Bones of Upper Limb
Total Page:16
File Type:pdf, Size:1020Kb
Load more
Recommended publications
-

The Morphology of Common Interosseous Artery and Its Clinical
Scholars Journal of Applied Medical Sciences (SJAMS) ISSN 2320-6691 (Online) Sch. J. App. Med. Sci., 2015; 3(3B):1126-1131 ISSN 2347-954X (Print) ©Scholars Academic and Scientific Publisher (An International Publisher for Academic and Scientific Resources) www.saspublisher.com Research Article The Morphology of Common Interosseous Artery and its Clinical Significance Waseem Al Talalwah1*, Dereje Getachew2 and Roger Soames3 1King Abdullah International Medical Research Center / King Saud bin Abdulaziz University for Health Sciences, College of Medicine, Department of Basic Medical Sciences Hospital – NGHA, Riyadh, P.O. Box 3660, Riyadh 2Anatomy Department, College of Medicine and Health sciences, Hawassa University, Awassa, 1560 3Centre for Anatomy and Human Identification, College of Art, Science and Engineering, University of Dundee Dundee, DD1 5EH, UK *Corresponding author Dr. Waseem Al-Talalwah Abstract: The common interosseous artery is main branch the ulnar artery which divides into anterior and posterior interosseous branches. The current study investigates common interosseous artery and its branch to provide detailed information regarding the morphology which would be of use to clinicians, orthopaedic surgeons, plastic surgeons and anatomists. Routine dissections of the right and left upper limb of 34 adult cadavers (20 male and 14 female: mean age 78.9 year) were undertaken. The common interosseous artery presents in 67.6% whereas it is congenital absence in 32.4%. The origin distance of bifurcation of common interosseous from the ulnar artery origin is between 33.11 and 33.45 mm. The anterior and posterior interosseous arteries present in 98.5% and 92.9% whereas they are congenital absence in 1.5% and 7.1% respectively in total cases. -

Additional Branch of Brachial Artery Terminating in Superficial Palmar Arch
International Journal of Advances in Science Engineering and Technology, ISSN(p): 2321 –8991, ISSN(e): 2321 –9009 Vol-6, Iss-1, Spl. Issue-2 Mar.-2018, http://iraj.in ADDITIONAL BRANCH OF BRACHIAL ARTERY TERMINATING IN SUPERFICIAL PALMAR ARCH 1BILLAKANTI PRAKASH BABU, 2HUBAN THOMAS 1Associate Professor, Kasturba Medical College/Manipal Academy of Higher Education, Anatomy Department, Kasturba Medical College,Manipal,KARNATAKA-INDIA,576104 2Senior Lecturer, Kasturba Medical College/Manipal Academy of Higher Education, Anatomy Department, Kasturba Medical College,Manipal,KARNATAKA-INDIA,576104 E-mail: [email protected], [email protected] Abstract - Superficial palmar arch is an arterial arcade in the palm of the hand formed by superficial branch of ulnar artery and can be completed on lateral side by superficial palmar branch of radial artery or any one of these arteries viz. princeps pollicis artery, radialis indicis artery or the median artery. The arch develops as a terminal plexus of axis artery of upper limb which is later joined by median, ulnar and radial arteries as these arteries develop. The present study was conducted in the Department of Anatomy, Kasturba Medical College, Manipal Academy of Higher Education, Manipal, India on 60 formalin fixed adult human cadaver hands. Out of 60 (30 on right and 30 on left side) in one specimen a unique variation was encountered in the arteries taking part in the formation of superficial palmar arch on the right side. Superficial palmar arch formation was normal and in addition an additional branch arose from the medial side of the brachial artery just below the middle of the arm. -

Anatomy, Shoulder and Upper Limb, Brachial Artery
NCBI Bookshelf. A service of the National Library of Medicine, National Institutes of Health. StatPearls [Internet]. Treasure Island (FL): StatPearls Publishing; 2018 Jan-. Anatomy, Shoulder and Upper Limb, Brachial Artery Authors Thomas N. Epperson1; Matthew Varacallo2. Affiliations 1 University of Louisville School of Med. 2 Department of Orthopaedic Surgery, University of Kentucky School of Medicine Last Update: January 4, 2019. Introduction The brachial artery is the extension of the axillary artery starting at the lower margin of the teres major muscle and is the major artery of the upper extremity. The brachial artery courses along the ventral surface of the arm and gives rise to multiple smaller branching arteries before reaching the cubital fossa.[1] These branching arteries include the deep brachial artery, the superior ulnar collateral artery, and the inferior ulnar collateral artery. Once the brachial artery reaches the cubital fossa, it divides into its terminal branches: the radial and ulnar arteries of the forearm. The brachial artery and its branches supply the biceps brachii muscle, triceps brachii muscle, and coracobrachialis muscle. The median nerve, a division of the brachial plexus, initially lies lateral to the brachial artery at its proximal segment. At its distal segment, the median nerve crosses the medial side of the brachial artery and lies in the ventral cubital fossa. Structure and Function The following are the branches of the brachial artery in order of origin, proximal to distal. Profunda Brachii/Deep Brachial Artery The first branch of the brachial artery, this branch of the brachial artery arises below the inferior border of the teres major muscle. -

Research Paper Medical Science Variant Brachial Artery with Incomplete Superficial Palmer Arch - a Case Report
Volume : 2 | Issue : 1 | Jan 2013 • ISSN No 2277 - 8160 Research Paper Medical Science Variant Brachial Artery with Incomplete Superficial Palmer Arch - A Case Report Dr. Sharadkumar Associate Professor, Department of Anatomy, K. J. Somaiya Medical College, So- Pralhad Sawant maiya Ayurvihar, Eastern Express Highway, Sion, Mumbai During routine dissection, of the right upper limb of a 70 years old donated embalmed male cadaver in the ABSTRACT Department of Anatomy, K.J. Somaiya Medical College, Sion, Mumbai, India, we observed a high level trifurcation of the brachial artery into the radial, ulnar and common interosseous arteries. The brachial artery trifurcated above the cubital fossa in the lower part of the arm. The ulnar artery travelled downward superficial to the superficial flexor muscles of the forearm. The common interosseous artery was longer in length. The common interosseous artery divided at unusual site in the cubital fossa into the anterior and posterior interosseous arteries. There were no associated altered anatomy of the nerves observed in the specimen. The variations were unilateral and the left upper limb was normal. The photographs of the high level trifurcation of the brachial artery into radial, ulnar and common interosseous artery were taken for proper documentation. Topographical anatomy of the normal and abnormal variations of the axillary artery are clinically important for surgeons, orthopaedicians operating on the supracondylar fracture of humerus and radiologists performing angiographic studies on the upper limb. KEYWORDS: Brachial Artery, Trifurcation, Radial Artery, Ulnar Artery, Common Interosseous Artery, Surgeons, Orthopaedicians Introduction: The brachial artery ends in the cubital fossa by dividing into the ra- dial and ulnar arteries. -

DVT Upper Extremity
UT Southwestern Department of Radiology Ultrasound – Upper Extremity Deep Venous Thrombosis Evaluation PURPOSE: To evaluate the upper extremity superficial and deep venous system for patency. SCOPE: Applies to all ultrasound venous Doppler studies of the lower extremities in Imaging Services / Radiology EPIC ORDERABLE: • UTSW: US DOPPLER VENOUS DVT UPPER EXTREMITY BILATERAL US DOPPLER VENOUS DVT UPPER EXTREMITY RIGHT US DOPPLER VENOUS DVT UPPER EXTREMITY LEFT • PHHS: US DOPPLER VENOUS DVT UPPER EXTREMITY BILATERAL US DOPPLER VENOUS DVT UPPER EXTREMITY RIGHT US DOPPLER VENOUS DVT UPPER EXTREMITY LEFT INDICATIONS: • Symptoms such as upper extremity swelling, pain, fever, warmth, change in color, palpable cord • Suspected venous occlusion, or DVT based on clinical prediction rules (eg. Well’s score or D- Dimer) • Indwelling or recent PICC or central line • Chest pain and/or shortness of breath • Suspected or known pulmonary embolus • Follow-up known deep venous thrombosis (DVT) CONTRAINDICATIONS: No absolute contraindications EQUIPMENT: Preferably a linear array transducer that allows for appropriate resolution of anatomy (frequency range of 9 mHz or greater), capable of duplex imaging. Sector or curvilinear transducers may be required for appropriate penetration in patients with edema or large body habitus. PATIENT PREPARATION: • None EXAMINATION: GENERAL GUIDELINES: A complete examination includes evaluation of the superficial and deep venous system of the upper extremity including the internal jugular, innominate, subclavian, axillary, paired brachial, basilic, and cephalic veins. EXAM INITIATION: • Introduce yourself to the patient • Verify patient identity using patient name and DOB • Explain test • Obtain patient history including symptoms. Enter and store data page US DVT Upper Extremity 05-31-2020.docx 1 | Page Revision date: 05-31-2020 UT Southwestern Department of Radiology • Place patient in supine position with arm extended TECHNICAL CONSIDERATIONS: • Review any prior imaging, making note of any previous thrombus burden. -

Locking Small Fragment Overview
Surgical Technique Locking Small Fragment Overview PERI-LOC™ Locked Plating System Locking Small Fragment Overview Surgical Technique Table of contents Product overview ...................................................................................2 Introduction .............................................................................................2 Indications ...............................................................................................2 Design features and benefits .................................................................3 System overview ....................................................................................4 Implant overview ...................................................................................10 Surgical technique ................................................................................23 Fracture reduction ...................................................................................23 Clavicle Locking Plate .............................................................................24 3.5mm Proximal Humerus Locking Plate ................................................25 Distal Humerus Locking Plates ...............................................................26 Olecranon Locking Plate .........................................................................28 3.5mm Lateral Proximal Tibia Locking Plate ......................................... 29 3.5mm Medial Distal Tibia Locking Plate .............................................. 30 3.5mm Anterolateral -

Bone Limb Upper
Shoulder Pectoral girdle (shoulder girdle) Scapula Acromioclavicular joint proximal end of Humerus Clavicle Sternoclavicular joint Bone: Upper limb - 1 Scapula Coracoid proc. 3 angles Superior Inferior Lateral 3 borders Lateral angle Medial Lateral Superior 2 surfaces 3 processes Posterior view: Acromion Right Scapula Spine Coracoid Bone: Upper limb - 2 Scapula 2 surfaces: Costal (Anterior), Posterior Posterior view: Costal (Anterior) view: Right Scapula Right Scapula Bone: Upper limb - 3 Scapula Glenoid cavity: Glenohumeral joint Lateral view: Infraglenoid tubercle Right Scapula Supraglenoid tubercle posterior anterior Bone: Upper limb - 4 Scapula Supraglenoid tubercle: long head of biceps Anterior view: brachii Right Scapula Bone: Upper limb - 5 Scapula Infraglenoid tubercle: long head of triceps brachii Anterior view: Right Scapula (with biceps brachii removed) Bone: Upper limb - 6 Posterior surface of Scapula, Right Acromion; Spine; Spinoglenoid notch Suprspinatous fossa, Infraspinatous fossa Bone: Upper limb - 7 Costal (Anterior) surface of Scapula, Right Subscapular fossa: Shallow concave surface for subscapularis Bone: Upper limb - 8 Superior border Coracoid process Suprascapular notch Suprascapular nerve Posterior view: Right Scapula Bone: Upper limb - 9 Acromial Clavicle end Sternal end S-shaped Acromial end: smaller, oval facet Sternal end: larger,quadrangular facet, with manubrium, 1st rib Conoid tubercle Trapezoid line Right Clavicle Bone: Upper limb - 10 Clavicle Conoid tubercle: inferior -
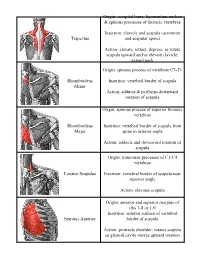
Trapezius Origin: Occipital Bone, Ligamentum Nuchae & Spinous Processes of Thoracic Vertebrae Insertion: Clavicle and Scapul
Origin: occipital bone, ligamentum nuchae & spinous processes of thoracic vertebrae Insertion: clavicle and scapula (acromion Trapezius and scapular spine) Action: elevate, retract, depress, or rotate scapula upward and/or elevate clavicle; extend neck Origin: spinous process of vertebrae C7-T1 Rhomboideus Insertion: vertebral border of scapula Minor Action: adducts & performs downward rotation of scapula Origin: spinous process of superior thoracic vertebrae Rhomboideus Insertion: vertebral border of scapula from Major spine to inferior angle Action: adducts and downward rotation of scapula Origin: transverse precesses of C1-C4 vertebrae Levator Scapulae Insertion: vertebral border of scapula near superior angle Action: elevates scapula Origin: anterior and superior margins of ribs 1-8 or 1-9 Insertion: anterior surface of vertebral Serratus Anterior border of scapula Action: protracts shoulder: rotates scapula so glenoid cavity moves upward rotation Origin: anterior surfaces and superior margins of ribs 3-5 Insertion: coracoid process of scapula Pectoralis Minor Action: depresses & protracts shoulder, rotates scapula (glenoid cavity rotates downward), elevates ribs Origin: supraspinous fossa of scapula Supraspinatus Insertion: greater tuberacle of humerus Action: abduction at the shoulder Origin: infraspinous fossa of scapula Infraspinatus Insertion: greater tubercle of humerus Action: lateral rotation at shoulder Origin: clavicle and scapula (acromion and adjacent scapular spine) Insertion: deltoid tuberosity of humerus Deltoid Action: -

01 Natsis.P65
Folia Morphol. Vol. 68, No. 4, pp. 193–200 Copyright © 2009 Via Medica R E V I E W A R T I C L E ISSN 0015–5659 www.fm.viamedica.pl Persistent median artery in the carpal tunnel: anatomy, embryology, clinical significance, and review of the literature K. Natsis1, G. Iordache2, I. Gigis1, A. Kyriazidou1, N. Lazaridis1, G. Noussios3, G. Paraskevas1 1Department of Anatomy, Medical School, Aristotle University of Thessaloniki, Greece 2University of Medicine and Pharmacy of Craiova, Romania 3Laboratory of Anatomy, Department of Physical Education and Sport Sciences (Serres), Aristotle University of Thessaloniki, Greece [Received 5 June 2009; Accepted 16 September 2009] The median artery usually regresses after the eighth week of intrauterine life, but in some cases it persists into adulthood. The persistent median artery (PMA) pas- ses through the carpal tunnel of the wrist, accompanying the median nerve. During anatomical dissection in our department, we found two unilateral cases of PMA originating from the ulnar artery. In both cases the PMA passed through the carpal tunnel, reached the palm, and anastomosed with the ulnar artery, forming a medio-ulnar type of superficial palmar arch. In addition, in both cases we observed a high division of the median nerve before entering the carpal tunnel. Such an artery may result in several complications such as carpal tunnel syndrome, pronator syndrome, or compression of the anterior interosseous nerve. Therefore, the presence of a PMA should be taken into consideration in clinical practice. This study presents two cases of PMA along with an embryological explanation, analysis of its clinical significance, and a review of the literature. -

Brachial Artery
VASCULAR Anatomy of the upper limb Dr Jamila EL M edany & Dr. Essam Eldin Salama Objectives At the end of the lecture, the students should be able to: • Identify the origin of the vascular supply for the upper limb. • Describe the main arteries and their branches of the arm, forearm & hand. • Describe the vascular arches for the hand. • Describe the superficial and deep veins of the upper limb Arteries Of The Upper Limb Right subclavian Left subclavian artery artery Axillary artery Brachial artery Ulnar artery Radial artery Palmar arches The Subclavian Artery The right artery originates from the brachiocephalic artery. The left artery Cotinues as originates from Axillary artery at the arch of the the lateral border aorta of the 1st rib The Axillary Artery Begins at the lateral border of the st 1 rib as continuation of the Subclavian artery subclavian artery. Continues as brachial artery at lower border of teres major muscle. Is closely related to the cords of brachial plexus and their branches Is enclosed within the axillary sheath. Is crossed anteriorly by the pectoralis minor muscle, and is st nd divided into three parts; 1 , 2 & Brachial artery Axillary artery 3rd. The 1st part of the axillary artery . Extends from the lateral st border of 1 rib to upper 1st part border of the pectoralis 2nd part minor muscle. Highest thoracic artery a. Related: 3rd part Pectoralis • Anterioly: to the minor pectoralis major muscle • Laterally: to the cords Teres of the brachial plexus. major . It gives; ONE branch: Highest thoracic artery The 2nd part of the axillary artery . -

Upper Extremity Fractures
Department of Rehabilitation Services Physical Therapy Standard of Care: Distal Upper Extremity Fractures Case Type / Diagnosis: This standard applies to patients who have sustained upper extremity fractures that require stabilization either surgically or non-surgically. This includes, but is not limited to: Distal Humeral Fracture 812.4 Supracondylar Humeral Fracture 812.41 Elbow Fracture 813.83 Proximal Radius/Ulna Fracture 813.0 Radial Head Fractures 813.05 Olecranon Fracture 813.01 Radial/Ulnar shaft fractures 813.1 Distal Radius Fracture 813.42 Distal Ulna Fracture 813.82 Carpal Fracture 814.01 Metacarpal Fracture 815.0 Phalanx Fractures 816.0 Forearm/Wrist Fractures Radius fractures: • Radial head (may require a prosthesis) • Midshaft radius • Distal radius (most common) Residual deformities following radius fractures include: • Loss of radial tilt (Normal non fracture average is 22-23 degrees of radial tilt.) • Dorsal angulation (normal non fracture average palmar tilt 11-12 degrees.) • Radial shortening • Distal radioulnar (DRUJ) joint involvement • Intra-articular involvement with step-offs. Step-off of as little as 1-2 mm may increase the risk of post-traumatic arthritis. 1 Standard of Care: Distal Upper Extremity Fractures Copyright © 2007 The Brigham and Women's Hospital, Inc. Department of Rehabilitation Services. All rights reserved. Types of distal radius fracture include: • Colle’s (Dinner Fork Deformity) -- Mechanism: fall on an outstretched hand (FOOSH) with radial shortening, dorsal tilt of the distal fragment. The ulnar styloid may or may not be fractured. • Smith’s (Garden Spade Deformity) -- Mechanism: fall backward on a supinated, dorsiflexed wrist, the distal fragment displaces volarly. • Barton’s -- Mechanism: direct blow to the carpus or wrist. -

Olecranon Bone Grafting for the Treatment of Nonunion After Distal Finger Replantation
Ercin et al. Plast Aesthet Res 2020;7:38 Plastic and DOI: 10.20517/2347-9264.2020.56 Aesthetic Research Original Article Open Access Olecranon bone grafting for the treatment of nonunion after distal finger replantation Burak Sercan Ercin1,2, Fatih Kabakas1,2, Musa Kemal Keles1,2, Ismail Bulent Ozcelik1,3,4, Berkan Mersa1,3,4 1IST-EL Microsurgery Group, Istanbul 34245, Turkey. 2Department of Plastic Surgery and Hand Surgery, Medicalpark Gebze Hospital, Kocaeli 41400, Turkey. 3Department of Hand Surgery, Yeni Yuzyil University, Gaziosmanpasa Hospital, Istanbul 34245, Turkey. 4Nisantasi University, Istanbul 34398, Turkey. Correspondence to: Dr. Burak Sercan Ercin, Department of Plastic Surgery and Hand Surgery, Medicalpark Gebze Hospital, Kocaeli 41400, Turkey. E-mail: [email protected] How to cite this article: Ercin BS, Kabakas F, Keles MK, Ozcelik IB, Mersa B. Olecranon bone grafting for the treatment of nonunion after distal finger replantation. Plast Aesthet Res 2020;7:38. http://dx.doi.org/10.20517/2347-9264.2020.56 Received: 29 Mar 2020 First Decision: 4 Jun 2020 Revised: 12 Jun 2020 Accepted: 7 Jul 2020 Published: 19 Jul 2020 Academic Editor: A Thione Copy Editor: Cai-Hong Wang Production Editor: Tian Zhang Abstract Aim: Although not very popular, the olecranon bone graft is a useful option for this type of operation due to the minimal donor morbidity and its ease of use in small bone defect reconstruction and non-union therapy. To our best knowledge, few studies have evaluated the use of the olecranon bone graft as a treatment for non-union after distal finger replantation. Our aim in this report was to present our experience of using olecranon grafts in our nonunion patients undergoing distal replantations.