HIV As an Occupational Disease: Expanding Traditional Workers' Compensation Coverage
Total Page:16
File Type:pdf, Size:1020Kb
Load more
Recommended publications
-

Grim Consequences of Workplace Traditional Bullying and Cyberbullying by Way of Mediation: a Case of Service Sector of Pakistan Mehwish Iftikhar , Loo-See Beh
International Journal of Recent Technology and Engineering (IJRTE) ISSN: 2277-3878, Volume-8 Issue-2S, July 2019 Grim Consequences of Workplace Traditional Bullying and Cyberbullying by Way of Mediation: A Case of Service Sector of Pakistan Mehwish Iftikhar , Loo-See Beh healthy workforce. Therefore, a healthy workforce is the Abstract: Various studies have been conducted to measure precondition of productivity and economic development bullying incidence and prevalence in multiple organizational (World Health Organization (WHO), 2007). Employee settings based on a variety of methods and research design. health plays a significant role in the efficiency of any Nonetheless, these studies indicate that bullying is a devastating organization. Accordingly, providing a healthy work and crippling problem that should be addressed in relation to its environment should be the leading priority of each adverse effects and implications. This study identified several organization. Every work environment is considered healthy gaps in the literature when expanded specifically to the service sector of Pakistan, where the problem of bullying is prevalent. if harmful working conditions are absent and This research endeavored to fill in the aforementioned gaps by health-promoting activities and actions are present. The precisely focusing on organizational climate as a cause of maintenance of occupational health is costly (i.e., to promote bullying (based on frustration–aggression theory and social and maintain the highest degree of physical, mental, and interaction approach), technology in relation to cyberbullying, emotional well-being of workers) and the burden of such cost and effects on employee health. Hence, this study contributes to is increasing. The WHO Factsheet (2014) indicated that a the emergent discussion in identifying the debilitating outcomes majority of countries faced an economic loss of 4% to 6% of of bullying. -

Mobbing, Subjective Perception, Demographic Factors And
Cent Eur J Public Health 2020; 28 (Suppl): S57–S64 MOBBING, SUBJECTIVE PERCEPTION, DEMOGRAPHIC FACTORS AND PREVALENCE OF BURNOUT SYNDROME IN NURSES Šárka Vévodová, Jiří Vévoda, Bronislava Grygová Department of Humanities and Social Sciences, Faculty of Health Sciences, Palacký University in Olomouc, Olomouc, Czech Republic SUMMARY Objectives: The aim of the study was to assess the prevalence of burnout syndrome and mobbing, to determine their mutual relationship, and to identify predictors related to the probability of occurrence of burnout syndrome in general nurses working in hospitals. Methods: The work is designed as a cross-sectional study. The research took place in 2018 and the sample included 250 general nurses. Sta- tistical evaluation was performed by means of descriptive statistics, Spearman’s correlation coefficient, and logistic regression. Three standardized questionnaires were used – Maslach Burnout Inventory, Negative Questionnaire Act and SUPSO. Results: The research revealed burnout syndrome in the area of emotional exhaustion in 28.8% of nurses, of depersonalization in 15.2%, and in the area of personal accomplishment in 38.4%. 51.2% of nurses never experienced mobbing at workplace, one act of mobbing over the last six months was reported by 17.6% of respondents, two and more acts by 31.2%. Logistic regression revealed that the probability of occurrence of burnout syndrome in the area of emotional exhaustion is influenced by age, sex and by the size of an urban area, it is increased by anxiety and depression. In the area of depersonalization the probability of incidence increases with impulsiveness and dejection. In the area of personal accomplishment the probability of burnout syndrome incidence is increased by the lack of psychological wellbeing and activeness, by restlessness and impulsiveness. -

Maximising the Value of Occupational Health & Safety and Workplace Wellness Reporting for a Global Workforce: a Practical
Maximising the value of Occupational Health & Safety and workplace wellness reporting for a global workforce: A practical guide for internationally operating employers London|Washington D.C. Commissioned by the Maximising the value of Occupational Health & Safety and workplace wellness reporting for a global workforce: A practical guide for internationally operating employers London|Washington D.C. Commissioned by the Contents i Foreword 3 4.2.3 The difficulty of developing cross-border health and wellness programmes 28 ii Executive summary 5 4.2.4 The difficulty of changing behaviours 28 1. Introduction 9 4.2.5 Current reporting frameworks are inadequate 28 2. The value of good sustainability reporting 10 4.2.6 The difficulty of developing relevant, 2.1 Sustainability reporting 11 insightful wellness metrics 28 2.1.1 What is sustainability reporting? 11 4.3 Best practice company characteristics 29 2.1.2 A progressive mainstreaming 5. Case studies: Best practices in OH&S of sustainability reporting 11 and risk management reporting—and 2.1.3 Benefits of sustainability reporting 12 how to get the most from them. 30 2.2 Occupational Health & Safety (OH&S) reporting 12 5.1 Integrating health and wellness into an overarching corporate strategy: UNILEVER 31 2.2.1 Trends in Occupational Health & Safety practice and reporting 12 5.2 Measuring activities and progress against specified targets: JOHNSON & JOHNSON 31 3. Guide: How to do OH&S reporting well 14 5.3 Collaborating with multiple stakeholders: 3.1 Foundational elements of good reporting 15 NOVO NORDISK 31 3.2 Using global reporting frameworks 17 6. -

The Workers Compensation Impacts of 2019 Coronavirus (COVID-19)
The workers compensation impacts of 2019 Coronavirus (COVID-19) A special report brought to you by 2 An overview of the 2019 Coronavirus (COVID-19) The primary Coronavirus disease 2019 (COVID-19) China. Incidents of COVID-19 have now been found infection, which can result in pneumonia and even globally, with the World Health Organization (WHO) death, originated from a seafood market in Wuhan declaring COVID-19 a global health emergency. City, Hubei Province of China. Subsequently, person-to-person transmission has occurred, Coronaviruses are a family of RNA viruses, primarily to health workers who had contact with including the common cold, SARS and MERS, those initially infected. This has led to widespread according to the WHO. While causing seasonal infections in China with hundreds of new confirmed influenza-like symptoms, they differ. This has infections daily across the globe. At the time of implications for hosts, transmissibility, susceptibility, writing (February 28, 2020), travel from Wuhan antiviral therapy, immunity, vaccines, etc. Multiple and the surrounding provinces has been banned, strains of COVID-19 have been identified, but the as Chinese authorities seek to limit spread of the impacts on humans, even within a specific strain, infection. Prior to this lockdown by Wuhan officials, are inconsistent. The described symptoms of which began on January 23, 2020, people affected COVID-19 vary between a mild upper respiratory by the virus travelled worldwide with the possibility infection and severe pneumonia, which could lead of further infections arising from person-to-person to death. The websites of the relevant Government contact in the places they visited. -

5115 Sbr Lcta Ta 21
SENATE BILL REPORT SB 5115 As of January 18, 2021 Title: An act relating to establishing health emergency labor standards. Brief Description: Establishing health emergency labor standards. Sponsors: Senators Keiser, Liias, Conway, Kuderer, Lovelett, Nguyen, Salomon, Stanford and Wilson, C.. Brief History: Committee Activity: Labor, Commerce & Tribal Affairs: 1/18/21. Brief Summary of Bill • Creates an occupational disease presumption for frontline workers during a public health emergency for the purposes of workers' compensation. • Requires employers to accommodate an employee's voluntary use of protective equipment during a public health emergency. • Prohibits discrimination against an employee who raises a reasonable concern about infection control in the workplace during a public health emergency and authorizes a person to bring actions on behalf of the Department of Labor and Industries (L&I) in court for violations of the retaliation provisions of the bill. • Expands the eligibility for Family and Medical Leave to employees that earn at least $1,000 in covered employment if their qualifying period includes a public health emergency. • Requires an employer to pay its lower-paid frontline employees health emergency pay during a public health emergency. • Requires employers to notify L&I when a certain percentage of their workforce becomes infected during a public health emergency. • Establishes additional sick leave for employees who are quarantined or This analysis was prepared by non-partisan legislative staff for the use of legislative members in their deliberations. This analysis is not part of the legislation nor does it constitute a statement of legislative intent. Senate Bill Report - 1 - SB 5115 infected, caring for someone who is quarantined or infected, or caring for their child due to school or child care closures during a public health emergency. -

Evaluation of Occupational Risk Factors for Nurses and Cnas
University of South Florida Scholar Commons Graduate Theses and Dissertations Graduate School January 2013 Evaluation of Occupational Risk Factors for Nurses and CNAs: Analysis of Florida Workers' Compensation Claims Database Sheila Mohammed University of South Florida, [email protected] Follow this and additional works at: http://scholarcommons.usf.edu/etd Part of the Occupational Health and Industrial Hygiene Commons, and the Toxicology Commons Scholar Commons Citation Mohammed, Sheila, "Evaluation of Occupational Risk Factors for Nurses and CNAs: Analysis of Florida Workers' Compensation Claims Database" (2013). Graduate Theses and Dissertations. http://scholarcommons.usf.edu/etd/4731 This Dissertation is brought to you for free and open access by the Graduate School at Scholar Commons. It has been accepted for inclusion in Graduate Theses and Dissertations by an authorized administrator of Scholar Commons. For more information, please contact [email protected]. Evaluation of Occupational Risk Factors for Nurses and CNAs: Analysis of Florida Workers’ Compensation Claims Database by Sheila Mohammed A dissertation submitted in partial fulfillment of the requirements for the degree of Doctor of Philosophy Department of Environmental and Occupational Health College of Public Health University of South Florida Major Professor: Raymond Harbison, Ph.D. Giffe Johnson, Ph.D. James McCluskey, M.D., Ph.D. Steve Morris, M.D. Date of Approval: June 3, 2013 Keywords: Musculoskeletal Injuries, Violence, Lifting, Falls, Puncture Wounds, Cost, Prevention Copyright © 2013, Sheila Mohammed Dedication I dedicate this dissertation to my mother, Zorida Mohammed, who did her very best to see that I got an education and never hindered my aspirations, and to Lisa Davis who shouldered much of my responsibilities so that I could have the time to explore and write this scientific work. -

Enough Is Enough Putting a Stop to Violence in the Health Care Sector
ENOUGH IS ENOUGH PUTTING A STOP TO VIOLENCE IN THE HEALTH CARE SECTOR ENOUGH IS - A DISCUSSION PAPER - ENOUGH JUNE 2017 THE CANADIAN FEDERATION OF NURSES UNIONS (CFNU) Published by: The Canadian Federation of Nurses Unions www.nursesunions.ca 2841 Riverside Drive Ottawa, ON K1V 8X7 613-526-4661 © 2017 The Canadian Federation of Nurses Unions All rights reserved. No part of this book may be reproduced or transmitted in any form or by any means, electronic or mechanical, including photocopying, recording, or by any information storage or retrieval system without the permission of the publisher. This book was prepared by the CFNU to provide information on a particular topic or topics. The views and opinions expressed within are solely those of the individuals to whom they are attributed and do not necessarily reflect the policies or views of the CFNU or its member organizations. Author: Carol Reichert Project team: Emily Doer, Oxana Genina Advisory committee: CFNU Occupational Health and Safety Network First edition, June 2017 ISBN: 978-0-9868382-9-3 About this discussion paper The Canadian Federation of Nurses Unions has produced this discussion paper in order to catalyze a national discussion on violence in health care – one that brings together the disparate stories from coast to coast, highlighting its broad and pervasive impacts. Further, this paper is intended to serve as a national Call to Action. As the national federation of nurses’ unions, representing close to 200,000 frontline care providers, and nursing students, the CFNU is calling on governments, employers, unions and frontline nurses themselves to work together to put a stop to violence in health care. -

Problems in Occupational Disease Compensation for Occupational Diseases
Upjohn Institute Press Problems in Occupational Disease Compensation for Occupational Diseases Leslie I. Boden Boston University Chapter 13 (pp. 323-326) in: Current Issues in Workers' Compensation James Chelius, ed. Kalamazoo, MI: W.E. Upjohn Institute for Employment Research, 1986 DOI: 10.17848/9780880995443.ch13 Copyright ©1986. W.E. Upjohn Institute for Employment Research. All rights reserved. 13 Problems in Occupational Disease Compensation Leslie I. Boden School of Public Health Boston University The papers presented in this section cover an important set of issues in workers' compensation for occupational diseases. First, we are presented with data indicating that the current state systems have serious problems compensating victims of asbestos-related diseases and, by inference, other occupational diseases which are even less well understood. Then, we are given proposals for solving the problems of compensating occupational diseases, solutions proposed to be implemented at the federal level. Spatz's paper presents a "best case" picture of occupa tional disease compensation in the United States. He chooses a state system with no artificial barriers to compensation; the most well-known occupational disease agent; and workers who had been under study and were therefore likely to be more aware of the occupational origin of their diseases. In spite of these favorable conditions, Spatz documents serious problems faced by survivors of insulation workers who died from asbestos-related diseases. The issues are familiar ones, echoing those discussed by Earth and Hunt, 1 and by Earth2 in his recent study of asbestos insulation workers. In Spatz's 313 314 Occupational Disease Compensation study, workers' compensation claims for asbestos-related disease were generally controverted, resulting in long delays, high legal expenses, and uncertain outcomes. -
WCIO Injury Description Codes Nature of Injury
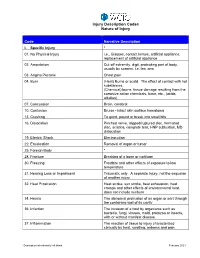
Injury Description Codes Nature of Injury Code Narrative Description I. Specific Injury * 01. No Physical Injury i.e., Glasses, contact lenses, artificial appliance, replacement of artificial appliance 02. Amputation Cut off extremity, digit, protruding part of body, usually by surgery, i.e. leg, arm 03. Angina Pectoris Chest pain 04. Burn (Heat) Burns or scald. The effect of contact with hot substances. (Chemical) burns. tissue damage resulting from the corrosive action chemicals, fume, etc., (acids, alkalies) 07. Concussion Brain, cerebral 10. Contusion Bruise - intact skin surface hematoma 13. Crushing To grind, pound or break into small bits 16. Dislocation Pinched nerve, slipped/ruptured disc, herniated disc, sciatica, complete tear, HNP subluxtion, MD dislocation 19. Electric Shock Electrocution 22. Enucleation Removal of organ or tumor 25. Foreign Body * 28. Fracture Breaking of a bone or cartilage 30. Freezing Frostbite and other effects of exposure to low temperature 31. Hearing Loss or Impairment Traumatic only. A separate injury, not the sequelae of another injury 32. Heat Prostration Heat stroke, sun stroke, heat exhaustion, heat cramps and other effects of environmental heat. does not include sunburn 34. Hernia The abnormal protrusion of an organ or part through the containing wall of its cavity 36. Infection The invasion of a host by organisms such as bacteria, fungi, viruses, mold, protozoa or insects, with or without manifest disease. 37. Inflammation The reaction of tissue to injury characterized clinically by heat, swelling, redness and pain *Description intentionally left blank. February 2021 Injury Description Codes Nature of Injury 38. Adverse reaction to a vaccination or * inoculation 40. -

Injury Description Codes Nature of Injury
Injury Description Codes Nature of Injury Code Narrative Description I. Specific Injury * 01. No Physical Injury i.e., Glasses, contact lenses, artificial appliance, replacement of artificial appliance 02. Amputation Cut off extremity, digit, protruding part of body, usually by surgery, i.e. leg, arm 03. Angina Pectoris Chest pain 04. Burn (Heat) Burns or scald. The effect of contact with hot substances. (Chemical) burns. tissue damage resulting from the corrosive action chemicals, fume, etc., (acids, alkalies) 07. Concussion Brain, cerebral 10. Contusion Bruise - intact skin surface hematoma 13. Crushing To grind, pound or break into small bits 16. Dislocation Pinched nerve, slipped/ruptured disc, herniated disc, sciatica, complete tear, HNP subluxtion, MD dislocation 19. Electric Shock Electrocution 22. Enucleation Removal of organ or tumor 25. Foreign Body * 28. Fracture Breaking of a bone or cartilage 30. Freezing Frostbite and other effects of exposure to low temperature 31. Hearing Loss or Impairment Traumatic only. A separate injury, not the sequelae of another injury 32. Heat Prostration Heat stroke, sun stroke, heat exhaustion, heat cramps and other effects of environmental heat. does not include sunburn 34. Hernia The abnormal protrusion of an organ or part through the containing wall of its cavity 36. Infection The invasion of a host by organisms such as bacteria, fungi, viruses, mold, protozoa or insects, with or without manifest disease. 37. Inflammation The reaction of tissue to injury characterized clinically by heat, swelling, redness and pain *Description intentionally left blank. May 25, 2021 Injury Description Codes Nature of Injury 38. Adverse reaction to a vaccination or * inoculation 40. -

National System for Recording and Notification of Occupational Diseases Practical Guide
InternationalInternational LabourLabour OfficeOffice GenevaGeneva National System for Recording and Notification of Occupational Diseases Practical guide Programme on Safety and Health at Work and the Environment (SafeWork) International Labour Organization Route des Morillons 4 CH -1211 Geneva 22 Switzerland TEL. + 41 22 7996715 FAX + 41 22 7996878 E-mail : safework @ ilo.org www.ilo.org / safework ILO National System for Recording and Notification of Occupational Diseases – Practical guide ISBN 978-92-2-127057-7 9 789221 270577 Programme on Safety and Health at Work and the Environment (SafeWork) National System for Recording and Notification of Occupational Diseases Practical guide International Labour Office, Geneva Copyright © International Labour Organization 2013 First published 2013 Publications of the International Labour Office enjoy copyright under Protocol 2 of the Universal Copyright Convention. Never- theless, short excerpts from them may be reproduced without authorization, on condition that the source is indicated. For rights of reproduction or translation, application should be made to ILO Publications (Rights and Permissions), International Labour Office, CH-1211 Geneva 22, Switzerland, or by email: [email protected]. The International Labour Office welcomes such applications. Libraries, institutions and other users registered with reproduction rights organizations may make copies in accordance with the licences issued to them for this purpose. Visit www.ifrro.org to find the reproduction rights organization in your country. -

F252-117-000 Occupational Disease Claims in Workers' Compensation
Occupational Disease Claims in Workers’ Compensation Coal miner Lee Hipshire, 1976. Courtesy of Earl Dotter. Working together to keep people working Occupational Disease Claims in Workers' Compensation Occupational diseases are different from occupational injuries. Occupational diseases are defined clinically, but in the workers’ compensation system, they are also defined legally. So that you can help workers who may be experiencing an occupational disease, this document will help you understand how the Department of Labor & Industries (L&I), or the self-insured employer, decides which claims to approve, or allow, due to occupational disease. This manual also explains how to gather the employment history needed to manage occupational disease claims and what conditions must be reported to L&I or another agency. Carpal tunnel syndrome, noise-induced hearing loss, and asthma, when work- related, are examples of conditions that L&I considers occupational diseases. When making determinations about occupational disease claims, it is important for health-care providers to keep in mind the following principles: A. Occupational disease claims must be filed within two years following the date the worker receives written notice from a physician that the occupational disease exists and a claim for disability benefits may be filed.1 B. Occupational disease is defined as an infection or disease that “arises naturally and proximately” out of employment.2 C. Claims based on mental conditions caused by stress are excluded from the occupational disease definition.3 Criteria for allowance of occupational disease claims To determine allowance of an occupational disease, claim managers use the following criteria: A. A physician must present an opinion that work conditions, on a more- probable-than-not basis (a greater than 50% chance), are a cause of the disease or have aggravated or “lit up” a preexisting condition; AND B.