PATIENT GUIDE to an ELECTRICAL CARDIOVERSION for the Treatment of Atrial Fibrillation Or Atrial Flutter
Total Page:16
File Type:pdf, Size:1020Kb
Load more
Recommended publications
-

Incidence of Post Cross Clamp Ventricular Fibrillation in Isolated Coronary Artery Bypass Surgery Using Del Nido Cardioplegia and Conventional Blood Cardioplegia
Jemds.com Original Research Article Incidence of Post Cross Clamp Ventricular Fibrillation in Isolated Coronary Artery Bypass Surgery Using del Nido Cardioplegia and Conventional Blood Cardioplegia Biju Kambil Thyagarajan1, Anandakuttan Sreenivasan2, Ravikrishnan Jayakumar3, Ratish Radhakrishnan4 1, 2, 3, 4 Department of Cardiovascular and Thoracic Surgery, Government T D Medical College, Alappuzha, Kerala, India. ABSTRACT BACKGROUND The cardiac surgical procedures and surgical outcomes witnessed a dramatic Corresponding Author: improvement with the introduction of cardiopulmonary bypass and cardioplegia Dr. Anandakuttan Sreenivasan, techniques. Ventricular fibrillation immediately after removal of aortic cross clamp is Department of Cardiovascular and an energy consuming process leading to myocardial injury in an already energy Thoracic Surgery, Government T D Medical College, Alappuzha, Kerala, India, depleted heart. Electrical cardioversion, which itself causes myocardial injury, is E-mail: [email protected] required to regain normal rhythm. Prevention of ventricular fibrillation is important in preventing myocardial injury. We retrospectively analysed the incidence of post DOI: 10.14260/jemds/2020/797 cross clamp ventricular fibrillation requiring electrical defibrillation in isolated coronary artery bypass surgery using del Nido cardioplegia and conventional blood How to Cite This Article: cardioplegia. Thyagarajan BK, Sreenivasan A, Jayakumar R, et al. Incidence of post cross clamp METHODS ventricular fibrillation in isolated coronary -
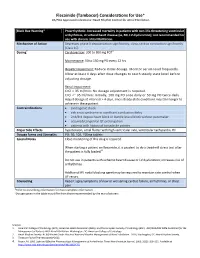
Flecainide Considerations For
Flecainide (Tambocor) Considerations for Use* US/FDA Approved Indications: Heart Rhythm Control for Atrial Fibrillation Black Box Warning* Proarrhythmic. Increased mortality in patients with non-life-threatening ventricular arrhythmias, structural heart disease (ie, MI, LV dysfunction); not recommended for use with chronic atrial fibrillation. Mechanism of Action Depresses phase 0 depolarization significantly, slows cardiac conduction significantly (Class 1C). Dosing† Cardioversion: 200 to 300 mg PO‡1 Maintenance: 50 to 150 mg PO every 12 hrs Hepatic Impairment: Reduce initial dosage. Monitor serum level frequently. Allow at least 4 days after dose changes to reach steady state level before adjusting dosage. Renal Impairment: CrCl > 35 ml/min: No dosage adjustment is required. CrCl <= 35 ml/min: Initially, 100 mg PO once daily or 50 mg PO twice daily. Adjust dosage at intervals > 4 days, since steady-state conditions may take longer to achieve in these patient Contraindications cardiogenic shock sick sinus syndrome or significant conduction delay 2nd/3rd degree heart block or bundle brand block without pacemaker acquired/congenital QT prolongation patients with history of torsade de pointes Major Side Effects hypotension, atrial flutter with high ventricular rate, ventricular tachycardia, HF Dosage forms and Strengths PO: 50, 100, 150mg tablets Special Notes Close monitoring of this drug is required. When starting a patient on flecainide, it is prudent to do a treadmill stress test after the patient is fully loaded.4 Do not use in patients with ischemic heart disease or LV dysfunction; increases risk of arrhythmias. Additional AV nodal blocking agent may be required to maintain rate control when AF recurs. -

Discharge Advice After Atrial Fibrillation Ablation
Oxford University Hospitals NHS Trust Oxford Heart Centre Discharge advice after Atrial Fibrillation ablation Information for patients page 2 This booklet contains important advice about discharge after your Atrial Fibrillation (AF) ablation. It contains information about what to do when you get home. Contents 1. Discharge summary 4 Follow-up 4 Transport 4 2. What to do when you get home 5 Puncture site care 5 Bleeding 6 Sedation/General Anaesthetic 6 After the catheter ablation 6 Recurrence of AF symptoms - what to do 6 Driving 7 Return to work 8 3. Medication 8 4. How to contact us 9 5. Further information 10 6. Message for doctor reviewing this patient 10 page 3 1. Discharge summary Your Consultant at the John Radcliffe Hospital is: ………………………….…............................................................…….. Follow-up You will be sent an appointment for follow-up in the Arrhythmia clinic. (This appointment will be sent in the post. If you do not receive a date for an appointment within 8 weeks, please call the John Radcliffe Hospital and ask to speak to the secretary of your Consultant. Follow-up appointments are currently planned approximately 3 to 4 months after your procedure.) Transport to your outpatient appointments If you have difficulty getting to your outpatient appointments your GP surgery may have the phone numbers of voluntary transport schemes which operate at subsidised rates. A directory of these services is available at www.oxonrcc.org.uk for residents of the Oxfordshire area. page 4 2. What to do when you get home When you are discharged home, you should have a quiet few days resting to recover from your procedure. -

Resuscitation and Defibrillation
AARC GUIDELINE: RESUSCITATION AND DEFIBRILLATION AARC Clinical Practice Guideline Resuscitation and Defibrillation in the Health Care Setting— 2004 Revision & Update RAD 1.0 PROCEDURE: signs, level of consciousness, and blood gas val- Recognition of signs suggesting the possibility ues—included in those conditions are or the presence of cardiopulmonary arrest, initia- 4.1 Airway obstruction—partial or complete tion of resuscitation, and therapeutic use of de- 4.2 Acute myocardial infarction with cardio- fibrillation in adults. dynamic instability 4.3 Life-threatening dysrhythmias RAD 2.0 DESCRIPTION/DEFINITION: 4.4 Hypovolemic shock Resuscitation in the health care setting for the 4.5 Severe infections purpose of this guideline encompasses all care 4.6 Spinal cord or head injury necessary to deal with sudden and often life- 4.7 Drug overdose threatening events affecting the cardiopul- 4.8 Pulmonary edema monary system, and involves the identification, 4.9 Anaphylaxis assessment, and treatment of patients in danger 4.10 Pulmonary embolus of or in frank arrest, including the high-risk de- 4.11 Smoke inhalation livery patient. This includes (1) alerting the re- 4.12 Defibrillation is indicated when cardiac suscitation team and the managing physician; (2) arrest results in or is due to ventricular fibril- using adjunctive equipment and special tech- lation.1-5 niques for establishing, maintaining, and moni- 4.13 Pulseless ventricular tachycardia toring effective ventilation and circulation; (3) monitoring the electrocardiograph and recogniz- -

MANAGING ATRIAL FIBRILLATION (AF) (MODULE 2) MODULE 2: MANAGING ATRIAL FIBRILLATION Ii CONTENTS
YOUR COMPLETE GUIDE TO ATRIAL FIBRILLATION MANAGING ATRIAL FIBRILLATION (AF) (MODULE 2) MODULE 2: MANAGING ATRIAL FIBRILLATION ii CONTENTS iii Overview of managing AF 28 How are blood thinners used to reduce the risk of stroke in AF? 1 What are the goals of managing AF and atrial flutter? 31 What are the signs of a stroke? 2 Rate Control Strategy: 32 Being realistic when managing AF How is the heart rate controlled? (a) Medicine (b) Procedures 9 Rhythm Control Strategy: How is the heart rhythm controlled? (a) Medicine (b) Procedures 25 Reducing the risk of stroke: How is my stroke risk assessed? HEARTANDSTROKE.CA/AFGUIDE Published: February 2014 © 2014 Canadian Cardiovascular Society and Heart and Stroke Foundation of Canada. All rights reserved. Unauthorized use prohibited. MODULE 2: MANAGING ATRIAL FIBRILLATION iii OVERVIEW OF MANAGING AF AF Diagnosed MODULE 1 Find and Treat Common Causes What is it? Is it harmful? MODULE 2 Manage Arrhythmia Symptoms Assess Stroke Risk (CHADS2) Rate Control Rhythm Control • Medicine • Medicine Blood Thinner, Aspirin, or Nothing • Procedures • Procedures MODULE 3 Living Well with AF What to Expect Understanding Following a from Your AF Common Responses Patient Stories Healthy Lifestyle Management Plan and Finding Support FACT SHEET: OVERVIEW OF MANAGING AF HEARTANDSTROKE.CA/AFGUIDE Published: February 2014 © 2014 Canadian Cardiovascular Society and Heart and Stroke Foundation of Canada. All rights reserved. Unauthorized use prohibited. MODULE 2: MANAGING ATRIAL FIBRILLATION iv WHAT ARE TWO WAYS TO MANAGE AF? While AF is a chronic condition, it can be managed by: • medicine • procedures Medicine is usually tried first to manage symptoms caused by AF. -

Cardiac Ablation: Types and Outcomes
CARDIAC ABLATION: TYPES AND OUTCOMES CARDIOVERSION AND ABLATION JASSIN M. JOURIA Dr. Jassin M. Jouria is a practicing Emergency Medicine physician, professor of academic medicine, and medical author. He graduated from Ross University School of Medicine and has completed his clinical clerkship training in various teaching hospitals throughout New York, including King’s County Hospital Center and Brookdale Medical Center, among others. Dr. Jouria has passed all USMLE medical board exams, and has served as a test prep tutor and instructor for Kaplan. He has developed several medical courses and curricula for a variety of educational institutions. Dr. Jouria has also served on multiple levels in the academic field including faculty member and Department Chair. Dr. Jouria continues to serve as a Subject Matter Expert for several continuing education organizations covering multiple basic medical sciences. He has also developed several continuing medical education courses covering various topics in clinical medicine. Recently, Dr. Jouria has been contracted by the University of Miami/Jackson Memorial Hospital’s Department of Surgery to develop an e-module training series for trauma patient management. Dr. Jouria is currently authoring an academic textbook on Human Anatomy & Physiology. ABSTRACT Atrial arrhythmias are serious disorders that can cause an irregular and/or rapid heartbeat, which can lead to serious clinical sequelae. Atrial fibrillation is an example of an atrial arrhythmia that can lead to blood clots, stroke, or heart failure. Electrical cardioversion and ablation are two procedures that can minimize these risks and treat atrial arrhythmia. Each of these treatments have risks and neither offers a complete success rate, but they can be very effective in providing greater quality of life, and extending the life expectancy of patients. -

Stress, Protocols, and Tracers
ASNC IMAGING GUIDELINES ASNC imaging guidelines for SPECT nuclear cardiology procedures: Stress, protocols, and tracers a b c Milena J. Henzlova, MD, W. Lane Duvall, MD, Andrew J. Einstein, MD, d e Mark I. Travin, MD, and Hein J. Verberne, MD a Mount Sinai Medical Center, New York, NY b Hartford Hospital, Hartford, CT c New York Presbyterian Hospital, Columbia University Medical Center, New York, NY d Montefiore Medical Center, Albert Einstein College of Medicine, Bronx, NY e Academic Medical Center, Amsterdam, The Netherlands doi:10.1007/s12350-015-0387-x Abbreviations LEHR Low energy high resolution A2A Adenosine 2a LVEF Left ventricular ejection fraction AHA American Heart Association MBq Megabecquerels ALARA As low as reasonably achievable mCi Millicuries AV Atrioventricular MPI Myocardial perfusion imaging BP Blood pressure MRI Magnetic resonance imaging CBF Coronary blood flow mSv Millisievert CAD Coronary artery disease NE Norepinephrine CPET Cardiopulmonary exercise testing NET1 Norepinephrine transporter-1 DSP Deconvolution of septal penetration NPO Nil per os (nothing by mouth) ECG Electrocardiogram NYHA New York Heart Association EF Ejection fraction PET Positron emission tomography ESRD End-stage renal disease ROI Region of interest HF Heart failure SPECT Single-photon emission computed HFrEF Heart failure (with) reduced ejection tomography fraction TAVR Transcatheter aortic valve replacement HMR Heart-to-mediastinum ratio WR Washout rate ICD Implantable cardioversion defibrillator WPW Wolff-Parkinson White IV Intravenous -

Cardiopulmonary Resuscitation in Prone Position
International Journal of Cardiovascular Sciences. 2021; 34(3):315-318 315 REVIEW ARTICLE Cardiopulmonary Resuscitation in Prone Position Leandro Menezes Alves da Costa,1 Rafael Amorim Belo Nunes,1,2 Thiago Luis Scudeler3 Hospital Alemão Oswaldo Cruz,1 de São Paulo, SP - Brazil Hospital das Clínicas da Faculdade de Medicina da Universidade de São Paulo,2 São Paulo, SP - Brazil Instituto do Coração (InCor),3 São Paulo, SP - Brazil Abstract effectively reduce the difference between transpulmonary dorsal and ventral pressures. In addition, PPV reduces Mechanical ventilation in prone position is an pulmonary compression and improves corporeal alternative strategy for patients with acute respiratory perfusion.6,7 Prone ventilation should be initiated in the discomfort syndrome (ARDS) to improve oxygenation first 36 hours of mechanical ventilation and ideally be in situations when traditional ventilation modalities maintained for 12 to 16 hours.4 have failed. However, due to the significant increase During this period of treatment, the patient may become in ARDS cases during the SARS-CoV-2 pandemic vulnerable to emergency situations, with cardiac arrest and the experimental therapeutic use of potentially as the diagnosis with the worst prognosis. Moreover, arrhythmogenic drugs, cardiopulmonary resuscitation the current use of experimental drugs may increase the in this unusual position could be needed. Therefore, occurrence of malignant arrhythmia. The combination of we will review the available scientific evidence of hydroxychloroquine and azithromycin -

APG Regulations
FINAL as of 8/22/08 Pursuant to the authority vested in the Commissioner of Health by Section 2807(2-a) of the Public Health Law, Part 86 of Title 10 of the Official Compilation of Codes, Rules and Regulations of the State of New York, is amended by adding a new Subpart 86-8, to be effective upon filing with the Secretary of State, to read as follows: SUBPART 86-8 OUTPATIENT SERVICES: AMBULATORY PATIENT GROUP (Statutory authority: Public Health Law § 2807(2-a)(e)) Sec. 86-8.1 Scope 86-8.2 Definitions 86-8.3 Record keeping, reports and audits 86-8.4 Capital reimbursement 86-8.5 Administrative rate appeals 86-8.6 Rates for new facilities during the transition period 86-8.7 APGs and relative weights 86-8.8 Base rates 86-8.9 Diagnostic coding and rate computation 86-8.10 Exclusions from payment 86-8.11 System updating 86-8.12 Payments for extended hours of operation § 86-8.1 Scope (a) This Subpart shall govern Medicaid rates of payments for ambulatory care services provided in the following categories of facilities for the following periods: (1) outpatient services provided by general hospitals on and after December 1, 2008; (2) emergency department services provided by general hospitals on and after January 1, 2009; (3) ambulatory surgery services provided by general hospitals on and after December 1, 2008; (4) ambulatory services provided by diagnostic and treatment centers on and after March 1, 2009; and (5) ambulatory surgery services provided by free-standing ambulatory surgery centers on and after March 1, 2009. -

Icd-9-Cm (2010)
ICD-9-CM (2010) PROCEDURE CODE LONG DESCRIPTION SHORT DESCRIPTION 0001 Therapeutic ultrasound of vessels of head and neck Ther ult head & neck ves 0002 Therapeutic ultrasound of heart Ther ultrasound of heart 0003 Therapeutic ultrasound of peripheral vascular vessels Ther ult peripheral ves 0009 Other therapeutic ultrasound Other therapeutic ultsnd 0010 Implantation of chemotherapeutic agent Implant chemothera agent 0011 Infusion of drotrecogin alfa (activated) Infus drotrecogin alfa 0012 Administration of inhaled nitric oxide Adm inhal nitric oxide 0013 Injection or infusion of nesiritide Inject/infus nesiritide 0014 Injection or infusion of oxazolidinone class of antibiotics Injection oxazolidinone 0015 High-dose infusion interleukin-2 [IL-2] High-dose infusion IL-2 0016 Pressurized treatment of venous bypass graft [conduit] with pharmaceutical substance Pressurized treat graft 0017 Infusion of vasopressor agent Infusion of vasopressor 0018 Infusion of immunosuppressive antibody therapy Infus immunosup antibody 0019 Disruption of blood brain barrier via infusion [BBBD] BBBD via infusion 0021 Intravascular imaging of extracranial cerebral vessels IVUS extracran cereb ves 0022 Intravascular imaging of intrathoracic vessels IVUS intrathoracic ves 0023 Intravascular imaging of peripheral vessels IVUS peripheral vessels 0024 Intravascular imaging of coronary vessels IVUS coronary vessels 0025 Intravascular imaging of renal vessels IVUS renal vessels 0028 Intravascular imaging, other specified vessel(s) Intravascul imaging NEC 0029 Intravascular -

ORIGINAL ARTICLE Predictable Spontaneous Beating in 96°/O of Coronary Bypass Operations
ORIGINAL ARTICLE Predictable Spontaneous Beating in 96°/o of Coronary Bypass Operations William I. Brenner, MD, FACS Kaiser Foundation Hospital Los Angeles, CA Keywords: Blood cardioplegia, spontaneous beating, cardioversion, coronary bypass, myocardial protection Abstract------------------ Materials and Methods-------------- To determine the incidence of spontaneous beating in isolated All patients were members of a large health maintenance coronary bypass operations, one cardiac surgeon's experience organization (The Kaiser Permanente Medical Care Program of with 677 consecutive cases over an 8 1/2 year period (1980- Southern California). This regionalized practice of cardiac 1988) was studied. Myocardial protection included hypothermic surgery with a traditionally conservative referral pattern by (4°C) blood cardioplegia containing procaine and papaverine, general practitioners, internists, and cardiologists tends to result topical cooling (4°C) and systemic hypothermia (25°C). During in cardiac surgical candidates with advanced coronary artery warming, 100 mg of lidocaine was administered when body disease. The patient profile was evolving during the years of the temperature reached 30°C. Six hundred fifty-one patients (96%) study {Table 1). However, the greater incidence of spontaneous had spontaneous beating after removal of the aortic cross-clamp beating in the 677 patients was consistent in spite of a following completion of distal anastamoses. Electrical seemingly worse patient profile, which included more elderly cardioversion was required immediately in 26 of these 677 patients, more female patients, more operations following recent patients (4%) and in an additional 32 (5%) later in the myocardial infarction, more urgent (rather than elective) operation, usually when ventricular fibrillation was induced by operations, more repeat coronary bypass operations, more use manipulation of the beating heart to inspect the distal of the internal mammary artery (a longer operation) and, for the anastamoses. -

Catheter Ablation for Atrial Fibrillation - Project ID: CRDT0913
Final Topic Refinement Document Catheter Ablation for Atrial Fibrillation - Project ID: CRDT0913 Date: 05/29/2014 Topic: Catheter Ablation for Atrial Fibrillation – Project ID: CRDT0913 EPC: Pacific Northwest EPC AHRQ Task Order Officer: Kim Wittenberg Partner: CMS 1 Final Topic Refinement Document Catheter Ablation for Atrial Fibrillation - Project ID: CRDT0913 Final Topic Refinement Document Key Questions In patients with longstanding persistent atrial fibrillation (AF), persistent AF, or paroxysmal AF (considered separately): Key Question 1. What is the comparative efficacy and effectiveness of AF catheter ablation on short- (6-12 months) and long- (>12 months) term outcomes in the general adult and Medicare populations? Comparisons of interest include: a) Catheter ablation compared with medical therapy b) Comparing ablation using different energy sources Key Question 2. What are the comparative short- and long-term complications and harms (e.g., periprocedural or device-related harms) associated with AF catheter ablation in the general adult and Medicare populations? Comparisons of interest include: a) Catheter ablation compared with medical therapy b) Comparing ablation using different energy sources Key Question 3. Are there modifications of efficacy, effectiveness, or harms of catheter ablation by patient-level characteristics such as age, sex, type of AF, comorbidities, risk for stroke or bleeding events, condition (i.e., patients with significant left ventricular dysfunction/heart failure or patients with significant left atrial enlargement or left ventricular hypertrophy), provider/setting characteristics or technique/approach? Comparisons of interest include: a) Catheter ablation compared with medical therapy b) Comparing ablation using different energy sources 2 Final Topic Refinement Document Catheter Ablation for Atrial Fibrillation - Project ID: CRDT0913 Draft Analytic Framework Figure 1.