Traumatic Injuries of the Foot and Ankle
Total Page:16
File Type:pdf, Size:1020Kb
Load more
Recommended publications
-
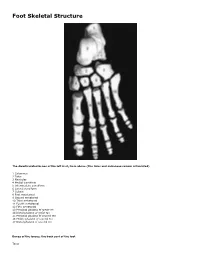
Skeletal Foot Structure
Foot Skeletal Structure The disarticulated bones of the left foot, from above (The talus and calcaneus remain articulated) 1 Calcaneus 2 Talus 3 Navicular 4 Medial cuneiform 5 Intermediate cuneiform 6 Lateral cuneiform 7 Cuboid 8 First metatarsal 9 Second metatarsal 10 Third metatarsal 11 Fourth metatarsal 12 Fifth metatarsal 13 Proximal phalanx of great toe 14 Distal phalanx of great toe 15 Proximal phalanx of second toe 16 Middle phalanx of second toe 17 Distal phalanx of second toe Bones of the tarsus, the back part of the foot Talus Calcaneus Navicular bone Cuboid bone Medial, intermediate and lateral cuneiform bones Bones of the metatarsus, the forepart of the foot First to fifth metatarsal bones (numbered from the medial side) Bones of the toes or digits Phalanges -- a proximal and a distal phalanx for the great toe; proximal, middle and distal phalanges for the second to fifth toes Sesamoid bones Two always present in the tendons of flexor hallucis brevis Origin and meaning of some terms associated with the foot Tibia: Latin for a flute or pipe; the shin bone has a fanciful resemblance to this wind instrument. Fibula: Latin for a pin or skewer; the long thin bone of the leg. Adjective fibular or peroneal, which is from the Greek for pin. Tarsus: Greek for a wicker frame; the basic framework for the back of the foot. Metatarsus: Greek for beyond the tarsus; the forepart of the foot. Talus (astragalus): Latin (Greek) for one of a set of dice; viewed from above the main part of the talus has a rather square appearance. -

Fractures Fractura Pathologica
Fractures Fractura pathologica Myeloma Fractura traumatica Fractura aperta/clausa Fractura simplex/multiplex Fractura comminutiva Fractura transversa/obliqua Fractura spiralis/longitudinalis Fractura compressiva/impressiva Fractura incuneata Infractio = f. partialis = f. incompleta Fractura cum dislocatione ad axim ad latus ad longitudinem cum contractione ad longitudinem cum distractione AO ClassificationAuthentic reports of fractures : 2 S 4220 Fractura colli chirurgici humeri l. dx. comminutiva AO 11-C3 Fracture Healing: 1: REPOSITIO = REDUCTIO fragmentorum CLOSED (short /long term) Fracture Healing: 2: FIXATIO = STABILISATIO fragmentorum PLASTER CAST INTERNAL FIXATION Fracture Healing: 2: FIXATIO = STABILISATIO fragmentorum INTERNAL FIXATION Fracture Healing: 2: FIXATIO = STABILISATIO fragmentorum Name the type of fracture A B C D E F Choose a bone and break it. Try to write as much detailed diagnosis as possible. Authentic reports :1 collement = severe damage of soft tissues Authentic reports :2 Fr. aperta TSCHERNE I - open fracture with small skin injury without its contusion - negligible bacterial contamination Profesor Dr. Harald Tscherne (1933), Traumatology Clinic, Hannover: Classification of fractures published in 1982, T. divides fracture into open and closed. The most important for him is the degree of the soft tissues damage. Authentic reports :3 1 A 45-year-old woman presented with a 3-month history of generalized body pains nonresponsive to analgesic agents. Along with low back pain, she had progressive difficulty in getting up from sitting and supine positions and in walking. There was no history of trauma or any medication intake. She is an orthodox believer who wears a black veil outdoors and is completely covered, with little exposure to the sun. An anteroposterior radio- graph of the pelvis showed an undisplaced transverse fracture of the shaft of both femurs. -

Biomechanical Comparison of Fixation Stability Using a Lisfranc Plate
Foot and Ankle Surgery 25 (2019) 71–78 Contents lists available at ScienceDirect Foot and Ankle Surgery journa l homepage: www.elsevier.com/locate/fas Biomechanical comparison of fixation stability using a Lisfranc plate $ versus transarticular screws a,b a,c, d d Nathan C. Ho , Sophia N. Sangiorgio *, Spenser Cassinelli , Stephen Shymon , d a,b a,c d John Fleming , Virat Agrawal , Edward Ebramzadeh , Thomas G. Harris a The J. Vernon Luck, Sr., M.D. Orthopaedic Research Center, Orthopaedic Institute for Children, in Alliance with UCLA, 403 W. Adams Blvd., Los Angeles, CA 90007, United States b University of Southern California Department of Biomedical Engineering, Los Angeles, CA, United States c University of California, Los Angeles Department of Orthopaedic Surgery, Los Angeles, CA, United States d Los Angeles County Harbor—UCLA Medical Center, Los Angeles, CA, United States A R T I C L E I N F O A B S T R A C T Article history: Background: To obtain adequate fixation in treating Lisfranc soft tissue injuries, the joint is commonly Received 3 March 2017 stabilized using multiple transarticular screws; however iatrogenic injury is a concern. Alternatively, two Received in revised form 28 July 2017 parallel, longitudinally placed plates, can be used to stabilize the 1st and 2nd tarsometatarsal joints; Accepted 8 August 2017 however this may not provide adequate stability along the Lisfranc ligament. Several biomechanical studies have comparedearliermethodsoffixation using platestothestandardtransarticularscrew fixationmethod, Keywords: highlighting the potential issue of transverse stability using plates. A novel dorsal plate is introduced, Lisfranc injury intended to provide transverse and longitudinal stability, without injury to the articular cartilage. -

Fractures of the Anterior Process of the Calcaneum; a Review and Proposed Treatment Algorithm
Foot and Ankle Surgery 25 (2019) 258–263 Contents lists available at ScienceDirect Foot and Ankle Surgery journal homepage: www.elsevier.com/locate/fas Review Fractures of the anterior process of the calcaneum; a review and proposed treatment algorithm a, b b b b Baljinder S. Dhinsa *, Ahmed Latif , Roland Walker , Ali Abbasian , Diane Back , b Sam Singh a William Harvey Hospital, Kennington Road, Willesborough, Ashford TN24 0LZ, United Kingdom b Guy’s and St Thomas’ NHS Foundation Trust, Great Maze Pond, London SE1 9RT, United Kingdom A R T I C L E I N F O A B S T R A C T Article history: Background: There remains a lack of recognition of these fractures, which leads to a delay in diagnosis and Received 18 June 2017 appropriate management. Received in revised form 1 February 2018 Methods: A comprehensive literature search was performed. Following inclusion and exclusion criteria, Accepted 3 February 2018 23 studies were available for analysis. Results: Delay in diagnosis is common and has a negative impact on outcome. If an APC fracture is Keywords: suspected; anteroposterior, lateral and oblique plain radiographs should be requested. Further Fracture investigation with computed tomography or magnetic resonance imaging is indicated if plain Calcaneum radiographs are inconclusive and patient remains symptomatic. Non-operative measures are usually Anterior process Avulsion adequate for most undisplaced fractures, however surgical intervention maybe required for large, intra- Compression articular fractures in the acute setting and for non-union. Calcaneocuboid Conclusions: A treatment algorithm is suggested that may help with the diagnosis and management of these injuries. -

Morphological and Biomechanical Implications of Cuboid Facet of the Navicular Bone in the Gait
Int. J. Morphol., 37(4):1397-1403, 2019. Morphological and Biomechanical Implications of Cuboid Facet of the Navicular Bone in the Gait Implicaciones Morfológicas y Biomecánicas de la Faceta Cuboídea del Navicular en la Marcha Eduardo Saldías1; Assumpció Malgosa1; Xavier Jordana1 & Albert Isidro2 SALDÍAS, E.; MALGOSA, A.; JORDANA, X. & ISIDRO, A. Morphological and biomechanical implications of cuboid facet of the navicular bone in the gait. Int. J. Morphol., 37(4):1397-1403, 2019. SUMMARY: The cuboid facet of the navicular bone is an irregular flat surface, present in non-human primates and some human ancestors. In modern humans, it is not always present and it is described as an “occasional finding”. To date, there is not enough data about its incidence in ancient and contemporary populations, nor a biomechanical explanation about its presence or absence. The aim of the study was to evaluate the presence of the cuboid facet in ancient and recent populations, its relationship with the dimensions of the midtarsal bones and its role in the biomechanics of the gait. 354 pairs of naviculars and other tarsal bones from historical and contemporary populations from Catalonia, Spain, have been studied. We used nine measurements applied to the talus, navicular, and cuboid to check its relationship with facet presence. To analyze biomechanical parameters of the facet, X-ray cinematography was used in living patients. The results showed that about 50 % of individuals developed this surface without differences about sex or series. We also observed larger sagittal lengths of the talar facet (LSAGTAL) in navicular bones with cuboid facet. No significant differences were found in the bones contact during any of the phases of the gait. -

Bones of the Upper and Lower Limb
Bones of the Upper and Lower limb Musculoskeletal block- Anatomy-lecture 1 Editing file Objectives Color guide : important in Red ✓ Classify the bones of the three regions of the lower Doctor note in Green limb (thigh, leg and foot). Extra information in Grey ✓ Memorize the main features of the – Bones of the thigh (femur & patella) – Bones of the leg (tibia & Fibula) – Bones of the foot (tarsals, metatarsals and phalanges) ✓ Recognize the side of the bone. Note: this lecture is based on female slides since Prof abuel makarem said only things that are mentioned in the female slides will come in the exam Note : All bones picture which are described in this lecture are bones on the right side of the body Before start :Please make yourself familiar with these terms to better understand the lecture Terms Meaning Example Ridge The long and narrow upper edge, angle, or crest The supracondylar ridges (in the distal part of of something (the humerus The trochlear notch (in the proximal part of the Notch An indentation, (incision) on an edge or surface (ulna A nodule or a small rounded projection on the Tubercles (Dorsal tubercle (in the distal part of the radius bone A hollow place (The Notch is not complete but the Subscapular fossa (in the concave part of the Fossa fossa is complete and both of them act as the lock (scapula (of the joint A large prominence on a bone usually serving for Deltoid tuberosity (in the humorous) and it Tuberosity the attachment of muscles or ligaments (is a connects the deltoid muscle (bigger projection than the Tubercle -

An Old Mismanaged Lisfranc Injury Treated by Gradual Deformity Correction Followed by the Second-Stage Internal fixation
Strat Traum Limb Recon (2017) 12:59–62 DOI 10.1007/s11751-016-0273-3 CASE REPORT An old mismanaged Lisfranc injury treated by gradual deformity correction followed by the second-stage internal fixation 1 1 1 1 Mehraj D. Tantray • Khurshid Kangoo • Asif Nazir • Muzamil Baba • 1 1 1 Raja Rameez • Syed Tabish • Syed Shahnawaz Received: 29 May 2016 / Accepted: 27 December 2016 / Published online: 5 January 2017 Ó The Author(s) 2017. This article is published with open access at Springerlink.com Abstract The Lisfranc fracture-dislocation of the foot is Keywords Lisfranc injury Á Ilizarov Á Late diagnosis uncommon and diagnosis is often missed. The Lisfranc joint involves the articulation between medial cuneiform and base of the second metatarsal and is considered a Introduction keystone to structural integrity to the midfoot. The articu- lation has a stabilization effect on longitudinal and trans- Injuries to the tarsometatarsal joints are not common and verse arches of the foot. A neglected or untreated injury to represent less than 0.2% of all orthopaedic injuries with the Lisfranc joint can lead to secondary arthritis and sig- a reported incidence of 1 per 55,000 individuals [1]. The nificant morbidity and disability. We present a case of a injury is commonly missed due to gross swelling mask- neglected Lisfranc fracture-dislocation in a 28-year-old ing the deformity and subtle findings on radiological female patient who presented 3 months after injury. A evaluation which requires careful attention. Re-examina- staged treatment of distraction with an Ilizarov ring fixator tion after the decrease in oedema for persistent pain and followed in the second stage by the removal of ring fixator aggravation of pain or instability on stress examination and internal fixation with K wires was performed. -

Part Fracture Dislocation Due to Stress Concentration at Intramedullary Nail End 1Devendra Chouhan, 2Vishal Kumar, 3Manish Kundanmal Kothari, 4Mandeep S Dhillon
JPMER Devendra Chouhan et al 10.5005/jp-journals-10028-1142 CASE REPORT Dissociation of Shaft of Humerus from Head in Three- part Fracture Dislocation due to Stress Concentration at Intramedullary Nail End 1Devendra Chouhan, 2Vishal Kumar, 3Manish Kundanmal Kothari, 4Mandeep S Dhillon ABSTRACT authors best knowledge. We report the first such case A three-part fracture dislocation of the proximal humerus of three-part fracture dislocation involving the greater usually dissociates from the shaft at the level of the surgical tuberosity and proximal shaft of humerus with a 25 years neck or the anatomical neck. Dissociation from the shaft below old Rush nail in situ. this level has not reported in the literature before. Here we describe the injury of a middle aged patient with a three-part CASE REPORT fracture dislocation of the humerus with dissociation of the head from the shaft at the level of proximal shaft humerus with A 60-year-old male presented in the emergency depart- a 25 years old Rush nail in situ. The dislocated head was found ment with acute pain in right shoulder following road abutting the thoracic wall. This case report highlights the effect traffic accident 8 hours ago. He was travelling on a bike of stress concentration at intramedullary nail ends in the upper limb as well as the need for an extended approach when the when a car hit him from the side. He was violently thrown dislocated head appears close to the thoracic wall. off his motorcycle followed by fall on an outstretched hand. He had no other complaints. -

Sport Following Lisfranc Injuries: a Systematic Review and Meta-Analysis
Foot and Ankle Surgery 25 (2019) 654–664 Contents lists available at ScienceDirect Foot and Ankle Surgery journal homepage: www.elsevier.com/locate/fas Return to sport following Lisfranc injuries: A systematic review and meta-analysis a, b c a Gregory Aidan James Robertson *, Kok Kiong Ang , Nicola Maffulli , Gary Keenan , d Alexander MacDonald Wood a Edinburgh Orthopaedic Trauma Unit, Royal Infirmary of Edinburgh, 51 Little France Crescent, Edinburgh EH16 4SA, United Kingdom b Edinburgh Medical School, University of Edinburgh, 47 Little France Crescent, Edinburgh EH16 4TJ, United Kingdom c Queen Mary University of London, Mile End Road, London E1 4NS, United Kingdom d Leeds General Infirmary, Great George St, Leeds LS1 3EX, United Kingdom A R T I C L E I N F O A B S T R A C T Article history: Background: Information regarding return rates (RR) and mean return times (RT) to sport following Received 25 April 2018 Lisfranc injuries remains limited. Received in revised form 17 July 2018 Methods: A systematic search of nine major databases was performed to identify all studies which Accepted 24 July 2018 recorded RR or RT to sport following lisfranc injuries. Results: Seventeen studies were included (n = 366). Keywords: For undisplaced (Stage 1) injuries managed nonoperatively (n = 35), RR was 100% and RT was 4.0 (0–15) Lisfranc wks. For stable minimally-displaced (Stage 2) injuries managed nonoperatively (n = 16), RR was 100% and Tarso-metarsal RT was 9.1 (4–14) wks. Mid-foot Return For the operatively-managed injuries, Percutaneous Reduction Internal Fixation (PRIF) (n = 42), showed Sport significantly better RR and RT compared to both: Open Reduction Internal Fixation (ORIF) (n = 139) (RR — Rate 98% vs 78%, p < 0.019; RT — 11.6 wks vs 19.6 wks, p < 0.001); and Primary Partial Arthrodesis (PPA) (n = 85) Time (RR — 98% vs 85%, p < 0.047; RT — 11.6 wks vs 22.0 wks, p < 0.002). -

Metacarpal Fractures
METACARPAL FRACTURES BY LORYN P. WEINSTEIN, MD, AND DOUGLAS P. HANEL, MD The majority of metacarpal fractures are closed injuries amenable to conservative treatment with external immobilization and subsequent rehabilitation. Internal fixation is favored for unstable fracture patterns and patients who require early motion. Percutaneous pinning usually is successful for metacarpal neck fractures and comminuted head fractures. Shaft and base fractures can be treated with pinning or open reduction and internal fixation; the latter, being more rigid, allows early rehabilitation. External fixation has a limited yet defined role for metacarpal fractures with complex soft-tissue injury and/or segmental bone loss. The recent development of bioabsorbable implants holds promise for skeletal rigidity with minimal soft-tissue morbidity, but long-term in vivo data support- ing the use of these implants is not currently available. Copyright © 2002 by the American Society for Surgery of the Hand arly treatment of metacarpal fractures was lim- Surgical techniques rapidly expanded to include ret- ited to the only tools available: manipulation rograde fracture pinning, intramedullary pinning, and Eand casting. The discovery of percutaneous transfixion pinning. Many of the K-wires in use today fracture fixation near the turn of the century opened have the same diamond-shaped tip and sizing speci- up a new world of possibilities. It was 25 years after fications as the original design. Bennett’s original manuscript that Lambotte de- The first plate and screw set for the hand was scribed the first surgical stabilization of a basilar introduced in the late 1930s. By today’s standards, the thumb fracture by using a thin carpenter’s nail.1 By Hermann Metacarpal Bone Set was quite lean; it 1913, Lambotte had authored a fracture text with included 3 longitudinal plates of 2, 3, and 4 holes, a multiple examples of pinning, wiring, and plating of drill, screwdriver, and 9 screws.1 Improvements in hand fractures. -

Lisfranc Injury and Midfoot Arthritis
Dr Todd Gothelf www.orthosports.com.au 47‐49 Burwood Road, Concord 29‐31 Dora Street, Hurstville 119‐121 Lethbridge Street, Penrith 160 Belmore Road, Randwick Dr Todd Gothelf Shoulder, Foot & Ankle Surgery Midfoot Sprains and Arthritis Todd K Gothelf Foot, Ankle, Shoulder Surgeon Dr Todd Gothelf Shoulder, Foot & Ankle Surgery Midfoot Arthritis • Arthritis of Tarsometatarsal complex • Lisfranc Complex • Major Causes – Lisfranc sprain – Primary Arthritis – Inflammatory Disease Dr Todd Gothelf Shoulder, Foot & Ankle Surgery Lisfranc Injury • One of the most common athletic foot injuries • Difficult Diagnosis • It will see you • Treatable When detected • Arthritis Preventable Dr Todd Gothelf Shoulder, Foot & Ankle Surgery Lisfranc Joints • Tarsometatarsal joint complex • Increased awareness • Fairly common injury in sports • Up to 20% overlooked on initial radiographs • Left untreated, can lead to arthritis, prolonged pain, difficulty returning to sport Dr Todd Gothelf Shoulder, Foot & Ankle Surgery Jacques Lisfranc • French Surgeon • Napolean Era • Described amputations through midfoot Dr Todd Gothelf Shoulder, Foot & Ankle Surgery Mechanism of injury • Direct Injury‐ Crush to Midfoot • Indirect Injury‐ Twisting • With toes planted • Ankle in plantar flexion • Forceful abduction of the midfoot Dr Todd Gothelf Shoulder, Foot & Ankle Surgery Anatomy • Medial cuneiform to the second metatarsal. • Intimately related to one another. • Bones offer primary stability • Held together by ligaments. Dr Todd Gothelf Shoulder, Foot & Ankle Surgery Anatomy‐ -

Fracture Lower Extremity Part II
CONTENTS FEMUR SHAFT BOTH BONE SUBTROCHANTERIC TIBIAL PLAFON FRACTURE LOWER FRACTURE ANKLE EXTREMITIES: PART 2 FRACTURE FEMUR FOOT SUPRACONDYLAR FRACTURE FEMUR CALCANEUS PATELLA TALUS WORAWAT LIMTHONGKUL, M.D. 14 JAN 2013 TIBIA LISFRANC’S TIBIAL PLATEAU METATARSAL 1 2 SUBTROCHANTERIC FRACTURE FEMUR A PART OF FRACTURE OCCUR BETWEEN TIP OF LESSER TROCHANTER AND A POINT 5 SUBTROCHANTERIC CM DISTALLY CALCAR FEMORALE FRACTURE LARGE FORCES ARE NEEDED TO CAUSE FRACTURES IN 5 CM YOUNG & ADULT INJURY IS RELATIVELY TRIVIAL IN ELDERLY 2° CAUSE: OSTEOPOROSIS, OSTEOMALACIA, PAGET’S 3 4 SUBTROCHANTERIC FRACTURE FEMUR TREATMENT INITIAL FEMUR SHAFT TRACTION DEFINITE FRACTURE ORIF WITH INTRAMEDULLARY NAIL OR 95 DEGREE HIP- SCREW-PLATE 5 6 FEMUR FRACTURE FILM HIPS SEVERE PAIN, UNABLE TO BEAR WEIGHT 10% ASSOCIATE FEMORAL SUPRACONDYLAR NECK FRACTURE FEMUR FRACTURE TREATMENT: ORIF WITH IM NAIL OR P&S COMPLICATION: HEMORRHAGE, NEUROVASCULAR INJURY, FAT EMBOLI 7 8 SUPRACONDYLAR FEMUR FRACTURE SUPRACONDYLAR ZONE DIRECT VIOLENCE IS THE USUAL CAUSE PATELLA FRACTURE LOOK FOR INTRA- ARTICULAR INVOLVEMENT CHECK TIBIAL PULSE TREATMENT: ORIF WITH P&S 9 10 PATELLA FRACTURE PATELLA FRACTURE FUNCTION: LENGTHENING THE ANTERIOR LEVER ARM DDX: BIPATITE PATELLA AND INCREASING THE (SUPEROLATERAL) EFFICIENCY OF THE QUADRICEPS. TREATMENT: DIRECT VS INDIRECT NON-DISPLACE, INJURY INTACT EXTENSOR : CYLINDRICAL CAST TEST EXTENSOR MECHANISM DISPLACE, DISRUPT EXTENSOR: ORIF WITH VERTICAL FRACTURE: TBW MERCHANT VIEW 11 12 PATELLAR DISLOCATION ADOLESCENT FEMALE DISLOCATION AROUND USUALLY