Antithrombotic Therapy in Atrial Fibrillation Associated with Valvular Heart Disease
Total Page:16
File Type:pdf, Size:1020Kb
Load more
Recommended publications
-

Non Commercial Use Only
Cardiogenetics 2017; volume 7:6304 Sudden death in a young patient with atrial fibrillation Case Report Correspondence: María Angeles Espinosa Castro, Inherited Cardiovascular Disease A 22-year-old man suffered a sudden Program, Cardiology Department, Gregorio María Tamargo, cardiac arrest without previous symptoms Marañón Hospital, Dr. Esquerdo, 46, 28007, María Ángeles Espinosa, while he was at rest, waiting for a subway Madrid, Spain. Víctor Gómez-Carrillo, Miriam Juárez, train. Cardiopulmonary resuscitation was Tel.: +34.91.586.82.90. immediately started using an Automated E-mail: [email protected] Francisco Fernández-Avilés, External Defibrillation that identified the Raquel Yotti Key words: KCNQ1; mutation; channelopa- presence of ventricular fibrillation and thy; sudden cardiac death; atrial fibrillation. Inherited Cardiovascular Disease delivered a shock. Return of spontaneous Program, Cardiology Department, circulation was achieved after three Contributions: MT, acquisition and interpreta- Gregorio Marañón Hospital, Madrid, attempts, being atrial fibrillation (AF) the tion of data for the work, ensuring that ques- Spain patient’s rhythm at this point (Figure 1). tions related to the accuracy or integrity of any He was admitted to our Cardiovascular part of the work is appropriately investigated Intensive Care Unit and therapeutic and resolved; MAE, conception of the work, hypothermia was performed over a period critical revision of the intellectual content, final approval of the version to be published, Abstract of 24 h. After completing hypothermia, ensuring that questions related to the accuracy rewarming, and another 24 h of controlled of any part of the work is appropriately inves- Sudden cardiac death (SCD) in young normothermia the patient awakened with no tigated and resolved; VG-C, acquisition and patients without structural heart disease is residual neurologic damage. -

Percutaneous Mitral Valve Therapies: State of the Art in 2020 LA ACP Annual Meeting
Percutaneous Mitral Valve Therapies: State of the Art in 2020 LA ACP Annual Meeting Steven R Bailey MD MSCAI, FACC, FAHA,FACP Professor and Chair, Department of Medicine Malcolm Feist Chair of Interventional Cardiology LSU Health Shreveport Professor Emeritus, UH Health San Antonio [email protected] SRB March 2020 Disclosure Statement of Financial Interest Within the past 12 months, I or my spouse/partner have had a financial interest/arrangement or affiliation with the organization(s) listed below. Affiliation/Financial Relationship Company • Grant/Research Support • None • Consulting Fees/Honoraria • BSCI, Abbot DSMB • Intellectual Property Rights • UTHSCSA • Other Financial Benefit • CCI Editor In Chief SRB March 2020 The 30,000 Ft View Maria SRB March 2020 SRB March 2020 Mitral Stenosis • The most common etiology of MS is rheumatic fever, with a latency of approximately 10 to 20 years after the initial streptococcal infection. Symptoms usually appear in adulthood • Other etiologies are rare but include: congenital MS radiation exposure atrial myxoma mucopolysaccharidoses • MS secondary to calcific annular disease is increasingly seen in elderly patients, and in patients with advanced chronic kidney disease. SRB March 2020 Mitral Stenosis • Mitral stenosis most commonly results from rheumatic heart disease fusion of the valve leaflet cusps at the commissures thickening and shortening of the chordae calcium deposition within the valve leaflets • Characteristic “fish-mouth” or “hockey stick” appearance on the echocardiogram (depending on view) SRB March 2020 Mitral Stenosis: Natural History • The severity of symptoms depends primarily on the degree of stenosis. • Symptoms often go unrecognized by patient and physician until significant shortness of breath, hemoptysis, or atrial fibrillation develops. -

How to Define Valvular Atrial Fibrillation?
Archives of Cardiovascular Disease (2015) 108, 530—539 Available online at ScienceDirect www.sciencedirect.com REVIEW How to define valvular atrial fibrillation? Comment définir la fibrillation atriale valvulaire ? ∗ Laurent Fauchier , Raphael Philippart, Nicolas Clementy, Thierry Bourguignon, Denis Angoulvant, Fabrice Ivanes, Dominique Babuty, Anne Bernard Service de cardiologie, faculté de médecine, université Franc¸ois-Rabelais, CHU Trousseau, Tours, France Received 3 June 2015; accepted 8 June 2015 Available online 14 July 2015 KEYWORDS Summary Atrial fibrillation (AF) confers a substantial risk of stroke. Recent trials compar- Atrial fibrillation; ing vitamin K antagonists (VKAs) with non-vitamin K antagonist oral anticoagulants (NOACs) in Valve disease; AF were performed among patients with so-called ‘‘non-valvular’’ AF. The distinction between Stroke ‘‘valvular’’ and ‘‘non-valvular’’ AF remains a matter of debate. Currently, ‘‘valvular AF’’ refers to patients with mitral stenosis or artificial heart valves (and valve repair in North American guidelines only), and should be treated with VKAs. Valvular heart diseases, such as mitral regur- gitation, aortic stenosis (AS) and aortic insufficiency, do not result in conditions of low flow in the left atrium, and do not apparently increase the risk of thromboembolism brought by AF. Post-hoc analyses suggest that these conditions probably do not make the thromboembolic risk less responsive to NOACs compared with most forms of ‘‘non-valvular’’ AF. The pathogenesis of thrombosis is probably different for blood coming into contact with a mechanical prosthetic valve compared with what occurs in most other forms of AF. This may explain the results of the only trial performed with a NOAC in patients with a mechanical prosthetic valve (only a few of whom had AF), where warfarin was more effective and safer than dabigatran. -

Echo in Asymptomatic Mitral and Aortic Regurgitation
2017 ASE Florida | Orlando, FL October 9, 2017 | 10:40 – 11:00 PM | 20 min | Grand Harbor Ballroom South Echo in Asymptomatic Mitral and Aortic Regurgitation Muhamed Sarić MD, PhD, MPA Director of Noninvasive Cardiology | Echo Lab Associate Professor of Medicine Disclosures Speakers Bureau (Philips, Medtronic) Advisory Board (Siemens) Regurgitation Axioms ▪Typically, regurgitation is NOT symptomatic unless severe ▪The opposite is not true: Severe regurgitation may be asymptomatic ▪ Chronic regurgitation leads to chamber dilatation on either side of the regurgitant valve Regurgitation Discovery ▪ Regurgitation as a anatomic entity was recognized in the 17th century ▪ Regurgitation was first clinically diagnosed by auscultation in the 19th century, well before the advent of echocardiography First Use of Regurgitation Term in English 1683 W. Charleton Three Anat. Lect. i. 18 Those [valves] that are placed in the inlet and outlet of the left Ventricle, to obviate the regurgitation of the bloud into the arteria venosa, and out of the aorta into the left Ventricle. Walter Charleton (1619 – 1707) English Physician Heart Murmur OXFORD ENGLISH DICTIONARY DEFINITION ▪ Any of various auscultatory sounds ▪ Adventitious sounds of cardiac or vascular origin [that is, separate from standard heart sounds: S1, S2, S3, S4] ▪ Sometimes of no significance ▪ But sometimes caused by valvular lesions of the heart or other diseases of the Στῆθος : Stēthos = chest circulatory system René Laënnec Stethoscope (1781 – 1826) (‘Chest examiner’) French Physician Hollow wooden cylinder Inventor of stethoscope in 1816 Laënnec Performing Auscultation Painted by Robert Alan Thom (1915 – 1979), American illustrator Commissioned by Parke, Davis & Co. 1816 1832 René Laënnec, James Hope French physician British physician Invents MONAURAL stethoscope separates MS from MR murmur 1852 1862 George Cammann Austin Flint Sr. -

Avalus™ Pericardial Aortic Surgical Valve System
FACT SHEET Avalus™ Pericardial Aortic Surgical Valve System Aortic stenosis is a common heart problem caused by a narrowing of the heart’s aortic valve due to excessive calcium deposited on the valve leaflets. When the valve narrows, it does not open or close properly, making the heart work harder to pump blood throughout the body. Eventually, this causes the heart to weaken and function poorly, which may lead to heart failure and increased risk for sudden cardiac death. Disease The standard treatment for patients with aortic valve disease is surgical aortic valve Overview: replacement (SAVR). During this procedure, a surgeon will make an incision in the sternum to open the chest and expose the heart. The diseased native valve is then Aortic removed and a new artificial valve is inserted. Once in place, the device is sewn into Stenosis the aorta and takes over the original valve’s function to enable oxygen-rich blood to flow efficiently out of the heart. For patients that are unable to undergo surgical aortic valve replacement, or prefer a minimally-invasive therapy option, an alternative procedure to treat severe aortic stenosis is called transcatheter aortic valve replacement (TAVR). The Avalus Pericardial Aortic Surgical Valve System is a next- generation aortic surgical valve from Medtronic, offering advanced design concepts and unique features for the millions of patients with severe aortic stenosis who are candidates for open- heart surgery. The Avalus Surgical Valve The Avalus valve, made of bovine tissue, is also the only stented surgical aortic valve on the market that is MRI-safe (without restrictions) enabling patients with severe aortic stenosis who have the Avalus valve to undergo screening procedures for potential co-morbidities. -

Common Types of Supraventricular Tachycardia: Diagnosis and Management RANDALL A
Common Types of Supraventricular Tachycardia: Diagnosis and Management RANDALL A. COLUCCI, DO, MPH, Ohio University College of Osteopathic Medicine, Athens, Ohio MITCHELL J. SILVER, DO, McConnell Heart Hospital, Columbus, Ohio JAY SHUBROOK, DO, Ohio University College of Osteopathic Medicine, Athens, Ohio The most common types of supraventricular tachycardia are caused by a reentry phenomenon producing acceler- ated heart rates. Symptoms may include palpitations (including possible pulsations in the neck), chest pain, fatigue, lightheadedness or dizziness, and dyspnea. It is unusual for supraventricular tachycardia to be caused by structurally abnormal hearts. Diagnosis is often delayed because of the misdiagnosis of anxiety or panic disorder. Patient history is important in uncovering the diagnosis, whereas the physical examination may or may not be helpful. A Holter moni- tor or an event recorder is usually needed to capture the arrhythmia and confirm a diagnosis. Treatment consists of short-term or as-needed pharmacotherapy using calcium channel or beta blockers when vagal maneuvers fail to halt or slow the rhythm. In those who require long-term pharmacotherapy, atrioventricular nodal blocking agents or class Ic or III antiarrhythmics can be used; however, these agents should generally be managed by a cardiologist. Catheter ablation is an option in patients with persistent or recurrent supraventricular tachycardia who are unable to tolerate long-term pharmacologic treatment. If Wolff-Parkinson-White syndrome is present, expedient referral -
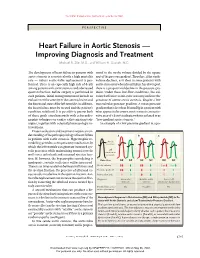
Heart Failure in Aortic Stenosis — Improving Diagnosis and Treatment Michael R
The new england journal of medicine perspective Heart Failure in Aortic Stenosis — Improving Diagnosis and Treatment Michael R. Zile, M.D., and William H. Gaasch, M.D. The development of heart failure in patients with tional to the stroke volume divided by the square aortic stenosis is associated with a high mortality root of the pressure gradient. Therefore, if the stroke rate — unless aortic-valve replacement is per- volume declines, as it does in some patients with formed. There is an especially high risk of death aortic stenosis in whom heart failure has developed, among patients with aortic stenosis and a decreased there is a proportional decline in the pressure gra- ejection fraction. Before surgery is performed in dient. Under these low-flow conditions, the cal- such patients, initial management must include an culated effective aortic-valve area may indicate the evaluation of the severity of the stenotic lesion and presence of severe aortic stenosis, despite a low the functional state of the left ventricle; in addition, transvalvular pressure gradient. A mean pressure the heart failure must be treated and the patient’s gradient that is less than 30 mm Hg in a patient with condition stabilized. It is possible to pursue both what appears to be severe aortic stenosis (an aortic- of these goals simultaneously with echocardio- valve area of <1 cm2) indicates what is referred to as graphic techniques or cardiac catheterization tech- “low-gradient aortic stenosis.” niques, together with selected pharmacologic in- An example of a low pressure gradient in a pa- terventions. Proper evaluation and treatment require an un- derstanding of the pathophysiology of heart failure ABC in patients with aortic stenosis. -

What Is Atrial Fibrillation?
ANSWERS Cardiovascular Conditions by heart What Is Atrial Fibrillation? Normally, your heart contracts and relaxes to a regular beat. Certain cells in your heart, called the sinus node, make electrical The illustrations above show normal conduction and contraction. signals that cause the heart to contract and pump blood. These electrical signals can be recorded using an electrocardiogram, or Sinus node ECG. Your doctor can read your ECG to find out if the electrical signals are normal. Left atrium In atrial fibrillation, or AFib, the heart’s Right atrium two small upper chambers (atria) beat irregularly and too fast, quivering instead of contracting properly. With atrial fibrillation, random electrical activity During AFib, some blood may not be interrupts the normal pumped efficiently from the atria into the conduction rhythm. ventricles. Blood that’s left behind can pool This prevents the atria from in the atria and form blood clots. properly contracting. How do I know I have atrial fibrillation? The risk of stroke is about five times higher in people with AFib. This is because blood can pool in the atria and blood Some people with AFib don’t have symptoms. Some of the clots can form. symptoms are: • Fast, irregular heartbeat What can be done to correct AFib? • Heart palpitations (rapid “flopping” or “fluttering” feeling in the chest) Treatment options may include one or more of the following: • Feeling lightheaded or faint • Medication to help slow your heart rate, such as beta • Chest pain or pressure blockers, certain calcium channel blockers or digoxin • Shortness of breath, especially when lying down • Medication to restore normal heart rhythm, such as • Tiring more easily (fatigue) beta blockers or antiarrhythmics • Procedures to stop or control the electrical impulses Can AFib lead to other problems? causing the AFib, such as electrical cardioversion or catheter ablation You can live with and manage AFib. -

How Do We Define Valvular Heart Disease When Considering Warfarin
CORRESPONDENCE Further clarification about this issue would be very much appreciated. Dr Andrew Reid, General Practitioner Tuakau The bpacnz editorial team asked cardiologist Stewart Mann to respond: This is a very relevant question and one that probably does not yet have a definitive answer. The RE-LY trial that compared the efficacy of warfarin and dabigatran had the exclusion criterion “moderate or severe mitral stenosis”. This study also excluded How do we define valvular heart disease when patients with a potentially reversible cause of AF which might considering warfarin or dabigatran in patients with include some valve disease amenable to surgery. Other valve atrial fibrillation? disease could be included. An analysis of patients with valve Dear Editor, disease included in the trial has been conducted and published I have a query from the summary article “An update on in abstract form.1 In the RE-LY trial, around 20% of patients had antithrombotic medications: What does primary care need to valve disease, most with mitral regurgitation but some with know?”, BPJ 73 (Feb, 2016) that I would very much appreciate aortic regurgitation, aortic stenosis or mild mitral stenosis. some further information on. There is no mention of patients with tissue valve prostheses or of those who might have had a valvuloplasty. The group with The article makes this comment: valve disease had poorer outcomes than those without valve “Dabigatran should NOT be prescribed to patients disease but there was no significant difference between those with valvular -

Accuracy of the Single Cycle Length Method for Calculation of Aortic Effective Orifice Area in Irregular Heart Rhythms
AORTIC STENOSIS Accuracy of the Single Cycle Length Method for Calculation of Aortic Effective Orifice Area in Irregular Heart Rhythms Kerry A. Esquitin, MD, Omar K. Khalique, MD, Qi Liu, MD, Susheel K. Kodali, MD, Leo Marcoff, MD, Tamim M. Nazif, MD, Isaac George, MD, Torsten P. Vahl, MD, Martin B. Leon, MD, and Rebecca T. Hahn, MD, New York, New York; and Morristown, New Jersey Introduction: In irregular heart rhythms, echocardiographic calculation of aortic effective orifice area (EOA) re- quires averaging measurements from multiple cardiac cycles. Whether a single cycle length method can be used to calculate aortic EOA in aortic stenosis with nonsinus rhythms is not known. Methods: Transthoracic echocardiograms of 100 patients with aortic stenosis and either atrial fibrillation (AF) or frequent ectopy (FE) were retrospectively reviewed. The aortic valve velocity time integral (VTIAV) and the left ven- tricular outflow tract VTI (VTILVOT) were measured by two methods: the standard method (averaging multiple beats) and the single cycle length method. The latter matches the R-R intervals for VTIAV and VTILVOT.Stroke volume, EOA, and Doppler velocity index were calculated by both methods in all patients. The single cycle length method was used for short and long R-R cycles in AF and for postectopic beats (long R-R cycles) in FE. Results: In AF, long R-R cycles resulted in larger stroke volumes (73 6 21 vs 63 6 18 mL; P # .0001) but no difference in EOA (0.84 6 0.27 vs 0.82 6 0.27 cm2; P = .11), whereas short R-R cycles resulted in smaller stroke volumes (55 6 18 vs 63 6 18 mL, P # .0001) but a larger EOA (0.86 6 0.28 vs 0.82 6 0.27 cm2; P = .01). -

Expert Consensus for Multi-Modality Imaging Evaluation Of
EACVI/ASE EXPERT CONSENSUS STATEMENT Expert Consensus for Multi-Modality Imaging Evaluation of Cardiovascular Complications of Radiotherapy in Adults: A Report from the European Association of Cardiovascular Imaging and the American Society of Echocardiography Patrizio Lancellotti,* Vuyisile T. Nkomo, Luigi P. Badano, Jutta Bergler, Jan Bogaert, Laurent Davin, Bernard Cosyns, Philippe Coucke, Raluca Dulgheru, Thor Edvardsen, Oliver Gaemperli, Maurizio Galderisi, Brian Griffin, Paul A. Heidenreich, Koen Nieman, Juan C. Plana, Steven C. Port, Marielle Scherrer-Crosbie, Ronald G. Schwartz, Igal A. Sebag, Jens-Uwe Voigt, Samuel Wann, and Phillip C. Yang, In collaboration with the European Society of Cardiology Working Groups on Nuclear Cardiology and Cardiac Computed Tomography and Cardiovascular Magnetic Resonance and the American Society of Nuclear Cardiology, Society for Cardiovascular Magnetic Resonance, and Society of Cardiovascular Computed Tomography, Liege, Brussels, Leuven, Belgium, Rochester, MN, Padua, Italy, Vienna, Austria, Bucharest, Romania, Oslo, Norway, Zurich, Switzerland, Naples, Italy, Cleveland, OH, Palo Alto, Stanford, CA, Rotterdam, The Netherlands, Milwaukee, WI, Boston, MA, Rochester, NY, Montreal, Quebec, Canada Cardiac toxicity is one of the most concerning side effects of anti-cancer therapy. The gain in life expectancy ob- tained with anti-cancer therapy can be compromised by increased morbidity and mortality associated with its cardiac complications. While radiosensitivity of the heart was initially recognized only in the early 1970s, the heart is regarded in the current era as one of the most critical dose-limiting organs in radiotherapy. Several clinical stud- ies have identified adverse clinical consequences of radiation-induced heart disease (RIHD) on the outcome of long-term cancer survivors. A comprehensive review of potential cardiac complications related to radiotherapy is warranted. -

Imaging and Impact of Myocardial Fibrosis in Aortic Stenosis
JACC: CARDIOVASCULAR IMAGING VOL. 12, NO. 2, 2019 ª 2019 THE AUTHORS. PUBLISHED BY ELSEVIER ON BEHALF OF THE AMERICAN COLLEGE OF CARDIOLOGY FOUNDATION. THIS IS AN OPEN ACCESS ARTICLE UNDER THE CC BY LICENSE (http://creativecommons.org/licenses/by/4.0/). FOCUS ISSUE: IMAGING IN AORTIC STENOSIS: PART II STATE-OF-THE-ART PAPER Imaging and Impact of Myocardial Fibrosis in Aortic Stenosis a b a c Rong Bing, MBBS, BMEDSCI, João L. Cavalcante, MD, Russell J. Everett, MD, BSC, Marie-Annick Clavel, DVM, PHD, a a David E. Newby, DM, PHD, DSC, Marc R. Dweck, MD, PHD ABSTRACT Aortic stenosis is characterized both by progressive valve narrowing and the left ventricular remodeling response that ensues. The only effective treatment is aortic valve replacement, which is usually recommended in patients with severe stenosis and evidence of left ventricular decompensation. At present, left ventricular decompensation is most frequently identified by the development of typical symptoms or a marked reduction in left ventricular ejection fraction <50%. However, there is growing interest in using the assessment of myocardial fibrosis as an earlier and more objective marker of left ventricular decompensation, particularly in asymptomatic patients, where guidelines currently rely on non- randomized data and expert consensus. Myocardial fibrosis has major functional consequences, is the key pathological process driving left ventricular decompensation, and can be divided into 2 categories. Replacement fibrosis is irreversible and identified using late gadolinium enhancement on cardiac magnetic resonance, while diffuse fibrosis occurs earlier, is potentially reversible, and can be quantified with cardiac magnetic resonance T1 mapping techniques. There is a substantial body of observational data in this field, but there is now a need for randomized clinical trials of myocardial imaging in aortic stenosis to optimize patient management.