The Two-Stage Brachial Artery–Brachial Vein Autogenous Fistula for Hemodialysis
Total Page:16
File Type:pdf, Size:1020Kb
Load more
Recommended publications
-

DVT Upper Extremity
UT Southwestern Department of Radiology Ultrasound – Upper Extremity Deep Venous Thrombosis Evaluation PURPOSE: To evaluate the upper extremity superficial and deep venous system for patency. SCOPE: Applies to all ultrasound venous Doppler studies of the lower extremities in Imaging Services / Radiology EPIC ORDERABLE: • UTSW: US DOPPLER VENOUS DVT UPPER EXTREMITY BILATERAL US DOPPLER VENOUS DVT UPPER EXTREMITY RIGHT US DOPPLER VENOUS DVT UPPER EXTREMITY LEFT • PHHS: US DOPPLER VENOUS DVT UPPER EXTREMITY BILATERAL US DOPPLER VENOUS DVT UPPER EXTREMITY RIGHT US DOPPLER VENOUS DVT UPPER EXTREMITY LEFT INDICATIONS: • Symptoms such as upper extremity swelling, pain, fever, warmth, change in color, palpable cord • Suspected venous occlusion, or DVT based on clinical prediction rules (eg. Well’s score or D- Dimer) • Indwelling or recent PICC or central line • Chest pain and/or shortness of breath • Suspected or known pulmonary embolus • Follow-up known deep venous thrombosis (DVT) CONTRAINDICATIONS: No absolute contraindications EQUIPMENT: Preferably a linear array transducer that allows for appropriate resolution of anatomy (frequency range of 9 mHz or greater), capable of duplex imaging. Sector or curvilinear transducers may be required for appropriate penetration in patients with edema or large body habitus. PATIENT PREPARATION: • None EXAMINATION: GENERAL GUIDELINES: A complete examination includes evaluation of the superficial and deep venous system of the upper extremity including the internal jugular, innominate, subclavian, axillary, paired brachial, basilic, and cephalic veins. EXAM INITIATION: • Introduce yourself to the patient • Verify patient identity using patient name and DOB • Explain test • Obtain patient history including symptoms. Enter and store data page US DVT Upper Extremity 05-31-2020.docx 1 | Page Revision date: 05-31-2020 UT Southwestern Department of Radiology • Place patient in supine position with arm extended TECHNICAL CONSIDERATIONS: • Review any prior imaging, making note of any previous thrombus burden. -

Brachial Artery
VASCULAR Anatomy of the upper limb Dr Jamila EL M edany & Dr. Essam Eldin Salama Objectives At the end of the lecture, the students should be able to: • Identify the origin of the vascular supply for the upper limb. • Describe the main arteries and their branches of the arm, forearm & hand. • Describe the vascular arches for the hand. • Describe the superficial and deep veins of the upper limb Arteries Of The Upper Limb Right subclavian Left subclavian artery artery Axillary artery Brachial artery Ulnar artery Radial artery Palmar arches The Subclavian Artery The right artery originates from the brachiocephalic artery. The left artery Cotinues as originates from Axillary artery at the arch of the the lateral border aorta of the 1st rib The Axillary Artery Begins at the lateral border of the st 1 rib as continuation of the Subclavian artery subclavian artery. Continues as brachial artery at lower border of teres major muscle. Is closely related to the cords of brachial plexus and their branches Is enclosed within the axillary sheath. Is crossed anteriorly by the pectoralis minor muscle, and is st nd divided into three parts; 1 , 2 & Brachial artery Axillary artery 3rd. The 1st part of the axillary artery . Extends from the lateral st border of 1 rib to upper 1st part border of the pectoralis 2nd part minor muscle. Highest thoracic artery a. Related: 3rd part Pectoralis • Anterioly: to the minor pectoralis major muscle • Laterally: to the cords Teres of the brachial plexus. major . It gives; ONE branch: Highest thoracic artery The 2nd part of the axillary artery . -

Brachial Vein Transposition with Consecutive Skin Incisions in a Hemodialysis Patient with Absence of Adequate Superficial Veins: a Case Report
Original Article Case Report Case Vascular Specialist International Vol. 36, No. 4, December 2020 pISSN 2288-7970 • eISSN 2288-7989 Brachial Vein Transposition with Consecutive Skin Incisions in a Hemodialysis Patient with Absence of Adequate Superficial Veins: A Case Report Pouya Tayebi1, Fatemeh Mahmoudlou2, Yasaman Daryabari2, and Atefeh Shamsian3 1Department of Vascular and Endovascular Surgery, Rouhani Hospital, Babol University of Medical Sciences, Babol, 2Student Research Committee, Babol University of Medical Sciences, Babol, 3MSc student in nursing, Rajaie Cardiovascular Medical and Research Center, Iran University of Medical Sciences,Tehran, Iran The creation of an arteriovenous fistula instead of a synthetic vascular graft is a Received September 24, 2020 Revised November 5, 2020 smart decision in hemodialysis patients who do not have a suitable superficial vein. Accepted November 30, 2020 Basilic vein transposition (BVT) is a viable option in most cases, except in patients who do not have a proper basilic vein. In patients with inadequate superficial veins, another source of the autogenous vein is the brachial vein, a deep vein of the up- per arm. Most surgeons choose a full medial arm incision to perform brachial vein Corresponding author: Pouya Tayebi exploration. We describe a patient in whom BVT was not possible and so brachial Department of Vascular and Endovascular Surgery, Rouhani Hospital, Babol University vein transposition using skip incisions was performed, with good results. of Medical Sciences, Keshavarz Boulevard, -

View, There Is No Doubt That the Elbow Should Be Reduced and Repositioned As Soon As the Diagnosis
ACTA SCIENTIFIC MEDICAL SCIENCES (ISSN: 2582-0931) Volume 4 Issue 1 January 2020 Case Report Use of A Brachial Vein Conduit and A Rotational Skin Flap Graft Repairing A Vascular Trauma Yuniel Hernandez Castillo* Consultant Angiologist and Vascular Surgeon, General Surgery, Milton Cato Memorial Hospital, Saint Vincent and the Grenadines, Caribbean *Corresponding Author: Yuniel Hernandez Castillo, Consultant Angiologist and Vascular Surgeon, General Surgery, Milton Cato Memorial Hospital, Saint Vincent and the Grenadines, Caribbean. Received: November 22, 2019; Published: December 04, 2019 DOI: 10.31080/ASMS.2020.04.0492 Abstract Introduction: Elbow dislocations are sometimes associated with neurovascular injuries where brachial artery is the most frequently injured artery requiring emergency and adequate often complex surgical treatment in order to manage their severe complications. The literature consists of only a few limited case reports on associated vascular or neurovascular injuries resulting from this type of trauma with no reference to the particular techniques we combined to treat our patient. Presentation of Case: We present a Brachial Artery reconstruction in a 31-year-old patient with an Open Complex Right Elbow Dislocation. In the Clinical and Surgical Examination an open wound in the Anterior-Medial Right Antecubital Fossa presented with to-End Anastomosis was conducted using an Autologous Reverse Brachial Vein Conduit graft from the ipsilateral arm under General accompanying Brachial Pedicle all structures Transection was confirm. To repair the Brachial Artery a Substitution By-Pass and End- Anesthesia. For the Wound Closure a Rotational Skin and subcutaneous Fat Flap Graft. Postoperative patient progress, it was suc- cessful developing no Systemic Complications nor Ischemic Signs in the Right Upper Limb being discharge for Out-Patient follow-up through the By-pass and distal limb. -

Vascular / Endovascular Surgery Vascular / Endovascular Surgery Combat Manual Combat Manual
Vascular / Endovascular Surgery / Endovascular Vascular Vascular / Endovascular Surgery Combat Manual Combat Manual Combat W. L. Gore & Associates, Inc. Flagstaff, AZ 86004 +65.67332882 (Asia Pacific) 800.437.8181 (United States) 00800.6334.4673 (Europe) 928.779.2771 (United States) goremedical.com Stone Stone AbuRahma Campbell GORE®, EXCLUDER®, TAG®, VIABAHN®, and designs are trademarks of W. L. Gore & Associates. AbuRahma © 2012, 2013 W. L. Gore & Associates, Inc. AS0315-EN1 JULY 2013 Campbell Compliments of W. L. Gore & Associates, Inc. This publication, compliments of W. L. Gore & Associates, Inc. (Gore), is intended to serve as an educational resource for medical students, residents, and fellows pursuing training in vascular and endovascular surgery. Readers are reminded to consult appropriate references before engaging in any patient diagnosis, treatment, or surgery, including Prescribing Information (including boxed warnings and medication guides), Instructions for Use, and other applicable current information available from manufacturers. Gore products referenced within are used within their FDA approved / cleared indications. Gore does not have knowledge of the indications and FDA approval / clearance status of non-Gore products, and Gore does not advise or recommend any surgical methods or techniques other than those described in the Instructions for Use for its devices. Gore makes no representations or warranties as to the PERCLOSE®, PROSTAR®, SPARTACORE®, STARCLOSE®, and SUPRACORE® are trademarks of Abbott Laboratories. surgical techniques, medical conditions, or other factors that OMNI FLUSH and SIMMONS SIDEWINDER are trademarks of AngioDynamics. ICAST is a trademark of Atrium Medical Corporation. ASPIRIN® is a trademark of Bayer HealthCare, LLC. MORPH® is a trademark of BioCardia, may be described in this publication. -

33. Vessels of the Upper Limb
BOGOMOLETS NATIONAL MEDICAL UNIVERSITY Department of Human Anatomy GUIDELINES Academic discipline HUMAN ANATOMY Module № 2 The theme of the lesson The vessels of the upper limb. Course І Faculties Medical 1,2,3,4, military, dental The number of hours 3 2017 1. Theme relevance: The anatomy of the shoulder and arm are very importance, because without the knowledge about peculiarities and variants of structure, form, location and mutual location of their anatomical structures, their age-specific it is impossible to diagnose in a proper time and correctly and to prescribe a necessary treatment to the patient. Surgeons and traumatologists usually pay much attention to the anatomy of the upper extremities. 2. Specific objectives: Describe, classify, analizy blood vessels of the scapular waist and forearm. a. axillaris –determine the borders of axillary artery, designate and demonstrate the branches axillary artery a.brachialis- determine the meatus, borders, branches . a. profunda brachii- branches. a.ulnaris- determine the borders, branches. a.radialis- determine the borders. Know the v.cephalica, basilica, mediana cubiti. 3. Basic level of preparation, including a knowledge of osteology, myology. The student should know the anatomy of the course: the structure, classification of the tubular bones of the upper limb, muscles of the arm and forearm, classification of the junction of the bones of the skeleton. To know peculiarities and variants of structure, form, location of upper extremities. 4. Tasks for independent work during preparation for classes. Magistral artery of the upper limb a.axillaris, a.brachalis, a.ulnaris, a.radial, superficial palmar arch, general digital palmar artery, proper palmar digital artery, deep palmar arch, palmar metacarpal artery. -

Of the Elbow Veins
DUPLEX PRE OPERATIVE MAPPING APPLICABILITY OF PERCUTANEOUS AVF CREATION BASED ON A PROSPECTIVE ULTRASOUND EVALUATION G.FRANCO CLINIQUE ARAGO PARIS Disclosure Speaker name: G. FRANCO ................................................................................. I have the following potential conflicts of interest to report: Consulting Employment in industry Shareholder in a healthcare company Owner of a healthcare company Other(s) + I do not have any potential conflict of interest AVF at wrist is the first option for vascular access creation (KDOQI, EBPG) despite: High early thrombosis and non-maturation rate ranging from 5 to 50% PERFORATING VEIN AT CUBITAL FOSSA Valuable resource for the creation of a vascular access Surprisingly it doesn’t take any place in the recommendations of AVF creation WHEREAS Easy to perform surgically or now better PERCUTANEOUSLY Allows future construction of AVF using the predilated veins if necessary: CV-BV -BR VEINS Percutaneous AVF creation with ELLIPSIS® vascular access system between deep communicating vein (DCV) and proximal radial artery (PRA) Needs to meet specific anatomic criteria The specific study of the deep communicating vein( DCV) at the elbow is not part of the USUAL VASCULAR MAPPING Except when it is the only drainage of the veins of the forearm BUT NOW The advent of percutaneous AVF creation MAKES THIS STUDY MANDATORY Knowledge of the venous arrangements of the cubital fossa may imply better outcomes and lower complications rates of the procedure THE ASSESSMENT BEFORE PERCUTANEOUS AV FISTULA IS FOCUSED ON THE ANTECUBITAL FOSSA. SPECIFIC EXAMINATION INCLUDES -DCV WALL QUALITY & Ø -DISTRIBUTION OF VENOUS M -PATENCY of CV/BV -RELATIONSHIP WITH THE PRA QUALITY OF PRA WALL and Ø -PATENCY OF BRACHIAL VEINS • SPONTANEOUS DRAINAGE FLOW • TOURNIQUET ABOVE THE ELBOW AND PROXIMAL • DRAINAGE TEST BELOW THE TOURNIQUET RA [BA] Calcifications downstream ∅ :2.8 mm -15mm with normal wall Proximal radial artery is about 30% bigger than distal radial artery . -
Upper Limb- Part II
Upper limb- Part II Muscles, Nerves and Arteries of the Arm Brachial fascia (deep fascia of the arm) Brachial fascia is a continuation of the pectoral and axillary fasciae and passes in the antebrachial fascia Brachial fascia sends 2 intermuscular septa (lateral and medial) dividing the arm into 2 compartments: Anterior compartment of arm Posterior compartment of arm Muscles of the arm Muscles of the anterior compartment of arm (flexors)- innervated by musculocutaneous nerve Coracobrachialis Biceps brachii Brachialis Muscles of the posterior compartment of arm (extensors)- innervated by radial nerve Triceps brachii Anconeus Coracobrachialis Muscles of the anterior compartment of arm Coracobrachialis Attachments Origin • Coracoid process of scapula Insertion • Medial third of medial surface of humerus body Innervation Musculocutaneous nerve which pierces its belly Muscles of the anterior compartment of arm Coracobrachialis Main action Resists downward dislocation of the head of humerus, especially during carrying heavy objects Flexion and adduction in the glenohumeral joint Biceps brachii Muscles of the anterior compartment of arm Biceps brachii Its proximal part is divided into 2 heads Short head Long head Origin of the short head Coracoid process of scapula Origin of the long head Supraglenoid tubercle of scapula Its tendon occupies intertubercular groove and is situated within the shoulder joint Insertion of the entire muscle Radial tuberosity (tendon situated within the cubital fossa) Bicipital aponeurosis -
SVU GLOSSARY of TERMS Ampere: a Unit of Electromotive Force; One Volt Acting Against the Resistance of One Ohm (See Ohm’S Law)
5TH EDITION GLOSSARY OF TERMS Terminology for the Vascular Ultrasound Technologist/ Sonographer SOCIETY FOR VASCULAR ULTRASOUND The VOICE for the Vascular Ultrasound Profession 5TH EDITION Glossary of Terms Terminology for the Vascular Ultrasound Technologist/ Sonographer CONTENTS Alphabetical Glossary . .1 Prefixes . .75 Suffixes . .76 Acronyms . .77 Acknowledgements The Glossary of Terms for the Vascular Technologists was first compiled in 1983 by the Education Committee of the then Society of Non-Invasive Vascular Technol- ogy, Mary Jane Pomajzl, Chair. The Glossary has since been updated three times. The second edition was published in 1989 under the direc- tion of Paula A. Heggerick, RDMS RVT FSVU, Chair, SVT Publication Committee. The third edition was published in 1995; Joanne E. Drago, LPN RVT, Chair. The fourth edition was revised and updated in 2001 due to the efforts of Jean White, RVT, Chair, and Allene Woodley, RN RVT; Joanne Spindell, RVT RDCS; Paula Gehr, RVT; Cathy Brown, BSCVN RN RVT RDCVS; and Michael Sampson, RVT. This fifth edition has been revised and updated in 2005 due to the efforts of Products Committee Chair Michel Comeaux, RN RVT RDMS FSVU; Tom Baer, MBA RVT RDMS RDCS; Debbie Pirt, AS RVT; William Harkrider, MD RVT; and Bill Zang, BS RVT RDMS. © Copyright 2005 Society for Vascular Ultrasound 4601 Presidents Drive, Suite 260 Lanham, MD 20706-4831 Tel. 301-459-7550 Fax: 301-459-5651 Web: www.svunet.org The VOICE for the Vascular Ultrasound Profession A A-C coupling (Alternating Current): Type of output signal to graphic display connection which responds to changes faster than 0.5Hz. -
Bones of Upper Limb
ARM, CUBITAL FOSSA & ELBOW JOINT Khaleel Alyahya, PhD, MEd King Saud University College of Medicine @khaleelya OBJECTIVES At the end of the lecture, students should: o - Describe the attachments, actions and innervations of: Biceps brachii Coracobrachialis Brachialis Triceps brachii o - Demonstrate the following features of the elbow joint: Articulating bones Capsule Lateral & medial collateral ligaments Synovial membrane o - Demonstrate the movements; flexion and extension of the elbow. o - List the main muscles producing the above movements. o - Define the boundaries of the cubital fossa and enumerate its contents. THE ARM THE ARM o An aponeurotic sheet separating various muscles of Lateral Medial the upper limbs, including intermuscul intermuscul lateral and medial humeral septa. ar septum ar septum o The lateral and medial intermuscular septa divide the Neurovascul distal part of the arm into two ski ar bundle compartments: n • Anterior compartments Fasci . also known as the flexor a compartment Humer • Posterior compartments us . also known as the extensor compartment ANTERIOR FASCIAL COMPARTMENT . Muscles: Biceps brachii, Coracobrachialis &Brachialis. Blood Vessels: Brachial artery & Basilic vein. Nerves: Musculocutaneous and Median. MUSCLES OF ANTERIOR COMPARTMENT Coracobrachialis Biceps Brachii Brachialis BICEPS BRACHII . Origin: Two heads: • Long Head from supraglenoid tubercle of scapula (intracapsular) • Short Head from the tip of coracoid process of scapula • The two heads join in the middle of the arm . Insertion: • In the posterior part of the radial tuberosity. • Into the deep fascia of the medial aspect of the forearm through bicipital aponeurosis. Nerve supply: • Musculocutaneous . Action: • Strong supinator of the forearm • used in screwing. • Powerful flexor of elbow • Weak flexor of shoulder CORACOBRACHIALIS . -
ARM and ELBOW Doctors Notes Editing File Notes/Extra Explanation Objectives
Color Code Important ARM AND ELBOW Doctors Notes Editing file Notes/Extra explanation Objectives ü Describe the attachments, actions and innervations of: • Biceps brachii • Coracobrachialis • Brachialis • Triceps brachii ü Demonstrate the following features of the elbow joint: • Articulating bones • Capsule • Lateral & medial collateral ligaments • Synovial membrane ü Demonstrate the movements; flexion and extension of the elbow. ü List the main muscles producing the above movements. ü Define the boundaries of the cubital fossa and enumerate its contents. Shoulder THE ARM: - An aponeurotic sheet separating various muscles A R M of the upper limbs, including lateral and medial Posterior Anterior humeral septa. view view Elbow - The lateral and medial intermuscular septa divide the distal part of the arm into two compartments: Arm Humerus Lateral Medial intermuscular intermuscular Posterior septum septum Anterior (flexor (extensor compartment) compartment) Neurovascular skin bundle Fascia Humerus Note: the radial and ulnar nerves begin in Anterior Fascial Compartment: the anterior compartment then pierce the intermuscular septum and enter the posterior compartment Radial Brachialis Basilic vein Median Biceps Ulnar brachii Brachial Musculocutaneous artery coracobrachiallis muscles Blood vessels Nerves Muscles Of Anterior Compartment: Coracobrachialis Biceps Brachii Brachialis Note: Brachi- means arm so any muscle with brachi in it’s name is related to the arm Coracoid Process BICEPS BRACHII: • Long Head from supraglenoid tubercle of scapula (intracapsular) Origin • Short Head from the tip of coracoid process of scapula The two heads join in the middle of the arm Insertion • In the posterior part of the radial tuberosity. • Into the deep fascia of the medial aspect of the forearm through bicipital aponeurosis. -
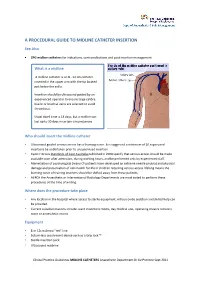
A Procedural Guide to Midline Catheter Insertion
A PROCEDURAL GUIDE TO MIDLINE CATHETER INSERTION See Also CPG midline catheters for indications, contraindications and post insertion management What is a midline A midline catheter is an 8 - 12 cm catheter inserted in the upper arm with the tip located just below the axilla. Insertion should be ultrasound guided by an experienced operator to ensure large calibre basilic or brachial veins are selected to avoid thrombosis. Usual dwell time is 14 days, but a midline can last up to 30 days in certain circumstances Who should insert the midline catheter • Ultrasound guided venous access has a learning curve. It is suggested a minimum of 20 supervised insertions be undertaken prior to unsupervised insertion. • Cystic Fibrosis Standards of Care Australia published in 2008 specify that venous access should be made available soon after admission, during working hours, and be performed only by experienced staff. • Minimization of psychological (many CF patients have developed an extreme needle phobia) and physical damage and preservation of vein health for life in children requiring venous access lifelong means the learning curve of training inserters should be shifted away from these patients. • At RCH the Anaesthetic or Interventional Radiology Departments are most suited to perform these procedures at the time of writing. Where does the procedure take place • Any location in the hospital where access to sterile equipment, nitrous oxide sedation and skilled help can be provided. • Current suitable locations include: ward treatment rooms, day