Rare Diagnosis of Krukenberg Tumor: Intrahepatic Cholangiocarcinoma
Total Page:16
File Type:pdf, Size:1020Kb
Load more
Recommended publications
-

Differential Diagnosis of Ovarian Mucinous Tumours Sigurd F
Differential Diagnosis of Ovarian Mucinous Tumours Sigurd F. Lax LKH Graz II Academic Teaching Hospital of the Medical University Graz Pathology Mucinous tumours of the ovary • Primary ➢Seromucinous tumours ➢Mucinous tumours ➢Benign, borderline, malignant • Secondary (metastatic) ➢Metastases (from gastrointestinal tract) • Metastases can mimic primary ovarian tumour Mucinous tumours: General • 2nd largest group after serous tumours • Gastro-intestinal differentiation (goblet cells) • Endocervical type> seromucinous tumours • Majority is unilateral, particularly cystadenomas and borderline tumours • Bilaterality: rule out metastatic origin • Adenoma>carcinoma sequence reflected by a mixture of benign, atypical proliferating and malignant areas within the same tumour Sero-mucinous ovarian tumours • Previous endocervical type of mucinous tumor • Mixture of at least 2 cell types: mostly serous • Association with endometriosis; multifocality • Similarity with endometrioid and serous tumours, also immunophenotype • CK7, ER, WT1 positive; CK20, cdx2 negativ • Most cystadenoma and borderline tumours • Carcinomas rare and difficult to diagnose Shappel et al., 2002; Dube et al., 2005; Vang et al. 2006 Seromucinous Borderline Tumour ER WT1 Seromucinous carcinoma being discontinued? • Poor reproducibility: Low to modest agreement from 39% to 56% for 4 observers • Immunophenotype not unique, overlapped predominantly with endometrioid and to a lesser extent with mucinous and low-grade serous carcinoma • Molecular features overlap mostly with endometrioid -

A Case of Krukenberg Tumor Metastasized from Colon Cancer In
A case of Krukenberg tumor metastasized from colon cancer in pregnancy Oztas E, Ozler S, Ersoy AO, Turker M, Zengın NI, Caglar AT, Danisman N Zekai Tahir Burak Women's Health Education and Research Hospital, Ankara, Turkey Objective Krukenberg tumor refers to gastrointestinal cancer metastatic to the ovaries and has an extremely poor prognosis, with a 5-year survival rate ranging from 12% to 23. 4%. Gastric cancer has been reported as the most frequent primary source of Krukenberg tumor; however, tumors of the colon, appendix, breast, lung, and pancreas have also been reported to metastasize into the ovaries. Krukenberg tumors are usually seen in the fifth decade of life, with an average age of 45 years and cases diagnosed during pregnancy are thus extremely rare. Methods We report a case of a Krukenberg tumor secondary to colon carcinoma in a pregnant woman with acute pelvic pain. The prenatal diagnosis was made at 17 weeks’ gestation. Results A 27-year-old, primigravida with a semisolid right adnexial mass was presented with acute pelvic pain at 17 weeks’ gestation. Ultrasonography revealed a semisolid right adnexial mass of 140×130 mm and ascites, as well as a single live fetus compatible for gestational age. The abdomen was tense, tender and distended so exploratory laparotomy was performed with the suspicion of ovarian torsion. During the operation, ascites, enlarged right ovary with the presence of a necrotic tumor measuring 160×140 mm causing ovarian torsion and omental metastasis were seen. Unilateral oophorectomy and omentectomy were then performed. Histopathological examination of the specimen revealed adenocarcinoma metastasis to the ovary and the omentum probably originating from a primary gastrointestinal carcinoma (Figure-1). -

Human Anatomy As Related to Tumor Formation Book Four
SEER Program Self Instructional Manual for Cancer Registrars Human Anatomy as Related to Tumor Formation Book Four Second Edition U.S. DEPARTMENT OF HEALTH AND HUMAN SERVICES Public Health Service National Institutesof Health SEER PROGRAM SELF-INSTRUCTIONAL MANUAL FOR CANCER REGISTRARS Book 4 - Human Anatomy as Related to Tumor Formation Second Edition Prepared by: SEER Program Cancer Statistics Branch National Cancer Institute Editor in Chief: Evelyn M. Shambaugh, M.A., CTR Cancer Statistics Branch National Cancer Institute Assisted by Self-Instructional Manual Committee: Dr. Robert F. Ryan, Emeritus Professor of Surgery Tulane University School of Medicine New Orleans, Louisiana Mildred A. Weiss Los Angeles, California Mary A. Kruse Bethesda, Maryland Jean Cicero, ART, CTR Health Data Systems Professional Services Riverdale, Maryland Pat Kenny Medical Illustrator for Division of Research Services National Institutes of Health CONTENTS BOOK 4: HUMAN ANATOMY AS RELATED TO TUMOR FORMATION Page Section A--Objectives and Content of Book 4 ............................... 1 Section B--Terms Used to Indicate Body Location and Position .................. 5 Section C--The Integumentary System ..................................... 19 Section D--The Lymphatic System ....................................... 51 Section E--The Cardiovascular System ..................................... 97 Section F--The Respiratory System ....................................... 129 Section G--The Digestive System ......................................... 163 Section -

Ovarian Carcinomas, Including Secondary Tumors: Diagnostically Challenging Areas
Modern Pathology (2005) 18, S99–S111 & 2005 USCAP, Inc All rights reserved 0893-3952/05 $30.00 www.modernpathology.org Ovarian carcinomas, including secondary tumors: diagnostically challenging areas Jaime Prat Department of Pathology, Hospital de la Santa Creu i Sant Pau, Autonomous University of Barcelona, Spain The differential diagnosis of ovarian carcinomas, including secondary tumors, remains a challenging task. Mucinous carcinomas of the ovary are rare and can be easily confused with metastatic mucinous carcinomas that may present clinically as a primary ovarian tumor. Most of these originate in the gastrointestinal tract and pancreas. International Federation of Gynecology and Obstetrics (FIGO) stage is the single most important prognostic factor, and stage I carcinomas have an excellent prognosis; FIGO stage is largely related to the histologic features of the ovarian tumors. Infiltrative stromal invasion proved to be biologically more aggressive than expansile invasion. Metastatic colon cancer is frequent and often simulates ovarian endometrioid adenocarcinoma. Although immunostains for cytokeratins 7 and 20 can be helpful in the differential diagnosis, they should always be interpreted in the light of all clinical information. Occasionally, endometrioid carcinomas may exhibit a microglandular pattern simulating sex cord-stromal tumors. However, typical endometrioid glands, squamous differentiation, or an adenofibroma component are each present in 75% of these tumors whereas immunostains for calretinin and alpha-inhibin are negative. Endometrioid carcinoma of the ovary is associated in 15–20% of the cases with carcinoma of the endometrium. Most of these tumors have a favorable outcome and they most likely represent independent primary carcinomas arising as a result of a Mu¨ llerian field effect. -

Please Bring Your ~Rotocol, but Do Not Bring Slides Or Microscopes to T He Meeting, CALIFORNIA TUMOR TISSUE REGISTRY
CALIFORNIA TUMOR TISSUE REGISTRY FIFTY- SEVENTH SEMI-ANNUAL SLIDE S~IINAR ON TIJMORS OF THE F~IALE GENITAL TRACT MODERATOR: RlCl!AlUJ C, KEMPSON, M, D, ASSOCIATE PROFESSOR OF PATHOLOGY & CO-DIRECTOR OF SURGICAL PATHOLOGY STANFORD UNIVERSITY MEDICAL CEllTER STANFOliD, CALIFORNIA CHAl~lAN : ALBERT HIRST, M, D, PROFESSOR OF PATHOLOGY LOMA LINDA UNIVERSITY MEDICAL CENTER L~.A LINDA, CALIPORNIA SUNDAY, APRIL 21, 1974 9 : 00 A. M. - 5:30 P,M, REGISTRATION: 7:30 A. M. PASADENA HILTON HOTEL PASADENA, CALIFORNIA Please bring your ~rotocol, but do not bring slides or microscopes to t he meeting, CALIFORNIA TUMOR TISSUE REGISTRY ~lELDON K, BULLOCK, M, D, (EXECUTIVE DIRECTOR) ROGER TERRY, ~1. Ii, (CO-EXECUTIVE DIRECTOR) ~Irs, June Kinsman Mrs. Coral Angus Miss G, Wilma Cline Mrs, Helen Yoshiyama ~fr s. Cheryl Konno Miss Peggy Higgins Mrs. Hataie Nakamura SPONSORS: l~BER PATHOLOGISTS AMERICAN CANCER SOCIETY, CALIFORNIA DIVISION CALIFORNIA MEDICAL ASSOCIATION LAC-USC MEDICAL CENlllR REGIONAL STUDY GRaJPS: LOS ANGELES SAN F~ICISCO CEt;TRAL VALLEY OAKLAND WEST LOS ANGELES SOUTH BAY SANTA EARBARA SAN DIEGO INLAND (SAN BERNARDINO) OHIO SEATTLE ORANGE STOCKTON ARGENTINA SACRJIMENTO ILLINOIS We acknowledge with thanks the voluntary help given by JOHN TRAGERMAN, M. D., PATHOLOGIST, LAC-USC MEDICAL CENlllR VIVIAN GILDENHORN, ASSOCIATE PATHOLOGIST, I~TERCOMMUNITY HOSPITAL ROBERT M. SILTON, M. D,, ASSISTANT PATHOLOGIST, CITY OF HOPE tiEDICAL CENTER JOHN N, O'DON~LL, H. D,, RESIDENT IN PATHOLOGY, LAC-USC MEDICAL CEN!ER JOHN R. CMIG, H. D., RESIDENT IN PATHOLOGY, LAC-USC MEDICAL CENTER CHAPLES GOLDSMITH, M, D. , RESIDENT IN PATHOLOGY, LAC-USC ~IEDICAL CEUTER HAROLD AMSBAUGH, MEDICAL STUDENT, LAC-USC MEDICAL GgNTER N~IE-: E, G. -

Primary Ovarian Signet Ring Cell Carcinoma: a Rare Case Report
MOLECULAR AND CLINICAL ONCOLOGY 9: 211-214, 2018 Primary ovarian signet ring cell carcinoma: A rare case report JI HYE KIM1, HEE JEONG CHA1,2, KYU-RAE KIM2,3 and KYUNGBIN KIM1 1Department of Pathology, Ulsan University Hospital, Ulsan 44033; 2Division of Pathology, University of Ulsan, College of Medicine, Seoul 05505; 3Department of Pathology, Asan Medical Center, Seoul 05505, Republic of Korea Received April 18, 2018; Accepted June 12, 2018 DOI: 10.3892/mco.2018.1653 Abstract. Signet ring cell carcinoma (SRCC) of the ovary is and may be challenging. We herein report the case a patient most commonly metastatic from a primary lesion. Primary diagnosed with primary SRCC of the ovary. ovarian SRCC is rare, and the distinction between primary and metastatic SRCC of the ovary may be difficult. We Case report herein present a case of primary SRCC of the ovary in a 54-year-old woman presenting with a right ovarian mass A 54-year-old woman was admitted to the Ulsan University sized 20.5x16.5x11.5 cm. Total abdominal hysterectomy with Hospital (Ulsan, South Korea) with a palpable firm abdominal bilateral salpingo-oophorectomy, partial omentectomy and mass. The patient exhibited no major symptoms and had no incidental appendectomy were performed. Upon histological specific past history. The patient underwent an abdominal examination, mucinous carcinoma composed predominantly computed tomography (CT) scan, which revealed a ~20-cm of signet ring cells was observed in the right ovary. The multiseptated cystic and solid mass arising from the right results of immunohistochemical examination included diffuse ovary. The abdominal CT scan did not reveal any lesions in positivity for cytokeratin (CK)7 and CK20, but the tumor was the gastrointestinal tract. -

A Rare Cause of Painless Haematuria- Adenocarcinoma of Appendix
Ju ry [ rnal e ul rg d u e S C f h o i l r u a Journal of Surgery r n g r i u e o ] J ISSN: 1584-9341 [Jurnalul de Chirurgie] Case Report Open Access A Rare Cause of Painless Haematuria- Adenocarcinoma of Appendix Shantanu Kumar Sahu1*, Shikhar Agarwal2, Sanjay Agrawal3, Shailendra Raghuvanshi4, Nadia Shirazi5, Saurabh Agrawal1 and Uma Sharma1 1Department of General Surgery, Himalayan Institute of Medical Sciences, Swami Rama Himalayan University, Uttarakhand, India 2Department of Urology, Himalayan Institute of Medical Sciences, Swami Rama Himalayan University, Uttarakhand, India 3Department of Anesthesia, Himalayan Institute of Medical Sciences, Swami Rama Himalayan University, Uttarakhand, India 4Department of Radiodiagnosis, Himalayan Institute of Medical Sciences, Swami Rama Himalayan University, Uttarakhand, India 5Department of Pathology, Himalayan Institute of Medical Sciences, Swami Rama Himalayan University, Uttarakhand, India Abstract Neoplasms of the appendix are rare, accounting for less than 0.5% of all gastrointestinal malignancies and found incidentally in approximately 1% of appendectomy specimen. Carcinoids are the most common appendicular tumors, accounting for approximately 66%, with cystadenocarcinoma accounting for 20% and adenocarcinoma accounting for 10%. Appendiceal adenocarcinomas fall into one of three separate histologic types. The most common mucinous type produces abundant mucin, the less common intestinal or colonic type closely mimics adenocarcinomas found in the colon, and the least common, signet ring cell adenocarcinoma, is quite virulent and associated with a poor prognosis. Adenocarcinoma of appendix is most frequently perforating tumour of gastrointestinal tract due to anatomical peculiarity of appendix which has an extremely thin subserosal and peritoneal coat and the thinnest muscle layer of the whole gastrointestinal tract. -

Pseudomyxoma Peritonei As a Result of Low Grade Appendiceal Mucinous Neoplasm in Association with Ovarian Fibroma
IOSR Journal of Dental and Medical Sciences (IOSR-JDMS) e-ISSN: 2279-0853, p-ISSN: 2279-0861. Volume 13, Issue 1 Ver. X. (Feb. 2014), PP 99-103 www.iosrjournals.org Pseudomyxoma Peritonei As A Result Of Low Grade Appendiceal Mucinous Neoplasm In Association With Ovarian Fibroma. Dr.Deepa.R1 , Dr.R.Sathyalakshmi2 , Dr. Nalli. R . Sumitra Devi3 , Dr. R. Padmavathi4 , Dr.Mary Lilly. S5 Department of Pathology, Stanley Medical College , Chennai , India1. Department of Pathology, Stanley Medical College , Chennai , India2. Department of Pathology, Stanley Medical College , Chennai , India3 Department of Pathology, Stanley Medical College , Chennai , India4. Department of Pathology, Stanley Medical College , Chennai , India5 Abstract: Context : Pseudomyxoma peritonei is a condition caused by the production of abundant mucin by tumor cells which fills the abdominal cavity.(1)The tumor causes fibrosis of tissues and impedes digestion and organ function. If left untreated, tumor and mucin can build up to the point where it compresses vital structures: the colon, the liver, kidneys, stomach, spleen, etc .This disease is most commonly caused by an appendiceal primary tumor. Aims : We describe a case of a 65 year old female with pseudomyxoma peritonei as a result of low grade appendiceal mucinous neoplasm in association with ovarian fibroma . No such cases have been reported in literature till date. Methods and Materials : The patient underwent Left ovariectomy with appendicectomy ,caecal perforation closure and diverting loop ileostomy. Conclusion : Thus we report a rare occurrence of pseudomyxoma peritonei as a result of low grade appendiceal mucinous neoplasm and ovarian fibroma. Key words : Mucinous neoplasm, appendix, ovarian fibroma I. -

Friedrich Krukenberg of Krukenberg's Tumor
Case report Friedrich Krukenberg of Krukenberg’s Tumor: Report of a series of cases Martin Gómez Zuleta, MD,1 Luis Fernando Benito, MD,2 Cristina Almonacid, MD.3 1 Assistant Professor in the Gastroenterology Unit Abstract of the Department of Internal Medicine at the Universidad Nacional de Colombia and Hospital El Krukenberg’s tumor is an ovarian tumor first described by the German physician Friedrich Krukenberg. It is a Tunal in Bogotá, Colombia metastasis of a primary tumor which is usually located in the stomach. This article presents a brief overview of 2 Third Year Surgery Resident at the Universidad de the history of these tumors and a series of 5 cases which were handled in our service. The aim of this article San Martin in Bogotá, Colombia 3 Pathologist at the Hospital El Tunal and the Clínica de is to demonstrate the complexity of this diagnosis, the therapeutic approach, and the pessimistic prognosis la Policía in Bogotá, Colombia that this condition has. ......................................... Received: 17-01-12 Key words Accepted: 15-05-12 Krukenberg’s tumor, gastric cancer. Friedrich Ernst Krukenberg (1871-1946) was a German of microscopic tubes and glands in Krukenberg tumors. In physician who worked in the city of Marburg under the 1981, Bouillon described in great detail what he called a tutelage of Felix Jacob Marchand, the Chief Medical Officer tubular Krukenberg tumor (3-5). of the Department of Pathology, during his undergraduate The use of the term Krukenberg tumor is based on text- education (1846-1928). Dr. Marchand had had six cases of books published by Scully, Young and Kurman. -

Krukenberg Tumor: Report of Six Cases
Gastroenterology & Hepatology: Open Access Mini Review Open Access Krukenberg tumor: report of six cases Abstract Volume 2 Issue 1 - 2015 Introduction: The Krukenberg tumor is a rare malignant tumor of the ovary, accounting Meryem EL Makkaoui, Fouad Haddad, Wafaa from 1% to 2% of all ovarian tumors. It is usually but not always a bilateral involvement Hliwa, Ahmed Bellabah, Wafaa Badre of ovaries from metastatic deposit from adenocarcinoma of stomach, and rarely from other Department of Gastroenterology, University of medicine, gastrointestinal (GI) and non GI organs. Morocco Patients and methods: We report a series of 6 patients with Krukenberg tumors treated at the Casablanca University Hospital between January 2008 and November 2014. Correspondence: Meryem EL Makkaoui, University Hospital Ibn Rochd, Casablanca, Morocco, Tel 676027418, Results: Mean age of the patients was 46 years; digestive signs predominated over pelvic Email signs. Bilateral forms were more frequent. Surgical treatment and palliative chemotherapy were given. The histological diagnosis is based on the presence of signet-ring cells Received: January 19, 2015 | Published: April 2, 2015 associated with a pseudo sarcoma stroma. The primary tumor was found in all of the cases. The prognosis was unfavorable due to late diagnosis. Conclusion: Krukenberg tumor is an ovarian metastasis of digestive tract cancer. The only hope for improved prognosis is to search for ovarian metastasis in all cases and prophylactic ovariectomy in women over 40 with digestive tract cancer. Keywords: krukenberg tumor, metastatic gastric adenocarcinoma, signet ring cell gastric carcinoma, palliative chemotherapy, surgery Abbreviations: GI, gastro-intestinal; CA 125, cancer antigen patients underwent radical surgery consisting of a total hysterectomy 125; CT scan, computerized tomography without adnexal and oophorectomy, the remaining four patients had biopsy because of the advanced local. -

Second Revised Proposed Regulation of the State
SECOND REVISED PROPOSED REGULATION OF THE STATE BOARD OF HEALTH LCB File No. R057-16 February 5, 2018 EXPLANATION – Matter in italics is new; matter in brackets [omitted material] is material to be omitted. AUTHORITY: §§1, 2, 4-9 and 11-15, NRS 457.065 and 457.240; §3, NRS 457.065 and 457.250; §10, NRS 457.065; §16, NRS 439.150, 457.065, 457.250 and 457.260. A REGULATION relating to cancer; revising provisions relating to certain publications adopted by reference by the State Board of Health; revising provisions governing the system for reporting information on cancer and other neoplasms established and maintained by the Chief Medical Officer; establishing the amount and the procedure for the imposition of certain administrative penalties by the Division of Public and Behavioral Health of the Department of Health and Human Services; and providing other matters properly relating thereto. Legislative Counsel’s Digest: Existing law defines the term “cancer” to mean “all malignant neoplasms, regardless of the tissue of origin, including malignant lymphoma and leukemia” and, before the 78th Legislative Session, required the reporting of incidences of cancer. (NRS 457.020, 457.230) Pursuant to Assembly Bill No. 42 of the 78th Legislative Session, the State Board of Health is: (1) authorized to require the reporting of incidences of neoplasms other than cancer, in addition to incidences of cancer, to the system for reporting such information established and maintained by the Chief Medical Officer; and (2) required to establish an administrative penalty to impose against any person who violates certain provisions which govern the abstracting of records of a health care facility relating to the neoplasms the Board requires to be reported. -
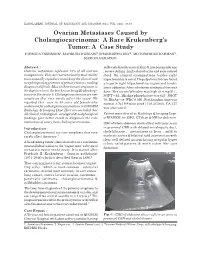
Ovarian Metastases Caused by Cholangiocarcinoma: a Rare
BANGLADESH JOURNAL OF RADIOLOGY AND IMAGING 2013; VOL. 21(2): 87-89 Ovarian Metastases Caused by Cholangiocarcinoma: A Rare Krukenberg’s Tumor: A Case Study FAHMIDA YESHMINE1, MAHBUBA HUSSAIN2, SHARMISTHA DEY3, MD TOWHIDUR RAHMAN3, MASKURA KHATUN4 Abstract : yellowish discoloration of skin & mucous membrane Ovarian metastases represent 10% of all ovarian , severe itching , high colored urine and pale colored malignancies. They are characterized by their ability stool. On clinical examinations tender right to occasionally reproduce mimicking the clinical and hypochondriac is noted. On palpation clinician found morphological appearance of primary tumors, making a mass in right hypochondriac region and tender diagnosis difficult. Most of these tumors originate in lower abdomen. After admission serological test was the digestive tract, the best known being Krukenberg’s done. Her serum bilirubin was high (8.4 mg/dl ) , tumor in the stomach. Cholangiocarcinomas are rare SGPT – 52. Alkaline phosphatase was 627 , SGOT neoplasia that very rarely affect the ovary. We 70, HbsAg –ve, WBC 8,020 , Prothrombin time was reported this case in 50 years old female who normal , CA-19.9 was raised ( 118.4 U/ml) , CA-125 underwent for radiological examinations in BIRDEM was also raised. Radiology & Imaging Dept. Here we concluded that all clinical, radiological , serological & morphological Patient was referred to Radiology & Imaging Dept. findings give better result to diagnosis the rare of BIRDEM for USG , CT Scan & MRI of abdomen. metastases of ovary from cholangiocarcinoma . USG of whole abdomen showed that soft tissue mass Introduction : in proximal CBD with dilated intrahepatic duct, Cholangiocarcinoma are rare neoplasia that very cholelithiasis , metastases in liver , mild to rarely affect the ovary.1 moderate ascites & bilateral solid ovarian mass with clear well defined margin having irregular hyper A Krukenberg tumor (also referred to as a carcinoma echoic solid pattern & moth eaten like cyst mucocellulare) refers to the “signet ring” subtype of formation.