Arrhythmic Genotypes in Familial Dilated Cardiomyopathy 33
Total Page:16
File Type:pdf, Size:1020Kb
Load more
Recommended publications
-

A Mutation in Lamin A/C Gene Previously Known to Cause Emery
ical C lin as C e f R o l e a p n o r r t u s o J Journal of Clinical Case Reports Chalissery et al., J Clin Case Rep 2016, 6:4 ISSN: 2165-7920 DOI: 10.4172/2165-7920.1000770 Case Report Open Access A Mutation in Lamin A/C Gene Previously Known to Cause Emery- Driefuss Muscular Dystrophy Causing A Phenotype of Limb Girdle Muscular Dystrophy Type 1B Albi J Chalissery1*, Tudor Munteanu1, Yvonne Langan2, Francesca Brett2 and Janice Redmond1 1Department of Neurology, St James’s Hospital, Ireland 2Department of Neurophysiology, St James’s Hospital, Ireland 3Department of Neuropathology, Beaumont Hospital, Dublin, Ireland *Corresponding author: Albi J Chalissery, Department of Neurology, St James’s Hospital, James’s Street, Dublin 8, Ireland, Tel +353 1 410 3000; E-mail: [email protected] Rec date: Feb 19, 2016; Acc date: Apr 13, 2016; Pub date: Apr 18, 2016 Copyright: © 2016 Chalissery AJ, et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited. Abstract Mutations in the lamin protein(found in the nuclear envelope) known to cause different allelic disorders including limb girdle muscular dystrophies (LGMD) and Emery-Dreifuss muscular dystrophy (EDMD). LGMDs are a heterogeneous group of disorders with progressive proximal muscle weakness in an autosomal inheritance pattern. LGMD type 1B is a disorder secondary to a mutation in the gene encoding Lamin A/C protein in the nuclear envelope. -
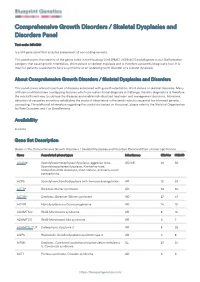
Blueprint Genetics Comprehensive Growth Disorders / Skeletal
Comprehensive Growth Disorders / Skeletal Dysplasias and Disorders Panel Test code: MA4301 Is a 374 gene panel that includes assessment of non-coding variants. This panel covers the majority of the genes listed in the Nosology 2015 (PMID: 26394607) and all genes in our Malformation category that cause growth retardation, short stature or skeletal dysplasia and is therefore a powerful diagnostic tool. It is ideal for patients suspected to have a syndromic or an isolated growth disorder or a skeletal dysplasia. About Comprehensive Growth Disorders / Skeletal Dysplasias and Disorders This panel covers a broad spectrum of diseases associated with growth retardation, short stature or skeletal dysplasia. Many of these conditions have overlapping features which can make clinical diagnosis a challenge. Genetic diagnostics is therefore the most efficient way to subtype the diseases and enable individualized treatment and management decisions. Moreover, detection of causative mutations establishes the mode of inheritance in the family which is essential for informed genetic counseling. For additional information regarding the conditions tested on this panel, please refer to the National Organization for Rare Disorders and / or GeneReviews. Availability 4 weeks Gene Set Description Genes in the Comprehensive Growth Disorders / Skeletal Dysplasias and Disorders Panel and their clinical significance Gene Associated phenotypes Inheritance ClinVar HGMD ACAN# Spondyloepimetaphyseal dysplasia, aggrecan type, AD/AR 20 56 Spondyloepiphyseal dysplasia, Kimberley -

Prenatalscreen® Standard Technical Report
About PrenatalScreen® Prenatal Test PrenatalScreen® Prenatal Test is a genetic test that analyses fetal DNA, obtained from CVS or amniotic fluid following an invasive prenatal diagnosis, to screen for monogenic disorders in the fetus. Using the latest technologies, including Next Generation Sequencing (NGS), PrenatalScreen® Prenatal Test screen 744 genes for mutations causing over 1.000 severe genetic disorders in the fetus. PrenatalScreen® Prenatal Test allows for a comprehensive care and enables patients to make more informed reproductive decisions. Offering PrenatalScreen® Prenatal Test to a patient during pregnancy allows her to gain more knowledge about the potential to pass along a condition to the fetus. Aim of the test PrenatalScreen® Prenatal Test analyses DNA extracted from fetal cells in the amniotic fluid, collected through amniocentesis, or in the chorionic villi through villocentesis (CVS). The aim of this diagnositc test is to assess severe genetic diseases in the fetus, including the most common diseases in the European population. Genes listed in Table 1 were selected according to the incidence in the population of the disease caused by mutations in such genes, the severity of the clinical phenotype at birth and the importance of the related pathogenetic picture, in accordance with the indications of the American College of Medical Genetics (ACMG)(Grody et al., Genet Med 2013:15:482–483). PrenatalScreen®: Indication for testing PrenatalScreen® Prenatal Test is intended for patients who meet any of the following criteria: • Personal/familial anamnesis of hereditary genetic diseases; • For expectant mothers wishing to reduce the risk of a genetic diseases in the fetus; • For natural or in vitro fertilization (IVF)-derived pregnancies: • For couples using heterologus IVF procedures (egg/sperm donors). -

Blueprint Genetics Comprehensive Skeletal Dysplasias and Disorders
Comprehensive Skeletal Dysplasias and Disorders Panel Test code: MA3301 Is a 251 gene panel that includes assessment of non-coding variants. Is ideal for patients with a clinical suspicion of disorders involving the skeletal system. About Comprehensive Skeletal Dysplasias and Disorders This panel covers a broad spectrum of skeletal disorders including common and rare skeletal dysplasias (eg. achondroplasia, COL2A1 related dysplasias, diastrophic dysplasia, various types of spondylo-metaphyseal dysplasias), various ciliopathies with skeletal involvement (eg. short rib-polydactylies, asphyxiating thoracic dysplasia dysplasias and Ellis-van Creveld syndrome), various subtypes of osteogenesis imperfecta, campomelic dysplasia, slender bone dysplasias, dysplasias with multiple joint dislocations, chondrodysplasia punctata group of disorders, neonatal osteosclerotic dysplasias, osteopetrosis and related disorders, abnormal mineralization group of disorders (eg hypopohosphatasia), osteolysis group of disorders, disorders with disorganized development of skeletal components, overgrowth syndromes with skeletal involvement, craniosynostosis syndromes, dysostoses with predominant craniofacial involvement, dysostoses with predominant vertebral involvement, patellar dysostoses, brachydactylies, some disorders with limb hypoplasia-reduction defects, ectrodactyly with and without other manifestations, polydactyly-syndactyly-triphalangism group of disorders, and disorders with defects in joint formation and synostoses. Availability 4 weeks Gene Set Description -

Arthrogryposis and Congenital Myasthenic Syndrome Precision Panel
Arthrogryposis and Congenital Myasthenic Syndrome Precision Panel Overview Arthrogryposis or arthrogryposis multiplex congenita (AMC) is a group of nonprogressive conditions characterized by multiple joint contractures found throughout the body at birth. It usually appears as a feature of other neuromuscular conditions or part of systemic diseases. Primary cases may present prenatally with decreased fetal movements associated with joint contractures as well as brain abnormalities, decreased muscle bulk and polyhydramnios whereas secondary causes may present with isolated contractures. Congenital Myasthenic Syndromes (CMS) are a clinically and genetically heterogeneous group of disorders characterized by impaired neuromuscular transmission. Clinically they usually present with abnormal fatigability upon exertion, transient weakness of extra-ocular, facial, bulbar, truncal or limb muscles. Severity ranges from mild, phasic weakness, to disabling permanent weakness with respiratory difficulties and ultimately death. The mode of inheritance of these diseases typically follows and autosomal recessive pattern, although dominant forms can be seen. The Igenomix Arthrogryposis and Congenital Myasthenic Syndrome Precision Panel can be as a tool for an accurate diagnosis ultimately leading to a better management and prognosis of the disease. It provides a comprehensive analysis of the genes involved in this disease using next-generation sequencing (NGS) to fully understand the spectrum of relevant genes involved, and their high or intermediate penetrance. -

Blueprint Genetics Left Ventricular Non-Compaction Cardiomyopathy
Left Ventricular Non-Compaction Cardiomyopathy (LVNC) Panel Test code: CA1801 Is a 33 gene panel that includes assessment of non-coding variants. Is ideal for patients with a clinical suspicion of left ventricular non-compaction cardiomyopathy. About Left Ventricular Non-Compaction Cardiomyopathy (LVNC) Left ventricular noncompaction (LVNC) is a cardiomyopathy characterized by a spongy appearance of the left ventricle and prominent trabeculations. Individuals may be asymptomatic, but common symptoms include arrhythmias, heart failure, and thromboembolism. LVNC can be seen in the context of congenital structural heart disease in children. LVNC is considered to have a significant amount of overlap with hypertrophic (HCM) and dilated cardiomyopathies (DCM). Many patients with clinical diagnosis of LVNC carry established mutations normally found in patients with clinical diagnosis of HCM or DCM. As the understanding of LVNC phenotype is still limited, we recommend genetic testing to follow HCM scheme if patient’s myocardial thickness exceeds 15 mm at any segment or DCM scheme when the LV size and function fulfill DCM criteria even when significant hypertrabeculation co-exists. Our Cardiomyopathy Panel provides highest diagnostic utility in cases with complex phenotype. Availability 4 weeks Gene Set Description Genes in the Left Ventricular Non-Compaction Cardiomyopathy (LVNC) Panel and their clinical significance Gene Associated phenotypes Inheritance ClinVar HGMD ABCC9 Atrial fibrillation, Cantu syndrome, Dilated cardiomyopathy (DCM) AD 27 -

Hutchinson-Gilford Progeria Syndrome—Current Status and Prospects for Gene Therapy Treatment
cells Review Hutchinson-Gilford Progeria Syndrome—Current Status and Prospects for Gene Therapy Treatment Katarzyna Piekarowicz † , Magdalena Machowska † , Volha Dzianisava and Ryszard Rzepecki * Laboratory of Nuclear Proteins, Faculty of Biotechnology, University of Wroclaw, Fryderyka Joliot-Curie 14a, 50-383 Wroclaw, Poland; [email protected] (K.P.); [email protected] (M.M.); [email protected] (V.D.) * Correspondence: [email protected]; Tel.: +48-71-3756308 † Joint first author. Received: 1 December 2018; Accepted: 19 January 2019; Published: 25 January 2019 Abstract: Hutchinson-Gilford progeria syndrome (HGPS) is one of the most severe disorders among laminopathies—a heterogeneous group of genetic diseases with a molecular background based on mutations in the LMNA gene and genes coding for interacting proteins. HGPS is characterized by the presence of aging-associated symptoms, including lack of subcutaneous fat, alopecia, swollen veins, growth retardation, age spots, joint contractures, osteoporosis, cardiovascular pathology, and death due to heart attacks and strokes in childhood. LMNA codes for two major, alternatively spliced transcripts, give rise to lamin A and lamin C proteins. Mutations in the LMNA gene alone, depending on the nature and location, may result in the expression of abnormal protein or loss of protein expression and cause at least 11 disease phenotypes, differing in severity and affected tissue. LMNA gene-related HGPS is caused by a single mutation in the LMNA gene in exon 11. The mutation c.1824C > T results in activation of the cryptic donor splice site, which leads to the synthesis of progerin protein lacking 50 amino acids. -

Blueprint Genetics Comprehensive Muscular Dystrophy / Myopathy Panel
Comprehensive Muscular Dystrophy / Myopathy Panel Test code: NE0701 Is a 125 gene panel that includes assessment of non-coding variants. In addition, it also includes the maternally inherited mitochondrial genome. Is ideal for patients with distal myopathy or a clinical suspicion of muscular dystrophy. Includes the smaller Nemaline Myopathy Panel, LGMD and Congenital Muscular Dystrophy Panel, Emery-Dreifuss Muscular Dystrophy Panel and Collagen Type VI-Related Disorders Panel. About Comprehensive Muscular Dystrophy / Myopathy Muscular dystrophies and myopathies are a complex group of neuromuscular or musculoskeletal disorders that typically result in progressive muscle weakness. The age of onset, affected muscle groups and additional symptoms depend on the type of the disease. Limb girdle muscular dystrophy (LGMD) is a group of disorders with atrophy and weakness of proximal limb girdle muscles, typically sparing the heart and bulbar muscles. However, cardiac and respiratory impairment may be observed in certain forms of LGMD. In congenital muscular dystrophy (CMD), the onset of muscle weakness typically presents in the newborn period or early infancy. Clinical severity, age of onset, and disease progression are highly variable among the different forms of LGMD/CMD. Phenotypes overlap both within CMD subtypes and among the congenital muscular dystrophies, congenital myopathies, and LGMDs. Emery-Dreifuss muscular dystrophy (EDMD) is a condition that affects mainly skeletal muscle and heart. Usually it presents in early childhood with contractures, which restrict the movement of certain joints – most often elbows, ankles, and neck. Most patients also experience slowly progressive muscle weakness and wasting, beginning with the upper arm and lower leg muscles and progressing to shoulders and hips. -

25. C:\Documents and Settings\Kwang-Il\My
The human disease network Goh K-I, Cusick ME, Valle D, Childs B, Vidal M, Barabasi′ A-L (2007) Proc Natl Acad Sci USA 104:8685-8690 Disorder Class Bone Coats Cancer Urolithiasise Osteopetrosis disease NDP Caffey van_Buchem Exudative Cardiovascular disease disease vitreoretinopathy Norrie SLC34A1 disease 439 LRP5 Connective tissue disorder Nevo Hyperostosis, syndrome COL1A1 endosteal Dermatological PLOD1 217 PAX9 Oligodontia Osteogenesis Osteoporosis 1164 Developmental Ehlers-Danlos imperfecta syndrome Arthropathy COL3A1 Hypodontia Ear, Nose, Throat Aneurysm, COL1A2 familial_arterial Myasthenic Witkop 733 syndrome Heart syndrome Pseudoachondroplasia Endocrine 3-methylglutaconicaciduria OPA3 WISP3 Optic Marfan block MSX1 atrophy OPA1 Aortic syndrome Paramyotonia Sick_sinus Gastrointestinal aneurysm congenita syndrome 3558 Intervertebral_disc Brugada SCN4A disease syndrome Syndactyly Spondyloepiphyseal COMP COL9A2 Hematological Glaucoma Weill-Marchesani Shprintzen-Goldberg Cramps, SCN5A Zlotogora-Ogur Cleft dysplasia syndrome syndrome potassium-aggravated Myotonia 2785 syndrome palate Parkes_Weber Basal_cell FBN1 congenita Oculodentodigital COL9A3 1432 Immunological 1414 CYP1B1 syndrome nevus_syndrome MASS Hypokalemic Acquired dysplasia Peters long_QT_syndrome Epiphyseal FLNB RASA1 PTCH Keratitis syndrome periodic MATN3 Metabolic SHH anomaly Eye Ectopia Thyrotoxic paralysis dysplasia Atelosteogenesis anomalies Marshall Larson Capillary Basal_cell Holoprosencephaly Coloboma, periodic KCNH2 PVRL1 malformations GJA1 Incontinentia syndrome SLC26A2 -

The Congenital and Limb-Girdle Muscular Dystrophies Sharpening the Focus, Blurring the Boundaries
NEUROLOGICAL REVIEW SECTION EDITOR: DAVID E. PLEASURE, MD The Congenital and Limb-Girdle Muscular Dystrophies Sharpening the Focus, Blurring the Boundaries Janbernd Kirschner, MD; Carsten G. Bo¨nnemann, MD uring the past decade, outstanding progress in the areas of congenital and limb- girdle muscular dystrophies has led to staggering clinical and genetic complexity. With the identification of an increasing number of genetic defects, individual enti- ties have come into sharper focus and new pathogenic mechanisms for muscular dys- Dtrophies, like defects of posttranslational O-linked glycosylation, have been discovered. At the same time, this progress blurs the traditional boundaries between the categories of congenital and limb- girdle muscular dystrophies, as well as between limb-girdle muscular dystrophies and other clini- cal entities, as mutations in genes such as fukutin-related protein, dysferlin, caveolin-3 and lamin A/C can cause a striking variety of phenotypes. We reviewed the different groups of proteins cur- rently recognized as being involved in congenital and limb-girdle muscular dystrophies, associ- ated them with the clinical phenotypes, and determined some clinical and molecular clues that are helpful in the diagnostic approach to these patients. Arch Neurol. 2004;61:189-199 Muscular dystrophies were first recog- phy. The age at onset may range from early nized as a disease entity with the detailed childhood to late adulthood.5 description of the clinical presentation of During the past decade, exciting Duchenne muscular dystrophy in 1852 and progress has been made in the field of CMD thereafter.1,2 About 50 years later, Batten3 and LGMD, emphasizing differences as published the first case reports of a con- well as commonalities between them. -

Mandibuloacral Dysplasia: a Premature Ageing Disease with Aspects of Physiological Ageing
Accepted Manuscript Title: MANDIBULOACRAL DYSPLASIA: A PREMATURE AGEING DISEASE WITH ASPECTS OF PHYSIOLOGICAL AGEING Authors: Vittoria Cenni, Maria Rosaria D’Apice, Paolo Garagnani, Marta Columbaro, Giuseppe Novelli, Claudio Franceschi, Giovanna Lattanzi PII: S1568-1637(17)30175-7 DOI: https://doi.org/10.1016/j.arr.2017.12.001 Reference: ARR 800 To appear in: Ageing Research Reviews Received date: 28-7-2017 Revised date: 9-11-2017 Accepted date: 1-12-2017 Please cite this article as: Cenni, Vittoria, D’Apice, Maria Rosaria, Garagnani, Paolo, Columbaro, Marta, Novelli, Giuseppe, Franceschi, Claudio, Lattanzi, Giovanna, MANDIBULOACRAL DYSPLASIA: A PREMATURE AGEING DISEASE WITH ASPECTS OF PHYSIOLOGICAL AGEING.Ageing Research Reviews https://doi.org/10.1016/j.arr.2017.12.001 This is a PDF file of an unedited manuscript that has been accepted for publication. As a service to our customers we are providing this early version of the manuscript. The manuscript will undergo copyediting, typesetting, and review of the resulting proof before it is published in its final form. Please note that during the production process errors may be discovered which could affect the content, and all legal disclaimers that apply to the journal pertain. MANDIBULOACRAL DYSPLASIA: A PREMATURE AGEING DISEASE WITH ASPECTS OF PHYSIOLOGICAL AGEING Vittoria Cenni1,2*, Maria Rosaria D’Apice3, Paolo Garagnani4,5, Marta Columbaro2, Giuseppe Novelli3,6, Claudio Franceschi4, Giovanna Lattanzi1,2*. 1CNR Institute of Molecular Genetics, Unit of Bologna, Via di Barbiano 1/10 I-40136, Bologna, Italy. 2Rizzoli Orthopedic Institute, Bologna, Via di Barbiano 1/10 I-40136, Bologna, Italy. 3Tor Vergata University Hospital, Viale Oxford 81, I-00133 Rome, Italy. -

Unweaving the Role of Nuclear Lamins in Neural Circuit Integrity
News and Thoughts www.cell-stress.com Unweaving the role of nuclear Lamins in neural circuit integrity Samantha L. Deal1 and Shinya Yamamoto1,2,3,4,* 1 Program in Developmental Biology, Baylor College of Medicine (BCM), Houston, TX 77030. 2 Department of Molecular and Human Genetics, BCM, Houston, TX 77030. 3 Department of Neuroscience, BCM, Houston, TX 77030. 4 Jan and Dan Duncan Neurological Research Institute, Texas Children’s Hospital, Houston, TX. * Corresponding Author: Shinya Yamamoto, Tel: +1-832-824-8119; E-mail: [email protected] Lamins are type-V intermediate filament proteins that Lamin A and Lamin C, are both made from the LMNA gene comprise the nuclear lamina. Although once consid- through alternative splicing, whereas two B-type Lamins, ered static structural components that provide physi- Lamin B1 and Lamin B2, are transcribed from LMNB1 and cal support to the inner nuclear envelope, recent stud- LMNB2 genes, respectively. One major difference between ies are revealing additional functional and regulatory these two types of Lamins is that type-B Lamins undergo roles for Lamins in chromatin organization, gene regu- farnesylation at their C-terminal CaaX box that regulates lation, DNA repair, cell division and signal transduc- their intranuclear localization, while mature type-A Lamins tion. In this issue of Cell Stress, Oyston et al. (2018) lack this modification. The two types of Lamins also differ in their expression patterns. While type-B Lamins are ubiq- reports the function of Lamin in the maintenance of uitously expressed throughout development, type-A Lam- nervous system integrity and neural circuit function ins are expressed at later stages when cells undergo differ- using Drosophila.