Olecranon Fractures Diagnosed? • the First Thing I Do Is Listen to Your Story
Total Page:16
File Type:pdf, Size:1020Kb
Load more
Recommended publications
-
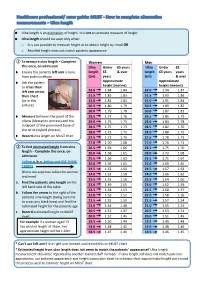
Ulna Length and Mid-Upper
Ulna length is an estimation of height. It is not an accurate measure of height Ulna length should be used only when: o It is not possible to measure height or to obtain height by recall OR o Recalled height does not match patients appearance ① To measure ulna length – Complete Women Men this once, on admission Ulna Under 65 years Ulna Under 65 Ensure the patients left arm is bare length 65 & over length 65 years years from palm to elbow (cm) years (cm) & over Ask the patient Approximate Approximate to cross their height (metres) height (metres) left arm across 32.0 1.84 1.84 32.0 1.94 1.87 their chest 31.5 1.83 1.83 31.5 1.93 1.86 (as in this 31.0 1.81 1.81 31.0 1.91 1.84 picture) 30.5 1.80 1.79 30.5 1.89 1.82 30.0 1.79 1.78 30.0 1.87 1.81 Measure between the point of the 29.5 1.77 1.76 29.5 1.85 1.79 elbow (olecranon process) and the 29.0 1.76 1.75 29.0 1.84 1.78 midpoint of the prominent bone of 28.5 1.75 1.73 28.5 1.82 1.76 the wrist (styloid process) 28.0 1.73 1.71 28.0 1.80 1.75 Record ulna length on MUST chart 27.5 1.72 1.70 27.5 1.78 1.73 27.0 1.70 1.68 27.0 1.76 1.71 ② To find estimated height from ulna 26.5 1.69 1.66 26.5 1.75 1.70 length – Complete this once, on 26.0 1.68 1.65 26.0 1.73 1.68 admission 25.5 1.66 1.63 25.5 1.71 1.67 Follow a. -
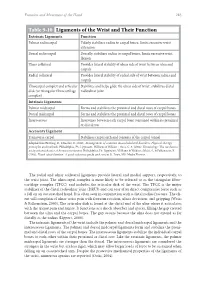
Table 9-10 Ligaments of the Wrist and Their Function
Function and Movement of the Hand 283 Table 9-10 Ligaments of the Wrist and Their Function Extrinsic Ligaments Function Palmar radiocarpal Volarly stabilizes radius to carpal bones; limits excessive wrist extension Dorsal radiocarpal Dorsally stabilizes radius to carpal bones; limits excessive wrist flexion Ulnar collateral Provides lateral stability of ulnar side of wrist between ulna and carpals Radial collateral Provides lateral stability of radial side of wrist between radius and carpals Ulnocarpal complex and articular Stabilizes and helps glide the ulnar side of wrist; stabilizes distal disk (or triangular fibrocartilage radioulnar joint complex) Intrinsic Ligaments Palmar midcarpal Forms and stabilizes the proximal and distal rows of carpal bones Dorsal midcarpal Forms and stabilizes the proximal and distal rows of carpal bones Interosseous Intervenes between each carpal bone contained within its proximal or distal row Accessory Ligament Transverse carpal Stabilizes carpal arch and contents of the carpal tunnel Adapted from Hertling, D., & Kessler, R. (2006). Management of common musculoskeletal disorders: Physical therapy principles and methods. Philadelphia, PA: Lippincott, Williams & Wilkins.; Oatis, C. A. (2004). Kinesiology: The mechanics and pathomechanics of human movement. Philadelphia, PA: Lippincott, Williams & Wilkins.; Weiss, S., & Falkenstein, N. (2005). Hand rehabilitation: A quick reference guide and review. St. Louis, MO: Mosby Elsevier. The radial and ulnar collateral ligaments provide lateral and medial support, respectively, to the wrist joint. The ulnocarpal complex is more likely to be referred to as the triangular fibro- cartilage complex (TFCC) and includes the articular disk of the wrist. The TFCC is the major stabilizer of the distal radioulnar joint (DRUJ) and can tear after direct compressive force such as a fall on an outstretched hand. -

The Appendicular Skeleton Appendicular Skeleton
THE SKELETAL SYSTEM: THE APPENDICULAR SKELETON APPENDICULAR SKELETON The primary function is movement It includes bones of the upper and lower limbs Girdles attach the limbs to the axial skeleton SKELETON OF THE UPPER LIMB Each upper limb has 32 bones Two separate regions 1. The pectoral (shoulder) girdle (2 bones) 2. The free part (30 bones) THE PECTORAL (OR SHOULDER) GIRDLE UPPER LIMB The pectoral girdle consists of two bones, the scapula and the clavicle The free part has 30 bones 1 humerus (arm) 1 ulna (forearm) 1 radius (forearm) 8 carpals (wrist) 19 metacarpal and phalanges (hand) PECTORAL GIRDLE - CLAVICLE The clavicle is “S” shaped The medial end articulates with the manubrium of the sternum forming the sternoclavicular joint The lateral end articulates with the acromion forming the acromioclavicular joint THE CLAVICLE PECTORAL GIRDLE - CLAVICLE The clavicle is convex in shape anteriorly near the sternal junction The clavicle is concave anteriorly on its lateral edge near the acromion CLINICAL CONNECTION - FRACTURED CLAVICLE A fall on an outstretched arm (F.O.O.S.H.) injury can lead to a fractured clavicle The clavicle is weakest at the junction of the two curves Forces are generated through the upper limb to the trunk during a fall Therefore, most breaks occur approximately in the middle of the clavicle PECTORAL GIRDLE - SCAPULA Also called the shoulder blade Triangular in shape Most notable features include the spine, acromion, coracoid process and the glenoid cavity FEATURES ON THE SCAPULA Spine - -

Locking Small Fragment Overview
Surgical Technique Locking Small Fragment Overview PERI-LOC™ Locked Plating System Locking Small Fragment Overview Surgical Technique Table of contents Product overview ...................................................................................2 Introduction .............................................................................................2 Indications ...............................................................................................2 Design features and benefits .................................................................3 System overview ....................................................................................4 Implant overview ...................................................................................10 Surgical technique ................................................................................23 Fracture reduction ...................................................................................23 Clavicle Locking Plate .............................................................................24 3.5mm Proximal Humerus Locking Plate ................................................25 Distal Humerus Locking Plates ...............................................................26 Olecranon Locking Plate .........................................................................28 3.5mm Lateral Proximal Tibia Locking Plate ......................................... 29 3.5mm Medial Distal Tibia Locking Plate .............................................. 30 3.5mm Anterolateral -

Bone Limb Upper
Shoulder Pectoral girdle (shoulder girdle) Scapula Acromioclavicular joint proximal end of Humerus Clavicle Sternoclavicular joint Bone: Upper limb - 1 Scapula Coracoid proc. 3 angles Superior Inferior Lateral 3 borders Lateral angle Medial Lateral Superior 2 surfaces 3 processes Posterior view: Acromion Right Scapula Spine Coracoid Bone: Upper limb - 2 Scapula 2 surfaces: Costal (Anterior), Posterior Posterior view: Costal (Anterior) view: Right Scapula Right Scapula Bone: Upper limb - 3 Scapula Glenoid cavity: Glenohumeral joint Lateral view: Infraglenoid tubercle Right Scapula Supraglenoid tubercle posterior anterior Bone: Upper limb - 4 Scapula Supraglenoid tubercle: long head of biceps Anterior view: brachii Right Scapula Bone: Upper limb - 5 Scapula Infraglenoid tubercle: long head of triceps brachii Anterior view: Right Scapula (with biceps brachii removed) Bone: Upper limb - 6 Posterior surface of Scapula, Right Acromion; Spine; Spinoglenoid notch Suprspinatous fossa, Infraspinatous fossa Bone: Upper limb - 7 Costal (Anterior) surface of Scapula, Right Subscapular fossa: Shallow concave surface for subscapularis Bone: Upper limb - 8 Superior border Coracoid process Suprascapular notch Suprascapular nerve Posterior view: Right Scapula Bone: Upper limb - 9 Acromial Clavicle end Sternal end S-shaped Acromial end: smaller, oval facet Sternal end: larger,quadrangular facet, with manubrium, 1st rib Conoid tubercle Trapezoid line Right Clavicle Bone: Upper limb - 10 Clavicle Conoid tubercle: inferior -
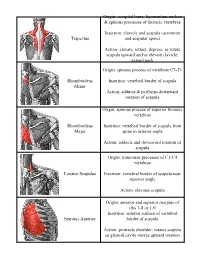
Trapezius Origin: Occipital Bone, Ligamentum Nuchae & Spinous Processes of Thoracic Vertebrae Insertion: Clavicle and Scapul
Origin: occipital bone, ligamentum nuchae & spinous processes of thoracic vertebrae Insertion: clavicle and scapula (acromion Trapezius and scapular spine) Action: elevate, retract, depress, or rotate scapula upward and/or elevate clavicle; extend neck Origin: spinous process of vertebrae C7-T1 Rhomboideus Insertion: vertebral border of scapula Minor Action: adducts & performs downward rotation of scapula Origin: spinous process of superior thoracic vertebrae Rhomboideus Insertion: vertebral border of scapula from Major spine to inferior angle Action: adducts and downward rotation of scapula Origin: transverse precesses of C1-C4 vertebrae Levator Scapulae Insertion: vertebral border of scapula near superior angle Action: elevates scapula Origin: anterior and superior margins of ribs 1-8 or 1-9 Insertion: anterior surface of vertebral Serratus Anterior border of scapula Action: protracts shoulder: rotates scapula so glenoid cavity moves upward rotation Origin: anterior surfaces and superior margins of ribs 3-5 Insertion: coracoid process of scapula Pectoralis Minor Action: depresses & protracts shoulder, rotates scapula (glenoid cavity rotates downward), elevates ribs Origin: supraspinous fossa of scapula Supraspinatus Insertion: greater tuberacle of humerus Action: abduction at the shoulder Origin: infraspinous fossa of scapula Infraspinatus Insertion: greater tubercle of humerus Action: lateral rotation at shoulder Origin: clavicle and scapula (acromion and adjacent scapular spine) Insertion: deltoid tuberosity of humerus Deltoid Action: -

Upper Extremity Fractures
Department of Rehabilitation Services Physical Therapy Standard of Care: Distal Upper Extremity Fractures Case Type / Diagnosis: This standard applies to patients who have sustained upper extremity fractures that require stabilization either surgically or non-surgically. This includes, but is not limited to: Distal Humeral Fracture 812.4 Supracondylar Humeral Fracture 812.41 Elbow Fracture 813.83 Proximal Radius/Ulna Fracture 813.0 Radial Head Fractures 813.05 Olecranon Fracture 813.01 Radial/Ulnar shaft fractures 813.1 Distal Radius Fracture 813.42 Distal Ulna Fracture 813.82 Carpal Fracture 814.01 Metacarpal Fracture 815.0 Phalanx Fractures 816.0 Forearm/Wrist Fractures Radius fractures: • Radial head (may require a prosthesis) • Midshaft radius • Distal radius (most common) Residual deformities following radius fractures include: • Loss of radial tilt (Normal non fracture average is 22-23 degrees of radial tilt.) • Dorsal angulation (normal non fracture average palmar tilt 11-12 degrees.) • Radial shortening • Distal radioulnar (DRUJ) joint involvement • Intra-articular involvement with step-offs. Step-off of as little as 1-2 mm may increase the risk of post-traumatic arthritis. 1 Standard of Care: Distal Upper Extremity Fractures Copyright © 2007 The Brigham and Women's Hospital, Inc. Department of Rehabilitation Services. All rights reserved. Types of distal radius fracture include: • Colle’s (Dinner Fork Deformity) -- Mechanism: fall on an outstretched hand (FOOSH) with radial shortening, dorsal tilt of the distal fragment. The ulnar styloid may or may not be fractured. • Smith’s (Garden Spade Deformity) -- Mechanism: fall backward on a supinated, dorsiflexed wrist, the distal fragment displaces volarly. • Barton’s -- Mechanism: direct blow to the carpus or wrist. -

Olecranon Bone Grafting for the Treatment of Nonunion After Distal Finger Replantation
Ercin et al. Plast Aesthet Res 2020;7:38 Plastic and DOI: 10.20517/2347-9264.2020.56 Aesthetic Research Original Article Open Access Olecranon bone grafting for the treatment of nonunion after distal finger replantation Burak Sercan Ercin1,2, Fatih Kabakas1,2, Musa Kemal Keles1,2, Ismail Bulent Ozcelik1,3,4, Berkan Mersa1,3,4 1IST-EL Microsurgery Group, Istanbul 34245, Turkey. 2Department of Plastic Surgery and Hand Surgery, Medicalpark Gebze Hospital, Kocaeli 41400, Turkey. 3Department of Hand Surgery, Yeni Yuzyil University, Gaziosmanpasa Hospital, Istanbul 34245, Turkey. 4Nisantasi University, Istanbul 34398, Turkey. Correspondence to: Dr. Burak Sercan Ercin, Department of Plastic Surgery and Hand Surgery, Medicalpark Gebze Hospital, Kocaeli 41400, Turkey. E-mail: [email protected] How to cite this article: Ercin BS, Kabakas F, Keles MK, Ozcelik IB, Mersa B. Olecranon bone grafting for the treatment of nonunion after distal finger replantation. Plast Aesthet Res 2020;7:38. http://dx.doi.org/10.20517/2347-9264.2020.56 Received: 29 Mar 2020 First Decision: 4 Jun 2020 Revised: 12 Jun 2020 Accepted: 7 Jul 2020 Published: 19 Jul 2020 Academic Editor: A Thione Copy Editor: Cai-Hong Wang Production Editor: Tian Zhang Abstract Aim: Although not very popular, the olecranon bone graft is a useful option for this type of operation due to the minimal donor morbidity and its ease of use in small bone defect reconstruction and non-union therapy. To our best knowledge, few studies have evaluated the use of the olecranon bone graft as a treatment for non-union after distal finger replantation. Our aim in this report was to present our experience of using olecranon grafts in our nonunion patients undergoing distal replantations. -

Olecranon Fractures Introduction
Olecranon Fractures Steven I. Rabin, M.D. Medical Director, Musculoskeletal Services Dreyer Medical Clinic Clinical Associate Professor, Loyola University Introduction: • General Comments – Diagnosis/Evaluation – Treatment Options – Complications • Specific Injuries (Fractures & Dislocations) – Isolated Olecranon Fractures – Complex Fractures – Olecranon Fractures in Children and the Elderly Olecranon Fracture Clinical Findings • Patients present with deformity, swelling & pain • Inability to Extend the Elbow • Don’t Miss: – Compartment Syndrome – Open wounds Remember the ulnar border is subcutaneous and even superficial wounds can expose the bone – Nerve injuries (especially ulnar nerve) Especially with open fractures Treatment of Olecranon Injuries • Successful Functional Outcome Correlates directly with: – Accuracy of Anatomic Joint Reduction – Restoration of Mechanical Stability that allows Early Motion – Respect for the Soft Tissues – Maintain the Extensor Mechanism Classification • Multiple attempts at classifying olecranon fractures: – Colton – Morrey – Schatzker – AO/ASIF –OTA • Classification helps decide treatment options Colton Classification • Type I: avulsion • Type II: oblique • Type III: associated with dislocation • Type IV: multisegmented Mayo Clinic Classification •Type I: Non-displaced 12% •Type II: Displaced/stable 82% • Type III: Elbow unstable 6% Morrey BF, JBJS 77A: 718-21, 1995 Treatment Overview • If Nondisplaced – Treat with Early Motion • If Displaced – Treat with Open Reduction – Transverse: Tension Band – -

2.0 Mm LCP Distal Ulna Plate TG
2.0 mm LCP Distal Ulna Plate. For capital and subcapital fractures of the ulna. Technique Guide Table of Contents Introduction 2.0 mm LCP Distal Ulna Plate 2 Indications 4 Surgical Technique Clinical Examples 5 Approach 6 Reduce Fracture and Position Plate 7 Fix Plate Distally 9 Adjust Length and Complete Fixation 11 Closure 13 Implant Removal 13 Product Information Implants 14 Instruments 16 IMPORTANT: This device has not been evaluated for safety and compatibility in the MR environment. This device has not been tested for heating or migration in the MR environment. Image intensifier control Synthes 2.0 mm LCP Distal Ulna Plate. For capital and subcapital fractures of the ulna. The distal ulna is an essential component of the distal radioulnar joint, which helps provide rotation to the forearm. The distal ulnar surface is also an important platform for stability of the carpus and, beyond it, the hand. Unstable fractures of the distal ulna therefore threaten both movement and stability of the wrist. The size and shape of the distal ulna, combined with the overlying mobile soft tissues, make application of standard implants difficult. The 2.0 mm LCP Distal Ulna Plate is specifically designed for use in fractures of the distal ulna. Features – Pointed hooks and locking screws in the head – Anatomically precontoured – Angular stability 2 Synthes 2.0 mm LCP Distal Ulna Plate Technique Guide Narrow plate design, low screw-plate profile, rounded edges and polished surface are designed to minimize irritation of overlying soft tissue Pointed hooks -

Shoulder Shoulder
SHOULDER SHOULDER ⦿ Connects arm to thorax ⦿ 3 joints ◼ Glenohumeral joint ◼ Acromioclavicular joint ◼ Sternoclavicular joint ⦿ https://www.youtube.com/watch?v=rRIz6oO A0Vs ⦿ Functional Areas ◼ scapulothoracic ◼ scapulohumeral SHOULDER MOVEMENTS ⦿ Global Shoulder ⦿ Arm (Shoulder Movement Joint) ◼ Elevation ◼ Flexion ◼ Depression ◼ Extension ◼ Abduction ◼ Abduction ◼ Adduction ◼ Adduction ◼ Medial Rotation ◼ Medial Rotation ◼ Lateral Rotation ◼ Lateral Rotation SHOULDER MOVEMENTS ⦿ Movement of shoulder can affect spine and rib cage ◼ Flexion of arm Extension of spine ◼ Extension of arm Flexion of spine ◼ Adduction of arm Ipsilateral sidebending of spine ◼ Abduction of arm Contralateral sidebending of spine ◼ Medial rotation of arm Rotation of spine ◼ Lateral rotation of arm Rotation of spine SHOULDER GIRDLE ⦿ Scapulae ⦿ Clavicles ⦿ Sternum ⦿ Provides mobile base for movement of arms CLAVICLE ⦿ Collarbone ⦿ Elongated S shaped bone ⦿ Articulates with Sternum through Manubrium ⦿ Articulates with Scapula through Acromion STERNOCLAVICULAR JOINT STERNOCLAVICULAR JOINT ⦿ Saddle Joint ◼ Between Manubrium and Clavicle ⦿ Movement ◼ Flexion - move forward ◼ Extension - move backward ◼ Elevation - move upward ◼ Depression - move downward ◼ Rotation ⦿ Usually movement happens with scapula Scapula Scapula ● Flat triangular bone ● 3 borders ○ Superior, Medial, Lateral ● 3 angles ○ Superior, Inferior, Lateral ● Processes and Spine ○ Acromion Process, Coracoid Process, Spine of Scapula ● Fossa ○ Supraspinous, Infraspinous, Subscapularis, Glenoid SCAPULA -
Both-Bone Forearm Fracture with Distal Radioulnar Joint Dislocation
A Case Report & Literature Review Both-Bone Forearm Fracture With Distal Radioulnar Joint Dislocation Michael K. Ryan, MD, Brendan J. MacKay, MD, and Nirmal C. Tejwani, MD and a concomitant ipsilateral DRUJ dislocation, and we review Abstract the literature on this uncommon injury pattern. Both-bone forearm fractures, also known as The patient provided written informed consent for print concomitant diaphyseal radius and ulna frac- and electronic publication of this case report. tures, and distal radioulnar joint (DRUJ) disloca- tions are each uncommon injuries in adult upper Case Report extremity trauma. DRUJ dislocations are more A 38-year-old man with no past medical history presented to often associated with radial shaft (Galeazzi) the emergency department after being thrown from a motor- fractures. In this article, we report the case of cycle. On arrival, he reported bilateral upper extremity pain. a patient who sustained a both-bone forearm Physical examination revealed closed deformities of the left fracture and DRUJ dislocation, and we review forearm and right wrist. Radiographs of the left upper extrem- the literature on this unique injury pattern. ity showed mid-diaphyseal radius and ulna fractures and a DRUJ dislocation (Figure 1). Radiographs of the right upper extremity showed a comminuted radial styloid fracture and widening of the scapholunate interval with dorsal interca- iaphyseal forearm fractures are relatively rare in or- lated segment instability deformity of the carpus. Both upper thopedic trauma, accounting for only 0.9% of all frac- extremity injuries were acceptably reduced and splinted. The 1 AJO Dtures. Both-bone forearm fractures, also known as patient also had a left-side subarachnoid hematoma, which concomitant diaphyseal radius and ulna fractures, are even was stable on serial computed tomography without contrast.