3 Anat 35 Bone Development
Total Page:16
File Type:pdf, Size:1020Kb
Load more
Recommended publications
-

Vocabulario De Morfoloxía, Anatomía E Citoloxía Veterinaria
Vocabulario de Morfoloxía, anatomía e citoloxía veterinaria (galego-español-inglés) Servizo de Normalización Lingüística Universidade de Santiago de Compostela COLECCIÓN VOCABULARIOS TEMÁTICOS N.º 4 SERVIZO DE NORMALIZACIÓN LINGÜÍSTICA Vocabulario de Morfoloxía, anatomía e citoloxía veterinaria (galego-español-inglés) 2008 UNIVERSIDADE DE SANTIAGO DE COMPOSTELA VOCABULARIO de morfoloxía, anatomía e citoloxía veterinaria : (galego-español- inglés) / coordinador Xusto A. Rodríguez Río, Servizo de Normalización Lingüística ; autores Matilde Lombardero Fernández ... [et al.]. – Santiago de Compostela : Universidade de Santiago de Compostela, Servizo de Publicacións e Intercambio Científico, 2008. – 369 p. ; 21 cm. – (Vocabularios temáticos ; 4). - D.L. C 2458-2008. – ISBN 978-84-9887-018-3 1.Medicina �������������������������������������������������������������������������veterinaria-Diccionarios�������������������������������������������������. 2.Galego (Lingua)-Glosarios, vocabularios, etc. políglotas. I.Lombardero Fernández, Matilde. II.Rodríguez Rio, Xusto A. coord. III. Universidade de Santiago de Compostela. Servizo de Normalización Lingüística, coord. IV.Universidade de Santiago de Compostela. Servizo de Publicacións e Intercambio Científico, ed. V.Serie. 591.4(038)=699=60=20 Coordinador Xusto A. Rodríguez Río (Área de Terminoloxía. Servizo de Normalización Lingüística. Universidade de Santiago de Compostela) Autoras/res Matilde Lombardero Fernández (doutora en Veterinaria e profesora do Departamento de Anatomía e Produción Animal. -

REVIEW ARTICLE Interactions Between GH, IGF-I, Glucocorticoids
0031-3998/02/5202-0137 PEDIATRIC RESEARCH Vol. 52, No. 2, 2002 Copyright © 2002 International Pediatric Research Foundation, Inc. Printed in U.S.A. REVIEW ARTICLE Interactions between GH, IGF-I, Glucocorticoids, and Thyroid Hormones during Skeletal Growth HELEN ROBSON, THOMAS SIEBLER, STEPHEN M. SHALET, AND GRAHAM R. WILLIAMS Department of Clinical Research [H.R.], Department of Endocrinology [S.M.S.], Christie Hospital National Health Service Trust, Manchester, U.K.; University Children’s Hospital, University of Leipzig, Leipzig, Germany [T.S.]; IC Molecular Endocrinology Group, Division of Medicine and MRC Clinical Sciences Centre, Faculty of Medicine, Imperial College School of Science Technology and Medicine, Hammersmith Hospital, London, U.K. [G.R.W.] ABSTRACT Linear growth occurs during development and the childhood Abbreviations years until epiphyseal fusion occurs. This process results from 5'-DI, 5'-iodothyronine deiodinase endochondral ossification in the growth plates of long bones and FGF, fibroblast growth factor is regulated by systemic hormones and paracrine or autocrine FGFR, fibroblast growth factor receptor factors. The major regulators of developmental and childhood GC, glucocorticoid growth are GH, IGF-I, glucocorticoids, and thyroid hormone. GHR, GH receptor Sex steroids are responsible for the pubertal growth spurt and GR, glucocorticoid receptor epiphyseal fusion. This review will consider interactions between HSPG, heparan sulfate proteoglycan GH, IGF-I, glucocorticoids, and thyroid hormone during linear 11HSD, 11-hydroxysteroid dehydrogenase growth. It is well known from physiologic and clinical studies IGF-IR, IGF-I receptor that these hormones interact at the level of the hypothalamus and IGFBP, IGF binding protein pituitary. Interacting effects on peripheral tissues such as liver are Ihh, Indian hedgehog also well understood, but we concentrate here on the epiphyseal JAK-2, Janus-activated kinase-2 growth plate as an important and newly appreciated target organ PTHrP, PTH-related peptide for convergent hormone action. -

Skeletal System
Skeletal System Overview • The skeletal system composed of bones, cartilages, joints, and ligaments, accounts for about 20% of the body mass (i.e., about 30 pounds in a 160-pound person). o Bones make up most of the skeleton o Cartilages occur only in isolated areas, such as the nose, parts of ribs, and the joints o Ligaments connect bones and reinforce joints, allowing required movements while restricting motions in other directions. o Joints are the junctions between bones which provide for the mobility of the skeleton Skeletal Cartilages • Human skeleton initially made up of cartilages and fibrous membranes; most are soon replaced with bone • In adults, the few areas where cartilage remains are mainly where flexible skeletal tissue is needed. • Cartilage tissue consists mainly of water—approximately 80%; high water content allows cartilage to be resilient (i.e., spring back to its original shape after being compressed). • Cartilage contains no nerves or blood vessels. • Perichondrium (“around the cartilage”) is dense irregular connective tissue; surrounds the cartilage and acts like a girdle to resist outward expansion when cartilage is compressed. o Perichondrium contains the blood vessels from which nutrients diffuse through the matrix to reach the cartilage cells. This mode of nutrient delivery limits cartilage thickness. • Three types of Cartilage Tissue in body o All three have cells called chondrocytes encased in small cavities (called lacunae) within an extracellular matrix containing a jellylike ground substance and fibers. o Skeletal cartilages contain representatives from all three types. Hyaline cartilages • Looks like frosted glass • Most abundant skeletal cartilages • Their chondrocytes appear spherical • Only fiber type in their matrix is fine collagen (undetectable microscopically) • Skeletal hyaline cartilages include: o Articular Cartilages —cover ends of most bones at movable joints o Costal cartilages —connect ribs to sternum o Respiratory cartilages —form skeleton of the larynx (voicebox) and reinforce other respiratory passages. -

The Epiphyseal Plate: Physiology, Anatomy, and Trauma*
3 CE CREDITS CE Article The Epiphyseal Plate: Physiology, Anatomy, and Trauma* ❯❯ Dirsko J. F. von Pfeil, Abstract: This article reviews the development of long bones, the microanatomy and physiology Dr.med.vet, DVM, DACVS, of the growth plate, the closure times and contribution of different growth plates to overall growth, DECVS and the effect of, and prognosis for, traumatic injuries to the growth plate. Details on surgical Veterinary Specialists of Alaska Anchorage, Alaska treatment of growth plate fractures are beyond the scope of this article. ❯❯ Charles E. DeCamp, DVM, MS, DACVS athologic conditions affecting epi foramen. Growth factors and multipotent Michigan State University physeal (growth) plates in imma stem cells support the formation of neo ture animals may result in severe natal bone consisting of a central marrow P 2 orthopedic problems such as limb short cavity surrounded by a thin periosteum. ening, angular limb deformity, or joint The epiphysis is a secondary ossifica incongruity. Understanding growth plate tion center in the hyaline cartilage forming anatomy and physiology enables practic the joint surfaces at the proximal and distal At a Glance ing veterinarians to provide a prognosis ends of the bones. Secondary ossification Bone Formation and assess indications for surgery. Injured centers can appear in the fetus as early Page E1 animals should be closely observed dur as 28 days after conception1 (TABLE 1). Anatomy of the Growth ing the period of rapid growth. Growth of the epiphysis arises from two Plate areas: (1) the vascular reserve zone car Page E2 Bone Formation tilage, which is responsible for growth of Physiology of the Growth Bone is formed by transformation of con the epiphysis toward the joint, and (2) the Plate nective tissue (intramembranous ossifica epiphyseal plate, which is responsible for Page E4 tion) and replacement of a cartilaginous growth in bone length.3 The epiphyseal 1 Growth Plate Closure model (endochondral ossification). -

A Regulator of Epiphyseal Plate Chondrocyte Proliferation, Hypertrophy, and Long Bone Growth
CHARACTERIZING AQP9: A REGULATOR OF EPIPHYSEAL PLATE CHONDROCYTE PROLIFERATION, HYPERTROPHY, AND LONG BONE GROWTH by Pontius Pu Tian Tang A thesis submitted in conformity with the requirements for the degree of Master of Science Institute of Medical Science University of Toronto © Copyright by Pontius Pu Tian Tang (2018) ii Abstract Characterizing Aqp9: a regulator of epiphyseal plate chondrocyte proliferation, hypertrophy, and long bone growth Pontius Pu Tian Tang Master of Science Institute of Medical Science University of Toronto 2018 Aquaporin-9 (AQP9) is a membrane channel protein suspected to regulate growth in the epiphyseal plate. As long bone defects often possess limited non-surgical options, novel factors underlying bone growth must be continuously explored to advance effective treatments. I hypothesized that Aqp9 is an important epiphyseal plate chondrocyte channel regulating the process of endochondral ossification. In this study, Aqp9 -/- mouse long bones compared to wildtype mouse long bones showed a neonatal hindlimb-specific acceleration of growth followed by reduced length in the juvenile age. Analysis of Aqp9 -/- epiphyseal plates and chondrocytes showed an early disposition for proliferation and aversion from hypertrophy, suggesting that Aqp9 may function similarly to genes such as Col10a1 and Mmp13. This study provides insight into chondrocyte membrane channel proteins and their regulation of the growing epiphyseal plate, demonstrating that Aqp9 may be a novel therapeutic target for the non-invasive intervention of leg length discrepancies. iii Acknowledgements I would like to take this opportunity to thank everyone who has helped me throughout my degree. Firstly, I would like to express my gratitude to my supervisor, Dr. -

Postnatal Maturation and Radiology of the Growing Spine Sharon E
Neurosurg Clin N Am 18 (2007) 431–461 Postnatal Maturation and Radiology of the Growing Spine Sharon E. Byrd, MDa,b,*, Elizabeth M. Comiskey, MDa,c aRush Medical College, 1653 West Congress Parkway, Chicago, IL 60612, USA bSection of Neuroradiology, Department of Diagnostic Radiology and Nuclear Medicine, Rush University Medical Center, 1653 West Congress Parkway, Chicago, IL 60612, USA cSection of Pediatric Radiology, Department of Diagnostic Radiology and Nuclear Medicine, Rush University Medical Center, 1653 West Congress Parkway, Chicago, IL 60612, USA The spine is part of the supporting framework Anatomy of the body and is composed of vertebrae, discs, The spine consists of osseous and soft tissue and ligaments. It continues to mature postnatally, components that provide support and mobility for with marked changes occurring predominantly in the body and a protective covering for the central the vertebrae during infancy, childhood, and early nervous system. The vertebral column is com- adolescence. Maturation of the spine is not only posed of 7 cervical, 12 thoracic, and 5 lumbar manifested by the ossification process but by vertebrae; the sacrum (composed of 5 fused changes in the shape of the vertebrae, spinal vertebrae that become progressively smaller); curvature, spinal canal, discs, and bone marrow. and the coccyx (3 to 5 rudimentary vertebrae). A The parts of the spine and the maturation process typical vertebra consists of a body and neural can be evaluated by various imaging modalities arch. The neural arch is composed of bilateral such as conventional plain spine imaging (CPSI pedicles, laminae, superior and inferior articulat- [plain spine radiography]), CT, and MRI. -

Nomina Histologica Veterinaria, First Edition
NOMINA HISTOLOGICA VETERINARIA Submitted by the International Committee on Veterinary Histological Nomenclature (ICVHN) to the World Association of Veterinary Anatomists Published on the website of the World Association of Veterinary Anatomists www.wava-amav.org 2017 CONTENTS Introduction i Principles of term construction in N.H.V. iii Cytologia – Cytology 1 Textus epithelialis – Epithelial tissue 10 Textus connectivus – Connective tissue 13 Sanguis et Lympha – Blood and Lymph 17 Textus muscularis – Muscle tissue 19 Textus nervosus – Nerve tissue 20 Splanchnologia – Viscera 23 Systema digestorium – Digestive system 24 Systema respiratorium – Respiratory system 32 Systema urinarium – Urinary system 35 Organa genitalia masculina – Male genital system 38 Organa genitalia feminina – Female genital system 42 Systema endocrinum – Endocrine system 45 Systema cardiovasculare et lymphaticum [Angiologia] – Cardiovascular and lymphatic system 47 Systema nervosum – Nervous system 52 Receptores sensorii et Organa sensuum – Sensory receptors and Sense organs 58 Integumentum – Integument 64 INTRODUCTION The preparations leading to the publication of the present first edition of the Nomina Histologica Veterinaria has a long history spanning more than 50 years. Under the auspices of the World Association of Veterinary Anatomists (W.A.V.A.), the International Committee on Veterinary Anatomical Nomenclature (I.C.V.A.N.) appointed in Giessen, 1965, a Subcommittee on Histology and Embryology which started a working relation with the Subcommittee on Histology of the former International Anatomical Nomenclature Committee. In Mexico City, 1971, this Subcommittee presented a document entitled Nomina Histologica Veterinaria: A Working Draft as a basis for the continued work of the newly-appointed Subcommittee on Histological Nomenclature. This resulted in the editing of the Nomina Histologica Veterinaria: A Working Draft II (Toulouse, 1974), followed by preparations for publication of a Nomina Histologica Veterinaria. -

Biology of Bone Repair
Biology of Bone Repair J. Scott Broderick, MD Original Author: Timothy McHenry, MD; March 2004 New Author: J. Scott Broderick, MD; Revised November 2005 Types of Bone • Lamellar Bone – Collagen fibers arranged in parallel layers – Normal adult bone • Woven Bone (non-lamellar) – Randomly oriented collagen fibers – In adults, seen at sites of fracture healing, tendon or ligament attachment and in pathological conditions Lamellar Bone • Cortical bone – Comprised of osteons (Haversian systems) – Osteons communicate with medullary cavity by Volkmann’s canals Picture courtesy Gwen Childs, PhD. Haversian System osteocyte osteon Picture courtesy Gwen Childs, PhD. Haversian Volkmann’s canal canal Lamellar Bone • Cancellous bone (trabecular or spongy bone) – Bony struts (trabeculae) that are oriented in direction of the greatest stress Woven Bone • Coarse with random orientation • Weaker than lamellar bone • Normally remodeled to lamellar bone Figure from Rockwood and Green’s: Fractures in Adults, 4th ed Bone Composition • Cells – Osteocytes – Osteoblasts – Osteoclasts • Extracellular Matrix – Organic (35%) • Collagen (type I) 90% • Osteocalcin, osteonectin, proteoglycans, glycosaminoglycans, lipids (ground substance) – Inorganic (65%) • Primarily hydroxyapatite Ca5(PO4)3(OH)2 Osteoblasts • Derived from mesenchymal stem cells • Line the surface of the bone and produce osteoid • Immediate precursor is fibroblast-like Picture courtesy Gwen Childs, PhD. preosteoblasts Osteocytes • Osteoblasts surrounded by bone matrix – trapped in lacunae • Function -

Bone Cartilage Dense Fibrous CT (Tendons & Nonelastic Ligaments) Dense Elastic CT (Elastic Ligaments)
Chapter 6 Content Review Questions 1-8 1. The skeletal system consists of what connective tissues? Bone Cartilage Dense fibrous CT (tendons & nonelastic ligaments) Dense elastic CT (elastic ligaments) List the functions of these tissues. Bone: supports the body, protects internal organs, provides levers on which muscles act, store minerals, and produce blood cells. Cartilage provides a model for bone formation and growth, provides a smooth cushion between adjacent bones, and provides firm, flexible support. Tendons attach muscles to bones and ligaments attach bone to bone. 2. Name the major types of fibers and molecules found in the extracellular matrix of the skeletal system. Collagen Proteoglycans Hydroxyapatite Water Minerals How do they contribute to the functions of tendons, ligaments, cartilage and bones? The collagen fibers of tendons and ligaments make these structures very tough, like ropes or cables. Collagen makes cartilage tough, whereas the water-filled proteoglycans make it smooth and resistant. As a result, cartilage is relatively rigid, but springs back to its original shape if it is bent or slightly compressed, and it is an excellent shock absorber. The extracellular matrix of bone contains collagen and minerals, including calcium and phosphate. Collagen is a tough, ropelike protein, which lends flexible strength to the bone. The mineral component gives the bone compression (weight-bearing) strength. Most of the mineral in the bone is in the form of hydroxyapatite. 3. Define the terms diaphysis, epiphysis, epiphyseal plate, medullary cavity, articular cartilage, periosteum, and endosteum. Diaphysis – the central shaft of a long bone. Epiphysis – the ends of a long bone. Epiphyseal plate – the site of growth in bone length, found between each epiphysis and diaphysis of a long bone and composed of cartilage. -

The Histology of Epiphyseal Union in Mammals
J. Anat. (1975), 120, 1, pp. 1-25 With 49 figures Printed in Great Britain The histology of epiphyseal union in mammals R. WHEELER HAINES* Visiting Professor, Department of Anatomy, Royal Free Hospital School of Medicine, London (Accepted 11 November 1974) INTRODUCTION Epiphyseal union may be defined as beginning with the completion of the first mineralized bridge between epiphyseal and diaphyseal bone and ending with the complete disappearance of the cartilaginous epiphyseal plate and its replacement by bone and marrow. The phases have been described by Sidhom & Derry (1931) and many others from radiographs, but histological material showing union in progress is rare, probably because of the rapidity with which union, once begun, comes to completion (Stephenson, 1924; Dawson, 1929). Dawson (1925, 1929) described the histology of 'lapsed union' in rats, where the larger epiphyses at the 'growing ends' of the long bones remain un-united through- out life. He and Becks et al. (1948) also discussed the early and complete type of union found at the distal end of the humerus in the rat. Here a single narrow per- foration pierced the cartilaginous plate near the olecranon fossa and later spread to destroy the whole plate. Lassila (1928) described a different type of union in the metatarsus of the calf, with multiple perforations of the plate. Apart from a few notes on human material (Haines & Mohiuddin, 1960, 1968), nothing else seems to have been published on the histology of union in mammals. In this paper more abundant material from dog and man is presented and will serve as a basis for discussion of the main features of the different types of union. -

The Musculoskeletal System Building Bodies Cells: Made of Molecules Such As Lipids (Fats), Glucose (Sugar), Glycogen (Startch) Proteins Etc
The Musculoskeletal System Building Bodies Cells: Made of molecules such as lipids (fats), glucose (sugar), glycogen (startch) proteins etc. These are the basic building blocks creating animal structures. Tissues: Collection of cells organized for a particular function. Ex: skin, muscles Organs: collections of tissues. Ex: Liver Organ system: collection of tissues that work together and have special functions in the body. Organ Systems: Circulatory Skeletal Respiratory Muscular Renal Endocrine Digestive Nervous Reproductive Skeletal + Muscular Systems = Musculoskeletal System Skeletal System: Comprised of bone joined by cartilage and ligaments Provides support for the body and protects the brain & organs Bone is the main component, material inside of bones is marrow which produces blood cells. Muscular System: Made up of muscle tissue to move the body. Functions: 1. Structure 3. Minerals reserve 2. Protection 4. Blood cell production Animal vs. Human Skeleton Humans have a clavicle or COLLAR BONE Differing Rib Pairs: Humans = 12 Cattle = 13+ Poultry = 7 Rabbit = 12 Humans have NO coccygeal vertebrae (tail) Human wrist = animal carpus Human ankle = animal tarpus Human foreman and leg have wider range of motion than animals. Human vs. Animal Skeleton (cont.) Number and placement of teeth: Humans = 32 evenly spaced Cattle = teeth mostly in back, approximately 8 up front Rabbit = all located in front of mouth Dogs = have 2 sets (milk teeth= 24) to 6 months old = 42 Skulls: Bone Structure: Bone Cells: Osteoblasts Osteocytes Osteoclasts Living bone is made up of: 50% water 26% mineral 20% protein 4% fat Dried bone made up of: 70% inorganic minerals- calcium, phosphate for hardness & strength 30% organic components- collagen fibers and cells give elasticity. -
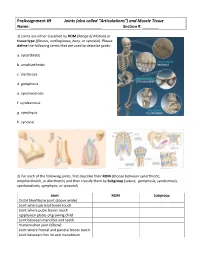
Preassignment #9 Joints (Also Called “Articulations”) and Muscle Tissue Name: Section #: __
PreAssignment #9 Joints (also called “Articulations”) and Muscle Tissue Name: _______________________________ Section #: _______ 1) Joints are either classified by ROM (Range of Motion) or tissue type (fibrous, cartilaginous, bony, or synovial). Please define the following terms that are used to describe joints: a. synarthrotic b. amphiarthrotic c. diarthrotic d. gomphosis e. synchondrosis f. syndesmosis g. symphysis h. synovial 2) For each of the following joints, first describe their ROM (choose between synarthrotic, amphiarthrotic, or diarthrotic) and then classify them by Subgroup (suture, gomphosis, syndesmosis, synchondrosis, symphysis, or synovial). Joint ROM Subgroup Distal tibiofibular joint (above ankle) Joint where parietal bones touch Joint where pubic bones touch Epiphyseal plates of growing child Joint between mandible and teeth Humeroulnar joint (elbow) Joint where frontal and parietal bones touch Joint between first rib and manubrium 3) Please label the parts of the generic synovial joint below. Use the terms: synovial membrane, ligament, periosteum, articular cartilage, synovial fluid, fibrous capsule, and joint capsule. Now, to see if you really understand joints, can you add labels for the diaphyseal cavity and epiphyseal line? 4) Synovial joints (or diarthroses) are usually classified as plane, hinge, saddle, ball-and-socket, or pivot joints. Note: I don’t list condyloid as a subgroup since it is really just a modified form of the hinges! For each of the following joints, please identify the classification to which they belong: a. humeroradial b. scapulohumeral c. interphalangeal d. atloaxis e. carpometacarpal #1 f. intercarpals g. proximal radioulnar h. sacroiliac 5) Movements at a joint are referred to as actions. For each of the following statements, tell me the proper action that is being used: a.