 2 categories. Replacement fibrosis is irreversible and identified using late gadolinium enhancement on cardiac magnetic resonance, while diffuse fibrosis occurs earlier, is potentially reversible, and can be quantified with cardiac magnetic resonance T1 mapping techniques. There is a substantial body of observational data in this field, but there is now a need for randomized clinical trials of myocardial imaging in aortic stenosis to optimize patient management. -

Pathology of the Aortic Valve: Aortic Valve Stenosis/Aortic Regurgitation
Current Cardiology Reports (2019) 21: 81 https://doi.org/10.1007/s11886-019-1162-4 STRUCTURAL HEART DISEASE (RJ SIEGEL AND NC WUNDERLICH, SECTION EDITORS) Pathology of the Aortic Valve: Aortic Valve Stenosis/Aortic Regurgitation Gregory A. Fishbein1 & Michael C. Fishbein1 Published online: 5 July 2019 # Springer Science+Business Media, LLC, part of Springer Nature 2019 Abstract Purpose of Review This discussion is intended to review the anatomy and pathology of the aortic valve and aortic root region, and to provide a basis for the understanding of and treatment of the important life-threatening diseases that affect the aortic valve. Recent Findings The most exciting recent finding is that less invasive methods are being developed to treat diseases of the aortic valve. There are no medical cures for aortic valve diseases. Until recently, open-heart surgery was the only effective method of treatment. Now percutaneous approaches to implant bioprosthetic valves into failed native or previously implanted bioprosthetic valves are being developed and utilized. A genetic basis for many of the diseases that affect the aortic valve is being discovered that also should lead to innovative approaches to perhaps prevent these disease. Sequencing of ribosomal RNA is assisting in identifying organisms causing endocarditis, leading to more effective antimicrobial therapy. Summary There is exciting, expanding, therapeutic innovation in the treatment of aortic valve disease. Keywords Aortic stenosis . Aortic regurgitation . Calcific degeneration . Bicuspid aortic valve . Rheumatic valve disease . Endocarditis . Transcatheter aortic valve implantation (TAVI) . Aortic valve replacement . Myxomatous degeneration . Endocarditis . Non-bacterial thrombotic endocarditis (NBME) Introduction aortic valve disease; however, effective methods of valve repair and replacement exist and percutaneous approaches Hemodynamically significant aortic valve disease, in one to treat aortic valve disease are being utilized with increasing form or another, is a relatively common disorder. -

Evaluation of the Mitral and Aortic Valves with Cardiac CT Angiography
PICTORIAL ESSAY Evaluation of the Mitral and Aortic Valves With Cardiac CT Angiography Samir V. Chheda, BS, Monvadi B. Srichai, MD, Robert Donnino, MD, Danny C. Kim, MD, Ruth P. Lim, MBBS, and Jill E. Jacobs, MD annulus shares structural continuity with the aortic annulus Abstract: Cardiac computed tomographic angiography (CTA) through 3 fibrous trigones (Fig. 1). Owing to this anatomic using multidetector computed tomographic scanners has proven to connection, diseases of the mitral annulus can affect the be a reliable technique to image the coronary vessels. CTA also aortic annulus and vice versa.1 Unless the mitral annulus is provides excellent visualization of the mitral and aortic valves, and calcified, its border is difficult to identify on CTA.2 yields useful information regarding valve anatomy and function. The mitral valve is the only cardiac valve with 2 Accordingly, an assessment of the valves should be performed whenever possible during CTA interpretation. In this paper, we leaflets. The anterior leaflet is semicircular in shape, highlight the imaging features of common functional and struc- whereas the posterior leaflet is rectangular. Owing to its tural left-sided valvular disorders that can be seen on CTA position within the left ventricle, the anterior leaflet also examinations. functions as a separation between the inflow and outflow tracts of the left ventricle. Key Words: computed tomography, cardiac, valves, angiography The 2 commissures are clefts that divide the 2 leaflets (J Thorac Imaging 2010;25:76–85) from each other. In some pathologic states, however, the commissural spaces may become obliterated and the leaflets appear fused. -

Congenital Heart Disease I: the Unrepaired Adult
Congenital Heart Disease I: The Unrepaired Adult Doreen DeFaria Yeh, MD FACC Assistant Professor, Harvard Medical School MGH Adult Congenital Heart Disease Program Echocardiography Section. No disclosures October 10, 2017; ASE Echo Florida Overview: Unrepaired Adult Congenital Heart Disease • Case review of common and uncommon congenital lesions 1 Natural History of Unrepaired CHD J Hoffman, 1965 Growing Adult CHD population • 1.2M Adults in the US with Congenital Heart Disease Pediatric patients Adult patients 40 30 50 50 60 70 1965 1985 2005 Williams et al. Report of the NHLBI working group on research in ACHD. J am Coll Cardiol 2006;47:701-7 2 46M history of a restrictive VSD new diastolic murmur 3 4 46M asymptomatic. You recommend: • A. Serial echo monitoring as the defect is restrictive • B. Percutaneous closure to the VSD and aortic root fistula • C. Surgical valve sparing aortic root replacement and VSD closure • D. Monitoring for LV volume load, then surgical correction 9 46M asymptomatic. You recommend: • A. Serial echo monitoring as the defect is restrictive • B. Percutaneous closure to the VSD and aortic root fistula • C. Surgical valve sparing aortic root replacement and VSD closure • D. Monitoring for LV volume load, then surgical correction 10 5 Ventricular Septal Defects • Inlet: • AV septal defect, may be associated with ASD • Outlet / Supracristal: • can lead to Ao RCC prolapse • Membranous: • Commonly closes spontaneously DeFaria, Liberthson, Bhatt. 2013 Associated Lesions: • Muscular: • Pulmonic stenosis, BAV, • May -

Echocardiographic Evaluation of Valvular Stenosis Melissa R
ECHOCARDIOGRAPHIC EVALUATION OF VALVULAR STENOSIS MELISSA R. CUNDANGAN, MD, FPCP, FPCC, FPSE AORTIC STENOSIS AORTIC STENOSIS • Obstruction to LV outflow • Decrease in aortic valve area • Normal: 3.0 – 4.0 cm2 • Mild : 1.5-2.0 cm2 • Moderate : 1.0 – 1.5 cm2 • Severe: < 1.0 cm2 Valvular Hear Disease, Chapter 63, Braunwarld’s Heart Disease 10th Edition 2014 AORTIC STENOSIS Causes: • Congenital (unicuspal, bicuspal, quadricuspal) • Rheumatic • Calcific/ Degenerative EAE/ASE recommendations for Echocardiographic assessment of valve stenosis, European Journal of Echocardiography 2009 ECHO EVALUATION OF AORTIC STENOSIS A. Evaluate the anatomy of the AV RCC DIASTOLE NCC LCC SYSTOLE EAE/ASE recommendations for Echocardiographic assessment of valve stenosis, European Journal of Echocardiography 2009 ECHO EVALUATION OF AORTIC STENOSIS fusion of RCC fusion of RCC and NCC and LCC ECHO EVALUATION OF AORTIC STENOSIS ECHO EVALUATION OF AORTIC STENOSIS ECHO EVALUATION OF AORTIC STENOSIS ECHO EVALUATION OF AORTIC STENOSIS B. Determine the aortic valve area by Continuity Equation EAE/ASE recommendations for Echocardiographic assessment of valve stenosis, European Journal of Echocardiography 2009 ECHO EVALUATION OF AORTIC STENOSIS C. Determine the transaortic jet velocity • measured using continuous-wave (CW) Doppler Valvular Hear Disease, Chapter 63, Braunwarld’s Heart Disease 10th Edition 2014 ECHO EVALUATION OF AORTIC STENOSIS D. Determine the transaortic gradient EAE/ASE recommendations for Echocardiographic assessment of valve stenosis, European Journal of Echocardiography 2009 ECHO EVALUATION OF AORTIC STENOSIS EAE/ASE recommendations for Echocardiographic assessment of valve stenosis, European Journal of Echocardiography 2009 • LOW FLOW LOW GRADIENT AORTIC STENOSIS • PARADOXICAL LOW FLOW LOW GRADIENT AORTIC STENOSIS Baseline echo AVA: 0.96 cm2 PIG: 57mmHg MG: 38 mmHg EF 31% PSEUDOSEVERE AORTIC STENOSIS .