Signs of Effective Breastfeeding
Total Page:16
File Type:pdf, Size:1020Kb
Load more
Recommended publications
-

Recognizing When a Child's Injury Or Illness Is Caused by Abuse
U.S. Department of Justice Office of Justice Programs Office of Juvenile Justice and Delinquency Prevention Recognizing When a Child’s Injury or Illness Is Caused by Abuse PORTABLE GUIDE TO INVESTIGATING CHILD ABUSE U.S. Department of Justice Office of Justice Programs 810 Seventh Street NW. Washington, DC 20531 Eric H. Holder, Jr. Attorney General Karol V. Mason Assistant Attorney General Robert L. Listenbee Administrator Office of Juvenile Justice and Delinquency Prevention Office of Justice Programs Innovation • Partnerships • Safer Neighborhoods www.ojp.usdoj.gov Office of Juvenile Justice and Delinquency Prevention www.ojjdp.gov The Office of Juvenile Justice and Delinquency Prevention is a component of the Office of Justice Programs, which also includes the Bureau of Justice Assistance; the Bureau of Justice Statistics; the National Institute of Justice; the Office for Victims of Crime; and the Office of Sex Offender Sentencing, Monitoring, Apprehending, Registering, and Tracking. Recognizing When a Child’s Injury or Illness Is Caused by Abuse PORTABLE GUIDE TO INVESTIGATING CHILD ABUSE NCJ 243908 JULY 2014 Contents Could This Be Child Abuse? ..............................................................................................1 Caretaker Assessment ......................................................................................................2 Injury Assessment ............................................................................................................4 Ruling Out a Natural Phenomenon or Medical Conditions -

Breastfeeding Complications (Women) 2001.04
05/2015 602 Breastfeeding Complications or Potential Complications (Women) Definition/Cut-off Value A breastfeeding woman with any of the following complications or potential complications for breastfeeding: Complications (or Potential Complications) Severe breast engorgement Cracked, bleeding or severely sore nipples Recurrent plugged ducts Age ≥ 40 years Mastitis (fever or flu-like symptoms with localized Failure of milk to come in by 4 days postpartum breast tenderness) Tandem nursing (breastfeeding two siblings who are Flat or inverted nipples not twins) Participant Category and Priority Level Category Priority Pregnant Women 1 Breastfeeding Women 1 Justification Severe breast engorgement Severe breast engorgement is often caused by infrequent nursing and/or ineffective removal of milk. This severe breast congestion causes the nipple-areola area to become flattened and tense, making it difficult for the baby to latch-on correctly. The result can be sore, damaged nipples and poor milk transfer during feeding attempts. This ultimately results in diminished milk supply. When the infant is unable to latch-on or nurse effectively, alternative methods of milk expression are necessary, such as using an electric breast pump. Recurrent plugged ducts A clogged duct is a temporary back-up of milk that occurs when one or more of the lobes of the breast do not drain well. This usually results from incomplete emptying of milk. Counseling on feeding frequency or method or advising against wearing an overly tight bra or clothing can assist. Mastitis Mastitis is a breast infection that causes a flu-like illness accompanied by an inflamed, painful area of the breast - putting both the health of the mother and successful breastfeeding at risk. -

Common Breastfeeding Questions
Common Breastfeeding Questions How often should my baby nurse? Your baby should nurse 8-12 times in 24 hours. Baby will tell you when he’s hungry by “rooting,” sucking on his hands or tongue, or starting to wake. Just respond to baby’s cues and latch baby on right away. Every mom and baby’s feeding patterns will be unique. Some babies routinely breastfeed every 2-3 hours around the clock, while others nurse more frequently while awake and sleep longer stretches in between feedings. The usual length of a breastfeeding session can be 10-15 minutes on each breast or 15-30 minutes on only one breast; just as long as the pattern is consistent. Is baby getting enough breastmilk? Look for these signs to be sure that your baby is getting enough breastmilk: Breastfeed 8-12 times each day, baby is sucking and swallowing while breastfeeding, baby has 3- 4 dirty diapers and 6-8 wet diapers each day, the baby is gaining 4-8 ounces a week after the first 2 weeks, baby seems content after feedings. If you still feel that your baby may not be getting enough milk, talk to your health care provider. How long should I breastfeed? The World Health Organization and the American Academy of Pediatrics recommends mothers to breastfeed for 12 months or longer. Breastmilk contains everything that a baby needs to develop for the first 6 months. Breastfeeding for at least the first 6 months is termed, “The Golden Standard.” Mothers can begin breastfeeding one hour after giving birth. -
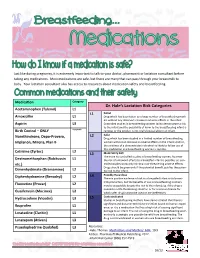
Dr. Hale's Lactation Risk Categories
Just like during pregnancy, it is extremely important to talk to your doctor, pharmacist or lactation consultant before taking any medications. Most medications are safe, but there are many that can pass through your breastmilk to baby. Your lactation consultant also has access to resources about medication safety and breastfeeding. Medication Category Dr. Hale’s Lactation Risk Categories Acetaminophen (Tylenol) L1 L1 Safest Amoxicillin L1 Drug which has been taken by a large number of breastfeeding moth- ers without any observed increase in adverse effects in the infant. Aspirin L3 Controlled studies in breastfeeding women fail to demonstrate a risk to the infant and the possibility of harm to the breastfeeding infant is Birth Control – ONLY Acceptable remote; or the product is not orally bioavailable in an infant. L2 Safer Norethindrone, Depo-Provera, Drug which has been studied in a limited number of breastfeeding Implanon, Mirena, Plan B women without an increase in adverse effects in the infant; And/or, the evidence of a demonstrated risk which is likely to follow use of this medication in a breastfeeding woman is remote. Cetrizine (Zyrtec) L2 L3 Moderately Safe There are no controlled studies in breastfeeding women, however Dextromethorphan (Robitussin L1 the risk of untoward effects to a breastfed infant is possible; or, con- etc.) trolled studies show only minimal non-threatening adverse effects. Drugs should be given only if the potential benefit justifies the poten- Dimenhydrinate (Dramamine) L2 tial risk to the infant. L4 Possibly Hazardous Diphenhydramine (Benadryl) L2 There is positive evidence of risk to a breastfed infant or to breast- milk production, but the benefits of use in breastfeeding mothers Fluoxetine (Prozac) L2 may be acceptable despite the risk to the infant (e.g. -

Melasma (1 of 8)
Melasma (1 of 8) 1 Patient presents w/ symmetric hyperpigmented macules, which can be confl uent or punctate suggestive of melasma 2 DIAGNOSIS No ALTERNATIVE Does clinical presentation DIAGNOSIS confirm melasma? Yes A Non-pharmacological therapy • Patient education • Camoufl age make-up • Sunscreen B Pharmacological therapy Monotherapy • Hydroquinone or • Tretinoin TREATMENT Responding to No treatment? See next page Yes Continue treatment © MIMSas required Not all products are available or approved for above use in all countries. Specifi c prescribing information may be found in the latest MIMS. B94 © MIMS 2019 Melasma (2 of 8) Patient unresponsive to initial therapy MELASMA A Non-pharmacological therapy • Patient education • Camoufl age make-up • Sunscreen B Pharmacological therapy Dual Combination erapy • Hydroquinone plus • Tretinoin or • Azelaic acid Responding to Yes Continue treatment treatment? as required No A Non-pharmacological therapy • Patient education • Camoufl age make-up • Sunscreen • Laser therapy • Dermabrasion B Pharmacological therapy Triple Combination erapy • Hydroquinone plus • Tretinoin plus • Topical steroid Chemical peels 1 MELASMA • Acquired hyperpigmentary skin disorder characterized by irregular light to dark brown macules occurring in the sun-exposed areas of the face, neck & arms - Occurs most commonly w/ pregnancy (chloasma) & w/ the use of contraceptive pills - Other factors implicated in the etiopathogenesis are photosensitizing medications, genetic factors, mild ovarian or thyroid dysfunction, & certain cosmetics • Most commonly aff ects Fitzpatrick skin phototypes III & IV • More common in women than in men • Rare before puberty & common in women during their reproductive years • Solar & ©ultraviolet exposure is the mostMIMS important factor in its development Not all products are available or approved for above use in all countries. -

Breastfeeding Contraindications
WIC Policy & Procedures Manual POLICY: NED: 06.00.00 Page 1 of 1 Subject: Breastfeeding Contraindications Effective Date: October 1, 2019 Revised from: October 1, 2015 Policy: There are very few medical reasons when a mother should not breastfeed. Identify contraindications that may exist for the participant. Breastfeeding is contraindicated when: • The infant is diagnosed with classic galactosemia, a rare genetic metabolic disorder. • Mother has tested positive for HIV (Human Immunodeficiency Syndrome) or has Acquired Immune Deficiency Syndrome (AIDS). • The mother has tested positive for human T-cell Lymphotropic Virus type I or type II (HTLV-1/2). • The mother is using illicit street drugs, such as PCP (phencyclidine) or cocaine (exception: narcotic-dependent mothers who are enrolled in a supervised methadone program and have a negative screening for HIV and other illicit drugs can breastfeed). • The mother has suspected or confirmed Ebola virus disease. Breastfeeding may be temporarily contraindicated when: • The mother is infected with untreated brucellosis. • The mother has an active herpes simplex virus (HSV) infection with lesions on the breast. • The mother is undergoing diagnostic imaging with radiopharmaceuticals. • The mother is taking certain medications or illicit drugs. Note: mothers should be provided breastfeeding support and a breast pump, when appropriate, and may resume breastfeeding after consulting with their health care provider to determine when and if their breast milk is safe for their infant and should be provided with lactation support to establish and maintain milk supply. Direct breastfeeding may be temporarily contraindicated and the mother should be temporarily isolated from her infant(s) but expressed breast milk can be fed to the infant(s) when: • The mother has untreated, active Tuberculosis (TB) (may resume breastfeeding once she has been treated approximately for two weeks and is documented to be no longer contagious). -

Clinical Update and Treatment of Lactation Insufficiency
Review Article Maternal Health CLINICAL UPDATE AND TREATMENT OF LACTATION INSUFFICIENCY ARSHIYA SULTANA* KHALEEQ UR RAHMAN** MANJULA S MS*** SUMMARY: Lactation is beneficial to mother’s health as well as provides specific nourishments, growth, and development to the baby. Hence, it is a nature’s precious gift for the infant; however, lactation insufficiency is one of the explanations mentioned most often by women throughout the world for the early discontinuation of breast- feeding and/or for the introduction of supplementary bottles. Globally, lactation insufficiency is a public health concern, as the use of breast milk substitutes increases the risk of morbidity and mortality among infants in developing countries, and these supplements are the most common cause of malnutrition. The incidence has been estimated to range from 23% to 63% during the first 4 months after delivery. The present article provides a literary search in English language of incidence, etiopathogensis, pathophysiology, clinical features, diagnosis, and current update on treatment of lactation insufficiency from different sources such as reference books, Medline, Pubmed, other Web sites, etc. Non-breast-fed infant are 14 times more likely to die due to diarrhea, 3 times more likely to die of respiratory infection, and twice as likely to die of other infections than an exclusively breast-fed child. Therefore, lactation insufficiency should be tackled in appropriate manner. Key words : Lactation insufficiency, lactation, galactagogue, breast-feeding INTRODUCTION Breast-feeding is advised becasue human milk is The synonyms of lactation insufficiency are as follows: species-specific nourishment for the baby, produces lactational inadequacy (1), breast milk insufficiency (2), optimum growth and development, and provides substantial lactation failure (3,4), mothers milk insufficiency (MMI) (2), protection from illness. -

SIDS and Other Sleep-Related Infant Deaths: Expansion of Recommendations for a Safe Infant Sleeping Environment
Organizational Principles to Guide and Define the Child Health Care System and/or Improve the Health of all Children POLICY STATEMENT SIDS and Other Sleep-Related Infant Deaths: Expansion of Recommendations for a Safe Infant Sleeping Environment TASK FORCE ON SUDDEN INFANT DEATH SYNDROME abstract KEY WORDS Despite a major decrease in the incidence of sudden infant death syn- SIDS, sudden infant death, infant mortality, sleep position, bed- sharing, tobacco, pacifier, immunization, bedding, sleep surface drome (SIDS) since the American Academy of Pediatrics (AAP) released ABBREVIATIONS its recommendation in 1992 that infants be placed for sleep in a non- SIDS—sudden infant death syndrome prone position, this decline has plateaued in recent years. Concur- SUID—sudden unexpected infant death rently, other causes of sudden unexpected infant death that occur AAP—American Academy of Pediatrics during sleep (sleep-related deaths), including suffocation, asphyxia, This document is copyrighted and is property of the American and entrapment, and ill-defined or unspecified causes of death have Academy of Pediatrics and its Board of Directors. All authors have filed conflict of interest statements with the American increased in incidence, particularly since the AAP published its last Academy of Pediatrics. Any conflicts have been resolved through statement on SIDS in 2005. It has become increasingly important to a process approved by the Board of Directors. The American address these other causes of sleep-related infant death. Many of the Academy of Pediatrics has neither solicited nor accepted any commercial involvement in the development of the content of modifiable and nonmodifiable risk factors for SIDS and suffocation are this publication. -

Definitions of Child Abuse and Neglect
STATE STATUTES Current Through March 2019 WHAT’S INSIDE Defining child abuse or Definitions of Child neglect in State law Abuse and Neglect Standards for reporting Child abuse and neglect are defined by Federal Persons responsible for the child and State laws. At the State level, child abuse and neglect may be defined in both civil and criminal Exceptions statutes. This publication presents civil definitions that determine the grounds for intervention by Summaries of State laws State child protective agencies.1 At the Federal level, the Child Abuse Prevention and Treatment To find statute information for a Act (CAPTA) has defined child abuse and neglect particular State, as "any recent act or failure to act on the part go to of a parent or caregiver that results in death, https://www.childwelfare. serious physical or emotional harm, sexual abuse, gov/topics/systemwide/ or exploitation, or an act or failure to act that laws-policies/state/. presents an imminent risk of serious harm."2 1 States also may define child abuse and neglect in criminal statutes. These definitions provide the grounds for the arrest and prosecution of the offenders. 2 CAPTA Reauthorization Act of 2010 (P.L. 111-320), 42 U.S.C. § 5101, Note (§ 3). Children’s Bureau/ACYF/ACF/HHS 800.394.3366 | Email: [email protected] | https://www.childwelfare.gov Definitions of Child Abuse and Neglect https://www.childwelfare.gov CAPTA defines sexual abuse as follows: and neglect in statute.5 States recognize the different types of abuse in their definitions, including physical abuse, The employment, use, persuasion, inducement, neglect, sexual abuse, and emotional abuse. -

Skin Care, Hair Care and Cosmetic Treatments in Pregnancy and Breastfeeding
Skin Care, Hair Care and Cosmetic Treatments in Pregnancy and Breastfeeding Information in this leaflet is general in nature and should not take the place of advice from your health care provider. With every pregnancy there is a 3 to 5% risk of having a baby with a birth defect. Issues for pregnancy Many pregnant women have skin and hair concerns just as they did before pregnancy. Sometimes conditions such as acne actually worsen during pregnancy because of hormonal changes and often women notice darkening of their skin (melasma). However, due to concern about potentially hazardous exposures to their unborn babies, pregnant women are often uncertain about which products are safe for them to use. Generally cosmetic treatments are discretionary (not medically necessary) and if safety is uncertain, women should consider whether the product or treatment is really required. There are several considerations when evaluating whether a specific skin or hair product is unsafe in pregnancy. Firstly, the active ingredient in the product needs to be considered unsafe. Secondly, it also has to be able to reach the unborn baby in its mother’s womb by inhalation or absorption through the mother’s skin (topical application). Although there is often limited information about the actual safety of specific ingredients in skin products during pregnancy, if it is known that skin absorption is minimal then the exposure to the unborn baby is generally insignificant and the product or treatment is regarded as safe. Below is a summary of current advice. Cosmetics, Moisturisers and other Skin Care Products Cosmetics and over the counter skin products generally contain ingredients that are unlikely to be harmful in pregnancy as they are used by applying to the skin (rather than swallowing a tablet). -

Overcoming Breastfeeding Concerns- Part 2
9/21/2018 OVERCOMING BREASTFEEDING Presented by: CONCERNS- PART 2 Kary Johnson, IBCLC OVERVIEW • Pacifiers • Pumping • Low Milk Supply • Feeding Multiples • Supplementation • Discharge Guidelines PICTURE FROM HTTPS://WWW.ETSY.COM/LISTING/464346270/BREAST-ENCOURAGEMENT-CARD-BREASTFEEDING 1 9/21/2018 PACIFIERS Step 9: Counsel mothers on the use and risks of feeding bottles, teats and pacifiers. What does the AAP say? •NG/Gavage •“Mothers of healthy term infants should be instructed to use pacifiers at •Hypoglycemia infant nap or sleep time after breastfeeding is well established, at Infant approximately 3 go 4 weeks of age.” •Lab draws • “Pacifier use should be limited to specific medical situations. These include Pain •Circumcision uses for pain relief, as a calming agent, or as part of a structured program •Illness for enhancing oral motor function.” •Medications Maternal •PMAD • NICU: to organize suck, swallow, breathe pattern of premature infant (in addition to reasons above) (AAP, 2012) PACIFIERS Ask yourself…what is the reason for use? Management: • All effort should be made to prevent separation of mom & baby (i.e. newborn nursery) • Avoid overuse • Be careful to not incorrectly pacify infant hunger • Non-nutritive sucking on mother’s breast is a great alternative Overuse or misuse results in: • Decreased breastfeeding duration • Reduced milk supply • Dental issues, difficulty weaning, and use well into childhood 2 9/21/2018 BREAST PUMPING Reasons a mother may need to pump: • Nipple trauma • Low milk supply • Late preterm infants -

Breastfeeding Matters
Breastfeeding Matters An important guide for breastfeeding families ACKNOWLEDGEMENTS Best Start by Health Nexus would like to thank the Public Health Units of Ontario who supported the creation and development of this provincial resource and generously shared their resources and expertise. We would also like to thank the parents and the experts who provided input for this booklet. Final review was done by Marg La Salle, RN, BScN, IBCLC, and BFI Lead Assessor. The information in this booklet is current at the time of production but information can change over time. Every effort will be made to ensure the information remains current. Throughout this resource, gender-specific language such as “woman”, “women” and “mother” is used in order to accurately cite the research referred to. We intend these terms to refer to all childbearing individuals, regardless of their gender identity or sexual orientation. Funded by the Government of Ontario. Table of Contents SECTION 1 .......................... 3 SECTION 4 ........................ 27 The Importance of Breastfeeding Important Things to Know • Risks of Not Breastfeeding • Waking a Sleepy Baby • Your Breastfeeding Rights • Calming a Fussy Baby • The Baby-Friendly Initiative • Burping Your Baby • Making an Informed Decision • Growth Spurts • Family Support • Sore Nipples • Peer Support • Using a Pacifier (Soother) • Engorgement SECTION 2 ........................ 11 • Storing Your Breast Milk Helping Your Baby Get a Good Start • Skin-to-Skin SECTION 5 ........................ 33 • Safe Positioning