Clinical Anatomy of the Lower Extremity
Total Page:16
File Type:pdf, Size:1020Kb
Load more
Recommended publications
-
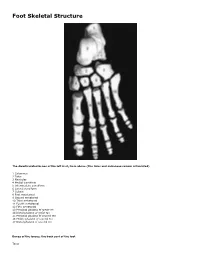
Skeletal Foot Structure
Foot Skeletal Structure The disarticulated bones of the left foot, from above (The talus and calcaneus remain articulated) 1 Calcaneus 2 Talus 3 Navicular 4 Medial cuneiform 5 Intermediate cuneiform 6 Lateral cuneiform 7 Cuboid 8 First metatarsal 9 Second metatarsal 10 Third metatarsal 11 Fourth metatarsal 12 Fifth metatarsal 13 Proximal phalanx of great toe 14 Distal phalanx of great toe 15 Proximal phalanx of second toe 16 Middle phalanx of second toe 17 Distal phalanx of second toe Bones of the tarsus, the back part of the foot Talus Calcaneus Navicular bone Cuboid bone Medial, intermediate and lateral cuneiform bones Bones of the metatarsus, the forepart of the foot First to fifth metatarsal bones (numbered from the medial side) Bones of the toes or digits Phalanges -- a proximal and a distal phalanx for the great toe; proximal, middle and distal phalanges for the second to fifth toes Sesamoid bones Two always present in the tendons of flexor hallucis brevis Origin and meaning of some terms associated with the foot Tibia: Latin for a flute or pipe; the shin bone has a fanciful resemblance to this wind instrument. Fibula: Latin for a pin or skewer; the long thin bone of the leg. Adjective fibular or peroneal, which is from the Greek for pin. Tarsus: Greek for a wicker frame; the basic framework for the back of the foot. Metatarsus: Greek for beyond the tarsus; the forepart of the foot. Talus (astragalus): Latin (Greek) for one of a set of dice; viewed from above the main part of the talus has a rather square appearance. -

Fractures of the Anterior Process of the Calcaneum; a Review and Proposed Treatment Algorithm
Foot and Ankle Surgery 25 (2019) 258–263 Contents lists available at ScienceDirect Foot and Ankle Surgery journal homepage: www.elsevier.com/locate/fas Review Fractures of the anterior process of the calcaneum; a review and proposed treatment algorithm a, b b b b Baljinder S. Dhinsa *, Ahmed Latif , Roland Walker , Ali Abbasian , Diane Back , b Sam Singh a William Harvey Hospital, Kennington Road, Willesborough, Ashford TN24 0LZ, United Kingdom b Guy’s and St Thomas’ NHS Foundation Trust, Great Maze Pond, London SE1 9RT, United Kingdom A R T I C L E I N F O A B S T R A C T Article history: Background: There remains a lack of recognition of these fractures, which leads to a delay in diagnosis and Received 18 June 2017 appropriate management. Received in revised form 1 February 2018 Methods: A comprehensive literature search was performed. Following inclusion and exclusion criteria, Accepted 3 February 2018 23 studies were available for analysis. Results: Delay in diagnosis is common and has a negative impact on outcome. If an APC fracture is Keywords: suspected; anteroposterior, lateral and oblique plain radiographs should be requested. Further Fracture investigation with computed tomography or magnetic resonance imaging is indicated if plain Calcaneum radiographs are inconclusive and patient remains symptomatic. Non-operative measures are usually Anterior process Avulsion adequate for most undisplaced fractures, however surgical intervention maybe required for large, intra- Compression articular fractures in the acute setting and for non-union. Calcaneocuboid Conclusions: A treatment algorithm is suggested that may help with the diagnosis and management of these injuries. -

Morphological and Biomechanical Implications of Cuboid Facet of the Navicular Bone in the Gait
Int. J. Morphol., 37(4):1397-1403, 2019. Morphological and Biomechanical Implications of Cuboid Facet of the Navicular Bone in the Gait Implicaciones Morfológicas y Biomecánicas de la Faceta Cuboídea del Navicular en la Marcha Eduardo Saldías1; Assumpció Malgosa1; Xavier Jordana1 & Albert Isidro2 SALDÍAS, E.; MALGOSA, A.; JORDANA, X. & ISIDRO, A. Morphological and biomechanical implications of cuboid facet of the navicular bone in the gait. Int. J. Morphol., 37(4):1397-1403, 2019. SUMMARY: The cuboid facet of the navicular bone is an irregular flat surface, present in non-human primates and some human ancestors. In modern humans, it is not always present and it is described as an “occasional finding”. To date, there is not enough data about its incidence in ancient and contemporary populations, nor a biomechanical explanation about its presence or absence. The aim of the study was to evaluate the presence of the cuboid facet in ancient and recent populations, its relationship with the dimensions of the midtarsal bones and its role in the biomechanics of the gait. 354 pairs of naviculars and other tarsal bones from historical and contemporary populations from Catalonia, Spain, have been studied. We used nine measurements applied to the talus, navicular, and cuboid to check its relationship with facet presence. To analyze biomechanical parameters of the facet, X-ray cinematography was used in living patients. The results showed that about 50 % of individuals developed this surface without differences about sex or series. We also observed larger sagittal lengths of the talar facet (LSAGTAL) in navicular bones with cuboid facet. No significant differences were found in the bones contact during any of the phases of the gait. -

The Femoral Hernia: Some Necessary Additions
International Journal of Clinical Medicine, 2014, 5, 752-765 Published Online July 2014 in SciRes. http://www.scirp.org/journal/ijcm http://dx.doi.org/10.4236/ijcm.2014.513102 The Femoral Hernia: Some Necessary Additions Ljubomir S. Kovachev Department of General Surgery, Medical University, Pleven, Bulgaria Email: [email protected] Received 28 April 2014; revised 27 May 2014; accepted 26 June 2014 Copyright © 2014 by author and Scientific Research Publishing Inc. This work is licensed under the Creative Commons Attribution International License (CC BY). http://creativecommons.org/licenses/by/4.0/ Abstract Purpose: The anatomic region through which most inguinal hernias emerge is overcrowded by various anatomical structures with intricate relationships. This is reflected by the wide range of anatomic interpretations. Material and Methods: A prospective anatomic study of over 100 fresh cadavers and 47 patients operated on for femoral hernias. Results: It was found that the transver- salis fascia did not continue distally into the lymphatic lacuna. Medially this fascia did not reach the lacunar ligament, but was rather positioned above it forming laterally the vascular sheath. Here the fascia participates in the formation of a fossa, which varies in width and depth—the pre- peritoneal femoral fossa. The results did not confirm the presence of a femoral canal. The dis- tances were measured between the pubic tubercle and the medial margin of the femoral vein, and between the inguinal and the Cooper’s ligaments. The results clearly indicate that in women with femoral hernias these distances are much larger. Along the course of femoral hernia exploration we established the presence of three zones that are rigid and narrow. -

Lower Extremity Clinical/Anatomical Review
LOWER EXTREMITY CLINICAL/ANATOMICAL REVIEW Clinical Condition Anatomy Cause Symptom Hip/Pelvis Femoral Hernia Femoral ring is a weak point in Increase in pressure in Bulge in anterior thigh abdomino-pelvic cavity; abdomen (lifting heavy below Inguinal Ligament Lymphatic vessels course object, cough, etc.) can through Femoral ring to force loop of bowel into Femoral Canal in medial part Femoral Canal (out of Femoral sheath (Sheath Saphenous opening) surrounds Fem. Art, Vein, Lymph) Hip Pointer Anterior Superior Iliac spine Fall on hip causes Bruise on hip (origin of Sartorius, Tens. contusion at spine Fasc. Lata m.) is subcutaneous Pulled Groin Adductor muscles of thigh take Tear in Adductor Pain in groin (at or near origin from pubis muscles can occur in pubis) contact sports Hamstring Pull Hamstring muscles of post. Excessive contraction Agonizing pain in thigh have common origin at (often in running) produces posterior thigh if muscles Ischial Tuberosity tear or avulsion of are avulsed hamstring muscles from Ischial tuberosity Gluteal Gait Gluteus Medius and Minimus Damage to Superior Gluteal Gait act to support body weight Gluteal Nerve or polio (Trendelenberg Sign): when standing (essential when pelvis tilts to down opposite leg is lifted in toward non-paralyzed walking) side when opposite (non- paralyzed) leg is lifted in walking Collateral Cruciate anastomosis links Damage to External Iliac Bleeding (can ligate circulation at hip Inf. Gluteal artery (from Int. or Femoral arteries (stab between Internal Iliac Iliac.) and Profunda -

Classification System of the Tibiofibular Syndesmosis Blood Supply and Its
www.nature.com/scientificreports OPEN Classifcation system of the tibiofbular syndesmosis blood supply and its clinical relevance Received: 16 February 2018 Izabela Mróz1, Piotr J. Bachul1,2, Krzysztof A. Tomaszewski1, Tomasz Bereza1, Krzysztof Gil3, Accepted: 7 June 2018 Jerzy A. Walocha1 & Artur Pasternak 1 Published: xx xx xxxx Due to the lack of anatomical studies concerning complexity of the tibiofbular syndesmosis blood supply, density of blood vessels with further organization of syndesmotic vascular variations is presented in clinically relevant classifcation system. The material for the study was obtained from cadaveric dissections. We dissected 50 human ankles observing diferent types of arterial blood supply. Our classifcation system is based on the vascular variations of the anterior aspect of tibiofbular syndesmosis and corresponds with vascular density. According to our study the mean vascular density of tibiofbular syndesmosis is relatively low (4.4%) and depends on the type of blood supply. The highest density was observed among ankles with complete vasculature and the lowest when lateral anterior malleolar artery was absent (5.8% vs. 3.5%, respectively). Awareness of various types of tibiofbular syndesmosis arterial blood supply is essential for orthopedic surgeons who operate in the ankle region and radiologists for the anatomic evaluation of this area. Knowledge about possible variations along with relatively low density of vessels may contribute to modifcation of treatment approach by the increase of the recommended time of syndesmotic screw stabilization in order to prevent healing complications. Tibiofbular syndesmosis is a fbrous connection localized between the fbular notch of the tibia and medial surface of the lateral ankle. -

Vessels and Circulation
CARDIOVASCULAR SYSTEM OUTLINE 23.1 Anatomy of Blood Vessels 684 23.1a Blood Vessel Tunics 684 23.1b Arteries 685 23.1c Capillaries 688 23 23.1d Veins 689 23.2 Blood Pressure 691 23.3 Systemic Circulation 692 Vessels and 23.3a General Arterial Flow Out of the Heart 693 23.3b General Venous Return to the Heart 693 23.3c Blood Flow Through the Head and Neck 693 23.3d Blood Flow Through the Thoracic and Abdominal Walls 697 23.3e Blood Flow Through the Thoracic Organs 700 Circulation 23.3f Blood Flow Through the Gastrointestinal Tract 701 23.3g Blood Flow Through the Posterior Abdominal Organs, Pelvis, and Perineum 705 23.3h Blood Flow Through the Upper Limb 705 23.3i Blood Flow Through the Lower Limb 709 23.4 Pulmonary Circulation 712 23.5 Review of Heart, Systemic, and Pulmonary Circulation 714 23.6 Aging and the Cardiovascular System 715 23.7 Blood Vessel Development 716 23.7a Artery Development 716 23.7b Vein Development 717 23.7c Comparison of Fetal and Postnatal Circulation 718 MODULE 9: CARDIOVASCULAR SYSTEM mck78097_ch23_683-723.indd 683 2/14/11 4:31 PM 684 Chapter Twenty-Three Vessels and Circulation lood vessels are analogous to highways—they are an efficient larger as they merge and come closer to the heart. The site where B mode of transport for oxygen, carbon dioxide, nutrients, hor- two or more arteries (or two or more veins) converge to supply the mones, and waste products to and from body tissues. The heart is same body region is called an anastomosis (ă-nas ′tō -mō′ sis; pl., the mechanical pump that propels the blood through the vessels. -

Reconstructive
RECONSTRUCTIVE Angiosomes of the Foot and Ankle and Clinical Implications for Limb Salvage: Reconstruction, Incisions, and Revascularization Christopher E. Attinger, Background: Ian Taylor introduced the angiosome concept, separating the M.D. body into distinct three-dimensional blocks of tissue fed by source arteries. Karen Kim Evans, M.D. Understanding the angiosomes of the foot and ankle and the interaction among Erwin Bulan, M.D. their source arteries is clinically useful in surgery of the foot and ankle, especially Peter Blume, D.P.M. in the presence of peripheral vascular disease. Paul Cooper, M.D. Methods: In 50 cadaver dissections of the lower extremity, arteries were injected Washington, D.C.; New Haven, with methyl methacrylate in different colors and dissected. Preoperatively, each Conn.; and Millburn, N.J. reconstructive patient’s vascular anatomy was routinely analyzed using a Dopp- ler instrument and the results were evaluated. Results: There are six angiosomes of the foot and ankle originating from the three main arteries and their branches to the foot and ankle. The three branches of the posterior tibial artery each supply distinct portions of the plantar foot. The two branches of the peroneal artery supply the anterolateral portion of the ankle and rear foot. The anterior tibial artery supplies the anterior ankle, and its continuation, the dorsalis pedis artery, supplies the dorsum of the foot. Blood flow to the foot and ankle is redundant, because the three major arteries feeding the foot have multiple arterial-arterial connections. By selectively performing a Doppler examination of these connections, it is possible to quickly map the existing vascular tree and the direction of flow. -

Vascular Anatomy of the Free Fibula Flap Including the Lateral Head of the Soleus Muscle Applied to Maxillo-Mandibular Reconstruction
Surgical and Radiologic Anatomy (2019) 41:447–454 https://doi.org/10.1007/s00276-018-2166-2 ORIGINAL ARTICLE Vascular anatomy of the free fibula flap including the lateral head of the soleus muscle applied to maxillo-mandibular reconstruction Lara Nokovitch1,2 · Julien Davrou2 · François Bidault4 · Bernard Devauchelle2 · Stéphanie Dakpé2 · Christian Vacher3,5 Received: 1 May 2018 / Accepted: 8 December 2018 / Published online: 14 December 2018 © Springer-Verlag France SAS, part of Springer Nature 2018 Abstract Purpose Initially described by Baudet in 1982, the fibula flap including the lateral head of the soleus muscle allows a one- stage reconstruction for large maxillo-mandibular defects. The aim of this study was to evaluate the number of muscular branches destined to the soleus muscle and their distance from the origin of the fibular artery, to assess the vascular anatomy of the free fibula flap including the lateral head of the soleus muscle applied to maxillo-mandibular reconstruction. Methods We performed a cadaveric anatomic study on ten lower limbs, and a CT angiography anatomic study on 38 legs. The number of soleus branches originating from the fibular artery, and the distance between the origin of the fibular artery and each of the identified branches were measured. Results The number of soleus branches destined to the lateral head of the soleus muscle is variable, with in our study 1–3 branches found. Soleus branches destined to the lateral head of the soleus muscle emerged at a distance ranging between 0 and 2.9 cm (mean value = 1.82 cm) from the origin of the fibular artery in 40% of cases, between 3 and 5.9 cm (mean value = 4.27 cm) from the origin of the fibular artery in 37% of cases, and was at a distance of 6 cm or more (mean value = 6.93 cm) from the origin of the fibular artery in 20% of cases. -

H21/1 H21/2 H21/3
H21/1 (1013026) H21/2 (1013281) H21/1 H21/3 (1013282) H21/2 H21/3 (1013026/1013281/1013282) 2 Latin 1 Vertebra lumbalis [L V], processus articularis 51 Lig. supraspinale superior 52 Lig. sacroiliacum posterius 2 Vertebra lumbalis [L V], corpus vertebrae 53 Lig. sacrococcygeum laterale 3 Vertebra lumbalis [L V], processus costiformis; 54 Lig. sacrococcygeum posterius superficiale; processus costalis Lig. sacrococcygeum dorsale superficiale 4 Crista iliaca 55 Lig. sacrococcygeum posterius profundum; 5 Spina iliaca anterior superior Lig. sacrococcygeum dorsale profundum 6 Fossa iliaca 56 Foramen ischiadicum minus 7 Articulatio sacroiliaca 57 Canalis obturatorius 8 Spina iliaca anterior inferior 58 Arcus iliopectineus 9 Corpus ossis ilii 59 Lig. lacunare 10 Corpus ossis pubis 60 Lacuna vasorum 11 Fossa acetabuli 61 Lacuna musculorum 12 Spina ischiadica 62 Pars abdominalis aortae; Aorta abdominalis 13 Ramus ossis ischii 63 Vena cava inferior 14 Ramus superior ossis pubis 64 Truncus lumbosacralis 15 Ramus inferior ossis pubis 65 Ductus deferens 16 Discus interpubicus; Fibrocartilago interpubica 66 Arteria iliaca externa 17 Pecten ossis pubis 67 Vena iliaca externa 18 Foramen obturatum 68 M. cremaster 19 Foramina sacralia anteriora 69 Nn. scrotales anteriores 20 Promontorium 70 N. dorsalis penis 21 Ala ossis sacri 71 Glans penis 22 Articulatio lumbosacralis, discus intervertebralis 72 A. dorsalis penis® 23 Vertebra lumbalis [L V], processus articularis 73 V. dorsalis profunda penis inferior 74 Tunica vaginalis testis 24 Os sacrum; processus articularis superior 75 Epididymis 25 Ala ossis ilii 76 Plexus pampiniformis 26 Crista sacralis medialis 77 M. pyramidalis 27 Limbus acetabuli; Margo acetabuli 78 M. rectus abdominis 28 Foramen ischiadicum majus 79 Vesica urinaria 29 Tuber ischiadicum 80 M. -

A Study of Popliteal Artery and Its Variations with Clinical Applications
Dissertation on A STUDY OF POPLITEAL ARTERY AND ITS VARIATIONS WITH CLINICAL APPLICATIONS. Submitted in partial fulfillment for M.D. DEGREE EXAMINATION BRANCH- XXIII, ANATOMY Upgraded Institute of Anatomy Madras Medical College and Rajiv Gandhi Government General Hospital, Chennai - 600 003 THE TAMILNADU Dr.M.G.R. MEDICAL UNIVERSITY CHENNAI – 600 032 TAMILNADU MAY-2018 CERTIFICATE This is to certify that this dissertation entitled “A STUDY OF POPLITEAL ARTERY AND ITS VARIATIONS WITH CLINICAL APPLICATIONS” is a bonafide record of the research work done by Dr.N.BAMA, Post graduate student in the Institute of Anatomy, Madras Medical College and Rajiv Gandhi Government General Hospital, Chennai- 03, in partial fulfillment of the regulations laid down by The Tamil Nadu Dr.M.G.R. Medical University for the award of M.D. Degree Branch XXIII- Anatomy, under my guidance and supervision during the academic year from 2015-2018. Dr. Sudha Seshayyan,M.B.B.S., M.S., Dr. B. Chezhian, M.B.B.S., M.S., Director & Professor, Associate Professor, Institute of Anatomy, Institute of Anatomy, Madras Medical College, Madras Medical College, Chennai– 600 003. Chennai– 600 003. The Dean, Madras Medical College & Rajiv Gandhi Govt. General Hospital, Chennai Chennai – 600003. ACKNOWLEDGEMENT I wish to express exquisite thankfulness and gratitude to my most respected teachers, guides Dr. B. Chezhian, Associate Professor Dr.Sudha Seshayyan, Director and Professor, Institute ofAnatomy, Madras Medical College, Chennai – 3, for their invaluable guidance, persistent support and quest for perfection which has made this dissertation take its present shape. I am thankful to Dr. R. Narayana Babu, M.D., DCH, Dean, Madras Medical College, Chennai – 3 for permitting me to avail the facilities in this college for performing this study. -

Compiled for Lower Limb
Updated: December, 9th, 2020 MSI ANATOMY LAB: STRUCTURE LIST Lower Extremity Lower Extremity Osteology Hip bone Tibia • Greater sciatic notch • Medial condyle • Lesser sciatic notch • Lateral condyle • Obturator foramen • Tibial plateau • Acetabulum o Medial tibial plateau o Lunate surface o Lateral tibial plateau o Acetabular notch o Intercondylar eminence • Ischiopubic ramus o Anterior intercondylar area o Posterior intercondylar area Pubic bone (pubis) • Pectineal line • Tibial tuberosity • Pubic tubercle • Medial malleolus • Body • Superior pubic ramus Patella • Inferior pubic ramus Fibula Ischium • Head • Body • Neck • Ramus • Lateral malleolus • Ischial tuberosity • Ischial spine Foot • Calcaneus Ilium o Calcaneal tuberosity • Iliac fossa o Sustentaculum tali (talar shelf) • Anterior superior iliac spine • Anterior inferior iliac spine • Talus o Head • Posterior superior iliac spine o Neck • Posterior inferior iliac spine • Arcuate line • Navicular • Iliac crest • Cuboid • Body • Cuneiforms: medial, intermediate, and lateral Femur • Metatarsals 1-5 • Greater trochanter • Phalanges 1-5 • Lesser trochanter o Proximal • Head o Middle • Neck o Distal • Linea aspera • L • Lateral condyle • L • Intercondylar fossa (notch) • L • Medial condyle • L • Lateral epicondyle • L • Medial epicondyle • L • Adductor tubercle • L • L • L • L • 1 Updated: December, 9th, 2020 Lab 3: Anterior and Medial Thigh Anterior Thigh Medial thigh General Structures Muscles • Fascia lata • Adductor longus m. • Anterior compartment • Adductor brevis m. • Medial compartment • Adductor magnus m. • Great saphenous vein o Adductor hiatus • Femoral sheath o Compartments and contents • Pectineus m. o Femoral canal and ring • Gracilis m. Muscles & Associated Tendons Nerves • Tensor fasciae lata • Obturator nerve • Iliotibial tract (band) • Femoral triangle: Boundaries Vessels o Inguinal ligament • Obturator artery o Sartorius m. • Femoral artery o Adductor longus m.