If Your Baby Is Born Early
Total Page:16
File Type:pdf, Size:1020Kb
Load more
Recommended publications
-

Recognizing When a Child's Injury Or Illness Is Caused by Abuse
U.S. Department of Justice Office of Justice Programs Office of Juvenile Justice and Delinquency Prevention Recognizing When a Child’s Injury or Illness Is Caused by Abuse PORTABLE GUIDE TO INVESTIGATING CHILD ABUSE U.S. Department of Justice Office of Justice Programs 810 Seventh Street NW. Washington, DC 20531 Eric H. Holder, Jr. Attorney General Karol V. Mason Assistant Attorney General Robert L. Listenbee Administrator Office of Juvenile Justice and Delinquency Prevention Office of Justice Programs Innovation • Partnerships • Safer Neighborhoods www.ojp.usdoj.gov Office of Juvenile Justice and Delinquency Prevention www.ojjdp.gov The Office of Juvenile Justice and Delinquency Prevention is a component of the Office of Justice Programs, which also includes the Bureau of Justice Assistance; the Bureau of Justice Statistics; the National Institute of Justice; the Office for Victims of Crime; and the Office of Sex Offender Sentencing, Monitoring, Apprehending, Registering, and Tracking. Recognizing When a Child’s Injury or Illness Is Caused by Abuse PORTABLE GUIDE TO INVESTIGATING CHILD ABUSE NCJ 243908 JULY 2014 Contents Could This Be Child Abuse? ..............................................................................................1 Caretaker Assessment ......................................................................................................2 Injury Assessment ............................................................................................................4 Ruling Out a Natural Phenomenon or Medical Conditions -

Evolution of Oviductal Gestation in Amphibians MARVALEE H
THE JOURNAL OF EXPERIMENTAL ZOOLOGY 266394-413 (1993) Evolution of Oviductal Gestation in Amphibians MARVALEE H. WAKE Department of Integrative Biology and Museum of Vertebrate Zoology, University of California,Berkeley, California 94720 ABSTRACT Oviductal retention of developing embryos, with provision for maternal nutrition after yolk is exhausted (viviparity) and maintenance through metamorphosis, has evolved indepen- dently in each of the three living orders of amphibians, the Anura (frogs and toads), the Urodela (salamanders and newts), and the Gymnophiona (caecilians). In anurans and urodeles obligate vivi- parity is very rare (less than 1%of species); a few additional species retain the developing young, but nutrition is yolk-dependent (ovoviviparity) and, at least in salamanders, the young may be born be- fore metamorphosis is complete. However, in caecilians probably the majority of the approximately 170 species are viviparous, and none are ovoviviparous. All of the amphibians that retain their young oviductally practice internal fertilization; the mechanism is cloaca1 apposition in frogs, spermato- phore reception in salamanders, and intromission in caecilians. Internal fertilization is a necessary but not sufficient exaptation (sensu Gould and Vrba: Paleobiology 8:4-15, ’82) for viviparity. The sala- manders and all but one of the frogs that are oviductal developers live at high altitudes and are subject to rigorous climatic variables; hence, it has been suggested that cold might be a “selection pressure” for the evolution of egg retention. However, one frog and all the live-bearing caecilians are tropical low to middle elevation inhabitants, so factors other than cold are implicated in the evolu- tion of live-bearing. -

Management of Neonates Born at ≤34 6/7 Weeks' Gestation with Suspected Or Proven Early-Onset Bacterial Sepsis Karen M
CLINICAL REPORT Guidance for the Clinician in Rendering Pediatric Care ≤ ’ Management of Neonates Born at 34 Karen M. Puopolo, MD, PhD, FAAP, a, b William E. Benitz, MD, FAAP, c Theoklis E. Zaoutis, MD, MSCE, FAAP, a, d 6/7COMMITTEE ONWeeks FETUS AND NEWBORN, GestationCOMMITTEE ON INFECTIOUS DISEASES With Suspected or Proven Early-Onset Bacterial Sepsis Early-onset sepsis (EOS) remains a serious and often fatal illness among abstract infants born preterm, particularly among newborn infants of the lowest gestational age. Currently, most preterm infants with very low birth weight are treated empirically with antibiotics for risk of EOS, often for prolonged aDepartment of Pediatrics, Perelman School of Medicine, University periods, in the absence of a culture-confirmed infection. Retrospective of Pennsylvania, Philadelphia, Pennsylvania; bChildren’s Hospital of studies have revealed that antibiotic exposures after birth are associated Philadelphia, and dRoberts Center for Pediatric Research, Philadelphia, Pennsylvania; and cDivision of Neonatal and Developmental Medicine, with multiple subsequent poor outcomes among preterm infants, making the Department of Pediatrics, School of Medicine, Stanford University, Palo risk/benefit balance of these antibiotic treatments uncertain. Gestational Alto, California age is the strongest single predictor of EOS, and the majority of preterm This document is copyrighted and is property of the American Academy of Pediatrics and its Board of Directors. All authors have births occur in the setting of other factors associated with risk of EOS, filed conflict of interest statements with the American Academy of Pediatrics. Any conflicts have been resolved through a process making it difficult to apply risk stratification strategies to preterm infants. -

Clinical Update and Treatment of Lactation Insufficiency
Review Article Maternal Health CLINICAL UPDATE AND TREATMENT OF LACTATION INSUFFICIENCY ARSHIYA SULTANA* KHALEEQ UR RAHMAN** MANJULA S MS*** SUMMARY: Lactation is beneficial to mother’s health as well as provides specific nourishments, growth, and development to the baby. Hence, it is a nature’s precious gift for the infant; however, lactation insufficiency is one of the explanations mentioned most often by women throughout the world for the early discontinuation of breast- feeding and/or for the introduction of supplementary bottles. Globally, lactation insufficiency is a public health concern, as the use of breast milk substitutes increases the risk of morbidity and mortality among infants in developing countries, and these supplements are the most common cause of malnutrition. The incidence has been estimated to range from 23% to 63% during the first 4 months after delivery. The present article provides a literary search in English language of incidence, etiopathogensis, pathophysiology, clinical features, diagnosis, and current update on treatment of lactation insufficiency from different sources such as reference books, Medline, Pubmed, other Web sites, etc. Non-breast-fed infant are 14 times more likely to die due to diarrhea, 3 times more likely to die of respiratory infection, and twice as likely to die of other infections than an exclusively breast-fed child. Therefore, lactation insufficiency should be tackled in appropriate manner. Key words : Lactation insufficiency, lactation, galactagogue, breast-feeding INTRODUCTION Breast-feeding is advised becasue human milk is The synonyms of lactation insufficiency are as follows: species-specific nourishment for the baby, produces lactational inadequacy (1), breast milk insufficiency (2), optimum growth and development, and provides substantial lactation failure (3,4), mothers milk insufficiency (MMI) (2), protection from illness. -

SIDS and Other Sleep-Related Infant Deaths: Expansion of Recommendations for a Safe Infant Sleeping Environment
Organizational Principles to Guide and Define the Child Health Care System and/or Improve the Health of all Children POLICY STATEMENT SIDS and Other Sleep-Related Infant Deaths: Expansion of Recommendations for a Safe Infant Sleeping Environment TASK FORCE ON SUDDEN INFANT DEATH SYNDROME abstract KEY WORDS Despite a major decrease in the incidence of sudden infant death syn- SIDS, sudden infant death, infant mortality, sleep position, bed- sharing, tobacco, pacifier, immunization, bedding, sleep surface drome (SIDS) since the American Academy of Pediatrics (AAP) released ABBREVIATIONS its recommendation in 1992 that infants be placed for sleep in a non- SIDS—sudden infant death syndrome prone position, this decline has plateaued in recent years. Concur- SUID—sudden unexpected infant death rently, other causes of sudden unexpected infant death that occur AAP—American Academy of Pediatrics during sleep (sleep-related deaths), including suffocation, asphyxia, This document is copyrighted and is property of the American and entrapment, and ill-defined or unspecified causes of death have Academy of Pediatrics and its Board of Directors. All authors have filed conflict of interest statements with the American increased in incidence, particularly since the AAP published its last Academy of Pediatrics. Any conflicts have been resolved through statement on SIDS in 2005. It has become increasingly important to a process approved by the Board of Directors. The American address these other causes of sleep-related infant death. Many of the Academy of Pediatrics has neither solicited nor accepted any commercial involvement in the development of the content of modifiable and nonmodifiable risk factors for SIDS and suffocation are this publication. -

Definitions of Child Abuse and Neglect
STATE STATUTES Current Through March 2019 WHAT’S INSIDE Defining child abuse or Definitions of Child neglect in State law Abuse and Neglect Standards for reporting Child abuse and neglect are defined by Federal Persons responsible for the child and State laws. At the State level, child abuse and neglect may be defined in both civil and criminal Exceptions statutes. This publication presents civil definitions that determine the grounds for intervention by Summaries of State laws State child protective agencies.1 At the Federal level, the Child Abuse Prevention and Treatment To find statute information for a Act (CAPTA) has defined child abuse and neglect particular State, as "any recent act or failure to act on the part go to of a parent or caregiver that results in death, https://www.childwelfare. serious physical or emotional harm, sexual abuse, gov/topics/systemwide/ or exploitation, or an act or failure to act that laws-policies/state/. presents an imminent risk of serious harm."2 1 States also may define child abuse and neglect in criminal statutes. These definitions provide the grounds for the arrest and prosecution of the offenders. 2 CAPTA Reauthorization Act of 2010 (P.L. 111-320), 42 U.S.C. § 5101, Note (§ 3). Children’s Bureau/ACYF/ACF/HHS 800.394.3366 | Email: [email protected] | https://www.childwelfare.gov Definitions of Child Abuse and Neglect https://www.childwelfare.gov CAPTA defines sexual abuse as follows: and neglect in statute.5 States recognize the different types of abuse in their definitions, including physical abuse, The employment, use, persuasion, inducement, neglect, sexual abuse, and emotional abuse. -

Overcoming Breastfeeding Concerns- Part 2
9/21/2018 OVERCOMING BREASTFEEDING Presented by: CONCERNS- PART 2 Kary Johnson, IBCLC OVERVIEW • Pacifiers • Pumping • Low Milk Supply • Feeding Multiples • Supplementation • Discharge Guidelines PICTURE FROM HTTPS://WWW.ETSY.COM/LISTING/464346270/BREAST-ENCOURAGEMENT-CARD-BREASTFEEDING 1 9/21/2018 PACIFIERS Step 9: Counsel mothers on the use and risks of feeding bottles, teats and pacifiers. What does the AAP say? •NG/Gavage •“Mothers of healthy term infants should be instructed to use pacifiers at •Hypoglycemia infant nap or sleep time after breastfeeding is well established, at Infant approximately 3 go 4 weeks of age.” •Lab draws • “Pacifier use should be limited to specific medical situations. These include Pain •Circumcision uses for pain relief, as a calming agent, or as part of a structured program •Illness for enhancing oral motor function.” •Medications Maternal •PMAD • NICU: to organize suck, swallow, breathe pattern of premature infant (in addition to reasons above) (AAP, 2012) PACIFIERS Ask yourself…what is the reason for use? Management: • All effort should be made to prevent separation of mom & baby (i.e. newborn nursery) • Avoid overuse • Be careful to not incorrectly pacify infant hunger • Non-nutritive sucking on mother’s breast is a great alternative Overuse or misuse results in: • Decreased breastfeeding duration • Reduced milk supply • Dental issues, difficulty weaning, and use well into childhood 2 9/21/2018 BREAST PUMPING Reasons a mother may need to pump: • Nipple trauma • Low milk supply • Late preterm infants -

Pediatric Respiratory Rates Age Rate (Breaths Per Minute)
Pediatric Respiratory Rates Age Rate (breaths per minute) Infant (birth–1 year) 30–60 Toddler (1–3 years) 24–40 Preschooler (3–6 years) 22–34 School-age (6–12 years) 18–30 Adolescent (12–18 years) 12–16 Pediatric Pulse Rates Age Low High Infant (birth–1 year) 100 160 Toddler (1–3 years) 90 150 Preschooler (3–6 years) 80 140 School-age (6–12 years) 70 120 Adolescent (12–18 years) 60 100 Pulse rates for a child who is sleeping may be 10 percent lower than the low rate listed. Low-Normal Pediatric Systolic Blood Pressure Age* Low Normal Infant (birth–1 year) greater than 60* Toddler (1–3 years) greater than 70* Preschooler (3–6 years) greater than 75 School-age (6–12 years) greater than 80 Adolescent (12–18 years) greater than 90 *Note: In infants and children aged three years or younger, the presence of a strong central pulse should be substituted for a blood pressure reading. Pediatric CUPS Assessment Category Assessment Actions Example Critical Absent airway, Perform rapid initial Severe traumatic injury breathing, or interventions and transport with respiratory arrest or circulation simultaneously cardiac arrest Unstable Compromised airway, Perform rapid initial Significant injury with breathing, or interventions and transport respiratory distress, circulation with simultaneously active bleeding, shock; altered mental status near-drowning; unresponsiveness Potentially Normal airway, Perform initial assessment Minor fractures; unstable breathing, circulation, with interventions; transport pedestrian struck by car and mental status BUT -
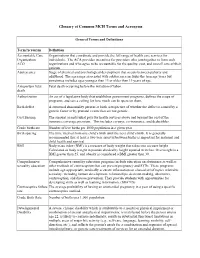
Glossary of Common MCH Terms and Acronyms
Glossary of Common MCH Terms and Acronyms General Terms and Definitions Term/Acronym Definition Accountable Care Organizations that coordinate and provide the full range of health care services for Organization individuals. The ACA provides incentives for providers who join together to form such ACO organizations and who agree to be accountable for the quality, cost, and overall care of their patients. Adolescence Stage of physical and psychological development that occurs between puberty and adulthood. The age range associated with adolescence includes the teen age years but sometimes includes ages younger than 13 or older than 19 years of age. Antepartum fetal Fetal death occurring before the initiation of labor. death Authorization An act of a legislative body that establishes government programs, defines the scope of programs, and sets a ceiling for how much can be spent on them. Birth defect A structural abnormality present at birth, irrespective of whether the defect is caused by a genetic factor or by prenatal events that are not genetic. Cost Sharing The amount an individual pays for health services above and beyond the cost of the insurance coverage premium. This includes co-pays, co-insurance, and deductibles. Crude birth rate Number of live births per 1000 population in a given year. Birth spacing The time interval from one child’s birth until the next child’s birth. It is generally recommended that at least a two-year interval between births is important for maternal and child health and survival. BMI Body mass index (BMI) is a measure of body weight that takes into account height. -

PSBC Obstetric Guideline: Prenatal Screening for Down Syndrome, Trisomy 18, and Open Neural Tube Defects 3 1
Perinatal Services BC Obstetric Guideline: Prenatal Screening for Down Syndrome, Trisomy 18, and Open Neural Tube Defects June 2020 Table of Contents EXECUTIVE SUMMARY � � � � � � � � � � � � � � � � � � � � � � � � � � � � � 2 1� INTRODUCTION � � � � � � � � � � � � � � � � � � � � � � � � � � � � � � � � 3 SIPS, IPS, Quad, NIPT � � � � � � � � � � � � � � � � � � � � � � � � � � � � 3 Open Neural Tube Defects (ONTDs) � � � � � � � � � � � � � � � � � � � � 4 Counselling � � � � � � � � � � � � � � � � � � � � � � � � � � � � � � � � � � � 4 Table 1: Summary of Prenatal Genetic Screening Tests � � � � � � � � 5 Table 2: Screening options available through the BC Prenatal Genetic Screening Program � � � � � � � � � � � � � � � � � 6 2� MANAGEMENT � � � � � � � � � � � � � � � � � � � � � � � � � � � � � � � � 7 3� RESOURCES � � � � � � � � � � � � � � � � � � � � � � � � � � � � � � � � � 10 BC Prenatal Genetic Screening Program Website � � � � � � � � � � 10 Other Useful Websites � � � � � � � � � � � � � � � � � � � � � � � � � � � 10 4� BIBLIOGRAPHY � � � � � � � � � � � � � � � � � � � � � � � � � � � � � � � 11 APPENDIX 1 � � � � � � � � � � � � � � � � � � � � � � � � � � � � � � � � � � � 12 Risk of Down Syndrome and Other Chromosome Abnormalities in Live Births by Maternal Age � � � � � � � � � � � 12 Tel: 604-877-2121 www.bcprenatalscreening.ca APPENDIX 2 � � � � � � � � � � � � � � � � � � � � � � � � � � � � � � � � � � � 13 Screen Cut-Offs and Performance of Screening Tests � � � � � � � 13 APPENDIX 3 � � � � � � � � � � � -

Genetic Testing for Reproductive Carrier Screening and Prenatal Diagnosis
Medical Coverage Policy Effective Date ............................................. 7/15/2021 Next Review Date ......................................12/15/2021 Coverage Policy Number .................................. 0514 Genetic Testing for Reproductive Carrier Screening and Prenatal Diagnosis Table of Contents Related Coverage Resources Overview ........................................................ 2 Genetics Coverage Policy ............................................ 2 Genetic Testing Collateral File Genetic Counseling ...................................... 2 Recurrent Pregnancy Loss: Diagnosis and Treatment Germline Carrier Testing for Familial Infertility Services Disease .......................................................... 3 Preimplantation Genetic Testing of an Embryo........................................................... 4 Preimplantation Genetic Testing (PGT-A) .. 5 Sequencing–Based Non-Invasive Prenatal Testing (NIPT) ............................................... 5 Invasive Prenatal Testing of a Fetus .......... 6 Germline Mutation Reproductive Genetic Testing for Recurrent Pregnancy Loss ...... 6 Germline Mutation Reproductive Genetic Testing for Infertility ..................................... 7 General Background .................................... 8 Genetic Counseling ...................................... 8 Germline Genetic Testing ............................ 8 Carrier Testing for Familial Disease ........... 8 Preimplantation Genetic Testing of an Embryo.......................................................... -

Cross-Linguistic Patterns in Infant Babbling
Cross-linguistic Patterns in Infant Babbling Andreea Geambașu, Mariska Scheel, and Clara C. Levelt 1. Introduction Infants begin to vocalize very soon after birth, and they begin to babble about six months after they are born (Oller, 1980). The babbling stage is distinct from the previous phase of vocalizations in that sounds – or gestures in infants acquiring sign language – are now clearly organized in a syllabic structure. As such, these utterances are the infant’s first linguistic productions. In the works of Stark (1980) and Oller (1980), two stages were identified within the babbling phase. Babies start with reduplicated babbling when they are six to eight months old, and progress into “variegated” (Oller, 1980) or “non- reduplicated” (Stark, 1980) babbling at 10 to 12 months. Work by Koopmans- van Beinum and van der Stelt (1986) outlines a similar line of development, with reduplicated babbling beginning at six months and lasting up until at least 12 months. They do not identify a specific non-reduplicated stage during this period. In addition, Roug, Landberg, and Lundberg (1989) also identified babbling stages similar to those proposed by Oller and Stark, with reduplicated (consonant) babbling beginning at seven months, and variegated babbling beginning at 12 months. The stages identified by these researchers differ only slightly. Where they crucially converge is on the consensus that infants begin their babbling at around six to eight months old, that they begin with reduplicated utterances, and that they transition into producing variegated utterances at around 10 to 12 months. The existence of these two stages has been disseminated in introductory linguistics textbooks for years (e.g., Hoff, 2008).