Pathology of Fungal Infection
Total Page:16
File Type:pdf, Size:1020Kb
Load more
Recommended publications
-

Next-Generation Sequencing for Hypothesis-Free Genomic Detection
Frickmann et al. BMC Microbiology (2019) 19:75 https://doi.org/10.1186/s12866-019-1448-0 RESEARCH ARTICLE Open Access Next-generation sequencing for hypothesis- free genomic detection of invasive tropical infections in poly-microbially contaminated, formalin-fixed, paraffin-embedded tissue samples – a proof-of-principle assessment Hagen Frickmann1,2* , Carsten Künne3, Ralf Matthias Hagen4, Andreas Podbielski2, Jana Normann2, Sven Poppert5,6, Mario Looso3 and Bernd Kreikemeyer2 Abstract Background: The potential of next-generation sequencing (NGS) for hypothesis-free pathogen diagnosis from (poly-)microbially contaminated, formalin-fixed, paraffin embedded tissue samples from patients with invasive fungal infections and amebiasis was investigated. Samples from patients with chromoblastomycosis (n = 3), coccidioidomycosis (n = 2), histoplasmosis (n = 4), histoplasmosis or cryptococcosis with poor histological discriminability (n = 1), mucormycosis (n = 2), mycetoma (n = 3), rhinosporidiosis (n = 2), and invasive Entamoeba histolytica infections (n = 6) were analyzed by NGS (each one Illumina v3 run per sample). To discriminate contamination from putative infections in NGS analysis, mean and standard deviation of the number of specific sequence fragments (paired reads) were determined and compared in all samples examined for the pathogens in question. Results: For matches between NGS results and histological diagnoses, a percentage of species-specific reads greater than the 4th standard deviation above the mean value of all 23 assessed sample materials was required. Potentially etiologically relevant pathogens could be identified by NGS in 5 out of 17 samples of patients with invasive mycoses and in 1 out of 6 samples of patients with amebiasis. Conclusions: The use of NGS for hypothesis-free pathogen diagnosis from contamination-prone formalin- fixed, paraffin-embedded tissue requires further standardization. -

Fungal Infections from Human and Animal Contact
Journal of Patient-Centered Research and Reviews Volume 4 Issue 2 Article 4 4-25-2017 Fungal Infections From Human and Animal Contact Dennis J. Baumgardner Follow this and additional works at: https://aurora.org/jpcrr Part of the Bacterial Infections and Mycoses Commons, Infectious Disease Commons, and the Skin and Connective Tissue Diseases Commons Recommended Citation Baumgardner DJ. Fungal infections from human and animal contact. J Patient Cent Res Rev. 2017;4:78-89. doi: 10.17294/2330-0698.1418 Published quarterly by Midwest-based health system Advocate Aurora Health and indexed in PubMed Central, the Journal of Patient-Centered Research and Reviews (JPCRR) is an open access, peer-reviewed medical journal focused on disseminating scholarly works devoted to improving patient-centered care practices, health outcomes, and the patient experience. REVIEW Fungal Infections From Human and Animal Contact Dennis J. Baumgardner, MD Aurora University of Wisconsin Medical Group, Aurora Health Care, Milwaukee, WI; Department of Family Medicine and Community Health, University of Wisconsin School of Medicine and Public Health, Madison, WI; Center for Urban Population Health, Milwaukee, WI Abstract Fungal infections in humans resulting from human or animal contact are relatively uncommon, but they include a significant proportion of dermatophyte infections. Some of the most commonly encountered diseases of the integument are dermatomycoses. Human or animal contact may be the source of all types of tinea infections, occasional candidal infections, and some other types of superficial or deep fungal infections. This narrative review focuses on the epidemiology, clinical features, diagnosis and treatment of anthropophilic dermatophyte infections primarily found in North America. -

Updating the Taxonomy of Dermatophytes of the BCCM/ IHEM Collection According to the New Standard: a Phylogenetic Approach
Mycopathologia https://doi.org/10.1007/s11046-019-00338-7 (0123456789().,-volV)( 0123456789().,-volV) ORIGINAL ARTICLE Updating the Taxonomy of Dermatophytes of the BCCM/ IHEM Collection According to the New Standard: A Phylogenetic Approach F. Baert . D. Stubbe . E. D’hooge . A. Packeu . M. Hendrickx Received: 23 January 2019 / Accepted: 30 April 2019 Ó Springer Nature B.V. 2019 Abstract Recent taxonomical revisions based on floccosum as the only representative, fell within the multilocus gene sequencing have provided some Nannizzia clade, whereas the phylogenetic analysis, clarifications to dermatophyte (Arthrodermataceae) based on the ITS region alone, differentiates Epider- family tree. These changes promoted us to investigate mophyton from Nannizzia as a separate genus. Re- the impact of the changed nomenclature of the identification and reclassification of many strains in dermatophyte strains in the BCCM/IHEM fungal the collection have had a profound impact on the collection, which contains strains of all dermatophyte composition of the BCCM/IHEM dermatophyte col- genera except for Ctenomyces. For 688 strains from lection. The biggest change is the decline of preva- this collection, both internal transcribed spacer region lence of Arthroderma strains; starting with 103 strains, (ITS) and partial b-tubulin (BT) sequences were only 22 strains remain in the genus after reassessment. aligned and a multilocus phylogenetic tree was Most Arthroderma strains were reclassified into Tri- constructed. The ITS ? BT phylogentic tree was able chophyton, with A. benhamiae and A. van- to distinguish the genera Arthroderma, Lophophyton, breuseghemii leaving the genus. The amount of Microsporum, Paraphyton, Nannizzia and Trichophy- Microsporum strains also dropped significantly with ton with high certainty. -

NEWSLETTER 2017•Issue 2
NEWSLETTER 2017•Issue 2 page 2 Deep dermatophytosis page 4 Deep dermatophytosis: A case report page 5 Fereydounia khargensis: A new and uncommon opportunistic yeast from Malaysia page 6 Itraconazole: A quick guide for clinicians Visit us at AFWGonline.com and sign up for updates Editors’ welcome Dr Mitzi M Chua Dr Ariya Chindamporn Adult Infectious Disease Specialist Associate Professor Associate Professor Department of Microbiology Department of Microbiology & Parasitology Faculty of Medicine Cebu Institute of Medicine Chulalongkorn University Cebu City, Philippines Bangkok, Thailand This year we celebrate the 8th year of AFWG: 8 years of pursuing excellence in medical mycology throughout the region; 8 years of sharing expertise and encouraging like-minded professionals to join us in our mission. We are happy to once again share some educational articles from our experts and keep you updated on our activities through this issue. Deep dermatophytosis may be a rare skin infection, but late diagnosis or ineffective treatment may lead to mortality in some cases. This issue of the AFWG newsletter focuses on this fungal infection that usually occurs in immunosuppressed individuals. Dr Pei-Lun Sun takes us through the basics of deep dermatophytosis, presenting data from published studies, and emphasizes the importance of treating superficial tinea infections before starting immunosuppressive treatment. Dr Ruojun Wang and Professor Ruoyu Li share a case of deep dermatophytosis caused by Trichophyton rubrum. In this issue, we also feature a new fungus, Fereydounia khargensis, first discovered in 2014. Ms Ratna Mohd Tap and Dr Fairuz Amran present 2 cases of F. khargensis and show how PCR sequencing is crucial to correct identification of this uncommon yeast. -

Fungal Evolution: Major Ecological Adaptations and Evolutionary Transitions
Biol. Rev. (2019), pp. 000–000. 1 doi: 10.1111/brv.12510 Fungal evolution: major ecological adaptations and evolutionary transitions Miguel A. Naranjo-Ortiz1 and Toni Gabaldon´ 1,2,3∗ 1Department of Genomics and Bioinformatics, Centre for Genomic Regulation (CRG), The Barcelona Institute of Science and Technology, Dr. Aiguader 88, Barcelona 08003, Spain 2 Department of Experimental and Health Sciences, Universitat Pompeu Fabra (UPF), 08003 Barcelona, Spain 3ICREA, Pg. Lluís Companys 23, 08010 Barcelona, Spain ABSTRACT Fungi are a highly diverse group of heterotrophic eukaryotes characterized by the absence of phagotrophy and the presence of a chitinous cell wall. While unicellular fungi are far from rare, part of the evolutionary success of the group resides in their ability to grow indefinitely as a cylindrical multinucleated cell (hypha). Armed with these morphological traits and with an extremely high metabolical diversity, fungi have conquered numerous ecological niches and have shaped a whole world of interactions with other living organisms. Herein we survey the main evolutionary and ecological processes that have guided fungal diversity. We will first review the ecology and evolution of the zoosporic lineages and the process of terrestrialization, as one of the major evolutionary transitions in this kingdom. Several plausible scenarios have been proposed for fungal terrestralization and we here propose a new scenario, which considers icy environments as a transitory niche between water and emerged land. We then focus on exploring the main ecological relationships of Fungi with other organisms (other fungi, protozoans, animals and plants), as well as the origin of adaptations to certain specialized ecological niches within the group (lichens, black fungi and yeasts). -

Candida Auris
microorganisms Review Candida auris: Epidemiology, Diagnosis, Pathogenesis, Antifungal Susceptibility, and Infection Control Measures to Combat the Spread of Infections in Healthcare Facilities Suhail Ahmad * and Wadha Alfouzan Department of Microbiology, Faculty of Medicine, Kuwait University, P.O. Box 24923, Safat 13110, Kuwait; [email protected] * Correspondence: [email protected]; Tel.: +965-2463-6503 Abstract: Candida auris, a recently recognized, often multidrug-resistant yeast, has become a sig- nificant fungal pathogen due to its ability to cause invasive infections and outbreaks in healthcare facilities which have been difficult to control and treat. The extraordinary abilities of C. auris to easily contaminate the environment around colonized patients and persist for long periods have recently re- sulted in major outbreaks in many countries. C. auris resists elimination by robust cleaning and other decontamination procedures, likely due to the formation of ‘dry’ biofilms. Susceptible hospitalized patients, particularly those with multiple comorbidities in intensive care settings, acquire C. auris rather easily from close contact with C. auris-infected patients, their environment, or the equipment used on colonized patients, often with fatal consequences. This review highlights the lessons learned from recent studies on the epidemiology, diagnosis, pathogenesis, susceptibility, and molecular basis of resistance to antifungal drugs and infection control measures to combat the spread of C. auris Citation: Ahmad, S.; Alfouzan, W. Candida auris: Epidemiology, infections in healthcare facilities. Particular emphasis is given to interventions aiming to prevent new Diagnosis, Pathogenesis, Antifungal infections in healthcare facilities, including the screening of susceptible patients for colonization; the Susceptibility, and Infection Control cleaning and decontamination of the environment, equipment, and colonized patients; and successful Measures to Combat the Spread of approaches to identify and treat infected patients, particularly during outbreaks. -

Fungal Infection in the Lung
CHAPTER Fungal Infection in the Lung 52 Udas Chandra Ghosh, Kaushik Hazra INTRODUCTION The following risk factors may predispose to develop Pneumonia is the leading infectious cause of death in fungal infections in the lungs 6 1, 2 developed countries . Though the fungal cause of 1. Acute leukemia or lymphoma during myeloablative pneumonia occupies a minor portion in the immune- chemotherapy competent patients, but it causes a major role in immune- deficient populations. 2. Bone marrow or peripheral blood stem cell transplantation Fungi may colonize body sites without producing disease or they may be a true pathogen, generating a broad variety 3. Solid organ transplantation on immunosuppressive of clinical syndromes. treatment Fungal infections of the lung are less common than 4. Prolonged corticosteroid therapy bacterial and viral infections and very difficult for 5. Acquired immunodeficiency syndrome diagnosis and treatment purposes. Their virulence varies from causing no symptoms to death. Out of more than 1 6. Prolonged neutropenia from various causes lakh species only few fungi cause human infection and 7. Congenital immune deficiency syndromes the most vulnerable organs are skin and lungs3, 4. 8. Postsplenectomy state RISK FACTORS 9. Genetic predisposition Workers or farmers with heavy exposure to bird, bat, or rodent droppings or other animal excreta in endemic EPIDEMIOLOGY OF FUNGAL PNEUMONIA areas are predisposed to any of the endemic fungal The incidences of invasive fungal infections have pneumonias, such as histoplasmosis, in which the increased during recent decades, largely because of the environmental exposure to avian or bat feces encourages increasing size of the population at risk. This population the growth of the organism. -

Severe Chromoblastomycosis-Like Cutaneous Infection Caused by Chrysosporium Keratinophilum
fmicb-08-00083 January 25, 2017 Time: 11:0 # 1 CASE REPORT published: 25 January 2017 doi: 10.3389/fmicb.2017.00083 Severe Chromoblastomycosis-Like Cutaneous Infection Caused by Chrysosporium keratinophilum Juhaer Mijiti1†, Bo Pan2,3†, Sybren de Hoog4, Yoshikazu Horie5, Tetsuhiro Matsuzawa6, Yilixiati Yilifan1, Yong Liu1, Parida Abliz7, Weihua Pan2,3, Danqi Deng8, Yun Guo8, Peiliang Zhang8, Wanqing Liao2,3* and Shuwen Deng2,3,7* 1 Department of Dermatology, People’s Hospital of Xinjiang Uygur Autonomous Region, Urumqi, China, 2 Department of Dermatology, Shanghai Changzheng Hospital, Second Military Medical University, Shanghai, China, 3 Key Laboratory of Molecular Medical Mycology, Shanghai Changzheng Hospital, Second Military Medical University, Shanghai, China, 4 CBS-KNAW Fungal Biodiversity Centre, Royal Netherlands Academy of Arts and Sciences, Utrecht, Netherlands, 5 Medical Mycology Research Center, Chiba University, Chiba, Japan, 6 Department of Nutrition Science, University of Nagasaki, Nagasaki, Japan, 7 Department of Dermatology, First Hospital of Xinjiang Medical University, Urumqi, China, 8 Department of Dermatology, The Second Affiliated Hospital of Kunming Medical University, Kunming, China Chrysosporium species are saprophytic filamentous fungi commonly found in the Edited by: soil, dung, and animal fur. Subcutaneous infection caused by this organism is Leonard Peruski, rare in humans. We report a case of subcutaneous fungal infection caused by US Centers for Disease Control and Prevention, USA Chrysosporium keratinophilum in a 38-year-old woman. The patient presented with Reviewed by: severe chromoblastomycosis-like lesions on the left side of the jaw and neck for 6 years. Nasib Singh, She also got tinea corporis on her trunk since she was 10 years old. -

Managing Athlete's Foot
South African Family Practice 2018; 60(5):37-41 S Afr Fam Pract Open Access article distributed under the terms of the ISSN 2078-6190 EISSN 2078-6204 Creative Commons License [CC BY-NC-ND 4.0] © 2018 The Author(s) http://creativecommons.org/licenses/by-nc-nd/4.0 REVIEW Managing athlete’s foot Nkatoko Freddy Makola,1 Nicholus Malesela Magongwa,1 Boikgantsho Matsaung,1 Gustav Schellack,2 Natalie Schellack3 1 Academic interns, School of Pharmacy, Sefako Makgatho Health Sciences University 2 Clinical research professional, pharmaceutical industry 3 Professor, School of Pharmacy, Sefako Makgatho Health Sciences University *Corresponding author, email: [email protected] Abstract This article is aimed at providing a succinct overview of the condition tinea pedis, commonly referred to as athlete’s foot. Tinea pedis is a very common fungal infection that affects a significantly large number of people globally. The presentation of tinea pedis can vary based on the different clinical forms of the condition. The symptoms of tinea pedis may range from asymptomatic, to mild- to-severe forms of pain, itchiness, difficulty walking and other debilitating symptoms. There is a range of precautionary measures available to prevent infection, and both oral and topical drugs can be used for treating tinea pedis. This article briefly highlights what athlete’s foot is, the different causes and how they present, the prevalence of the condition, the variety of diagnostic methods available, and the pharmacological and non-pharmacological management of the -

HIV Infection and AIDS
G Maartens 12 HIV infection and AIDS Clinical examination in HIV disease 306 Prevention of opportunistic infections 323 Epidemiology 308 Preventing exposure 323 Global and regional epidemics 308 Chemoprophylaxis 323 Modes of transmission 308 Immunisation 324 Virology and immunology 309 Antiretroviral therapy 324 ART complications 325 Diagnosis and investigations 310 ART in special situations 326 Diagnosing HIV infection 310 Prevention of HIV 327 Viral load and CD4 counts 311 Clinical manifestations of HIV 311 Presenting problems in HIV infection 312 Lymphadenopathy 313 Weight loss 313 Fever 313 Mucocutaneous disease 314 Gastrointestinal disease 316 Hepatobiliary disease 317 Respiratory disease 318 Nervous system and eye disease 319 Rheumatological disease 321 Haematological abnormalities 322 Renal disease 322 Cardiac disease 322 HIV-related cancers 322 306 • HIV INFECTION AND AIDS Clinical examination in HIV disease 2 Oropharynx 34Neck Eyes Mucous membranes Lymph node enlargement Retina Tuberculosis Toxoplasmosis Lymphoma HIV retinopathy Kaposi’s sarcoma Progressive outer retinal Persistent generalised necrosis lymphadenopathy Parotidomegaly Oropharyngeal candidiasis Cytomegalovirus retinitis Cervical lymphadenopathy 3 Oral hairy leucoplakia 5 Central nervous system Herpes simplex Higher mental function Aphthous ulcers 4 HIV dementia Kaposi’s sarcoma Progressive multifocal leucoencephalopathy Teeth Focal signs 5 Toxoplasmosis Primary CNS lymphoma Neck stiffness Cryptococcal meningitis 2 Tuberculous meningitis Pneumococcal meningitis 6 -

Exd.13726 - Auteur(S)
Institutional Repository - Research Portal Dépôt Institutionnel - Portail de la Recherche University of Namurresearchportal.unamur.be RESEARCH OUTPUTS / RÉSULTATS DE RECHERCHE In vitro models of dermatophyte infection to investigate epidermal barrier alterations Faway, Émilie; Lambert De Rouvroit, Catherine; Poumay, Yves Published in: Experimental dermatology DOI: Author(s)10.1111/exd.13726 - Auteur(s) : Publication date: 2018 Document Version PublicationPublisher's date PDF, - also Date known de aspublication Version of record : Link to publication Citation for pulished version (HARVARD): Faway, É, Lambert De Rouvroit, C & Poumay, Y 2018, 'In vitro models of dermatophyte infection to investigate Permanentepidermal link barrier - Permalien alterations', Experimental : dermatology, vol. 27, no. 8, pp. 915-922. https://doi.org/10.1111/exd.13726 Rights / License - Licence de droit d’auteur : General rights Copyright and moral rights for the publications made accessible in the public portal are retained by the authors and/or other copyright owners and it is a condition of accessing publications that users recognise and abide by the legal requirements associated with these rights. • Users may download and print one copy of any publication from the public portal for the purpose of private study or research. • You may not further distribute the material or use it for any profit-making activity or commercial gain • You may freely distribute the URL identifying the publication in the public portal ? Take down policy If you believe that this document -
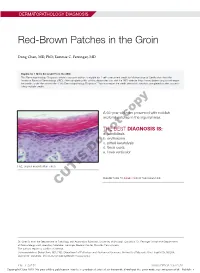
Red-Brown Patches in the Groin
DERMATOPATHOLOGY DIAGNOSIS Red-Brown Patches in the Groin Dong Chen, MD, PhD; Tammie C. Ferringer, MD Eligible for 1 MOC SA Credit From the ABD This Dermatopathology Diagnosis article in our print edition is eligible for 1 self-assessment credit for Maintenance of Certification from the American Board of Dermatology (ABD). After completing this activity, diplomates can visit the ABD website (http://www.abderm.org) to self-report the credits under the activity title “Cutis Dermatopathology Diagnosis.” You may report the credit after each activity is completed or after accumu- lating multiple credits. A 66-year-old man presented with reddish arciform patchescopy in the inguinal area. THE BEST DIAGNOSIS IS: a. candidiasis b. noterythrasma c. pitted keratolysis d. tinea cruris Doe. tinea versicolor H&E, original magnification ×600. PLEASE TURN TO PAGE 419 FOR THE DIAGNOSIS CUTIS Dr. Chen is from the Department of Pathology and Anatomical Sciences, University of Missouri, Columbia. Dr. Ferringer is from the Departments of Dermatology and Laboratory Medicine, Geisinger Medical Center, Danville, Pennsylvania. The authors report no conflict of interest. Correspondence: Dong Chen, MD, PhD, Department of Pathology and Anatomical Sciences, University of Missouri, One Hospital Dr, MA204, DC018.00, Columbia, MO 65212 ([email protected]). 416 I CUTIS® WWW.MDEDGE.COM/CUTIS Copyright Cutis 2018. No part of this publication may be reproduced, stored, or transmitted without the prior written permission of the Publisher. DERMATOPATHOLOGY DIAGNOSIS DISCUSSION THE DIAGNOSIS: Erythrasma rythrasma usually involves intertriginous areas surface (Figure 1) compared to dermatophyte hyphae that (eg, axillae, groin, inframammary area). Patients tend to be parallel to the surface.2 E present with well-demarcated, minimally scaly, red- Pitted keratolysis is a superficial bacterial infection brown patches.