Bionic Upper Limb Reconstruction: a Valuable Alternative in Global Brachial Plexus Avulsion Injuries—A Case Series
Total Page:16
File Type:pdf, Size:1020Kb
Load more
Recommended publications
-

Clinical Presentations of Lumbar Disc Degeneration and Lumbosacral Nerve Lesions
Hindawi International Journal of Rheumatology Volume 2020, Article ID 2919625, 13 pages https://doi.org/10.1155/2020/2919625 Review Article Clinical Presentations of Lumbar Disc Degeneration and Lumbosacral Nerve Lesions Worku Abie Liyew Biomedical Science Department, School of Medicine, Debre Markos University, Debre Markos, Ethiopia Correspondence should be addressed to Worku Abie Liyew; [email protected] Received 25 April 2020; Revised 26 June 2020; Accepted 13 July 2020; Published 29 August 2020 Academic Editor: Bruce M. Rothschild Copyright © 2020 Worku Abie Liyew. This is an open access article distributed under the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original work is properly cited. Lumbar disc degeneration is defined as the wear and tear of lumbar intervertebral disc, and it is mainly occurring at L3-L4 and L4-S1 vertebrae. Lumbar disc degeneration may lead to disc bulging, osteophytes, loss of disc space, and compression and irritation of the adjacent nerve root. Clinical presentations associated with lumbar disc degeneration and lumbosacral nerve lesion are discogenic pain, radical pain, muscular weakness, and cutaneous. Discogenic pain is usually felt in the lumbar region, or sometimes, it may feel in the buttocks, down to the upper thighs, and it is typically presented with sudden forced flexion and/or rotational moment. Radical pain, muscular weakness, and sensory defects associated with lumbosacral nerve lesions are distributed on -
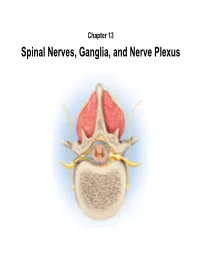
Spinal Nerves, Ganglia, and Nerve Plexus Spinal Nerves
Chapter 13 Spinal Nerves, Ganglia, and Nerve Plexus Spinal Nerves Posterior Spinous process of vertebra Posterior root Deep muscles of back Posterior ramus Spinal cord Transverse process of vertebra Posterior root ganglion Spinal nerve Anterior ramus Meningeal branch Communicating rami Anterior root Vertebral body Sympathetic ganglion Anterior General Anatomy of Nerves and Ganglia • Spinal cord communicates with the rest of the body by way of spinal nerves • nerve = a cordlike organ composed of numerous nerve fibers (axons) bound together by connective tissue – mixed nerves contain both afferent (sensory) and efferent (motor) fibers – composed of thousands of fibers carrying currents in opposite directions Anatomy of a Nerve Copyright © The McGraw-Hill Companies, Inc. Permission required for reproduction or display. Epineurium Perineurium Copyright © The McGraw-Hill Companies, Inc. Permission required for reproduction or display. Endoneurium Nerve Rootlets fiber Posterior root Fascicle Posterior root ganglion Anterior Blood root vessels Spinal nerve (b) Copyright by R.G. Kessel and R.H. Kardon, Tissues and Organs: A Text-Atlas of Scanning Electron Microscopy, 1979, W.H. Freeman, All rights reserved Blood vessels Fascicle Epineurium Perineurium Unmyelinated nerve fibers Myelinated nerve fibers (a) Endoneurium Myelin General Anatomy of Nerves and Ganglia • nerves of peripheral nervous system are ensheathed in Schwann cells – forms neurilemma and often a myelin sheath around the axon – external to neurilemma, each fiber is surrounded by -

A Step Towards Stereotactic Navigation During Pelvic Surgery: 3D Nerve Topography
View metadata, citation and similar papers at core.ac.uk brought to you by CORE provided by Erasmus University Digital Repository Surgical Endoscopy and Other Interventional Techniques https://doi.org/10.1007/s00464-018-6086-3 A step towards stereotactic navigation during pelvic surgery: 3D nerve topography A. R. Wijsmuller1,2 · C. Giraudeau3 · J. Leroy4 · G. J. Kleinrensink5 · E. Rociu6 · L. G. Romagnolo7 · A. G. F. Melani7,8,9 · V. Agnus2 · M. Diana3 · L. Soler3 · B. Dallemagne2 · J. Marescaux2 · D. Mutter2 Received: 10 May 2017 / Accepted: 1 February 2018 © The Author(s) 2018. This article is an open access publication Abstract Background Long-term morbidity after multimodal treatment for rectal cancer is suggested to be mainly made up by nerve- injury-related dysfunctions. Stereotactic navigation for rectal surgery was shown to be feasible and will be facilitated by highlighting structures at risk of iatrogenic damage. The aim of this study was to investigate the ability to make a 3D map of the pelvic nerves with magnetic resonance imaging (MRI). Methods A systematic review was performed to identify a main positional reference for each pelvic nerve and plexus. The nerves were manually delineated in 20 volunteers who were scanned with a 3-T MRI. The nerve identifiability rate and the likelihood of nerve identification correctness were determined. Results The analysis included 61 studies on pelvic nerve anatomy. A main positional reference was defined for each nerve. On MRI, the sacral nerves, the lumbosacral plexus, and the obturator nerve could be identified bilaterally in all volunteers. The sympathetic trunk could be identified in 19 of 20 volunteers bilaterally (95%). -

35. Lumbar Plexus. Sacral Plexus. Coccygeal Plexus
GUIDELINES Students’ independent work during preparation to practical lesson Academic discipline HUMAN ANATOMY Topic LUMBAR PLEXUS. SACRAL PLEXUS. COCCYGEAL PLEXUS 1. Relevance of the topic Lumbar, sacral and coccygeal plexuses innervate the skin of the abdomen, lower back and lower extremities and all the muscles of the lower limbs. Acquired knowledge is the basis for many fields of practical medicine, such as neurology, surgery and traumatology. 2. Specific objectives After the lesson the student should know and be able to: - describe the sources of the formation of the lumbar plexus; - classify the nerves of the lumbar plexus; - to be able to demonstrate and define the branches of the lumbar plexus; - describe sources of sacral plexus formation; - classify sacral plexus nerves; - be able to demonstrate and identify short and long branches of the sacral plexus; - describe the sources of formation coccygeal plexus; - classify coccygeal plexus nerves; - be able to demonstrate and identify branches of coccygeal plexus; - to explain the innervation of muscles and skin in the areas of the lower back and lower extremity. 3. Basic level of preparation For practical this lesson a student should know and be able: - to know the anatomy of the spine, pelvis, lower extremities; - to analyze and show large and small pelvis, their bones; - to analyze and demonstrate bones and joints of the lower limbs; - to demonstrate muscles of the abdomen, perineum, pelvic girdle and lower limbs; - to know the anatomy (external and internal structure) of the spinal cord; - to know the spinal nerve anatomy. 4. Tasks for independent work during preparation for the classes 4.1. -

Management of Metastatic Tumors Invading the Peripheral Nervous System
Neurosurg Focus 22 (6):E14, 2007 Management of metastatic tumors invading the peripheral nervous system JOHN GACHIANI, M.D.,1 DANIEL H. KIM, M.D.,3 ADRIANE NELSON, M.D.,2 AND DAVID KLINE, M.D.1 Departments of 1Neurosurgery and 2Pathology, Louisiana State University Health Sciences Center; 3Department of Neurosurgery, Ochsner Clinic Foundation, New Orleans, Louisiana Object. The authors present the results of a retrospective review of 37 surgically treated metastases to nerve (malignant peripheral non–neural sheath nerve tumors). Tumor frequencies, presentations, management, and prognosis are discussed. Methods. Thirty-seven patients who were treated for metastases to nerve between 1969 and 2006 at the Louisiana State University Health Sciences Center were identified in a review of patient records. Notes regarding patient history and physical examination findings were reviewed to provide informa- tion on presenting symptoms and signs. Imaging and histopathological examination results were also reviewed. Cases were analyzed depending on the primary tumor and the location of metastasis. Results. There included 37 surgically treated lesions, 16 of which originated in the breast and 10 of which originated in the lung. In two cases melanomas had metastasized to nerve, and one tumor each had metastasized from the bladder, rectum, skin, head and neck, and thyroid, and from a primary Ewing sarcoma. There was a single lymphoma that had metastasized to the radial nerve and one chor- doma and one osteosarcoma, each of which had metastasized to the brachial plexus. Conclusions. The nervous system is involved in numerous ways by oncological process. Direct involvement of the peripheral nervous system occurs mostly from direct extension, although it occa- sionally occurs because of distant spread from the primary tumor to nerve. -
Spinal Nerves and Reflexes
Central Nervous System - Spinal Nerves and Reflexes Chapter 13B Spinal Nerves - Number There are 31 pairs of spinal nerves…a total of 62 nerves. Spinal cord is located in the vertebral canal. Spinal nerves exit vertebral column through intervertebral foramina. Intervertebral foramen Vertebral canal Spinal Nerves Interneuron Sensory neuron Sensory fiber Spinal nerve Motor neuron Motor fiber All spinal nerves are mixed nerves….contain sensory and motor fibers. Spinal Nerves - Supply N V C2–C3 C2 C 3 C3 C4 Spinal nerves go to skin, muscles and some T2 C4 C5 T3 T1 of the internal organs. T4 T2 T5 C5 T3 T T 6 4 T7 T5 T8 Dermatomes: areas of the skin that is T2 T6 T9 T T2 T7 10 connected to a specific spinal nerve. T11 T8 T12 T9 C L1 6 T10 L2 T T L3 1 11 L4 C Myotomes: specific muscles that are C6 L 7 T12 5 L1 supplied by a specific spinal nerve. S4S L 3 2 S2 C8 C8 T L3 L1 1 1 S5 C7 S1 L5 L4 S2 L2 KEY L5 L Spinal cord regions 3 = Cervical = Thoracic S = Lumbar 1 = Sacral L4 ANTERIOR POSTERIOR Spinal Nerves - Branches Spinal nerve Dorsal Dorsal root Dorsal root ganglion ramus Spinal nerve Ventral Dorsal horn ramus Ventral Ventral root horn Rami communicantes After exiting vertebral column, EACH spinal nerve splits into branches, called rami: 1. Dorsal ramus: contains nerves that serve the dorsal portions of the trunk- carry visceral motor, somatic motor, and sensory information to and from the skin and muscles of the back. -

BOOK REVIEW Central Nerve Plexus Injury
Spinal Cord (2009) 47, 271–272 & 2009 International Spinal Cord Society All rights reserved 1362-4393/09 $32.00 www.nature.com/sc BOOK REVIEW Central nerve plexus injury Carlstedt T even though the book was published in 2007, only about 10% Central Nerve Plexus Injury, London, Imperial College Press, 2007, of the references listed in this chapter were published after 192 pages, US $128.00 2000, and the most recent papers were published in 2004. ISBN-10: 1860945732; ISBN-13: 978-1860945731 In Chapter 7, the author describes his approach to managing the brachial and lumbosacral plexuses. His Spinal Cord (2009) 47, 271–272; doi:10.1038/sc.2008.111 descriptions of surgical procedures are well written. How- ever, the quality of the photographs of surgical procedures is The fact that neurons from the central nervous system can less than satisfactory in most instances. regenerate into peripheral nerves has been known for a long In Chapter 8, Dr Carlstedt describes his experiences with time.1 Now,inhisbook,DrCarlstedtappliesthisconceptto intradural root repair in a limited series of patients. He repair avulsion injuries of the brachial and lumbosacral plexus. attributes any and all recovery experienced by these patients In Chapter 1 of his book, Dr Carlstedt briefly describes the to the spinal procedure and then challenges the axiom that history of brachial plexus repair, up to his first cases of root normal function cannot be restored after any procedure in reimplantation into the spinal cord. the brachial plexus, excluding neurolysis. The fact that he In Chapter 2, he reviews the mechanisms and patterns of fails to consider other nonsurgical sources of recovery within root avulsion, reinforcing the concept that the lower roots of his small series of patients is disturbing. -

The Intrinsic Cardiac Nervous System and Its Role in Cardiac Pacemaking and Conduction
Journal of Cardiovascular Development and Disease Review The Intrinsic Cardiac Nervous System and Its Role in Cardiac Pacemaking and Conduction Laura Fedele * and Thomas Brand * Developmental Dynamics, National Heart and Lung Institute (NHLI), Imperial College, London W12 0NN, UK * Correspondence: [email protected] (L.F.); [email protected] (T.B.); Tel.: +44-(0)-207-594-6531 (L.F.); +44-(0)-207-594-8744 (T.B.) Received: 17 August 2020; Accepted: 20 November 2020; Published: 24 November 2020 Abstract: The cardiac autonomic nervous system (CANS) plays a key role for the regulation of cardiac activity with its dysregulation being involved in various heart diseases, such as cardiac arrhythmias. The CANS comprises the extrinsic and intrinsic innervation of the heart. The intrinsic cardiac nervous system (ICNS) includes the network of the intracardiac ganglia and interconnecting neurons. The cardiac ganglia contribute to the tight modulation of cardiac electrophysiology, working as a local hub integrating the inputs of the extrinsic innervation and the ICNS. A better understanding of the role of the ICNS for the modulation of the cardiac conduction system will be crucial for targeted therapies of various arrhythmias. We describe the embryonic development, anatomy, and physiology of the ICNS. By correlating the topography of the intracardiac neurons with what is known regarding their biophysical and neurochemical properties, we outline their physiological role in the control of pacemaker activity of the sinoatrial and atrioventricular nodes. We conclude by highlighting cardiac disorders with a putative involvement of the ICNS and outline open questions that need to be addressed in order to better understand the physiology and pathophysiology of the ICNS. -

Overview of Spinal Nerves
Spinal Nerves Boundless Overview of Spinal Nerves Spinal nerves, a part of the PNS, generally refers to mixed nerves, with motor, sensory, and autonomic signals between the CNS and the body. 1. fig. 1 shows a spinal nerve Spinal nerves arise from a combination of nerve fibers: the dorsal and ventral roots of the spinal cord. Afferent sensory axons, bringing sensory information from the body to the spinal cord and brain, travel through the dorsal roots of the spinal cord, and efferent motor axons, bringing motor information from the brain to the body, travel through the ventral roots of the spinal cord. All spinal nerves except the first pair emerge from the spinal column through an opening between vertebrae, called an intervertebral foramen. The spinal nerves are typically labeled by their location in the body: thoracic, lumbar, or sacral. Dorsal Root: Also known as the posterior root, the afferent sensory root of a spinal nerve. Autonomic: Acting or occurring involuntarily, without conscious control. Intervertebral Foramen: The foramen allows for the passage of the spinal nerve root, dorsal root ganglion, the spinal artery of the segmental artery, communicating veins between the internal and external plexuses, recurrent meningeal (sinu- vertebral) nerves, and transforaminal ligaments. 2. Source URL: https://www.boundless.com/physiology/peripheral-nervous-system-pns/spinal-nerves/ Saylor URL: http://www.saylor.org/courses/psych402/ Attributed to: [Boundless] www.saylor.org Page 1 of 12 fig. 2 shows intervertebral foramina Intervertebral foramina are indicated by arrows. Spinal Nerves The term spinal nerve generally refers to a mixed spinal nerve, which carries motor, sensory, and autonomic signals between the spinal cord and the body. -

The Spinal Cord and Spinal Nerves
14 The Nervous System: The Spinal Cord and Spinal Nerves PowerPoint® Lecture Presentations prepared by Steven Bassett Southeast Community College Lincoln, Nebraska © 2012 Pearson Education, Inc. Introduction • The Central Nervous System (CNS) consists of: • The spinal cord • Integrates and processes information • Can function with the brain • Can function independently of the brain • The brain • Integrates and processes information • Can function with the spinal cord • Can function independently of the spinal cord © 2012 Pearson Education, Inc. Gross Anatomy of the Spinal Cord • Features of the Spinal Cord • 45 cm in length • Passes through the foramen magnum • Extends from the brain to L1 • Consists of: • Cervical region • Thoracic region • Lumbar region • Sacral region • Coccygeal region © 2012 Pearson Education, Inc. Gross Anatomy of the Spinal Cord • Features of the Spinal Cord • Consists of (continued): • Cervical enlargement • Lumbosacral enlargement • Conus medullaris • Cauda equina • Filum terminale: becomes a component of the coccygeal ligament • Posterior and anterior median sulci © 2012 Pearson Education, Inc. Figure 14.1a Gross Anatomy of the Spinal Cord C1 C2 Cervical spinal C3 nerves C4 C5 C 6 Cervical C 7 enlargement C8 T1 T2 T3 T4 T5 T6 T7 Thoracic T8 spinal Posterior nerves T9 median sulcus T10 Lumbosacral T11 enlargement T12 L Conus 1 medullaris L2 Lumbar L3 Inferior spinal tip of nerves spinal cord L4 Cauda equina L5 S1 Sacral spinal S nerves 2 S3 S4 S5 Coccygeal Filum terminale nerve (Co1) (in coccygeal ligament) Superficial anatomy and orientation of the adult spinal cord. The numbers to the left identify the spinal nerves and indicate where the nerve roots leave the vertebral canal. -
Autonomic Nervous System
NERVOUS SYSTEM OUTLINE 18.1 Comparison of the Somatic and Autonomic Nervous Systems 540 18.2 Overview of the Autonomic Nervous System 542 18 18.3 Parasympathetic Division 545 18.3a Cranial Nerves 545 18.3b Sacral Spinal Nerves 545 18.3c Effects and General Functions of the Parasympathetic Division 545 Autonomic 18.4 Sympathetic Division 547 18.4a Organization and Anatomy of the Sympathetic Division 547 18.4b Sympathetic Pathways 550 Nervous 18.4c Effects and General Functions of the Sympathetic Division 550 18.5 Other Features of the Autonomic Nervous System 552 System 18.5a Autonomic Plexuses 552 18.5b Neurotransmitters and Receptors 553 18.5c Dual Innervation 554 18.5d Autonomic Reflexes 555 18.6 CNS Control of Autonomic Function 556 18.7 Development of the Autonomic Nervous System 557 MODULE 7: NERVOUS SYSTEM mck78097_ch18_539-560.indd 539 2/14/11 3:46 PM 540 Chapter Eighteen Autonomic Nervous System n a twisting downhill slope, an Olympic skier is concentrat- Recall from figure 14.2 (page 417) that the somatic nervous O ing on controlling his body to negotiate the course faster than system and the autonomic nervous system are part of both the anyone else in the world. Compared to the spectators in the viewing central nervous system and the peripheral nervous system. The areas, his pupils are more dilated, and his heart is beating faster SNS operates under our conscious control, as exemplified by vol- and pumping more blood to his skeletal muscles. At the same time, untary activities such as getting out of a chair, picking up a ball, organ system functions not needed in the race are practically shut walking outside, and throwing the ball for the dog to chase. -

Dynamic Sling to Support Upper Extremity Post Brachial Plexus Injury To
Dynamic Sling to Support Upper Extremity Post Brachial Plexus Injury to Return to Active Lifestyle Final Report December 12th, 2012 Team Members Amy Martin (Team Leader) Lindy Couwenhoven (Communicator) Stephen Monette (BWIG) Clair Kurzynski (BSAC) Clients Karen Blaschke, OTR Margaret Overstake Advisor John Puccinelli, Ph.D. 1 Table of Contents Abstract 4 Problem Motivation 5 Client Description 6 Current Devices 6 Marketed Devices 6 Past Prototypes 8 Design Requirements 8 Design Alternatives 9 Backpack Design 9 Ring Design 10 One Strap Design 11 Design Matrix 12 Patient Comfort 13 Effectiveness 13 Ease of Use 14 Adjustability 14 Safety 14 Cost 14 Preliminary Analysis 15 Final Design 16 Fabrication 18 2 Testing 19 Usability 19 Applied Force 20 Final Budget 22 Future Work 22 Timeline 23 References 25 Appendix 26 Product Design Specifications 26 Free Body Diagram Analysis 29 Testing: Raw Data 31 Usability Testing Evaluation Form 33 Usability Testing Instructions 34 3 Abstract The brachial plexus is a network of nerves in the shoulder that can cause varying levels of sensation and motor loss if damaged [1, 2]. Karen Blaschke is an occupational therapist with UW Hospitals and Clinics, and she works with patients that have experienced brachial plexus injury including our client, Margaret Overstake. Our design team was asked to create a dynamic sling that would allow someone with a brachial plexus injury to return to an active lifestyle. The sling should be adaptable for patients at different levels of rehabilitation. The final design we chose to pursue incorporates a chest strap with components that distribute the weight of the injured arm to the opposite shoulder.