Compartment Syndrome Craig Young MD
Total Page:16
File Type:pdf, Size:1020Kb
Load more
Recommended publications
-

Case Report Forearm Compartment Syndrome Following Thrombolytic Therapy for Massive Pulmonary Embolism: a Case Report and Review of Literature
Hindawi Publishing Corporation Case Reports in Orthopedics Volume 2011, Article ID 678525, 4 pages doi:10.1155/2011/678525 Case Report Forearm Compartment Syndrome following Thrombolytic Therapy for Massive Pulmonary Embolism: A Case Report and Review of Literature Ravi Badge and Mukesh Hemmady Department of Trauma and Orthopaedics Surgery, Wrightington, Wigan and Leigh NHS Trust, Wigan WN1 2NN, UK Correspondence should be addressed to Ravi Badge, [email protected] Received 2 November 2011; Accepted 6 December 2011 Academic Editor: M. K. Lyons Copyright © 2011 R. Badge and M. Hemmady. This is an open access article distributed under the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original work is properly cited. Use of thrombolytic therapy in pulmonary embolism is restricted in cases of massive embolism. It achieves faster lysis of the thrombus than the conventional heparin therapy thus reducing the morbidity and mortality associated with PE. The compartment syndrome is a well-documented, potentially lethal complication of thrombolytic therapy and known to occur in the limbs involved for vascular lines or venepunctures. The compartment syndrome in a conscious and well-oriented patient is mainly diagnosed on clinical ground with its classical signs and symptoms like disproportionate pain, tense swollen limb and pain on passive stretch. However these findings may not be appropriately assessed in an unconscious patient and therefore the clinicians should have high index of suspicion in a patient with an acutely swollen tense limb. In such scenarios a prompt orthopaedic opinion should be considered. In this report, we present a case of acute compartment syndrome of the right forearm in a 78 years old male patient following repeated attempts to secure an arterial line for initiating the thrombolytic therapy for the management of massive pulmonary embolism. -

Orthopedic Trauma Postoperative Care and Rehab
Orthopedic Trauma Postoperative Care and Rehab Serge Charles Kaska, MD Name that Beach 100$ Still 100$ 75$ 50$ 1$ Omaha • June 6th 1941 • !st Infantry Division • 2000 KIA LIFE OR LIMB THREAT 1. Compartment Syndrome 2. Fat Emboli Syndrome 3. Pulmonary Embolism 4. Shock Compartment syndrome case A 16 year old male was retrieving a tire from his truck bed on the side of the highway in the pouring rain when a car careens off of the road and sandwiches the patients legs between the bumpers at freeway speed. Acute compartment syndrome Compartment syndrome DEFINED Definition: Elevated tissue pressure within a closed fascial space • Pathogenesis – Too much in-flow: results in edema or hemorrhage – Decreased outflow: results in venous obstruction caused by tight dressing and/or cast. • Reduces tissue perfusion • Results in cell death Compartment syndrome tissue survival • Muscle – 3-4 hours: reversible changes – 6 hours: variable damage – 8 hours: irreversible changes • Nerve – 2 hours: looses nerve conduction – 4 hours: neuropraxia – 8 hours: irreversible changes Physical exam 1. Pain 2. Pain 3. Pain Physical exam • Inspection – Swelling, skin is tight and shiny • Motion – Active motion will be refused or unable. Must see dorsiflexion • Palpation – Severe pain with palpation • Alarming pain with passive stretch Physical exam • Dorsiflexion Physical Exam • Palpation – Severe pain with palpation • Alarming pain with passive stretch Physical exam • Evaluations from nurses, therapists, and orthotech’s are CRITICAL • If you call a doctor and say that -
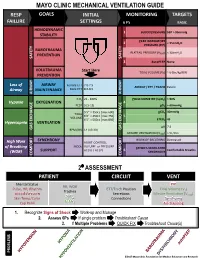
Mechanical Ventilation Guide
MAYO CLINIC MECHANICAL VENTILATION GUIDE RESP GOALS INITIAL MONITORING TARGETS FAILURE SETTINGS 6 P’s BASIC HEMODYNAMIC 1 BLOOD PRESSURE SBP > 90mmHg STABILITY PEAK INSPIRATORY 2 < 35cmH O PRESSURE (PIP) 2 BAROTRAUMA PLATEAU PRESSURE (P ) < 30cmH O PREVENTION PLAT 2 SAFETY SAFETY 3 AutoPEEP None VOLUTRAUMA Start Here TIDAL VOLUME (V ) ~ 6-8cc/kg IBW PREVENTION T Loss of AIRWAY Female ETT 7.0-7.5 AIRWAY / ETT / TRACH Patent Airway MAINTENANCE Male ETT 8.0-8.5 AIRWAY AIRWAY FiO2 21 - 100% PULSE OXIMETRY (SpO2) > 90% Hypoxia OXYGENATION 4 PEEP 5 [5-15] pO2 > 60mmHg 5’5” = 350cc [max 600] pCO2 40mmHg TIDAL 6’0” = 450cc [max 750] 5 VOLUME 6’5” = 500cc [max 850] ETCO2 45 Hypercapnia VENTILATION pH 7.4 GAS GAS EXCHANGE BPM (RR) 14 [10-30] GAS EXCHANGE MINUTE VENTILATION (VMIN) > 5L/min SYNCHRONY WORK OF BREATHING Decreased High Work ASSIST CONTROL MODE VOLUME or PRESSURE of Breathing PATIENT-VENTILATOR AC (V) / AC (P) 6 Comfortable Breaths (WOB) SUPPORT SYNCHRONY COMFORT COMFORT 2⁰ ASSESSMENT PATIENT CIRCUIT VENT Mental Status PIP RR, WOB Pulse, HR, Rhythm ETT/Trach Position Tidal Volume (V ) Trachea T Blood Pressure Secretions Minute Ventilation (V ) SpO MIN Skin Temp/Color 2 Connections Synchrony ETCO Cap Refill 2 Air-Trapping 1. Recognize Signs of Shock Work-up and Manage 2. Assess 6Ps If single problem Troubleshoot Cause 3. If Multiple Problems QUICK FIX Troubleshoot Cause(s) PROBLEMS ©2017 Mayo Clinic Foundation for Medical Education and Research CAUSES QUICK FIX MANAGEMENT Bleeding Hemostasis, Transfuse, Treat cause, Temperature control HYPOVOLEMIA Dehydration Fluid Resuscitation (End points = hypoxia, ↑StO2, ↓PVI) 3rd Spacing Treat cause, Beware of hypoxia (3rd spacing in lungs) Pneumothorax Needle D, Chest tube Abdominal Compartment Syndrome FLUID Treat Cause, Paralyze, Surgery (Open Abdomen) OBSTRUCTED BLOOD RETURN Air-Trapping (AutoPEEP) (if not hypoxic) Pop off vent & SEE SEPARATE CHART PEEP Reduce PEEP Cardiac Tamponade Pericardiocentesis, Drain. -

Acute Compartment Syndrome Complicating Deep Venous Thrombosis
SMGr up Case Report SM Journal of Acute Compartment Syndrome Case Reports Complicating Deep Venous Thrombosis Senthil Dhayalan1*, David Jardine1*, Tony Goh2 and Nicholas Lash3 1Senior registrar and General Physician, Dept of General Medicine, NZ 2Consultant Radiologist, Dept of Radiology, NZ 3Orthopaediac Surgeon, Dept of Orthopaedics, NZ A 40-yr old, heavily-built man initially presented to his general practitioner 2 days before Article Information admission with recent onset of pain and swelling in his left calf. A duplex ultrasound scan Received date: Nov 21, 2018 demonstrated a popliteal and lower leg deep vein thrombosis [DVT], extending 15 cm above the Accepted date: Nov 26, 2018 knee into the femoral vein. He was started appropriately on enoxaparin 130 mg bd. Despite the Published date: Nov 27, 2018 treatment, the pain got worse, particularly when standing, and he was admitted for symptom control. Five weeks earlier he had undergone anterior cruciate ligament repair of the left knee, *Corresponding author [without heparin prophylaxis] and made a satisfactory recovery (Figure 1). Jardine D, General Medicine On examination he was mildly distressed with a low-normal blood pressure [110/70 mmHg] Department, Christchurch hospital, and a persistent low-grade fever [temperature ranged from 37.0-37.8 oC]. The left leg was moderately Private Bag 4710, Christchurch 8140, diffusely swollen, slightly warm and darker in colour [figure]. The pain was localised to the posterior New Zealand, compartments and was exacerbated by dorsi-flexing the ankle and squeezing the gastrocnemius. Email: [email protected] There were no signs of joint effusion, thrombophlebitis, lymphadenopathy or cellulitis. -

Bilateral Atraumatic Compartment Syndrome of the Legs Leading to Rhabdomyolysis and Acute Renal Failure Following Prolonged Kneeling in a Heroin Addict
PAJT 10.5005/jp-journals-10030-1075 CASE REPORTBilateral Atraumatic Compartment Syndrome of the Legs Leading to Rhabdomyolysis and Acute Renal Failure Bilateral Atraumatic Compartment Syndrome of the Legs Leading to Rhabdomyolysis and Acute Renal Failure Following Prolonged Kneeling in a Heroin Addict. A Case Report and Review of Relevant Literature Saptarshi Biswas, Ramya S Rao, April Duckworth, Ravi Kothuru, Lucio Flores, Sunil Abrol ABSTRACT cerrado, que interfiere con la circulación de los componentes mioneurales del compartimento. Síndrome compartimental Introduction: Compartment syndrome is defined as a symptom bilateral de las piernas es una presentación raro que requiere complex caused by increased pressure of tissue fluid in a closed una intervención quirúrgica urgente. En un reporte reciente osseofascial compartment which interferes with circulation (Khan et al 2012), ha habido reportados solo 8 casos de to the myoneural components of the compartment. Bilateral síndrome compartimental bilateral. compartment syndrome of the legs is a rare presentation Se sabe que el abuso de heroína puede causar el síndrome requiring emergent surgical intervention. In a recent case report compartimental y rabdomiólisis traumática y atraumática. El (Khan et al 2012) there have been only eight reported cases hipotiroidismo también puede presentarse independiente con cited with bilateral compartment syndrome. rabdomiólisis. Heroin abuse is known to cause compartment syndrome, traumatic and atraumatic rhabdomyolysis. Hypothyroidism can Presentación del caso: Presentamos un caso de una mujer also independently present with rhabdomyolysis. de 22 años quien presentó con tumefacción bilateral de las piernas asociado con la perdida de la sensación, después Case presentation: We present a case of a 22 years old female de pasar dos días arrodillado contra una pared después de who presented with bilateral swelling of the legs with associated usar heroína intravenosa. -

Assessment, Management and Decision Making in the Treatment of Polytrauma Patients with Head Injuries
Compartment Syndrome Andrew H. Schmidt, M.D. Professor, Dept. of Orthopedic Surgery, Univ. of Minnesota Chief, Department of Orthopaedic Surgery Hennepin County Medical Center April 2016 Disclosure Information Andrew H. Schmidt, M.D. Conflicts of Commitment/ Effort Board of Directors: OTA Critical Issues Committee: AOA Editorial Board: J Knee Surgery, J Orthopaedic Trauma Medical Director, Director Clinical Research: Hennepin County Med Ctr. Disclosure of Financial Relationships Royalties: Thieme, Inc.; Smith & Nephew, Inc. Consultant: Medtronic, Inc.; DGIMed; Acumed; St. Jude Medical (spouse) Stock: Conventus Orthopaedics; Twin Star Medical; Twin Star ECS; Epien; International Spine & Orthopedic Institute, Epix Disclosure of Off-Label and/or investigative Uses I will not discuss off label use and/or investigational use in my presentation. Objectives • Review Pathophysiology of Acute Compartment Syndrome • Review Current Diagnosis and Treatment – Risk Factors – Clinical Findings – Discuss role and technique of compartment pressure monitoring. Pathophysiology of Compartment Syndrome Pressure Inflexible Fascia Injured Muscle Vascular Consequences of Elevated Intracompartment Pressure: A-V Gradient Theory Pa (High) Pv (Low) artery arteriole capillary venule vein Local Blood Pa - Pv Flow = R Matsen, 1980 Increased interstitial pressure Pa (High) Tissue ischemia artery arteriole capillary venule vein Lysis of cell walls Release of osmotically active cellular contents into interstitial fluid Increased interstitial pressure More cellular -

Western Trauma Association Critical Decisions in Trauma: Penetrating Chest Trauma
WTA 2014 ALGORITHM Western Trauma Association Critical Decisions in Trauma: Penetrating chest trauma Riyad Karmy-Jones, MD, Nicholas Namias, MD, Raul Coimbra, MD, Ernest E. Moore, MD, 09/30/2020 on BhDMf5ePHKav1zEoum1tQfN4a+kJLhEZgbsIHo4XMi0hCywCX1AWnYQp/IlQrHD3Ypodx1mzGi19a2VIGqBjfv9YfiJtaGCC1/kUAcqLCxGtGta0WPrKjA== by http://journals.lww.com/jtrauma from Downloaded Martin Schreiber, MD, Robert McIntyre, Jr., MD, Martin Croce, MD, David H. Livingston, MD, Jason L. Sperry, MD, Ajai K. Malhotra, MD, and Walter L. Biffl, MD, Portland, Oregon Downloaded from http://journals.lww.com/jtrauma his is a recommended algorithm of the Western Trauma Historical Perspective TAssociation for the acute management of penetrating chest The precise incidence of penetrating chest injury, varies injury. Because of the paucity of recent prospective randomized depending on the urban environment and the nature of the trials on the evaluation and management of penetrating chest review. Overall, penetrating chest injuries account for 1% to injury, the current algorithms and recommendations are based 13% of trauma admissions, and acute exploration is required in by on available published cohort, observational and retrospective BhDMf5ePHKav1zEoum1tQfN4a+kJLhEZgbsIHo4XMi0hCywCX1AWnYQp/IlQrHD3Ypodx1mzGi19a2VIGqBjfv9YfiJtaGCC1/kUAcqLCxGtGta0WPrKjA== 5% to 15% of cases; exploration is required in 15% to 30% of studies, and the expert opinion of the Western Trauma Asso- patients who are unstable or in whom active hemorrhage is ciation members. The two algorithms should be reviewed in the suspected. Among patients managed by tube thoracostomy following sequence: Figure 1 for the management and damage- alone, complications including retained hemothorax, empy- control strategies in the unstable patient and Figure 2 for the ema, persistent air leak, and/or occult diaphragmatic injuries management and definitive repair strategies in the stable patient. -

Secondary Abdominal Compartment Syndrome Following Severe Extremity Injury: Unavoidable Or Unnecessary?
Session IV Poster # 1 SECONDARY ABDOMINAL COMPARTMENT SYNDROME FOLLOWING SEVERE EXTREMITY INJURY: UNAVOIDABLE OR UNNECESSARY? Bryan A Cotton MD, Michael C Madigan BS, Clinton D Kemp MD, J Chad Johnson MD PhD, John A Morris Jr MD*, Vanderbilt University Medical Center, Nashville, TN Introduction: Secondary abdominal compartment syndrome (2ACS) is the development of ACS in the absence of abdominal injury. 2ACS is often viewed as an unavoidable sequela of the large volume crystalloid resuscitation “required” to treat severe shock. We hypothesized that early, aggressive resuscitation techniques place patients with severe extremity injuries at risk for developing 2ACS. Methods: The TRACS database was queried for all patients with extremity AIS of 3 or greater and abdominal AIS of 0 treated at our institution between 01/01/2001-12/31/2005. The study group included those patients who developed 2ACS, while the comparison cohort included those who did not develop 2ACS. Results: 48 patients developed 2 ACS and were compared to 48 randomly sampled patients who had extremity AIS of ? 3 and abdomen AIS of 0. There were no differences between the groups with respect to age, sex, race, or individual AIS scores. However, the 2ACS group had a higher ISS (25.6 vs 21.4, p=0.02), higher OR crystalloid administration (9.9 L vs 2.7 L, p<0.001), and more frequent use of a rapid infuser (12.5% vs 0.0%, p=0.01). 65% of those who developed 2ACS did so within 12 hours of admission. Multiple logistic regression identified pre-hospital and ED crystalloid volume as predictors of 2ACS. -

Idiopathic Acute Compartment Syndrome of the Leg with Incidental Deep Venous Thrombosis: a Case Report
Open Access Case Report DOI: 10.7759/cureus.5130 Idiopathic Acute Compartment Syndrome of the Leg with Incidental Deep Venous Thrombosis: A Case Report Ehizogie Edigin 1 , Hafeez Shaka 1 1. Internal Medicine, John H. Stroger Jr. Hospital of Cook County, Chicago, USA Corresponding author: Ehizogie Edigin, [email protected] Abstract Acute compartment syndrome (ACS) is an emergency. The majority of cases are caused by underlying trauma, especially fractures. Idiopathic atraumatic ACS of the leg is very rare. The diagnosis and management of ACS should focus on the clinical presentation to avoid delay in fasciotomy for limb salvage. ACS of the leg can be caused by massive proximal iliofemoral thrombosis and rarely occlusive popliteal vein thrombosis with total or near total occlusion. Nonocclusive distal popliteal vein thrombosis, especially if chronic, does not cause ACS and when seen in a patient with ACS, it is likely an incidental finding rather than the cause of the compartment syndrome. This is a case of idiopathic ACS of the right leg occurring in the presence of an incidental right chronic nonocclusive distal popliteal vein thrombosis. Categories: Cardiology, Emergency Medicine, Orthopedics Keywords: acute compartment syndrome, deep vein thrombosis, anticoagulation, fasciotomy, idiopathic acute compartment syndrome, spontaneous acute compartment syndrome, acute extremity compartment syndrome Introduction Acute compartment syndrome (ACS) occurs when increased pressure within a compartment, bounded by unyielding fascial membranes, compromises the circulation and function of the tissues within that space [1]. This increased pressure compromises the function and with time, the viability of the limb affected. However, the diagnosis can be challenging as the symptoms associated with ACS can also be found in other often more common conditions [2]. -

Acute Compartment Syndrome of the Foot After an Ankle Sprain: a Case Report
Journal of Research and Practice on the Musculoskeletal System JOURNAL OF RESEARCH AND PRACTICE ON THE MUSCULOSKELETAL SYSTEM Case Report Acute compartment syndrome of the foot after an ankle sprain: a case report Christos Christoforidis, Panagiotis Lepetsos, Stamatios Papadakis, Anastasios Gketsos, Theodoros Balfousias, George Macheras 4th Orthopaedic Department, KAT Hospital, Athens, Greece Abstract The aim of this study is to report the case of a patient with an acute foot compartment syndrome after an ankle sprain, discussing the diagnostic challenges and rarity of such an uncommon complication of a very common and low-trauma event. A 19-year old young man presented at the emergency department for a twisting injury of his left ankle. Physical and radiological evaluation revealed a 2nd degree lateral ankle sprain and the patient was treated conservatively. Two days later, the patient returned to the emergency department, late at night, with worsening and excruciating pain of his left foot and inability to walk. Physical evaluation showed severe swelling of the left foot and decreased range of active and passive motion. X-rays and CT scan were negative for fractures. An emergency fasciotomy of the lateral and medial compartment of the foot was performed and necrotic muscle parts were removed. Postoperatively, patient’s symptoms were controlled and a week later he was discharged from the hospital. Twelve months later, the patient is pain-free with full range of motion of his left ankle and foot. Keywords: Acute compartment syndrome, Ankle sprain,Fasciotomy, Muscle necrosis, Intracompartmental pressure Introduction normal. Anteroposterior and lateral X-rays of the ankle joint were negative for fracture. -

ORIGINAL ARTICLES Surgical Treatment for 'Brain Compartment Syndrome' in Children with Severe Head Injury
ORIGINAL ARTICLES Surgical treatment for ‘brain compartment syndrome’ in children with severe head injury A A Figaji, A G Fieggen, A Argent, J C Peter Objectives. Traumatic brain injury accounts for a high Outcome measures. Computed tomography (CT) scanning, ICP percentage of deaths in children. Raised intracranial pressure control, clinical outcome. (ICP) due to brain swelling within the closed compartment of Results. Despite the very poor clinical condition of these the skull leads to death or severe neurological disability if not children preoperatively, aggressive management of the raised effectively treated. We report our experience with 12 children pressure resulted in unexpectedly good outcomes. who presented with cerebral herniation due to traumatic brain Conclusion. Aggressive surgical measures to decrease ICP in swelling in whom decompressive craniectomy was used as an the emergency situation can be of considerable benefit; the emergency. key concepts are selection of appropriate patients and early Design. Prospective, observational. intervention. Setting. Red Cross Children’s Hospital. S Afr Med J 2006; 96: 969-975. Subjects. Children with severe traumatic brain injury and cerebral swelling. Compartment syndrome of the limbs or the abdomen is sustained at the moment of impact, it is now recognised that a well-known entity in general surgical and orthopaedic avoidance or early treatment of secondary insults can make a practice, characterised by an increase of pressure within dramatic difference to outcome in individual patients.2 Of these a musculofascial compartment leading to progressive secondary insults, raised ICP is the most widely recognised. neurovascular dysfunction. Although it has not been described Space-occupying traumatic haematomas causing raised as such, raised pressure within the intracranial compartment is ICP are readily removed via emergency craniotomy, thereby arguably the most dramatic example of the same pathological relieving pressure on the brain. -

Upper Extremity Acute Compartment Syndrome During Tissue Plasminogen Activator Therapy for Pulmonary Embolism in a Morbidly Obese Patient
CASE REPORT – OPEN ACCESS International Journal of Surgery Case Reports 8 (2015) 175–178 View metadata, citation and similar papers at core.ac.uk brought to you by CORE Contents lists available at ScienceDirect provided by Elsevier - Publisher Connector International Journal of Surgery Case Reports journal homepage: www.casereports.com Upper extremity acute compartment syndrome during tissue plasminogen activator therapy for pulmonary embolism in a morbidly obese patient Serkan Tuna a, Tahir Mutlu Duymus b, Serhat Mutlu b,∗, Ismail Emre Ketenci a, Ayhan Ulusoy a a Department of Orthopaedics, Haydarpasa Numune Training Research Hospital, Istanbul, Turkey b Department of Orthopaedics, Kanuni Sultan Suleyman Training and Research Hospital, Istanbul, Turkey article info abstract Article history: INTRODUCTION: Deep vein thrombosis (DVT) and pulmonary embolism (PE) are more frequently observed Received 2 October 2014 in morbidly obese patients. Tissue plasminogen activator (tPA) is a thrombolytic agent which dissolves Received in revised form 11 January 2015 the thrombus more rapidly than conventional heparin therapy and reduces the mortality and morbidity Accepted 13 January 2015 rates associated with PE. Compartment syndrome is a well-known and documented complication of Available online 15 January 2015 thrombolytic treatment. In awake, oriented and cooperative patients, the diagnosis of compartment syndrome is made based on clinical findings including swelling, tautness, irrational and continuous pain, Keywords: altered sensation, and severe pain due to passive stretching. These clinical findings may not be able to be Compartment syndrome Fasciotomy adequately assessed in unconscious patients. Morbid obesity PRESENTATION OF CASE: In this case report, we present compartment syndrome observed, for which tPA fasciotomy was performed on the upper right extremity of a 46-year old morbidly obese, conscious female patient who was receiving tPA due to a massive pulmonary embolism.