Accuracy of the Single Cycle Length Method for Calculation of Aortic Effective Orifice Area in Irregular Heart Rhythms
Total Page:16
File Type:pdf, Size:1020Kb
Load more
Recommended publications
-

Non Commercial Use Only
Cardiogenetics 2017; volume 7:6304 Sudden death in a young patient with atrial fibrillation Case Report Correspondence: María Angeles Espinosa Castro, Inherited Cardiovascular Disease A 22-year-old man suffered a sudden Program, Cardiology Department, Gregorio María Tamargo, cardiac arrest without previous symptoms Marañón Hospital, Dr. Esquerdo, 46, 28007, María Ángeles Espinosa, while he was at rest, waiting for a subway Madrid, Spain. Víctor Gómez-Carrillo, Miriam Juárez, train. Cardiopulmonary resuscitation was Tel.: +34.91.586.82.90. immediately started using an Automated E-mail: [email protected] Francisco Fernández-Avilés, External Defibrillation that identified the Raquel Yotti Key words: KCNQ1; mutation; channelopa- presence of ventricular fibrillation and thy; sudden cardiac death; atrial fibrillation. Inherited Cardiovascular Disease delivered a shock. Return of spontaneous Program, Cardiology Department, circulation was achieved after three Contributions: MT, acquisition and interpreta- Gregorio Marañón Hospital, Madrid, attempts, being atrial fibrillation (AF) the tion of data for the work, ensuring that ques- Spain patient’s rhythm at this point (Figure 1). tions related to the accuracy or integrity of any He was admitted to our Cardiovascular part of the work is appropriately investigated Intensive Care Unit and therapeutic and resolved; MAE, conception of the work, hypothermia was performed over a period critical revision of the intellectual content, final approval of the version to be published, Abstract of 24 h. After completing hypothermia, ensuring that questions related to the accuracy rewarming, and another 24 h of controlled of any part of the work is appropriately inves- Sudden cardiac death (SCD) in young normothermia the patient awakened with no tigated and resolved; VG-C, acquisition and patients without structural heart disease is residual neurologic damage. -

Antithrombotic Therapy in Atrial Fibrillation Associated with Valvular Heart Disease
Europace (2017) 0, 1–21 EHRA CONSENSUS DOCUMENT doi:10.1093/europace/eux240 Antithrombotic therapy in atrial fibrillation associated with valvular heart disease: a joint consensus document from the European Heart Rhythm Association (EHRA) and European Society of Cardiology Working Group on Thrombosis, endorsed by the ESC Working Group on Valvular Heart Disease, Cardiac Arrhythmia Society of Southern Africa (CASSA), Heart Rhythm Society (HRS), Asia Pacific Heart Rhythm Society (APHRS), South African Heart (SA Heart) Association and Sociedad Latinoamericana de Estimulacion Cardıaca y Electrofisiologıa (SOLEACE) Gregory Y. H. Lip1*, Jean Philippe Collet2, Raffaele de Caterina3, Laurent Fauchier4, Deirdre A. Lane5, Torben B. Larsen6, Francisco Marin7, Joao Morais8, Calambur Narasimhan9, Brian Olshansky10, Luc Pierard11, Tatjana Potpara12, Nizal Sarrafzadegan13, Karen Sliwa14, Gonzalo Varela15, Gemma Vilahur16, Thomas Weiss17, Giuseppe Boriani18 and Bianca Rocca19 Document Reviewers: Bulent Gorenek20 (Reviewer Coordinator), Irina Savelieva21, Christian Sticherling22, Gulmira Kudaiberdieva23, Tze-Fan Chao24, Francesco Violi25, Mohan Nair26, Leandro Zimerman27, Jonathan Piccini28, Robert Storey29, Sigrun Halvorsen30, Diana Gorog31, Andrea Rubboli32, Ashley Chin33 and Robert Scott-Millar34 * Corresponding author. Tel/fax: þ44 121 5075503. E-mail address: [email protected] Published on behalf of the European Society of Cardiology. All rights reserved. VC The Author 2017. For permissions, please email: [email protected]. 2 G.Y.H. Lip 1Institute of Cardiovascular Sciences, University of Birmingham and Aalborg Thrombosis Research Unit, Department of Clinical Medicine, Aalborg University, Denmark (Chair, representing EHRA); 2Sorbonne Universite´ Paris 6, ACTION Study Group, Institut De Cardiologie, Groupe Hoˆpital Pitie´-Salpetrie`re (APHP), INSERM UMRS 1166, Paris, France; 3Institute of Cardiology, ‘G. -

Avalus™ Pericardial Aortic Surgical Valve System
FACT SHEET Avalus™ Pericardial Aortic Surgical Valve System Aortic stenosis is a common heart problem caused by a narrowing of the heart’s aortic valve due to excessive calcium deposited on the valve leaflets. When the valve narrows, it does not open or close properly, making the heart work harder to pump blood throughout the body. Eventually, this causes the heart to weaken and function poorly, which may lead to heart failure and increased risk for sudden cardiac death. Disease The standard treatment for patients with aortic valve disease is surgical aortic valve Overview: replacement (SAVR). During this procedure, a surgeon will make an incision in the sternum to open the chest and expose the heart. The diseased native valve is then Aortic removed and a new artificial valve is inserted. Once in place, the device is sewn into Stenosis the aorta and takes over the original valve’s function to enable oxygen-rich blood to flow efficiently out of the heart. For patients that are unable to undergo surgical aortic valve replacement, or prefer a minimally-invasive therapy option, an alternative procedure to treat severe aortic stenosis is called transcatheter aortic valve replacement (TAVR). The Avalus Pericardial Aortic Surgical Valve System is a next- generation aortic surgical valve from Medtronic, offering advanced design concepts and unique features for the millions of patients with severe aortic stenosis who are candidates for open- heart surgery. The Avalus Surgical Valve The Avalus valve, made of bovine tissue, is also the only stented surgical aortic valve on the market that is MRI-safe (without restrictions) enabling patients with severe aortic stenosis who have the Avalus valve to undergo screening procedures for potential co-morbidities. -

Common Types of Supraventricular Tachycardia: Diagnosis and Management RANDALL A
Common Types of Supraventricular Tachycardia: Diagnosis and Management RANDALL A. COLUCCI, DO, MPH, Ohio University College of Osteopathic Medicine, Athens, Ohio MITCHELL J. SILVER, DO, McConnell Heart Hospital, Columbus, Ohio JAY SHUBROOK, DO, Ohio University College of Osteopathic Medicine, Athens, Ohio The most common types of supraventricular tachycardia are caused by a reentry phenomenon producing acceler- ated heart rates. Symptoms may include palpitations (including possible pulsations in the neck), chest pain, fatigue, lightheadedness or dizziness, and dyspnea. It is unusual for supraventricular tachycardia to be caused by structurally abnormal hearts. Diagnosis is often delayed because of the misdiagnosis of anxiety or panic disorder. Patient history is important in uncovering the diagnosis, whereas the physical examination may or may not be helpful. A Holter moni- tor or an event recorder is usually needed to capture the arrhythmia and confirm a diagnosis. Treatment consists of short-term or as-needed pharmacotherapy using calcium channel or beta blockers when vagal maneuvers fail to halt or slow the rhythm. In those who require long-term pharmacotherapy, atrioventricular nodal blocking agents or class Ic or III antiarrhythmics can be used; however, these agents should generally be managed by a cardiologist. Catheter ablation is an option in patients with persistent or recurrent supraventricular tachycardia who are unable to tolerate long-term pharmacologic treatment. If Wolff-Parkinson-White syndrome is present, expedient referral -
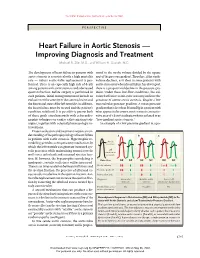
Heart Failure in Aortic Stenosis — Improving Diagnosis and Treatment Michael R
The new england journal of medicine perspective Heart Failure in Aortic Stenosis — Improving Diagnosis and Treatment Michael R. Zile, M.D., and William H. Gaasch, M.D. The development of heart failure in patients with tional to the stroke volume divided by the square aortic stenosis is associated with a high mortality root of the pressure gradient. Therefore, if the stroke rate — unless aortic-valve replacement is per- volume declines, as it does in some patients with formed. There is an especially high risk of death aortic stenosis in whom heart failure has developed, among patients with aortic stenosis and a decreased there is a proportional decline in the pressure gra- ejection fraction. Before surgery is performed in dient. Under these low-flow conditions, the cal- such patients, initial management must include an culated effective aortic-valve area may indicate the evaluation of the severity of the stenotic lesion and presence of severe aortic stenosis, despite a low the functional state of the left ventricle; in addition, transvalvular pressure gradient. A mean pressure the heart failure must be treated and the patient’s gradient that is less than 30 mm Hg in a patient with condition stabilized. It is possible to pursue both what appears to be severe aortic stenosis (an aortic- of these goals simultaneously with echocardio- valve area of <1 cm2) indicates what is referred to as graphic techniques or cardiac catheterization tech- “low-gradient aortic stenosis.” niques, together with selected pharmacologic in- An example of a low pressure gradient in a pa- terventions. Proper evaluation and treatment require an un- derstanding of the pathophysiology of heart failure ABC in patients with aortic stenosis. -

What Is Atrial Fibrillation?
ANSWERS Cardiovascular Conditions by heart What Is Atrial Fibrillation? Normally, your heart contracts and relaxes to a regular beat. Certain cells in your heart, called the sinus node, make electrical The illustrations above show normal conduction and contraction. signals that cause the heart to contract and pump blood. These electrical signals can be recorded using an electrocardiogram, or Sinus node ECG. Your doctor can read your ECG to find out if the electrical signals are normal. Left atrium In atrial fibrillation, or AFib, the heart’s Right atrium two small upper chambers (atria) beat irregularly and too fast, quivering instead of contracting properly. With atrial fibrillation, random electrical activity During AFib, some blood may not be interrupts the normal pumped efficiently from the atria into the conduction rhythm. ventricles. Blood that’s left behind can pool This prevents the atria from in the atria and form blood clots. properly contracting. How do I know I have atrial fibrillation? The risk of stroke is about five times higher in people with AFib. This is because blood can pool in the atria and blood Some people with AFib don’t have symptoms. Some of the clots can form. symptoms are: • Fast, irregular heartbeat What can be done to correct AFib? • Heart palpitations (rapid “flopping” or “fluttering” feeling in the chest) Treatment options may include one or more of the following: • Feeling lightheaded or faint • Medication to help slow your heart rate, such as beta • Chest pain or pressure blockers, certain calcium channel blockers or digoxin • Shortness of breath, especially when lying down • Medication to restore normal heart rhythm, such as • Tiring more easily (fatigue) beta blockers or antiarrhythmics • Procedures to stop or control the electrical impulses Can AFib lead to other problems? causing the AFib, such as electrical cardioversion or catheter ablation You can live with and manage AFib. -

Imaging and Impact of Myocardial Fibrosis in Aortic Stenosis
JACC: CARDIOVASCULAR IMAGING VOL. 12, NO. 2, 2019 ª 2019 THE AUTHORS. PUBLISHED BY ELSEVIER ON BEHALF OF THE AMERICAN COLLEGE OF CARDIOLOGY FOUNDATION. THIS IS AN OPEN ACCESS ARTICLE UNDER THE CC BY LICENSE (http://creativecommons.org/licenses/by/4.0/). FOCUS ISSUE: IMAGING IN AORTIC STENOSIS: PART II STATE-OF-THE-ART PAPER Imaging and Impact of Myocardial Fibrosis in Aortic Stenosis a b a c Rong Bing, MBBS, BMEDSCI, João L. Cavalcante, MD, Russell J. Everett, MD, BSC, Marie-Annick Clavel, DVM, PHD, a a David E. Newby, DM, PHD, DSC, Marc R. Dweck, MD, PHD ABSTRACT Aortic stenosis is characterized both by progressive valve narrowing and the left ventricular remodeling response that ensues. The only effective treatment is aortic valve replacement, which is usually recommended in patients with severe stenosis and evidence of left ventricular decompensation. At present, left ventricular decompensation is most frequently identified by the development of typical symptoms or a marked reduction in left ventricular ejection fraction <50%. However, there is growing interest in using the assessment of myocardial fibrosis as an earlier and more objective marker of left ventricular decompensation, particularly in asymptomatic patients, where guidelines currently rely on non- randomized data and expert consensus. Myocardial fibrosis has major functional consequences, is the key pathological process driving left ventricular decompensation, and can be divided into 2 categories. Replacement fibrosis is irreversible and identified using late gadolinium enhancement on cardiac magnetic resonance, while diffuse fibrosis occurs earlier, is potentially reversible, and can be quantified with cardiac magnetic resonance T1 mapping techniques. There is a substantial body of observational data in this field, but there is now a need for randomized clinical trials of myocardial imaging in aortic stenosis to optimize patient management. -

HRS/EHRA/APHRS Expert Consensus Statement on the Diagnosis and Management of Patients with Inherited Primary Arrhythmia Syndromes
This document is embargoed until May 10, 2013 at 9:30 am MST. Document will publish in HeartRhythm, EP Europace, and Journal of Arrhythmias in the fall of 2013. HRS/EHRA/APHRS Expert Consensus Statement on the Diagnosis and Management of Patients with Inherited Primary Arrhythmia Syndromes Developed in partnership with the Heart Rhythm Society (HRS), the European Heart Rhythm Association (EHRA), a registered branch of the European Society of Cardiology, and the Asia Pacific Heart Rhythm Society (APHRS); and in collaboration with the American College of Cardiology Foundation (ACCF), the American Heart Association (AHA), the Pediatric and Congenital Electrophysiology Society (PACES) and the Association for European Pediatric and Congenital Cardiology (AEPC). Document endorsed by HRS, EHRA and APHRS May, 2013. Endorsements pending from ACCF, AHA, PACES, and AEPC. Writing Group Chairs Silvia G. Priori, MD, PhD, Fondazione Salvatore Maugeri, Department of Molecular Medicine University of Pavia, Pavia, ITALY (HRS Chairperson) Arthur A. Wilde, MD, PhD, University of Amsterdam, Amsterdam, NETHERLANDS (EHRA Chairperson) Minoru Horie, MD, PhD, Shiga University of Medical Sciences, Otsu, JAPAN (APHRS Chairperson) Yongkeun Cho, MD, PhD, Kyungpook National University, Daegu, SOUTH KOREA (APHRS Chairperson) Writing Group Members Elijah R. Behr, MA, MBBS, MD, FRCP, St. Georges University of London, UNITED KINGDOM Charles Berul, MD, FHRS, CCDS, Children’s National Medical Center, Washington, DC, UNITED STATES Nico Blom, MD, PhD, Academical Medical Center, AMSTERDAM, Leiden University Medical Center, Leiden, NETHERLANDS* Josep Brugada, MD, PhD, University of Barcelona, Barcelona, SPAIN Chern-En Chiang, MD, PhD, Taipei Veteran’s General Hospital, Taipei, TAIWAN © Heart Rhythm Society, European Heart Rhythm Association, a registered branch of the European Society of Cardiology, and the Asia Pacific Heart Rhythm Society 1 This document is embargoed until May 10, 2013 at 9:30 am MST. -

Mixed Connective Tissue Disease Presenting As Atrial Fibrillation, Fever, Lymphadenopathy, and Pericardial Effusion
J Case Rep Images Med 2016;2:24–30. Mathew Jr. et al. 24 www.edoriumjournals.com/case-reports/jcrm CCASEASE REPORT PEER REVIEWED OPE| OPEN NACCESS ACCESS Mixed connective tissue disease presenting as atrial fibrillation, fever, lymphadenopathy, and pericardial effusion Jacob Mathew Jr., Tanner Kim, Timilyn Nunu, Jay Jahanmir ABSTRACT autoimmune condition affecting almost every major organ of the body, defined by the presence Introduction: Mixed connective tissue disease of overlapping features from other connective (MCTD) is a poorly understood rheumatologic tissue diseases. The use of available classification condition that presents with clinical symptoms criteria and newly available biomarkers can related to the underlying presence of distinct assist in earlier diagnosis. While the condition overlapping autoimmune conditions. Patients can is considered incurable, prognosis is good be identified by the presence of a shared antibody with use of glucocorticoid therapy. This case to the U1 small nuclear ribonucleoprotein highlights the need to keep heightened suspicion autoantigen. While the condition is considered for entities such as MCTD in patients who have incurable, prognosis is relatively good with most various symptoms that may fit multiple distinct patients responding well to glucocorticoids. autoimmune conditions. We report a case in which a patient presented with multiple nonspecific symptoms but was Keywords: Mixed connective tissue disease found to have multiple organ involvement that (MCTD), Rheumatology, Reactive lymphadenop- ultimately was tied to MCTD. Case Report: We athy report a 48-year-old male admitted with multiple nonspecific symptoms who was found to have How to cite this article atrial fibrillation, pericardial effusion, pleural effusions, diffuse lymphadenopathy and among Mathew Jr., J, Kim T, Nunu T, Jahanmir J. -

Atrial Fibrillation: Diagnosis and Treatment CECILIA GUTIERREZ, MD, and DANIEL G
Atrial Fibrillation: Diagnosis and Treatment CECILIA GUTIERREZ, MD, and DANIEL G. BLANCHARD, MD, University of California, San Diego, La Jolla, California Atrial fibrillation is the most common cardiac arrhythmia. It impairs cardiac function and increases the risk of stroke. The incidence of atrial fibrillation increases with age. Key treatment issues include deciding when to restore normal sinus rhythm, when to control rate only, and how to prevent thromboembolism. Rate control is the preferred manage- ment option in most patients. Rhythm control is an option for patients in whom rate control cannot be achieved or who have persistent symptoms despite rate control. The current recommendation for strict rate control is a resting heart rate of less than 80 beats per minute. However, one study has shown that more lenient rate control of less than 110 beats per minute while at rest was not inferior to strict rate control in preventing cardiac death, heart failure, stroke, and life- threatening arrhythmias. Anticoagulation therapy is needed with rate control and rhythm control to prevent stroke. Warfarin is superior to aspirin and clopidogrel in preventing stroke despite its narrow therapeutic range and increased risk of bleeding. Tools that predict the risk of stroke (e.g., CHADS2) and the risk of bleeding (e.g., Outpatient Bleed- ing Risk Index) are helpful in making decisions about anticoagulation therapy. Surgical options for atrial fibrillation include disruption of abnormal conduction pathways in the atria, and obliteration of the left atrial appendage. Catheter ablation is an option for restoring normal sinus rhythm in patients with paroxysmal atrial fibrillation and normal left atrial size. -

Management of Asymptomatic Arrhythmias
Europace (2019) 0, 1–32 EHRA POSITION PAPER doi:10.1093/europace/euz046 Downloaded from https://academic.oup.com/europace/advance-article-abstract/doi/10.1093/europace/euz046/5382236 by PPD Development LP user on 25 April 2019 Management of asymptomatic arrhythmias: a European Heart Rhythm Association (EHRA) consensus document, endorsed by the Heart Failure Association (HFA), Heart Rhythm Society (HRS), Asia Pacific Heart Rhythm Society (APHRS), Cardiac Arrhythmia Society of Southern Africa (CASSA), and Latin America Heart Rhythm Society (LAHRS) David O. Arnar (Iceland, Chair)1*, Georges H. Mairesse (Belgium, Co-Chair)2, Giuseppe Boriani (Italy)3, Hugh Calkins (USA, HRS representative)4, Ashley Chin (South Africa, CASSA representative)5, Andrew Coats (United Kingdom, HFA representative)6, Jean-Claude Deharo (France)7, Jesper Hastrup Svendsen (Denmark)8,9, Hein Heidbu¨chel (Belgium)10, Rodrigo Isa (Chile, LAHRS representative)11, Jonathan M. Kalman (Australia, APHRS representative)12,13, Deirdre A. Lane (United Kingdom)14,15, Ruan Louw (South Africa, CASSA representative)16, Gregory Y. H. Lip (United Kingdom, Denmark)14,15, Philippe Maury (France)17, Tatjana Potpara (Serbia)18, Frederic Sacher (France)19, Prashanthan Sanders (Australia, APHRS representative)20, Niraj Varma (USA, HRS representative)21, and Laurent Fauchier (France)22 ESC Scientific Document Group: Kristina Haugaa23,24, Peter Schwartz25, Andrea Sarkozy26, Sanjay Sharma27, Erik Kongsga˚rd28, Anneli Svensson29, Radoslaw Lenarczyk30, Maurizio Volterrani31, Mintu Turakhia32, -

Atrial Fibrillation in Acute Myocardial Infarction
Original Article Atrial Fibrillation in Acute Myocardial Infarction Radha Bhattarai1, Sergey Anatolevich Sayganov1 1Department of hospital therapy and cardiology Northwestern State Medical University, Vasilevsky Ostrov, Bolshoe Prospect 85, Saint-Petersburg, Russia. ABSTRACT Background and Aim: New-onset atrial fibrillation frequently complicates acute myocardial infarction. The incidence ranges from 6 - 21% “1”.We aim to determine the incidence of atrial fibrillation in the setting of acute myocardial infarction. Methods: This was a single center prospective study, conducted in the coronary care unit of Saint-Petersburg Pokrovskaya city hospital, Russia, during the period, June 2013 to June 2014. Sixty consecutive patients of acute myocardial infarction with atrial fibrillation were included in this study. Onset, duration, and mode of termination of atrial fibrillation, clinical factors associated with its presentation and its relation with patient outcome were evaluated. Results: Among the 60 patients 33 (55%) had inferior wall myocardial infarction and 27 (45%) patients had anterior wall myocardial infarction. In patients with inferior wall myocardial infarction the onset of atrial fibrillation occurred within 24 hours in 30 (91%) patients, after 24 hour in 3 (9%) patients. The episode lasted for less than 24 hours in 12 (36%), and more than 24 hours in 21 (64%) patients. In anterior wall myocardial infarction atrial fibrillation occurred within 24 hours in 2 (7%) patients, on the second day in 25 (93%). The episode lasted less than 24 hours in 3 (11%), 48 hours in (85%), 72 hours in 1 (4%) Citation patients. There was a significant difference in the Radha Bhattarai, Sergey Anatolevich Sayganov. onset and duration of atrial fibrillation in relation to Atrial Fibrillation in Acute Myocardial Infarction.