Resident Manual of Trauma to the Face, Head, and Neck
Total Page:16
File Type:pdf, Size:1020Kb
Load more
Recommended publications
-

Reference Sheet 1
MALE SEXUAL SYSTEM 8 7 8 OJ 7 .£l"00\.....• ;:; ::>0\~ <Il '"~IQ)I"->. ~cru::>s ~ 6 5 bladder penis prostate gland 4 scrotum seminal vesicle testicle urethra vas deferens FEMALE SEXUAL SYSTEM 2 1 8 " \ 5 ... - ... j 4 labia \ ""\ bladderFallopian"k. "'"f"";".'''¥'&.tube\'WIT / I cervixt r r' \ \ clitorisurethrauterus 7 \ ~~ ;~f4f~ ~:iJ 3 ovaryvagina / ~ 2 / \ \\"- 9 6 adapted from F.L.A.S.H. Reproductive System Reference Sheet 3: GLOSSARY Anus – The opening in the buttocks from which bowel movements come when a person goes to the bathroom. It is part of the digestive system; it gets rid of body wastes. Buttocks – The medical word for a person’s “bottom” or “rear end.” Cervix – The opening of the uterus into the vagina. Circumcision – An operation to remove the foreskin from the penis. Cowper’s Glands – Glands on either side of the urethra that make a discharge which lines the urethra when a man gets an erection, making it less acid-like to protect the sperm. Clitoris – The part of the female genitals that’s full of nerves and becomes erect. It has a glans and a shaft like the penis, but only its glans is on the out side of the body, and it’s much smaller. Discharge – Liquid. Urine and semen are kinds of discharge, but the word is usually used to describe either the normal wetness of the vagina or the abnormal wetness that may come from an infection in the penis or vagina. Duct – Tube, the fallopian tubes may be called oviducts, because they are the path for an ovum. -

The Evolutionary History of the Human Face
This is a repository copy of The evolutionary history of the human face. White Rose Research Online URL for this paper: https://eprints.whiterose.ac.uk/145560/ Version: Accepted Version Article: Lacruz, Rodrigo S, Stringer, Chris B, Kimbel, William H et al. (5 more authors) (2019) The evolutionary history of the human face. Nature Ecology and Evolution. pp. 726-736. ISSN 2397-334X https://doi.org/10.1038/s41559-019-0865-7 Reuse Items deposited in White Rose Research Online are protected by copyright, with all rights reserved unless indicated otherwise. They may be downloaded and/or printed for private study, or other acts as permitted by national copyright laws. The publisher or other rights holders may allow further reproduction and re-use of the full text version. This is indicated by the licence information on the White Rose Research Online record for the item. Takedown If you consider content in White Rose Research Online to be in breach of UK law, please notify us by emailing [email protected] including the URL of the record and the reason for the withdrawal request. [email protected] https://eprints.whiterose.ac.uk/ THE EVOLUTIONARY HISTORY OF THE HUMAN FACE Rodrigo S. Lacruz1*, Chris B. Stringer2, William H. Kimbel3, Bernard Wood4, Katerina Harvati5, Paul O’Higgins6, Timothy G. Bromage7, Juan-Luis Arsuaga8 1* Department of Basic Science and Craniofacial Biology, New York University College of Dentistry; and NYCEP, New York, USA. 2 Department of Earth Sciences, Natural History Museum, London, UK 3 Institute of Human Origins and School of Human Evolution and Social Change, Arizona State University, Tempe, AZ. -

The Morphometry of the Angle of Mandible and Its Correlation with Age and Sex in the Ethekwini Metropolitan Region: a Panoramic Study
Int. J. Morphol., 35(2):661-666, 2017. The Morphometry of the Angle of Mandible and its Correlation with Age and Sex in the eThekwini Metropolitan Region: A Panoramic Study Morfometría del Angulo de la Mandíbula y su Correlación con Edad y Sexo en la Región Metropolitana eThekwini: Un Estudio Panorámico S. Pillay1; S. Ishwarkumar1; B.Z. De Gama1 & P. Pillay1 PILLAY, S.; ISHWARKUMAR, S.; DE GAMA, B. Z. & PILLAY, P. The morphometry of the angle of mandible and its correlation with age and sex in the eThekwini metropolitan region: A panoramic study. Int. J. Morphol., 35(2):661-666, 2017. SUMMARY: The angle of mandible is formed by the tangent line joining the posterior margin of the ramus and the base of the mandible. The angle of mandible has population-specific characteristics therefore; it is imperative to the field of forensic anthropology for age and sex determination. Literary reports regarding the use of the angle of mandible for age and sex determination vary, as some studies support it, while other studies have documented inefficiencies. Therefore, the aim of this investigation was to document the morphometry of the angle of mandible and to determine if a correlation between the angle of mandible, age and sex exists. Sixty four digital panoramic radiographs (n=128) of individuals between 16-30 years were morphometrically analysed using the Dicom Digital Imaging Software. The data was captured and analysed using the Statistical Package for Social Science (SPSS version 23.0). Despite females having a greater angle of mandible than males, no statistically significant correlation was found between the size of the angle of mandible and sex (p=0.088). -
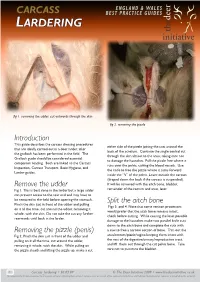
Introduction Remove the Udder Removing the Pizzle (Penis)
fig . removing the udder, cut outwards through the skin fig 2. removing the pizzle Introduction This guide describes the carcass dressing procedures either side of the pizzle joining the cuts around the that are ideally carried out in a deer larder, after back of the scrotum. Continue the single central cut the gralloch has been performed in the field. The through the skin almost to the anus, taking care not Gralloch guide should be considered essential to damage the haunches. Pull the pizzle free where it companion reading. Both are linked to the Carcass runs over the pelvis, cutting the blood vessels. Use Inspection, Carcass Transport, Basic Hygiene, and the knife to free the pizzle where it turns forward Larder guides. inside the “V” of the pelvis. Leave outside the carcass (draped down the back if the carcass is suspended). Remove the udder It will be removed with the aitch bone, bladder, Fig 1. This is best done in the larder but a large udder remainder of the rectum and anus, later. can prevent access to the rear end and may have to be removed in the field before opening the stomach. Split the aitch bone Pinch the skin just in front of the udder and pulling Figs 3. and 4. Note that some venison processors on it all the time, cut around the udder, removing it would prefer that the aitch bone remains intact, whole, with the skin. Do not take the cut any further check before cutting. While causing the least possible rearwards until back in the larder. -

Effects of Glans Penis Augmentation Using Hyaluronic Acid Gel for Premature Ejaculation
International Journal of Impotence Research (2004) 16, 547–551 & 2004 Nature Publishing Group All rights reserved 0955-9930/04 $30.00 www.nature.com/ijir Effects of glans penis augmentation using hyaluronic acid gel for premature ejaculation JJ Kim1, TI Kwak1, BG Jeon1, J Cheon1 and DG Moon1* 1Department of Urology, Korea University College of Medicine, Sungbuk-ku, Seoul, Korea The main limitation of medical treatment for premature ejaculation is recurrence after withdrawal of medication. We evaluated the effect of glans penis augmentation using injectable hyaluronic acid (HA) gel for the treatment of premature ejaculation via blocking accessibility of tactile stimuli to nerve receptors. In 139 patients of premature ejaculation, dorsal neurectomy (Group I, n ¼ 25), dorsal neurectomy with glandular augmentation (Group II, n ¼ 49) and glandular augmentation (Group III, n ¼ 65) were carried out, respectively. Two branches of dorsal nerve preserving that of midline were cut at 2 cm proximal to coronal sulcus. For glandular augmentation, 2 cc of HA was injected into the glans penis, subcutaneously. At 6 months after each procedure, changes of glandular circumference were measured by tapeline in Groups II and III. In each groups, ejaculation time, patient’s satisfaction and partner’s satisfaction were also assessed. There was no significant difference in preoperative ejaculation time among three groups. Preoperative ejaculation times were 89.2740.29, 101.54759.42 and 96.5752.32 s in Groups I, II and III, respectively. Postoperative ejaculation times were significantly increased to 235.6758.6, 324.247107.58 and 281.9793.2 s in Groups I, II and III, respectively (Po0.01). -

Standard Human Facial Proportions
Name:_____________________________________________ Date:__________________Period: __________________ Standard Human Facial Proportions: The standard proportions for the human head can help you place facial features and find their orientation. The list below gives an idea of ideal proportions. • The eyes are halfway between the top of the head and the chin. • The face is divided into 3 parts from the hairline to the eyebrow, from the eyebrow to the bottom of the nose, and from the nose to the chin. • The bottom of the nose is halfway between the eyes and the chin. • The mouth is one third of the distance between the nose and the chin. • The distance between the eyes is equal to the width of one eye. • The face is about the width of five eyes and about the height of about seven eyes. • The base of the nose is about the width of the eye. • The mouth at rest is about the width of an eye. • The corners of the mouth line up with the centers of the eye. Their width is the distance between the pupils of the eye. • The top of the ears line up slightly above the eyes in line with the outer tips of the eyebrows. • The bottom of the ears line up with the bottom of the nose. • The width of the shoulders is equal to two head lengths. • The width of the neck is about ½ a head. Facial Feature Examples.docx Page 1 of 13 Name:_____________________________________________ Date:__________________Period: __________________ PROFILE FACIAL PROPORTIONS Facial Feature Examples.docx Page 2 of 13 Name:_____________________________________________ Date:__________________Period: -

The Gonial Angle Relation with Different Dentitiontal Status on Orthopantomogram in Iraqi Sample
Republic of Iraq Ministry of Higher Education And scientific Research University of Baghdad College of Dentistry The Gonial angle relation with different dentitiontal status on orthopantomogram in iraqi sample A project Submitted to Collage of Dentistry, University of Baghdad. Department of Oral and Maxillofacial Radiology in fulfillment for the requirement to award the degree B.D.S Done by Hadeer Majid Ali 5th Grade Supervisor Dr. Alaa Salah Mahdi B.D.S, M.SC. Oral and Maxillofacial Radiology Baghdad Iraq 2018_1439 Dedication To my parents who were their for me in every step of the way with their have love and support… To my supervisor for his guidance, help and endless support throughout this project… Hadeer Majid Ali Abstract Abstract Background: Mandibular angle plays an important role in ensuring a harmonious facial profile from esthetic point of view so it is a representative of mandible morphology. Resorption of alveolar bone is the best recognized feature of mandibular aging in the edentate subjects and changes of the mandibular cortical shape and thickness may be used as indications to many abnormalities, such as osteoporosis. Panoramic radiographs are a useful tool for the measurement because majority of dentists request an Orthopantomogram for patients during routine dental examination. The Aim of the study: to correlated the gonial angle relation with different dentitional status they are in three group dentulous, partial dentulous and edentulous using digital panoramic imaging system with age, gender and dental status. Subjects, Materials and Methods: This study was conducted on 30 Iraqi in three group dentulous , partial dentulous and edentulous attending to the digital panoramic clinic of the hospital of college of dentistry university of Baghdad Information from each subject was recorded in a special case sheet. -

Mandibular Fractures, Diagnostics, Postoperative Complications
Journal of Medical Sciences. March 23, 2020 - Volume 8 | Issue 13. Electronic-ISSN: 2345-0592 Medical Sciences 2020 Vol. 8 (13), p. 45-52 e-ISSN: 2345-0592 Medical Sciences Online issue Indexed in Index Copernicus Official website: www.medicsciences.com Mandibular fractures, diagnostics, postoperative complications Shahaf Givony1 1 Lithuanian University of Health Sciences. Academy of Medicine. Faculty of Odonthology. ABSTRACT Mandibular fractures usually happen among young males at the age of 16-30 years old. The mandible which has been rated as the second facial bone with the highest rate of injuries, tends to break much more often compared to any other bone of the cranium and represent up to 70% of the cases. This tendency to fracture may be explained by the protruded position, mobility and particular shape of it. The tendency for a mandibular fracture may also be explained by the common risk factors such as vehicle accidents and physical violence that are part of our daily life. There are many other risk factors according to the literature which differ between individuals due to the different socio-economic status, culture, technology and environment. Before the clinical examination of the fracture, it is obligatory to make sure that a clear airway path presents with no other fatal injuries. The examination may be supported by imaging methods which together will approve the diagnosis and method of treatment. Patients with a fracture of the mandible may suffer from post-operative complications which may occur after a short or long duration of the treatment. Those complications may be malocclusion, infections, trismus, damaged teeth and soft tissue, esthetic disfiguration, functional problems, pain and many more. -

View of Urothelial and Metastatic Carcinoma Including Clinical Presentation, Diagnostic Testing, Treatment and Chiropractic Considerations Is Discussed
Daniels et al. Chiropractic & Manual Therapies (2016) 24:14 DOI 10.1186/s12998-016-0097-8 CASE REPORT Open Access Bladder metastasis presenting as neck, arm and thorax pain: a case report Clinton J. Daniels1,2,3*, Pamela J. Wakefield1,2 and Glenn A. Bub1,2 Abstract Background: A case of metastatic carcinoma secondary to urothelial carcinoma presenting as musculoskeletal pain is reported. A brief review of urothelial and metastatic carcinoma including clinical presentation, diagnostic testing, treatment and chiropractic considerations is discussed. Case presentation: This patient presented in November 2014 with progressive neck, thorax and upper extremity pain. Computed tomography revealed a destructive soft tissue mass in the cervical spine and additional lytic lesion of the 1st rib. Prompt referral was made for surgical consultation and medical management. Conclusion: Distant metastasis is rare, but can present as a musculoskeletal complaint. History of carcinoma should alert the treating chiropractic physician to potential for serious disease processes. Keywords: Chiropractic, Neck pain, Transitional cell carcinoma, Bladder cancer, Metastasis, Case report Background serious complication of UC is distant metastasis—with Urothelial carcinoma (UC), also known as transitional higher stage cancer and lymph involvement worsening cell carcinoma (TCC), accounts for more than 90 % of prognosis and cancer survival rate [10]. The 5-year all bladder cancers and commonly metastasizes to the cancer-specific survival rate of UC is estimated to be pelvic lymph nodes, lungs, liver, bones and adrenals or 78 % [10, 11]. brain [1, 2]. The spread of bladder cancer is mainly done Neck pain accounts for 24 % of all disorders seen by via the lymphatic system with the most frequent location chiropractors [12]. -

The Cat Mandible (II): Manipulation of the Jaw, with a New Prosthesis Proposal, to Avoid Iatrogenic Complications
animals Review The Cat Mandible (II): Manipulation of the Jaw, with a New Prosthesis Proposal, to Avoid Iatrogenic Complications Matilde Lombardero 1,*,† , Mario López-Lombardero 2,†, Diana Alonso-Peñarando 3,4 and María del Mar Yllera 1 1 Unit of Veterinary Anatomy and Embryology, Department of Anatomy, Animal Production and Clinical Veterinary Sciences, Faculty of Veterinary Sciences, Campus of Lugo—University of Santiago de Compostela, 27002 Lugo, Spain; [email protected] 2 Engineering Polytechnic School of Gijón, University of Oviedo, 33203 Gijón, Spain; [email protected] 3 Department of Animal Pathology, Faculty of Veterinary Sciences, Campus of Lugo—University of Santiago de Compostela, 27002 Lugo, Spain; [email protected] 4 Veterinary Clinic Villaluenga, calle Centro n◦ 2, Villaluenga de la Sagra, 45520 Toledo, Spain * Correspondence: [email protected]; Tel.: +34-982-822-333 † Both authors contributed equally to this manuscript. Simple Summary: The small size of the feline mandible makes its manipulation difficult when fixing dislocations of the temporomandibular joint or mandibular fractures. In both cases, non-invasive techniques should be considered first. When not possible, fracture repair with internal fixation using bone plates would be the best option. Simple jaw fractures should be repaired first, and caudal to rostral. In addition, a ventral approach makes the bone fragments exposure and its manipulation easier. However, the cat mandible has little space to safely place the bone plate screws without damaging the tooth roots and/or the mandibular blood and nervous supply. As a consequence, we propose a conceptual model of a mandibular prosthesis that would provide biomechanical Citation: Lombardero, M.; stabilization, avoiding any unintended (iatrogenic) damage to those structures. -

Pattern of Skeletal Injuries in Child Physical Abuse
1 Bahrain Medical Bulletin, Vol. 33, No. 2, June 2011 Pattern of Skeletal Injuries in Physically Abused Children Fadheela Al-Mahroos, MD, MHPE* Eshraq A Al-Amer, MD, ABMS (Ped)** Nabar J Umesh, MD, DMRE*** Ali I Alekri, FRCSI, CABS (Ortho)**** Objective: The aim of this study is to identify the frequency and patterns of skeletal injuries among victims of child abuse in Bahrain. Design: Retrospective. Setting: Child Protection Unit at Salmaniya Medical Complex. Method: Child’s characteristics, type of skeletal injuries, location, pattern, radiological findings, and associated other injuries of 36 children were reviewed. Data management and analysis was done using SPSS for Windows, version 18. Result: Thirty-six children with skeletal injuries resulting from child physical abuse were seen from 1991 to 2009. Twenty-three (64%) were males and 13 (36%) were females; the mean age was 3.8 years. Twenty-three (64%) were ≤ 3 years old. Multiple fractures were documented in 19 (53%) children. Bone fracture types and frequency were as follow: 10 (28%) affecting the femur, 9 (25%) skull, 8 (22%) humerus, 6 (17%) rib, 4 (11%) radius, 4 (11%) ulna and 2 (6%) tibia. Other bones less frequently affected were mandible, nasal bone, vertebral, metatarsals, and calcaneus fractures. In addition, other injuries included slipped femoral epiphysis, large bilateral hematoma in vastus lateralis, and full thickness tendon Achilles tear. Hundred percent of rib, ulnar, radial and tibial fractures were in children under one year old. In addition, 7 (78%) of skull fractures, 5 (62%) of humerus fractures, and 5 (50) of femur fractures were under one year old. -

Anatomy Review Upper Extremity WARNING: the Content in This Slideshow Contains Some Sports Footage That May Be Gross
BONES Anatomy Review Upper Extremity WARNING: The content in this slideshow contains some sports footage that may be gross. If you don’t like bodily injuries be warned! SKULL/ FACE Four major bones fuse together to create our cranium . → parietal,temporal,occipital and frontal bones Two major bones of the jaw . → Mandible and Maxilla INJURIES TO THE SKULL & FACE This is raccoon eyes, and battle sign which indicate a skull fracture. Common cause is blunt force trauma to the head, for example, getting hit in the head with a baseball. Often seen in individuals who are beaten or abused. INJURIES TO THE SKULL & FACE This is a picture of Victor Hedman a top defenseman in the NHL. INJURY: laceration to the face. CAUSE: helmet visor was pushed into his face. Lacerations are common during sports and either treated with stitches or glue INJURIES TO THE SKULL & FACE Mandibular Fracture Video Link above is for a Fracture to the mandible Sidney Crosby was hit in the face by a 90 mph slapshot! INJURY: Mandibular Fracture TREATMENT: Surgery ( Jaw was wired shut) He was also provided with a Jaw shield ANTERIOR TORSO Ribs- Remember ribs are discussed in pairs True ribs vs. False ribs- true ribs connect directly to the sternum false ribs do not. Sternum- Broken down into three parts: 1. Manubrium 2. Body 3. Xiphoid process INJURIES TO THE ANTERIOR TORSO INJURY: Fractured Ribs CAUSE: A direct blow or trauma to the ribs Usually detected on x-ray POSTERIOR TORSO Vertebrae → 7 cervical 12 thoracic 5 lumbar BONES OF THE ARM 3 Major bones make up the shoulder: 1.